Obstetrics
|
WikiDoc Resources for Obstetrics |
|
Articles |
|---|
|
Most recent articles on Obstetrics |
|
Media |
|
Evidence Based Medicine |
|
Clinical Trials |
|
Ongoing Trials on Obstetrics at Clinical Trials.gov Clinical Trials on Obstetrics at Google
|
|
Guidelines / Policies / Govt |
|
US National Guidelines Clearinghouse on Obstetrics
|
|
Books |
|
News |
|
Commentary |
|
Definitions |
|
Patient Resources / Community |
|
Patient resources on Obstetrics Discussion groups on Obstetrics Patient Handouts on Obstetrics Directions to Hospitals Treating Obstetrics Risk calculators and risk factors for Obstetrics
|
|
Healthcare Provider Resources |
|
Causes & Risk Factors for Obstetrics |
|
Continuing Medical Education (CME) |
|
International |
|
|
|
Business |
|
Experimental / Informatics |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]
Overview
Obstetrics (from the Latin obstare, "to stand by") is the surgical specialty dealing with the care of a woman and her offspring during pregnancy, childbirth and the puerperium (the period shortly after birth). Midwifery is the equivalent non-surgical specialty. Most obstetricians are also gynaecologists. See Obstetrics and gynaecology.
The average gestational period for humans is 40 weeks by gestational age and 38 weeks by fertilization age. This is divided into three trimesters.
Antenatal care
In obstetric practice, an obstetrician or midwife sees a pregnant woman on a regular basis to check the progress of the pregnancy, to verify the absence of ex-novo disease, to monitor the state of preexisting disease and its possible effect on the ongoing pregnancy. A woman's schedule of antenatal appointment varies according to the presence of risk factors, such as diabetes, and local resources.
Some of the clinically and statistically more important risk factors that must be systematically excluded, especially in advancing pregnancy, are pre-eclampsia, abnormal placentation, abnormal fetal presentation and Intrauterine Growth Retardation.
For example, to identify pre-eclampsia, blood-pressure and albuminuria (level of urine protein) are checked at every opportunity.
Placenta praevia must be excluded (PP = low lying placenta that, at least partially, obstructs the birth canal and therefore warrants elective caesarean delivery); this can only be achieved with the use of an ultrasound scan.
In late pregnancy fetal presentation must be established: cepfalic presentation (head first) is the norm but the fetus may present feet-first or buttocks-first (breech), side-on (transverse), or at an angle (oblique presentation).
Intrauterine Growth Retardation is a general designation, where the fetus is smaller than expected when compared to its gestational age (in this case fetal growth parameters show a tendency to drop off from the 50th percentile eventually falling below the 10th percentile, when plotted on a fetal growth chart). Causes can be intrinsic (to the fetus) or extrinsic (maternal or placental problems).
Signs

Trimesters
First trimester: elevated β-hCG (human chorionic gonadotrophin) of up to 100,000 mIU/mL by 10 weeks GA is thought to contribute to morning sickness, fatigue, mood swings and food cravings. The symptoms can last through 12 to 16 weeks of gestation.
Second trimester: The abdomen shows an obvious swelling arising from the pelvis, starting the "obvious phase" of pregnancy. Hyperpigmentation, including linea nigra, may appear.
Third trimester: The mother may experience backaches due to increased strain. Typically, the curvature of the spine is changed as pregnancy evolves in order to counteract the change in weight distribution. The mother may also suffer mild urinary incontinence due to pressure on the bladder by the pregnant uterus, as well as heartburn(due to compression of the stomach).
Overall
- Bluish discoloration of vagina and cervix (Chadwick's sign)
- Softening and cyanosis of cervix after 4 weeks (Goodell's sign)
- Softening of uterus after 6 weeks (Hegar's or Ladin's sign)
- Breast swelling and tenderness
- Linea nigra from umbilicus to pubis
- Telangiectasias
- Palmar erythema
- Amenorrhea
- Nausea and vomiting
- Breast pain
- Fetal movement
- Sciatica (Pain caused by compression of the sciatic nerve)
Maternal physiology
During pregnancy, the woman undergoes many physiological changes, which are entirely normal, including cardiovascular, hematologic, metabolic, renal and respiratory changes that become very important in the event of complications.
Cardiovascular
The woman is the sole provider of nourishment for the embryo and later, the fetus, and so her plasma and blood volume slowly increase by 40-50% over the course of the pregnancy to accommodate the changes. This results in overall vasodilation, an increase in heart rate (15 beats/min more than usual), stroke volume, and cardiac output. Cardiac output increases by about 50%, mostly during the first trimester. The systemic vascular resistance also drops due to the smooth muscle relaxation caused by elevated progesterone, leading to a fall in blood pressure. Diastolic blood pressure consequently decreases between 12-26 weeks, and increases again to prepregnancy levels by 36 weeks. If the blood pressure remains abnormal beyond 36 weeks, the woman should be investigated for pre-eclampsia, a condition that precedes eclampsia.
Hematology
- The plasma volume increases by 50% and the red blood cell volume increases only by 20-30%.
- Consequently, the hematocrit decreases.
- White blood cell count increases and may peak at over 20 mil/mL in stressful conditions.
- Decrease in platelet concentration to a minimal normal values of 100-150 mil/mL
- The pregnant woman also becomes hypercoagulable due to increased liver production of coagulation factors, mainly fibrinogen and factor VIII.
Metabolism
During pregnancy, both protein metabolism and carbohydrate metabolism are affected. One kilogram of extra protein is deposited, with half going to the fetus and placenta, and another half going to uterine contractile proteins, breast glandular tissue, plasma protein, and hemoglobin.
Nutrition
- Increased caloric requirement by 300 kcal/day
- Gain of 20 to 30 lb (10 to 15 kg)
- Increased protein requirement to 70 or 75 g/day
- Increased folate requirement from 0.4 to 0.8 mg/day (important in preventing neural tube defects)
All patients are advised to take prenatal vitamins to compensate for the increased nutritional requirements. The use of Omega 3 fatty acids supports mental and visual development of infants.[1] Choline supplementation of research mammals supports mental development that lasts throughout life.[2]
Gastrointestinal
- nausea and vomiting ("morning sickness") may be due to elevated Beta-hCG, which should resolve by 14 to 16 weeks
- prolonged gastric empty time
- decreased gastroesophageal sphincter tone, which can lead to acid reflux
- decreased colonic motility, which leads to increased water absorption and constipation
Renal
- Increase in kidney and ureter size
- Increased glomerular filtration rate (GFR) by 50%, which subsides around 20 weeks postpartum
- Decreased BUN (blood urea nitrogen) and creatinine, and glucosuria (due to saturated tubular reabsorption)
- Persistent glucosuria can suggest gestational diabetes
- Decreased BUN (blood urea nitrogen) and creatinine, and glucosuria (due to saturated tubular reabsorption)
- Increased renin-angiotensin system, causing increased aldosterone levels
- Plasma sodium does not change because this is offset by the increase in GFR
Pulmonary
- Increased tidal volume (30-40%)
- Decreased total lung capacity (TLC) by 5% due to elevation of diaphragm from uteral compression
- Decreased expiratory reserve volume
- Increased minute ventilation (30-40%) which causes a decrease in PaCO2 and a compensated respiratory alkalosis
All of these changes can contribute to the dyspnea (shortness of breath) that a pregnant woman may experience.
Endocrine
- Increased estrogen, which is mainly produced in the placenta
- Fetal well being is associated with maternal estrogen levels
- Causes an increase in thyroxine-binding globulin (TBG)
- Increased human chorionic gonadotropin (β-hCG), which is produced by the placenta. This maintains progesterone production by the corpus luteum
- Human placental lactogen (hPL) is produced by the placenta and ensures nutrient supply to the fetus. It also causes lipolysis and is an insulin antagonist, which is a diabetogenic effect.
- Increased progesterone production, first by corpus luteum and later by the placenta. Its main course of action is to relax smooth muscle.
- Increased prolactin
- Increased alkaline phosphatase
Musculoskeleton and dermatology
- Lower back pain due to a shift in gravity
- Increased estrogen can cause spider angiomata and palmar erythema
- Increase melanocyte stimulating hormone (MSH) can cause hyperpigmentation of nipples, umbilicus, abdominal midline (linea nigra), perineum, and face (melasma or chloasma)
Others
- Edema, or swelling, of the feet is common during pregnancy, partly because the enlarging uterus compresses veins and lymphatic drainage from the legs.
Prenatal care
Prenatal care is important in screening for various complications of pregnancy. This includes routine office visits with physical exams and routine lab tests:
First trimester
- complete blood count (CBC)
- blood type (blood transfusion may be needed in an emergency)
- general antibody screen (indirect Coombs test) for HDN
- Rh D negative antenatal patients should receive RhoGam at 28 weeks to prevent Rh disease.
- Rapid plasma reagent (RPR) which screens for syphilis
- Rubella antibody screen
- Hepatitis B surface antigen
- Gonorrhea and Chlamydia culture
- PPD for tuberculosis
- Pap smear
- Urinalysis and culture
- HIV screen
- Group B Streptococcus screen -- will receive IV penicillin if positive (if mother is allergic, alternative therapies include IV clindamycin or IV vancomycin)
Second trimester
- MSAFP/triple screen (maternal serum alpha-fetoprotein) - elevation correlated with neural tube defects and decrease correlated with Down's syndrome
- ultrasound
- amniocentesis in older patients
Third trimester
- hematocrit (if low, mother will receive iron supplementation)
- Glucose loading test (OGTT, GLT, GTT) - screens for gestational diabetes; if > 140 mg/dL, a glucose tolerance test (GTT) is administered; a fasting glucose > 105 mg/dL suggests gestational diabetes.
Complications
See Complications of pregnancy
Fetal assessments
- Common
- ultrasound is used for many functions:
- Dating the gestational age of a pregnancy, most accurate in first trimester
- Detecting fetal anomalies in the second trimester
- biophysical profiles (BPP)
- Blood flow velocity in umbilical cord -- decrease/absence/reversal or diastolic blood flow in the umbilical artery is worrisome.
- Congenital anomalies can be diagnosed with second trimester ultrasound
- Fetal karyotype for the screening of genetic diseases can be obtained via amniocentesis or chorionic villus sampling (CVS)
- Uncommon
- Fetal hematocrit for the assessment of fetal anemia, Rh isoimmunization, or hydrops can be determined by percutaneous umbilical blood sampling (PUBS) which is done by placing a needle through the abdomen into the uterus and taking a portion of the umbilical cord.
- Fetal lung maturity is associated with how much surfactant the fetus is producing. Reduced production of surfactant indicates decreased lung maturity and is a high risk factor for neonatal respiratory distress syndrome (NRDS). Typically a lecithin:sphingomyelin ratio greater than 1.5 is associated with increased lung maturity.
- Nonstress test (NST) for fetal heart rate
- Oxytocin challenge test
Induction
Reasons to induce include:
- pre-eclampsia
- IUGR
- diabetes
- other general medical condition, such as renal disease
- "postdates" - the pregnancy has lasted longer than 41 weeks after the last menstrual period
Induction may occur any time after 34 weeks of gestation if the risk to the fetus or mother is greater than the risk of delivering a premature fetus regardless of lung maturity.
If a woman does not eventually labour by 41-42 weeks, induction may be performed, as the placenta may become unstable after this date.
Induction may be achieved via several methods:
- pessary of Prostin cream, prostaglandin E2
- iv. or oral administration of misoprostol
- cervical insertion of a 30-mL Foley catheter
- rupturing the amniotic membranes
- intravenous infusion of synthetic oxytocin (Pitocin or Syntocinon)
Labor
During labor itself, the obstetrician may be called on to do a number of things:
- monitor the progress of labor, by reviewing the nursing chart, performing vaginal examination, and assessing the trace produced by a fetal monitoring device (the cardiotocograph)
- accelerate the progress of labor by infusion of the hormone oxytocin
- provide pain relief, either by nitrous oxide (nowadays uncommon, at least in the U.S.), opiates, or by epidural anesthesia done by anaethestists, an anesthesiologist, or a nurse anesthetist.
- surgically assisting labor, by forceps or the Ventouse (a suction cap applied to the fetus' head)
- Caesarean section, if vaginal delivery is decided against or appears too difficult. Caesarean section can either be elective, that is, arranged before labor, or decided during labor as an alternative to hours of waiting. True "emergency" Cesarean sections (where minutes count) are a rarity.
Antenatal
During the time immediately after birth both baby as well as mother are hormonally cued to bond, the mother through the release of oxytocin a hormone also released with breastfeeding.
Emergencies in obstetrics
Two main emergencies are ectopic pregnancy and (pre)eclampsia.
- Ectopic pregnancy is when an embryo implants in the Fallopian tube or (rarely) on the ovary or inside the peritoneal cavity. This may cause massive internal bleeding.
- Pre-eclampsia is a disease which is defined by a combination of signs and symptoms that are related to maternal hypertension. The cause is unknown, and markers are being sought to predict its development from the earlist stages of pregnancy.
Some unknown factors cause vascular damage in the [endothelium], causing hypertension and proteinuria. If severe, it progresses to fulminant pre-eclampsia, with headaches and visual disturbances. This is a prelude to eclampsia, where a convulsion occurs, which can be fatal.
Imaging, monitoring and care
In present society, medical science has developed a number of procedures to monitor pregnancy.
Antenatal record
On the first visit to her obstetrician or midwife, the pregnant woman is asked to carry out the antenatal record, which constitutes a medical history and physical examination.
On subsequent visits, the gestational age (GA) is rechecked with each visit.
Symphysis-fundal height (SFH; in cm) should equal gestational age after 20 weeks of gestation, and the fetal growth should be plotted on a curve during the antenatal visits.
The fetus is palpated by the midwife or obstetrician using Leopold maneuver to determine the position of the baby. Blood pressure should also be monitored, and may be up to 140/90 in normal pregnancies. High blood pressure indicates hypertension and possibly pre-eclampsia, if severe swelling (edema) and spilled protein in the urine are also present.
Fetal screening is also used to help assess the viability of the fetus, as well as congenital problems. Genetic counseling is often offered for families who may be at an increased risk to have a child with a genetic condition.
Amniocentesis at around the 20th week is sometimes done for women 35 or older to check for Down's Syndrome and other chromosome abnormalities in the fetus.
Even earlier than amniocentesis is performed, the mother may undergo the triple test, nuchal screening, nasal bone, alpha-fetoprotein screening and Chorionic villus sampling, also to check for disorders such as Down Syndrome. Amniocentesis is a prenatal genetic screening of the fetus, which involves inserting a needle through the mother's abdominal wall and uterine wall, to extract fetal DNA from the amniotic fluid. There is a risk of miscarriage and fetal injury with amniocentesis because it involves penetrating the uterus with the baby still in utero.
Imaging
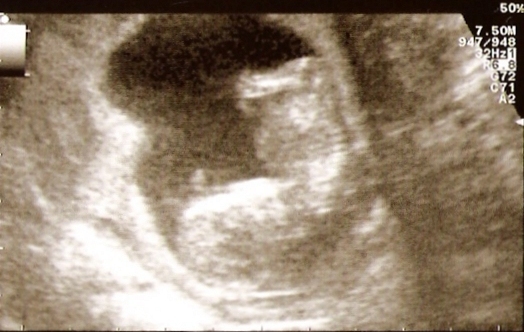
Imaging is another important way to monitor a pregnancy. The mother and fetus are also usually imaged in the first trimester of pregnancy. This is done to predict problems with the mother; confirm that a pregnancy is present inside the uterus; guess the gestational age; determine the number of fetuses and placentae; evaluate for an ectopic pregnancy and first trimester bleeding; and assess for early signs of anomalies.
X-rays and computerized tomography (CT) are not used, especially in the first trimester, due to the ionizing radiation, which has teratogenic effects on the fetus. Instead, ultrasound is the imaging method of choice in the first trimester and throughout the pregnancy, because it emits no radiation, is portable, and allows for realtime imaging. Ultrasound imaging may be done at any time throughout the pregnancy, but usually happens at the 12th week (dating scan) and the 20th week (detailed scan).
A normal gestation would reveal a gestational sac, yolk sac, and fetal pole. The gestational age can be assessed by evaluating the mean gestation sac diameter (MGD) before week 6, and the crown-rump length after week 6. Multiple gestation is evaluated by the number of placentae and amniotic sacs present.
Pregnancy has different cultural aspects related to the perception of the body, the relationship with partner and to the meaning of the event.
Terms and definitions
- embryo - conceptus between time of fertilization to 10 weeks of gestation
- fetus - from 10 weeks of gestation to time of birth
- infant - time of birth to 1 year of age
- gestational age - time from last menstrual period (LMP) up to present
- first trimester - up to 14 weeks of gestation
- second trimester - 14 to 28 weeks of gestation
- third trimester - 28 weeks to delivery
- viability - minimum age for fetus survival, ca. third trimester
- previable infant - delivered prior to 24 weeks
- preterm infant - delivered between 24-37 weeks
- term infant - delivered between 37-42 weeks
- gravidity (G) - number of times a woman has been pregnant
- parity (P) - number of pregnancies with a birth beyond 20 weeks GA or an infant weighing more than 500 g
- Ga Pw-x-y-z - a = number of pregnancies, w = number of term births, x = number of preterm births, y = number of abortions (spontaneous or therapeutic), z = number of living children; for example, G4P1-2-1-3 means the woman had a total of 4 pregnancies, of which 1 is of term, 2 are preterm, 1 miscarriage or therapeutic abortion, and 3 total living children (1 term + 2 preterm).
See also
- List of obstetric topics
- Gynecology
- Home birth
- Maternal health
- Midwifery
- Obstetric ultrasonography
- Puerperium
References
- ↑ "Omega-3 least known of pregnancy "Big 3"". Retrieved 2008-01-01.
- ↑ Tees RC, Mohammadi E (1999). <226::AID-DEV7>3.0.CO;2-H "The effects of neonatal choline dietary supplementation on adult spatial and configural learning and memory in rats". Dev Psychobiol. 35 (3): 226–40. PMID 10531535.
Further reading
- J Lane (July 1987). "A provincial surgeon and his obstetric practice: Thomas W. Jones of Henley-in-Arden, 1764–1846". Medical History. 31 (3): 333&ndash, 348.
Template:Obstetrical procedures Template:Urogenital surgical and other procedures
bn:ধাত্রীবিদ্যা bg:Акушерство da:Obstetrik de:Geburtshilfe el:Μαιευτική ga:Cnáimhseachas id:Obstetrik ia:Obstetricia it:Ostetricia ne:प्रसवशास्त्र nl:Verloskunde qu:Wachachiq sv:Obstetrik uk:Акушерство