Supraventricular tachycardia
For patient information click here
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Joseph Nasr, M.D.[2]; Abdelrahman Ibrahim Abushouk, MD[3]
Synonyms and keywords: SVT
Overview
Supraventricular tachycardia (SVT) encompasses tachyarrhythmias that originate from or conduct through the atria or atrioventricular (AV) node, occurring at a heart rate greater than 100 beats per minute.[1] SVTs typically conduct through the His-Purkinje system and appear as narrow QRS tachyarrhythmias on electrocardiogram (ECG), although wide-complex presentations can occur with aberrant conduction or pre-excitation.[1] There are several classification systems for SVT, based on site of origin, QRS width, pulse regularity, and AV node dependence.[2][3] The major subtypes of paroxysmal SVT (PSVT) include AV nodal re-entry tachycardia (AVNRT), AV reciprocating tachycardia (AVRT), and focal atrial tachycardia (AT).[1] Other SVTs include sinus tachycardia, inappropriate sinus tachycardia, sinus node re-entry tachycardia, atrial fibrillation, atrial flutter, junctional tachycardia, multifocal atrial tachycardia, and Wolff-Parkinson-White (WPW) syndrome.[2][3]
The prevalence of PSVT in the United States is estimated at 168 to 332 per 100,000 individuals.[1] Approximately 50% of patients with PSVT are aged 45 to 64 years, and 67.5% are female.[1] PSVT is generally benign, but untreated PSVT may be associated with high symptom burden and, rarely, tachycardia-mediated cardiomyopathy.[1] SVTs can be separated into two groups based on whether they involve the AV node for impulse maintenance. AV node-dependent tachycardias can be terminated by slowing conduction through the AV node, whereas AV node-independent tachycardias will not usually be terminated by AV nodal blocking maneuvers, although transient AV block may unmask the underlying rhythm abnormality.[2][3]
First-line acute therapy for hemodynamically stable patients includes vagal maneuvers and intravenous adenosine.[2][3] Emergent synchronized cardioversion is recommended for hemodynamically unstable patients.[2][4] For long-term prevention of recurrent symptomatic PSVT, catheter ablation is recommended as first-line therapy, with single-procedure success rates of 94.3% to 98.5%.[1] Pharmacotherapy with beta-blockers, nondihydropyridine calcium channel blockers, or antiarrhythmic agents remains an alternative for patients who are not candidates for or prefer not to undergo ablation.[2][3][1]
Classification
There are several classification systems for supraventricular tachycardia, based on site of origin, QRS width, pulse regularity, and AV node dependence.[2][3]
- Supraventricular tachycardia can be classified based on site of origin into:
- Physiological sinus tachycardia
- Atrial tachycardia (focal and multifocal)
- Atrioventricular tachycardia, including AVNRT and AVRT
- Supraventricular tachycardia can be classified based on QRS width into:
- Narrow complex tachycardia (QRS ≤120 ms): sinus tachycardia, atrial flutter, atrial fibrillation, focal atrial tachycardia, multifocal atrial tachycardia, sinus node re-entry tachycardia, AVNRT, orthodromic AVRT, and junctional tachycardia.[2][1]
- Wide complex tachycardia (QRS >120 ms): SVT with aberrant conduction, SVT with pre-existing bundle branch block, antidromic AVRT, and atrial fibrillation with WPW (pre-excited AF).[2][3][1]
- Supraventricular tachycardia can be classified based on pulse regularity into:
- Regular: sinus tachycardia, atrial flutter with fixed conduction ratio, sinus node re-entry tachycardia, AVNRT, AVRT, and junctional tachycardia.[2][3]
- Irregular: atrial fibrillation, multifocal atrial tachycardia, and atrial flutter with variable block.[2][3]
- Supraventricular tachycardia can be classified based on AV node dependence into:
- AV node dependent: AVNRT and AVRT (orthodromic and antidromic).[2][3]
- AV node independent: Focal atrial tachycardia, atrial flutter, atrial fibrillation, multifocal atrial tachycardia, and inappropriate sinus tachycardia.[2][3]
Causes
Causes by Organ System
There are several causes and precipitants of supraventricular tachycardia across multiple organ systems. Major associated comorbidities include chronic pulmonary disease (15.7%), diabetes (12.5%), heart failure (8.4%), cerebrovascular disease (7.8%), and peripheral vascular disease (7.6%).[1] A comprehensive list is provided in the table below.
Differentiating Among the Different Types of Supraventricular Tachycardia
The individual subtypes of SVT can be distinguished from each other by certain physiological and electrical characteristics, many of which present on the patient's ECG. Supraventricular tachycardias must be differentiated from each other because management strategies may vary.[2][3] The response to AV nodal blockade with vagal maneuvers or adenosine is a key diagnostic tool: termination suggests an AV node-dependent arrhythmia, whereas persistence with AV block unmasking atrial activity suggests an AV node-independent arrhythmia.[1]
| Epidemiology | Rate | Rhythm | P waves | PR Interval | QRS complex | Response to maneuvers | |
|---|---|---|---|---|---|---|---|
| Sinus Tachycardia | More common in children and elderly; physiological response to stress, fever, pain, hypovolemia, etc. | Greater than 100 bpm | Regular | Upright, consistent, and normal in morphology | 0.12–0.20 sec and shortens with high heart rate | Less than or equal to 120 ms, consistent, and normal in morphology | Gradual slowing with vagal maneuvers; does not terminate abruptly.[2][3] |
| Atrial Fibrillation | More common in the elderly, following bypass surgery, in mitral valve disease, and in hyperthyroidism | Ventricular rate typically 110 to 180 bpm when uncontrolled | Irregularly irregular | Absent; fibrillatory waves | Absent | Less than or equal to 120 ms in the absence of aberrant conduction or pre-excitation | Does not terminate with adenosine or vagal maneuvers; may transiently slow ventricular rate.[2][3] |
| Atrial Flutter | More common in the elderly, structural heart disease, and post-cardiac surgery | Atrial rate typically 250–350 bpm; ventricular rate depends on conduction ratio | Regular with fixed block; may be irregular with variable block | Sawtooth pattern of flutter waves at 250 to 350 per minute | Varies depending upon the magnitude of the block | Less than or equal to 120 ms, consistent, and normal in morphology | Does not terminate; adenosine or vagal maneuvers may transiently increase AV block and unmask flutter waves.[2][3] |
| AV Nodal Reentry Tachycardia (AVNRT) | Most common PSVT, accounting for approximately 60% of cases; more common in females.[1] | 140–250 bpm in adults; can exceed 250 bpm in children | Regular | In typical AVNRT, the P wave is usually superimposed on or buried within the QRS complex, producing a pseudo-r' in V1 or pseudo-S in inferior leads.[2][3] | Cannot be calculated when the P wave is obscured by the QRS complex | Less than or equal to 120 ms, consistent, and normal in morphology | Terminates with adenosine or vagal maneuvers because it is AV node dependent.[2][3] |
| AV Reciprocating Tachycardia (AVRT) | Second most common PSVT, accounting for approximately 30% of cases; more common in males and occurs at a younger age than AVNRT.[1] | Typically 150–250 bpm | Regular | In orthodromic AVRT, a retrograde P wave is seen after the QRS complex.[2][3] | Short RP interval in orthodromic AVRT | Orthodromic: narrow QRS. Antidromic: wide QRS with pre-excitation. | Orthodromic AVRT terminates with adenosine or vagal maneuvers. Antidromic AVRT requires caution with adenosine; IV procainamide is preferred in selected pre-excited tachycardias.[2][3][1] |
| Inappropriate Sinus Tachycardia | Uncommon; most patients are in their late 20s to early 30s; more common in women.[2][3] | Resting heart rate >100 bpm with exaggerated heart rate response to minimal exertion | Regular | Normal morphology and precede the QRS complex | Normal | Less than or equal to 120 ms, consistent, and normal in morphology | Gradual slowing with vagal maneuvers; does not terminate abruptly. Adenosine may cause transient slowing.[2][3] |
| Junctional Tachycardia | Common after heart surgery, digitalis toxicity, or as an escape rhythm in AV block | Typically 110–250 bpm; nonparoxysmal junctional tachycardia 70–130 bpm | Regular | Usually inverted or retrograde; may be buried in the QRS complex or follow it | Usually buried in the QRS complex or short RP interval | Less than or equal to 120 ms, consistent, and normal in morphology | May not terminate with adenosine or vagal maneuvers; adenosine may cause transient slowing.[2][3] |
| Focal Atrial Tachycardia | Accounts for approximately 10% of PSVT and can occur at any age.[1] | Atrial rate typically 100–250 bpm | Regular; may be irregular if multifocal | P wave morphology differs from sinus P wave | Variable; depends on AV conduction | Less than or equal to 120 ms, consistent, and normal in morphology | Usually does not terminate with adenosine, although triggered-activity AT may terminate; vagal maneuvers may increase AV block without terminating tachycardia.[2][3][1] |
| Multifocal Atrial Tachycardia (MAT) | High incidence in the elderly and in patients with COPD or acute illness | Atrial rate >100 bpm | Irregular | P waves of varying morphology from at least three different foci | Variable PR intervals, RR intervals, and PP intervals | Less than or equal to 120 ms, consistent, and normal in morphology | Does not terminate with adenosine or vagal maneuvers. Treatment is directed at the underlying condition.[2][3] |
| Sinus Node Reentry Tachycardia | Uncommon; described among patients undergoing electrophysiology study for SVTs | 100 to 150 bpm | Regular | Upright P waves identical or nearly identical to sinus P waves | Normal PR interval | Less than or equal to 120 ms, consistent, and normal in morphology | Often terminates abruptly with vagal maneuvers, unlike sinus tachycardia, which slows gradually.[2][3] |
| Wolff-Parkinson-White Syndrome | Estimated prevalence of WPW pattern is approximately 100–300 per 100,000 worldwide.[2][3] | During orthodromic AVRT: 150–250 bpm. During pre-excited AF: ventricular rate can be very rapid. | Regular during AVRT; irregular during pre-excited AF | During sinus rhythm: P wave is normal but followed by short PR interval and delta wave | Short PR interval during sinus rhythm due to pre-excitation | During sinus rhythm: Delta wave and widened QRS due to ventricular pre-excitation | Orthodromic AVRT may terminate with vagal maneuvers or adenosine. Adenosine, verapamil, diltiazem, and digoxin are contraindicated in pre-excited AF because they may accelerate conduction over the accessory pathway and precipitate ventricular fibrillation. IV procainamide or ibutilide is preferred for pre-excited AF.[2][3][1] |
Differentiating Supraventricular Tachycardia from Ventricular Tachycardia
For a detailed discussion of how to distinguish ventricular tachycardia (VT) from supraventricular tachycardia (SVT), please visit the wide complex tachycardia differential diagnosis page.
When the diagnosis is uncertain, wide complex tachycardia should be treated as ventricular tachycardia until proven otherwise.[2][3] In brief, the diagnosis of ventricular tachycardia is more likely if:
- There is a history of myocardial infarction, congestive heart failure, or structural heart disease
- Ventricular tachycardia is more common in the elderly
- The electrical axis is −90 to −180 degrees
- The QRS is >140 ms
- There is AV dissociation
- There are positive or negative QRS complexes in all the precordial leads (concordance)
- The morphology of the QRS complexes resembles that of a previous premature ventricular contraction (PVC)
- The rate is usually 150–200 bpm
- The rhythm is usually regular
- The PR interval is variable
- Ventricular tachycardia does not typically terminate in response to adenosine or vagal maneuvers
Diagnosis
Symptoms
Symptoms that are common to SVT include the following:[1]
- Palpitations (86% of patients)
- Chest pain or sensation of tightness (47%)
- Shortness of breath (38%)
- Dizziness, lightheadedness, or presyncope
- Syncope, particularly with rapid rates or structural heart disease
- Anxiety
- Sweating
- Polyuria due to release of atrial natriuretic peptide during SVT[2][3]
- Neck pulsation ("frog sign"), particularly in AVNRT due to simultaneous atrial and ventricular contraction against closed AV valves[2][3]
Electrocardiogram
Shown below is an ECG depicting a tachycardia at a rate of 190/min with narrow QRS complexes indicating supraventricular tachycardia.
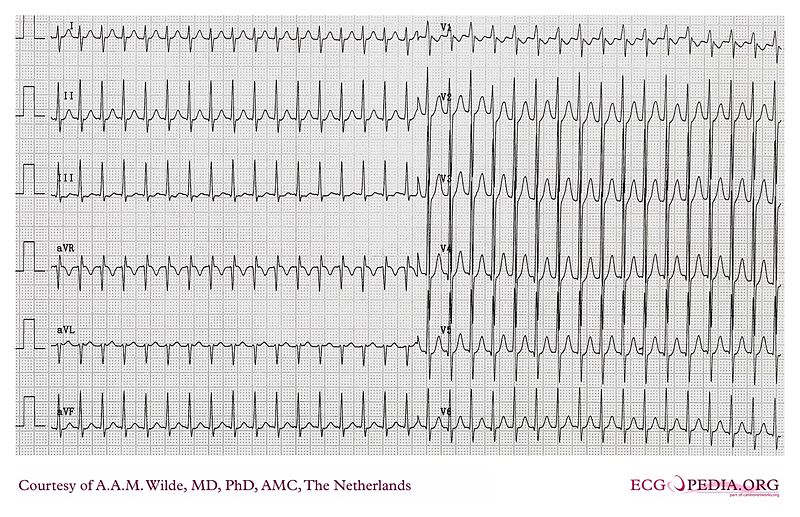
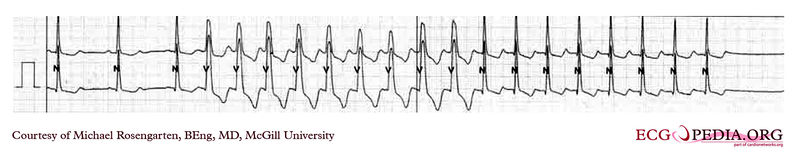
Shown below is an ECG recording of a patient who goes from sinus rhythm to a wide complex tachycardia at about 130/min.
- The wide QRS disappears after nine complexes and is replaced by narrow complexes at a slightly slower rate.
- No P wave activity is seen.
- This is a supraventricular tachycardia with aberrancy.
- In this case, a rate-dependent left bundle branch block is the likely explanation.
Diagnostic Workup
- A 12-lead ECG during tachycardia is the cornerstone of diagnosis and should be obtained whenever possible.[2][3][1]
- Comparison with a baseline ECG in sinus rhythm is essential to identify pre-excitation, delta waves, and pre-existing bundle branch block.[2][3]
- Ambulatory monitoring, including Holter monitor, event recorder, or implantable loop recorder, is recommended when episodes are not captured on standard ECG.[2][1]
- Electrophysiology (EP) study is the gold standard for definitive diagnosis of SVT mechanism and is typically performed at the time of catheter ablation.[2][3][1]
Treatment
Acute Treatment
Hemodynamically Unstable Patients
- Emergent synchronized cardioversion is recommended for patients with hemodynamically unstable SVT, including hypotension, acutely altered mental status, signs of shock, chest pain, or acute heart failure, when vagal maneuvers or adenosine are ineffective or not feasible.[2][3][4]
- Typical initial energy for synchronized cardioversion of SVT is 50 to 100 J.[4]
- Sedation is required for synchronized cardioversion in conscious patients when clinically feasible.[4]
Hemodynamically Stable Patients
Vagal Maneuvers
- Vagal maneuvers are recommended as first-line therapy for termination of hemodynamically stable SVT.[2][3][1]
- The modified Valsalva maneuver is more effective than the standard Valsalva maneuver. In the REVERT trial, conversion occurred in 43% with modified Valsalva compared with 17% with standard Valsalva.[5]
- Carotid sinus massage is an alternative vagal maneuver. Auscultation for carotid bruits should be performed before carotid sinus massage.[2][3]
- Facial immersion in cold water is another vagal maneuver.[2][3]
Acute Pharmacotherapy
- Intravenous adenosine is the first-line pharmacological agent for acute termination of hemodynamically stable SVT when vagal maneuvers fail.[2][3]
- Dosing: 6 mg rapid IV push; if ineffective after 1–2 minutes, 12 mg rapid IV push; a second 12 mg dose may be repeated.[2][3]
- Adenosine should be administered via a large-bore peripheral IV or central line, followed by a rapid saline flush.[2][3]
- Contraindications: Adenosine is contraindicated in pre-excited atrial fibrillation because AV blockade can induce rapid ventricular conduction over the accessory pathway and precipitate ventricular fibrillation.[2][3]
- Caution is advised in patients with severe asthma due to risk of bronchoconstriction.[4]
- Adenosine may induce atrial fibrillation by shortening the atrial refractory period.[4]
- Intravenous nondihydropyridine calcium channel blockers such as verapamil or diltiazem are alternatives when adenosine is ineffective or contraindicated.[2][3][1]
- Intravenous beta-blockers such as metoprolol or esmolol are guideline-recommended alternatives if adenosine is ineffective.[2][3]
- Intravenous procainamide is preferred for selected patients with hemodynamically stable wide-complex SVT, pre-excited AF, or antidromic AVRT.[2][3]
- Intravenous ibutilide is an alternative for pre-excited AF.[2][3]
- Etripamil (Cardamyst) is an intranasal, short-acting, nondihydropyridine calcium channel blocker indicated for conversion of acute symptomatic episodes of PSVT to sinus rhythm in adults.[6]
Algorithm for Acute SVT Management
- Assess hemodynamic stability.
- If unstable, perform emergent synchronized cardioversion.
- If stable, perform vagal maneuvers, preferably modified Valsalva.
- If vagal maneuvers fail, give IV adenosine.
- If adenosine fails, consider IV verapamil, IV diltiazem, or IV beta-blocker in appropriate patients.
- If wide-complex SVT, antidromic AVRT, or pre-excited AF is suspected, consider IV procainamide or ibutilide.
- Avoid adenosine, verapamil, diltiazem, digoxin, and beta-blockers in pre-excited AF.
- If pharmacological measures fail or instability develops, perform synchronized cardioversion.[2][3][4]
Prevention
Catheter Ablation
- Catheter ablation is recommended as first-line therapy for prevention of recurrent symptomatic PSVT, including AVNRT, AVRT, and symptomatic WPW syndrome.[2][3][1]
- Catheter ablation is safe, cost-effective, and often curative for PSVT.[1]
- AVNRT ablation: A meta-analysis of treatment groups demonstrated a single-procedure success rate of 94.3% (95% CI, 91.2%–97.4%).[1]
- A contemporary cohort of 877 patients undergoing AVNRT ablation reported long-term success of 95.5% with a 0.4% risk of AV block requiring a pacemaker.[9]
- AVRT/accessory pathway ablation: In a longitudinal cohort of 2,169 patients, acute success was 98.5%, with a 0.3% risk of AV block requiring a pacemaker.[1]
- Focal atrial tachycardia ablation: Acute success is approximately 77%.[1]
- Both radiofrequency ablation and cryoablation are effective for AVNRT.[10]
- Near-zero fluoroscopy approaches using 3D electroanatomic mapping systems have demonstrated favorable long-term outcomes compared with conventional fluoroscopy-guided ablation, with the benefit of reduced radiation exposure.[11]
- In the German Ablation Quality Registry, the periprocedural success rate was 96.3% overall and 98.9% for AVNRT. After 1 year, 74.1% of patients perceived ablation as successful.[12]
Pharmacological Prevention
- For patients who are not candidates for or prefer not to undergo catheter ablation, pharmacological therapy is recommended for prevention of recurrent SVT.[2][3][1]
- AVNRT and orthodromic AVRT without pre-excitation on baseline ECG:
- First-line: Oral beta-blockers, diltiazem, or verapamil.[2][3]
- Second-line: Oral flecainide or propafenone, with or without a beta-blocker or calcium channel blocker.[2][3]
- Third-line: Oral sotalol, dofetilide, or amiodarone.[2][3]
- WPW syndrome / pre-excitation:
- AV nodal blocking agents should be avoided as monotherapy in patients with pre-excitation because they may enhance conduction over the accessory pathway.[2][3][1]
- Oral flecainide or propafenone are preferred pharmacological options in selected WPW patients.[2][3]
- Catheter ablation is strongly recommended for symptomatic WPW syndrome.[2][3]
- Focal atrial tachycardia:
- Inappropriate sinus tachycardia:
- Beta-blockers are first-line therapy.[2][3]
- Ivabradine may be considered for patients refractory to or intolerant of beta-blockers.[2][3]
- Multifocal atrial tachycardia:
- Treatment is directed at the underlying condition.[2][3]
- Rate control with nondihydropyridine calcium channel blockers or beta-blockers may be used, although beta-blockers should be used cautiously in patients with severe COPD.[2][3]
- AV nodal ablation with pacemaker implantation may be considered in refractory cases.[2][3]
Pill-in-the-Pocket Approach
- For patients with infrequent but prolonged episodes of PSVT who prefer to avoid daily medication or catheter ablation, a "pill-in-the-pocket" approach may be considered.[2][3][1]
- This approach may involve patient self-administration of oral diltiazem plus propranolol at the onset of symptoms in selected patients.[1]
- This approach should be tested first in a monitored setting to ensure safety and tolerability.[2][3]
Special Populations
Pregnancy
SVT management during pregnancy should balance maternal clinical stability, fetal safety, and drug-specific risks.[13] The risk of SVT increases during pregnancy, and approximately 20% of patients with pre-existing SVT have exacerbations during pregnancy.[14]
Acute SVT in Pregnancy
- Vagal maneuvers are recommended as first-line therapy.[13]
- IV adenosine is recommended as first-line pharmacological therapy in hemodynamically stable patients.[13]
- Synchronized cardioversion is recommended for hemodynamically unstable patients, using energy dosing as in the nonpregnant patient.[13]
- IV metoprolol or propranolol is reasonable when adenosine is ineffective or contraindicated.[13]
- IV verapamil, diltiazem, or procainamide may be considered when adenosine and beta-blockers are ineffective or contraindicated.[13]
Chronic Prevention of SVT in Pregnancy
- First-line options include oral metoprolol, propranolol, and/or digoxin.[13]
- Atenolol should generally be avoided due to risk of fetal growth restriction.[13]
- Oral verapamil may be used as a second-line option.[13]
- For WPW syndrome, oral flecainide or propafenone may be used in selected patients.[13]
- Alternative antiarrhythmics such as flecainide, propafenone, or sotalol may be reasonable when first-line agents fail.[13]
- Amiodarone is typically avoided but may be considered in refractory, life-threatening cases.[13]
- Dronedarone is contraindicated in pregnancy.[13]
- Catheter ablation is reasonable for drug-refractory SVT, ideally after the first trimester using minimal or zero fluoroscopy techniques.[13]
- Preconception catheter ablation should be considered for eligible patients with known PSVT who are planning pregnancy.[1]
Athletes
- PSVT can be provoked by intense physical activity, and individuals with exercise-associated PSVT should undergo evaluation for structural heart disease.[1]
- Catheter ablation is recommended for athletes with WPW syndrome when clinically indicated because WPW can be associated with sudden cardiac arrest in young athletes.[15]
Elderly
Diagnostic and therapeutic approaches to SVT should be individualized in patients more than 75 years of age to incorporate age, comorbid illness, physical and cognitive function, patient preferences, and severity of symptoms.[2] Data have consistently demonstrated that ablation is highly successful in selected older patients.[2] In a German multicenter registry of 3,234 consecutive patients undergoing AVNRT ablation, 259 patients were >75 years of age, with comparable success rates to younger patients.[2] Caution is advised when performing carotid sinus massage in older patients because of potential thromboembolic risk.[2] Therapeutic decisions should balance the risks and benefits of ablation versus long-term pharmacological therapy, particularly in patients with comorbidities and polypharmacy.[2]
Adult Congenital Heart Disease (ACHD)
SVT management in adult congenital heart disease requires specialized consideration.[2] SVT is observed in 10% to 20% of ACHD patients and is associated with increased risk of heart failure, stroke, and sudden cardiac death.[2] The most common mechanism of SVT in ACHD patients is macroreentrant atrial tachycardia, also called atrial flutter, which often involves the cavotricuspid isthmus.[2] Management of ACHD patients should be undertaken in collaboration with a cardiologist who has specialized training or experience in managing such patients.[2]
Acute Treatment in ACHD
- Acute antithrombotic therapy is recommended in ACHD patients who have atrial tachycardia or atrial flutter, aligned with recommended antithrombotic therapy for patients with atrial fibrillation.[2]
- Synchronized cardioversion is recommended for hemodynamically unstable ACHD patients with SVT.[2]
- IV diltiazem or esmolol may be used with caution in hemodynamically stable ACHD patients with SVT, with careful monitoring for hypotension.[2]
- IV adenosine is recommended for acute treatment in ACHD patients with SVT. Adenosine is unlikely to terminate atrial reentry tachycardia or atrial flutter but may be diagnostic by producing transient AV block.[2]
- IV ibutilide or procainamide can be effective for hemodynamically stable ACHD patients with atrial flutter.[2]
Ongoing Management in ACHD
- Catheter ablation is reasonable for recurrent symptomatic SVT in ACHD patients.[2]
- Patients should be referred to centers with experience in complex congenital heart disease ablations.[2]
- The development of atrial arrhythmias in ACHD patients may indicate progressive hemodynamic changes that require functional and hemodynamic assessment.[2]
- Pharmacological options include beta-blockers, sotalol, and dofetilide in selected patients.[2]
- Flecainide should be used cautiously and is generally reserved for selected patients without ventricular dysfunction who do not respond to other therapy.[2]
Wolff-Parkinson-White Syndrome: Risk Stratification and Sudden Cardiac Death
The overall incidence of sudden cardiac death in WPW syndrome is approximately 1 event per 1,000 person-years.[15] Risk is higher in children than adults.[15] The lifetime risk of sudden cardiac death in WPW is low but is concentrated in younger patients.[15]
High-risk accessory pathway features include:
- Shortest pre-excited RR interval ≤250 ms
- Anterograde accessory pathway effective refractory period ≤240 ms
- Multiple accessory pathways
- Ebstein anomaly
- AVRT precipitating pre-excited atrial fibrillation or atrial flutter[2][15]
Catheter ablation is first-line therapy for symptomatic WPW syndrome.[2][15] For asymptomatic patients with WPW pattern, shared decision-making, EP study, and possible ablation are reasonable in adults, particularly in patients with high-risk occupations or competitive athletes.[2][15] Intermittent preexcitation does not reliably exclude high-risk accessory pathway properties.[15]
Prognosis
- The overall prognosis of patients with PSVT in the absence of structural heart disease is good, especially when treated with catheter ablation.[16]
- With pharmacotherapy alone, approximately 50% of patients continue to have at least monthly symptoms.[16]
- Tachycardia-mediated cardiomyopathy may occur in patients with persistent or frequent SVT.[1]
- PSVT has been associated with increased risk of stroke in observational studies, although the mechanism requires further elucidation.[1]
- PSVT may lead to inappropriate shocks in patients with implantable cardioverter-defibrillators due to misclassification of arrhythmia as ventricular tachyarrhythmia.[1]
- Among patients with infrequent episodes of AVNRT and tolerable symptoms who defer ablation and pharmacotherapy, a substantial proportion may eventually become asymptomatic.[1]
Indications for Cardiology Referral
Referral to cardiology or electrophysiology is appropriate for:
- Recurrent symptomatic PSVT for consideration of catheter ablation
- Symptomatic WPW syndrome for EP study and ablation
- Asymptomatic WPW pattern on ECG for risk stratification, particularly in patients with high-risk occupations, competitive athletes, or pediatric patients
- SVT refractory to first-line pharmacotherapy
- Wide-complex tachycardia of uncertain etiology
- SVT in the setting of structural heart disease or adult congenital heart disease
- Suspected tachycardia-mediated cardiomyopathy
- SVT causing hemodynamic compromise or syncope
- Patients requiring antiarrhythmic drug therapy beyond beta-blockers or calcium channel blockers[2][3][1]
References
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 1.14 1.15 1.16 1.17 1.18 1.19 1.20 1.21 1.22 1.23 1.24 1.25 1.26 1.27 1.28 1.29 1.30 1.31 1.32 1.33 1.34 1.35 1.36 1.37 1.38 1.39 1.40 Peng G, Zei PC (February 2024). "Diagnosis and Management of Paroxysmal Supraventricular Tachycardia". JAMA. 331 (7): 601–610. doi:10.1001/jama.2024.0076. PMID 38497695 Check
|pmid=value (help). - ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 2.11 2.12 2.13 2.14 2.15 2.16 2.17 2.18 2.19 2.20 2.21 2.22 2.23 2.24 2.25 2.26 2.27 2.28 2.29 2.30 2.31 2.32 2.33 2.34 2.35 2.36 2.37 2.38 2.39 2.40 2.41 2.42 2.43 2.44 2.45 2.46 2.47 2.48 2.49 2.50 2.51 2.52 2.53 2.54 2.55 2.56 2.57 2.58 2.59 2.60 2.61 2.62 2.63 2.64 2.65 2.66 2.67 2.68 2.69 2.70 2.71 2.72 2.73 2.74 2.75 2.76 2.77 2.78 2.79 2.80 2.81 2.82 2.83 2.84 2.85 2.86 2.87 2.88 2.89 Page RL, Joglar JA, Caldwell MA, Calkins H, Conti JB, Deal BJ, Estes NA 3rd, Field ME, Goldberger ZD, Hammill SC, Indik JH, Lindsay BD, Olshansky B, Russo AM, Shen WK, Tracy CM, Al-Khatib SM (April 2016). "2015 ACC/AHA/HRS Guideline for the Management of Adult Patients With Supraventricular Tachycardia: A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines and the Heart Rhythm Society". J Am Coll Cardiol. 67 (13): e27–e115. doi:10.1016/j.jacc.2015.08.856. PMID 26409259.
- ↑ 3.00 3.01 3.02 3.03 3.04 3.05 3.06 3.07 3.08 3.09 3.10 3.11 3.12 3.13 3.14 3.15 3.16 3.17 3.18 3.19 3.20 3.21 3.22 3.23 3.24 3.25 3.26 3.27 3.28 3.29 3.30 3.31 3.32 3.33 3.34 3.35 3.36 3.37 3.38 3.39 3.40 3.41 3.42 3.43 3.44 3.45 3.46 3.47 3.48 3.49 3.50 3.51 3.52 3.53 3.54 3.55 3.56 3.57 3.58 3.59 3.60 3.61 3.62 3.63 3.64 Brugada J, Katritsis DG, Arbelo E, Arribas F, Bax JJ, Blomström-Lundqvist C, Calkins H, Corrado D, Deftereos SG, Diller GP, Gomez-Doblas JJ, Gorenek B, Grace A, Ho SY, Kaski JC, Kuck KH, Lambiase PD, Sacher F, Sarquella-Brugada G, Suwalski P, Zaza A (February 2020). "2019 ESC Guidelines for the management of patients with supraventricular tachycardia". Eur Heart J. 41 (5): 655–720. doi:10.1093/eurheartj/ehz467. PMID 31504425.
- ↑ 4.0 4.1 4.2 4.3 4.4 4.5 4.6 Wigginton JG, Agarwal S, Bartos JA, Coute RA, Drennan IR, Haamid A, Kudenchuk PJ, Link MS, Panchal AR, Pelter MM, Del Rios M, Rodriguez AJ, Perman SM, Sanko S, Kotini-Shah P, Kurz MC (October 2025). "Part 9: Adult Advanced Life Support: 2025 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care". Circulation. 152 (16_suppl_2): S538–S577. doi:10.1161/CIR.0000000000001376. PMID 41122884 Check
|pmid=value (help). - ↑ Appelboam A, Reuben A, Mann C, Gagg J, Ewings P, Barton A, Lobban T, Dayer M, Vickery J, Benger J (October 2015). "Postural modification to the standard Valsalva manoeuvre for emergency treatment of supraventricular tachycardias (REVERT): a randomised controlled trial". Lancet. 386 (10005): 1747–1753. doi:10.1016/S0140-6736(15)61485-4. PMID 26314489.
- ↑ "Cardamyst prescribing information". Food and Drug Administration. 2025. Retrieved 2026-04-27.
- ↑ Stambler BS, Camm AJ, Alings M, Dorian P, Ip J, Reiffel J, Sager PT, Wight D, Wijesuriya N, Plat F, NODE-301 and RAPID Investigators (July 2023). "Self-administered intranasal etripamil using a symptom-prompted, repeat-dose regimen for atrioventricular-nodal-dependent supraventricular tachycardia (RAPID): a multicentre, randomised trial". Lancet. 402 (10396): 118–128. doi:10.1016/S0140-6736(23)00776-6. PMID 37331368 Check
|pmid=value (help). Vancouver style error: initials (help) - ↑ Ip JE, Coutu B, Ip JH, Noseworthy PA, Parody ML, Rafii F, Sears SF, Singh N, Stambler BS, Tahirkheli NK, Agudelo-Uribe J, Hu D, Shardonofsky S, Sheikh MB, Holz A, Bharucha DB, Camm AJ (September 2025). "Etripamil Nasal Spray for Recurrent Paroxysmal Supraventricular Tachycardia Conversion: Results From the NODE-303 Open-Label Study". J Cardiovasc Electrophysiol. doi:10.1111/jce.70086. PMID 40931676 Check
|pmid=value (help). - ↑ Chrispin J, Misra S, Marine JE, Spragg D, Rickard J, Barth AS, Kolandaivelu A, Tandri H, Berger RD, Calkins H (April 2018). "Current management and clinical outcomes for catheter ablation of atrioventricular nodal re-entrant tachycardia". Europace. 20 (4): e51–e59. doi:10.1093/europace/eux110. PMID 28541507.
- ↑ Siranart N, Keawkanha P, Pajareya P (March 2024). "Efficacy and safety between radiofrequency ablation and types of cryoablation catheters for atrioventricular nodal reentrant tachycardia: A network meta-analysis and systematic review". Pacing Clin Electrophysiol. 47 (3): 353–364. doi:10.1111/pace.14915.
- ↑ Bergonti M, Dello Russo A, Sicuso R (September 2021). "Long-Term Outcomes of Near-Zero Radiation Ablation of Paroxysmal Supraventricular Tachycardia: A Comparison With Fluoroscopy-Guided Approach". JACC Clin Electrophysiol. 7 (9): 1108–1117. doi:10.1016/j.jacep.2021.02.017.
- ↑ Brachmann J, Lewalter T, Kuck KH, Andresen D, Willems S, Spitzer SG, Eckardt L, Hoffmann E, Schumacher B, Tebbenjohanns J, Hochadel M, Senges J (May 2017). "Long-term symptom improvement and patient satisfaction following catheter ablation of supraventricular tachycardia: insights from the German ablation registry". Eur Heart J. 38 (17): 1317–1326. doi:10.1093/eurheartj/ehx101. PMID 28329395.
- ↑ 13.00 13.01 13.02 13.03 13.04 13.05 13.06 13.07 13.08 13.09 13.10 13.11 13.12 13.13 Joglar JA, Kapa S, Saarel EV, Dubin AM, Gorenek B, Hameed AB, Lara de Melo S, Leal MA, Mondésert B, Pacheco LD, Robinson MR, Sarkozy A, Silversides CK, Spears D, Srinivas SK, Strasburger JF, Tedrow UB, Wright JM, Zelop CM, Zentner D (October 2023). "2023 HRS expert consensus statement on the management of arrhythmias during pregnancy". Heart Rhythm. 20 (10): e175–e264. doi:10.1016/j.hrthm.2023.05.017. PMID 37211147 Check
|pmid=value (help). - ↑ Tamirisa KP, Elkayam U, Briller JE (January 2022). "Arrhythmias in Pregnancy". JACC Clin Electrophysiol. 8 (1): 120–135. doi:10.1016/j.jacep.2021.10.004.
- ↑ 15.0 15.1 15.2 15.3 15.4 15.5 15.6 15.7 "2024 HRS expert consensus statement on arrhythmias in the athlete: evaluation, treatment, and return to play". Heart Rhythm. 21 (10): e151–e246. October 2024. doi:10.1016/j.hrthm.2024.05.018.
- ↑ 16.0 16.1 Kotadia ID, Williams SE, O'Neill M (January 2020). "Supraventricular tachycardia: An overview of diagnosis and management". Clin Med (Lond). 20 (1): 43–47. doi:10.7861/clinmed.cme.20.1.3. PMC 6964177 Check
|pmc=value (help). PMID 31941731.