COVID-19-associated myocardial infarction
Main article:COVID-19
For COVID-19 frequently asked inpatient questions, click here
For COVID-19 frequently asked outpatient questions, click here
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Sara Zand, M.D.[2] Sara Haddadi, M.D.[3]
Synonyms and keywords: Novel coronavirus, covid-19, COVID-19, SARS-CoV-2, Myocardial Infarction, MI, ST Elevation Myocardial Infarction, STEMI, Non ST Elevation Myocardial Infarction, NSTEMI
Overview
On March 11, 2020, the World Health Organization declared the COVID-19 outbreak as a pandemic. Coronavirus disease 2019 (COVID-19) has negative effect on patients with ST-segment elevation myocardial infarction (STEMI). STEMI can be the first manifestation of COVID-19. Reported case series addressed the significant reduction of STEMI presentation and cath lab activation rate during first wave of pandemic period. So, the number of out-of hospital cardiac arrest increased due to late presentation of STEMI in italy. Additionally, there was an increased incidence of acute thrombotic STEMI among patients undergoing coronary angiography suggestive of increased inflammation and platelet activation and direct viral interaction with ACE2 receptors. However, one-third of STEMI patients undergoing angiography had non-obstructive culprit lesion indicating of type2 myocardial infarction, myocarditis secondary to SARS-COV-2 infection, SARS-COV-2 related endothelial dysfunction, or cytokine storm. STEMI patients with confirmed COVID-19 presented with lower conventional risk factors and were more likely to present with deteriotated clinical status and higher killip class and progression to cardiogenic shock as well as higher mortality rate due to COVID-19 thrombogenicity and high thrombisis burden in coronary arteries.
Historical Perspective
- COVID-19 (SARS-CoV-2) outbreak initiated and was discovered in December, 2019 in Wuhan, Hubei Province, China.[1]
- On March 11, 2020, the World Health Organization declared the COVID-19 outbreak a pandemic.
- Even before the pandemic declaration, concerns about the management of Acute Myocardial Infarction in COVID-19 era started to rise and on March 11, 2020, Zeng et al addressed this issue by introducing Protocols From Sichuan Provincial People's Hospital for Acute MI diagnosis and treatment protocol adjustment during COVID-19.[2]
- "Be Prepared" is the title of a paper published on March 15, 2020, discussing the longer time from symptom onset to first medical contact in STEMI patients due to the COVID-19 outbreak.The call for maximizing acute care resources, maintaining access to services while limiting nosocomial COVID-19 infection was one of the earliest in regards to COVID-19-associated myocardial infarction.[3]
- On Apr 13, 2020, Frankie Tam 'et al.' compared Time Components of STEMI Care Before and After COVID-19 Outbreak[4]
- On March 31, 2020, Kang discussed underlying diseases such as cardiovascular disease as a risk factor developing a serious and severe COVID-19.[5]
- On June 9, 2020, Fried et al. discussed 4 cases showing a variety of cardiovascular presentations of COVID-19 and one of the uncertainties as whether or not the staff should proceed to coronary angiography in response to ECG changes and positive troponin[6]
Classification
Myocardial infarction may be classified according to two sub-types:
- Non ST Elevation Myocardial Infarction (NSTEMI)
- ST Elevation Myocardial Infarction (STEMI)
Pathophysiology
The mechanism of COVID-19 myocardial infarction is not fully understood and is likely multi-factorial.
- It is thought that thrombotic consequences of covid-19 cab be the result of inflammatory response, sequelae of severe disease, direct viral interaction with ACE-2 receptors.
- The increased incidence of thrombotic STEMI has been noted in the reported case series.
- Microvascular coagulopathy as well as myocardial dysfunction have been addressed in patients with or without obstructive coronary artery disease.
- Two potential mechanisms for myocardial infarction in the setting of COVID-19 infection include:[7]
- Plaque rupture in the setting of the inflammatory condition/shear stress caused by the virus
- Exacerbation of pre-existing coronary artery disease
- The cytokine release caused by the virus may lead to vascular inflammation, plaque instability, myocardial inflammation, a hypercoagulable state, and direct myocardial suppression. For hypercoagulable state in COVID-19, click here
- Increased inflammatory response may also lead to endothelial dysfunction causing the formation of microthrombi.[8]
- ACE-2 is the receptor of SARS-CoV 2 which is highly expressed on cardiac pericytes. Therefore it can be speculated that the pericyte damage by the virus results in endothelial cell damage which leads to microvascular impairment.[9]
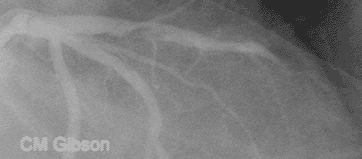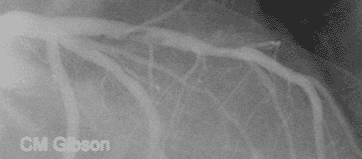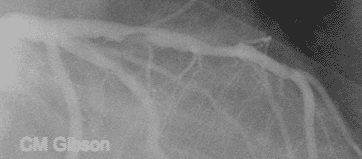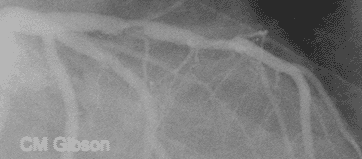
- The above video shows plaque rupture or disruption of an atherosclerotic plaque in the mid left anterior descending artery (LAD) .
- To view Non-ST-elevation myocardial infarction pathophysiology click here
- To view ST-elevation myocardial infarction pathophysiology click here
Pathological changes:
- In cardiac tissue: observations range from minimal change to interstitial inflammatory infiltration and myocyte necrosis
- In the vasculature: findings include micro-thrombosis and vascular inflammation[10]
Causes
According to the Fourth Universal Definition of MI, there are two clinical classifications of the disease based on the causes:
- Type 1: MI caused by acute atherothrombotic CAD precipitated by atherosclerotic plaque disruption (rupture or erosion).
- Type 2: MI due to a mismatch between oxygen demand and supply, possible causes are hypotension due to septic state and hypoxemia due to respiratory failure
Most of the MIs associated with COVID-19 are type 2 indicating the cause to be the primary infection, hemodynamic disturbance, or respiratory deterioration.[11] [8]
Differentiating Myocardial infarction from other Diseases
- For further information about the differential diagnosis, click here.
- To view the differential diagnosis of COVID-19, click here.
Epidemiology and Demographics
- The exact incidence of STEMI associated COVID-19 is not fully understood yet. However, during the first wave of pandemic, the number of hospitalized STEMI patients decreased in comparison with the parallel year.[12][13][14][15]
Age
Gender
Race
- STEMI associated covid-19 were more commonly observed among minorities including Hispanic, Black ethnicity.[16]
Risk Factors
Common risk factors in the development of acute coronary syndrome including STEMI and non-STEMI are listed below:[17]
- Age (men >45 and women >55)
- Diabetes mellitus
- Hypercholesterolemia
- Hypertension
- Smoking
- Obesity
- Lack of physical activity
- Family history of heart disease
- History of HTN, DM and pre-eclampsia during pregnancy
For Risk factors associated with COVID-19 please click here
Screening
Due to the higher mortality of patients with COVID-19 and cardiovascular comorbidities, it advisable to triage patients with COVID-19 based on their underlying CVD for a more aggressive treatment plan.[18]
Natural History, Complications and Prognosis
- STEMI in the setting of COVID-19 may be the first clinical manifestation of the disease. [19]
- The causes of decrease rate of hospitalized acute MI associated COVID-19 during the first wave of COVID-19 can be explained by fear of contracting the virus in the hospital, reduced air pollution, limited physical activity due to social restrictions, availability of telemedicine for controlling the chronic diseases.[20][21]
- However, previous studies showed the increase rate of acute MI immediately after stressful events such as earthquakes, or terrorist attacks.[22]
- Early clinical features include typical chest pain, dyspnea, arrhythmia, hemodynamic collapse, or syncope.
- Patients with MI associated COVID-19 experienced longer total ischemic time, more severe condition at the time of admission, higher rate of in-hospital advers events. [23]
- STEMI patients with COVID-19 were more likely to develop cardiogenic shock and were less likey to receive invasive coronary angiography.[16]
- Ischemic time and door to ballon time increased in patients with STEMI associated COVID-19.[24]
- About 40% of STEMI patients in the setting of COVID-19 do not have culprit lesion in coronary angiography.[25]
- The clinical feature in the setting of non-thrombotic STEMI may be due to type2 myocardial infarction, myocarditis secondary to SARS-COV-2 infection, SARS-COV-2 related endothelial dysfunction, cytokine storm.
- In STEMI associated COVID-19, the rate of arterial thrombosis burden was higher than non-covid-19 patients, so the clinical status should be established in covid-19 patients.[26]
- Complications of STEMI associated COVID-19 are:
- Higher incidence of multiple thrombotic culprit lesions
- Higher stent thrombosis
- Higher thrombus grade
- Lower rate to myocardial blush grade
- Increased use of GP2b/3a inhibitors
- Higher thrombosis aspiration
- Higher rate of pre-hospital cardiac arrest
- Higher admission days
- Lower LVEF, higher myocardial damage , and toponin levels
- Increased in-hospital mortality
- Prognosis was generally poor, and the mortality rate of patients presented with STEMI associated COVID-19 was high.
- Table bellow shown the reported cases of TIMI flow zero or no-reflow in patients with thrombotic STEMI associated COVID-19 undergoing percutaneous coronary intervention.
| Age, sex | Cardiovascular history | Symptoms | Laboratory findings | Timing according to covid-19 infection | Concomitant covid-19 complications | Covid-19 severity | Diagnosis | Vessle | Treatment | Outcome |
|---|---|---|---|---|---|---|---|---|---|---|
| 65 years, male | Hypertension, diabetes mellitus | New chest pain, shortness of breath | High levels of troponin, CRP, D-dimer | 7 days | Sinus bradycardia, complete heart block, inferior STelevation | Mild | Inferior STEMI | 100% RCA stenosis, moderate LAD stenosis, NO visible edge dissection in IVUS | ASA, ticagrelor, heparin, eptifibatide , PCI of RCA, ballon angioplasty, thrombectomy, vasodilation, IABP | Cardiogenic shock after PCI despite patency of stent or no evidence of edge dissection in IVUS, expired due to persistent microvascular thrombosis |
| 74 years, female | Hypertension, diabetes mellitus, hyperlipidemia | Shortness of breath, fever, myalgia, hypoxic respiratory failure, new onset chest pain 5 days after admission | High levels of troponin, CRP, ferritin, D-dimer | 8 days | Severe lung infiltration | Antrolateral STEMI | 100% distal LAD lesion, | ASA, clopidogrel, enoxaparin, intubation, urgent catheterization, thrombectomy, PCI of LAD lesion, ballon angioplasty, stent placement, no achieved distal flow | Expired due to sepsis and respiratory failure |
Diagnosis
Diagnostic Study of Choice
- Acute Myocardial Infarction is defined as an acute myocardial injury with clinical evidence of acute myocardial ischemia plus rise and/or fall of cardiac troponin values with at least one value above the 99th percentile upper reference limit and at least one of the following:
- Symptoms of myocardial ischemia including new ischemic ECG changes
- Development of pathological Q waves
- Imaging evidence of new loss of viable myocardium
- New regional wall motion abnormality in a pattern consistent with an ischemic etiology
- Identification of a coronary thrombus by angiography or autopsy (not for type 2 or 3 MI).[11]
- For ST-elevation myocardial infarction diagnostic criteria please click here
- Considering the diagnostic criteria, it is not difficult to differentiate STEMI from other causes of chest pain or equivalent anginal symptoms. However, during COVID-19 pandemic other causes of COVID-19-associated myocardial injury such as COVID-19-associated stress cardiomyopathy or COVID-19-associated myocarditis should be the top of the differential diagnosis list.
- EKG criteria are not specific and may also be present in other COVID-19-associated myocardial injury conditions associated with COVID-19.
- Although elevated troponin is also a non-specific finding, for patients with a high troponin level and suspected STEMI, echocardiography is not generally performed due to the emergent need for angiography.
- For critically ill patients due to COVID-19, the decision to perform angiography or reperfusion should be done on a case by case basis.
History and Symptoms
There are no specific symptoms associated with COVID-19-associated-Myocardial infarction. Common symptoms in patients with acute MI is listed below:[27]
- Substernal chest pain
- Occurs at rest or exertion
- Radiation to neck, []jaw]], left []shoulder]] and left arm
- Aggravated by physical activity and []emotional stress]]
- Relieved by rest, nitroglycerin or both
- Chest discomfort described crushing, squeezing, burning, choking, tightness, or aching
- Dyspnea
- Diaphoresis
- Nausea and vomiting
- Fatigue
- Syncope[27]
For non-ST elevation myocardial infarction history and symptoms please click here
For ST elevation myocardial infarction history and symptoms please click here
Physical Examination
- For non-ST elevation myocardial infarction physical examination please click here
- For STEMI physical examination please click here
Laboratory Findings
- Laboratory finding in patients with STEMI associated COVID-19 showed increase levels of inflammatory markers including lymphopnea, D-dimer, C- reactive protein as well as increased troponin and CK-MB levels.
- Higher D-dimer level in COVID-19 patients with STEMI was correlated with thrombus grade, myocardial blush grade, need for higher dose of heparin during primary PCI.
Electrocardiogram
There are no specific ECG findings associated with both COVID-19 and Myocardial infarction.
- For non-ST-elevation myocardial infarction electrocardiogram please click here
- For ST-elevation myocardial infarction electrocardiogram please click here
- For COVID-19 electrocardiogram findings please click here
X-ray
There are no specific X-ray findings associated with both COVID-19 and Myocardial infarction.
- For X-ray findings in COVID-19 please click here
- For X-ray findings in Myocardial Infarction please click here
Echocardiography
- In a study done among 28 patients with COVID-19 with STEMI, the following echocardiographic findings were reported:[19]
- Localized wall motion abnormalities
- Diffuse hypokinesia
- Left ventricular ejection fraction was lower than 50% in about 61% of the individuals.
- For COVID-19 echocardiography please click here
- For non-STEMI Echocardiography please click here
- For STEMI Echocardiography please click here
CT scan
- There are no specific CT scan findings related to COVID-19-associated myocardial infarction.
MRI
- There are no MRI findings related to COVID-19-associated myocardial infarction.
Other Imaging Studies
Coronary Angiography
- In one study done among patients with COVID-19 with STEMI, coronary angiography failed to reveal any culprit lesion in about 40% of the patients. However, in the remaining patients, coronary angiography was able to localize a lesion.[19]
- For non-STEMI coronary angiography please click here
- For STEMI coronary angiography please click here
Other Diagnostic Studies
- There are no specific other diagnostic studies related to COVID-19-associated myocardial infarction.
Treatment
Medical Therapy
In patients with ACS and COVID-19, treatment should follow the guidelines of the updated Society for Cardiovascular Angiography and Interventions.[10] [28]
- Treatment of STEMI and COVID-19:
- Intravenous thrombolysis as first-line therapy for STEMI patients with confirmed COVID-19 since most hospitals do not have protected cardiac catheterization labs.[29]
- According to the latest European Society of Cardiology (ESC) guidance for the management of cardiac complications related to COVID-19, if STEMI is diagnosed timely primary percutaneous intervention should be performed, irrespective of COVID-19 diagnosis. Fibrinolysis should be the first treatment choice when percutaneous intervention is not feasible within 12 hours of symptom onset.
- Treatment of NSTEMI should be based on risk stratification:
- High-risk cases: immediate invasive strategy
- Intermediate/low-risk cases: non-invasive strategies such as coronary CT-angiography with regular follow-ups should be the treatment of choice.[8]
Primary Prevention
- Effective measure for primary prevention of MI associated COVID-19 is vaccination.
- Other primary prevention strategies include measures to reduce the occurrence of myocardial injury among COVID-19 patients. Recent studies have suggested the use of medications improving microcirculation, especially for the high-risk group such as males, smokers, diabetic patients, and patients with established cardiovascular disease comorbidities.[8]
- For Risk factors associated with COVID-19 please click here
Secondary Prevention
- There are no established measures for the secondary prevention of COVID-19-associated myocardial infarction.
- For ST-elevation myocardial infarction secondary prevention please click here
References
- ↑ Meng X, Deng Y, Dai Z, Meng Z (June 2020). "COVID-19 and anosmia: A review based on up-to-date knowledge". Am J Otolaryngol. 41 (5): 102581. doi:10.1016/j.amjoto.2020.102581. PMC 7265845 Check
|pmc=value (help). PMID 32563019 Check|pmid=value (help). - ↑ Zeng, Jie; Huang, Jianxin; Pan, Lingai (2020). "How to balance acute myocardial infarction and COVID-19: the protocols from Sichuan Provincial People’s Hospital". Intensive Care Medicine. 46 (6): 1111–1113. doi:10.1007/s00134-020-05993-9. ISSN 0342-4642.
- ↑ Ardati, Amer K.; Mena Lora, Alfredo J. (2020). "Be Prepared". Circulation: Cardiovascular Quality and Outcomes. 13 (4). doi:10.1161/CIRCOUTCOMES.120.006661. ISSN 1941-7713.
- ↑ Tam, Chor-Cheung Frankie; Cheung, Kent-Shek; Lam, Simon; Wong, Anthony; Yung, Arthur; Sze, Michael; Lam, Yui-Ming; Chan, Carmen; Tsang, Tat-Chi; Tsui, Matthew; Tse, Hung-Fat; Siu, Chung-Wah (2020). "Impact of Coronavirus Disease 2019 (COVID-19) Outbreak on ST-Segment–Elevation Myocardial Infarction Care in Hong Kong, China". Circulation: Cardiovascular Quality and Outcomes. 13 (4). doi:10.1161/CIRCOUTCOMES.120.006631. ISSN 1941-7713.
- ↑ Kang, Yun-Jung (2020). "Mortality Rate of Infection With COVID-19 in Korea From the Perspective of Underlying Disease". Disaster Medicine and Public Health Preparedness: 1–3. doi:10.1017/dmp.2020.60. ISSN 1935-7893.
- ↑ Fried, Justin A.; Ramasubbu, Kumudha; Bhatt, Reema; Topkara, Veli K.; Clerkin, Kevin J.; Horn, Evelyn; Rabbani, LeRoy; Brodie, Daniel; Jain, Sneha S.; Kirtane, Ajay J.; Masoumi, Amirali; Takeda, Koji; Kumaraiah, Deepa; Burkhoff, Daniel; Leon, Martin; Schwartz, Allan; Uriel, Nir; Sayer, Gabriel (2020). "The Variety of Cardiovascular Presentations of COVID-19". Circulation. 141 (23): 1930–1936. doi:10.1161/CIRCULATIONAHA.120.047164. ISSN 0009-7322.
- ↑ Bansal, Manish (2020). "Cardiovascular disease and COVID-19". Diabetes & Metabolic Syndrome: Clinical Research & Reviews. 14 (3): 247–250. doi:10.1016/j.dsx.2020.03.013. ISSN 1871-4021.
- ↑ 8.0 8.1 8.2 8.3 Montone, Rocco A; Iannaccone, Giulia; Meucci, Maria Chiara; Gurgoglione, Filippo; Niccoli, Giampaolo (2020). "Myocardial and Microvascular Injury Due to Coronavirus Disease 2019". European Cardiology Review. 15. doi:10.15420/ecr.2020.22. ISSN 1758-3764.
- ↑ Xiong, Chenglong; Feng, Yi; Chen, Mingquan; Li, Xiangjie; Chen, Liang (2020). "The ACE2 expression in human heart indicates new potential mechanism of heart injury among patients infected with SARS-CoV-2". Cardiovascular Research. 116 (6): 1097–1100. doi:10.1093/cvr/cvaa078. ISSN 0008-6363.
- ↑ 10.0 10.1 Kang Y, Chen T, Mui D, Ferrari V, Jagasia D, Scherrer-Crosbie M; et al. (2020). "Cardiovascular manifestations and treatment considerations in covid-19". Heart. doi:10.1136/heartjnl-2020-317056. PMC 7211105 Check
|pmc=value (help). PMID 32354800 Check|pmid=value (help). - ↑ 11.0 11.1 Thygesen K, Alpert JS, Jaffe AS, Chaitman BR, Bax JJ, Morrow DA; et al. (2018). "Fourth Universal Definition of Myocardial Infarction (2018)". J Am Coll Cardiol. 72 (18): 2231–2264. doi:10.1016/j.jacc.2018.08.1038. PMID 30153967.
- ↑ 12.0 12.1 De Rosa S, Spaccarotella C, Basso C, Calabrò MP, Curcio A, Filardi PP; et al. (2020). "Reduction of hospitalizations for myocardial infarction in Italy in the COVID-19 era". Eur Heart J. 41 (22): 2083–2088. doi:10.1093/eurheartj/ehaa409. PMC 7239145 Check
|pmc=value (help). PMID 32412631 Check|pmid=value (help). - ↑ Garcia S, Albaghdadi MS, Meraj PM, Schmidt C, Garberich R, Jaffer FA; et al. (2020). "Reduction in ST-Segment Elevation Cardiac Catheterization Laboratory Activations in the United States During COVID-19 Pandemic". J Am Coll Cardiol. 75 (22): 2871–2872. doi:10.1016/j.jacc.2020.04.011. PMC 7151384 Check
|pmc=value (help). PMID 32283124 Check|pmid=value (help). - ↑ Solomon MD, McNulty EJ, Rana JS, Leong TK, Lee C, Sung SH; et al. (2020). "The Covid-19 Pandemic and the Incidence of Acute Myocardial Infarction". N Engl J Med. doi:10.1056/NEJMc2015630. PMID 32427432 Check
|pmid=value (help). - ↑ De Filippo O, D'Ascenzo F, Angelini F, Bocchino PP, Conrotto F, Saglietto A; et al. (2020). "Reduced Rate of Hospital Admissions for ACS during Covid-19 Outbreak in Northern Italy". N Engl J Med. doi:10.1056/NEJMc2009166. PMC 7224608 Check
|pmc=value (help). PMID 32343497 Check|pmid=value (help). - ↑ 16.0 16.1 Garcia S, Dehghani P, Grines C, Davidson L, Nayak KR, Saw J, Waksman R, Blair J, Akshay B, Garberich R, Schmidt C, Ly HQ, Sharkey S, Mercado N, Alfonso CE, Misumida N, Acharya D, Madan M, Hafiz AM, Javed N, Shavadia J, Stone J, Alraies MC, Htun W, Downey W, Bergmark BA, Ebinger J, Alyousef T, Khalili H, Hwang CW, Purow J, Llanos A, McGrath B, Tannenbaum M, Resar J, Bagur R, Cox-Alomar P, Stefanescu Schmidt AC, Cilia LA, Jaffer FA, Gharacholou M, Salinger M, Case B, Kabour A, Dai X, Elkhateeb O, Kobayashi T, Kim HH, Roumia M, Aguirre FV, Rade J, Chong AY, Hall HM, Amlani S, Bagherli A, Patel R, Wood DA, Welt FG, Giri J, Mahmud E, Henry TD (April 2021). "Initial Findings From the North American COVID-19 Myocardial Infarction Registry". J Am Coll Cardiol. 77 (16): 1994–2003. doi:10.1016/j.jacc.2021.02.055. PMC 8054772 Check
|pmc=value (help). PMID 33888249 Check|pmid=value (help). Vancouver style error: initials (help) - ↑ Fuster V, Badimon L, Cohen M, Ambrose JA, Badimon JJ, Chesebro J (1988). "Insights into the pathogenesis of acute ischemic syndromes". Circulation. 77 (6): 1213–20. PMID 3286036.
- ↑ Guo T, Fan Y, Chen M, Wu X, Zhang L, He T; et al. (2020). "Cardiovascular Implications of Fatal Outcomes of Patients With Coronavirus Disease 2019 (COVID-19)". JAMA Cardiol. doi:10.1001/jamacardio.2020.1017. PMC 7101506 Check
|pmc=value (help). PMID 32219356 Check|pmid=value (help). - ↑ 19.0 19.1 19.2 Stefanini, Giulio G.; Montorfano, Matteo; Trabattoni, Daniela; Andreini, Daniele; Ferrante, Giuseppe; Ancona, Marco; Metra, Marco; Curello, Salvatore; Maffeo, Diego; Pero, Gaetano; Cacucci, Michele; Assanelli, Emilio; Bellini, Barbara; Russo, Filippo; Ielasi, Alfonso; Tespili, Maurizio; Danzi, Gian Battista; Vandoni, Pietro; Bollati, Mario; Barbieri, Lucia; Oreglia, Jacopo; Lettieri, Corrado; Cremonesi, Alberto; Carugo, Stefano; Reimers, Bernhard; Condorelli, Gianluigi; Chieffo, Alaide (2020). "ST-Elevation Myocardial Infarction in Patients With COVID-19". Circulation. 141 (25): 2113–2116. doi:10.1161/CIRCULATIONAHA.120.047525. ISSN 0009-7322.
- ↑ Metzler B, Siostrzonek P, Binder RK, Bauer A, Reinstadler SJ (May 2020). "Decline of acute coronary syndrome admissions in Austria since the outbreak of COVID-19: the pandemic response causes cardiac collateral damage". Eur Heart J. 41 (19): 1852–1853. doi:10.1093/eurheartj/ehaa314. PMC 7184486 Check
|pmc=value (help). PMID 32297932 Check|pmid=value (help). - ↑ Mafham MM, Spata E, Goldacre R, Gair D, Curnow P, Bray M, Hollings S, Roebuck C, Gale CP, Mamas MA, Deanfield JE, de Belder MA, Luescher TF, Denwood T, Landray MJ, Emberson JR, Collins R, Morris E, Casadei B, Baigent C (August 2020). "COVID-19 pandemic and admission rates for and management of acute coronary syndromes in England". Lancet. 396 (10248): 381–389. doi:10.1016/S0140-6736(20)31356-8. PMC 7429983 Check
|pmc=value (help). PMID 32679111 Check|pmid=value (help). Vancouver style error: initials (help) - ↑ Leor J, Poole WK, Kloner RA (February 1996). "Sudden cardiac death triggered by an earthquake". N Engl J Med. 334 (7): 413–9. doi:10.1056/NEJM199602153340701. PMID 8552142.
- ↑ Fardman A, Zahger D, Orvin K, Oren D, Kofman N, Mohsen J, Tsafrir O, Asher E, Rubinshtein R, Jamal J, Efraim R, Halabi M, Shacham Y, Fortis LH, Cohen T, Klempfner R, Segev A, Beigel R, Matetzky S (2021). "Acute myocardial infarction in the Covid-19 era: Incidence, clinical characteristics and in-hospital outcomes-A multicenter registry". PLoS One. 16 (6): e0253524. doi:10.1371/journal.pone.0253524. PMC 8213163 Check
|pmc=value (help). PMID 34143840 Check|pmid=value (help). - ↑ De Luca G, Cercek M, Jensen LO, Vavlukis M, Calmac L, Johnson T, Roura I Ferrer G, Ganyukov V, Wojakowski W, von Birgelen C, Versaci F, Ten Berg J, Laine M, Dirksen M, Casella G, Kala P, Díez Gil JL, Becerra V, De Simone C, Carrill X, Scoccia A, Lux A, Kovarnik T, Davlouros P, Gabrielli G, Flores Rios X, Bakraceski N, Levesque S, Guiducci V, Kidawa M, Marinucci L, Zilio F, Galasso G, Fabris E, Menichelli M, Manzo S, Caiazzo G, Moreu J, Sanchis Forés J, Donazzan L, Vignali L, Teles R, Bosa Ojeda F, Lehtola H, Camacho-Freiere S, Kraaijeveld A, Antti Y, Boccalatte M, Martínez-Luengas IL, Scheller B, Alexopoulos D, Uccello G, Faurie B, Gutierrez Barrios A, Wilbert B, Cortese G, Moreno R, Parodi G, Kedhi E, Verdoia M (December 2020). "Impact of COVID-19 pandemic and diabetes on mechanical reperfusion in patients with STEMI: insights from the ISACS STEMI COVID 19 Registry". Cardiovasc Diabetol. 19 (1): 215. doi:10.1186/s12933-020-01196-0. PMC 7747477 Check
|pmc=value (help). PMID 33339541 Check|pmid=value (help). Vancouver style error: missing comma (help) - ↑ Stefanini GG, Montorfano M, Trabattoni D, Andreini D, Ferrante G, Ancona M, Metra M, Curello S, Maffeo D, Pero G, Cacucci M, Assanelli E, Bellini B, Russo F, Ielasi A, Tespili M, Danzi GB, Vandoni P, Bollati M, Barbieri L, Oreglia J, Lettieri C, Cremonesi A, Carugo S, Reimers B, Condorelli G, Chieffo A (June 2020). "ST-Elevation Myocardial Infarction in Patients With COVID-19: Clinical and Angiographic Outcomes". Circulation. 141 (25): 2113–2116. doi:10.1161/CIRCULATIONAHA.120.047525. PMC 7302062 Check
|pmc=value (help). PMID 32352306 Check|pmid=value (help). - ↑ Choudry FA, Hamshere SM, Rathod KS, Akhtar MM, Archbold RA, Guttmann OP, Woldman S, Jain AK, Knight CJ, Baumbach A, Mathur A, Jones DA (September 2020). "High Thrombus Burden in Patients With COVID-19 Presenting With ST-Segment Elevation Myocardial Infarction". J Am Coll Cardiol. 76 (10): 1168–1176. doi:10.1016/j.jacc.2020.07.022. PMC 7833185 Check
|pmc=value (help). PMID 32679155 Check|pmid=value (help). - ↑ 27.0 27.1 Abidov A, Rozanski A, Hachamovitch R, Hayes SW, Aboul-Enein F, Cohen I; et al. (2005). "Prognostic significance of dyspnea in patients referred for cardiac stress testing". N Engl J Med. 353 (18): 1889–98. doi:10.1056/NEJMoa042741. PMID 16267320. Review in: Evid Based Med. 2006 Jun;11(3):91
- ↑ Szerlip M, Anwaruddin S, Aronow HD, Cohen MG, Daniels MJ, Dehghani P; et al. (2020). "Considerations for cardiac catheterization laboratory procedures during the COVID-19 pandemic perspectives from the Society for Cardiovascular Angiography and Interventions Emerging Leader Mentorship (SCAI ELM) Members and Graduates". Catheter Cardiovasc Interv. doi:10.1002/ccd.28887. PMID 32212409 Check
|pmid=value (help). - ↑ Ullah W, Sattar Y, Saeed R, Ahmad A, Boigon MI, Haas DC; et al. (2020). "As the COVID-19 pandemic drags on, where have all the STEMIs gone?". Int J Cardiol Heart Vasc. 29: 100550. doi:10.1016/j.ijcha.2020.100550. PMC 7261452 Check
|pmc=value (help). PMID 32550258 Check|pmid=value (help).