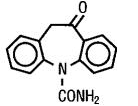
Oxcarbazepine
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Vignesh Ponnusamy, M.B.B.S. [2]
WikiDoc MAKES NO GUARANTEE OF VALIDITY. WikiDoc is not a professional health care provider, nor is it a suitable replacement for a licensed healthcare provider. WikiDoc is intended to be an educational tool, not a tool for any form of healthcare delivery. The educational content on WikiDoc drug pages is based upon the FDA package insert, National Library of Medicine content and practice guidelines / consensus statements. WikiDoc does not promote the administration of any medication or device that is not consistent with its labeling. Please read our full disclaimer here.
Overview
Oxcarbazepine is an antiepileptic drug that is FDA approved for the treatment of partial seizures. Common adverse reactions include dizziness, somnolence, diplopia, fatigue, nausea, vomiting, ataxia, abnormal vision, abdominal pain, tremor, dyspepsia, abnormal gait.
Adult Indications and Dosage
FDA-Labeled Indications and Dosage (Adult)
Partial Seizures
- Adjunctive Therapy for Adults
- Treatment with Oxcarbazepine should be initiated with a dose of 600 mg/day, given in a twice-a-day regimen. If clinically indicated, the dose may be increased by a maximum of 600 mg/day at approximately weekly intervals; the recommended daily dose is 1200 mg/day. Daily doses above 1200 mg/day show somewhat greater effectiveness in controlled trials, but most patients were not able to tolerate the 2400 mg/day dose, primarily because of CNS effects. It is recommended that the patient be observed closely and plasma levels of the concomitant AEDs be monitored during the period of Oxcarbazepine titration, as these plasma levels may be altered, especially at Oxcarbazepine doses greater than 1200 mg/day.
- Conversion to Monotherapy for Adults
- Patients receiving concomitant AEDs may be converted to monotherapy by initiating treatment with Oxcarbazepine at 600 mg/day (given in a twice-a-day regimen) while simultaneously initiating the reduction of the dose of the concomitant AEDs. The concomitant AEDs should be completely withdrawn over 3-6 weeks, while the maximum dose of Oxcarbazepine should be reached in about 2-4 weeks. Oxcarbazepine may be increased as clinically indicated by a maximum increment of 600 mg/day at approximately weekly intervals to achieve the recommended daily dose of 2400 mg/day. A daily dose of 1200 mg/day has been shown in one study to be effective in patients in whom monotherapy has been initiated with Oxcarbazepine. Patients should be observed closely during this transition phase.
- Initiation of Monotherapy for Adults
- Patients not currently being treated with AEDs may have monotherapy initiated with Oxcarbazepine. In these patients, Oxcarbazepine should be initiated at a dose of 600 mg/day (given in a twice-a-day regimen); the dose should be increased by 300 mg/day every third day to a dose of 1200 mg/day. Controlled trials in these patients examined the effectiveness of a 1200 mg/day dose; a dose of 2400 mg/day has been shown to be effective in patients converted from other AEDs to Oxcarbazepine monotherapy
Off-Label Use and Dosage (Adult)
Guideline-Supported Use
There is limited information regarding Off-Label Guideline-Supported Use of Oxcarbazepine in adult patients.
Non–Guideline-Supported Use
There is limited information regarding Off-Label Non–Guideline-Supported Use of Oxcarbazepine in adult patients.
Pediatric Indications and Dosage
FDA-Labeled Indications and Dosage (Pediatric)
Partial Seizures
- Adjunctive Therapy for Pediatric Patients (Aged 2-16 Years)
- In pediatric patients aged 4-16 years, treatment should be initiated at a daily dose of 8-10 mg/kg generally not to exceed 600 mg/day, given in a twice-a-day regimen. The target maintenance dose of Oxcarbazepine should be achieved over two weeks, and is dependent upon patient weight, according to the following chart:
- 20-29 kg - 900 mg/day
- 29.1-39 kg - 1200 mg/day
- >39 kg – 1800 mg/day
- In pediatric patients aged 4-16 years, treatment should be initiated at a daily dose of 8-10 mg/kg generally not to exceed 600 mg/day, given in a twice-a-day regimen. The target maintenance dose of Oxcarbazepine should be achieved over two weeks, and is dependent upon patient weight, according to the following chart:
- In the clinical trial, in which the intention was to reach these target doses, the median daily dose was 31 mg/kg with a range of 6-51 mg/kg.
- In pediatric patients aged 2-<4 years, treatment should also be initiated at a daily dose of 8-10 mg/kg generally not to exceed 600 mg/day, given in a twice-a-day regimen. For patients under 20 kg, a starting dose of 16-20 mg/kg may be considered. The maximum maintenance dose of Oxcarbazepine should be achieved over 2-4 weeks and should not exceed 60 mg/kg/day in a twice-a-day regimen.
- In the clinical trial in pediatric patients (2 to 4 years of age) in which the intention was to reach the target dose of 60 mg/kg/day, 50% of patients reached a final dose of at least 55 mg/kg/day.
- Under adjunctive therapy (with and without enzyme-inducing AEDs), when normalized by body weight, apparent clearance (L/hr/kg) decreased when age increased such that children 2 to <4 years of age may require up to twice the oxcarbazepine dose per body weight compared to adults; and children 4 to ≤12 years of age may require a 50% higher oxcarbazepine dose per body weight compared to adults.
- Conversion to Monotherapy for Pediatric Patients (Aged 4-16 Years)
- Patients receiving concomitant antiepileptic drugs may be converted to monotherapy by initiating treatment with Oxcarbazepine at approximately 8-10 mg/kg/day given in a twice-a-day regimen, while simultaneously initiating the reduction of the dose of the concomitant antiepileptic drugs. The concomitant antiepileptic drugs can be completely withdrawn over 3-6 weeks while Oxcarbazepine may be increased as clinically indicated by a maximum increment of 10 mg/kg/day at approximately weekly intervals to achieve the recommended daily dose. Patients should be observed closely during this transition phase.
- The recommended total daily dose of Oxcarbazepine is shown in the table below.
- Initiation of Monotherapy for Pediatric Patients (Aged 4-16 Years)
- Patients not currently being treated with antiepileptic drugs may have monotherapy initiated with Oxcarbazepine. In these patients, Oxcarbazepine should be initiated at a dose of 8-10 mg/kg/day given in a twice-a-day regimen. The dose should be increased by 5 mg/kg/day every third day to the recommended daily dose shown in the table below.
Off-Label Use and Dosage (Pediatric)
Guideline-Supported Use
There is limited information regarding Off-Label Guideline-Supported Use of Oxcarbazepine in pediatric patients.
Non–Guideline-Supported Use
There is limited information regarding Off-Label Non–Guideline-Supported Use of Oxcarbazepine in pediatric patients.
Contraindications
- Oxcarbazepine should not be used in patients with a known hypersensitivity to oxcarbazepine or to any of its components.
Warnings
Precautions
- Hyponatremia
- Clinically significant hyponatremia (sodium <125 mmol/L) can develop during Oxcarbazepine use. In the 14 controlled epilepsy studies 2.5% of Oxcarbazepine-treated patients (38/1,524) had a sodium of less than 125 mmol/L at some point during treatment, compared to no such patients assigned placebo or active control (carbamazepine and phenobarbital for adjunctive and monotherapy substitution studies, and phenytoin and valproate for the monotherapy initiation studies). Clinically significant hyponatremia generally occurred during the first three months of treatment with Oxcarbazepine, although there were patients who first developed a serum sodium <125 mmol/L more than one year after initiation of therapy. Most patients who developed hyponatremia were asymptomatic but patients in the clinical trials were frequently monitored and some had their Oxcarbazepine dose reduced, discontinued, or had their fluid intake restricted for hyponatremia. Whether or not these maneuvers prevented the occurrence of more severe events is unknown. Cases of symptomatic hyponatremia have been reported during post-marketing use. In clinical trials, patients whose treatment with Oxcarbazepine was discontinued due to hyponatremia generally experienced normalization of serum sodium within a few days without additional treatment.
- Measurement of serum sodium levels should be considered for patients during maintenance treatment with Oxcarbazepine, particularly if the patient is receiving other medications known to decrease serum sodium levels (for example, drugs associated with inappropriate ADH secretion) or if symptoms possibly indicating hyponatremia develop (e.g., nausea, malaise, headache, lethargy, confusion, obtundation, or increase in seizure frequency or severity).
- Anaphylactic Reactions and Angioedema
- Rare cases of anaphylaxis and angioedema involving the larynx, glottis, lips and eyelids have been reported in patients after taking the first or subsequent doses of Oxcarbazepine. Angioedema associated with laryngeal edema can be fatal. If a patient develops any of these reactions after treatment with Oxcarbazepine, the drug should be discontinued and an alternative treatment started. These patients should not be rechallenged with the drug.
- Patients with a Past History of Hypersensitivity Reaction to Carbamazepine
- Patients who have had hypersensitivity reactions to carbamazepine should be informed that approximately 25%-30% of them will experience hypersensitivity reactions with Oxcarbazepine. For this reason patients should be specifically questioned about any prior experience with carbamazepine, and patients with a history of hypersensitivity reactions to carbamazepine should ordinarily be treated with Oxcarbazepine only if the potential benefit justifies the potential risk. If signs or symptoms of hypersensitivity develop, Oxcarbazepine should be discontinued immediately.
- Serious Dermatological Reactions
- Serious dermatological reactions, including Stevens-Johnson syndrome (SJS) and toxic epidermal necrolysis (TEN), have been reported in both children and adults in association with Oxcarbazepine use. Such serious skin reactions may be life threatening, and some patients have required hospitalization, with very rare reports of fatal outcome. The median time of onset for reported cases was 19 days after treatment initiation. Recurrence of the serious skin reactions following rechallenge with Oxcarbazepine has also been reported.
- The reporting rate of TEN and SJS associated with Oxcarbazepine use, which is generally accepted to be an underestimate due to underreporting, exceeds the background incidence rate estimates by a factor of 3- to 10-fold. Estimates of the background incidence rate for these serious skin reactions in the general population range between 0.5 to 6 cases per million-person years. Therefore, if a patient develops a skin reaction while taking Oxcarbazepine, consideration should be given to discontinuing Oxcarbazepine use and prescribing another antiepileptic medication.
- Association with HLA-B*1502
- Patients carrying the HLA-B*1502 allele may be at increased risk for SJS/TEN with oxcarbazepine treatment.
- Human Leukocyte Antigen (HLA) allele B*1502 increases the risk for developing SJS/TEN in patients treated with carbamazepine. The chemical structure of oxcarbazepine is similar to that of carbamazepine. Available clinical evidence, and data from nonclinical studies showing a direct interaction between oxcarbazepine and HLA-B*1502 protein, suggest that the HLA-B*1502 allele may also increase the risk for SJS/TEN with oxcarbazepine.
- The frequency of HLA-B*1502 allele ranges from 2 to 12% in Han Chinese populations, is about 8% in Thai populations, and above 15% in the Philippines and in some Malaysian populations. Allele frequencies up to about 2% and 6% have been reported in Korea and India, respectively. The frequency of the HLA-B*1502 allele is negligible in people from European descent, several African populations, indigenous peoples of the Americas, Hispanic populations, and in Japanese (<1%).
- Testing for the presence of the HLA-B*1502 allele should be considered in patients with ancestry in genetically at-risk populations, prior to initiating treatment with oxcarbazepine. The use of oxcarbazepine should be avoided in patients positive for HLA-B*1502 unless the benefits clearly outweigh the risks. Consideration should also be given to avoid the use of other drugs associated with SJS/TEN in HLA-B*1502 positive patients, when alternative therapies are otherwise equally acceptable. Screening is not generally recommended in patients from populations in which the prevalence of HLA-B*1502 is low, or in current oxcarbazepine users, as the risk of SJS/TEN is largely confined to the first few months of therapy, regardless of HLA B*1502 status.
- The use of HLA-B*1502 genotyping has important limitations and must never substitute for appropriate clinical vigilance and patient management. The role of other possible factors in the development of, and morbidity from, SJS/TEN, such as antiepileptic drug (AED) dose, compliance, concomitant medications, comorbidities, and the level of dermatologic monitoring have not been well characterized.
- Suicidal Behavior and Ideation
- Antiepileptic drugs (AEDs), including Oxcarbazepine, increase the risk of suicidal thoughts or behavior in patients taking these drugs for any indication. Patients treated with any AED for any indication should be monitored for the emergence or worsening of depression, suicidal thoughts or behavior, and/or any unusual changes in mood or behavior.
- Pooled analyses of 199 placebo-controlled clinical trials (mono- and adjunctive therapy) of 11 different AEDs showed that patients randomized to one of the AEDs had approximately twice the risk (adjusted Relative Risk 1.8, 95% CI:1.2, 2.7) of suicidal thinking or behavior compared to patients randomized to placebo. In these trials, which had a median treatment duration of 12 weeks, the estimated incidence rate of suicidal behavior or ideation among 27,863 AED-treated patients was 0.43%, compared to 0.24% among 16,029 placebo-treated patients, representing an increase of approximately one case of suicidal thinking or behavior for every 530 patients treated. There were four suicides in drug-treated patients in the trials and none in placebo-treated patients, but the number is too small to allow any conclusion about drug effect on suicide.
- The increased risk of suicidal thoughts or behavior with AEDs was observed as early as one week after starting drug treatment with AEDs and persisted for the duration of treatment assessed. Because most trials included in the analysis did not extend beyond 24 weeks, the risk of suicidal thoughts or behavior beyond 24 weeks could not be assessed.
- The risk of suicidal thoughts or behavior was generally consistent among drugs in the data analyzed. The finding of increased risk with AEDs of varying mechanisms of action and across a range of indications suggests that the risk applies to all AEDs used for any indication. The risk did not vary substantially by age (5-100 years) in the clinical trials analyzed. Table 2 shows absolute and relative risk by indication for all evaluated AEDs.
- The relative risk for suicidal thoughts or behavior was higher in clinical trials for epilepsy than in clinical trials for psychiatric or other conditions, but the absolute risk differences were similar for the epilepsy and psychiatric indications.
- Anyone considering prescribing Oxcarbazepine or any other AED must balance the risk of suicidal thoughts or behavior with the risk of untreated illness. Epilepsy and many other illnesses for which AEDs are prescribed are themselves associated with morbidity and mortality and an increased risk of suicidal thoughts and behavior. Should suicidal thoughts and behavior emerge during treatment, the prescriber needs to consider whether the emergence of these symptoms in any given patient may be related to the illness being treated.
- Patients, their caregivers, and families should be informed that AEDs increase the risk of suicidal thoughts and behavior and should be advised of the need to be alert for the emergence or worsening of the signs and symptoms of depression, any unusual changes in mood or behavior, or the emergence of suicidal thoughts, behavior, or thoughts about self-harm. Behaviors of concern should be reported immediately to healthcare providers.
- Withdrawal of AEDs
- As with all antiepileptic drugs, Oxcarbazepine should be withdrawn gradually to minimize the potential of increased seizure frequency.
- Cognitive/Neuropsychiatric Adverse Events
- Use of Oxcarbazepine has been associated with central nervous system-related adverse events. The most significant of these can be classified into three general categories: 1) cognitive symptoms including psychomotor slowing, difficulty with concentration, and speech or language problems, 2) somnolence or fatigue, and 3) coordination abnormalities, including ataxia and gait disturbances.
Adult Patients
- In one large, fixed-dose study, Oxcarbazepine was added to existing AED therapy (up to three concomitant AEDs). By protocol, the dosage of the concomitant AEDs could not be reduced as Oxcarbazepine was added, reduction in Oxcarbazepine dosage was not allowed if intolerance developed, and patients were discontinued if unable to tolerate their highest target maintenance doses. In this trial, 65% of patients were discontinued because they could not tolerate the 2400 mg/day dose of Oxcarbazepine on top of existing AEDs. The adverse events seen in this study were primarily CNS related and the risk for discontinuation was dose related.
- In this trial, 7.1% of oxcarbazepine-treated patients and 4% of placebo-treated patients experienced a cognitive adverse event. The risk of discontinuation for these events was about 6.5 times greater on oxcarbazepine than on placebo. In addition, 26% of oxcarbazepine-treated patients and 12% of placebo-treated patients experienced somnolence. The risk of discontinuation for somnolence was about 10 times greater on oxcarbazepine than on placebo. Finally, 28.7% of oxcarbazepine-treated patients and 6.4% of placebo-treated patients experienced ataxia or gait disturbances. The risk for discontinuation for these events was about seven times greater on oxcarbazepine than on placebo.
- In a single placebo-controlled monotherapy trial evaluating 2400 mg/day of Oxcarbazepine, no patients in either treatment group discontinued double-blind treatment because of cognitive adverse events, somnolence, ataxia, or gait disturbance.
- In the two dose-controlled conversion to monotherapy trials comparing 2400 mg/day and 300 mg/day Oxcarbazepine, 1.1% of patients in the 2400 mg/day group discontinued double-blind treatment because of somnolence or cognitive adverse events compared to 0% in the 300 mg/day group. In these trials, no patients discontinued because of ataxia or gait disturbances in either treatment group.
Pediatric Patients
- A study was conducted in pediatric patients (3 to 17 years old) with inadequately controlled partial seizures in which Oxcarbazepine was added to existing AED therapy (up to two concomitant AEDs). By protocol, the dosage of concomitant AEDs could not be reduced as Oxcarbazepine was added. Oxcarbazepine was titrated to reach a target dose ranging from 30 mg/kg to 46 mg/kg (based on a patient's body weight with fixed doses for predefined weight ranges).
- Cognitive adverse events occurred in 5.8% of oxcarbazepine-treated patients (the single most common event being concentration impairment, 4 of 138 patients) and in 3.1% of patients treated with placebo. In addition, 34.8% of oxcarbazepine-treated patients and 14.0% of placebo-treated patients experienced somnolence. (No patient discontinued due to a cognitive adverse event or somnolence.). Finally, 23.2% of oxcarbazepine-treated patients and 7.0% of placebo-treated patients experienced ataxia or gait disturbances. Two (1.4%) oxcarbazepine-treated patients and 1 (0.8%) placebo-treated patient discontinued due to ataxia or gait disturbances.
- Drug Reaction with Eosinophilia and Systemic Symptoms (Dress syndrome/Multi-Organ Hypersensitivity)
- Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS), also known as multi-organ hypersensitivity, has occurred with oxcarbazepine. Some of these events have been fatal or life-threatening. DRESS syndrome typically, although not exclusively, presents with fever, rash, and/or lymphadenopathy, in association with other organ system involvement, such as hepatitis, nephritis, hematologic abnormalities, myocarditis, or myositis, sometimes resembling an acute viral infection. Eosinophilia is often present. This disorder is variable in its expression, and other organ systems not noted here may be involved. It is important to note that early manifestations of hypersensitivity (e.g., fever, lymphadenopathy) may be present even though rash is not evident. If such signs or symptoms are present, the patient should be evaluated immediately. Oxcarbazepine should be discontinued if an alternative etiology for the signs or symptoms cannot be established. Although there are no case reports to indicate cross sensitivity with other drugs that produce this syndrome, the experience amongst drugs associated with DRESS/multi-organ hypersensitivity would indicate this to be a possibility.
- Hematologic Events
- Rare reports of pancytopenia, agranulocytosis, and leukopenia have been seen in patients treated with Oxcarbazepine during postmarketing experience. Discontinuation of the drug should be considered if any evidence of these hematologic events develop.
- Seizure Control During Pregnancy
- Due to physiological changes during pregnancy, plasma levels of the active metabolite of oxcarbazepine, the 10-monohydroxy derivative (MHD), may gradually decrease throughout pregnancy. It is recommended that patients be monitored carefully during pregnancy. Close monitoring should continue through the postpartum period because MHD levels may return after delivery.
- Laboratory Tests
- Serum sodium levels below 125 mmol/L have been observed in patients treated with Oxcarbazepine. Experience from clinical trials indicates that serum sodium levels return toward normal when the Oxcarbazepine dosage is reduced or discontinued, or when the patient was treated conservatively (e.g., fluid restriction).
- Laboratory data from clinical trials suggest that Oxcarbazepine use was associated with decreases in T4, without changes in T3 or TSH.
Adverse Reactions
Clinical Trials Experience
- Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
Most Common Adverse Reactions in All Clinical Studies
- Adjunctive Therapy/Monotherapy in Adults Previously Treated with other AEDs: The most commonly observed (≥5%) adverse reactions seen in association with Oxcarbazepine and substantially more frequent than in placebo-treated patients were: dizziness, somnolence, diplopia, fatigue, nausea, vomiting, ataxia, abnormal vision, abdominal pain, tremor, dyspepsia, abnormal gait.
- Approximately 23% of these 1,537 adult patients discontinued treatment because of an adverse experience. The adverse reactions most commonly associated with discontinuation were: dizziness (6.4%), diplopia (5.9%), ataxia (5.2%), vomiting (5.1%), nausea (4.9%), somnolence (3.8%), headache (2.9%), fatigue (2.1%), abnormal vision (2.1%), tremor (1.8%), abnormal gait (1.7%), rash (1.4%), hyponatremia (1.0%).
- Monotherapy in Adults Not Previously Treated with other AEDs: The most commonly observed (≥5%) adverse reactions seen in association with Oxcarbazepine in these patients were similar to those in previously treated patients.
- Approximately 9% of these 295 adult patients discontinued treatment because of an adverse experience. The adverse reactions most commonly associated with discontinuation were: dizziness (1.7%), nausea (1.7%), rash (1.7%), headache (1.4%).
- Adjunctive Therapy/Monotherapy in Pediatric Patients 4 Years Old and Above Previously Treated with other AEDs: The most commonly observed (≥5%) adverse reactions seen in association with Oxcarbazepine in these patients were similar to those seen in adults.
- Approximately 11% of these 456 pediatric patients discontinued treatment because of an adverse experience. The adverse reactions most commonly associated with discontinuation were: somnolence (2.4%), vomiting (2.0%), ataxia (1.8%), diplopia (1.3%), dizziness (1.3%), fatigue (1.1%), nystagmus (1.1%).
- Monotherapy in Pediatric Patients 4 Years Old and Above Not Previously Treated with other AEDs: The most commonly observed (≥5%) adverse reactions seen in association with Oxcarbazepine in these patients were similar to those in adults.
- Approximately 9.2% of 152 pediatric patients discontinued treatment because of an adverse experience. The adverse reactions most commonly associated (≥1%) with discontinuation were rash (5.3%) and maculopapular rash (1.3%).
- Adjunctive Therapy/Monotherapy in Pediatric Patients 1 Month to <4 Years Old Previously Treated or Not Previously Treated with other AEDs: The most commonly observed (≥5%) adverse reactions seen in association with Oxcarbazepine in these patients were similar to those seen in older children and adults except for infections and infestations which were more frequently seen in these younger children.
- Approximately 11% of these 241 pediatric patients discontinued treatment because of an adverse experience. The adverse reaction most commonly associated with discontinuation were: convulsions (3.7%), status epilepticus (1.2%), and ataxia (1.2%).
- Incidence in Controlled Clinical Studies: The prescriber should be aware that the figures in Tables 3, 4, 5 and 6 cannot be used to predict the frequency of adverse reactions in the course of usual medical practice where patient characteristics and other factors may differ from those prevailing during clinical studies. Similarly, the cited frequencies cannot be directly compared with figures obtained from other clinical investigations involving different treatments, uses, or investigators. An inspection of these frequencies, however, does provide the prescriber with one basis to estimate the relative contribution of drug and nondrug factors to the adverse event incidences in the population studied.
- Controlled Clinical Studies of Adjunctive Therapy/Monotherapy in Adults Previously Treated with other AEDs: Table 3 lists treatment-emergent signs and symptoms that occurred in at least 2% of adult patients with epilepsy treated with Oxcarbazepine or placebo as adjunctive treatment and were numerically more common in the patients treated with any dose of Oxcarbazepine. Table 4 lists treatment-emergent signs and symptoms in patients converted from other AEDs to either high dose Oxcarbazepine or low dose (300 mg) Oxcarbazepine. Note that in some of these monotherapy studies patients who dropped out during a preliminary tolerability phase are not included in the tables.
- Controlled Clinical Study of Monotherapy in Adults Not Previously Treated with other AEDs: Table 5 lists treatment-emergent signs and symptoms in a controlled clinical study of monotherapy in adults not previously treated with other AEDs that occurred in at least 2% of adult patients with epilepsy treated with Oxcarbazepine or placebo and were numerically more common in the patients treated with Oxcarbazepine.
- Controlled Clinical Studies of Adjunctive Therapy/Monotherapy in Pediatric Patients Previously Treated with other AEDs: Table 6 lists treatment-emergent signs and symptoms that occurred in at least 2% of pediatric patients with epilepsy treated with Oxcarbazepine or placebo as adjunctive treatment and were numerically more common in the patients treated with Oxcarbazepine.
- Other Events Observed in Association with the Administration of Oxcarbazepine
- In the paragraphs that follow, the adverse events, other than those in the preceding tables or text, that occurred in a total of 565 children and 1,574 adults exposed to Oxcarbazepine and that are reasonably likely to be related to drug use are presented. Events common in the population, events reflecting chronic illness and events likely to reflect concomitant illness are omitted particularly if minor. They are listed in order of decreasing frequency. Because the reports cite events observed in open label and uncontrolled trials, the role of Oxcarbazepine in their causation cannot be reliably determined.
Body as a Whole
Fever, malaise, pain chest precordial, rigors, weight decrease.
Cardiovascular System
Bradycardia, cardiac failure, cerebral hemorrhage, hypertension, hypotension postural, palpitation, syncope, tachycardia.
Digestive System
Appetite increased, blood in stool, cholelithiasis, colitis, duodenal ulcer, dysphagia, enteritis, eructation, esophagitis, flatulence, gastric ulcer, gingival bleeding, gum hyperplasia, hematemesis, rectal hemorrhage, hemorrhoids, hiccup, mouth dry, pain biliary, pain right hypochondrium, retching, sialoadenitis, stomatitis, stomatitis ulcerative.
Hematologic and Lymphatic System
Laboratory Abnormality
Gamma-GT increased, hyperglycemia, hypocalcemia, hypoglycemia, hypokalemia, liver enzymes elevated, serum transaminase increased.
Musculoskeletal System
Hypertonia muscle.
Nervous System
Aggressive reaction, amnesia, anguish, anxiety, apathy, aphasia, aura, convulsions aggravated, delirium, delusion, depressed level of consciousness, dysphonia, dystonia, emotional lability, euphoria, extrapyramidal disorder, feeling drunk, hemiplegia, hyperkinesia, hyperreflexia, hypoesthesia, hypokinesia, hyporeflexia, hypotonia, hysteria, libido decreased, libido increased, manic reaction, migraine, muscle contractions involuntary, nervousness, neuralgia, oculogyric crisis, panic disorder, paralysis, paroniria, personality disorder, psychosis, ptosis, stupor, tetany.
Respiratory System
Asthma, dyspnea, epistaxis, laryngismus, pleurisy.
Skin and Appendages
Acne, alopecia, angioedema, bruising, contact dermatitis, eczema, facial rash, flushing, folliculitis, heat rash, hot flushes, photosensitivity reaction, pruritus genital, psoriasis, purpura, rash erythematous, rash maculopapular, vitiligo, urticaria.
Special Senses
Accommodation abnormal, cataract, conjunctival hemorrhage, edema eye, hemianopia, mydriasis, otitis externa, photophobia, scotoma, taste perversion, tinnitus, xerophthalmia.
Surgical and Medical Procedures
Procedure dental oral, procedure female reproductive, procedure musculoskeletal, procedure skin.
Urogenital and Reproductive System
Dysuria, hematuria, intermenstrual bleeding, leukorrhea, menorrhagia, micturition frequency, pain renal, pain urinary tract, polyuria, priapism, renal calculus.
Other
Postmarketing Experience
- The following adverse events have been observed in named patient programs or postmarketing experience. Because these reactions are reported voluntarily from a population of uncertain size, it is not possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Digestive System
Pancreatitis and/or lipase and/or amylase increase
Hematologic and Lymphatic Systems
Metabolism
Skin and subcutaneous tissue disorders
Erythema multiforme, Stevens-Johnson syndrome, toxic epidermal necrolysis, Acute Generalized Exanthematous Pustulosis (AGEP)
Musculoskeletal, connective tissue and bone disorders
There have been reports of decreased bone mineral density, osteoporosis and fractures in patients on long-term therapy with oxcarbazepine.
Drug Interactions
- Oxcarbazepine can inhibit CYP2C19 and induce CYP3A4/5 with potentially important effects on plasma concentrations of other drugs. The inhibition of CYP2C19 by oxcarbazepine and MHD can cause increased plasma concentrations of drugs that are substrates of CYP2C19. Oxcarbazepine and MHD induce a subgroup of the cytochrome P450 3A family (CYP3A4 and CYP3A5) responsible for the metabolism of dihydropyridine calcium antagonists, oral contraceptives and cyclosporine resulting in a lower plasma concentration of these drugs.
- In addition, several AEDs that are cytochrome P450 inducers can decrease plasma concentrations of oxcarbazepine and MHD. No autoinduction has been observed with Oxcarbazepine.
- Antiepileptic Drugs
- Potential interactions between Oxcarbazepine and other AEDs were assessed in clinical studies. The effect of these interactions on mean AUCs and Cmin are summarized in Table 7.
- In vivo, the plasma levels of phenytoin increased by up to 40% when Oxcarbazepine was given at doses above 1200 mg/day. Therefore, when using doses of Oxcarbazepine greater than 1200 mg/day during adjunctive therapy, a decrease in the dose of phenytoin may be required. The increase of phenobarbital level, however, is small (15%) when given with Oxcarbazepine.
- Strong inducers of cytochrome P450 enzymes (i.e., carbamazepine, phenytoin and phenobarbital) have been shown to decrease the plasma levels of MHD (29%-40%).
- No autoinduction has been observed with Oxcarbazepine.
- Hormonal Contraceptives
- Coadministration of Oxcarbazepine with an oral contraceptive has been shown to influence the plasma concentrations of the two hormonal components, ethinylestradiol (EE) and levonorgestrel (LNG). The mean AUC values of EE were decreased by 48% [90% CI: 22-65] in one study and 52% [90% CI: 38-52] in another study. The mean AUC values of LNG were decreased by 32% [90% CI: 20-45] in one study and 52% [90% CI: 42-52] in another study. Therefore, concurrent use of Oxcarbazepine with hormonal contraceptives may render these contraceptives less effective. Studies with other oral or implant contraceptives have not been conducted.
- After repeated coadministration of Oxcarbazepine, the AUC of felodipine was lowered by 28% [90% CI: 20-33]. Verapamil produced a decrease of 20% [90% CI: 18-27] of the plasma levels of MHD.
- Other Drug Interactions
- Cimetidine, erythromycin and dextropropoxyphene had no effect on the pharmacokinetics of MHD. Results with warfarin show no evidence of interaction with either single or repeated doses of Oxcarbazepine.
- Drug/Laboratory Test Interactions
- There are no known interactions of Oxcarbazepine with commonly used laboratory tests.
Use in Specific Populations
Pregnancy
- Pregnancy Category C
- There are no adequate and well-controlled clinical studies of Oxcarbazepine in pregnant women; however, Oxcarbazepine is closely related structurally to carbamazepine, which is considered to be teratogenic in humans. Given this fact, and the results of the animal studies described, it is likely that Oxcarbazepine is a human teratogen. Oxcarbazepine should be used during pregnancy only if the potential benefit justifies the potential risk to the fetus.
- Increased incidences of fetal structural abnormalities and other manifestations of developmental toxicity (embryolethality, growth retardation) were observed in the offspring of animals treated with either oxcarbazepine or its active 10-hydroxy metabolite (MHD) during pregnancy at doses similar to the maximum recommended human dose.
- When pregnant rats were given oxcarbazepine (30, 300, or 1000 mg/kg) orally throughout the period of organogenesis, increased incidences of fetal malformations (craniofacial, cardiovascular, and skeletal) and variations were observed at the intermediate and high doses (approximately 1.2 and 4 times, respectively, the maximum recommended human dose [MRHD] on a mg/m2 basis). Increased embryofetal death and decreased fetal body weights were seen at the high dose. Doses ≥300 mg/kg were also maternally toxic (decreased body weight gain, clinical signs), but there is no evidence to suggest that teratogenicity was secondary to the maternal effects.
- In a study in which pregnant rabbits were orally administered MHD (20, 100, or 200 mg/kg) during organogenesis, embryofetal mortality was increased at the highest dose (1.5 times the MRHD on a mg/m2 basis). This dose produced only minimal maternal toxicity.
- In a study in which female rats were dosed orally with oxcarbazepine (25, 50, or 150 mg/kg) during the latter part of gestation and throughout the lactation period, a persistent reduction in body weights and altered behavior (decreased activity) were observed in offspring exposed to the highest dose (0.6 times the MRHD on a mg/m2 basis). Oral administration of MHD (25, 75, or 250 mg/kg) to rats during gestation and lactation resulted in a persistent reduction in offspring weights at the highest dose (equivalent to the MRHD on a mg/m2 basis).
- To provide information regarding the effects of in utero exposure to Oxcarbazepine, physicians are advised to recommend that pregnant patients taking Oxcarbazepine enroll in the NAAED Pregnancy Registry. This can be done by calling the toll free number 1-888-233-2334, and must be done by patients themselves. Information on the registry can also be found at the website http://www.aedpregnancyregistry.org/
- Australian Drug Evaluation Committee (ADEC) Pregnancy Category
There is no Australian Drug Evaluation Committee (ADEC) guidance on usage of Oxcarbazepine in women who are pregnant.
Labor and Delivery
- The effect of Oxcarbazepine on labor and delivery in humans has not been evaluated.
Nursing Mothers
- Oxcarbazepine and its active metabolite (MHD) are excreted in human milk. A milk-to-plasma concentration ratio of 0.5 was found for both. Because of the potential for serious adverse reactions to Oxcarbazepine in nursing infants, a decision should be made about whether to discontinue nursing or to discontinue the drug in nursing women, taking into account the importance of the drug to the mother.
Pediatric Use
- Oxcarbazepine is indicated for use as adjunctive therapy for partial seizures in patients aged 2-16 years. Oxcarbazepine is also indicated as monotherapy for partial seizures in patients aged 4-16 years. Oxcarbazepine has been given to 898 patients between the ages of 1 month-17 years in controlled clinical trials (332 treated as monotherapy) and about 677 patients between the ages of 1 month-17 years in other trials.
Geriatic Use
- There were 52 patients over age 65 in controlled clinical trials and 565 patients over the age of 65 in other trials. Following administration of single (300 mg) and multiple (600 mg/day) doses of Oxcarbazepine in elderly volunteers (60-82 years of age), the maximum plasma concentrations and AUC values of MHD were 30%-60% higher than in younger volunteers (18-32 years of age). Comparisons of creatinine clearance in young and elderly volunteers indicate that the difference was due to age-related reductions in creatinine clearance.
Gender
There is no FDA guidance on the use of Oxcarbazepine with respect to specific gender populations.
Race
There is no FDA guidance on the use of Oxcarbazepine with respect to specific racial populations.
Renal Impairment
- In renally-impaired patients (creatinine clearance <30 mL/min), the elimination half-life of MHD is prolonged with a corresponding two-fold increase in AUC. Oxcarbazepine therapy should be initiated at one-half the usual starting dose and increased, if necessary, at a slower than usual rate until the desired clinical response is achieved.
Hepatic Impairment
There is no FDA guidance on the use of Oxcarbazepine in patients with hepatic impairment.
Females of Reproductive Potential and Males
There is no FDA guidance on the use of Oxcarbazepine in women of reproductive potentials and males.
Immunocompromised Patients
There is no FDA guidance one the use of Oxcarbazepine in patients who are immunocompromised.
Administration and Monitoring
Administration
- Oral
Monitoring
There is limited information regarding Monitoring of Oxcarbazepine in the drug label.
IV Compatibility
There is limited information regarding IV Compatibility of Oxcarbazepine in the drug label.
Overdosage
Acute Overdose
Signs and Symptoms
- Isolated cases of overdose with Oxcarbazepine have been reported. The maximum dose taken was approximately 24,000 mg. All patients recovered with symptomatic treatment.
Management
- There is no specific antidote. Symptomatic and supportive treatment should be administered as appropriate. Removal of the drug by gastric lavage and/or inactivation by administering activated charcoal should be considered.
Chronic Overdose
There is limited information regarding Chronic Overdose of Oxcarbazepine in the drug label.
Pharmacology
| |
| |
Oxcarbazepine
| |
| Systematic (IUPAC) name | |
| 10,11-dihydro- 10-oxo- 5H-dibenz(b,f)azepine- 5-carboxamide | |
| Identifiers | |
| CAS number | |
| ATC code | N03 |
| PubChem | |
| DrugBank | |
| Chemical data | |
| Formula | Template:OrganicBox atomTemplate:OrganicBox atomTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBox atomTemplate:OrganicBoxTemplate:OrganicBox atomTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBox |
| Mol. mass | 252.268 g/mol |
| SMILES | & |
| Pharmacokinetic data | |
| Bioavailability | > 95% |
| Protein binding | ? |
| Metabolism | Hepatic (Cytosolic Enzymes & Glucuronic Acid) |
| Half life | 1–5 hours (healthy adults) |
| Excretion | Renal |
| Therapeutic considerations | |
| Pregnancy cat. |
C(US) |
| Legal status |
POM(UK) [[Prescription drug|Template:Unicode-only]](US) |
| Routes | Oral (Tablets or Suspension) |
Mechanism of Action
- The pharmacological activity of oxcarbazepine is primarily exerted through the 10-monohydroxy metabolite (MHD) of oxcarbazepine. The precise mechanism by which Oxcarbazepine and MHD exert their antiseizure effect is unknown; however, in vitro electrophysiological studies indicate that they produce blockade of voltage-sensitive sodium channels, resulting in stabilization of hyperexcited neural membranes, inhibition of repetitive neuronal firing, and diminution of propagation of synaptic impulses. These actions are thought to be important in the prevention of seizure spread in the intact brain. In addition, increased potassium conductance and modulation of high voltage activated calcium channels may contribute to the anticonvulsant effects of the drug. No significant interactions of oxcarbazepine or MHD with brain neurotransmitter or modulator receptor sites have been demonstrated.
Structure
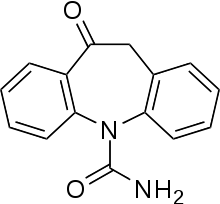
- Oxcarbazepine Tablet is an antiepileptic drug available as 150 mg, 300 mg and 600 mg film-coated tablets for oral administration. Oxcarbazepine is 10,11-Dihydro-10-oxo-5H-dibenz[b,ƒ]azepine-5-carboxamide, and its structural formula is
- Oxcarbazepine is a white to faintly orange crystalline powder. It is slightly soluble in chloroform, dichloromethane, acetone, and methanol and practically insoluble in ethanol, ether and water. Its molecular weight is 252.27.
- Oxcarbazepine film-coated tablets contain the following inactive ingredients: colloidal silicon dioxide, crospovidone, hypromellose, iron oxide yellow, iron oxide red, magnesium stearate, microcrystalline cellulose, polyethylene glycol, talc, and titanium dioxide.
Pharmacodynamics
- Oxcarbazepine and its active metabolite (MHD) exhibit anticonvulsant properties in animal seizure models. They protected rodents against electrically induced tonic extension seizures and, to a lesser degree, chemically induced clonic seizures, and abolished or reduced the frequency of chronically recurring focal seizures in Rhesus monkeys with aluminum implants. No development of tolerance (i.e., attenuation of anticonvulsive activity) was observed in the maximal electroshock test when mice and rats were treated daily for five days and four weeks, respectively, with oxcarbazepine or MHD.
Pharmacokinetics
- Following oral administration of Oxcarbazepine Tablets, oxcarbazepine is completely absorbed and extensively metabolized to its pharmacologically active 10-monohydroxy metabolite (MHD). In a mass balance study in people, only 2% of total radioactivity in plasma was due to unchanged oxcarbazepine, with approximately 70% present as MHD, and the remainder attributable to minor metabolites.
- The half-life of the parent is about two hours, while the half-life of MHD is about nine hours, so that MHD is responsible for most antiepileptic activity.
- Absorption
- Based on MHD concentrations, Oxcarbazepine Tablets and suspension were shown to have similar bioavailability.
- After single-dose administration of Oxcarbazepine Tablets to healthy male volunteers under fasted conditions, the median tmax was 4.5 (range 3 to 13) hours.
- Steady-state plasma concentrations of MHD are reached within 2-3 days in patients when Oxcarbazepine Tablet is given twice a day. At steady state the pharmacokinetics of MHD are linear and show dose proportionality over the dose range of 300 to 2400 mg/day.
- Effect of Food: Food has no effect on the rate and extent of absorption of Oxcarbazepine Tablets. Therefore, Oxcarbazepine Tablets can be taken with or without food.
- Distribution
- The apparent volume of distribution of MHD is 49L.
- Approximately 40% of MHD is bound to serum proteins, predominantly to albumin. Binding is independent of the serum concentration within the therapeutically relevant range. Oxcarbazepine and MHD do not bind to alpha-1-acid glycoprotein.
- Metabolism and Excretion
- Oxcarbazepine is rapidly reduced by cytosolic enzymes in the liver to its 10-monohydroxy metabolite, MHD, which is primarily responsible for the pharmacological effect of Oxcarbazepine. MHD is metabolized further by conjugation with glucuronic acid. Minor amounts (4% of the dose) are oxidized to the pharmacologically inactive 10,11-dihydroxy metabolite (DHD).
- Oxcarbazepine is cleared from the body mostly in the form of metabolites which are predominantly excreted by the kidneys. More than 95% of the dose appears in the urine, with less than 1% as unchanged oxcarbazepine. Fecal excretion accounts for less than 4% of the administered dose. Approximately 80% of the dose is excreted in the urine either as glucuronides of MHD (49%) or as unchanged MHD (27%); the inactive DHD accounts for approximately 3% and conjugates of MHD and oxcarbazepine account for 13% of the dose.
- The half-life of the parent is about two hours, while the half-life of MHD is about nine hours.
- Special Populations
- Hepatic Impairment
- The pharmacokinetics and metabolism of oxcarbazepine and MHD were evaluated in healthy volunteers and hepatically-impaired subjects after a single 900-mg oral dose. Mild-to-moderate hepatic impairment did not affect the pharmacokinetics of oxcarbazepine and MHD. No dose adjustment for Oxcarbazepine is recommended in patients with mild-to-moderate hepatic impairment. The pharmacokinetics of oxcarbazepine and MHD have not been evaluated in severe hepatic impairment and, therefore, caution should be exercised when dosing severely impaired patients.
- Renal Impairment
- There is a linear correlation between creatinine clearance and the renal clearance of MHD. When Oxcarbazepine is administered as a single 300-mg dose in renally-impaired patients (creatinine clearance <30 mL/min), the elimination half-life of MHD is prolonged to 19 hours, with a two-fold increase in AUC. Dose adjustment for Oxcarbazepine is recommended in these patients.
- Pediatrics
- Weight-adjusted MHD clearance decreases as age and weight increases, approaching that of adults. The mean weight adjusted clearance in children 2 years-<4 years of age is approximately 80% higher on average than that of adults. Therefore, MHD exposure in these children is expected to be about one-half that of adults when treated with a similar weight-adjusted dose. The mean weight-adjusted clearance in children 4-12 years of age is approximately 40% higher on average than that of adults. Therefore, MHD exposure in these children is expected to be about three-quarters that of adults when treated with a similar weight-adjusted dose. As weight increases, for patients 13 years of age and above, the weight-adjusted MHD clearance is expected to reach that of adults.
- Pregnancy
- Geriatrics
- Following administration of single (300 mg) and multiple (600 mg/day) doses of Oxcarbazepine to elderly volunteers (60-82 years of age), the maximum plasma concentrations and AUC values of MHD were 30%-60% higher than in younger volunteers (18-32 years of age). Comparisons of creatinine clearance in young and elderly volunteers indicate that the difference was due to age-related reductions in creatinine clearance.
- Gender
- No gender-related pharmacokinetic differences have been observed in children, adults, or the elderly.
- Race
- No specific studies have been conducted to assess what effect, if any, race may have on the disposition of oxcarbazepine.
- Drug Interactions:
- In Vitro
- Oxcarbazepine can inhibit CYP2C19 and induce CYP3A4/5 with potentially important effects on plasma concentrations of other drugs. In addition, several AEDs that are cytochrome P450 inducers can decrease plasma concentrations of oxcarbazepine and MHD.
- Oxcarbazepine was evaluated in human liver microsomes to determine its capacity to inhibit the major cytochrome P450 enzymes responsible for the metabolism of other drugs. Results demonstrate that oxcarbazepine and its pharmacologically active 10-monohydroxy metabolite (MHD) have little or no capacity to function as inhibitors for most of the human cytochrome P450 enzymes evaluated (CYP1A2, CYP2A6, CYP2C9, CYP2D6, CYP2E1, CYP4A9 and CYP4A11) with the exception of CYP2C19 and CYP3A4/5. Although inhibition of CYP3A4/5 by oxcarbazepine and MHD did occur at high concentrations, it is not likely to be of clinical significance. The inhibition of CYP2C19 by oxcarbazepine and MHD, is clinically relevant.
- In vitro, the UDP-glucuronyl transferase level was increased, indicating induction of this enzyme. Increases of 22% with MHD and 47% with oxcarbazepine were observed. As MHD, the predominant plasma substrate, is only a weak inducer of UDP-glucuronyl transferase, it is unlikely to have an effect on drugs that are mainly eliminated by conjugation through UDP-glucuronyl transferase (e.g., valproic acid, lamotrigine).
- In addition, oxcarbazepine and MHD induce a subgroup of the cytochrome P450 3A family (CYP3A4 and CYP3A5) responsible for the metabolism of dihydropyridine calcium antagonists, oral contraceptives and cyclosporine resulting in a lower plasma concentration of these drugs.
- As binding of MHD to plasma proteins is low (40%), clinically significant interactions with other drugs through competition for protein binding sites are unlikely.
Nonclinical Toxicology
- Carcinogenesis
- In two-year carcinogenicity studies, oxcarbazepine was administered in the diet at doses of up to 100 mg/kg/day to mice and by gavage at doses of up to 250 mg/kg/day to rats, and the pharmacologically active 10-hydroxy metabolite (MHD) was administered orally at doses of up to 600 mg/kg/day to rats. In mice, a dose-related increase in the incidence of hepatocellular adenomas was observed at oxcarbazepine doses ≥70 mg/kg/day or approximately 0.1 times the maximum recommended human dose (MRHD) on a mg/m2 basis. In rats, the incidence of hepatocellular carcinomas was increased in females treated with oxcarbazepine at doses ≥25 mg/kg/day (0.1 times the MRHD on a mg/m2 basis), and incidences of hepatocellular adenomas and/or carcinomas were increased in males and females treated with MHD at doses of 600 mg/kg/day (2.4 times the MRHD on a mg/m2 basis) and ≥250 mg/kg/day (equivalent to the MRHD on a mg/m2 basis), respectively. There was an increase in the incidence of benign testicular interstitial cell tumors in rats at 250 mg oxcarbazepine/kg/day and at ≥250 mg MHD/kg/day, and an increase in the incidence of granular cell tumors in the cervix and vagina in rats at 600 mg MHD/kg/day.
- Mutagenesis
- Oxcarbazepine increased mutation frequencies in the Ames test in vitro in the absence of metabolic activation in one of five bacterial strains. Both oxcarbazepine and MHD produced increases in chromosomal aberrations and polyploidy in the Chinese hamster ovary assay in vitro in the absence of metabolic activation. MHD was negative in the Ames test, and no mutagenic or clastogenic activity was found with either oxcarbazepine or MHD in V79 Chinese hamster cells in vitro. Oxcarbazepine and MHD were both negative for clastogenic or aneugenic effects (micronucleus formation) in an in vivo rat bone marrow assay.
- Impairment of Fertility
- In a fertility study in which rats were administered MHD (50, 150, or 450 mg/kg) orally prior to and during mating and early gestation, estrous cyclicity was disrupted and numbers of corpora lutea, implantations, and live embryos were reduced in females receiving the highest dose (approximately two times the MRHD on a mg/m2 basis).
Clinical Studies
- The effectiveness of Oxcarbazepine as adjunctive and monotherapy for partial seizures in adults, and as adjunctive therapy in children aged 2-16 years was established in seven multicenter, randomized, controlled trials.
- The effectiveness of Oxcarbazepine as monotherapy for partial seizures in children aged 4-16 years was determined from data obtained in the studies described, as well as by pharmacokinetic/pharmacodynamic considerations.
Oxcarbazepine Monotherapy Trials
- Four randomized, controlled, double-blind, multicenter trials, conducted in a predominately adult population, demonstrated the efficacy of Oxcarbazepine as monotherapy. Two trials compared Oxcarbazepine to placebo and two trials used a randomized withdrawal design to compare a high dose (2400 mg) with a low dose (300 mg) of Oxcarbazepine, after substituting Oxcarbazepine 2400 mg/day for one or more antiepileptic drugs (AEDs). All doses were administered on a twice-a-day schedule. A fifth randomized, controlled, rater-blind, multicenter study, conducted in a pediatric population, failed to demonstrate a statistically significant difference between low and high dose Oxcarbazepine treatment groups.
- One placebo-controlled Oxcarbazepine trial was conducted in 102 patients (11-62 years of age) with refractory partial seizures who had completed an inpatient evaluation for epilepsy surgery. Patients had been withdrawn from all AEDs and were required to have 2-10 partial seizures within 48 hours prior to randomization. Patients were randomized to receive either placebo or Oxcarbazepine given as 1500 mg/day on Day 1 and 2400 mg/day thereafter for an additional nine days, or until one of the following three exit criteria occurred: 1) the occurrence of a fourth partial seizure, excluding Day 1, 2) two new-onset secondarily generalized seizures, where such seizures were not seen in the one-year period prior to randomization, or 3) occurrence of serial seizures or status epilepticus. The primary measure of effectiveness was a between-group comparison of the time to meet exit criteria. There was a statistically significant difference in favor of Oxcarbazepine (see Figure 1), p=0.0001.
- The second placebo-controlled trial was conducted in 67 untreated patients (8-69 years of age) with newly-diagnosed and recent-onset partial seizures. Patients were randomized to placebo or Oxcarbazepine, initiated at 300 mg twice a day and titrated to 1200 mg/day (given as 600 mg twice a day) in six days, followed by maintenance treatment for 84 days. The primary measure of effectiveness was a between-group comparison of the time to first seizure. The difference between the two treatments was statistically significant in favor of Oxcarbazepine (see Figure 2), p=0.046.
- A third trial substituted Oxcarbazepine monotherapy at 2400 mg/day for carbamazepine in 143 patients (12-65 years of age) whose partial seizures were inadequately controlled on carbamazepine (CBZ) monotherapy at a stable dose of 800 to 1600 mg/day, and maintained this Oxcarbazepine dose for 56 days (baseline phase). Patients who were able to tolerate titration of Oxcarbazepine to 2400 mg/day during simultaneous carbamazepine withdrawal were randomly assigned to either 300 mg/day of Oxcarbazepine or 2400 mg/day Oxcarbazepine. Patients were observed for 126 days or until one of the following four exit criteria occurred: 1) a doubling of the 28-day seizure frequency compared to baseline, 2) a two-fold increase in the highest consecutive two-day seizure frequency during baseline, 3) a single generalized seizure if none had occurred during baseline, or 4) a prolonged generalized seizure. The primary measure of effectiveness was a between-group comparison of the time to meet exit criteria. The difference between the curves was statistically significant in favor of the Oxcarbazepine 2400 mg/day group (see Figure 3), p=0.0001.
- Another monotherapy substitution trial was conducted in 87 patients (11-66 years of age) whose seizures were inadequately controlled on one or two AEDs. Patients were randomized to either Oxcarbazepine 2400 mg/day or 300 mg/day and their standard AED regimen(s) were eliminated over the first six weeks of double-blind therapy. Double-blind treatment continued for another 84 days (total double-blind treatment of 126 days) or until one of the four exit criteria described for the previous study occurred. The primary measure of effectiveness was a between-group comparison of the percentage of patients meeting exit criteria. The results were statistically significant in favor of the Oxcarbazepine 2400 mg/day group (14/34; 41.2%) compared to the Oxcarbazepine 300 mg/day group (42/45; 93.3%) (p<0.0001). The time to meeting one of the exit criteria was also statistically significant in favor of the Oxcarbazepine 2400 mg/day group (see Figure 4), p=0.0001.
- A monotherapy trial was conducted in 92 pediatric patients (1 month to 16 years of age) with inadequately-controlled or new-onset partial seizures. Patients were hospitalized and randomized to either Oxcarbazepine 10 mg/kg/day or were titrated up to 40-60 mg/kg/day within three days while withdrawing the previous AED on the second day of Oxcarbazepine therapy. Seizures were recorded through continuous video-EEG monitoring from Day 3 to Day 5. Patients either completed the 5-day treatment or met one of the two exit criteria: 1) three study-specific seizures (i.e., electrographic partial seizures with a behavioral correlate), 2) a prolonged study-specific seizure. The primary measure of effectiveness was a between-group comparison of the time to meet exit criteria in which the difference between the curves was not statistically significant (p=0.904). The majority of patients from both dose groups completed the 5-day study without exiting.
- Although this study failed to demonstrate an effect of oxcarbazepine as monotherapy in pediatric patients, several design elements, including the short treatment and assessment period, the absence of a true placebo, and the likely persistence of plasma levels of previously administered AEDs during the treatment period, make the results uninterpretable. For this reason, the results do not undermine the conclusion, based on pharmacokinetic/pharmacodynamic considerations, that oxcarbazepine is effective as monotherapy in pediatric patients 4 years old and older.
Oxcarbazepine Adjunctive Therapy Trials
- The effectiveness of Oxcarbazepine as an adjunctive therapy for partial seizures was established in two multicenter, randomized, double-blind, placebo-controlled trials, one in 692 patients (15-66 years of age) and one in 264 pediatric patients (3-17 years of age), and in one multicenter, rater-blind, randomized, age-stratified, parallel-group study comparing two doses of Oxcarbazepine in 128 pediatric patients (1 month to <4 years of age).
- Patients in the two placebo-controlled trials were on 1-3 concomitant AEDs. In both of the trials, patients were stabilized on optimum dosages of their concomitant AEDs during an 8-week baseline phase. Patients who experienced at least 8 (minimum of 1-4 per month) partial seizures during the baseline phase were randomly assigned to placebo or to a specific dose of Oxcarbazepine in addition to their other AEDs.
- In these studies, the dose was increased over a two-week period until either the assigned dose was reached, or intolerance prevented increases. Patients then entered a 14- (pediatrics) or 24-week (adults) maintenance period.
- In the adult trial, patients received fixed doses of 600, 1200 or 2400 mg/day. In the pediatric trial, patients received maintenance doses in the range of 30-46 mg/kg/day, depending on baseline weight. The primary measure of effectiveness in both trials was a between-group comparison of the percentage change in partial seizure frequency in the double-blind treatment phase relative to baseline phase. This comparison was statistically significant in favor of Oxcarbazepine at all doses tested in both trials (p=0.0001 for all doses for both trials). The number of patients randomized to each dose, the median baseline seizure rate, and the median percentage seizure rate reduction for each trial are shown in Table 8. It is important to note that in the high-dose group in the study in adults, over 65% of patients discontinued treatment because of adverse events; only 46 (27%) of the patients in this group completed the 28-week study, an outcome not seen in the monotherapy studies.
- Subset analyses of the antiepileptic efficacy of Oxcarbazepine with regard to gender in these trials revealed no important differences in response between men and women. Because there were very few patients over the age of 65 in controlled trials, the effect of the drug in the elderly has not been adequately assessed.
- The third adjunctive therapy trial enrolled 128 pediatric patients (1 month to <4 years of age) with inadequately-controlled partial seizures on 1-2 concomitant AEDs. Patients who experienced at least 2 study-specific seizures (i.e., electrographic partial seizures with a behavioral correlate) during the 72-hour baseline period were randomly assigned to either Oxcarbazepine10 mg/kg/day or were titrated up to 60 mg/kg/day within 26 days. Patients were maintained on their randomized target dose for 9 days and seizures were recorded through continuous video-EEG monitoring during the last 72 hours of the maintenance period. The primary measure of effectiveness in this trial was a between-group comparison of the change in seizure frequency per 24 hours compared to the seizure frequency at baseline. For the entire group of patients enrolled, this comparison was statistically significant in favor of Oxcarbazepine 60 mg/kg/day. In this study, there was no evidence that Oxcarbazepine was effective in patients below the age of 2 years (N=75).
How Supplied
- 150 mg Film-Coated Tablets: Oval, Orange yellow film coated tablet, scored on both sides, debossed with ‘J’ and ‘232’ on either side of the score line on one side.
- Bottles of 100 NDC 59746-232-01.
- Bottles of 500 NDC 59746-232-05.
- 300 mg Film-Coated Tablets: Oval, Orange yellow film coated tablet, scored on both sides, debossed with ‘J’ and ‘233’ on either side of the score line on one side.
- Bottles of 100 NDC 59746-233-01.
- Bottles of 500 NDC 59746-233-05.
- 600 mg Film-Coated Tablets: Oval, Orange yellow film coated tablet, scored on both sides, debossed with ‘J’ and ‘234’ on either side of the score line on one side.
- Bottles of 100 NDC 59746-234-01.
- Bottles of 500 NDC 59746-234-05
- Store at 20°C to 25°C (68°F - 77°F) excursions permitted to 15°-30°C (59°-86°F). Dispense in tight container (USP).
Storage
There is limited information regarding Oxcarbazepine Storage in the drug label.
Images
Drug Images
{{#ask: Page Name::Oxcarbazepine |?Pill Name |?Drug Name |?Pill Ingred |?Pill Imprint |?Pill Dosage |?Pill Color |?Pill Shape |?Pill Size (mm) |?Pill Scoring |?NDC |?Drug Author |format=template |template=DrugPageImages |mainlabel=- |sort=Pill Name }}
Package and Label Display Panel
{{#ask: Label Page::Oxcarbazepine |?Label Name |format=template |template=DrugLabelImages |mainlabel=- |sort=Label Page }}
Patient Counseling Information
- Patients and caregivers should be informed of the availability of a Medication Guide, and they should be instructed to read the Medication Guide prior to taking Oxcarbazepine Tablets.
- Patients should be advised that Oxcarbazepine Tablets may reduce the serum sodium concentrations especially if they are taking other medications that can lower sodium. Patients should be advised to report symptoms of low sodium like nausea, tiredness, lack of energy, confusion, and more frequent or more severe seizures.
- Anaphylactic reactions and angioedema may occur during treatment with Oxcarbazepine Tablets. Patients should be advised to report immediately signs and symptoms suggesting angioedema (swelling of the face, eyes, lips, tongue or difficulty in swallowing or breathing) and to stop taking the drug until they have consulted with their physician.
- Patients who have exhibited hypersensitivity reactions to carbamazepine should be informed that approximately 25%-30% of these patients may experience hypersensitivity reactions with Oxcarbazepine. Patients should be advised that if they experience a hypersensitivity reaction while taking Oxcarbazepine Tablets they should consult with their physician immediately.
- Patients should be advised that serious skin reactions have been reported in association with Oxcarbazepine Tablets. In the event a skin reaction should occur while taking Oxcarbazepine Tablets, patients should consult with their physician immediately
- Patients should be instructed that a fever associated with other organ system involvement (rash, lymphadenopathy, etc.) may be drug related and should be reported to the physician immediately
- Patients should be advised that there have been rare reports of blood disorders reported in patients treated with Oxcarbazepine. Patients should be instructed to immediately consult with their physician if they experience symptoms suggestive of blood disorders.
- Female patients of childbearing age should be warned that the concurrent use of Oxcarbazepine with hormonal contraceptives may render this method of contraception less effective. Additional non-hormonal forms of contraception are recommended when using Oxcarbazepine.
- Patients, their caregivers, and families should be counseled that AEDs, including Oxcarbazepine Tablets, may increase the risk of suicidal thoughts and behavior and should be advised of the need to be alert for the emergence or worsening of symptoms of depression, any unusual changes in mood or behavior, or the emergence of suicidal thoughts, behavior, or thoughts about self-harm. Behaviors of concern should be reported immediately to healthcare providers.
- Caution should be exercised if alcohol is taken in combination with Oxcarbazepine therapy, due to a possible additive sedative effect.
- Patients should be advised that Oxcarbazepine Tablets may cause dizziness and somnolence. Accordingly, patients should be advised not to drive or operate machinery until they have gained sufficient experience on Oxcarbazepine Tablets to gauge whether it adversely affects their ability to drive or operate machinery.
- Patients should be encouraged to enroll in the North American Antiepileptic Drug (NAAED) Pregnancy Registry if they become pregnant. This registry is collecting information about the safety of antiepileptic drugs during pregnancy. To enroll, patients can call the toll free number 1-888-233-2334.
Precautions with Alcohol
- Caution should be exercised if alcohol is taken in combination with Oxcarbazepine therapy, due to a possible additive sedative effect.
Brand Names
- OXCARBAZEPINE®[1]
Look-Alike Drug Names
There is limited information regarding Oxcarbazepine Look-Alike Drug Names in the drug label.
Price
References
The contents of this FDA label are provided by the National Library of Medicine.
{{#subobject:
|Page Name=Oxcarbazepine
|Pill Name=No image.jpg
|Drug Name=
|Pill Ingred=|+sep=;
|Pill Imprint=
|Pill Dosage={{{dosageValue}}} {{{dosageUnit}}}
|Pill Color=|+sep=;
|Pill Shape=
|Pill Size (mm)=
|Pill Scoring=
|Pill Image=
|Drug Author=
|NDC=
}}
{{#subobject:
|Label Page=Oxcarbazepine |Label Name=Oxcarbazepine10.png
}}
{{#subobject:
|Label Page=Oxcarbazepine |Label Name=Oxcarbazepine11.png
}}
{{#subobject:
|Label Page=Oxcarbazepine |Label Name=Oxcarbazepine12.png
}}
{{#subobject:
|Label Page=Oxcarbazepine |Label Name=Oxcarbazepine13.png
}}