Myopathy
| Myopathy | |
 | |
|---|---|
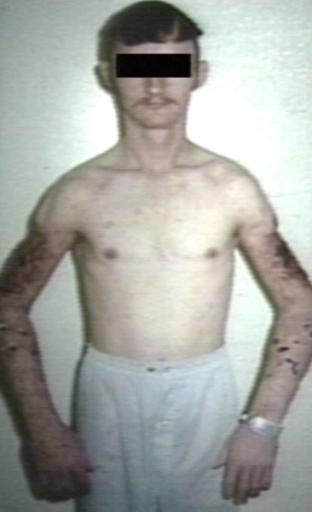
| Myopathy: Metabolic {Acid maltase) Image courtesy of Professor Peter Anderson DVM PhD and published with permission © PEIR, University of Alabama at Birmingham, Department of Pathology | |
| ICD-10 | G71 - G72 |
| ICD-9 | 359.4 - 359.9 |
| DiseasesDB | 8723 |
| eMedicine | emerg/328 |
| MeSH | D009135 |
Template:Search infobox Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]
Overview
In medicine, a myopathy is a neuromuscular disease in which the muscle fibers do not function for any one of many reasons, resulting in muscular weakness. "Myopathy" simply means muscle disease (myo- Greek μυσ "muscle" + pathy Greek "suffering"). This meaning implies that the primary defect is within the muscle, as opposed to the nerves ("neuropathies" or "neurogenic" disorders) or elsewhere (e.g., the brain etc.). Muscle cramps, stiffness, and spasm can also be associated with myopathy.
Classes
Because myopathy is such a general term, there are several classes of myopathy.... (ICD-10 codes are provided where available.)
- (G71.0) Dystrophies (or muscular dystrophies) are a subgroup of myopathies characterized by muscle degeneration and regeneration. Clinically, muscular dystrophies are typically progressive, because the muscles' ability to regenerate is eventually lost, leading to progressive weakness, often leading to use of a wheelchair, and eventually death, usually related to respiratory weakness.
- (G71.1) Myotonia
- (G71.2) The congenital myopathies do not show evidence for either a progressive dystrophic process (i.e., muscle death) or inflammation, but instead characteristic microscopic changes are seen in association with reduced contractile ability of the muscles. Among others, different congenital myopathies include:
- (G71.2) nemaline myopathy (characterized by presence of "nemaline rods" in the muscle),
- (G71.2) multi/minicore myopathy (characterized by multiple small "cores" or areas of disruption in the muscle fibers),
- (G71.2) centronuclear myopathy (or myotubular myopathy) (in which the nuclei are abnormally found in the center of the muscle fibers) is a rare muscle wasting disorder that occurs in three forms:
- The most severe form is present at birth, which is inherited as an X-linked genetic trait, and can cause severe respiratory muscle weakness. This is the form of centronuclear myopathy currently referred to as myotubular myopathy.
- A less severe form of centronuclear myopathy that may present itself at birth or in early childhood progresses slowly and is inherited as an autosomal recessive genetic trait.
- The least severe of the three forms of centronuclear myopathy first appears during the second and third decades of life and is slowly progressive; it is inherited as an autosomal dominant genetic trait.
- (G71.3) Mitochondrial myopathies are due to defects in mitochondria, which provide a critical source of energy for muscle.
- (G72.3) Familial periodic paralysis
- (G72.4) Inflammatory myopathies are caused by problems with the immune system attacking components of the muscle, leading to signs of inflammation in the muscle.
- (G73.6) Metabolic myopathies result from defects in biochemical metabolism that primarily affect muscle
- (G73.6/E74.0) Glycogen storage diseases may affect muscle
- (G73.6/E75) Lipid storage disorder
- (M33.0-M33.1) Dermatomyositis, (M33.2) polymyositis, inclusion body myositis, and related myopathies
- (M61) Myositis ossificans
- (M62.89) Rhabdomyolysis and (R82.1) myoglobinurias
- Common muscle (R25.2) cramps and (M25.6) stiffness, and (R29.0) tetany
Causes
Life Threatening Causes
Common Causes
- Aconitase deficiency
- Becker muscular dystrophy
- Brody myopathy
- Caveolin-3 related distal myopathy
- Congenital muscular dystrophy
- Desmin-related myopathy
- Distal myopathy 2
- Duchenne muscular dystrophy
- Emery-dreifuss muscular dystrophy
- Familial partial lipodystrophy type 2
- Laing distal myopathy
- Lama2-related muscular dystrophy
- Limb girdle muscular dystrophy
- Mitochondrial myopathy
- Mitochondrial trifunctional protein deficiency
- Miyoshi muscular dystrophy 2
- Muscular dystrophy
- Myoneurogastrointestinal encephalopathy syndrome
- Myosin storage myopathy
- Myotonia congenita
- Myotonic dystrophy
- Nonaka myopathy
- Osteomalacia
- Polymyositis
- Rigid spine muscular dystrophy
- Rippling muscle disease
- Salih myopathy
- Spheroid body myopathy
- Tubular aggregate myopathy
- Ullrich congenital muscular dystrophy
- Welander muscular dystrophy
Causes by Organ System
Causes in Alphabetical Order
- Aconitase deficiency
- Addison's disease
- Adenosine monophosphate deaminase deficiency
- Alcoholism
- Aldolase a deficiency
- Alpha-mannosidase deficiency
- Amish nemaline myopathy
- Amyloidosis
- Anoctaminopathy
- Arnold stickler bourne syndrome
- Arthrogryposis
- Atorvastatin
- Barth syndrome
- Becker muscular dystrophy
- Bethlem myopathy
- Bezafibrate
- Borud syndrome
- Brody myopathy
- Brown recluse spider poisoning
- Calpainopathy
- Carey-fineman-ziter syndrome
- Carnitine deficiency
- Carnitine palmitoyltransferase 2 deficiency
- Caveolin-3 related distal myopathy
- Chanarin-dorfman disease
- Chloroquine
- Christian syndrome 1
- Chronic hypokalemia
- Clevudine
- Colchicine
- Congenital muscular dystrophy
- Cushing's disease
- Cytochrome-c oxidase deficiency
- Dermatomyositis
- Desmin-related myopathy
- Diabetes
- Distal myopathy 2
- Duchenne muscular dystrophy
- Efavirenz
- Emery-dreifuss muscular dystrophy
- Ethanol
- Familial partial lipodystrophy type 2
- Forbes disease
- Freeman-sheldon syndrome
- Fukuyama congenital muscular dystrophy
- Gigantism
- Glutaric acidemia type 2
- Glycerol kinase deficiency
- Glycogen branching deficiency
- Glycogen storage diseases
- Glycogenosis
- Hereditary fibrosing poikiloderma
- Hiv-1 disease
- Hypercalcemia
- Hyperkalemia
- Hypermagnesemia
- Hyperparathyroidism
- Hyperthyroidism
- Hypocalcaemia
- Hypokalaemia
- Hyponatremia
- Hypothyroidism
- Kearns-sayre syndrome
- Lactate dehydrogenase deficiency
- Laing distal myopathy
- Lama2-related muscular dystrophy
- Limb girdle muscular dystrophy
- Long chain hydroxyacyl-coa dehydrogenase deficiency
- Lundberg ii syndrome
- Malignancy
- Malignant hyperthermia
- Marinesco-sjogren-garland syndrome
- Melas
- Merrf
- Mitochondrial myopathy
- Mitochondrial trifunctional protein deficiency
- Miyoshi muscular dystrophy 2
- Molybdenum cofactor deficiency
- Muscle-eye-brain disease
- Muscular dystrophy
- Myoneurogastrointestinal encephalopathy syndrome
- Myosin storage myopathy
- Myotonia congenita
- Myotonic dystrophy
- Neutral lipid storage disease
- Niacin
- Nonaka myopathy
- Osteomalacia
- Periodic paralysis
- Phencyclidine
- Phosphogylcerate mutase 2 deficiency
- Plasma membrane carnitine transporter deficiency
- Polymyositis
- Polyneuropathy
- Pork tapeworm
- Pravastatin
- Prednisolone
- Progressive external ophthalmoplegia
- Proximal renal tubular acidosis
- Rickets
- Rigid spine muscular dystrophy
- Rippling muscle disease
- Rosuvastatin
- Salih myopathy
- Sarcoidosis
- Short chain acyl-coa dehydrogenase deficiency
- Simvastatin
- Spheroid body myopathy
- Steroids
- Stormorken syndrome
- Subacute necrotising encephalomyelopathy
- Tel hashomer camptodactyly syndrome
- Telbivudine
- Thyroid eye disease
- Tk2-related mitochondrial dna depletion syndrome
- Triosephosphate isomerase deficiency
- Tubular aggregate myopathy
- Type iii glycogen storage disease
- Udd-markesbery tardive muscular dystrophy
- Ullrich congenital muscular dystrophy
- Walker-warburg syndrome
- Welander muscular dystrophy
- Wieacker-wolff syndrome
- Woods black norbury syndrome
- Xanthine oxidase deficiency
- Zidovudine
Differential Diagnosis of Muscle Weakness
To review the differential diagnosis of Proximal muscle weakness, click here.
To review the differential diagnosis of Distal muscle weakness, click here.
To review the differential diagnosis of inflammatory myopathy, click here.
To review the differential diagnosis of Muscle weakness and Fever, click here.
To review the differential diagnosis of Muscle weakness and Myalgia, click here.
To review the differential diagnosis of Muscle weakness and Gait abnormality, click here.
To review the differential diagnosis of Muscle weakness and Neuropathy, click here.
To review the differential diagnosis of Muscle weakness and stiffness, click here.
To review the differential diagnosis of Muscle weakness and Myoglobinuria, click here.
To review the differential diagnosis of Muscle weakness and Atrophy, click here.
| Organ system | Disease | Symptoms | History | Physical
Examination |
Diagnosis | ||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Age of onset | Muscle weakness | Fever | Myalgia | Contractures | Gait abnormality | Neuropathy | Atrophy | Stiffness | Myoglobinuria | Other features | Laboratory Findings | Creatine Kinase | Muscle Biopsy | Electromyogram | |||||
| Medication−induced | Corticosteroids[1] | Variable | Proximal | − | + | − | − | − | + | − | − |
|
|
|
|
|
|
| |
| Statins[2] | 60+ | Proximal | − | + | − | − | − | − | − | −/+(Rhabdomyolysis) |
|
|
|
|
|
|
| ||
| Alcohol[3] | Variable | Proximal | − | − | − | + | +/− | − | − | − |
|
|
|
|
|
| |||
| Organ system | Disease | Age of onset | Muscle weakness | Fever | Myalgia | Contractures | Gait abnormality | Neuropathy | Atrophy | Stiffness | Myoglobinuria | Other features | History | Physical
Examination |
Laboratory Findings | Creatine Kinase | Muscle Biopsy | Electromyogram | |
| Endocrine | Cushing's disease[4] | 25 −45 | Proximal | − | − | − | − | − | + | − | − |
|
|
|
|
|
|
Normal | |
| Adrenal insufficiency[5] | 30−50 years | Proximal | − | + | − | − | − | − | + | − |
|
|
|
|
|
| |||
| Hyperaldosteronism with myopathy[6] | 50 | Proximal & distal |
− | − | − | − | − | − | − | + |
|
|
|
| |||||
| Hyperthyroidism[7] | 40 | Proximal | − | − | − | − | − | + | + | + |
|
|
|
|
|
||||
| Hypothyroidism[8] | 55 | Proximal | − | + | + | − | − | + | + | + Rhabdomyolysis |
|
|
|
|
|
|
| ||
| Diabetic infraction[9] | 45 | Proximal | + | + | − | − | + | + | − | − |
|
|
|
| |||||
| Organ system | Disease | Age of onset | Muscle weakness | Fever | Myalgia | Contractures | Gait abnormality | Neuropathy | Atrophy | Stiffness | Myoglobinuria | Other features | History | Physical
Examination |
Laboratory Findings | Creatine Kinase | Muscle Biopsy | Electromyogram | |
| Inflammatory/ Rheumatologic | Dermatomyositis[10] | 40s−50s Can affect children |
Proximal | + | + | − | − | − | − | + | − |
|
|
|
|||||
| Polymyositis[11] | > 18 years | Proximal | + | + | − | − | − | − | + | − |
|
|
|
|
| ||||
| Inclusion body myositis[12] | 50s | Proximal & distal |
− | − | − | − | − | − | − | − |
|
|
|
|
|
|
|||
| Fibromyalgia[13] | 40−50s | Generalized | − | − | − | − | + | − | − | − |
|
|
|
|
|
|
| ||
| Polymyalgia Rheumatica[14] | 50s | Diffuse | + | + | − | − | − | − | + | − |
|
|
|
|
| ||||
| Organ system | Disease | Age of onset | Muscle weakness | Fever | Myalgia | Contractures | Gait abnormality | Neuropathy | Atrophy | Stiffness | Myoglobinuria | Other features | History | Physical
Examination |
Laboratory Findings | Creatine Kinase | Muscle Biopsy | Electromyogram | |
| Genetic | Becker muscular dystrophy[15] | <13yrs | Proximal | − | − | + | + | − | + | − | − |
|
|
|
|
|
|
||
| Duchenne muscular dystrophy[16] | <13 yrs | Proximal | − | − | + | + | − | + | − | − |
|
|
|
|
| ||||
| Limb−girdle muscular dystrophies[17] | <15 yrs | Proximal | − | + | + | + | − | + | − | − |
|
|
|
|
|
|
|||
| Myotonic dystrophy[18] | <18 years | Proximal & distal |
− | − | + | + | − | − | + | − |
|
|
|
|
|
|
|||
| Glycogen storage disease[19] | Variable | Proximal | − | − | − | − | − | + | − | − |
|
|
|
| |||||
| Organ system | Disease | Age of onset | Muscle weakness | Fever | Myalgia | Contractures | Gait abnormality | Neuropathy | Atrophy | Stiffness | Myoglobinuria | Other features | History | Physical
Examination |
Laboratory Findings | Creatine Kinase | Muscle Biopsy | Electromyogram | |
| Infectious | Lyme disease[20] | Variable | Proximal | + | + | − | +/− | + | − | − | − |
|
|
|
|
|
|
| |
| Influenza[21] | Variable | Proximal and Distal | + | + | − | + | − | − | − | + |
|
|
|
|
|
|
| ||
| Polio[22] | <5 yrs | Proximal | − | − | − | + | + | + | − | − |
|
|
|
|
|
|
| ||
| Syphilis[23] | Variable | Negative | − | − | − | + | + | − | − | − |
|
|
|
|
|
|
| ||
| Pyomyositis[24] | Variable | Proximal & Distal |
+ | + | − | − | − | − | + | − |
|
|
|
|
| ||||
| Organ system | Disease | Age of onset | Muscle weakness | Fever | Myalgia | Contractures | Gait abnormality | Neuropathy | Atrophy | Stiffness | Myoglobinuria | Other features | History | Physical
Examination |
Laboratory Findings | Creatine Kinase | Muscle Biopsy | Electromyogram | |
| Neurologic | ALS[25] | >35 | Proximal & Distal
|
− | − | − | − | + | + | + | − |
|
|
|
|
|
| ||
| Stroke[26] | >65 | Proximal & distal |
− | − | − | + | + | + | − | − |
|
|
|
|
|
|
| ||
| GBS[27] | 18 −350 | Proximal | − | − | − | + | − | − | + | − |
|
|
|
|
|
| |||
| Multiple Sclerosis[28] | 30's | Proximal & distal |
− | − | − | + | + | − | − | − |
|
|
|
|
|
|
| ||
| Organ system | Disease | Age of onset | Muscle weakness | Fever | Myalgia | Contractures | Gait abnormality | Neuropathy | Atrophy | Stiffness | Myoglobinuria | Other features | History | Physical
Examination |
Laboratory Findings | Creatine Kinase | Muscle Biopsy | Electromyogram | |
| Neuromuscular | Botulinum[29] | Variable | Distal | − | − | − | + | − | − | + | − |
|
|
|
|
|
|
| |
| Lambert−Eaton syndrome[30] | Variable | Distal | − | − | + | + | − | − | + | − |
|
|
| ||||||
| Myasthenia gravis[31] | Variable | Proximal | − | − | + | + | − | − | + | − |
|
| |||||||
Treatment
Because different types of myopathies are caused by many different pathways, there is no single treatment for myopathy. Treatments range from treatment of the symptoms to very specific cause-targeting treatments. Drug therapy, physical therapy, bracing for support, surgery, and even acupuncture are current treatments for a variety of myopathies.
Prognosis
The prognosis for individuals with a myopathy varies. Some individuals have a normal life span and little or no disability. For others, however, the disorder may be progressive, severely disabling, life-threatening, or fatal.
References
- ↑ Gupta A, Gupta Y (September 2013). "Glucocorticoid-induced myopathy: Pathophysiology, diagnosis, and treatment". Indian J Endocrinol Metab. 17 (5): 913–6. doi:10.4103/2230-8210.117215. PMC 3784879. PMID 24083177.
- ↑ Tomaszewski M, Stępień KM, Tomaszewska J, Czuczwar SJ (2011). "Statin-induced myopathies". Pharmacol Rep. 63 (4): 859–66. PMID 22001973.
- ↑ Preedy VR, Adachi J, Ueno Y, Ahmed S, Mantle D, Mullatti N, Rajendram R, Peters TJ (November 2001). "Alcoholic skeletal muscle myopathy: definitions, features, contribution of neuropathy, impact and diagnosis". Eur. J. Neurol. 8 (6): 677–87. PMID 11784353.
- ↑ Sharma V, Borah P, Basumatary LJ, Das M, Goswami M, Kayal AK (July 2014). "Myopathies of endocrine disorders: A prospective clinical and biochemical study". Ann Indian Acad Neurol. 17 (3): 298–302. doi:10.4103/0972-2327.138505. PMC 4162016. PMID 25221399.
- ↑ Ruff RL, Weissmann J (August 1988). "Endocrine myopathies". Neurol Clin. 6 (3): 575–92. PMID 3065602.
- ↑ Sambrook MA, Heron JR, Aber GM (April 1972). "Myopathy in association with primary hyperaldosteronism". J. Neurol. Neurosurg. Psychiatry. 35 (2): 202–7. PMC 494037. PMID 5037033.
- ↑ Li Q, Liu Y, Zhang Q, Tian H, Li J, Li S (July 2017). "Myopathy in hyperthyroidism as a consequence of rapid reduction of thyroid hormone: A case report". Medicine (Baltimore). 96 (30): e7591. doi:10.1097/MD.0000000000007591. PMC 5627834. PMID 28746208.
- ↑ Khaleeli AA, Griffith DG, Edwards RH (September 1983). "The clinical presentation of hypothyroid myopathy and its relationship to abnormalities in structure and function of skeletal muscle". Clin. Endocrinol. (Oxf). 19 (3): 365–76. PMID 6627693.
- ↑ Horton WB, Taylor JS, Ragland TJ, Subauste AR (2015). "Diabetic muscle infarction: a systematic review". BMJ Open Diabetes Res Care. 3 (1): e000082. doi:10.1136/bmjdrc-2015-000082. PMC 4410119. PMID 25932331.
- ↑ Dalakas MC (1991). "Polymyositis, dermatomyositis and inclusion-body myositis". N Engl J Med. 325 (21): 1487–98. doi:10.1056/NEJM199111213252107. PMID 1658649.
- ↑ Dalakas MC (1991). "Polymyositis, dermatomyositis and inclusion-body myositis". N Engl J Med. 325 (21): 1487–98. doi:10.1056/NEJM199111213252107. PMID 1658649.
- ↑ Dalakas MC (1991). "Polymyositis, dermatomyositis and inclusion-body myositis". N Engl J Med. 325 (21): 1487–98. doi:10.1056/NEJM199111213252107. PMID 1658649.
- ↑ Ohara N, Katada S, Yamada T, Mezaki N, Suzuki H, Suzuki A, Hanyu O, Yoneoka Y, Kawachi I, Shimohata T, Kakita A, Nishizawa M, Sone H (2016). "Fibromyalgia in a Patient with Cushing's Disease Accompanied by Central Hypothyroidism". Intern. Med. 55 (21): 3185–3190. doi:10.2169/internalmedicine.55.5926. PMC 5140872. PMID 27803417.
- ↑ Myklebust G, Gran JT (1996). "A prospective study of 287 patients with polymyalgia rheumatica and temporal arteritis: clinical and laboratory manifestations at onset of disease and at the time of diagnosis". Br J Rheumatol. 35 (11): 1161–8. PMID 8948307.
- ↑ Flanigan KM (August 2014). "Duchenne and Becker muscular dystrophies". Neurol Clin. 32 (3): 671–88, viii. doi:10.1016/j.ncl.2014.05.002. PMID 25037084.
- ↑ Flanigan KM (August 2014). "Duchenne and Becker muscular dystrophies". Neurol Clin. 32 (3): 671–88, viii. doi:10.1016/j.ncl.2014.05.002. PMID 25037084.
- ↑ Guglieri M, Straub V, Bushby K, Lochmüller H (October 2008). "Limb-girdle muscular dystrophies". Curr. Opin. Neurol. 21 (5): 576–84. doi:10.1097/WCO.0b013e32830efdc2. PMID 18769252.
- ↑ Udd B, Krahe R (October 2012). "The myotonic dystrophies: molecular, clinical, and therapeutic challenges". Lancet Neurol. 11 (10): 891–905. doi:10.1016/S1474-4422(12)70204-1. PMID 22995693.
- ↑ Kannourakis G (April 2002). "Glycogen storage disease". Semin. Hematol. 39 (2): 103–6. PMID 11957192.
- ↑ Schoenen J, Sianard-Gainko J, Carpentier M, Reznik M (August 1989). "Myositis during Borrelia burgdorferi infection (Lyme disease)". J. Neurol. Neurosurg. Psychiatry. 52 (8): 1002–5. PMC 1031843. PMID 2795056.
- ↑ Bove KE, Hilton PK, Partin J, Farrell MK (1983). "Morphology of acute myopathy associated with influenza B infection". Pediatr Pathol. 1 (1): 51–66. PMID 6687269.
- ↑ Howard RS (June 2005). "Poliomyelitis and the postpolio syndrome". BMJ. 330 (7503): 1314–8. doi:10.1136/bmj.330.7503.1314. PMC 558211. PMID 15933355.
- ↑ French P (January 2007). "Syphilis". BMJ. 334 (7585): 143–7. doi:10.1136/bmj.39085.518148.BE. PMC 1779891. PMID 17235095.
- ↑ Crum NF (September 2004). "Bacterial pyomyositis in the United States". Am. J. Med. 117 (6): 420–8. doi:10.1016/j.amjmed.2004.03.031. PMID 15380499.
- ↑ Zarei S, Carr K, Reiley L, Diaz K, Guerra O, Altamirano PF, Pagani W, Lodin D, Orozco G, Chinea A (2015). "A comprehensive review of amyotrophic lateral sclerosis". Surg Neurol Int. 6: 171. doi:10.4103/2152-7806.169561. PMC 4653353. PMID 26629397.
- ↑ Baldwin K, Orr S, Briand M, Piazza C, Veydt A, McCoy S (May 2010). "Acute ischemic stroke update". Pharmacotherapy. 30 (5): 493–514. doi:10.1592/phco.30.5.493. PMID 20412000.
- ↑ van Doorn PA (June 2013). "Diagnosis, treatment and prognosis of Guillain-Barré syndrome (GBS)". Presse Med. 42 (6 Pt 2): e193–201. doi:10.1016/j.lpm.2013.02.328. PMID 23628447.
- ↑ Goldenberg MM (March 2012). "Multiple sclerosis review". P T. 37 (3): 175–84. PMC 3351877. PMID 22605909.
- ↑ Cherington M (June 2004). "Botulism: update and review". Semin Neurol. 24 (2): 155–63. doi:10.1055/s-2004-830901. PMID 15257512.
- ↑ Titulaer MJ, Lang B, Verschuuren JJ (December 2011). "Lambert-Eaton myasthenic syndrome: from clinical characteristics to therapeutic strategies". Lancet Neurol. 10 (12): 1098–107. doi:10.1016/S1474-4422(11)70245-9. PMID 22094130.
- ↑ Jayam Trouth A, Dabi A, Solieman N, Kurukumbi M, Kalyanam J (2012). "Myasthenia gravis: a review". Autoimmune Dis. 2012: 874680. doi:10.1155/2012/874680. PMC 3501798. PMID 23193443.