COVID-19 physical examination
For COVID-19 frequently asked outpatient questions, click here
For COVID-19 frequently asked inpatient questions, click here
|
COVID-19 Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
COVID-19 physical examination On the Web |
|
American Roentgen Ray Society Images of COVID-19 physical examination |
|
Risk calculators and risk factors for COVID-19 physical examination |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Sabawoon Mirwais, M.B.B.S, M.D.[2]; Syed Hassan A. Kazmi BSc, MD [3]; Javaria Anwer M.D.[4]
Synonyms and keywords:COVID physical exam, SARS CoV2 physical exam, SARS CoV2 physical examination, COVID-19 physical findings.
Overview
COVID-19 is a rapidly evolving situation and a heterogenous disease entity. A suspected or confirmed CVOVID-19 patient can have as common finding as fever and as unique yet significant finding as anosmia. Although, the common physical examination findings among patients infected with coronavirus include fever, cough, and shortness of breath.[1] The patient may just have abdominal pain and tenderness on examination.[2] The general appearance of the patient infected with coronavirus-19 depends on the severity of the illness. High clinical suspicion and careful physical exam are they key to early diagnosis and treatment of COVID-19 infection.
The Cochrane Collaboration has reviewed both the History and Symptoms | Physical Examination[3].
Physical Examination
Physical exam of a suspected or confirmed case of COVID-19 patient should be conducted in a private room, preferably a negative pressure one. The examiner should have PPE that includes gloves, gowns or aprons, masks, or respirators covering the mouth and nose, goggles, and face shields.[4] Due to the risk of aerosol spread of the SARS-CoV-2 virus, CDC recommends that protective eyewear (such as goggles or a face shield) should cover the front and sides of the face with no gaps between glasses and the face.[5] If possible and the patient is in no respiratory distress, patient should wear a surgical mask.[6]
Appearance of the Patient
- General appearance of the patient infected with SARS-CoV-2 virus (cause of COVID-19) depends on the severity of the illness and the presence of infection associated complications involving different organ systems.
- Patients with mild disease may appear healthy.
- Patients will appear sick, lethargic, and short of breath in severe disease.
- Patient may appear dehydrated (decreased skin turgor and dry mucosa) due to increased respiratory rate, nausea and vomiting,
- Anxiety is an important accompanying factor with majority of patients visiting hospitals, provided the heterogeneous nature of the disease. A healthy patient may worry regarding contracting the infection while visiting the hospital or doctor's office.
- Cyanosis depicts severe hypoxemia and the need for supplemental oxygen.
Vital Signs
- Pulse:
- Heart rate: A normal heart rate is between 60 and 100 bpm with a few exceptions such as athletes. A healthy asymptomatic patient may have a normal heart rate but that does not rule out infection. Sinus tachycardia, the most common type of arrhythmia among COVID-19 patients can be due to fever, hypoxia, shock due to sepsis, and anxiety. Some pathologic causes of arrhythmias include ventricular tachyarrhythmia[7], atrial fibrillation (pulse rate 100 to 175 bpm) and atrial flutter (pulse rate 150 bpm).
- Rhythm: Sinus tachycardia has a regular rhythm. An irregular pulse due to a few pathologic arrhythmias can be due to atrial fibrillation and ventricular tachyarrhythmia and COVID-19-associated Guillain-Barre syndrome.
- Volume: A low volume pulse indicates dehydration and the potential need to rehydration therapy.
- Character: A fast but weak pulse depicts shock. A raised, full and bounding pulse can be observed due to fever or simply patient anxiety.
- Temperature:Fever (>100.4°F )[8] is a common temperature finding (observed in 89% patients) with rest of the patients being a febrile. Temperature of the patient can be in any range (102°F-99.5°F) reported.[9] Although body temperature is a good screening tool, afebrile patients have been confirmed to have COVID-19 infection. A recent non-peer reviewed case report describes acute hypothermia in a COVID-19 patient.(30.2°F).[10]
- Respiratory rate: Normal respiratory rate among adults is 12 to 16 breaths per minute. Tachypnea(> 30 breaths/min) among COVID-19 positive patient sis the response to lung inflammation or can be a sign of progressive respiratory failure and can be found in COVID-19-associated pneumonia, ARDS and COVID-19-associated Guillain-Barre syndrome. A respiratory rate of > 28-30 / min, or dyspnea, warrant the administration of oxygen by of 40% venturi mask. Oxygen saturation, respiratory rate, CXR and importantly dyspnea help determine the need for invasive mechanical ventilation.[11].
- Oxygen saturation: SpO2 < 93-94% warrants the administration of oxygen by of 40% venturi mask and marks severe disease. In younger individuals, the arterial oxygen saturation is more important than it appears. The deterioration of inflammatory lung injury is manifested by a decrease in oxygen saturation (< 93%) first, followed by dyspnea among younger individuals with no other comorbidities.[12]
- Blood pressure: Low blood pressure can be due to dehydration, septic shock, heart failure or pathologic arrhythmias associated with COVID-19. Hypertension is itself a risk for severe COVID-19 infection.[13]
Skin
- Skin examination of patients with COVID-19 includes the following lesions:
- Erythema multiforme-like[14] Further studies are required to evaluate exact etiology these lesions to be COVID-19, drug intake or any other conditions.
- Erythematous maculo-papular[15]: Acral eruption of erythemato‐violaceous papules and macules, with possible bullous evolution, or digital swelling can be observed.
- Urticarial[16][17]
- Chickenpox-like[16][18]
- Purpuric peri-flexural[19]
- Transient livedo reticularis[20]
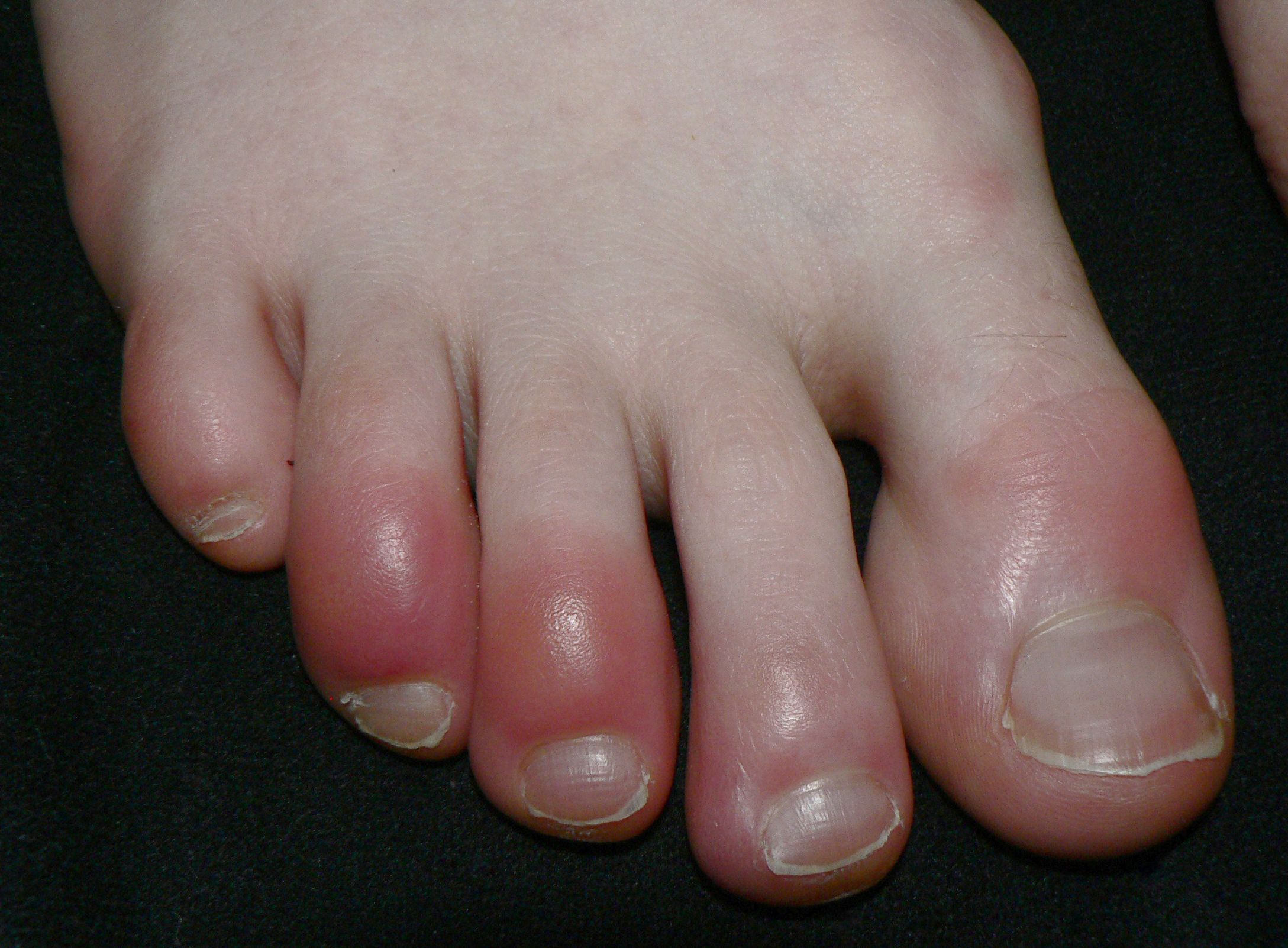
- Acro-ischemic[21]: The lesion constitutes finger or toe cyanosis, skin bullae and dry gangrene.
- Chilblain-like[22]:They constitute bilateral red-purple papules on the dorsum of the fingers and diffuse erythema on the subungual area of thumb. During the COVID-19 disease course, pseudo‐chilblain patterns may appear.[23]
HEENT
- Head exam: Patients with fluid retention due to COVID-19-associated acute kidney injury may have edema (especially peri-orbital) and swelling of face and extremities. Cervical lymphadenopathy can be present although very few cases have been reported.[24]
- Eye exam:
- Conjunctivitis: has been reported but there is no well established data regarding this manifestation.[25]
- Epiphora: Patients can have teary eyes due to conjunctivitis itself or foreign body sensation.[26]
- Papilledema can be due to increased ICP or cranial nerve palsy.
- Although there are no reports of blurred vision but visual acuity should be accessed.
- Ear exam: A case report of COVID-19 associated otitis media demonstartes hyperemia and bulging tympanic membrane among the patient. Audiometry and tympanometry can help investigate hearing sequelae.[27]
- Nasal exam: Runny nose and nasal congestion are relatively common physical exam findings.
- Throat exam: Throat congestion, Tonsil edema have been reported.[24]
Neck
- On inspection, a patient with severe hypoxia will be using accessory muscles for respiration visible on the neck exam. A direct sign of increased work of breathing is palpation of the sternomastoid and detecting the phasic contraction.[28]
- Jugular venous pressure:[29]
- High JVP or Jugular Venous Distension (JVD) can be a sign of COVID-19-associated heart failure or COVID-19-associated myocarditis.
- Low JVP: Demonstrates low CVP indication low intravascular volume. Among patients with COVID-19 associated ARDS, CVP guides the fluid management.
Lungs
| Lung examination findings in COVID-19 | |||
|---|---|---|---|
| Physical exam | Mild-moderate infection (Pneumonia)[30] | Severe infection (ARDS)[31] | |
| Inspection | Tachypnea
Maybe normal respiratory rate |
Dyspnea
Tachypnea [Respiratory rate (≥ 30 breaths/min) indicates severe disease] Increased work of breathing using accessory muscles lethargic and dehydrated patient | |
| Palpation | Increased vocal fremitus
Diminished chest expansion at the affected side |
Decreased vocal fremitus (accompanying pneumothorax) Diminished chest movements at the affected side | |
| Percussion | Dull percussion note | Tympanic note if pneumothorax accompanies | |
| Auscultation | Decreased breath sounds if pleural effusion accompanies
Bronchial breath sounds (click here to listen) |
Decreased breath sounds over a lung may indicate a pneumothorax or endotracheal tube down the right main bronchus Rales may or may not be present | |
Heart
- Pulse pressure: A narrow pulse pressure may indicate hypovolemic shock requiring fluid therapy or fulminant myocarditis.
- Palpation: The apical impulse may be displaced laterally if there is left ventricular dilation in COVID-19-associated myocarditis or COVID-19-associated heart failure. A parasternal heave may be observed depicting COVID-19-associated heart failure.
- Cardiac auscultation may demonstrate tachycardia or arrhythmias (irregular beat).
- S3 or asummation gallop especially in significant biventricular dysfunction, COVID-19-associated heart failure or COVID-19-associated cardiogenic shock
- Mitral or tricuspid murmurs (holosystolic murmurs) may also be noted in the presence of significant ventricular dilation leading to regurgitant flow across AV valves. Among COVID-19-associated heart failure and COVID-19-associated myocarditis.
- Pericardial friction rub and low intensity heart sounds may be evident if pericardium is involved causing pericarditis and effusion respectively.[32]
Abdomen
- Some patients with COVID-19 may report abdominal pain but abdominal exam findings to be positive is very rare.[33] Based on three case reports describing patients' atypical COVID-19 presenting complaints the following findings can be observed among patients:[34][2][35]
- Inspection: Slight abdominal distension on day 4 of admission in a single case presenting as acute pancreatitis.
- Palpation: One COVID-19 positive patient had abdominal tenderness and rebound tenderness at the right iliac fossa with no diagnostic proof of acute appendicitis. Direct epigastric and peri-umbilical tenderness is reported in only one case. The presence of hepatomegaly among patients with COVID-19-associated hepatic injury maybe a forethought of organomegaly.[36]
- Percussion: No abnormal findings have been reported.
- Auscultation: Hypo/hyperactive bowel sounds have not been reported.
Back
- Gait can be impaired and the patient will have flaccid paralysis among COVID-19-associated Guillain-Barre syndrome and COVID-19-associated polyneuritis cranialis.
Genitourinary
- There are no reports of genitourinary manifestations of COVID-19 but due to the association of SARS with orchitis due to autoimmune mechanisms, urologists recommend that genitourinary examination of patients infected with SARS-CoV-2 virus (case of COVID-19) is usually not be missed.[37]
Neuromuscular
- Mental status exam: Glasgow coma scale can gauge the conscious state of the patient. Confusion can be due to severe dehydration, electrolyte imbalances such as among COVID-19-associated acute kidney injury, COVID-19-associated encephalitis, COVID-19-associated meningitis or COVID-19-associated stroke. Moreover, a patient can be unconscious.
- Cranial Nerve exam: Any cranial nerve can be involved with physical exam findings such as:
- Cranial Nerve 1 or Olfactory nerve should be examined to evaluate for anosmia. Studies suggests that anosmia can be an important clue, helping the diagnosis of COVID-19 specially in the early stages.[38] According to a study published anosmia and aguesia could be strong predictors of COVID-19 infection.[39]
- Cranial nerve III: Ophthalmoparesis.[40]
- CN-VII: facial weakness ( frequent finding) in GBS. Other cranial nerves involved in the disease include CN- III, V, VI, IX, X and XII resulting in ptosis, facial droop, dysphagia and dysarthria and diplopia.[41]
- Sensory system exam: Absent withdrawal to painful stimuli is observed in encephalitis.[42] Hypesthesia associated with COVID has been reported.[43][44][45]
- Motor system exam:
- Muscle power and muscle tone: Paresis and atonia due to direct muscle injury is associated with COVID-19.[46] Bilateral ascending flaccid paralysis or quadriparesis is observed in COVID-19-associated Guillain-Barre syndrome.[44]
- Gait: Gait ataxia has also been reported among COVID-19 cases but is very rare.
- Reflexes: Deep tendon areflexia or hyporeflexia is observed in COVID-19-associated Guillain-Barre syndrome and COVID-19-associated Miller-Fischer syndrome. A study describing three patients with encephalitis reports absent corneal reflex, gag reflexes, oculocephalic reflex, diminished deep tendon reflexes and myoclonus affecting bilateral arms and legs.[42]
Extremities
- Patients with fluid retention due to COVID-19-associated acute kidney injury, COVID-19-associated heart failure, COVID-19-associated myocarditis or COVID-19-associated hepatic injury have pedal edema on examination.
- COVID-19 toes: As explained earlier, pseudo-chilblain patterns may appear on toes widely known as COVID toes. A patient presented with purple toes should be tested for COVID-19 virus infection.[23]
References
- ↑ Zhu, Jieyun; Ji, Pan; Pang, Jielong; Zhong, Zhimei; Li, Hongyuan; He, Cuiying; Zhang, Jianfeng; Zhao, Chunling (2020). "Clinical characteristics of 3062 COVID‐19 patients: A meta‐analysis". Journal of Medical Virology. doi:10.1002/jmv.25884. ISSN 0146-6615.
- ↑ 2.0 2.1 Hadi A, Werge M, Kristiansen KT, Pedersen UG, Karstensen JG, Novovic S, Gluud LL (June 2020). "Coronavirus Disease-19 (COVID-19) associated with severe acute pancreatitis: Case report on three family members". Pancreatology. 20 (4): 665–667. doi:10.1016/j.pan.2020.04.021. PMC 7199002 Check
|pmc=value (help). PMID 32387082 Check|pmid=value (help). - ↑ Struyf T, Deeks JJ, Dinnes J, Takwoingi Y, Davenport C, Leeflang MM; et al. (2021). "Signs and symptoms to determine if a patient presenting in primary care or hospital outpatient settings has COVID-19". Cochrane Database Syst Rev. 2: CD013665. doi:10.1002/14651858.CD013665.pub2. PMID 33620086 Check
|pmid=value (help). - ↑ "www.cdc.gov" (PDF).
- ↑ Guo T, Fan Y, Chen M, Wu X, Zhang L, He T; et al. (2020). "Cardiovascular Implications of Fatal Outcomes of Patients With Coronavirus Disease 2019 (COVID-19)". JAMA Cardiol. doi:10.1001/jamacardio.2020.1017. PMC 7101506 Check
|pmc=value (help). PMID 32219356 Check|pmid=value (help). - ↑ (PDF) https://www.cdc.gov/sars/about/fs-SARS.pdf. Missing or empty
|title=(help) - ↑ Guan, Wei-jie; Ni, Zheng-yi; Hu, Yu; Liang, Wen-hua; Ou, Chun-quan; He, Jian-xing; Liu, Lei; Shan, Hong; Lei, Chun-liang; Hui, David S.C.; Du, Bin; Li, Lan-juan; Zeng, Guang; Yuen, Kwok-Yung; Chen, Ru-chong; Tang, Chun-li; Wang, Tao; Chen, Ping-yan; Xiang, Jie; Li, Shi-yue; Wang, Jin-lin; Liang, Zi-jing; Peng, Yi-xiang; Wei, Li; Liu, Yong; Hu, Ya-hua; Peng, Peng; Wang, Jian-ming; Liu, Ji-yang; Chen, Zhong; Li, Gang; Zheng, Zhi-jian; Qiu, Shao-qin; Luo, Jie; Ye, Chang-jiang; Zhu, Shao-yong; Zhong, Nan-shan (2020). "Clinical Characteristics of Coronavirus Disease 2019 in China". New England Journal of Medicine. 382 (18): 1708–1720. doi:10.1056/NEJMoa2002032. ISSN 0028-4793.
- ↑ Allard, Nicolas; Maruani, Ari; Cret, Corina; Ameri, Alain (2020). "Acute hypothermia in Covid 19: A case report". eNeurologicalSci: 100248. doi:10.1016/j.ensci.2020.100248. ISSN 2405-6502.
- ↑ Tobin, Martin J. (2020). "Basing Respiratory Management of COVID-19 on Physiological Principles". American Journal of Respiratory and Critical Care Medicine. 201 (11): 1319–1320. doi:10.1164/rccm.202004-1076ED. ISSN 1073-449X.
- ↑ Cascella M, Rajnik M, Cuomo A, Dulebohn SC, Di Napoli R. PMID 32150360 Check
|pmid=value (help). Missing or empty|title=(help) - ↑ Jimenez-Cauhe J, Ortega-Quijano D, Carretero-Barrio I, Suarez-Valle A, Saceda-Corralo D, Moreno-Garcia Del Real C, Fernandez-Nieto D (May 2020). "Erythema multiforme-like eruption in patients with COVID-19 infection: clinical and histological findings". Clin. Exp. Dermatol. doi:10.1111/ced.14281. PMID 32385858 Check
|pmid=value (help). - ↑ Recalcati, S. (2020). "Cutaneous manifestations in COVID‐19: a first perspective". Journal of the European Academy of Dermatology and Venereology. 34 (5). doi:10.1111/jdv.16387. ISSN 0926-9959.
- ↑ 16.0 16.1 Recalcati, S. (2020). "Cutaneous manifestations in COVID‐19: a first perspective". Journal of the European Academy of Dermatology and Venereology. 34 (5). doi:10.1111/jdv.16387. ISSN 0926-9959.
- ↑ Fernandez-Nieto, D; Ortega-Quijano, D; Segurado-Miravalles, G; Pindado-Ortega, C; Prieto-Barrios, M; Jimenez-Cauhe, J (2020). "Comment on: Cutaneous manifestations in COVID-19: a first perspective. Safety concerns of clinical images and skin biopsies". Journal of the European Academy of Dermatology and Venereology. doi:10.1111/jdv.16470. ISSN 0926-9959.
- ↑ Tammaro, A.; Adebanjo, G.A.R.; Parisella, F.R.; Pezzuto, A.; Rello, J. (2020). "Cutaneous manifestations in COVID‐19: the experiences of Barcelona and Rome". Journal of the European Academy of Dermatology and Venereology. doi:10.1111/jdv.16530. ISSN 0926-9959.
- ↑ Jimenez-Cauhe, Juan; Ortega-Quijano, Daniel; Prieto-Barrios, Marta; Moreno-Arrones, Oscar M.; Fernandez-Nieto, Diego (2020). "Reply to "COVID-19 can present with a rash and be mistaken for dengue": Petechial rash in a patient with COVID-19 infection". Journal of the American Academy of Dermatology. doi:10.1016/j.jaad.2020.04.016. ISSN 0190-9622.
- ↑ Manalo, Iviensan F.; Smith, Molly K.; Cheeley, Justin; Jacobs, Randy (2020). "A dermatologic manifestation of COVID-19: Transient livedo reticularis". Journal of the American Academy of Dermatology. doi:10.1016/j.jaad.2020.04.018. ISSN 0190-9622.
- ↑ Fernandez-Nieto, D.; Jimenez-Cauhe, J.; Suarez-Valle, A.; Moreno-Arrones, O.M.; Saceda-Corralo, D.; Arana-Raja, A.; Ortega-Quijano, D. (2020). "Characterization of acute acro-ischemic lesions in non-hospitalized patients: a case series of 132 patients during the COVID-19 outbreak". Journal of the American Academy of Dermatology. doi:10.1016/j.jaad.2020.04.093. ISSN 0190-9622.
- ↑ Piccolo, V.; Neri, I.; Filippeschi, C.; Oranges, T.; Argenziano, G.; Battarra, V.C.; Berti, S.; Manunza, F.; Fortina, A.B.; Di Lernia, V.; Boccaletti, V.; De Bernardis, G.; Brunetti, B.; Mazzatenta, C.; Bassi, A. (2020). "Chilblain‐like lesions during COVID‐19 epidemic: a preliminary study on 63 patients". Journal of the European Academy of Dermatology and Venereology. doi:10.1111/jdv.16526. ISSN 0926-9959.
- ↑ 23.0 23.1 Galván Casas, C.; Català, A.; Carretero Hernández, G.; Rodríguez‐Jiménez, P.; Fernández‐Nieto, D.; Rodríguez‐Villa Lario, A.; Navarro Fernández, I.; Ruiz‐Villaverde, R.; Falkenhain‐López, D.; Llamas Velasco, M.; García‐Gavín, J.; Baniandrés, O.; González‐Cruz, C.; Morillas‐Lahuerta, V.; Cubiró, X.; Figueras Nart, I.; Selda‐Enriquez, G.; Romaní, J.; Fustà‐Novell, X.; Melian‐Olivera, A.; Roncero Riesco, M.; Burgos‐Blasco, P.; Sola Ortigosa, J.; Feito Rodriguez, M.; García‐Doval, I. (2020). "Classification of the cutaneous manifestations of
COVID
‐19: a rapid prospective nationwide consensus study in Spain with 375 cases". British Journal of Dermatology. doi:10.1111/bjd.19163. ISSN 0007-0963. line feed character in
|title=at position 50 (help) - ↑ 24.0 24.1 Krajewska J, Krajewski W, Zub K, Zatoński T (July 2020). "COVID-19 in otolaryngologist practice: a review of current knowledge". Eur Arch Otorhinolaryngol. 277 (7): 1885–1897. doi:10.1007/s00405-020-05968-y. PMC 7166003 Check
|pmc=value (help). PMID 32306118 Check|pmid=value (help). - ↑ Seah I, Agrawal R (April 2020). "Can the Coronavirus Disease 2019 (COVID-19) Affect the Eyes? A Review of Coronaviruses and Ocular Implications in Humans and Animals". Ocul. Immunol. Inflamm. 28 (3): 391–395. doi:10.1080/09273948.2020.1738501. PMC 7103678 Check
|pmc=value (help). PMID 32175797 Check|pmid=value (help). - ↑ Wu P, Duan F, Luo C, Liu Q, Qu X, Liang L, Wu K (March 2020). "Characteristics of Ocular Findings of Patients With Coronavirus Disease 2019 (COVID-19) in Hubei Province, China". JAMA Ophthalmol. doi:10.1001/jamaophthalmol.2020.1291. PMC 7110919 Check
|pmc=value (help). PMID 32232433 Check|pmid=value (help). - ↑ Fidan, Vural (2020). "New type of corona virus induced acute otitis media in adult". American Journal of Otolaryngology. 41 (3): 102487. doi:10.1016/j.amjoto.2020.102487. ISSN 0196-0709.
- ↑ Tobin, Martin J. (2019). "Why Physiology Is Critical to the Practice of Medicine". Clinics in Chest Medicine. 40 (2): 243–257. doi:10.1016/j.ccm.2019.02.012. ISSN 0272-5231.
- ↑ Semler MW, Wheeler AP, Thompson BT, Bernard GR, Wiedemann HP, Rice TW (April 2016). "Impact of Initial Central Venous Pressure on Outcomes of Conservative Versus Liberal Fluid Management in Acute Respiratory Distress Syndrome". Crit. Care Med. 44 (4): 782–9. doi:10.1097/CCM.0000000000001555. PMC 4792704. PMID 26741580.
- ↑ de Jongh TO, Thiadens HA (2011). "[Physical examination of the lungs in suspected pneumonia]". Ned Tijdschr Geneeskd (in Dutch; Flemish). 155: A2656. PMID 21329538.
- ↑ Gibson, Peter G; Qin, Ling; Puah, Ser Hon (2020). "COVID
‐19 acute respiratory distress syndrome (
ARDS
): clinical features and differences from typical pre‐
COVID
‐19
ARDS". Medical Journal of Australia. doi:10.5694/mja2.50674. ISSN 0025-729X. line feed character in
|title=at position 6 (help) - ↑ Siripanthong B, Nazarian S, Muser D, Deo R, Santangeli P, Khanji MY, Cooper LT, Chahal C (May 2020). "Recognizing COVID-19-related myocarditis: The possible pathophysiology and proposed guideline for diagnosis and management". Heart Rhythm. doi:10.1016/j.hrthm.2020.05.001. PMC 7199677 Check
|pmc=value (help). PMID 32387246 Check|pmid=value (help). Vancouver style error: initials (help) - ↑ Wong SH, Lui RN, Sung JJ (May 2020). "Covid-19 and the digestive system". J. Gastroenterol. Hepatol. 35 (5): 744–748. doi:10.1111/jgh.15047. PMID 32215956 Check
|pmid=value (help). - ↑ Poggiali E, Ramos PM, Bastoni D, Vercelli A, Magnacavallo A (2020). "Abdominal Pain: A Real Challenge in Novel COVID-19 Infection". Eur J Case Rep Intern Med. 7 (4): 001632. doi:10.12890/2020_001632. PMC 7162568 Check
|pmc=value (help). PMID 32309266 Check|pmid=value (help). - ↑ Abdalhadi A, Alkhatib M, Mismar AY, Awouda W, Albarqouni L (2020). "Can COVID 19 present like appendicitis?". IDCases. 21: e00860. doi:10.1016/j.idcr.2020.e00860. PMC 7265835 Check
|pmc=value (help). PMID 32523872 Check|pmid=value (help). - ↑ Li J, Fan JG (March 2020). "Characteristics and Mechanism of Liver Injury in 2019 Coronavirus Disease". J Clin Transl Hepatol. 8 (1): 13–17. doi:10.14218/JCTH.2020.00019. PMC 7132021 Check
|pmc=value (help). PMID 32274341 Check|pmid=value (help). - ↑ Wang, Shangqian; Zhou, Xiang; Zhang, Tongtong; Wang, Zengjun (2020). "The need for urogenital tract monitoring in COVID-19". Nature Reviews Urology. 17 (6): 314–315. doi:10.1038/s41585-020-0319-7. ISSN 1759-4812.
- ↑ Lee Y, Min P, Lee S, Kim SW (May 2020). "Prevalence and Duration of Acute Loss of Smell or Taste in COVID-19 Patients". J. Korean Med. Sci. 35 (18): e174. doi:10.3346/jkms.2020.35.e174. PMC 7211515 Check
|pmc=value (help). PMID 32383370 Check|pmid=value (help). - ↑ Menni, Cristina; Valdes, Ana M.; Freidin, Maxim B.; Sudre, Carole H.; Nguyen, Long H.; Drew, David A.; Ganesh, Sajaysurya; Varsavsky, Thomas; Cardoso, M. Jorge; El-Sayed Moustafa, Julia S.; Visconti, Alessia; Hysi, Pirro; Bowyer, Ruth C. E.; Mangino, Massimo; Falchi, Mario; Wolf, Jonathan; Ourselin, Sebastien; Chan, Andrew T.; Steves, Claire J.; Spector, Tim D. (2020). "Real-time tracking of self-reported symptoms to predict potential COVID-19". Nature Medicine. doi:10.1038/s41591-020-0916-2. ISSN 1078-8956.
- ↑ Dinkin M, Gao V, Kahan J, Bobker S, Simonetto M, Wechsler P, Harpe J, Greer C, Mints G, Salama G, Tsiouris AJ, Leifer D (May 2020). "COVID-19 presenting with ophthalmoparesis from cranial nerve palsy". Neurology. doi:10.1212/WNL.0000000000009700. PMID 32358218 Check
|pmid=value (help). - ↑ "Guillain-Barre Syndrome Clinical Presentation: History, Physical Examination".
- ↑ 42.0 42.1 Benameur, Karima; Agarwal, Ankita; Auld, Sara C.; Butters, Matthew P.; Webster, Andrew S.; Ozturk, Tugba; Howell, J. Christina; Bassit, Leda C.; Velasquez, Alvaro; Schinazi, Raymond F.; Mullins, Mark E.; Hu, William T. (2020). "Encephalopathy and Encephalitis Associated with Cerebrospinal Fluid Cytokine Alterations and Coronavirus Disease, Atlanta, Georgia, USA, 2020". Emerging Infectious Diseases. 26 (9). doi:10.3201/eid2609.202122. ISSN 1080-6040.
- ↑ "Cranial neuropathy soon after COVID-19 onset - American Academy of Ophthalmology".
- ↑ 44.0 44.1 Sedaghat Z, Karimi N (June 2020). "Guillain Barre syndrome associated with COVID-19 infection: A case report". J Clin Neurosci. 76: 233–235. doi:10.1016/j.jocn.2020.04.062. PMC 7158817 Check
|pmc=value (help). PMID 32312628 Check|pmid=value (help). - ↑ Gupta A, Paliwal VK, Garg RK (July 2020). "Is COVID-19-related Guillain-Barré syndrome different?". Brain Behav. Immun. 87: 177–178. doi:10.1016/j.bbi.2020.05.051. PMC 7239011 Check
|pmc=value (help). PMID 32445789 Check|pmid=value (help). - ↑ Sheraton M, Deo N, Kashyap R, Surani S (May 2020). "A Review of Neurological Complications of COVID-19". Cureus. 12 (5): e8192. doi:10.7759/cureus.8192. PMC 7243063 Check
|pmc=value (help). PMID 32455089 Check|pmid=value (help).