Statins
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]
The statins (or HMG-CoA reductase inhibitors) form a class of hypolipidemic drugs used to lower cholesterol levels in people with or at risk of cardiovascular disease. They lower cholesterol by inhibiting the enzyme HMG-CoA reductase, which is the rate-limiting enzyme of the mevalonate pathway of cholesterol synthesis. Inhibition of this enzyme in the liver stimulates LDL receptors, resulting in an increased clearance of low-density lipoprotein (LDL) from the bloodstream and a decrease in blood cholesterol levels. The first results can be seen after one week of use and the effect is maximal after four to six weeks.
History
Template:Seealso Akira Endo and Masao Kuroda of Tokyo, Japan commenced research into inhibitors of HMG-CoA reductase in 1971 (Endo 1992). This team reasoned that certain microorganisms may produce inhibitors of the enzyme to defend themselves against other organisms, as mevalonate is a precursor of many substances required by organisms for the maintenance of their cell wall (ergosterol) or cytoskeleton (isoprenoids).[1]
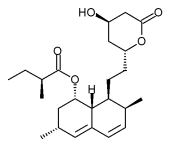
The first agent isolated was mevastatin (ML-236B), a molecule produced by Penicillium citrinum. The pharmaceutical company Merck & Co. showed an interest in the Japanese research in 1976, and isolated lovastatin (mevinolin, MK803), the first commercially marketed statin, from the mold Aspergillus terreus. Dr Endo was awarded the 2006 Japan Prize for his work on the development of statins.
Indications and uses
Statins, the most potent cholesterol-lowering agents available, lower LDL cholesterol (so-called "bad cholesterol") by 30–50%.[2] However, they have less effect than the fibrates or niacin in reducing triglycerides and raising HDL-cholesterol ("good cholesterol"). Professional guidelines generally require that the patient has tried a cholesterol-lowering diet before statin use is considered; statins or other pharmacologic agents may then be recommended for patients who do not meet their lipid-lowering goals through diet and lifestyle approaches.
The indications for the prescription of statins have broadened over the years. Initial studies, such as the Scandinavian Simvastatin Survival Study (4S), supported the use of statins in secondary prevention for cardiovascular disease, or as primary prevention only when the risk for cardiovascular disease was significantly raised (as indicated by the Framingham risk score).[3] Indications were broadened considerably by studies such as the Heart Protection Study (HPS), which showed preventative effects of statin use in specific risk groups, such as diabetics. The ASTEROID trial, published in 2006, using only a statin at high dose, achieved lower than usual target calculated LDL values and showed disease regression within the coronary arteries using intravascular ultrasonography.[4]
Based on clinical trials, the National Cholesterol Education Program guidelines, and the increasing focus on aggressively lowering LDL-cholesterol, the statins continue to play an important role in both the primary and secondary prevention of coronary heart disease, myocardial infarction, stroke and peripheral artery disease.
Research continues into other areas where statins also appear to have a favorable effect: inflammation, dementia,[5] cancer,[6] nuclear cataracts,[7] and pulmonary hypertension.[citation needed]
Members
The statins are divided into two groups: fermentation-derived and synthetic.
The statins include, in alphabetical order (brand names vary in different countries):
| Statin | Brand name | Derivation |
| Atorvastatin | Lipitor, Torvast | Synthetic |
| Cerivastatin | Lipobay, Baycol. (Withdrawn from the market in August, 2001 due to risk of serious adverse effects) | Synthetic |
| Fluvastatin | Lescol, Lescol XL | Synthetic |
| Lovastatin | Mevacor, Altocor | Fermentation-derived |
| Mevastatin | - | Naturally-occurring compound. Found in red yeast rice. |
| Pitavastatin | Livalo, Pitava | Synthetic |
| Pravastatin | Pravachol, Selektine, Lipostat | Fermentation-derived |
| Rosuvastatin | Crestor | Synthetic |
| Simvastatin | Zocor, Lipex | Fermentation-derived. (Simvastatin is a synthetic derivate of a fermentation product) |
| Simvastatin+Ezetimibe | Vytorin | Combination therapy |
| Lovastatin+Niacin extended-release | Advicor | Combination therapy |
| Atorvastatin+Amlodipine Besylate | Caduet | Combination therapy - Cholesterol+Blood Pressure |
LDL-lowering potency varies between agents. Cerivastatin is the most potent, followed by (in order of decreasing potency) rosuvastatin, atorvastatin, simvastatin, lovastatin, pravastatin, and fluvastatin.[8] The relative potency of pitavastatin has not yet been fully established.
Comparative effectiveness
No large scale comparison exists that examines the effectiveness of the various statins against one another.
An independent analysis has been done to compare atorvastatin, pravastatin and simvastatin, based on their effectiveness against placebos. It found that, at commonly prescribed doses, there are no statistically significant differences in reducing cardiovascular morbidity and mortality.[9]
Safety
Adverse effects
While some patients on statin therapy report myalgias, muscle cramps, or far less-frequent gastrointestinal or other symptoms, similar symptoms are also reported with placebo use in all the large statin safety/efficacy trials and usually resolve, either on their own or on temporarily lowering/stopping the dose. Liver enzyme derangements may also occur, typically in about 0.5%,[citation needed] are also seen at similar rates with placebo use and repeated enzyme testing, and generally return to normal either without discontinuance over time or after briefly discontinuing the drug. Multiple other side-effects occur rarely; typically also at similar rates with only placebo in the large statin safety/efficacy trials.
A clearer major safety concern, myositis, myopathy, rarely with rhabdomyolysis (the pathological breakdown of skeletal muscle) may lead to acute renal failure when muscle breakdown products damage the kidney. Coenzyme Q10 (ubiquinone) levels are decreased in statin use;[10] Q10 supplements are sometimes used to treat statin-associated myopathy, though evidence of their effectiveness is currently lacking.[11]
One 2004 study found that of 10,000 patients treated for one year, 0.44 will develop rhabdomyolysis. Cerivastatin, which was withdrawn by its manufacturer for this reason in 2001, had a much higher incidence (more than 10x).[12] All commonly used statins show somewhat similar results, however the newer statins, characterized by longer pharmacological half-lives and more cellular specificity, have had a better ratio of efficacy to lower adverse effect rates. The risk of myopathy is lowest with pravastatin and fluvastatin probably because they are more hydrophillic and as a result have less muscle penetration.
Despite initial concerns that statins might increase the risk of cancer, various studies concluded later that statins have no influence on cancer risk (including the heart protection study and a 2006 meta-analysis[13]). Indeed, a 2005 trial showed that patients taking statins for over 5 years reduced their risk of colorectal cancer by 50%; this effect was not exhibited by fibrates. The trialists warn that the number needed to treat would approximate 5000, making statins unlikely tools for primary prevention.[14]
Drug interactions
Combining any statin with a fibrate, another category of lipid-lowering drugs, increases the risks for rhabdomyolysis to almost 6.0 per 10,000 person-years.[12] Most physicians have now abandoned routine monitoring of liver enzymes and creatine kinase, although they still consider this prudent in those on high-dose statins or in those on statin/fibrate combinations, and mandatory in the case of muscle cramps or of deterioration in renal function.
Consumption of grapefruit or grapefruit juice inhibits the metabolism of statins—furanocoumarins in grapefruit juice inhibit the cytochrome P450 enzyme CYP3A4, which is involved in the metabolism of most statins (however it is a major inhibitor of only atorvastatin, lovastatin and simvastatin) and some other medications[15] (it had been thought that flavonoids were responsible). This increases the levels of the statin, increasing the risk of dose-related adverse effects (including myopathy/rhabdomyolysis). Consequently, consumption of grapefruit juice is not recommended in patients undergoing therapy with most statins. An alternative, somewhat risky, approach is that some users take grapefruit juice to enhance the effect of lower (hence cheaper) doses of statins. This is not recommended as a result of the increased risk and potential for statin toxicity.
Pharmacogenomics
A 2004 study showed that patients with one of two common single nucleotide polymorphisms (small genetic variations) in the HMG-CoA reductase gene were less responsive to statins.[16]
Mode of action
Cholesterol lowering
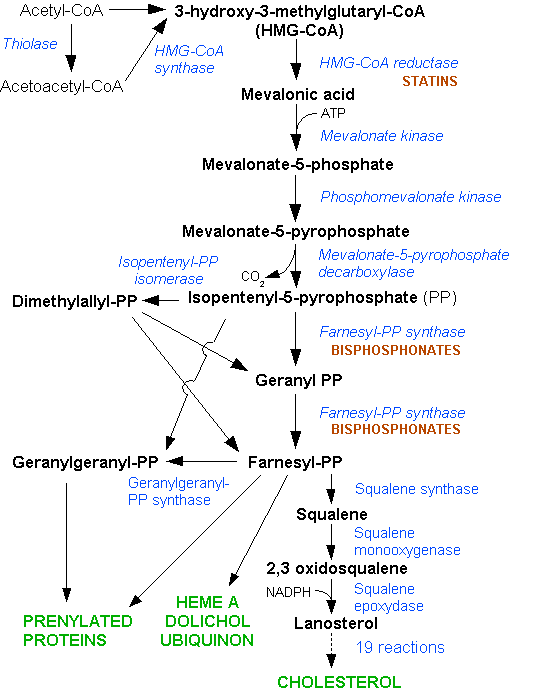
Most circulating cholesterol is manufactured internally, in amounts of about 1000 mg/day, via steroid biosynthesis through the HMG-CoA reductase pathway. Cholesterol, both from dietary intake and secreted into the duodenum as bile from the liver, is typically absorbed at a rate of 50% by the small intestines. The typical diet in the United States and many other Western countries is estimated as adding about 200–300 mg/day to intestinal intake, an amount much smaller than that secreted into the intestine in the bile. Thus internal production is an important factor.
Cholesterol is not water-soluble, and is therefore carried in the blood in the form of lipoproteins, the type being determined by the apoprotein, a protein coating that acts as an emulsifier. The relative balance between these lipoproteins is determined by various factors, including genetics, diet, and insulin resistance. Low density lipoprotein (LDL) and very low density lipoprotein (VLDL) carry cholesterol toward tissues, and elevated levels of these lipoproteins are associated with atheroma formation (fat-containing deposits in the arterial wall) and cardiovascular disease. High density lipoprotein, in contrast, carries cholesterol back to the liver and is associated with protection against cardiovascular disease.
Statins act by competitively inhibiting HMG-CoA reductase, the first committed enzyme of the HMG-CoA reductase pathway. By reducing intracellular cholesterol levels, they cause liver cells to make more LDL receptors, leading to increased clearance of low-density lipoprotein from the bloodstream.[17]
Direct evidence of the action of statin-based cholesterol lowering on atherosclerosis was presented in the ASTEROID trial, which demonstrated regression of atheroma employing intravascular ultrasound.[4]
Non-cholesterol related actions
Statins exhibit action beyond lipid-lowering activity in the prevention of atherosclerosis. Researchers hypothesize that statins prevent cardiovascular disease via four proposed mechanisms (all subjects of a large body of biomedical research):[18]
- Improving endothelial function
- Modulate inflammatory responses
- Maintain plaque stability
- Prevent thrombus formation
Controversy
Some scientists take a skeptical view of the need for many people to require statin treatment. The International Network of Cholesterol Skeptics is a group that has questioned the "lipid hypothesis" that supports cholesterol lowering as a preventive measure for heart disease, and has argued that statins - especially at higher doses - may not be as beneficial or safe as suggested.[19] Similarly, some authors argue that recommendations for the expanded use of statins to stave off cardiovascular disease are not supported by evidence.[20]
References
- ↑ Endo A (1992). "The discovery and development of HMG-CoA reductase inhibitors" (PDF). J. Lipid Res. 33 (11): 1569–82. PMID 1464741.
- ↑ Jones P, Kafonek S, Laurora I, Hunninghake D (1998). "Comparative dose efficacy study of atorvastatin versus simvastatin, pravastatin, lovastatin, and fluvastatin in patients with hypercholesterolemia (the CURVES study)". Am J Cardiol. 81 (5): 582–7. PMID 9514454.
- ↑ Wilson P, D'Agostino R, Levy D, Belanger A, Silbershatz H, Kannel W (1998). "Prediction of coronary heart disease using risk factor categories". Circulation. 97 (18): 1837–47. PMID 9603539.
- ↑ 4.0 4.1 Nissen S, Nicholls S, Sipahi I, Libby P, Raichlen J, Ballantyne C, Davignon J, Erbel R, Fruchart J, Tardif J, Schoenhagen P, Crowe T, Cain V, Wolski K, Goormastic M, Tuzcu E (2006). "Effect of very high-intensity statin therapy on regression of coronary atherosclerosis: the ASTEROID trial". JAMA. 295 (13): 1556–65. PMID 16533939.
- ↑ Wolozin, B (July 19, 2007). "Simvastatin is associated with a reduced incidence of dementia and Parkinson's disease". BMC Medicine. 5: 20. doi:10.1186/1741-7015-5-20. PMID 17640385. Unknown parameter
|coauthors=ignored (help) PMC 1955446 - ↑ Khurana, V (May 2007). "Statins reduce the risk of lung cancer in humans: a large case-control study of US veterans". Chest. 131 (5): 1282–1288. PMID 17494779. Unknown parameter
|coauthors=ignored (help) - ↑ Klein, Barbara E. K., MD, MPH (2006). "Statin Use and Incident Nuclear Cataract". JAMA. 295 (23): 2752–8. PMID 16788130. Unknown parameter
|coauthors=ignored (help); Unknown parameter|month=ignored (help) - ↑ Shepherd J, Hunninghake DB, Barter P, McKenney JM, Hutchinson HG (2003). "Guidelines for lowering lipids to reduce coronary artery disease risk: a comparison of rosuvastatin with atorvastatin, pravastatin, and simvastatin for achieving lipid-lowering goals". Am. J. Cardiol. 91 (5A): 11C–17C, discussion 17C-19C. doi:10.1016/S0002-9149(03)00004-3. PMID 12646338.
- ↑ Zhou Z, Rahme E, Pilote L (2006). "Are statins created equal? Evidence from randomized trials of pravastatin, simvastatin, and atorvastatin for cardiovascular disease prevention". Am. Heart J. 151 (2): 273–81. doi:10.1016/j.ahj.2005.04.003. PMID 16442888.
- ↑ Ghirlanda G, Oradei A, Manto A, Lippa S, Uccioli L, Caputo S, Greco A, Littarru G (1993). "Evidence of plasma CoQ10-lowering effect by HMG-CoA reductase inhibitors: a double-blind, placebo-controlled study". J Clin Pharmacol. 33 (3): 226–9. PMID 8463436.
- ↑ Marcoff L, Thompson PD (2007). "The role of coenzyme Q10 in statin-associated myopathy: a systematic review". J. Am. Coll. Cardiol. 49 (23): 2231–7. doi:10.1016/j.jacc.2007.02.049. PMID 17560286.
- ↑ 12.0 12.1 Graham DJ, Staffa JA, Shatin D; et al. (2004). "Incidence of hospitalized rhabdomyolysis in patients treated with lipid-lowering drugs". JAMA. 292 (21): 2585–90. doi:10.1001/jama.292.21.2585. PMID 15572716.
- ↑ Dale KM, Coleman CI, Henyan NN, Kluger J, White CM (2006). "Statins and cancer risk: a meta-analysis". JAMA. 295 (1): 74–80. doi:10.1001/jama.295.1.74. PMID 16391219.
- ↑ Poynter JN, Gruber SB, Higgins PD; et al. (2005). "Statins and the risk of colorectal cancer". N. Engl. J. Med. 352 (21): 2184–92. doi:10.1056/NEJMoa043792. PMID 15917383.
- ↑ Kane GC, Lipsky JJ (2000). "Drug-grapefruit juice interactions". Mayo Clin. Proc. 75 (9): 933–42. PMID 10994829.
- ↑ Chasman DI, Posada D, Subrahmanyan L, Cook NR, Stanton VP, Ridker PM (2004). "Pharmacogenetic study of statin therapy and cholesterol reduction". JAMA. 291 (23): 2821–7. doi:10.1001/jama.291.23.2821. PMID 15199031.
- ↑ Ma PT, Gil G, Südhof TC, Bilheimer DW, Goldstein JL, Brown MS (1986). "Mevinolin, an inhibitor of cholesterol synthesis, induces mRNA for low density lipoprotein receptor in livers of hamsters and rabbits" (PDF). Proc. Natl. Acad. Sci. U.S.A. 83 (21): 8370–4. PMID 3464957. PMC 386930
- ↑ Furberg CD (1999). "Natural Statins and Stroke Risk". Circulation. 99: 185–188. PMID 9892578.
- ↑ Ravnskov U, Rosch P, Sutter M, Houston M (2006). "Should we lower cholesterol as much as possible?". BMJ. 332 (7553): 1330–2. doi:10.1136/bmj.332.7553.1330. PMID 16740566.
- ↑ Abramson J, Wright J (2007). "Are lipid-lowering guidelines evidence-based?". Lancet. 369 (9557): 168–9. doi:10.1016/S0140-6736(07)60084-1. PMID 17240267.
External links
- Statin page at Bandolier, an evidence-based medicine journal
de:Statin it:statina nl:Statine fi:Statiini th:สแตติน sv:Statiner