COVID-19-associated arrhythmia and conduction system disease
For COVID-19 frequently asked inpatient questions, click here
For COVID-19 frequently asked outpatient questions, click here
|
COVID-19 Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
COVID-19-associated arrhythmia and conduction system disease On the Web |
|
American Roentgen Ray Society Images of COVID-19-associated arrhythmia and conduction system disease |
|
FDA on COVID-19-associated arrhythmia and conduction system disease |
|
CDC on COVID-19-associated arrhythmia and conduction system disease |
|
COVID-19-associated arrhythmia and conduction system disease in the news |
|
Blogs on COVID-19-associated arrhythmia and conduction system disease |
|
Risk calculators and risk factors for COVID-19-associated arrhythmia and conduction system disease |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1] Associate Editor(s)-in-Chief: Tayyaba Ali, M.D.[2]
Overview
Cardiac rhythm problems are increasingly recognized as a clinical manifestation of COVID-19. There is also anecdotal evidence of sudden cardiac death among COVID-19 patients. According to a study, 51 of 85 fatal cases of COVID-19 from Wuhan developed an arrhythmia, and 2 patients died of malignant arrhythmia.
Historical Perspective
- Diseases of heart and lung are the most common causes of COVID-19-related death.[1]
- Cardiac rhythm problems are increasingly recognized as a clinical manifestation of COVID-19.[2]
- There is also anecdotal evidence of sudden cardiac death among COVID-19 patients.[3] According to a study, 51 of 85 fatal cases of COVID-19 from Wuhan developed an arrhythmia, and 2 patients died of malignant arrhythmia.[4]
Classification
- COVID-19-associated arrhythmia may be classified into two subtypes/groups:
-
- COVID-19 patients with inherited arrhythmia syndromes, including long and short QT syndrome, Brugada syndrome, and catecholaminergic polymorphic ventricular tachycardia, are believed to be more liable to pro-arrhythmic consequences of SARS-CoV-2 which include stress, fever, use of antiviral medications and electrolyte disturbance.[5]
Pathophysiology
- Respiratory disease is the chief target of Coronavirus disease 2019 (COVID-19). One-third of patients with the severe disease also reported other symptoms including arrhythmia. According to a study done in Wuhan, China, 16.7% of hospitalized and 44.4% of ICU patients with COVID-19 had arrhythmias.[6]
- Severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) utilizes S-spike to bind to angiotensin-converting enzyme 2 (ACE2) receptors to enter the cells.
- Type 1 and type 2 pneumocytes exhibit ACE 2 receptors in the lung. Studies report that coronary endothelial cells in the heart and intrarenal endothelial cells and renal tubular epithelial cells in the kidney exhibit ACE2. ACE2 is an inverse regulator of the renin-angiotensin system.[7]
- The interaction between SARS-CoV-2 and ACE2 can bring about changes in ACE2 pathways prompting intense injury to the lung, heart, and endothelial cells. Hypoxia and electrolyte abnormalities that are common in the acute phase of severe COVID-19 can potentiate cardiac arrhythmias.
- Binding of SARS-CoV-2 to ACE2 receptors can result in hypokalemia which causes various types of arrhythmia.
- Elevated levels of cytokines as a result of the systemic inflammatory response of the severe Coronavirus disease 2019 (COVID-19) can cause injury to multiple organs, including cardiac myocytes.[8]In COVID-19 patients, excessive ranges of circulating cytokines, especially interleukin (IL)-6 is related to in-hospital death.[9]
- As a result of cytokine storm triggered by Sars-CoV-2 that includes IL-6, tumor necrosis factor (TNF) α, and IL-1, duration of ventricular action potential can be prolonged. Studies suggest that cytokine storm can modulate the function of cardiomyocyte ion channels such as Na+, K+ and Ca+ channels (inflammatory cardiac channelopathies).[10]
- According to the data based on studies on previous Severe acute respiratory syndrome (SARS) and the Middle East respiratory syndrome (MERS) epidemic and the ongoing COVID-19 outbreak, multiple mechanisms have been suggested for cardiac damage.[11]
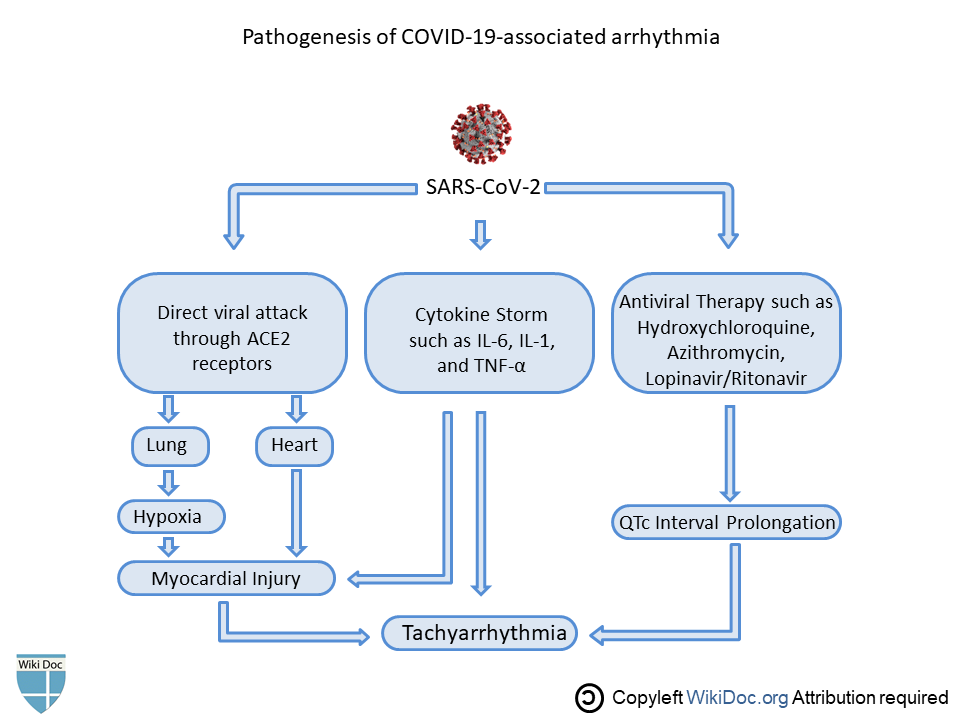
Clinical Features
Epidemiology and Demographics
- According to the available data on COVID-19-associated arrhythmia, the prevalence of arrhythmias and conduction system disease in patients with COVID-19 varies from population to population. The incidence of COVID-19-associated arrhythmia and conduction system disease in asymptomatic, mildly ill, critically ill, and recovered patients is not known.[3]
- According to a cohort of 137 COVID-19 patients from Hubei province, 10 patients were reported to have palpitations as one of the earliest symptoms.[12]
- In a cohort of 138 COVID-19 patients from Wuhan, arrhythmias were observed in 17 percent of hospitalized patients because of COVID-19-related pneumonia, and in 44 percent of patients admitted to an intensive care unit.[2]
Age
- There is not much data available to delineate the age group of COVID-19 patients prone to develop arrhythmia.
Gender
- There is not much data available to delineate the gender of COVID-19 patients prone to develop arrhythmia.
Race
- There is not enough data on racial predilection for COVID-19-associated arrhythmia.
Risk Factors
- Common risk factors in the development of COVID-19-associated arrhythmia are:
- Patients who present with other cardiovascular complications in the setting of COVID-19 infection, such as myocardial injury or myocardial ischemia.[9]
- Patients with hypoxia, shock (septic or cardiogenic), or evidence of widespread systemic inflammation.[13]
- Patients with electrolyte disturbances (eg, hypokalemia).[14]
- Patients who are receiving QT-prolonging therapies and who may develop polymorphic ventricular tachycardia (VT).[13]
- Patients with fever, which can unmask cases of cardiac channelopathies such as Brugada syndrome and long QT syndrome.[15][16]
Natural History, Complications and Prognosis
- Cardiac arrhythmia is considered as one of the earliest manifestations of COVID-19.
- Prognosis is generally poor in patients with COVID-19-associated arrhythmia and conduction system disease. According to the data available, the Arrhythmia rate is more frequent in Intensive care unit (ICU) patients.[6]
- To browse COVID-19 history, complications, and prognosis, Click here.
Diagnosis
Symptoms
Arrhythmia or conduction system disease is the nonspecific clinical presentation of COVID-19. Patients may be tachycardic (with or without palpitations) in the setting of other COVID-19-related symptoms (eg, fever, shortness of breath, pain, etc).
- Palpitations: According to a study done in Hubei province,palpitations were reported as a presenting symptom by 7.3 percent of patients.[12][9]
- Prolong QT Interval: According to a multicenter study done in New York that involved 4250 COVID-19 patients, 260 patients (6.1 percent) had corrected QT interval (QTc) >500 milliseconds at the time of admittance. However, in another study that involved 84 patients who got hydroxychloroquine and azithromycin, the baseline QTc interval was 435 milliseconds before receiving these medications.[17][18]
- Atrial Arrhythmia: According to a study, among 393 patients with COVID-19, atrial arrhythmias were more common among patients requiring invasive mechanical ventilation than noninvasive mechanical ventilation (17.7 versus 1.9 percent).[19]
- Ventricular Arrhythmia: According to a study done in Wuhan, China. among 187 hospitalized patients with COVID-19, 11 patients (5.9 percent) developed ventricular tachyarrhythmias.[20]
- Cardiac Arrest: According to a Lombardia Cardiac Arrest Registry (Lombardia CARe) of the region Lombardia in Italy. Out of 9806 cases of COVID-19, 362 cases of out-of-hospital cardiac arrest were reported during the study time frame in 2020. During a similar period in 2019, 229 cases of out-of-hospital cardiac arrest were reported, which means an increment of 58% was observed in 2020 among COVID-19 patients. According to the records from a tertiary care hospital in Wuhan. Out of 761 patients with severe COVID-19, 151 patients developed in-hospital cardiac arrest. 136 patients received resuscitation. Out of 136 patients, 119 patients had a respiratory cause. 10 patients had a cardiac cause. 7 patients had other causes. Ventricular fibrillation or pulseless ventricular tachycardia was observed in 8 patients (5.9%), Pulseless electrical activity in 6 patients (4.4%), and asystole in 122 COVID-19 patients (89.7%).[21][22]
Diagnostic Testing
- ECG: Most patients with the severe COVID-19, and especially patients who receive QT-prolonging medications, should have a baseline electrocardiogram (ECG) performed at the time of admission to the hospital.The best technique to get the QT interval is with a 12-lead electrocardiogram (ECG). However, to scale back exposure to hospital workers, this could not perpetually be possible. A single-lead ECG might underestimate the QT interval, and there ought to be an effort to use a multiple-lead telemetry system to observe the QT interval.[23][24]
- Transthoracic echocardiography: Transthoracic echocardiography is recommended for an inpatient with heart failure, arrhythmia, ECG changes, or newly diagnosed cardiomegaly on chest x-ray or CT-chest.[25]
Physical Examination
- Patients with COVID-19-associated arrhythmia and conduction system disease on cardiac auscultation reveal tachycardia or arrhythmias (irregular beat).
- Sinus tachycardia, the most common type of arrhythmia in COVID-19 patients can be due to fever, hypoxia, shock due to sepsis, and anxiety. Some pathologic causes of arrhythmias include ventricular tachyarrhythmia, atrial fibrillation (pulse rate 100 to 175 bpm) and atrial flutter (pulse rate 150 bpm).[26]
Laboratory Findings
- There are no specific laboratory findings associated with COVID-19-associated arrhythmia.
- COVID-19 patients with elevated troponin T experienced higher risk of ventricular arrhythmias (17.3% in high troponin T group versus 1.5% in normal troponin T group, P < 0.001).[5]
Imaging Findings
- There are no imaging study findings associated with COVID-19-associated arrhythmia.
Other Diagnostic Studies
- Myocardial biomarkers ought to be assessed in all patients with COVID‐19.
- We ought to consider that myocardial injury may bring about atrial or ventricular fibrosis, the substrate for resulting cardiovascular arrhythmias.
- COVID-19 patients with evidence of myocardial injury should undergo cardiac magnetic resonance to assess the extent of myocardial scar.[27]
Treatment
Medical Therapy
- Polymorphic Ventricular Tachycardia (torsades de pointes): All patients with torsades de pointes (TdP) should be determined if they are hemodynamically stable or unstable through immediate evaluation of the symptoms, vital signs, and level of consciousness.[28]
- Unstable patients: Patients with COVID-19 with sustained torsades de pointes (TdP) usually become hemodynamically unstable, severely symptomatic because of perfusion failure, or pulseless and should be treated according to standard resuscitation algorithms, including cardioversion/defibrillation. Initial treatment with antiarrhythmic medications is not indicated for hemodynamically unstable or pulseless patients except intravenous (IV) magnesium.
- Stable patients: In a patient with a single episode of TdP, treatment with IV magnesium along with correction of metabolic/electrolyte disturbances or removal of any inciting medications may be sufficient. The patient should be kept under observation until the electrolytes, and the QT interval nearly normalizes. An IV bolus of 2-gram magnesium sulfate is the standard therapy for an adult. This is equivalent to a dose of 8.12 mmol of magnesium. The clinical situation of a patient determines the rate of magnesium infusion. Infusion occurs over one to two minutes in patients with pulseless cardiac arrest. The infusion should occur over 15 minutes in patients without cardiac arrest as a rapid IV bolus of magnesium can result in hypotension and asystole. Some patients are given a continuous bolus of IV magnesium at a rate of 3 to 20 mg/min until the QT interval is below 0.50 seconds.[29][30]
- Other Cardiac arrhythmia: The treatment for other arrhythmias in COVID-19 patients is the same as in patients with arrhythmias without COVID-19 infection. To browse the treatment of other arrhythmias, Click here.
Surgery
- To have a better insight of treatment for different types of arrhythmia, Click here.
Prevention
- Fever can increase the risk of ventricular arrhythmias in patients with Brugada syndrome. Studies have shown significant results with acetaminophen which lowers fever. Patients with prior history of syncope and who develop type 1 ECG finding of Brugada Syndrome should head to the Emergency department if acetaminophen is unable to normalize the arrhythmia.[31]
References
- ↑ Ruan Q, Yang K, Wang W, Jiang L, Song J (2020). "Correction to: Clinical predictors of mortality due to COVID-19 based on an analysis of data of 150 patients from Wuhan, China". Intensive Care Med. 46 (6): 1294–1297. doi:10.1007/s00134-020-06028-z. PMC 7131986 Check
|pmc=value (help). PMID 32253449 Check|pmid=value (help). - ↑ 2.0 2.1 Wang D, Hu B, Hu C, Zhu F, Liu X, Zhang J; et al. (2020). "Clinical Characteristics of 138 Hospitalized Patients With 2019 Novel Coronavirus-Infected Pneumonia in Wuhan, China". JAMA. doi:10.1001/jama.2020.1585. PMC 7042881 Check
|pmc=value (help). PMID 32031570 Check|pmid=value (help). - ↑ 3.0 3.1 Lakkireddy DR, Chung MK, Gopinathannair R, Patton KK, Gluckman TJ, Turagam M; et al. (2020). "Guidance for Cardiac Electrophysiology During the COVID-19 Pandemic from the Heart Rhythm Society COVID-19 Task Force; Electrophysiology Section of the American College of Cardiology; and the Electrocardiography and Arrhythmias Committee of the Council on Clinical Cardiology, American Heart Association". Circulation. 141 (21): e823–e831. doi:10.1161/CIRCULATIONAHA.120.047063. PMC 7243667 Check
|pmc=value (help). PMID 32228309 Check|pmid=value (help). - ↑ Du Y, Tu L, Zhu P, Mu M, Wang R, Yang P; et al. (2020). "Clinical Features of 85 Fatal Cases of COVID-19 from Wuhan. A Retrospective Observational Study". Am J Respir Crit Care Med. 201 (11): 1372–1379. doi:10.1164/rccm.202003-0543OC. PMC 7258652 Check
|pmc=value (help). PMID 32242738 Check|pmid=value (help). - ↑ 5.0 5.1 Duan K, Liu B, Li C, Zhang H, Yu T, Qu J; et al. (2020). "Effectiveness of convalescent plasma therapy in severe COVID-19 patients". Proc Natl Acad Sci U S A. 117 (17): 9490–9496. doi:10.1073/pnas.2004168117. PMC 7196837 Check
|pmc=value (help). PMID 32253318 Check|pmid=value (help). - ↑ 6.0 6.1 Wang, Dawei; Hu, Bo; Hu, Chang; Zhu, Fangfang; Liu, Xing; Zhang, Jing; Wang, Binbin; Xiang, Hui; Cheng, Zhenshun; Xiong, Yong; Zhao, Yan; Li, Yirong; Wang, Xinghuan; Peng, Zhiyong (2020). "Clinical Characteristics of 138 Hospitalized Patients With 2019 Novel Coronavirus–Infected Pneumonia in Wuhan, China". JAMA. 323 (11): 1061. doi:10.1001/jama.2020.1585. ISSN 0098-7484.
- ↑ Xu, Zhe; Shi, Lei; Wang, Yijin; Zhang, Jiyuan; Huang, Lei; Zhang, Chao; Liu, Shuhong; Zhao, Peng; Liu, Hongxia; Zhu, Li; Tai, Yanhong; Bai, Changqing; Gao, Tingting; Song, Jinwen; Xia, Peng; Dong, Jinghui; Zhao, Jingmin; Wang, Fu-Sheng (2020). "Pathological findings of COVID-19 associated with acute respiratory distress syndrome". The Lancet Respiratory Medicine. 8 (4): 420–422. doi:10.1016/S2213-2600(20)30076-X. ISSN 2213-2600.
- ↑ Chen, Mao; Prendergast, Bernard; Redwood, Simon; Xiong, Tian-Yuan (2020). "Coronaviruses and the cardiovascular system: acute and long-term implications". European Heart Journal. 41 (19): 1798–1800. doi:10.1093/eurheartj/ehaa231. ISSN 0195-668X.
- ↑ 9.0 9.1 9.2 Driggin E, Madhavan MV, Bikdeli B, Chuich T, Laracy J, Biondi-Zoccai G; et al. (2020). "Cardiovascular Considerations for Patients, Health Care Workers, and Health Systems During the COVID-19 Pandemic". J Am Coll Cardiol. 75 (18): 2352–2371. doi:10.1016/j.jacc.2020.03.031. PMC 7198856 Check
|pmc=value (help). PMID 32201335 Check|pmid=value (help). - ↑ Lazzerini PE, Laghi-Pasini F, Boutjdir M, Capecchi PL (2019). "Cardioimmunology of arrhythmias: the role of autoimmune and inflammatory cardiac channelopathies". Nat Rev Immunol. 19 (1): 63–64. doi:10.1038/s41577-018-0098-z. PMID 30552387.
- ↑ Clerkin, Kevin J.; Fried, Justin A.; Raikhelkar, Jayant; Sayer, Gabriel; Griffin, Jan M.; Masoumi, Amirali; Jain, Sneha S.; Burkhoff, Daniel; Kumaraiah, Deepa; Rabbani, LeRoy; Schwartz, Allan; Uriel, Nir (2020). "COVID-19 and Cardiovascular Disease". Circulation. 141 (20): 1648–1655. doi:10.1161/CIRCULATIONAHA.120.046941. ISSN 0009-7322.
- ↑ 12.0 12.1 Liu K, Fang YY, Deng Y, Liu W, Wang MF, Ma JP; et al. (2020). "Clinical characteristics of novel coronavirus cases in tertiary hospitals in Hubei Province". Chin Med J (Engl). 133 (9): 1025–1031. doi:10.1097/CM9.0000000000000744. PMC 7147277 Check
|pmc=value (help). PMID 32044814 Check|pmid=value (help). - ↑ 13.0 13.1 Lazzerini PE, Boutjdir M, Capecchi PL (2020). "COVID-19, Arrhythmic Risk, and Inflammation: Mind the Gap!". Circulation. 142 (1): 7–9. doi:10.1161/CIRCULATIONAHA.120.047293. PMID 32286863 Check
|pmid=value (help). - ↑ Skogestad J, Aronsen JM (2018). "Hypokalemia-Induced Arrhythmias and Heart Failure: New Insights and Implications for Therapy". Front Physiol. 9: 1500. doi:10.3389/fphys.2018.01500. PMC 6234658. PMID 30464746.
- ↑ Amin AS, Herfst LJ, Delisle BP, Klemens CA, Rook MB, Bezzina CR; et al. (2008). "Fever-induced QTc prolongation and ventricular arrhythmias in individuals with type 2 congenital long QT syndrome". J Clin Invest. 118 (7): 2552–61. doi:10.1172/JCI35337. PMC 2423868. PMID 18551196.
- ↑ Chang D, Saleh M, Garcia-Bengo Y, Choi E, Epstein L, Willner J (2020). "COVID-19 Infection Unmasking Brugada Syndrome". HeartRhythm Case Rep. doi:10.1016/j.hrcr.2020.03.012. PMC 7138191 Check
|pmc=value (help). PMID 32292696 Check|pmid=value (help). - ↑ Richardson S, Hirsch JS, Narasimhan M, Crawford JM, McGinn T, Davidson KW; et al. (2020). "Presenting Characteristics, Comorbidities, and Outcomes Among 5700 Patients Hospitalized With COVID-19 in the New York City Area". JAMA. doi:10.1001/jama.2020.6775. PMC 7177629 Check
|pmc=value (help). PMID 32320003 Check|pmid=value (help). - ↑ Giudicessi, John R.; Noseworthy, Peter A.; Friedman, Paul A.; Ackerman, Michael J. (2020). "Urgent Guidance for Navigating and Circumventing the QTc-Prolonging and Torsadogenic Potential of Possible Pharmacotherapies for Coronavirus Disease 19 (COVID-19)". Mayo Clinic Proceedings. 95 (6): 1213–1221. doi:10.1016/j.mayocp.2020.03.024. ISSN 0025-6196.
- ↑ Goyal, Parag; Choi, Justin J.; Pinheiro, Laura C.; Schenck, Edward J.; Chen, Ruijun; Jabri, Assem; Satlin, Michael J.; Campion, Thomas R.; Nahid, Musarrat; Ringel, Joanna B.; Hoffman, Katherine L.; Alshak, Mark N.; Li, Han A.; Wehmeyer, Graham T.; Rajan, Mangala; Reshetnyak, Evgeniya; Hupert, Nathaniel; Horn, Evelyn M.; Martinez, Fernando J.; Gulick, Roy M.; Safford, Monika M. (2020). "Clinical Characteristics of Covid-19 in New York City". New England Journal of Medicine. 382 (24): 2372–2374. doi:10.1056/NEJMc2010419. ISSN 0028-4793.
- ↑ Guo T, Fan Y, Chen M, Wu X, Zhang L, He T; et al. (2020). "Cardiovascular Implications of Fatal Outcomes of Patients With Coronavirus Disease 2019 (COVID-19)". JAMA Cardiol. doi:10.1001/jamacardio.2020.1017. PMC 7101506 Check
|pmc=value (help). PMID 32219356 Check|pmid=value (help). - ↑ Baldi, Enrico; Sechi, Giuseppe M.; Mare, Claudio; Canevari, Fabrizio; Brancaglione, Antonella; Primi, Roberto; Klersy, Catherine; Palo, Alessandra; Contri, Enrico; Ronchi, Vincenza; Beretta, Giorgio; Reali, Francesca; Parogni, Pierpaolo; Facchin, Fabio; Bua, Davide; Rizzi, Ugo; Bussi, Daniele; Ruggeri, Simone; Oltrona Visconti, Luigi; Savastano, Simone (2020). "Out-of-Hospital Cardiac Arrest during the Covid-19 Outbreak in Italy". New England Journal of Medicine. doi:10.1056/NEJMc2010418. ISSN 0028-4793.
- ↑ Shao, Fei; Xu, Shuang; Ma, Xuedi; Xu, Zhouming; Lyu, Jiayou; Ng, Michael; Cui, Hao; Yu, Changxiao; Zhang, Qing; Sun, Peng; Tang, Ziren (2020). "In-hospital cardiac arrest outcomes among patients with COVID-19 pneumonia in Wuhan, China". Resuscitation. 151: 18–23. doi:10.1016/j.resuscitation.2020.04.005. ISSN 0300-9572.
- ↑ Gandhi, Rajesh T.; Solomon, Caren G.; Lynch, John B.; del Rio, Carlos (2020). "Mild or Moderate Covid-19". New England Journal of Medicine. doi:10.1056/NEJMcp2009249. ISSN 0028-4793.
- ↑ Chang, David; Saleh, Moussa; Gabriels, James; Ismail, Haisam; Goldner, Bruce; Willner, Jonathan; Beldner, Stuart; Mitra, Raman; John, Roy; Epstein, Laurence M. (2020). "Inpatient Use of Ambulatory Telemetry Monitors for COVID-19 Patients Treated With Hydroxychloroquine and/or Azithromycin". Journal of the American College of Cardiology. 75 (23): 2992–2993. doi:10.1016/j.jacc.2020.04.032. ISSN 0735-1097.
- ↑ Inciardi, Riccardo M.; Lupi, Laura; Zaccone, Gregorio; Italia, Leonardo; Raffo, Michela; Tomasoni, Daniela; Cani, Dario S.; Cerini, Manuel; Farina, Davide; Gavazzi, Emanuele; Maroldi, Roberto; Adamo, Marianna; Ammirati, Enrico; Sinagra, Gianfranco; Lombardi, Carlo M.; Metra, Marco (2020). "Cardiac Involvement in a Patient With Coronavirus Disease 2019 (COVID-19)". JAMA Cardiology. doi:10.1001/jamacardio.2020.1096. ISSN 2380-6583.
- ↑ Guo, Tao; Fan, Yongzhen; Chen, Ming; Wu, Xiaoyan; Zhang, Lin; He, Tao; Wang, Hairong; Wan, Jing; Wang, Xinghuan; Lu, Zhibing (2020). "Cardiovascular Implications of Fatal Outcomes of Patients With Coronavirus Disease 2019 (COVID-19)". JAMA Cardiology. doi:10.1001/jamacardio.2020.1017. ISSN 2380-6583.
- ↑ Kochi, Adriano Nunes; Tagliari, Ana Paula; Forleo, Giovanni Battista; Fassini, Gaetano Michele; Tondo, Claudio (2020). "Cardiac and arrhythmic complications in patients with COVID‐19". Journal of Cardiovascular Electrophysiology. 31 (5): 1003–1008. doi:10.1111/jce.14479. ISSN 1045-3873.
- ↑ Panchal, Ashish R.; Berg, Katherine M.; Kudenchuk, Peter J.; Del Rios, Marina; Hirsch, Karen G.; Link, Mark S.; Kurz, Michael C.; Chan, Paul S.; Cabañas, José G.; Morley, Peter T.; Hazinski, Mary Fran; Donnino, Michael W. (2018). "2018 American Heart Association Focused Update on Advanced Cardiovascular Life Support Use of Antiarrhythmic Drugs During and Immediately After Cardiac Arrest: An Update to the American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care". Circulation. 138 (23). doi:10.1161/CIR.0000000000000613. ISSN 0009-7322.
- ↑ Tzivoni, D; Banai, S; Schuger, C; Benhorin, J; Keren, A; Gottlieb, S; Stern, S (1988). "Treatment of torsade de pointes with magnesium sulfate". Circulation. 77 (2): 392–397. doi:10.1161/01.CIR.77.2.392. ISSN 0009-7322.
- ↑ Neumar, R. W.; Otto, C. W.; Link, M. S.; Kronick, S. L.; Shuster, M.; Callaway, C. W.; Kudenchuk, P. J.; Ornato, J. P.; McNally, B.; Silvers, S. M.; Passman, R. S.; White, R. D.; Hess, E. P.; Tang, W.; Davis, D.; Sinz, E.; Morrison, L. J. (2010). "Part 8: Adult Advanced Cardiovascular Life Support: 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care". Circulation. 122 (18_suppl_3): S729–S767. doi:10.1161/CIRCULATIONAHA.110.970988. ISSN 0009-7322.
- ↑ Wu CI, Postema PG, Arbelo E, Behr ER, Bezzina CR, Napolitano C; et al. (2020). "SARS-CoV-2, COVID-19, and inherited arrhythmia syndromes". Heart Rhythm. doi:10.1016/j.hrthm.2020.03.024. PMC 7156157 Check
|pmc=value (help). PMID 32244059 Check|pmid=value (help).