Waldenström's macroglobulinemia pathophysiology
|
Waldenström's macroglobulinemia Microchapters |
|
Differentiating Waldenström's macroglobulinemia from other Diseases |
|---|
|
Diagnosis |
|
Treatment |
|
Case Studies |
|
Waldenström's macroglobulinemia pathophysiology On the Web |
|
American Roentgen Ray Society Images of Waldenström's macroglobulinemia pathophysiology |
|
Directions to Hospitals Treating Waldenström's macroglobulinemia |
|
Risk calculators and risk factors for Waldenström's macroglobulinemia pathophysiology |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Sara Mohsin, M.D.[2], Roukoz A. Karam, M.D.[3], Mirdula Sharma, MBBS [4]; Grammar Reviewer: Natalie Harpenau, B.S.[5]
Overview
Waldenstrom's macroglobulinemia is an uncontrolled clonal proliferation of terminally differentiated B lymphocytes, which are normally involved in humoral immunity. Two main factors mediating this disease include IgM paraprotein secretion and tissue infiltration with neoplastic lymphoplasmacytic cells. Genes involved in the pathogenesis of WM include MYD88-L265P, and CXCR4 alongwith various other cytogenetic and epigenetic abnormalities. In patients of Waldenstrom's macroglobulinemia, there is an increased incidence of diffuse large B-cell lymphoma, myelodysplastic syndrome (acute myeloid leukemia), brain tumor, and renal MALT lymphoma. Two histologic subtypes include lymphoplasmacytoid and lymphoplasmacytic which invade the lymphoid organs such as spleen, lymph nodesand bone marrow. Bone marrow is infiltrated by small lymphocytes, well-formed plasma cells, and plasmacytoid lymphocytes in diffuse, interstitial, nodular, paratrabecular, nodular-interstitial and mixed paratrabacular-nodular patterns. Lymph nodes infiltration shows Dutcher and Russell bodies, mast cells, and hemosiderin-laden macrophages. Peripheral smear shows circulating malignant cells with a plasmacytoid appearance, having basophilic cytoplasm, perinuclearhalo, and nucleus with "clock-face" chromatin without nucleoli. Immunohistochemistry shows pan B-cell surface antigens such as Ig+CD19+, CD20+, CD22+, CD79A+ and variable expression of some other antigens.
Pathophysiology
- Waldenstrom's macroglobulinemia arises from terminally differentiated B lymphocytes. which are normally involved in humoral immunity
B lymphocytes
Development
- B cells develop from hematopoietic stem cells (HSCs) in bone marrow[1]
- Then undergo 2 types of selection in bone marrow:
- Immature B cells then migrate from bone marrow to secondary lymphoid organs (SLOs) such as spleen and lymph nodes
- B cell activation begins when the B cell binds to an antigen via its BCR in SLOs
Function
- Lymphocyte subtype of white blood cells
- Function as a part of humoral immunity which is a component of adaptive immune system
- Secrete antibodies
- Secrete cytokines
- Classified as professional antigen-presenting cells (APCs)
Factors mediating Waldenstrom's macroglobulinemia
- It is understood that WM is mediated by 2 major factors:
- The secretion of IgM paraprotein:
- The infiltration of tissues with neoplastic lymphoplasmacytic cells:
- Mainly the bone marrow, spleen,and lymph nodes
- Sometimes the liver, gastrointestinal tract, lungs, kidneys, skin, eyes, and central nervous system
Genetics
- The exact pathogenesis of Waldenstrom's macroglobulinemia is not completely understood; however, its familial pattern of involvement supports the role played by genetic factors in the pathogenesis of this disease[5][6]
- Development of WM is the result of multiple genetic mutations[7]
- Somatic hypermutations of immunoglobulin heavy chain gene, without any intraclonal variation, suggests that the cell of origin is a post-germinal center B cell that has undergone affinity maturation as well as chromosomal abnormalities play a part in the pathogenesis of this disease:
- A mutation of the MYD88 gene (L265P) has been found in more than 90% of patients with Waldenstrom's macroglobulinemia, while it has rarely presented in patients with other types of mature B-cell tumors[8][9][10][11][12][13][14][15]
- MYD88: The activating point mutation of MYD88 augments signaling by Toll-like receptor and Bruton tyrosine kinase (BTK), which leads to activation of transcription factors of the NF-kB family which are involved in growth and survival of both normal and neoplastic B cells by preventing apoptosis. Point mutation of MYD88 leads to leucine to proline substitution in codon 265 (L265P) of MYD88 and produces constantly overactive protein causing proliferation of malignant cells that should normally undergo apoptosis.The opening
<ref>tag is malformed or has a bad name - Monoclonal gammopathy of undetermined significance patients found to have MYD88 L265P mutation have significantly higher risk of progression to Waldenström macroglobulinemia or to other lymphoproliferative disordersThe opening
<ref>tag is malformed or has a bad name
- MYD88: The activating point mutation of MYD88 augments signaling by Toll-like receptor and Bruton tyrosine kinase (BTK), which leads to activation of transcription factors of the NF-kB family which are involved in growth and survival of both normal and neoplastic B cells by preventing apoptosis. Point mutation of MYD88 leads to leucine to proline substitution in codon 265 (L265P) of MYD88 and produces constantly overactive protein causing proliferation of malignant cells that should normally undergo apoptosis.The opening
- Less commonly (30-35%), nonsense or frameshift mutations in the C-X-C chemokine receptor type 4 (CXCR4) 5338X gene have also been reported in patients with Waldenstrom's macroglobulinemia. Mutations in CXCR4 are similar to those seen in patients with the warts, hypogammaglobulinemia, infection, and myelokathexis (WHIM) syndrome:[16]
- Patients with Waldenstrom's macroglobulinemia with co-existing mutation of MYD88 & CXCR4 are more likely to have hyper-viscosity syndrome and bone marrow involvement[7]
- Somatic hypermutation in IGHV/IG gene rearrangement[17]
- ARIDA mutations (17%)
- A mutation of the MYD88 gene (L265P) has been found in more than 90% of patients with Waldenstrom's macroglobulinemia, while it has rarely presented in patients with other types of mature B-cell tumors[8][9][10][11][12][13][14][15]
Cytogenetics
- Many cytogenetic abnormalities were reported in Waldenstrom's macroglobulinemia's patients including:
- Deletion of the long arm of chromosome 6q21-22.1 (most common, 50%)[18]
- t(9;14) (p13;q32) (50% of patients)[17]
- Trisomy 4 (20%)[17]
- Deletion of long arm of chromosome 10, 12 or 20
- Trisomy 3
- Trisomy 5
- Monosomy 8[19]
- Deletions of regions of 13q14 that include MIRN15A and MIRN16-1[20]
- t(11;18) (q21;q21) involving API-malt1[20]
- t(8;14)
- t(14;18)
Epigenetics:
- Three most common epigenetic causes are:
- DNA methylation, histone acetylation, and non-coding RNAs such as miRNAs[21]
- Upregulation of miRNAs 155, 184, 206, 363, 494, and 542-3p occurs in Waldenström macroglobulinemia; among which miRNA-155 has a crucial role in tumor cell growth and proliferation in Waldenström macroglobulinemia
- Gene transcription through histone acetylation occurs following increased expression of miRNA-206 and reduced expression of miRNA-9
Associated Conditions
Several studies showed an increased incidence of following second cancers in patients with Waldenstrom's macroglobulinemia:[22]
- Diffuse large B-cell lymphoma
- Myelodysplastic syndrome/Acute myeloid leukemia
- Brain tumor
- Renal MALT lymphoma [23]
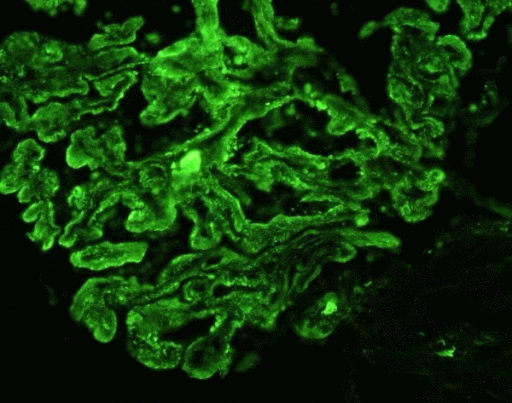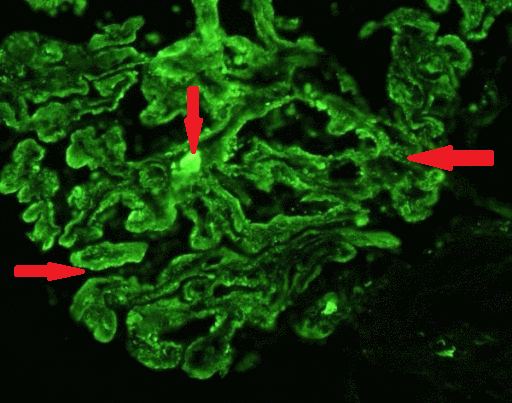
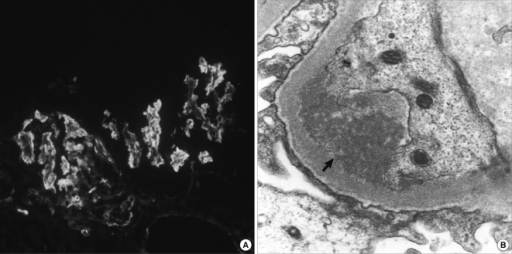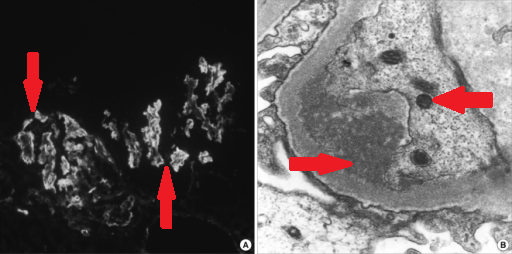
Microscopic Pathology
- Following lymphoid organs are involved in WM:
- Bone marrow
- Lymph nodes (nodal involvement is characterized by paracortical and hilar infiltration with frequent sparing of the subscapular and marginal sinuses)
- Spleen
- After a detailed clinicopathological assessment and review of the published literature, the following diagnostic criteria was proposed for WM:[24]
- IgM monoclonal gammopathy of any concentration
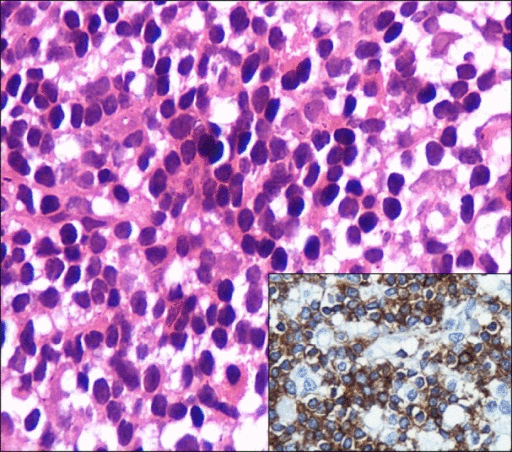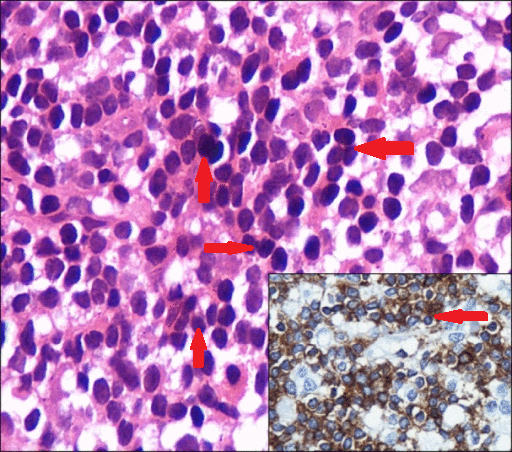
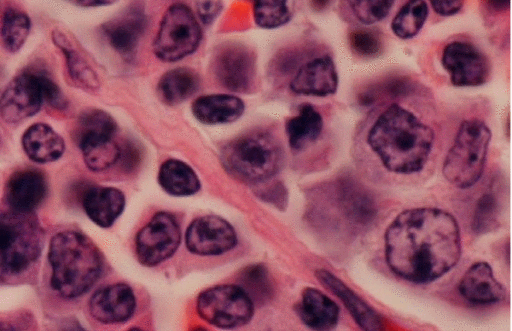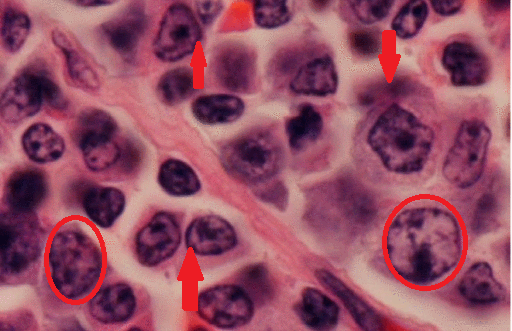
- Bone marrow infiltration by:[25][26][27]
- Small lymphocytes with clumped chromatin, inconspicuous nucleoli, and sparse cytoplasm
- Well-formed plasma cells
- Plasmacytoid lymphocytes (have cytologic features intermediate between above 2 extremes), in following patterns:[28][29]
- Diffuse
- Interstitial
- Nodular
- Paratrabecular
- Nodular-interstitial
- Mixed paratrabacular-nodular
- WM has two histologic subtypes:[29]
- Lymphoplasmacytoid (73%)
- Lymphoplasmacytic (27%)
- The cytologic composition and the degree of plasmacytic differentiation varies from case to case
- The bone marrow contains variable numbers of pleomorphic lymphoid cells
- Russell bodies (cytoplasmic) or Dutcher bodies (pseudonuclear) which are positive for periodic acid Schiff, can be seen due to accumulation of cytoplasmic IgM in some bone marrow cells
- Mast cell hyperplasia is common and may stimulate tumor cell proliferation and monoclonal IgM secretion
- Gene expression profiling has indicated that lymphoid cells of WM more closely resemble those of chronic lymphocytic leukemia than those of myeloma[30]
- Lymph nodes involvement has following characteristics:
- Dutcher and Russell bodies, mast cells, and hemosiderin-laden macrophages comprise the typical characteristic lymph node involvement
- Numerous non-caseating granulomas are rarely observed
- Lymph node architecture is frequently preserved
- Diffuse and interstitial infiltration pattern is observed containing small lymphocytes, plasma cells, and plasmacytoid cells
- Sometimes, large, immunoblast-like cells may be present
- Often, sinuses remain open, and may contain histiocytes reacting to secreted periodic acid Schiff (PAS) positive immunoglobulin
- Proliferation centers, which are the hallmark of chronic lymphocytic leukemia/small lymphocytic leukemia, are absent, as is paler-appearing marginal zone differentiation, which is seen in marginal zone lymphoma
- Spleen involvement comprises of:
- Both red and white pulp
- Infiltration in a diffuse pattern
- No distinct marginal zone or nodularity in the red pulp
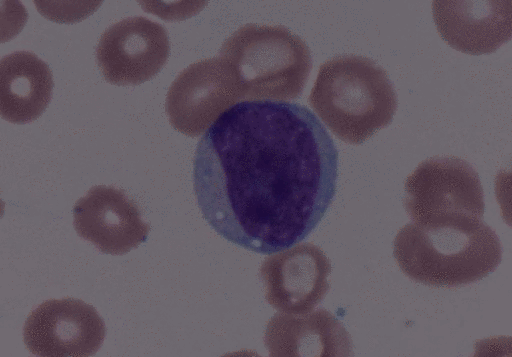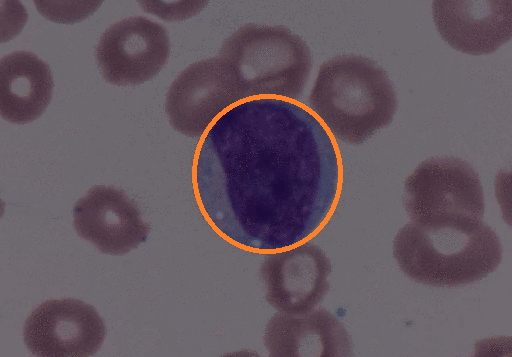
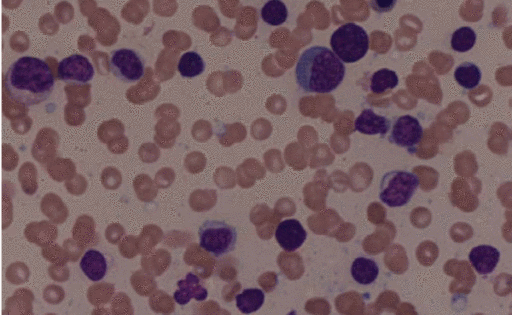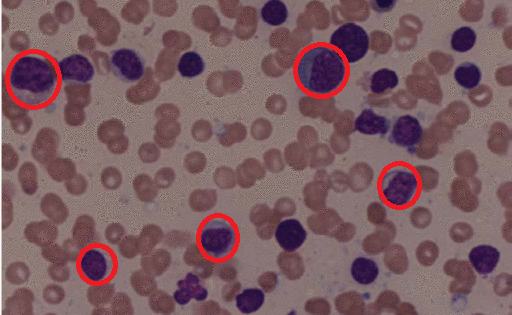
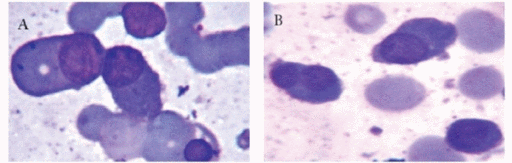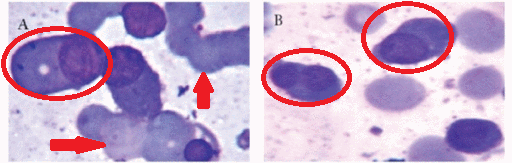
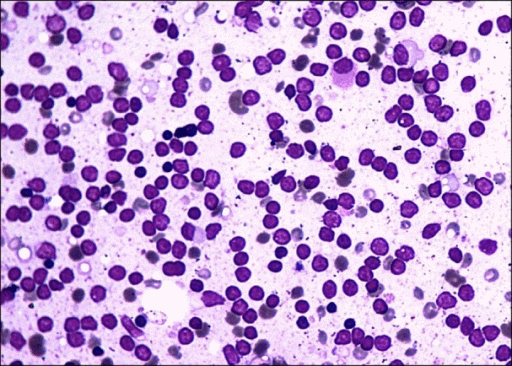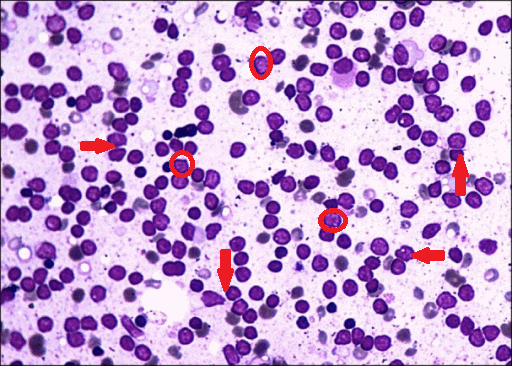
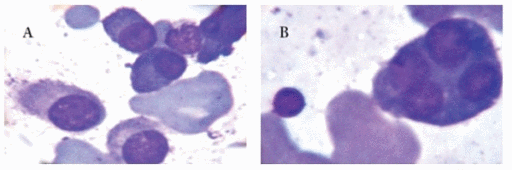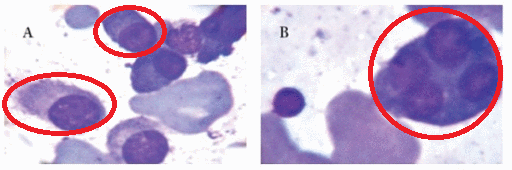
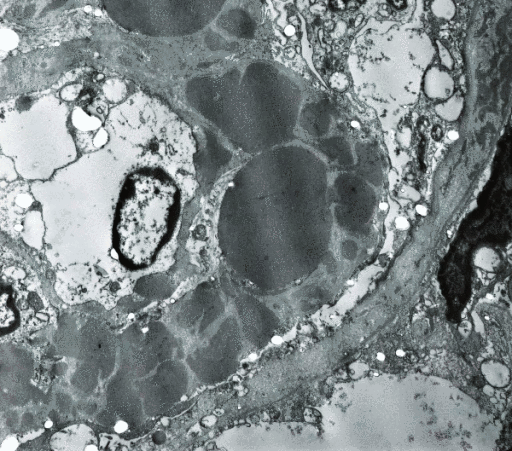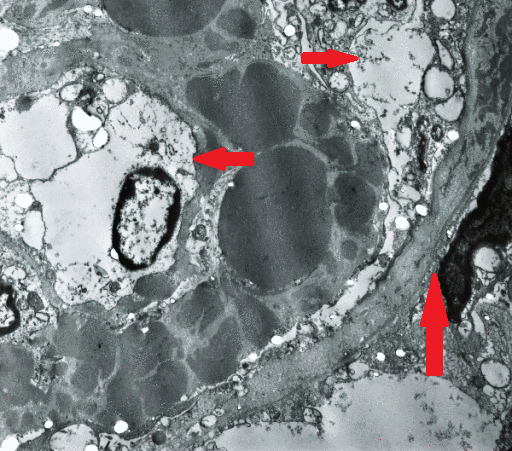
- Peripheral blood contains:
- Circulating malignant cells with a plasmacytoid appearance (i.e, resembling a plasma cell)
- These cells are typically oval-shaped with abundant basophilic cytoplasm
- Round and eccentrically located nucleus with a perinuclear halo, or cytoplasmic clearing
- Nucleus has "clock-face" or "spoke wheel" chromatin without nucleoli
 |
 |
 |
 |
 |
 |
 |
 |
 |
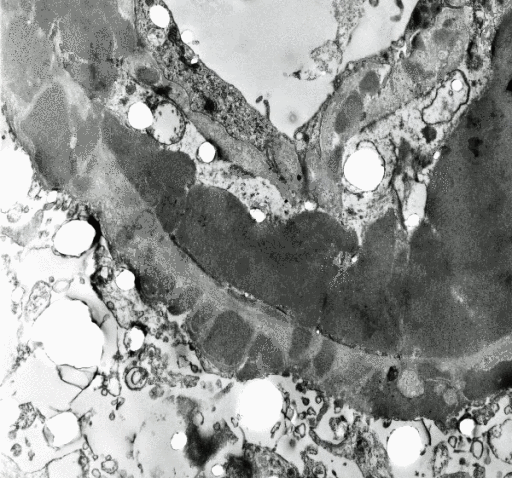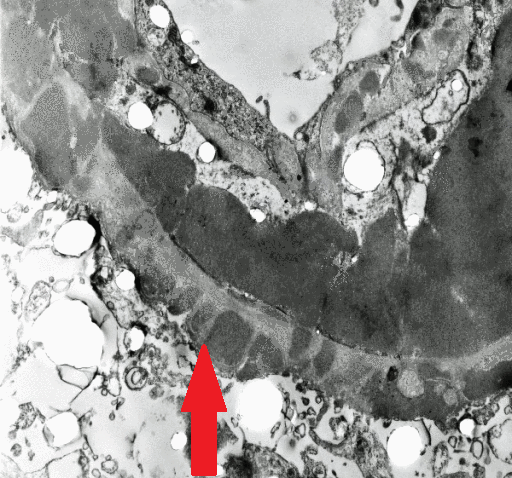 |
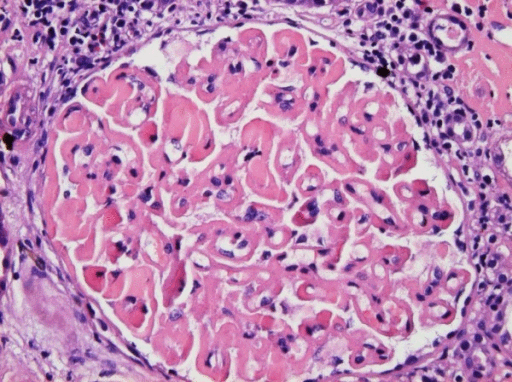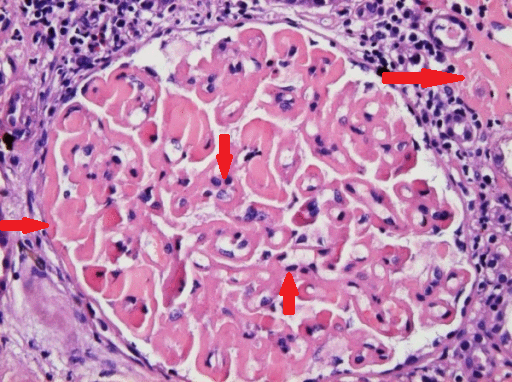 |
 |
 |
Immunohistochemistry
Malignant cells in Waldenstrom's macroglobulinemia have following immunophenotypic characteristics:[27][7]
- Express pan B-cell surface antigens with following immunophenotype:[31][32][24]
- Variable expression of:
- Following aren't expressed:
- IgM positive (mostly)
- IgG positive (few)
- IgA (rare)
- IgD negative (lack)
References
- ↑ Kondo, Motonari (2010-11-01). "Lymphoid and myeloid lineage commitment in multipotent hematopoietic progenitors". Immunological Reviews. 238 (1): 37–46. doi:10.1111/j.1600-065X.2010.00963.x. ISSN 1600-065X. PMC 2975965. PMID 20969583.
- ↑ Martensson, Inga-Lill; Almqvist, Nina; Grimsholm, Ola; Bernardi, Angelina (2010). "The pre-B cell receptor checkpoint". FEBS Letters. 584 (12): 2572–9. doi:10.1016/j.febslet.2010.04.057. PMID 20420836.
- ↑ LeBien, Tucker W.; Tedder, Thomas F. (2008-09-01). "B lymphocytes: how they develop and function". Blood. 112 (5): 1570–1580. doi:10.1182/blood-2008-02-078071. ISSN 0006-4971. PMC 2518873. PMID 18725575.
- ↑ Murphy, Kenneth (2012). Janeway's Immunobiology (8th ed.). New York: Garland Science. ISBN 9780815342434.
- ↑ Royer RH, Koshiol J, Giambarresi TR, Vasquez LG, Pfeiffer RM, McMaster ML (2010). "Differential characteristics of Waldenström macroglobulinemia according to patterns of familial aggregation". Blood. 115 (22): 4464–71. doi:10.1182/blood-2009-10-247973. PMC 2881498. PMID 20308603.
- ↑ Treon SP, Hunter ZR, Aggarwal A, Ewen EP, Masota S, Lee C; et al. (2006). "Characterization of familial Waldenstrom's macroglobulinemia". Ann Oncol. 17 (3): 488–94. doi:10.1093/annonc/mdj111. PMID 16357024.
- ↑ 7.0 7.1 7.2 Ngo VN, Young RM, Schmitz R, Jhavar S, Xiao W, Lim KH, Kohlhammer H, Xu W, Yang Y, Zhao H, Shaffer AL, Romesser P, Wright G, Powell J, Rosenwald A, Muller-Hermelink HK, Ott G, Gascoyne RD, Connors JM, Rimsza LM, Campo E, Jaffe ES, Delabie J, Smeland EB, Fisher RI, Braziel RM, Tubbs RR, Cook JR, Weisenburger DD, Chan WC, Staudt LM (2011). "Oncogenically active MYD88 mutations in human lymphoma". Nature. 470 (7332): 115–9. doi:10.1038/nature09671. PMID 21179087.
- ↑ Treon, Steven P.; Xu, Lian; Yang, Guang; Zhou, Yangsheng; Liu, Xia; Cao, Yang; Sheehy, Patricia; Manning, Robert J.; Patterson, Christopher J.; Tripsas, Christina; Arcaini, Luca; Pinkus, Geraldine S.; Rodig, Scott J.; Sohani, Aliyah R.; Harris, Nancy Lee; Laramie, Jason M.; Skifter, Donald A.; Lincoln, Stephen E.; Hunter, Zachary R. (2012). "MYD88 L265P Somatic Mutation in Waldenström's Macroglobulinemia". New England Journal of Medicine. 367 (9): 826–833. doi:10.1056/NEJMoa1200710. ISSN 0028-4793.
- ↑ Varettoni M, Arcaini L, Zibellini S, Boveri E, Rattotti S, Riboni R; et al. (2013). "Prevalence and clinical significance of the MYD88 (L265P) somatic mutation in Waldenstrom's macroglobulinemia and related lymphoid neoplasms". Blood. 121 (13): 2522–8. doi:10.1182/blood-2012-09-457101. PMID 23355535.
- ↑ Shi M, Spurgeon S, Press R, Olson S, Fan G (2015). "MYD88 mutation analysis of a rare composite chronic lymphocyte leukemia and lymphoplasmacytic lymphoma by flow cytometry cell sorting". Ann Hematol. 94 (11): 1941–4. doi:10.1007/s00277-015-2460-6. PMID 26231802.
- ↑ Yang G, Zhou Y, Liu X, Xu L, Cao Y, Manning RJ; et al. (2013). "A mutation in MYD88 (L265P) supports the survival of lymphoplasmacytic cells by activation of Bruton tyrosine kinase in Waldenström macroglobulinemia". Blood. 122 (7): 1222–32. doi:10.1182/blood-2012-12-475111. PMID 23836557.
- ↑ Ngo VN, Young RM, Schmitz R, Jhavar S, Xiao W, Lim KH; et al. (2011). "Oncogenically active MYD88 mutations in human lymphoma". Nature. 470 (7332): 115–9. doi:10.1038/nature09671. PMC 5024568. PMID 21179087.
- ↑ Mori N, Ohwashi M, Yoshinaga K, Mitsuhashi K, Tanaka N, Teramura M; et al. (2013). "L265P mutation of the MYD88 gene is frequent in Waldenström's macroglobulinemia and its absence in myeloma". PLoS One. 8 (11): e80088. doi:10.1371/journal.pone.0080088. PMC 3818242. PMID 24224040.
- ↑ Abeykoon JP, Paludo J, King RL, Ansell SM, Gertz MA, LaPlant BR; et al. (2018). "MYD88 mutation status does not impact overall survival in Waldenström macroglobulinemia". Am J Hematol. 93 (2): 187–194. doi:10.1002/ajh.24955. PMID 29080258.
- ↑ Steven P. Treon, Lian Xu, Guang Yang, Yangsheng Zhou, Xia Liu, Yang Cao, Patricia Sheehy, Robert J. Manning, Christopher J. Patterson, Christina Tripsas, Luca Arcaini, Geraldine S. Pinkus, Scott J. Rodig, Aliyah R. Sohani, Nancy Lee Harris, Jason M. Laramie, Donald A. Skifter, Stephen E. Lincoln & Zachary R. Hunter (2012). "MYD88 L265P somatic mutation in Waldenstrom's macroglobulinemia". The New England journal of medicine. 367 (9): 826–833. doi:10.1056/NEJMoa1200710. PMID 22931316. Unknown parameter
|month=ignored (help) - ↑ Zachary R. Hunter, Lian Xu, Guang Yang, Yangsheng Zhou, Xia Liu, Yang Cao, Robert J. Manning, Christina Tripsas, Christopher J. Patterson, Patricia Sheehy & Steven P. Treon (2014). "The genomic landscape of Waldenstrom macroglobulinemia is characterized by highly recurring MYD88 and WHIM-like CXCR4 mutations, and small somatic deletions associated with B-cell lymphomagenesis". Blood. 123 (11): 1637–1646. doi:10.1182/blood-2013-09-525808. PMID 24366360. Unknown parameter
|month=ignored (help) - ↑ 17.0 17.1 17.2 Yun S, Johnson AC, Okolo ON, Arnold SJ, McBride A, Zhang L; et al. (2017). "Waldenström Macroglobulinemia: Review of Pathogenesis and Management". Clin Lymphoma Myeloma Leuk. 17 (5): 252–262. doi:10.1016/j.clml.2017.02.028. PMC 5413391. PMID 28366781.
- ↑ Treon, S. P.; Hunter, Z. R.; Aggarwal, A.; Ewen, E. P.; Masota, S.; Lee, C.; Santos, D. Ditzel; Hatjiharissi, E.; Xu, L.; Leleu, X.; Tournilhac, O.; Patterson, C. J.; Manning, R.; Branagan, A. R.; Morton, C. C. (2006). "Characterization of familial Waldenström's macroglobulinemia". Annals of Oncology. 17 (3): 488–494. doi:10.1093/annonc/mdj111. ISSN 1569-8041.
- ↑ Roelandt F. J. Schop, W. Michael Kuehl, Scott A. Van Wier, Gregory J. Ahmann, Tammy Price-Troska, Richard J. Bailey, Syed M. Jalal, Ying Qi, Robert A. Kyle, Philip R. Greipp & Rafael Fonseca (2002). "Waldenstrom macroglobulinemia neoplastic cells lack immunoglobulin heavy chain locus translocations but have frequent 6q deletions". Blood. 100 (8): 2996–3001. doi:10.1182/blood.V100.8.2996. PMID 12351413. Unknown parameter
|month=ignored (help) - ↑ 20.0 20.1 Braggio E, Keats JJ, Leleu X, Van Wier S, Jimenez-Zepeda VH, Valdez R; et al. (2009). "Identification of copy number abnormalities and inactivating mutations in two negative regulators of nuclear factor-kappaB signaling pathways in Waldenstrom's macroglobulinemia". Cancer Res. 69 (8): 3579–88. doi:10.1158/0008-5472.CAN-08-3701. PMC 2782932. PMID 19351844.
- ↑ Waldenström macroglobulinemia. International Waldenström Macroglobulinemia foundation (2015)http://www.iwmf.com/sites/default/files/docs/WM_Review_Ghobrial_Jan2014.pdf Accessed on November 12, 2015
- ↑ Morra E, Varettoni M, Tedeschi A, Arcaini L, Ricci F, Pascutto C, Rattotti S, Vismara E, Paris L, Cazzola M (2013). "Associated cancers in Waldenström macroglobulinemia: clues for common genetic predisposition". Clin Lymphoma Myeloma Leuk. 13 (6): 700–3. doi:10.1016/j.clml.2013.05.008. PMID 24070824.
- ↑ Chi PJ, Pei SN, Huang TL, Huang SC, Ng HY, Lee CT (2014). "Renal MALT lymphoma associated with Waldenström macroglobulinemia". J. Formos. Med. Assoc. 113 (4): 255–7. doi:10.1016/j.jfma.2011.02.007. PMID 24685302.
- ↑ 24.0 24.1 Owen RG (2003). "Developing diagnostic criteria in Waldenstrom's macroglobulinemia". Semin Oncol. 30 (2): 196–200. doi:10.1053/sonc.2003.50069. PMID 12720135.
- ↑ Morice WG, Chen D, Kurtin PJ, Hanson CA, McPhail ED (2009). "Novel immunophenotypic features of marrow lymphoplasmacytic lymphoma and correlation with Waldenström's macroglobulinemia". Mod Pathol. 22 (6): 807–16. doi:10.1038/modpathol.2009.34. PMID 19287458.
- ↑ Owen RG, Treon SP, Al-Katib A, Fonseca R, Greipp PR, McMaster ML; et al. (2003). "Clinicopathological definition of Waldenstrom's macroglobulinemia: consensus panel recommendations from the Second International Workshop on Waldenstrom's Macroglobulinemia". Semin Oncol. 30 (2): 110–5. doi:10.1053/sonc.2003.50082. PMID 12720118.
- ↑ 27.0 27.1 Ansell, Stephen M.; Kyle, Robert A.; Reeder, Craig B.; Fonseca, Rafael; Mikhael, Joseph R.; Morice, William G.; Bergsagel, P. Leif; Buadi, Francis K.; Colgan, Joseph P.; Dingli, David; Dispenzieri, Angela; Greipp, Philip R.; Habermann, Thomas M.; Hayman, Suzanne R.; Inwards, David J.; Johnston, Patrick B.; Kumar, Shaji K.; Lacy, Martha Q.; Lust, John A.; Markovic, Svetomir N.; Micallef, Ivana N.M.; Nowakowski, Grzegorz S.; Porrata, Luis F.; Roy, Vivek; Russell, Stephen J.; Short, Kristen E. Detweiler; Stewart, A. Keith; Thompson, Carrie A.; Witzig, Thomas E.; Zeldenrust, Steven R.; Dalton, Robert J.; Rajkumar, S. Vincent; Gertz, Morie A. (2010). "Diagnosis and Management of Waldenström Macroglobulinemia: Mayo Stratification of Macroglobulinemia and Risk-Adapted Therapy (mSMART) Guidelines". Mayo Clinic Proceedings. 85 (9): 824–833. doi:10.4065/mcp.2010.0304. ISSN 0025-6196.
- ↑ Owen RG, Barrans SL, Richards SJ, O'Connor SJ, Child JA, Parapia LA; et al. (2001). "Waldenström macroglobulinemia. Development of diagnostic criteria and identification of prognostic factors". Am J Clin Pathol. 116 (3): 420–8. doi:10.1309/4LCN-JMPG-5U71-UWQB. PMID 11554171.
- ↑ 29.0 29.1 Andriko JA, Aguilera NS, Chu WS, Nandedkar MA, Cotelingam JD (1997). "Waldenström's macroglobulinemia: a clinicopathologic study of 22 cases". Cancer. 80 (10): 1926–35. PMID 9366295.
- ↑ Chng WJ, Schop RF, Price-Troska T, Ghobrial I, Kay N, Jelinek DF; et al. (2006). "Gene-expression profiling of Waldenstrom macroglobulinemia reveals a phenotype more similar to chronic lymphocytic leukemia than multiple myeloma". Blood. 108 (8): 2755–63. doi:10.1182/blood-2006-02-005488. PMC 1895596. PMID 16804116.
- ↑ Dimopoulos MA, Gertz MA, Kastritis E, Garcia-Sanz R, Kimby EK, Leblond V; et al. (2009). "Update on treatment recommendations from the Fourth International Workshop on Waldenstrom's Macroglobulinemia". J Clin Oncol. 27 (1): 120–6. doi:10.1200/JCO.2008.17.7865. PMID 19047284.
- ↑ Vijay A, Gertz MA (2007). "Waldenström macroglobulinemia". Blood. 109 (12): 5096–103. doi:10.1182/blood-2006-11-055012. PMID 17303694.