Mediastinal mass differential diagnosis
|
Mediastinal mass Microchapters |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Trusha Tank, M.D.[2]
Overview
The mediastinum is a non-delineated group of structures in the thorax (chest), surrounded by loose connective tissue. It is the central compartment of the thoracic cavity. It contains the heart, the great vessels of the heart, esophagus, trachea, thymus, and lymph nodes of the central chest. A wide variety of diseases involving mediastinal structures may present as a mediastinal mass or widening of the mediastinum on imaging studies. Mediastinal widening is diagnosed by the mediastinum measuring greater than 8 cm in width on PA chest x-ray. The mediastinal mass may present with symptoms or even without any symptoms. Mediastinal mass may cause a variety of symptoms by the mass pressing against surrounding mediastinal structures, collectively known as mediastinal syndrome. Mediastinal may can be differentiated depending on their location in mediastinal cavity into: Anterior mediastinal mass, middle mediastinal mass, or posterior mediastinal mass. Mediastinal mass may also be differentiated according to the content of the mass such as: cystic, fatty or solid (tumor).
Mediastinal Mass Differential Diagnosis
Wide variety of medical conditions can present as a mediastinal mass on radiological imaging.
- Mediastinal mass may cause obstruction, entrapment or infiltration of other mediastinal organs such as: trachea, bronchi, esophagus, aorta, superior vena cava (SVC), or heart.
- Symptoms caused by any kind of mediastinal mass is collectively known as: Mediastinal syndrome
- Mediastinal syndrome includes:
- Symptoms caused by compression of the trachea: Dyspnea and respiratory insufficiency.
- Symptoms caused by compression of the esophagus: Dysphagia.
- Symptoms caused by compression of SVC causes superior vena cava syndrome: Vein distention, edema of the face or upper extremities and a positive Pemberton's sign.
- Pemberton's sign: Development of suffusion, plethora, or duskiness upon elevation of the arms above the head in patient
- Superior vena cava syndrome is the most severe complication of mediastinal syndrome and a medical emergency.
| ABBREVIATIONS: N/A: Not available, SOB: Shortness of breath, M/C: Most common, RI: Respiratory insufficiency, NM: Neuromuscular system, SVCS: Superior vena cava syndrome, SLE: Systemic lupus erythematosus disease, T3: Triiodothyronine, T4: Thyroxine, TSH: Thyroid stimulating hormone, TFT: Thyroid function test, MRI: Magnetic resonance imaging, CNS: Central nervous system, CSF: Cerebrospinal fluid, FNA: Fine needle aspiration, CBC: Complete blood count, COPD: Chronic obstructive pulmonary disease, AIDS: Acquired immune deficiency syndrome, HIV: Human immunodeficiency virus, Hep C: Hepatitis C virus, HTLV-1: human T-lymphotropic virus, EBV: Epstein Barr virus, HHV-8: Human herpes virus-8 | ||||||||
| Disease | Causes/risk factors | Clinical presentation | Paraclinical findings | |||||
|---|---|---|---|---|---|---|---|---|
| General symptoms | Mediastinal syndrome | |||||||
| Dyspnea/
RI |
Dysphagia | SVCS | Gold standard | Image | Additional findings | |||
| Anterior mediastinal mass | ||||||||
| Tumors | ||||||||
| Thymoma | + | + | + | Biopsy: | 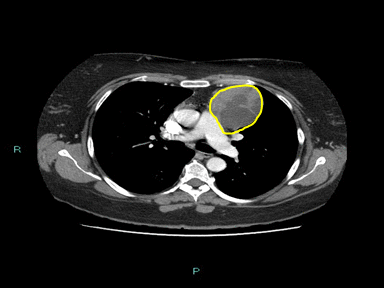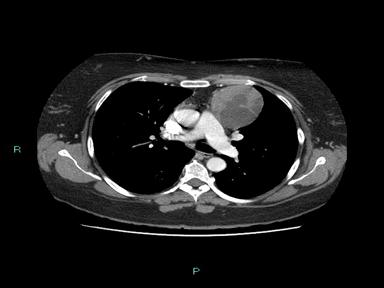 |
Associated condition
| ||
| Disease | Etiology | Symptoms | Dyspnea/
RI |
Dysphagia | SVCS | Gold standard | Image | Additional findings |
| Fatty mass |
|
- | - | - | MRI: | 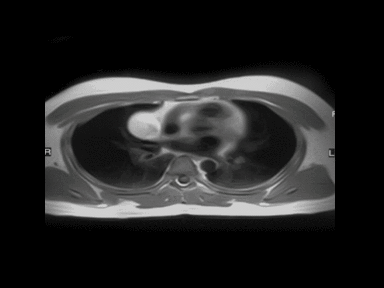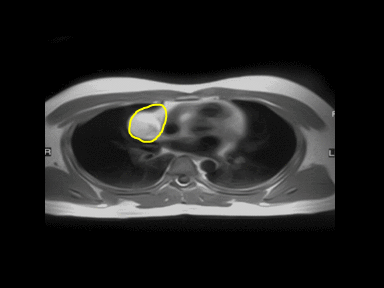 |
Fatty mass can be: | |
| Non-Hodgkin lymphoma |
|
+/- | +/- | +/- | Excisional lymph node biopsy with immunohistochemical study | 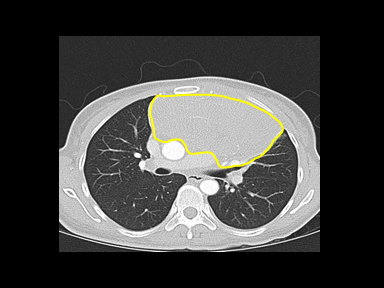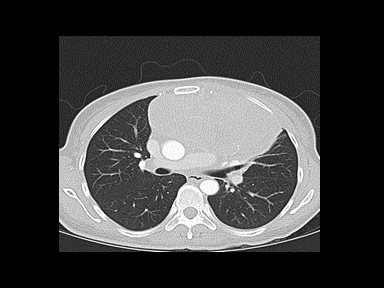 |
| |
| Disease | Etiology | Symptoms | Dyspnea/
RI |
Dysphagia | SVCS | Gold standard | Image | Additional findings |
| Hodgkin's lymphoma | Epstein-Barr virus
|
Other
|
+ | + | +/- | Lymph node biopsy with immunohistochemistry
|
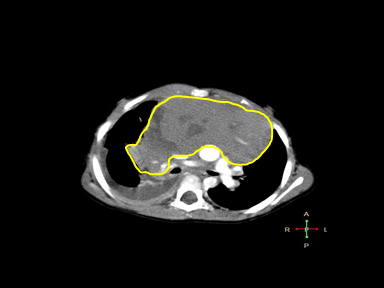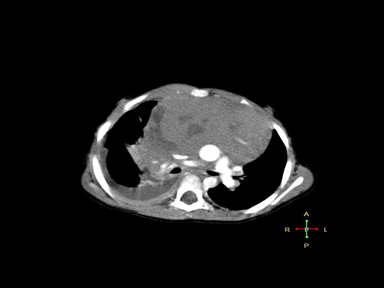 |
Positron emission tomography (PET)
|
| Mediastinal germ cell tumor
(Non-teratomatous) |
|
+ | - | - | Biopsy may help differentiate histopathological subtypes including: | 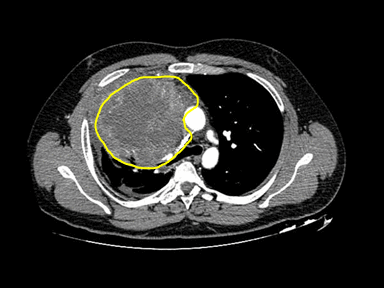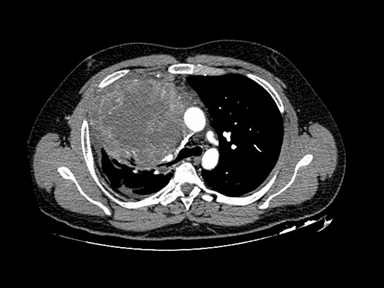 |
CT scan:
Laboratory finding: | |
| Teratoma |
|
Benign
|
+/- | +/- | +/- | Chest CT scan:
|
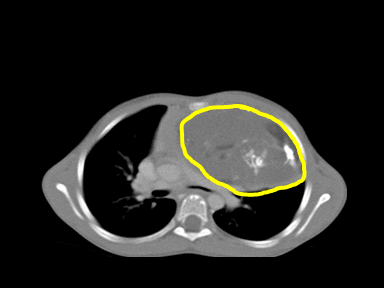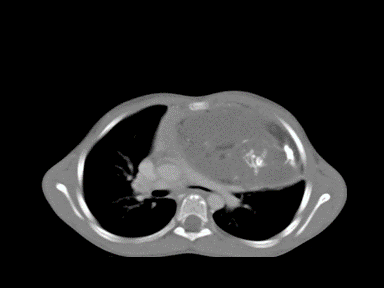 |
|
| Disease | Etiology | Symptoms | Dyspnea/
RI |
Dysphagia | SVCS | Gold standard | Image | Additional findings |
| Cystic mass | ||||||||
| Thymic cyst | Congenital
|
- | - | + | Biopsy with histopathology and cytology | 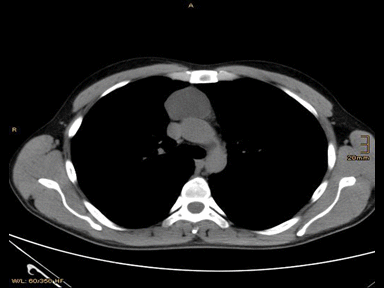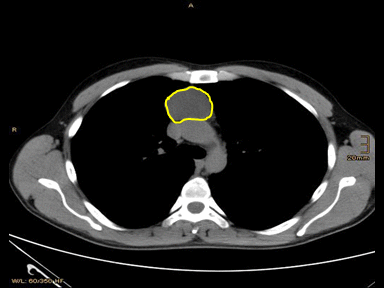 |
CT scan: | |
| Thyroid gland disease | ||||||||
| Mediastinal goiter |
|
+ | + | - | Radioactive iodine scan:
|
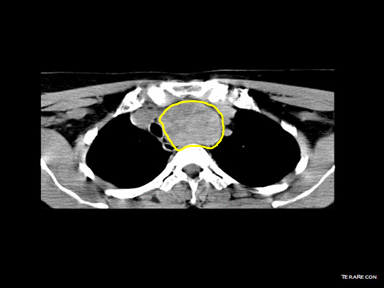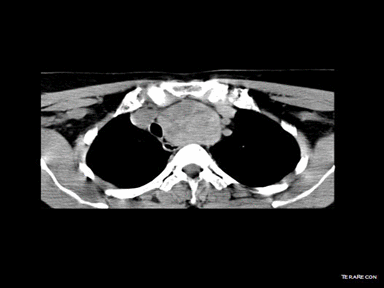 |
Hyperactive gland (hyperthyroid):
Hypoactive gland (hypothyroid): Normal functioning gland (euthyroid): | |
| Disease | Etiology | Symptoms | Dyspnea/
RI |
Dysphagia | SVCS | Gold standard | Image | Additional findings |
| Middle mediastinal mass | ||||||||
| Cardiovascular Disease | ||||||||
| Pericardial effusion |
|
|
+ | +/- | - | Echocardiography guided pericardiocentesis:
|
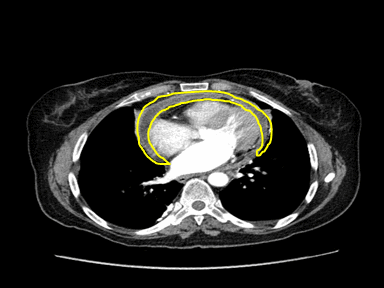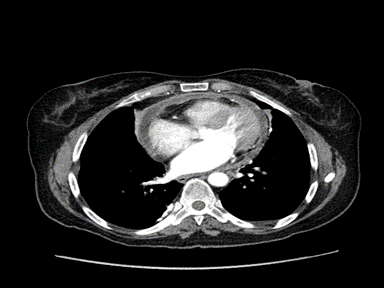 |
Physical findings:
EKG:
|
| Aortic dissection | + | +/- | + | MRI: | 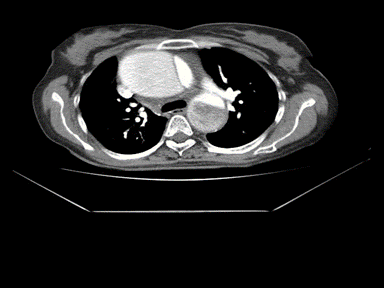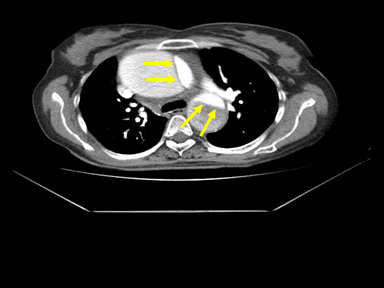 |
TEE:
CTA:
| ||
| Disease | Etiology | Symptoms | Dyspnea/
RI |
Dysphagia | SVCS | Gold standard | Image | Additional findings |
| Superior vena cava obstruction | Compression of SVC from: |
|
+ | + | ++ | Contrast-enhanced CT scan:
|
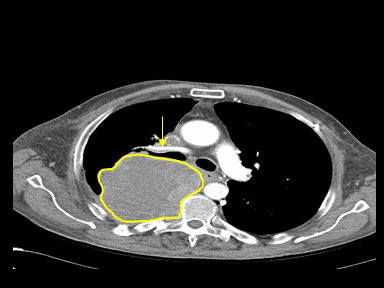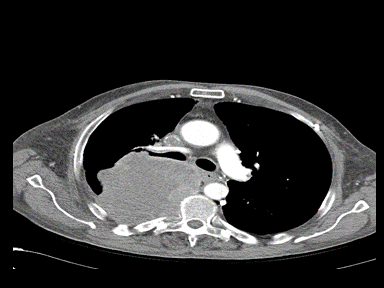 |
Invasive contrast venography:
|
| Partial anomalous pulmonary venous connection |
|
+ | - | - | MRI with contrast:
|
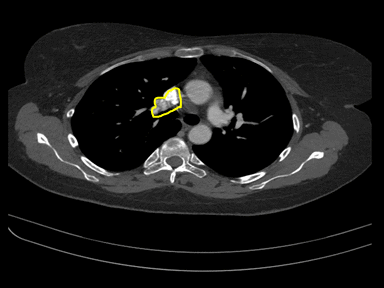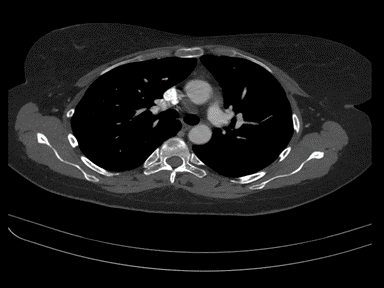 |
Associated with
PFT:
| |
| Gastrointestinal tract disease | ||||||||
| Esophageal achalasia |
|
+ | + | - | High resolution manometry (HRM): | 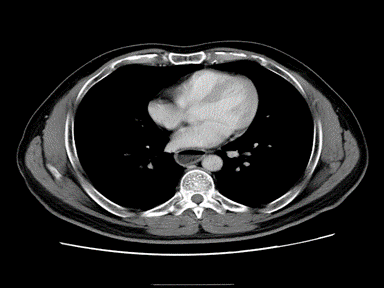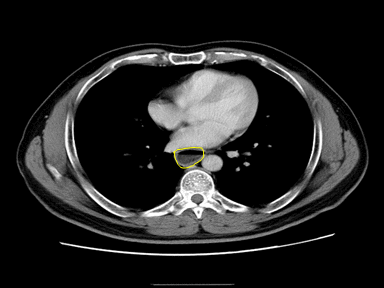 |
X ray:
| |
| Disease | Etiology | Symptoms | Dyspnea/
RI |
Dysphagia | SVCS | Gold standard | Image | Additional findings |
| Esophageal cancer |
|
|
- | + | - | Endoscopy with biopsy:
|
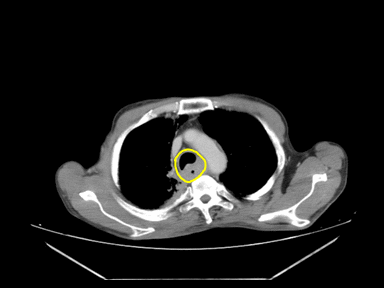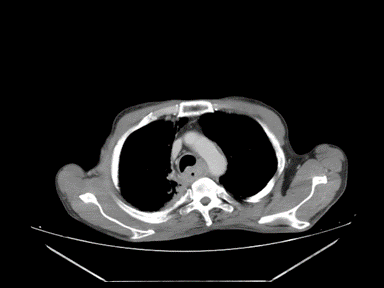 |
Barium swallow:
|
| Esophageal rupture |
|
Other: Patients with cervical perforations can present with |
+ | + | - | Esophagogram:
|
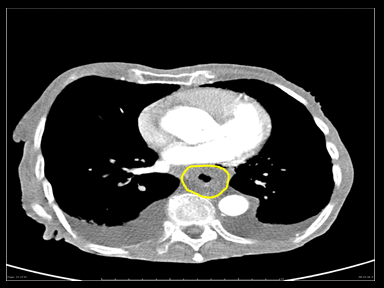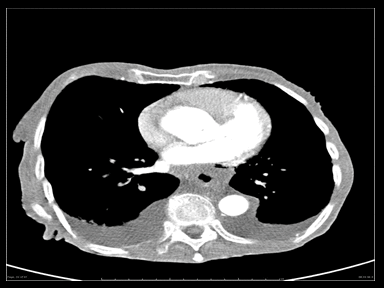 |
CT scan:
|
| Hiatus hernia |
|
- | + | - | High resolution manometry with esophageal pressure topography (EPT):
|
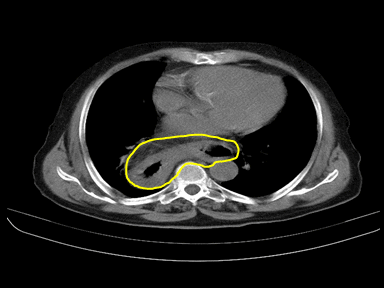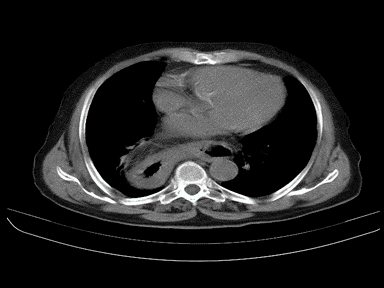 |
Ultrasound:
Ultrasound in pediatric population:
| |
| Disease | Etiology | Symptoms | Dyspnea/
RI |
Dysphagia | SVCS | Gold standard | Image | Additional findings |
| Pulmonary disease | ||||||||
| Hilar lymphadenopathy | Lymphadenopathy:
|
Constituitional symptoms like: | + | - | - | Lymph node biopsy and histopathology | 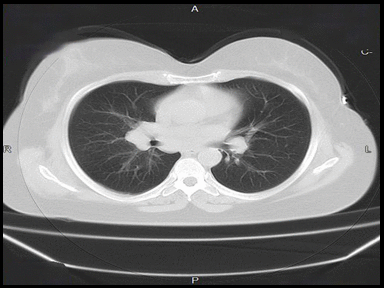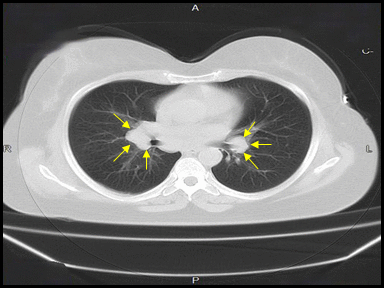 |
CT scan |
| Pneumomediastinum |
|
|
+ | - | - | CT scan:
Pediatric pneumomediastinum: |
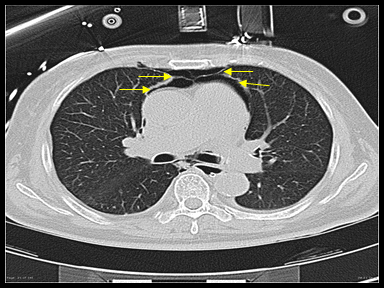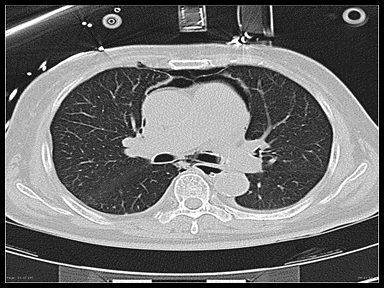 |
Physical exam:
|
| Disease | Etiology | Symptoms | Dyspnea/
RI |
Dysphagia | SVCS | Gold standard | Image | Additional findings |
| Sarcoidosis |
Immune system
|
Cutaneous sarcoidosis
|
+ | - | - | Endoscopy with biopsy and histopathology
|
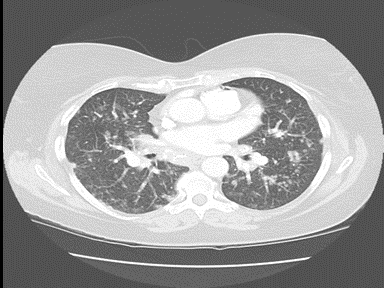 |
Laboratory findings:
|
| Disease | Etiology | Symptoms | Dyspnea/
RI |
Dysphagia | SVCS | Gold standard | Image | Additional findings |
| Infectious disease | ||||||||
| Mediastinitis |
Risk factors: |
+ | - | - | Culture and sensitivity of mediastinal tissue collected by biopsy/aspiration | 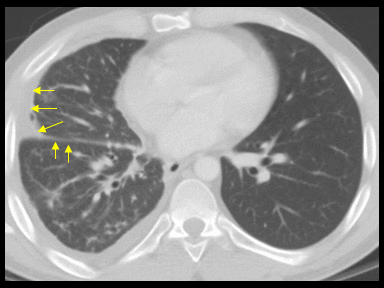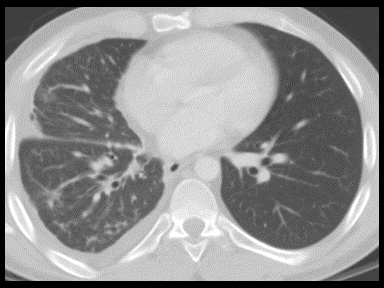 |
Physical exam
| |
| Anthrax | B. anthracis
People at higher risk include
|
+ | - | - | Culture and sensitivity: | 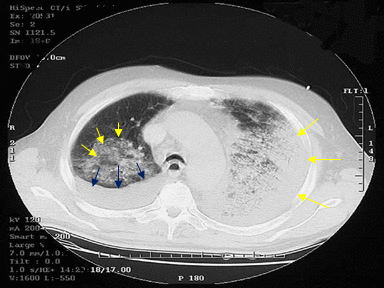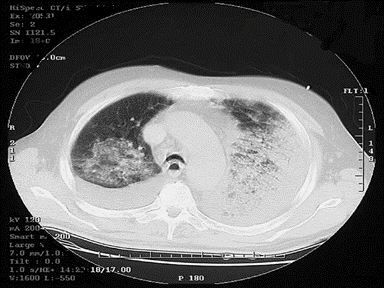 |
CT scan
| |
| Tuberculosis | M. tuberculosis
Traveling or living in endemic regions (Sub-saharan African, Russia, India, Pakistan, China)
The risk of contracting TB increases in:
|
|
+ | - | - | Culture and sensitivity | 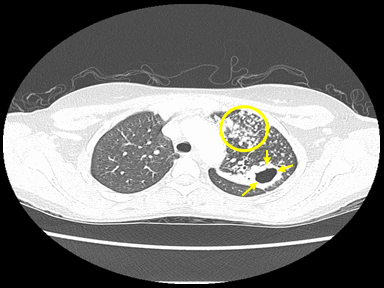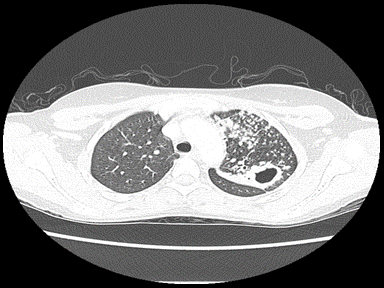 |
Chest X-ray
|
| Disease | Etiology | Symptoms | Dyspnea/
RI |
Dysphagia | SVCS | Gold standard | Image | Additional findings |
| Cystic mass | ||||||||
| Bronchogenic cyst |
|
|
+ | - | - | CT scan | 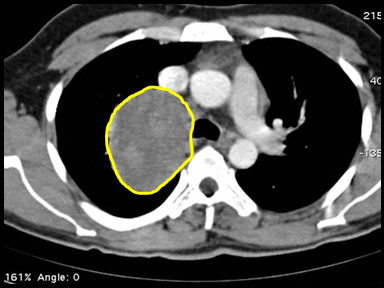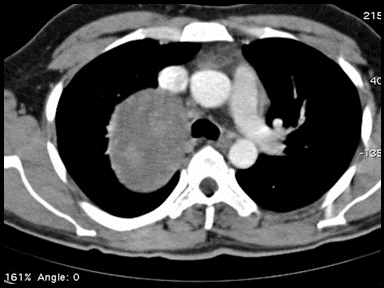 |
CT scan:
|
| Esophageal duplication cysts |
|
|
- | + | - | Endoscopic ultrasound (EUS)
|
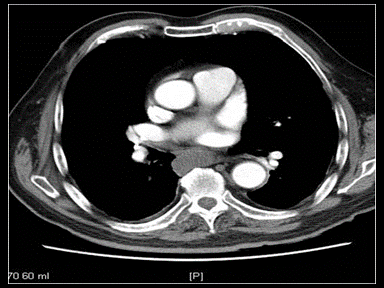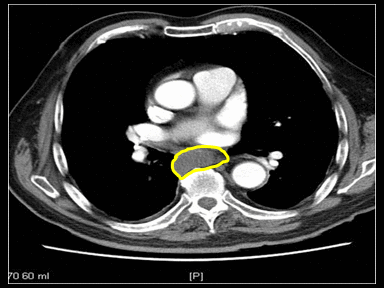 |
Endoscopic ultrasound-guided FNA
|
| Disease | Etiology | Symptoms | Dyspnea/
RI |
Dysphagia | SVCS | Gold standard | Image | Additional findings |
| Lymphangioma |
|
|
+ | + | - | Histopathology and cytology | 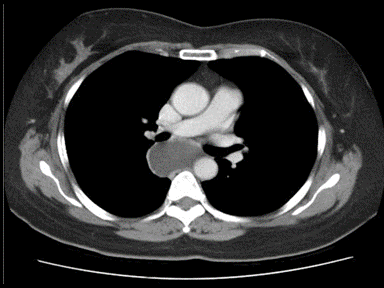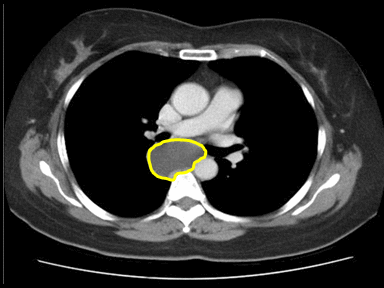 |
|
| Chronic inflammatory disease | ||||||||
| Churg-Strauss syndrome | + | +/- | - | Lung biopsy
4 out of 6 positive :
|
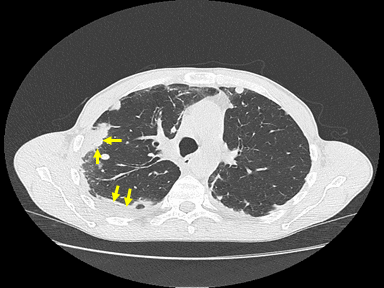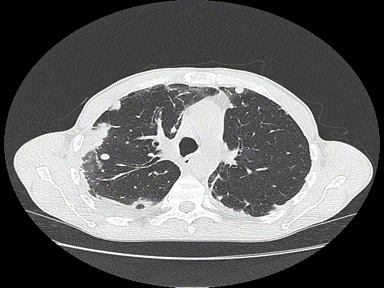 |
High-resolution computerized tomography (HRCT):
| ||
| Disease | Etiology | Symptoms | Dyspnea/
RI |
Dysphagia | SVCS | Gold standard | Image | Additional findings |
| Posterior mediastinal mass | ||||||||
| Cystic mass | ||||||||
| Mediastinal neurenteric cyst | + | +/- | - | CT scan:
|
 |
Postnatal chest X-ray:
| ||
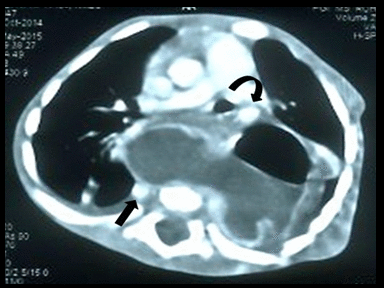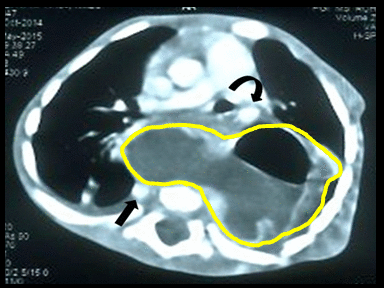
| Pancreatic pseudocyst |
|
- | - | - | Histopathology and cytology of cyst and fluid content | 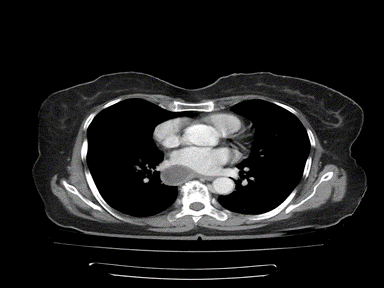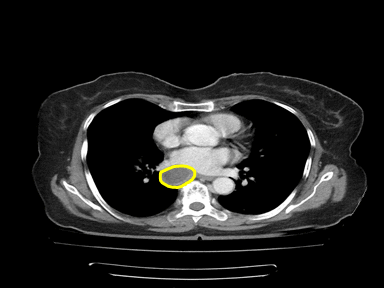 |
CT scan
| |
| Disease | Etiology | Symptoms | Dyspnea/
RI |
Dysphagia | SVCS | Gold standard | Image | Additional findings |
| Central nervous system disease | ||||||||
| Meningocele |
Maternal nutritional factors
Environmental factors
|
Symptoms depend on the severity of the defect
Difficulties with executive functions including:
|
- | - | - | Prenatal 2D/3D ultrasound:
|
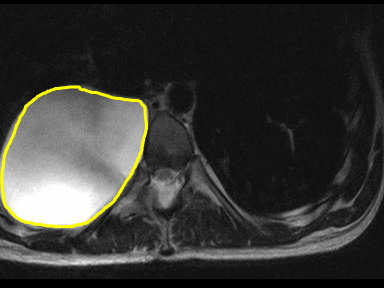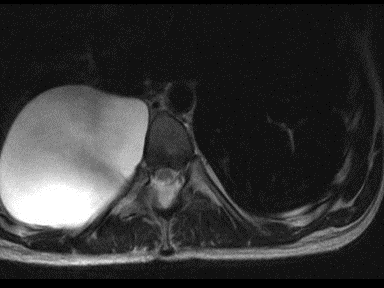 |
Laboratory tests:
MRI:
|
| Neurilemmoma |
|
- | - | - | Biopsy with histopathology | 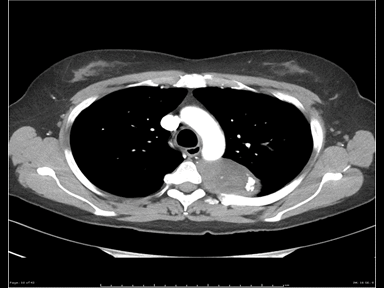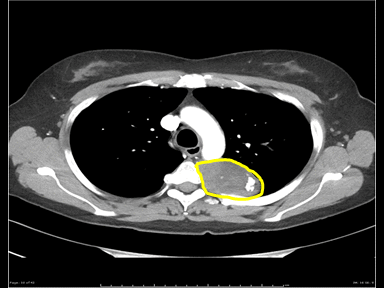 |
MRI | |
| ABBREVIATIONS: N/A: Not available, SOB: Shortness of breath, M/C: Most common, RI: Respiratory insufficiency, NM: Neuromuscular system, SVCS: Superior vena cava syndrome, SLE: Systemic lupus erythematosus disease, T3: Triiodothyronine, T4: Thyroxine, TSH: Thyroid stimulating hormone, TFT: Thyroid function test, MRI: Magnetic resonance imaging, CNS: Central nervous system, CSF: Cerebrospinal fluid, FNA: Fine needle aspiration, CBC: Complete blood count, COPD: Chronic obstructive pulmonary disease, AIDS: Acquired immune deficiency syndrome, HIV: Human immunodeficiency virus, Hep C: Hepatitis C virus, HTLV-1: human T-lymphotropic virus, EBV: Epstein Barr virus, HHV-8: Human herpes virus-8 | ||||||||
References
- ↑ Juanpere S, Cañete N, Ortuño P, Martínez S, Sanchez G, Bernado L (February 2013). "A diagnostic approach to the mediastinal masses". Insights Imaging. 4 (1): 29–52. doi:10.1007/s13244-012-0201-0. PMID 23225215.
- ↑ Scagliori E, Evangelista L, Panunzio A, Calabrese F, Nannini N, Polverosi R; et al. (2015). "Conflicting or complementary role of computed tomography (CT) and positron emission tomography (PET)/CT in the assessment of thymic cancer and thymoma: our experience and literature review". Thorac Cancer. 6 (4): 433–42. doi:10.1111/1759-7714.12197. PMC 4511321. PMID 26273398.
- ↑ Thomas CR, Wright CD, Loehrer PJ (1999). "Thymoma: state of the art". Journal of Clinical Oncology : Official Journal of the American Society of Clinical Oncology. 17 (7): 2280–9. PMID 10561285. Retrieved 2012-01-18. Unknown parameter
|month=ignored (help) - ↑ Juanpere S, Cañete N, Ortuño P, Martínez S, Sanchez G, Bernado L (February 2013). "A diagnostic approach to the mediastinal masses". Insights Imaging. 4 (1): 29–52. doi:10.1007/s13244-012-0201-0. PMID 23225215.
- ↑ Molinari F, Bankier AA, Eisenberg RL (November 2011). "Fat-containing lesions in adult thoracic imaging". AJR Am J Roentgenol. 197 (5): W795–813. doi:10.2214/AJR.11.6932. PMID 22021525.
- ↑ Juanpere S, Cañete N, Ortuño P, Martínez S, Sanchez G, Bernado L (February 2013). "A diagnostic approach to the mediastinal masses". Insights Imaging. 4 (1): 29–52. doi:10.1007/s13244-012-0201-0. PMID 23225215.
- ↑ Sandlund JT (2015). "Non-Hodgkin Lymphoma in Children". Curr Hematol Malig Rep. 10 (3): 237–43. doi:10.1007/s11899-015-0277-y. PMID 26174528.
- ↑ Armitage JO, Gascoyne RD, Lunning MA, Cavalli F (2017). "Non-Hodgkin lymphoma". Lancet. 390 (10091): 298–310. doi:10.1016/S0140-6736(16)32407-2. PMID 28153383.
- ↑ K. J. Flavell & P. G. Murray (2000). "Hodgkin's disease and the Epstein-Barr virus". Molecular pathology : MP. 53 (5): 262–269. PMID 11091850. Unknown parameter
|month=ignored (help) - ↑ J. J. Goedert, T. R. Cote, P. Virgo, S. M. Scoppa, D. W. Kingma, M. H. Gail, E. S. Jaffe & R. J. Biggar (1998). "Spectrum of AIDS-associated malignant disorders". Lancet (London, England). 351 (9119): 1833–1839. PMID 9652666. Unknown parameter
|month=ignored (help) - ↑ M. Tinguely, R. Vonlanthen, E. Muller, C. C. Dommann-Scherrer, J. Schneider, J. A. Laissue & B. Borisch (1998). "Hodgkin's disease-like lymphoproliferative disorders in patients with different underlying immunodeficiency states". Modern pathology : an official journal of the United States and Canadian Academy of Pathology, Inc. 11 (4): 307–312. PMID 9578079. Unknown parameter
|month=ignored (help) - ↑ Vardhana S, Younes A (2016). "The immune microenvironment in Hodgkin lymphoma: T cells, B cells, and immune checkpoints". Haematologica. 101 (7): 794–802. doi:10.3324/haematol.2015.132761. PMC 5004458. PMID 27365459.
- ↑ Hodgkin-lymphoma. Canadian Cancer Society. http://www.cancer.ca/en/cancer-information/cancer-type/hodgkin-lymphoma/diagnosis/?region=ab Accessed on September 11, 2015
- ↑ 14.00 14.01 14.02 14.03 14.04 14.05 14.06 14.07 14.08 14.09 14.10 14.11 14.12 Juanpere S, Cañete N, Ortuño P, Martínez S, Sanchez G, Bernado L (February 2013). "A diagnostic approach to the mediastinal masses". Insights Imaging. 4 (1): 29–52. doi:10.1007/s13244-012-0201-0. PMID 23225215.
- ↑ Juanpere S, Cañete N, Ortuño P, Martínez S, Sanchez G, Bernado L (February 2013). "A diagnostic approach to the mediastinal masses". Insights Imaging. 4 (1): 29–52. doi:10.1007/s13244-012-0201-0. PMID 23225215.
- ↑ Yalagachin GH (June 2013). "Anterior mediastinal teratoma- a case report with review of literature". Indian J Surg. 75 (Suppl 1): 182–4. doi:10.1007/s12262-012-0569-6. PMID 24426558.
- ↑ No TH, Seol SH, Seo GW, Kim DI, Yang SY, Jeong CH, Hwang YH, Kim JY (September 2015). "Benign Mature Teratoma in Anterior Mediastinum". J Clin Med Res. 7 (9): 726–8. doi:10.14740/jocmr2270w. PMC 4522994. PMID 26251691.
- ↑ Juanpere S, Cañete N, Ortuño P, Martínez S, Sanchez G, Bernado L (February 2013). "A diagnostic approach to the mediastinal masses". Insights Imaging. 4 (1): 29–52. doi:10.1007/s13244-012-0201-0. PMID 23225215.
- ↑ "Benign thyroid enlargement (non-toxic multinodular goiter): Overview".
- ↑ Juanpere S, Cañete N, Ortuño P, Martínez S, Sanchez G, Bernado L (February 2013). "A diagnostic approach to the mediastinal masses". Insights Imaging. 4 (1): 29–52. doi:10.1007/s13244-012-0201-0. PMID 23225215.
- ↑ Vanneman MW, Fikry K, Quraishi SA, Schoenfeld W (August 2015). "A Young Man with a Mediastinal Mass and Sudden Cardiac Arrest". Ann Am Thorac Soc. 12 (8): 1235–9. doi:10.1513/AnnalsATS.201504-212CC. PMID 26317273.
- ↑ Salem K, Mulji A, Lonn E (November 1999). "Echocardiographically guided pericardiocentesis - the gold standard for the management of pericardial effusion and cardiac tamponade". Can J Cardiol. 15 (11): 1251–5. PMID 10579740.
- ↑ Juanpere S, Cañete N, Ortuño P, Martínez S, Sanchez G, Bernado L (February 2013). "A diagnostic approach to the mediastinal masses". Insights Imaging. 4 (1): 29–52. doi:10.1007/s13244-012-0201-0. PMID 23225215.
- ↑ Weissmann-Brenner A, Schoen R, Divon MY (2004). "Aortic dissection in pregnancy". Obstet Gynecol. 103 (5 Pt 2): 1110–3. doi:10.1097/01.AOG.0000124984.82336.43. PMID 15121626.
- ↑ Brooke V, Goswami S, Mohanty A, Kasi PM (2012). "Aortic dissection and renal failure in a patient with severe hypothyroidism". Case Rep Med. 2012: 842562. doi:10.1155/2012/842562. PMC 3399550. PMID 22829842.
- ↑ "Classification of diabetic retinopathy from fluorescein angiograms. ETDRS report number 11. Early Treatment Diabetic Retinopathy Study Research Group". Ophthalmology. 98 (5 Suppl): 807–22. 1991. PMID 2062514.
- ↑ Juanpere S, Cañete N, Ortuño P, Martínez S, Sanchez G, Bernado L (February 2013). "A diagnostic approach to the mediastinal masses". Insights Imaging. 4 (1): 29–52. doi:10.1007/s13244-012-0201-0. PMID 23225215.
- ↑ Uberoi R (2006). "Quality assurance guidelines for superior vena cava stenting in malignant disease". Cardiovasc Intervent Radiol. 29 (3): 319–22. doi:10.1007/s00270-005-0284-9. PMID 16502166.
- ↑ Cohen R, Mena D, Carbajal-Mendoza R, Matos N, Karki N (2008). "Superior vena cava syndrome: A medical emergency?". Int. J. Angiol. 17 (1): 43–6. PMID 22477372.
- ↑ Juanpere S, Cañete N, Ortuño P, Martínez S, Sanchez G, Bernado L (February 2013). "A diagnostic approach to the mediastinal masses". Insights Imaging. 4 (1): 29–52. doi:10.1007/s13244-012-0201-0. PMID 23225215.
- ↑ Sears EH, Aliotta JM, Klinger JR (2012). "Partial anomalous pulmonary venous return presenting with adult-onset pulmonary hypertension". Pulm Circ. 2 (2): 250–5. doi:10.4103/2045-8932.97637. PMC 3401879. PMID 22837866.
- ↑ Broy C, Bennett S (June 2008). "Partial anomalous pulmonary venous return". Mil Med. 173 (6): 523–4. PMID 18595412.
- ↑ Gockel I, Müller M, Schumacher J (2012). "Achalasia--a disease of unknown cause that is often diagnosed too late". Dtsch Arztebl Int. 109 (12): 209–14. doi:10.3238/arztebl.2012.0209. PMC 3329145. PMID 22532812.
- ↑ Ghoshal UC, Daschakraborty SB, Singh R (2012). "Pathogenesis of achalasia cardia". World J. Gastroenterol. 18 (24): 3050–7. doi:10.3748/wjg.v18.i24.3050. PMC 3386318. PMID 22791940.
- ↑ Ates F, Vaezi MF (2015). "The Pathogenesis and Management of Achalasia: Current Status and Future Directions". Gut Liver. 9 (4): 449–63. doi:10.5009/gnl14446. PMC 4477988. PMID 26087861.
- ↑ Boeckxstaens GE, Zaninotto G, Richter JE (2013). "Achalasia". Lancet. doi:10.1016/S0140-6736(13)60651-0. PMID 23871090.
- ↑ Corley DA, Kerlikowske K, Verma R, Buffler P. Protective association of aspirin/NSAIDs and esophageal cancer: a systematic review and meta-analysis. Gastroenterology 2003;124:47-56. PMID 12512029. See also NCI - "Esophageal Cancer (PDQ®): Prevention".
- ↑ Wong A, Fitzgerald RC. Epidemiologic risk factors for Barrett's esophagus and associated adenocarcinoma. Clin Gastroenterol Hepatol. 2005 Jan;3(1):1-10. PMID 15645398
- ↑ Ye W, Held M, Lagergren J, Engstrand L, Blot WJ, McLaughlin JK, Nyren O. Helicobacter pylori infection and gastric atrophy: risk of adenocarcinoma and squamous-cell carcinoma of the esophagus and adenocarcinoma of the gastric cardia. J Natl Cancer Inst. 2004 Mar 3;96(5):388-96. PMID 14996860
- ↑ Nakajima S, Hattori T. Oesophageal adenocarcinoma or gastric cancer with or without eradication of Helicobacter pylori infection in chronic atrophic gastritis patients: a hypothetical opinion from a systematic review. Aliment Pharmacol Ther. 2004 Jul;20 Suppl 1:54-61. PMID 15298606
- ↑ NCI Prevention: Dietary Factors, based on Chainani-Wu N. Diet and oral, pharyngeal, and esophageal cancer. Nutr Cancer 2002;44:104-26. PMID 12734057.
- ↑ McGovern M, Egerton MJ (1991). "Spontaneous perforation of the cervical oesophagus". Med. J. Aust. 154 (4): 277–8. PMID 1994204.
- ↑ Wilson RF, Sarver EJ, Arbulu A, Sukhnandan R (1971). "Spontaneous perforation of the esophagus". Ann. Thorac. Surg. 12 (3): 291–6. PMID 5112482.
- ↑ Bladergroen MR, Lowe JE, Postlethwait RW (1986). "Diagnosis and recommended management of esophageal perforation and rupture". Ann. Thorac. Surg. 42 (3): 235–9. PMID 3753071.
- ↑ Dodds WJ, Stewart ET, Vlymen WJ (1982). "Appropriate contrast media for evaluation of esophageal disruption". Radiology. 144 (2): 439–41. doi:10.1148/radiology.144.2.7089304. PMID 7089304.
- ↑ James AE, Montali RJ, Chaffee V, Strecker EP, Vessal K (1975). "Barium or gastrografin: which contrast media for diagnosis of esophageal tears?". Gastroenterology. 68 (5 Pt 1): 1103–13. PMID 1126592.
- ↑ Schwartz SS (1975). "Letter: Barium or gastrografin: which contrast media for diagnosis of esophageal tears?". Gastroenterology. 69 (6): 1377. PMID 1193339.
- ↑ Vessal K, Montali RJ, Larson SM, Chaffee V, James AE (1975). "Evaluation of barium and gastrografin as contrast media for the diagnosis of esophageal ruptures or perforations". Am J Roentgenol Radium Ther Nucl Med. 123 (2): 307–19. PMID 1115308.
- ↑ Khajanchee YS, Cassera MA, Swanström LL, Dunst CM (January 2013). "Diagnosis of Type-I hiatal hernia: a comparison of high-resolution manometry and endoscopy". Dis. Esophagus. 26 (1): 1–6. doi:10.1111/j.1442-2050.2011.01314.x. PMID 22320417.
- ↑ Chang P, Friedenberg F (2014). "Obesity and GERD". Gastroenterol Clin North Am. 43 (1): 161–73. doi:10.1016/j.gtc.2013.11.009. PMC 3920303. PMID 24503366.
- ↑ Jash, Debraj; Maji, Arnab; Patra, Anupam; Sarkar, Supriya (2013). "Approach to unequal hilum on chest X-ray". The Journal of Association of Chest Physicians. 1 (2): 32. doi:10.4103/2320-8775.123204. ISSN 2320-8775.
- ↑ Mohseni S, Shojaiefard A, Khorgami Z, Alinejad S, Ghorbani A, Ghafouri A (2014). "Peripheral lymphadenopathy: approach and diagnostic tools". Iran J Med Sci. 39 (2 Suppl): 158–70. PMC 3993046. PMID 24753638.
- ↑ Mohseni S, Shojaiefard A, Khorgami Z, Alinejad S, Ghorbani A, Ghafouri A (2014). "Peripheral lymphadenopathy: approach and diagnostic tools". Iran J Med Sci. 39 (2 Suppl): 158–70. PMC 3993046. PMID 24753638.
- ↑ Lymph node enlargment. Radiopedia. http://radiopaedia.org/articles/lymph-node-enlargement Accessed on May 9, 2016
- ↑ Utsumi T, Shiono H, Fukai I, Akashi A (2007). "Artificial pneumomediastinum facilitates thoracoscopic surgery in anterior mediastinum". Interactive cardiovascular and thoracic surgery. 6 (3): 411–2. doi:10.1510/icvts.2006.147355. PMID 17669882.
- ↑ name="pmid18721592">Caceres M, Ali SZ, Braud R, Weiman D, Garrett HE (September 2008). "Spontaneous pneumomediastinum: a comparative study and review of the literature". Ann. Thorac. Surg. 86 (3): 962–6. doi:10.1016/j.athoracsur.2008.04.067. PMID 18721592.
- ↑ Kim, Hye Rin; Yoo, Seung Min; Lee, Hwa Yeon; Han, Jin Hee; Frazier, Aletta A; White, Charles S (2016). "Presence of subpleural pulmonary interstitial emphysema as an indication of single or multiple alveolar ruptures on CT in patients with spontaneous pneumomediastinum". Acta Radiologica. 57 (12): 1483–1489. doi:10.1177/0284185116629830. ISSN 0284-1851.
- ↑ . doi:10.3978/j.issn.2072-1439.2015.01.11. Missing or empty
|title=(help) - ↑ Chiu CY, Wong KS, Yao TC, Huang JL (March 2005). "Asthmatic versus non-asthmatic spontaneous pneumomediastinum in children". Asian Pac. J. Allergy Immunol. 23 (1): 19–22. PMID 15997870.
- ↑ Iyer VN, Joshi AY, Ryu JH (May 2009). "Spontaneous pneumomediastinum: analysis of 62 consecutive adult patients". Mayo Clin. Proc. 84 (5): 417–21. doi:10.1016/S0025-6196(11)60560-0. PMC 2676124. PMID 19411438.
- ↑ Dionísio, Patrícia; Martins, Luís; Moreira, Susana; Manique, Alda; Macedo, Rita; Caeiro, Fátima; Boal, Luísa; Bárbara, Cristina (2017). "Spontaneous pneumomediastinum: experience in 18 patients during the last 12 years". Jornal Brasileiro de Pneumologia. 43 (2): 101–105. doi:10.1590/s1806-37562016000000052. ISSN 1806-3756.
- ↑ Teirstein AS, Judson MA, Baughman RP, et al: The spectrum of biopsy sites for the diagnosis of sarcoidosis. Sarcoidosis Vasc Diffuse Lung Dis 22(2):139 146, 2005.
- ↑ Judson MA, Boan AD, Lackland DT: The clinical course of sarcoidosis: presentation, diagnosis, and treatment in a large white and black cohort in the United States. Sarcoidosis, vasculitis, and diffuse lung diseases : official journal of WASOG 2012, 29(2):119-127.
- ↑ Roberts SD, Mirowski GW, Wilkes D, Kwo PY, Knox KS: Sarcoidosis. Part II: extrapulmonary and systemic manifestations. Journal of the American Academy of Dermatology 2004, 51(4):628-630.
- ↑ Lieberman J, Nosal A, Schlessner A, Sastre-Foken A: Serum angiotensin-converting enzyme for diagnosis and therapeutic evaluation of sarcoidosis. Am Rev Respir Dis 120(2):329–335, 1979.
- ↑ Martínez Vallina P, Espinosa Jiménez D, Hernández Pérez L, Triviño Ramírez A (2011). "[Mediastinitis]". Arch Bronconeumol. 47 Suppl 8: 32–6. doi:10.1016/S0300-2896(11)70065-5. PMID 23351519.
- ↑ Lewandowski B, Pakla P, Wołek W, Jednakiewicz M, Nicpoń J (2014). "A fatal case of descending necrotizing mediastinitis as a complication of odontogenic infection. A case report". Kardiochir Torakochirurgia Pol. 11 (3): 324–8. doi:10.5114/kitp.2014.45685. PMC 4283893. PMID 26336443.
- ↑ Symptoms of mediastinitis. Right Diagnosis (2015). http://www.rightdiagnosis.com/m/mediastinitis/symptoms.htm Accessed on September 28, 2015
- ↑ Mediastinitis: parotid abscess complication. Brazilian Journal of Otorhinolaryngology (2013). http://www.scielo.br/scielo.php?pid=S1808-86942014000300268&script=sci_arttext Accessed on September 28, 2015
- ↑ "Symptoms | Anthrax | CDC".
- ↑ "Anthrax in Humans and Animals" (PDF).
- ↑ "Tuberculosis Fact Sheet".
- ↑ Griffith D, Kerr C (1996). "Tuberculosis: disease of the past, disease of the present". J Perianesth Nurs. 11 (4): 240–5. PMID 8964016.
- ↑ Juanpere S, Cañete N, Ortuño P, Martínez S, Sanchez G, Bernado L (February 2013). "A diagnostic approach to the mediastinal masses". Insights Imaging. 4 (1): 29–52. doi:10.1007/s13244-012-0201-0. PMID 23225215.
- ↑ Liu R, Adler DG (July 2014). "Duplication cysts: Diagnosis, management, and the role of endoscopic ultrasound". Endosc Ultrasound. 3 (3): 152–60. doi:10.4103/2303-9027.138783. PMC 4145475. PMID 25184121.
- ↑ Hellmich B, Ehlers S, Csernok E, Gross WL (2003). "Update on the pathogenesis of Churg-Strauss syndrome". Clin. Exp. Rheumatol. 21 (6 Suppl 32): S69–77. PMID 14740430.
- ↑ Safran T, Masckauchan M, Maj J, Green L (December 2017). "Wells syndrome secondary to influenza vaccination: A case report and review of the literature". Hum Vaccin Immunother: 1–3. doi:10.1080/21645515.2017.1417714. PMID 29240526.
- ↑ Szczeklik W, Sokołowska B, Mastalerz L, Grzanka P, Górka J, Pacułt K, Miszalski-Jamka T, Soja J, Musiał J (October 2010). "Pulmonary findings in Churg-Strauss syndrome in chest X-rays and high resolution computed tomography at the time of initial diagnosis". Clin. Rheumatol. 29 (10): 1127–34. doi:10.1007/s10067-010-1530-3. PMID 20623310.
- ↑ Silva CI, Müller NL, Fujimoto K, Johkoh T, Ajzen SA, Churg A (May 2005). "Churg-Strauss syndrome: high resolution CT and pathologic findings". J Thorac Imaging. 20 (2): 74–80. PMID 15818205.
- ↑ Feng RE, Xu WB, Shi JH, Mahmoudi A, Mu WB, Zheng WJ, Zhu YJ, Liu HR (March 2011). "Pathological and high resolution CT findings in Churg-Strauss syndrome". Chin. Med. Sci. J. 26 (1): 1–8. PMID 21496416.
- ↑ Invalid
<ref>tag; no text was provided for refs namedpmid2322521512 - ↑ Setty, HAN; Hegde, KKS; Narvekar, VN (2005). "Neurenteric cyst of the posterior mediastinum". Australasian Radiology. 49 (2): 151–153. doi:10.1111/j.1440-1673.2005.01360.x. ISSN 0004-8461.
- ↑ Elta, Grace H; Enestvedt, Brintha K; Sauer, Bryan G; Marie Lennon, Anne (2018). "ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts". The American Journal of Gastroenterology. 113 (4): 464–479. doi:10.1038/ajg.2018.14. ISSN 0002-9270.
- ↑ Juanpere S, Cañete N, Ortuño P, Martínez S, Sanchez G, Bernado L (February 2013). "A diagnostic approach to the mediastinal masses". Insights Imaging. 4 (1): 29–52. doi:10.1007/s13244-012-0201-0. PMID 23225215.
- ↑ "What is Spina Bifida | CDC".
- ↑ Edwards RJ, Witchell C, Pople IK (December 2003). "Chronic headaches in adults with spina bifida and associated hydrocephalus". Eur J Pediatr Surg. 13 Suppl 1: S13–7. doi:10.1055/s-2003-44751. PMID 14758561.
- ↑ Duncan BK (November 1985). "Isolation of insertion, deletion, and nonsense mutations of the uracil-DNA glycosylase (ung) gene of Escherichia coli K-12". J. Bacteriol. 164 (2): 689–95. PMID 2997126.
- ↑ Flenley DC (December 1985). "Disordered breathing during sleep: discussion paper". J R Soc Med. 78 (12): 1031–3. doi:10.1177/014107688507801211. PMID 4067977.
- ↑ Mitchell LE, Adzick NS, Melchionne J, Pasquariello PS, Sutton LN, Whitehead AS (2004). "Spina bifida". Lancet. 364 (9448): 1885–95. doi:10.1016/S0140-6736(04)17445-X. PMID 15555669.
- ↑ Juanpere S, Cañete N, Ortuño P, Martínez S, Sanchez G, Bernado L (February 2013). "A diagnostic approach to the mediastinal masses". Insights Imaging. 4 (1): 29–52. doi:10.1007/s13244-012-0201-0. PMID 23225215.
- ↑ "Schwannoma | Genetic and Rare Diseases Information Center (GARD) – an NCATS Program".