Muscle atrophy
| Muscle atrophy | |
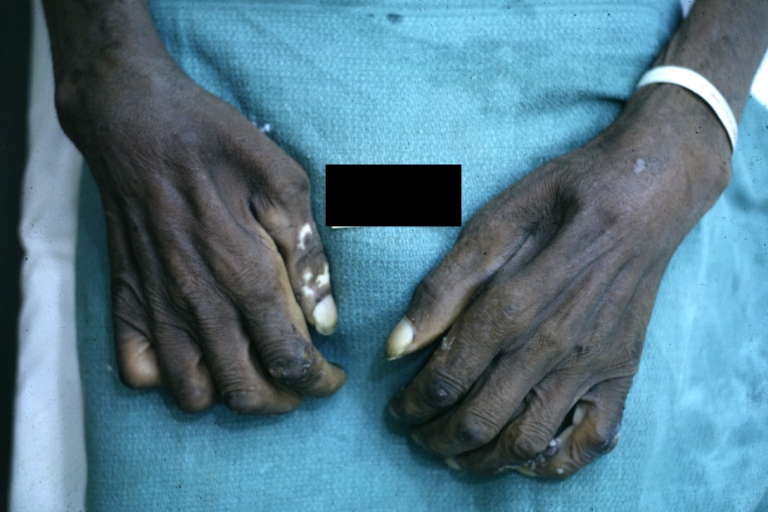 | |
|---|---|
| Muscle atrophy. Image courtesy of Professor Peter Anderson DVM PhD and published with permission © PEIR, University of Alabama at Birmingham, Department of Pathology |
|
WikiDoc Resources for Muscle atrophy |
|
Articles |
|---|
|
Most recent articles on Muscle atrophy Most cited articles on Muscle atrophy |
|
Media |
|
Powerpoint slides on Muscle atrophy |
|
Evidence Based Medicine |
|
Clinical Trials |
|
Ongoing Trials on Muscle atrophy at Clinical Trials.gov Trial results on Muscle atrophy Clinical Trials on Muscle atrophy at Google
|
|
Guidelines / Policies / Govt |
|
US National Guidelines Clearinghouse on Muscle atrophy NICE Guidance on Muscle atrophy
|
|
Books |
|
News |
|
Commentary |
|
Definitions |
|
Patient Resources / Community |
|
Patient resources on Muscle atrophy Discussion groups on Muscle atrophy Patient Handouts on Muscle atrophy Directions to Hospitals Treating Muscle atrophy Risk calculators and risk factors for Muscle atrophy
|
|
Healthcare Provider Resources |
|
Causes & Risk Factors for Muscle atrophy |
|
Continuing Medical Education (CME) |
|
International |
|
|
|
Business |
|
Experimental / Informatics |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1] Template:AB Associate Editor(s)-in-Chief: Cafer Zorkun, M.D., Ph.D. [2] Luke Rusowicz-Orazem, B.S.
Muscle atrophy refers to a decrease in the size of skeletal muscle, which occurs in a variety of settings. Atrophy may or may not be distinct from "sarcopenia", which is the loss of muscle seen in the aged.
When a muscle atrophies, it necessarily becomes weaker, since the ability to exert force is related to mass.
Clinical settings of atrophy
There are many diseases and conditions which cause a decrease in muscle mass, known as atrophy, including: inactivity, as seen when a cast is put on a limb, or upon extended bedrest (which can occur during a prolonged illness); cachexia - which is a "body-wasting" syndrome that is a co-morbidity of cancer and Congestive Heart Failure; Chronic Obstructive Pulmonary Disease; burns, liver failure, etc. Other syndromes or conditions which can induce skeletal muscle atrophy are congestive heart disease, liver disease, and starvation.
Causes
Life Threatening Causes
- Alcoholism
- Amyotrophic lateral sclerosis
- Back tumor
- Cerebrovascular accident
- Arachnoiditis
- Chondroblastoma
- Chronic kidney disease
- Embolism of great vessel
- Hepatoma
- Herpes zoster
- Hip cancer
- Hiv
- Ischemic palsy
- Malignancy
- Marasmus
- Multiple sclerosis
- Neurodegeneration
- Neurosyphilis
- Parasitic infections
- Parkinson's disease
- Polio
- Polyarteritis nodosa
- Polymyositis
- Primary biliary cirrhosis
- Primary lateral sclerosis
- Rib tumor
- Soft tissue hemorrhage
- Spinal cord tumor
- Spinal tumor
- Stroke
- Tuberculosis
Common Causes
- Adult progressive spinal muscular atrophy
- Adult sma
- Athermoatous disease
- Back tumor
- Becker's muscular dystrophy
- Cachexia
- Camurati-engelmann disease
- Carpal tunnel syndrome
- Cerebellar ataxia
- Cervical spondylosis
- Chondroblastoma
- Congenital muscular dystrophy
- Disuse of limb
- Duchenne muscular dystrophy
- Erb-goldflam
- Erb's dystrophy
- Fascioscapulohumeral
- Foix-alajouanine syndrome
- Fosmn syndrome
- Fukuyama type muscular dystrophy
- Furukawa-takagi-nakao syndrome
- Gamstorp-wohlfart syndrome
- Hematomyelia
- Hereditary inclusion body myopathy
- Hereditary peripheral nervous disorder
- Herniated disk
- Hip cancer
- Hypertrophic neuropathy of dejerine-sottas
- Immobility
- Immobilized fractures
- Inclusion body myopathy
- Inclusion body myositis
- Joint disuse
- Joint inflammation
- Joint injuries
- Kuskokwim disease
- Lambert-eaton myasthenic syndrome
- Landouzy-dejerine muscular dystrophy
- Legg-calve-perthes disease
- Letterer-siwe disease
- Limb-girdle muscular dystrophy type
- Lumbar canal stenosis
- Lumbar spondylosis
- Meniscal tear
- Mitochondrial myopathy
- Motor neuropathy
- Muscle disuse
- Muscle injury
- Muscular dystrophy
- Muscular fibrosis
- Muscular phosphorylase kinase deficiency
- Myasthenia
- Myasthenic syndrome
- Myopathy
- Nadh coq reductase
- Nemalin myopathy
- Nodulosis-arthropathy-osteolysis syndrome
- Osteoarthritis
- Osteogenesis imperfecta
- Paralysis of limbs
- Polymyositis
- Posterior column ataxia
- Primary biliary cirrhosis
- Primary lateral sclerosis
- Primary muscle disease
- Progressive spinal muscular atrophy
- Prolapsed lumbar intervertebral disc
- Prolonged immobilization
- Proximal spinal muscular atrophy
- Salvioli syndrome
- Soft tissue edema
- Soft tissue hemorrhage
- Spinal cord injury
- Spinal cord lesion
- Spinal cord tumor
- Spinal muscular atrophy
- Spinal tumor
- Spinocerebellar ataxia
- Subacute combined degeneration of the spinal cord
- Syphilitic amyotrophy
- Syringomyelia
- Thoracic outlet syndrome
- Vacuolar myopathy
- Volkmann's contracture
- Welander distal myopathy
Causes by Organ System
Causes in Alphabetical Order
- Acanthocytosis
- Acyl-coa dehydrogenase
- Addison's disease
- Adrenal dysfunction
- Adult progressive spinal muscular atrophy
- Adult sma
- Aids wasting syndrome
- Alcoholic neuropathy
- Alcoholism
- Allan-herndon-dudley syndrome
- Alves castelo dos santos syndrome
- Amyotrophic lateral sclerosis
- Andersen disease
- Andrade's syndrome
- Ankylosis
- Anorexia nervosa
- Arachnoiditis
- Arthritis
- Arthrogryposis
- Ataxia
- Athermoatous disease
- Back tumor
- Bacterial infections
- Balo's concentric sclerosis
- Banti syndrome
- Bard-pic syndrome
- Becker's muscular dystrophy
- Bed rest
- Bethlem myopathy
- Bovine spongiform encephalopathy
- Bruyn-scheltens syndrome
- Buerger's disease
- Burns
- Cachexia
- Camurati-engelmann disease
- Carnitine deficiency
- Carpal tunnel syndrome
- Cerebellar ataxia
- Cerebrovascular accident
- Cervical spondylosis
- Charcot-marie-tooth disease
- Charlevoix-saguenay spastic ataxia
- Chondroblastoma
- Chronic diarrhoea
- Chronic kidney disease
- Cocaine
- Coenzyme q 10 (coq10) deficiency
- Complex 1 mitochondrial respiratory chain deficiency
- Congenital disorder of glycosylation
- Congenital muscular dystrophy
- Coxsacki b virus
- Creutzfeldt-jakob disease
- Cushing's disease
- Cutler syndrome
- Cytoplasmic body myopathy
- Damage to nerve supplying muscle
- Decreased appetite
- Degenerative motor system disease
- Dermatomyositis
- Diabetes
- Diabetic neuropathy
- Disuse of limb
- Drug use
- Duchenne muscular dystrophy
- Dyskeratosis congenita of zinsser-cole-engman
- Dystrophia myotonica 1
- Embolism of great vessel
- Emery-dreifuss syndrome
- Endocrine disorders
- Erb-goldflam
- Erb's dystrophy
- Facwa syndrome
- Fascioscapulohumeral
- Foix-alajouanine syndrome
- Fosmn syndrome
- Friedreich ataxia
- Fukuyama type muscular dystrophy
- Furukawa-takagi-nakao syndrome
- Gamstorp-wohlfart syndrome
- Gangliosidosis
- Generalized myasthenia gravis
- Glandular fever
- Glycogen storage myopathy
- Hematomyelia
- Hepatoma
- Hereditary inclusion body myopathy
- Hereditary peripheral nervous disorder
- Herniated disk
- Herpes zoster
- Hexane
- Hip cancer
- Hiv
- Hookworm infestation
- Hypercortisolism
- Hyperthyroidism
- Hypertrophic neuropathy of dejerine-sottas
- Hypothyroidism
- Immobility
- Immobilized fractures
- Inclusion body myopathy
- Inclusion body myositis
- Incontinentia pigmenti
- Intercostal neuralgia
- Intestinal capillariasis
- Intramedullary astrocytoma
- Intramedullary ependymoma
- Ischemic palsy
- Jequier-kozlowski-skeletal dysplasia
- Joint disuse
- Joint inflammation
- Joint injuries
- Juvenile rheumatoid arthritis
- Kuskokwim disease
- Kwashiorkor
- Lambert-eaton myasthenic syndrome
- Landouzy-dejerine muscular dystrophy
- Legg-calve-perthes disease
- Leiner disease
- Leprosy
- Letterer-siwe disease
- Levine-critchley syndrome
- Lightwood-albright syndrome
- Limb-girdle muscular dystrophy type
- Lipidosis with triglyceride storage disease
- Lower motor neurone lesion
- Lumbar canal stenosis
- Lumbar spondylosis
- Lupine poisoning
- Madsam
- Malabsorption syndrome
- Malaria
- Malignancy
- Malnutrition
- Marasmus
- Marinesco-sjogren syndrome
- Mc leod neuroacanthocytosis syndrome
- Medications
- Meningovascular malformations
- Meniscal tear
- Mental retardation
- Metachromatic leukodystrophy
- Minicore disease
- Mitochondrial encephalomyopathy
- Mitochondrial myopathy
- Mitochondrial neurogastrointestinal encephalopathy syndrome
- Miyoshi myopathy
- Morse-rawnsley-sargent syndrome
- Motor neurone disease
- Motor neuropathy
- Multicentric osteolysis
- Multifocal motor neuropathy
- Multiminicore disease
- Multiple sclerosis
- Multiple system atrophy
- Muscle disuse
- Muscle injury
- Muscular dystrophy
- Muscular fibrosis
- Muscular phosphorylase kinase deficiency
- Myasthenia
- Myasthenic syndrome
- Mycobacterium kansasii
- Myopathy
- Myotonic dystrophy
- Nadh coq reductase
- Nemalin myopathy
- Nephrotic syndrome
- Nerve compression
- Nerve entrapment
- Nerve injury
- Neu-laxova syndrome
- Neurodegeneration
- Neuropathy
- Neurosyphilis
- Nodulosis-arthropathy-osteolysis syndrome
- Obal syndrome
- Oculopharyngeal dystrophy
- Old age
- Olivopontocerebellar atrophy i
- Osteoarthritis
- Osteogenesis imperfecta
- Palmoplantar keratoderma
- Pantothenate kinase-associated neurodegeneration
- Paralysis of limbs
- Parasitic infections
- Parkinson disease
- Parkinson's disease
- Parsonage turner syndrome
- Passos-bueno syndrome
- Penicillamine
- Pergolide
- Peripheral nerve trauma
- Peripheral neuritis
- Peripheral neuropathy
- Polio
- Polyarteritis nodosa
- Polymyositis
- Polyradiculoneuropathy
- Pontocerebellar hypoplasia
- Posterior column ataxia
- Post-polio syndrome
- Primary biliary cirrhosis
- Primary lateral sclerosis
- Primary muscle disease
- Progressive spinal muscular atrophy
- Prolapsed lumbar intervertebral disc
- Prolonged immobilization
- Prolonged steroid therapy
- Protein deficiency
- Proximal spinal muscular atrophy
- Radiculopathy
- Reflex sympathetic dystrophy syndrome
- Rheumatoid arthritis
- Rib tumor
- Richards-rundle syndrome
- Rud syndrome
- Salvioli syndrome
- Sandhoff disease
- Sarcoidosis
- Schistosomiasis
- Schwartz-jampel syndrome
- Scleroatonic muscular dystrophy
- Short chain acyl coa dehydrogenase deficiency
- Singleton-merten syndrome
- Small syndrome
- Soft tissue edema
- Soft tissue hemorrhage
- Spinal bulbar motor neuropathy
- Spinal cord injury
- Spinal cord lesion
- Spinal cord tumor
- Spinal muscular atrophy
- Spinal tumor
- Spinocerebellar ataxia
- Statins
- Steroid use
- Storm syndrome
- Stroke
- Subacute combined degeneration of the spinal cord
- Surgical ligation of major vessel
- Syphilitic amyotrophy
- Syringomyelia
- Tay sachs
- Thoracic outlet syndrome
- Thrombosis of great vessel
- Thyrocerebral-retinal syndrome
- Thyroid disease
- Thyroid dysfunction
- Thyrotoxicosis
- Tourniquet paralysis
- Toxoplasmosis
- Trichinosis
- Tropical sprue
- Troyer syndrome
- Tuberculosis
- Type iv glycogen storage disease
- Ulerythema ophryogenesis
- Undiagnosed diabetes mellitus
- Vacuolar myopathy
- Vascular disease
- Viral infections
- Volkmann's contracture
- Wasting syndrome
- Welander distal myopathy
- Wieacker syndrome
- Wieacker-wolff syndrome
- Wilson's disease
- Wohlwill-andrade syndrome
- X-linked mental retardation
Other muscles diseases, distinct from atrophy
During aging, there is a gradual decrease in the ability to maintain skeletal muscle function and mass. This condition is called "sarcopenia". The exact cause of sarcopenia is unknown, but it may be due to a combination of the gradual failure in the "satellite cells" which help to regenerate skeletal muscle fibers, and a decrease in sensitivity to or the availability of critical secreted growth factors which are necessary to maintain muscle mass and satellite cell survival.
In addition to the simple loss of muscle mass (atrophy), or the age-related decrease in muscle function (sarcopenia), there are other diseases which may be caused by structural defects in the muscle (muscular dystrophy), or by inflammatory reactions in the body directed against muscle (the myopathies).
Pathophysiology
Muscle atrophy occurs by a change in the normal balance between protein synthesis and protein degradation. During atrophy, there is a down-regulation of protein synthesis pathways, and an activation of protein breakdown pathways. The particular protein degradation pathway which seems to be responsible for much of the muscle loss seen in a muscle undergoing atrophy is the "ATP-dependent, ubiquitin/proteasome pathway. In this system, particular proteins are targeted for destruction by the ligation of at least four copies of a small peptide called ubiquitin onto a substrate protein. When a substrate is thus "poly-ubiquitinated", it is targeted for destruction by the proteasome. Particular enzymes in the ubiquitin/proteasome pathway allow ubiquitination to be directed to some proteins but not others - specificity is gained by coupling targeted proteins to an "E3 ubiquitin ligase". Each E3 ubiquitin ligase binds to a particular set of substrates, causing their ubiquitination.
Diagnostic Findings
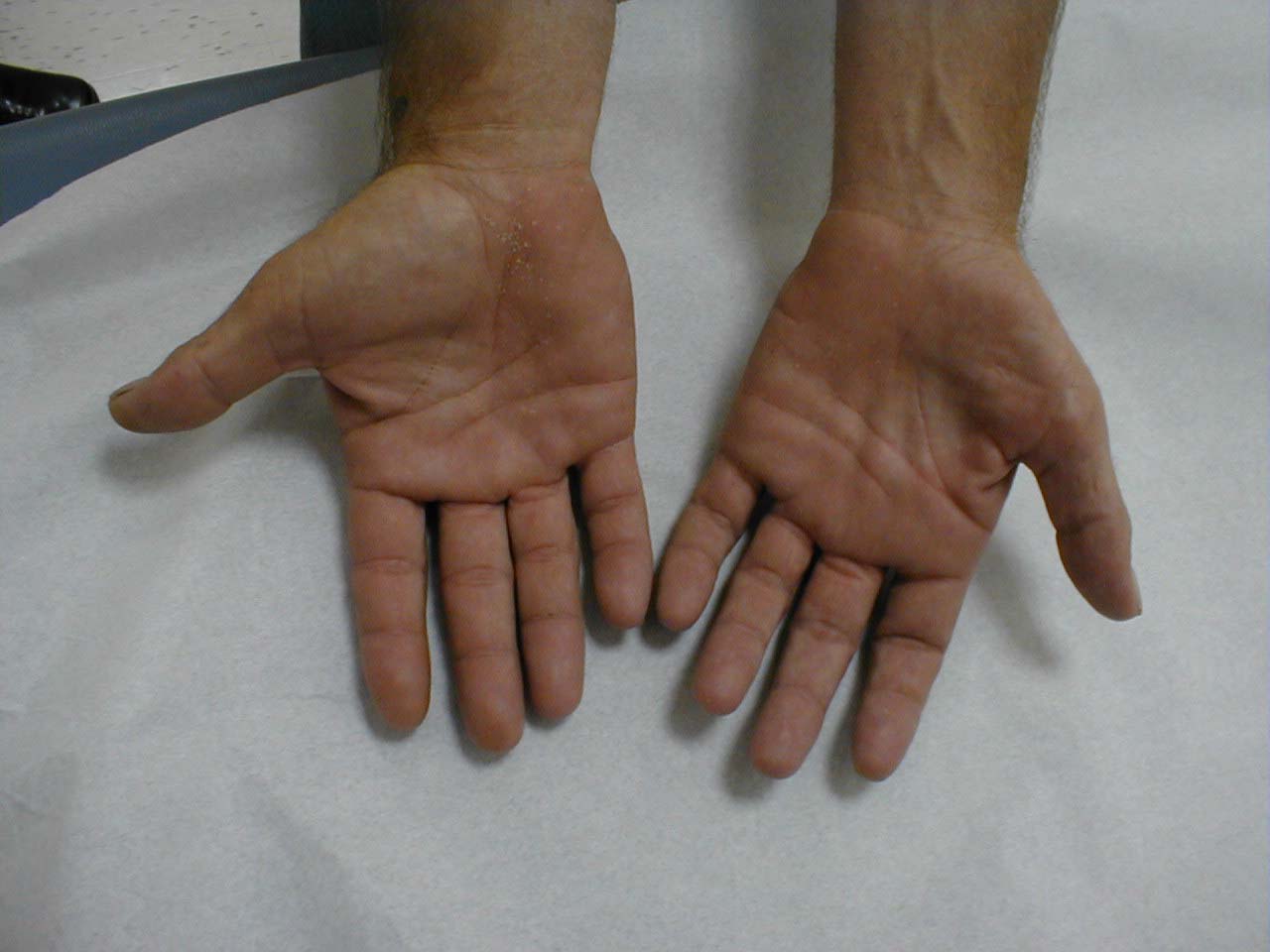
-
Muscle Wasting Left Hand: Atrophic flattening most prominently seen in the thenar and hypothenar muscles, resulting from generalized denervation.
Potential treatment
Muscle atrophy can be opposed by the signaling pathways which induce muscle hypertrophy, or an increase in muscle size. Therefore one way in which exercise induces an increase in muscle mass is to downregulate the pathways which have the opposite effect.
See also
- Muscle weakness
- Muscle dystrophy
External links
- Muscular+atrophy at the US National Library of Medicine Medical Subject Headings (MeSH)