Rabies pathophysiology: Difference between revisions
No edit summary |
m (Bot: Removing from Primary care) |
||
| (9 intermediate revisions by 3 users not shown) | |||
| Line 1: | Line 1: | ||
__NOTOC__ | __NOTOC__ | ||
{{Rabies}} | {{Rabies}} | ||
{{CMG}} | {{CMG}}; {{AE}} {{HK}} | ||
== Overview == | == Overview == | ||
The ''[[ | The ''[[rabies virus]]'' is categorized as a [[Lyssavirus]]. The [[molecular biology]] of rabies consists of bullet shaped [[virus]] with helical symmetry that has a length of approximately 180 nm. Rabies typically has its greatest effect on the [[brain]]. Rabies is typically defined by [[encephalitis]] and [[myelitis]]. Various carnivorous animal species have been identified as the source of ''[[rabies virus]]'' (RV). In Africa and Asia, domestic dogs are the main reservoirs of ''[[rabies virus]] [[infection]].'' Whereas, in the United States, racoons, foxes, skunks, coyotes, possums and bats are understood to be responsible for the spread of [[rabies virus]].The [[neuromuscular junction]] is the major site of entry into [[neurons]]. RV infects [[peripheral nerves]] and then reaches the [[CNS|central nervous system (CNS)]] via retrograde [[axonal]] transport''.'' The primary mechanism involved in the neuroinvasion of RV is trans-synaptic [[neuronal]] spread. RV infects [[Neuron|neurons]] and leads to the degeneration of the [[neuronal]] processes by disrupting [[Cytoskeleton|cytoskeletal]] integrity. [[Histopathologic]] evidence of rabies [[encephalomyelitis]] ([[inflammation]]) in [[brain]] [[Tissue (biology)|tissue]] and [[meninges]] includes, [[Mononuclear cells|mononuclear]] infiltration, [[Perivascular cell|perivascular]] cuffing of [[lymphocytes]] or [[polymorphonuclear cells]], [[lymphocytic]] foci, Babes nodules consisting of [[glial cells]] and [[Negri bodies]]. | ||
==Pathophysiology== | ==Pathophysiology== | ||
The [[organism]] causing rabies is called [[ | The [[organism]] causing rabies is called [[rabies virus|r''abies virus'' (RV)]], a negative-stranded [[RNA virus]] of the [[rhabdovirus]] family. Rabies is an acute [[encephalomyelitis]] that causes disease in the human host via two features associated with the ''[[rabies virus]]'' (RV):<ref name="pmid8301314">{{cite journal |vauthors=Mrak RE, Young L |title=Rabies encephalitis in humans: pathology, pathogenesis and pathophysiology |journal=J. Neuropathol. Exp. Neurol. |volume=53 |issue=1 |pages=1–10 |year=1994 |pmid=8301314 |doi= |url=}}</ref><ref name="pmid15119770">{{cite journal |vauthors=Lafon M |title=Subversive neuroinvasive strategy of rabies virus |journal=Arch. Virol. Suppl. |volume= |issue=18 |pages=149–59 |year=2004 |pmid=15119770 |doi= |url=}}</ref> | ||
* Neurotropism | * Neurotropism | ||
* Neuroinvasiveness | * Neuroinvasiveness | ||
| Line 13: | Line 13: | ||
=== Transmission === | === Transmission === | ||
'''Common route of tranmission''' | '''Common route of tranmission''' | ||
* Various carnivorous animal species have been identified as the source of ''[[ | * Various carnivorous animal species have been identified as the source of ''[[rabies virus]]'' (RV)<ref name="pmid7777317">{{cite journal |vauthors=Swanepoel R, Barnard BJ, Meredith CD, Bishop GC, Brückner GK, Foggin CM, Hübschle OJ |title=Rabies in southern Africa |journal=Onderstepoort J. Vet. Res. |volume=60 |issue=4 |pages=325–46 |year=1993 |pmid=7777317 |doi= |url=}}</ref><ref name="pmid10396757">{{cite journal |vauthors=Bingham J, Foggin CM, Wandeler AI, Hill FW |title=The epidemiology of rabies in Zimbabwe. 2. Rabies in jackals (Canis adustus and Canis mesomelas) |journal=Onderstepoort J. Vet. Res. |volume=66 |issue=1 |pages=11–23 |year=1999 |pmid=10396757 |doi= |url=}}</ref> | ||
* In Africa and Asia, domestic dogs are the main reservoirs of [[infection]] from '' | * In Africa and Asia, domestic dogs are the main reservoirs of [[infection]] from ''[[rabies virus]]''<ref name="urlwww.who.int">{{cite web |url=http://www.who.int/bulletin/volumes/83/5/360.pdf |title=www.who.int |format= |work= |accessdate=}}</ref> | ||
* In the United States, racoons, foxes, skunks, coyotes, possums and bats rather than dogs spread the [[infection]] through [[bites]]<ref name="urlCDC - Rabies Surveillance in the U.S.: Wild Animals - Rabies">{{cite web |url=https://www.cdc.gov/rabies/location/usa/surveillance/wild_animals.html |title=CDC - Rabies Surveillance in the U.S.: Wild Animals - Rabies |format= |work= |accessdate=}}</ref><ref>Constantine DG, Woodall DF. | * In the United States, racoons, foxes, skunks, coyotes, possums and bats rather than dogs spread the [[infection]] through [[bites]]<ref name="urlCDC - Rabies Surveillance in the U.S.: Wild Animals - Rabies">{{cite web |url=https://www.cdc.gov/rabies/location/usa/surveillance/wild_animals.html |title=CDC - Rabies Surveillance in the U.S.: Wild Animals - Rabies |format= |work= |accessdate=}}</ref><ref>Constantine DG, Woodall DF. | ||
Related Articles, Links | Related Articles, Links | ||
| Line 26: | Line 26: | ||
</ref> | </ref> | ||
* Three stages of rabies have been known to occurr in dogs. The first stage is a one to three day period characterized by behavioral changes and is known as the [[Prodrome|prodromal stage]]. The second stage is the excitative stage, which lasts three to four days. It is this stage that is often known as ''furious rabies'' due to the tendency of the affected dog to be hyper-reactive to external stimuli and [[bite]] at anything near. The third stage is the ''[[Paralysis|paralytic]] stage'' and is caused by damage to [[motor neuron]]s. Incoordination is seen due to rear [[Paralysis|limb paralysis]] and [[drooling]] and [[Dysphagia|difficulty swallowing]] is caused by [[paralysis]] of [[Facial muscles|facial]] and [[throat]] [[muscles]]. Death is usually caused by [[respiratory arrest]].<ref name="Ettinger_1995">{{cite book|author=Ettinger, Stephen J.;Feldman, Edward C.|title=Textbook of Veterinary Internal Medicine|edition=4th ed.|publisher=W.B. Saunders Company|year=1995|id=ISBN 0-7216-6795-3}}</ref> | * Three stages of rabies have been known to occurr in dogs. The first stage is a one to three day period characterized by behavioral changes and is known as the [[Prodrome|prodromal stage]]. The second stage is the excitative stage, which lasts three to four days. It is this stage that is often known as ''furious rabies'' due to the tendency of the affected dog to be hyper-reactive to external stimuli and [[bite]] at anything near. The third stage is the ''[[Paralysis|paralytic]] stage'' and is caused by damage to [[motor neuron]]s. Incoordination is seen due to rear [[Paralysis|limb paralysis]] and [[drooling]] and [[Dysphagia|difficulty swallowing]] is caused by [[paralysis]] of [[Facial muscles|facial]] and [[throat]] [[muscles]]. Death is usually caused by [[respiratory arrest]].<ref name="Ettinger_1995">{{cite book|author=Ettinger, Stephen J.;Feldman, Edward C.|title=Textbook of Veterinary Internal Medicine|edition=4th ed.|publisher=W.B. Saunders Company|year=1995|id=ISBN 0-7216-6795-3}}</ref> | ||
* Transmission of the ''[[ | * Transmission of the ''[[rabies virus]]'' starts when a human is bit by an animal harboring the virus in its [[salivary glands]]<ref>''The Merck manual of Medical Information. Second Home Edition'', (2003), p. 484.</ref> | ||
* The RV remains cell-free after initial [[inoculation]] | * The RV remains cell-free after initial [[inoculation]] so, rigorous [[wound]] cleaning may reduce the chances of [[infection]]<ref name="urlRabies | Clinical Infectious Diseases | Oxford Academic2">{{cite web |url=https://academic.oup.com/cid/article/30/1/4/323391/Rabies |title=Rabies | Clinical Infectious Diseases | Oxford Academic |format= |work= |accessdate=}}</ref> | ||
* RV infects [[peripheral nerves]] and then reaches the [[CNS|central nervous system (CNS)]] via retrograde [[axonal]] transport | * RV infects [[peripheral nerves]] and then reaches the [[CNS|central nervous system (CNS)]] via retrograde [[axonal]] transport | ||
[[Image:Rabies.jpg|center|The infectious path of rabies virus in a raccoon]]'''Less common routes of transmission''' | [[Image:Rabies.jpg|center|The infectious path of rabies virus in a raccoon]]'''Less common routes of transmission''' | ||
* Less common routes of transmission include:<ref name="urlwww.microbiologyresearch.org">{{cite web |url=http://www.microbiologyresearch.org/docserver/fulltext/jmm/55/6/785.pdf?expires=1506531826&id=id&accname=guest&checksum=353665C6666FEF02DA139F5B5AE0E35F |title=www.microbiologyresearch.org |format= |work= |accessdate=}}</ref><ref name="urlCDC - Transmission - Rabies">{{cite web |url=https://www.cdc.gov/rabies/transmission/index.html |title=CDC - Transmission - Rabies |format= |work= |accessdate=}}</ref><ref name="urlwww.microbiologyresearch.org2">{{cite web |url=http://www.microbiologyresearch.org/docserver/fulltext/jmm/55/6/785.pdf?expires=1506531826&id=id&accname=guest&checksum=353665C6666FEF02DA139F5B5AE0E35F |title=www.microbiologyresearch.org |format= |work= |accessdate=}}</ref> | * Less common routes of transmission of [[rabies virus]] include:<ref name="urlwww.microbiologyresearch.org">{{cite web |url=http://www.microbiologyresearch.org/docserver/fulltext/jmm/55/6/785.pdf?expires=1506531826&id=id&accname=guest&checksum=353665C6666FEF02DA139F5B5AE0E35F |title=www.microbiologyresearch.org |format= |work= |accessdate=}}</ref><ref name="urlCDC - Transmission - Rabies">{{cite web |url=https://www.cdc.gov/rabies/transmission/index.html |title=CDC - Transmission - Rabies |format= |work= |accessdate=}}</ref><ref name="urlwww.microbiologyresearch.org2">{{cite web |url=http://www.microbiologyresearch.org/docserver/fulltext/jmm/55/6/785.pdf?expires=1506531826&id=id&accname=guest&checksum=353665C6666FEF02DA139F5B5AE0E35F |title=www.microbiologyresearch.org |format= |work= |accessdate=}}</ref> | ||
** [[Contamination]] of [[mucous membranes]] (i.e., [[Eye|eyes]], [[nose]], [[mouth]]) | ** [[Contamination]] of [[mucous membranes]] (i.e., [[Eye|eyes]], [[nose]], [[mouth]]) | ||
** [[Aerosol]] transmission | ** [[Aerosol]] transmission | ||
| Line 37: | Line 37: | ||
===Virology=== | ===Virology=== | ||
The [[ | The [[rabies virus|rabies virus (RV)]] belongs to the [[genus]] ''[[Lyssavirus]]''. This [[genus]] of [[RNA virus]]es also includes the Aravan virus, [[Australian bat lyssavirus]], [[Duvenhage virus]], European bat lyssavirus 1, European bat lyssavirus 2, Irkut virus, Khujand virus, [[Lagos bat virus]], [[Mokola virus]] and West Caucasian bat [[virus]]. [[Lyssavirus|Lyssaviruses]] have helical symmetry, so their [[infectious]] particles are approximately cylindrical in shape. | ||
* The virus has a bullet-like shape with a length of about 180 nm and a cross-sectional diameter of about 75 nm<ref name="urlRhabdoviruses: Rabies Virus - Medical Microbiology - NCBI Bookshelf">{{cite web |url=https://www.ncbi.nlm.nih.gov/books/NBK8618/ |title=Rhabdoviruses: Rabies Virus - Medical Microbiology - NCBI Bookshelf |format= |work= |accessdate=}}</ref><ref name="pmid9880004">{{cite journal |vauthors=Iseni F, Barge A, Baudin F, Blondel D, Ruigrok RW |title=Characterization of rabies virus nucleocapsids and recombinant nucleocapsid-like structures |journal=J. Gen. Virol. |volume=79 ( Pt 12) |issue= |pages=2909–19 |year=1998 |pmid=9880004 |doi=10.1099/0022-1317-79-12-2909 |url=}}</ref> | * The virus has a bullet-like shape with a length of about 180 nm and a cross-sectional diameter of about 75 nm<ref name="urlRhabdoviruses: Rabies Virus - Medical Microbiology - NCBI Bookshelf">{{cite web |url=https://www.ncbi.nlm.nih.gov/books/NBK8618/ |title=Rhabdoviruses: Rabies Virus - Medical Microbiology - NCBI Bookshelf |format= |work= |accessdate=}}</ref><ref name="pmid9880004">{{cite journal |vauthors=Iseni F, Barge A, Baudin F, Blondel D, Ruigrok RW |title=Characterization of rabies virus nucleocapsids and recombinant nucleocapsid-like structures |journal=J. Gen. Virol. |volume=79 ( Pt 12) |issue= |pages=2909–19 |year=1998 |pmid=9880004 |doi=10.1099/0022-1317-79-12-2909 |url=}}</ref> | ||
| Line 51: | Line 51: | ||
=== Pathogenesis === | === Pathogenesis === | ||
'''Incubation period and eclipse phase''' | '''Incubation period and eclipse phase''' | ||
* The incubation period may vary from a few days to several years, but is typically 1 to 3 months<ref name="pmid9224533">{{cite journal |vauthors=Charlton KM, Nadin-Davis S, Casey GA, Wandeler AI |title=The long incubation period in rabies: delayed progression of infection in muscle at the site of exposure |journal=Acta Neuropathol. |volume=94 |issue=1 |pages=73–7 |year=1997 |pmid=9224533 |doi= |url=}}</ref><ref name="urlRabies | Clinical Infectious Diseases | Oxford Academic">{{cite web |url=https://academic.oup.com/cid/article/30/1/4/323391/Rabies |title=Rabies | Clinical Infectious Diseases | Oxford Academic |format= |work= |accessdate=}}</ref> | * The [[incubation period]] may vary from a few days to several years, but is typically 1 to 3 months<ref name="pmid9224533">{{cite journal |vauthors=Charlton KM, Nadin-Davis S, Casey GA, Wandeler AI |title=The long incubation period in rabies: delayed progression of infection in muscle at the site of exposure |journal=Acta Neuropathol. |volume=94 |issue=1 |pages=73–7 |year=1997 |pmid=9224533 |doi= |url=}}</ref><ref name="urlRabies | Clinical Infectious Diseases | Oxford Academic">{{cite web |url=https://academic.oup.com/cid/article/30/1/4/323391/Rabies |title=Rabies | Clinical Infectious Diseases | Oxford Academic |format= |work= |accessdate=}}</ref> | ||
* After gaining entry into human host, the [[RV]] enters into an eclipse phase, during which, the host [[immune]] defenses may confer [[cell-mediated immunity]] against [[viral infection]] because RV is a good [[antigen]]<ref name="urlCDC - Doctors: Transmission - Rabies">{{cite web |url=https://www.cdc.gov/rabies/specific_groups/doctors/transmission.html |title=CDC - Doctors: Transmission - Rabies |format= |work= |accessdate=}}</ref><ref name="pmid21601053">{{cite journal |vauthors=Israsena N, Mahavihakanont A, Hemachudha T |title=Rabies virus infection and microRNAs |journal=Adv. Virus Res. |volume=79 |issue= |pages=329–44 |year=2011 |pmid=21601053 |doi=10.1016/B978-0-12-387040-7.00015-9 |url=}}</ref> | * After gaining entry into human host, the [[RV]] enters into an eclipse phase, during which, the host [[immune]] defenses may confer [[cell-mediated immunity]] against [[viral infection]] because RV is a good [[antigen]]<ref name="urlCDC - Doctors: Transmission - Rabies">{{cite web |url=https://www.cdc.gov/rabies/specific_groups/doctors/transmission.html |title=CDC - Doctors: Transmission - Rabies |format= |work= |accessdate=}}</ref><ref name="pmid21601053">{{cite journal |vauthors=Israsena N, Mahavihakanont A, Hemachudha T |title=Rabies virus infection and microRNAs |journal=Adv. Virus Res. |volume=79 |issue= |pages=329–44 |year=2011 |pmid=21601053 |doi=10.1016/B978-0-12-387040-7.00015-9 |url=}}</ref> | ||
'''Neuromuscular junction invasion''' | '''Neuromuscular junction invasion''' | ||
* The [[neuromuscular junction]] is the major site of entry into [[neurons]]<ref name="pmid3890406">{{cite journal |vauthors=Burrage TG, Tignor GH, Smith AL |title=Rabies virus binding at neuromuscular junctions |journal=Virus Res. |volume=2 |issue=3 |pages=273–89 |year=1985 |pmid=3890406 |doi= |url=}}</ref> | * The [[neuromuscular junction]] is the major site of entry into [[neurons]]<ref name="pmid3890406">{{cite journal |vauthors=Burrage TG, Tignor GH, Smith AL |title=Rabies virus binding at neuromuscular junctions |journal=Virus Res. |volume=2 |issue=3 |pages=273–89 |year=1985 |pmid=3890406 |doi= |url=}}</ref> | ||
* The RV uses the [[acetylcholine receptors]] and other receptors such as the neutral [[cell adhesion]] [[molecule]] (NCAM) to gain entry into the [[neuron]] via [[endocytosis]]<ref name="pmid9696812">{{cite journal |vauthors=Thoulouze MI, Lafage M, Schachner M, Hartmann U, Cremer H, Lafon M |title=The neural cell adhesion molecule is a receptor for rabies virus |journal=J. Virol. |volume=72 |issue=9 |pages=7181–90 |year=1998 |pmid=9696812 |pmc=109940 |doi= |url=}}</ref> | * The RV uses the [[acetylcholine receptors]] and other [[receptors]] such as the neutral [[cell adhesion]] [[molecule]] (NCAM) to gain entry into the [[neuron]] via [[endocytosis]]<ref name="pmid9696812">{{cite journal |vauthors=Thoulouze MI, Lafage M, Schachner M, Hartmann U, Cremer H, Lafon M |title=The neural cell adhesion molecule is a receptor for rabies virus |journal=J. Virol. |volume=72 |issue=9 |pages=7181–90 |year=1998 |pmid=9696812 |pmc=109940 |doi= |url=}}</ref> | ||
* Fusion of the [[viral]] membrane with [[Endosomal membrane|endosomal membranes]] liberates the [[viral]] [[nucleocapsid]] into the [[cytosol]], where [[transcription]] and [[replication]] occur<ref name="pmid15885837">{{cite journal |vauthors=Finke S, Conzelmann KK |title=Replication strategies of rabies virus |journal=Virus Res. |volume=111 |issue=2 |pages=120–31 |year=2005 |pmid=15885837 |doi=10.1016/j.virusres.2005.04.004 |url=}}</ref> | * Fusion of the [[viral]] membrane with [[Endosomal membrane|endosomal membranes]] liberates the [[viral]] [[nucleocapsid]] into the [[cytosol]], where [[transcription]] and [[replication]] occur<ref name="pmid15885837">{{cite journal |vauthors=Finke S, Conzelmann KK |title=Replication strategies of rabies virus |journal=Virus Res. |volume=111 |issue=2 |pages=120–31 |year=2005 |pmid=15885837 |doi=10.1016/j.virusres.2005.04.004 |url=}}</ref> | ||
'''Inter-neuronal spread''' | '''Inter-neuronal spread''' | ||
* The main mechanism involved in the neuroinvasion of RV is trans-synaptic [[neuronal]] spread | * The main mechanism involved in the neuroinvasion of RV is trans-synaptic [[neuronal]] spread | ||
* The following [[proteins]] lead to the spread of [[virus]] between the [[neurons]], once the virus gains entry into the [[body]]:<ref name="pmid15981467">{{cite journal |vauthors=Dietzschold B, Schnell M, Koprowski H |title=Pathogenesis of rabies |journal=Curr. Top. Microbiol. Immunol. |volume=292 |issue= |pages=45–56 |year=2005 |pmid=15981467 |doi= |url=}}</ref> | * The following [[proteins]] lead to the spread of [[virus]] between the [[neurons]], once the [[virus]] gains entry into the [[body]]:<ref name="pmid15981467">{{cite journal |vauthors=Dietzschold B, Schnell M, Koprowski H |title=Pathogenesis of rabies |journal=Curr. Top. Microbiol. Immunol. |volume=292 |issue= |pages=45–56 |year=2005 |pmid=15981467 |doi= |url=}}</ref><ref name="urlRabies Virus P Protein Interacts with STAT1 and Inhibits Interferon Signal Transduction Pathways">{{cite web |url=http://jvi.asm.org/content/79/22/14411.abstract |title=Rabies Virus P Protein Interacts with STAT1 and Inhibits Interferon Signal Transduction Pathways |format= |work= |accessdate=}}</ref> | ||
** [[Rabies virus]] [[G protein]]: RV to spread from the post-synaptic site to the pre-synaptic site | ** [[Rabies virus]] [[G protein]] ([[glycoprotein]]): RV to spread from the [[post-synaptic]] site to the pre-synaptic site | ||
** Rabies virus P protein: important determinant of retrograde transport of the [[virus]] within [[axons]] | ** [[Rabies virus]] P protein (a [[Cofactor (biochemistry)|cofactor]] for [[RNA]] [[polymerase]]): important determinant of retrograde transport of the [[virus]] within [[axons]] | ||
'''CNS invasion''' | '''CNS invasion''' | ||
* Trans-synaptic [[neuronal]] spread leads to spread of [[infection]] to the [[CNS]] from the [[peripheral nerves]] | * Trans-synaptic [[neuronal]] spread leads to spread of [[infection]] to the [[CNS]] from the [[peripheral nerves]] | ||
* RV forms [[cytoplasmic]] [[inclusion bodies]] called [[Negri bodies]] in the [[neurons]], which are composed of the [[viral]] N and P proteins (all [[viral]] [[RNA|RNAs]] [[genome]], antigenome, and every [[mRNA]] have been known to be found inside the [[inclusion bodies]]- suggesting that they play a role in [[viral replication]] and life cycle)<ref name="pmid19494013">{{cite journal |vauthors=Lahaye X, Vidy A, Pomier C, Obiang L, Harper F, Gaudin Y, Blondel D |title=Functional characterization of Negri bodies (NBs) in rabies virus-infected cells: Evidence that NBs are sites of viral transcription and replication |journal=J. Virol. |volume=83 |issue=16 |pages=7948–58 |year=2009 |pmid=19494013 |pmc=2715764 |doi=10.1128/JVI.00554-09 |url=}}</ref> | * RV forms [[cytoplasmic]] [[inclusion bodies]] called [[Negri bodies]] in the [[neurons]], which are composed of the [[viral]] N and P proteins (all [[viral]] [[RNA|RNAs]] [[genome]], antigenome, and every [[mRNA]] have been known to be found inside the [[inclusion bodies]]- suggesting that they play a role in [[viral replication]] and life cycle)<ref name="pmid19494013">{{cite journal |vauthors=Lahaye X, Vidy A, Pomier C, Obiang L, Harper F, Gaudin Y, Blondel D |title=Functional characterization of Negri bodies (NBs) in rabies virus-infected cells: Evidence that NBs are sites of viral transcription and replication |journal=J. Virol. |volume=83 |issue=16 |pages=7948–58 |year=2009 |pmid=19494013 |pmc=2715764 |doi=10.1128/JVI.00554-09 |url=}}</ref> | ||
* RV infects [[neurons]] and leads to [[Degeneration (medical)|degeneration]] of the [[neuronal]] processes by disrupting [[cytoskeletal]] integrity<ref name="pmid16014967">{{cite journal |vauthors=Li XQ, Sarmento L, Fu ZF |title=Degeneration of neuronal processes after infection with pathogenic, but not attenuated, rabies viruses |journal=J. Virol. |volume=79 |issue=15 |pages=10063–8 |year=2005 |pmid=16014967 |pmc=1181611 |doi=10.1128/JVI.79.15.10063-10068.2005 |url=}}</ref> | * RV infects [[neurons]] and leads to [[Degeneration (medical)|degeneration]] of the [[neuronal]] processes by disrupting [[cytoskeletal]] integrity<ref name="pmid16014967">{{cite journal |vauthors=Li XQ, Sarmento L, Fu ZF |title=Degeneration of neuronal processes after infection with pathogenic, but not attenuated, rabies viruses |journal=J. Virol. |volume=79 |issue=15 |pages=10063–8 |year=2005 |pmid=16014967 |pmc=1181611 |doi=10.1128/JVI.79.15.10063-10068.2005 |url=}}</ref> | ||
* The [[hypothalamus]] | * The [[hypothalamus]] is understood to be affected most severely by [[Rabies virus|RV]] [[infection]]<ref name="pmid11115243">{{cite journal |vauthors=Pleasure SJ, Fischbein NJ |title=Correlation of clinical and neuroimaging findings in a case of rabies encephalitis |journal=Arch. Neurol. |volume=57 |issue=12 |pages=1765–9 |year=2000 |pmid=11115243 |doi= |url=}}</ref> | ||
==Microscopic Pathology== | ==Microscopic Pathology== | ||
[[Histologic]] examination of [[biopsy]] or [[autopsy]] [[tissues]] is occasionally useful in diagnosing unsuspected cases of rabies that have not been tested by routine methods. When [[brain tissue]] from rabies virus-infected animals are stained with a histologic stain, such as [[hematoxylin]] and [[eosin]], evidence of [[encephalomyelitis]] may be recognized. [[Histopathologic]] evidence of rabies encephalomyelitis ([[inflammation]]) in [[brain]] [[Tissue (biology)|tissue]] and [[meninges]] includes the following: | [[Histologic]] examination of [[biopsy]] or [[autopsy]] [[tissues]] is occasionally useful in diagnosing unsuspected cases of rabies that have not been tested by routine methods. When [[brain tissue]] from rabies virus-infected animals are stained with a histologic stain, such as [[hematoxylin]] and [[eosin]], evidence of [[encephalomyelitis]] may be recognized. [[Histopathologic]] evidence of rabies encephalomyelitis ([[inflammation]]) in [[brain]] [[Tissue (biology)|tissue]] and [[meninges]] includes the following:<ref name="pmid6176396">{{cite journal |vauthors=Théodoridès J |title=[Histological research on rabies in the 19th century] |language=French |journal=Clio Med |volume=16 |issue=2-3 |pages=83–92 |year=1981 |pmid=6176396 |doi= |url=}}</ref><ref name="pmid8804019">{{cite journal |vauthors=Kristensson K, Dastur DK, Manghani DK, Tsiang H, Bentivoglio M |title=Rabies: interactions between neurons and viruses. A review of the history of Negri inclusion bodies |journal=Neuropathol. Appl. Neurobiol. |volume=22 |issue=3 |pages=179–87 |year=1996 |pmid=8804019 |doi= |url=}}</ref><ref name="pmid15956158">{{cite journal |vauthors=Burton EC, Burns DK, Opatowsky MJ, El-Feky WH, Fischbach B, Melton L, Sanchez E, Randall H, Watkins DL, Chang J, Klintmalm G |title=Rabies encephalomyelitis: clinical, neuroradiological, and pathological findings in 4 transplant recipients |journal=Arch. Neurol. |volume=62 |issue=6 |pages=873–82 |year=2005 |pmid=15956158 |doi=10.1001/archneur.62.6.873 |url=}}</ref><ref name="pmid19494013">{{cite journal |vauthors=Lahaye X, Vidy A, Pomier C, Obiang L, Harper F, Gaudin Y, Blondel D |title=Functional characterization of Negri bodies (NBs) in rabies virus-infected cells: Evidence that NBs are sites of viral transcription and replication |journal=J. Virol. |volume=83 |issue=16 |pages=7948–58 |year=2009 |pmid=19494013 |pmc=2715764 |doi=10.1128/JVI.00554-09 |url=}}</ref> | ||
#[[Mononuclear cell|Mononuclear]] [[Infiltration (medical)|infiltration]] | #[[Mononuclear cell|Mononuclear]] [[Infiltration (medical)|infiltration]] | ||
| Line 80: | Line 80: | ||
{{#ev:youtube|NP5CYphae5Y}} | {{#ev:youtube|NP5CYphae5Y}} | ||
==References== | |||
{{Reflist|2}} | {{Reflist|2}} | ||
{{WH}} | |||
{{WS}} | |||
[[Category:Disease]] | [[Category:Disease]] | ||
[[Category:Viral diseases]] | [[Category:Viral diseases]] | ||
[[Category:Mononegavirales]] | [[Category:Mononegavirales]] | ||
| Line 90: | Line 92: | ||
[[Category:Emergency medicine]] | [[Category:Emergency medicine]] | ||
[[Category:Intensive care medicine]] | [[Category:Intensive care medicine]] | ||
[[Category:Infectious disease]] | |||
[[Category:Medicine]] | |||
Latest revision as of 23:56, 29 July 2020
|
Rabies Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Rabies pathophysiology On the Web |
|
American Roentgen Ray Society Images of Rabies pathophysiology |
|
Risk calculators and risk factors for Rabies pathophysiology |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Syed Hassan A. Kazmi BSc, MD [2]
Overview
The rabies virus is categorized as a Lyssavirus. The molecular biology of rabies consists of bullet shaped virus with helical symmetry that has a length of approximately 180 nm. Rabies typically has its greatest effect on the brain. Rabies is typically defined by encephalitis and myelitis. Various carnivorous animal species have been identified as the source of rabies virus (RV). In Africa and Asia, domestic dogs are the main reservoirs of rabies virus infection. Whereas, in the United States, racoons, foxes, skunks, coyotes, possums and bats are understood to be responsible for the spread of rabies virus.The neuromuscular junction is the major site of entry into neurons. RV infects peripheral nerves and then reaches the central nervous system (CNS) via retrograde axonal transport. The primary mechanism involved in the neuroinvasion of RV is trans-synaptic neuronal spread. RV infects neurons and leads to the degeneration of the neuronal processes by disrupting cytoskeletal integrity. Histopathologic evidence of rabies encephalomyelitis (inflammation) in brain tissue and meninges includes, mononuclear infiltration, perivascular cuffing of lymphocytes or polymorphonuclear cells, lymphocytic foci, Babes nodules consisting of glial cells and Negri bodies.
Pathophysiology
The organism causing rabies is called rabies virus (RV), a negative-stranded RNA virus of the rhabdovirus family. Rabies is an acute encephalomyelitis that causes disease in the human host via two features associated with the rabies virus (RV):[1][2]
- Neurotropism
- Neuroinvasiveness
Transmission
Common route of tranmission
- Various carnivorous animal species have been identified as the source of rabies virus (RV)[3][4]
- In Africa and Asia, domestic dogs are the main reservoirs of infection from rabies virus[5]
- In the United States, racoons, foxes, skunks, coyotes, possums and bats rather than dogs spread the infection through bites[6][7][8][9]
- Three stages of rabies have been known to occurr in dogs. The first stage is a one to three day period characterized by behavioral changes and is known as the prodromal stage. The second stage is the excitative stage, which lasts three to four days. It is this stage that is often known as furious rabies due to the tendency of the affected dog to be hyper-reactive to external stimuli and bite at anything near. The third stage is the paralytic stage and is caused by damage to motor neurons. Incoordination is seen due to rear limb paralysis and drooling and difficulty swallowing is caused by paralysis of facial and throat muscles. Death is usually caused by respiratory arrest.[10]
- Transmission of the rabies virus starts when a human is bit by an animal harboring the virus in its salivary glands[11]
- The RV remains cell-free after initial inoculation so, rigorous wound cleaning may reduce the chances of infection[12]
- RV infects peripheral nerves and then reaches the central nervous system (CNS) via retrograde axonal transport
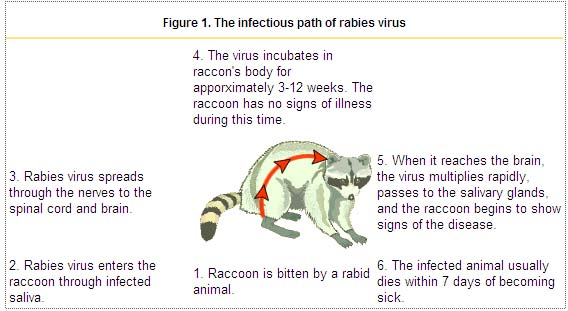
Less common routes of transmission
- Less common routes of transmission of rabies virus include:[13][14][15]
- Contamination of mucous membranes (i.e., eyes, nose, mouth)
- Aerosol transmission
- Corneal and other organ transplantation from infected donor
Virology
The rabies virus (RV) belongs to the genus Lyssavirus. This genus of RNA viruses also includes the Aravan virus, Australian bat lyssavirus, Duvenhage virus, European bat lyssavirus 1, European bat lyssavirus 2, Irkut virus, Khujand virus, Lagos bat virus, Mokola virus and West Caucasian bat virus. Lyssaviruses have helical symmetry, so their infectious particles are approximately cylindrical in shape.
- The virus has a bullet-like shape with a length of about 180 nm and a cross-sectional diameter of about 75 nm[16][17]
- One end is rounded or conical and the other end is planar or concave[18]
- The lipoprotein envelope carries knob-like spikes composed of Glycoprotein G. Spikes do not cover the planar end of the virion (virus particle)[19]
- Beneath the envelope is the membrane or matrix (M) protein layer which may be invaginated at the planar end. The core of the virion consists of helically arranged ribonucleoprotein[20]
- The genome is unsegmented linear antisense RNA. Also present in the nucleocapsid are RNA dependent RNA transcriptase and some structural proteins
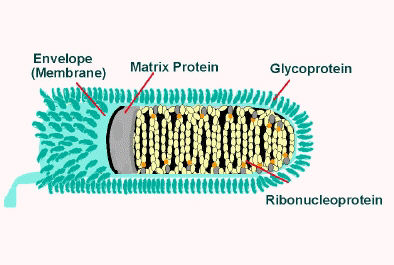
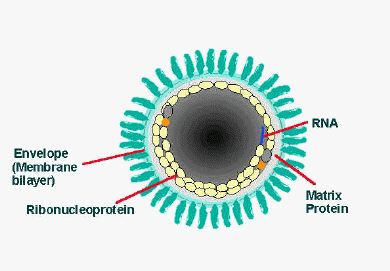
Longitudinal and cross-sectional schematic view of rabies virus
Pathogenesis
Incubation period and eclipse phase
- The incubation period may vary from a few days to several years, but is typically 1 to 3 months[21][22]
- After gaining entry into human host, the RV enters into an eclipse phase, during which, the host immune defenses may confer cell-mediated immunity against viral infection because RV is a good antigen[23][24]
Neuromuscular junction invasion
- The neuromuscular junction is the major site of entry into neurons[25]
- The RV uses the acetylcholine receptors and other receptors such as the neutral cell adhesion molecule (NCAM) to gain entry into the neuron via endocytosis[26]
- Fusion of the viral membrane with endosomal membranes liberates the viral nucleocapsid into the cytosol, where transcription and replication occur[27]
Inter-neuronal spread
- The main mechanism involved in the neuroinvasion of RV is trans-synaptic neuronal spread
- The following proteins lead to the spread of virus between the neurons, once the virus gains entry into the body:[28][29]
- Rabies virus G protein (glycoprotein): RV to spread from the post-synaptic site to the pre-synaptic site
- Rabies virus P protein (a cofactor for RNA polymerase): important determinant of retrograde transport of the virus within axons
CNS invasion
- Trans-synaptic neuronal spread leads to spread of infection to the CNS from the peripheral nerves
- RV forms cytoplasmic inclusion bodies called Negri bodies in the neurons, which are composed of the viral N and P proteins (all viral RNAs genome, antigenome, and every mRNA have been known to be found inside the inclusion bodies- suggesting that they play a role in viral replication and life cycle)[30]
- RV infects neurons and leads to degeneration of the neuronal processes by disrupting cytoskeletal integrity[31]
- The hypothalamus is understood to be affected most severely by RV infection[32]
Microscopic Pathology
Histologic examination of biopsy or autopsy tissues is occasionally useful in diagnosing unsuspected cases of rabies that have not been tested by routine methods. When brain tissue from rabies virus-infected animals are stained with a histologic stain, such as hematoxylin and eosin, evidence of encephalomyelitis may be recognized. Histopathologic evidence of rabies encephalomyelitis (inflammation) in brain tissue and meninges includes the following:[33][34][35][30]
- Mononuclear infiltration
- Perivascular cuffing of lymphocytes or polymorphonuclear cells
- Lymphocytic foci
- Babes nodules consisting of glial cells
- Negri bodies
{{#ev:youtube|NP5CYphae5Y}}
References
- ↑ Mrak RE, Young L (1994). "Rabies encephalitis in humans: pathology, pathogenesis and pathophysiology". J. Neuropathol. Exp. Neurol. 53 (1): 1–10. PMID 8301314.
- ↑ Lafon M (2004). "Subversive neuroinvasive strategy of rabies virus". Arch. Virol. Suppl. (18): 149–59. PMID 15119770.
- ↑ Swanepoel R, Barnard BJ, Meredith CD, Bishop GC, Brückner GK, Foggin CM, Hübschle OJ (1993). "Rabies in southern Africa". Onderstepoort J. Vet. Res. 60 (4): 325–46. PMID 7777317.
- ↑ Bingham J, Foggin CM, Wandeler AI, Hill FW (1999). "The epidemiology of rabies in Zimbabwe. 2. Rabies in jackals (Canis adustus and Canis mesomelas)". Onderstepoort J. Vet. Res. 66 (1): 11–23. PMID 10396757.
- ↑ "www.who.int" (PDF).
- ↑ "CDC - Rabies Surveillance in the U.S.: Wild Animals - Rabies".
- ↑ Constantine DG, Woodall DF. Related Articles, Links Transmission experiments with bat rabies isolates: reactions of certain Carnivora, possum, rodents, and bats to rabies virus of red bat origin when exposed by bat bite or by intrasmuscular inoculation. Am J Vet Res. 1966 Jan;27(116):24-32. No abstract available. PMID: 5913032 [PubMed - indexed for MEDLINE]
- ↑ Constantine DG 1967 Rabies transmission by air in bat caves. US Pub Health Serv, Publ. 1617
- ↑ 1: Am J Vet Res. 1960 May;21:507-10.Links Resistance of the opossum to rabies virus.BEAMER PD, MOHR CO, BARR TR. PMID: 13797881 [PubMed - indexed for MEDLINE]
- ↑ Ettinger, Stephen J.;Feldman, Edward C. (1995). Textbook of Veterinary Internal Medicine (4th ed. ed.). W.B. Saunders Company. ISBN 0-7216-6795-3.
- ↑ The Merck manual of Medical Information. Second Home Edition, (2003), p. 484.
- ↑ "Rabies | Clinical Infectious Diseases | Oxford Academic".
- ↑ "www.microbiologyresearch.org" (PDF).
- ↑ "CDC - Transmission - Rabies".
- ↑ "www.microbiologyresearch.org" (PDF).
- ↑ "Rhabdoviruses: Rabies Virus - Medical Microbiology - NCBI Bookshelf".
- ↑ Iseni F, Barge A, Baudin F, Blondel D, Ruigrok RW (1998). "Characterization of rabies virus nucleocapsids and recombinant nucleocapsid-like structures". J. Gen. Virol. 79 ( Pt 12): 2909–19. doi:10.1099/0022-1317-79-12-2909. PMID 9880004.
- ↑ Hummeler K, Koprowski H, Wiktor TJ (1967). "Structure and development of rabies virus in tissue culture". J. Virol. 1 (1): 152–70. PMC 375516. PMID 4918232.
- ↑ Gaudin Y, Ruigrok RW, Tuffereau C, Knossow M, Flamand A (1992). "Rabies virus glycoprotein is a trimer". Virology. 187 (2): 627–32. PMID 1546457.
- ↑ Mebatsion T, Weiland F, Conzelmann KK (1999). "Matrix protein of rabies virus is responsible for the assembly and budding of bullet-shaped particles and interacts with the transmembrane spike glycoprotein G". J. Virol. 73 (1): 242–50. PMC 103828. PMID 9847327.
- ↑ Charlton KM, Nadin-Davis S, Casey GA, Wandeler AI (1997). "The long incubation period in rabies: delayed progression of infection in muscle at the site of exposure". Acta Neuropathol. 94 (1): 73–7. PMID 9224533.
- ↑ "Rabies | Clinical Infectious Diseases | Oxford Academic".
- ↑ "CDC - Doctors: Transmission - Rabies".
- ↑ Israsena N, Mahavihakanont A, Hemachudha T (2011). "Rabies virus infection and microRNAs". Adv. Virus Res. 79: 329–44. doi:10.1016/B978-0-12-387040-7.00015-9. PMID 21601053.
- ↑ Burrage TG, Tignor GH, Smith AL (1985). "Rabies virus binding at neuromuscular junctions". Virus Res. 2 (3): 273–89. PMID 3890406.
- ↑ Thoulouze MI, Lafage M, Schachner M, Hartmann U, Cremer H, Lafon M (1998). "The neural cell adhesion molecule is a receptor for rabies virus". J. Virol. 72 (9): 7181–90. PMC 109940. PMID 9696812.
- ↑ Finke S, Conzelmann KK (2005). "Replication strategies of rabies virus". Virus Res. 111 (2): 120–31. doi:10.1016/j.virusres.2005.04.004. PMID 15885837.
- ↑ Dietzschold B, Schnell M, Koprowski H (2005). "Pathogenesis of rabies". Curr. Top. Microbiol. Immunol. 292: 45–56. PMID 15981467.
- ↑ "Rabies Virus P Protein Interacts with STAT1 and Inhibits Interferon Signal Transduction Pathways".
- ↑ 30.0 30.1 Lahaye X, Vidy A, Pomier C, Obiang L, Harper F, Gaudin Y, Blondel D (2009). "Functional characterization of Negri bodies (NBs) in rabies virus-infected cells: Evidence that NBs are sites of viral transcription and replication". J. Virol. 83 (16): 7948–58. doi:10.1128/JVI.00554-09. PMC 2715764. PMID 19494013.
- ↑ Li XQ, Sarmento L, Fu ZF (2005). "Degeneration of neuronal processes after infection with pathogenic, but not attenuated, rabies viruses". J. Virol. 79 (15): 10063–8. doi:10.1128/JVI.79.15.10063-10068.2005. PMC 1181611. PMID 16014967.
- ↑ Pleasure SJ, Fischbein NJ (2000). "Correlation of clinical and neuroimaging findings in a case of rabies encephalitis". Arch. Neurol. 57 (12): 1765–9. PMID 11115243.
- ↑ Théodoridès J (1981). "[Histological research on rabies in the 19th century]". Clio Med (in French). 16 (2–3): 83–92. PMID 6176396.
- ↑ Kristensson K, Dastur DK, Manghani DK, Tsiang H, Bentivoglio M (1996). "Rabies: interactions between neurons and viruses. A review of the history of Negri inclusion bodies". Neuropathol. Appl. Neurobiol. 22 (3): 179–87. PMID 8804019.
- ↑ Burton EC, Burns DK, Opatowsky MJ, El-Feky WH, Fischbach B, Melton L, Sanchez E, Randall H, Watkins DL, Chang J, Klintmalm G (2005). "Rabies encephalomyelitis: clinical, neuroradiological, and pathological findings in 4 transplant recipients". Arch. Neurol. 62 (6): 873–82. doi:10.1001/archneur.62.6.873. PMID 15956158.