COVID-19-associated heart failure: Difference between revisions
| Line 53: | Line 53: | ||
[[File:Mitra.Figure 3.jpg]] | [[File:Mitra.Figure 3.jpg]] | ||
{| class="wikitable" | |||
|+ | |||
|- | |||
| align="center" style="background: #4479BA; color: #FFFFFF |'''Common Precipitating factors in COVID-19 patients''' | |||
|- | |||
|'''[[Cardiac]]''' | |||
|- | |||
| | |||
* [[Myocardial ischemia]] | |||
|- | |||
| | |||
* [[Arrhythmias]] (tachy- or brady Arrhythmias) | |||
|- | |||
| | |||
* [[Stress-induced cardiomyopathy]] | |||
|- | |||
| | |||
* [[Myocardial injury]] | |||
|- | |||
| | |||
*Myocarditis | |||
|- | |||
|- | |||
|'''Pressure overload ''' | |||
|- | |||
| | |||
*[[Hypertensive urgency]] or emergency | |||
|- | |||
|- | |||
|'''Volume overload ''' | |||
|- | |||
| | |||
* Decreased compliance with [[diuretics]] | |||
|- | |||
| | |||
* Renal dysfunction | |||
|- | |||
|- | |||
|'''Pulmonary''' | |||
|- | |||
| | |||
*[[Acute Pulmonary embolism]] | |||
|- | |||
| | |||
*[[Hypoxia]] | |||
|- | |||
| | |||
*[[Pneumonia]] | |||
|- | |||
| | |||
*[[Acute respiratory distress syndrome]] | |||
|- | |||
|- | |||
|'''Increased systemic metabolic demand ''' | |||
|- | |||
| | |||
*[[Fever]] | |||
|- | |||
| | |||
*[[Sepsis]] | |||
|- | |||
|- | |||
|'''Iatrogenic''' | |||
|- | |||
| | |||
*Cardiovascular toxicity of medications | |||
|- | |||
| | |||
*Aggressive fluid resuscitation | |||
|- | |||
|- | |||
|'''Others''' | |||
|- | |||
| | |||
*Anemia | |||
|- | |||
| | |||
*Decreased compliance with heart failure medications | |||
==Causes== | ==Causes== | ||
Revision as of 10:05, 17 July 2020
For COVID-19 frequently asked inpatient questions, click here
For COVID-19 frequently asked outpatient questions, click here
|
COVID-19 Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
COVID-19-associated heart failure On the Web |
|
American Roentgen Ray Society Images of COVID-19-associated heart failure |
|
Risk calculators and risk factors for COVID-19-associated heart failure |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Mitra Chitsazan, M.D.[2]Mandana Chitsazan, M.D. [3]
Synonyms and keywords: Novel coronavirus, COVID-19, Wuhan coronavirus, coronavirus disease-19, coronavirus disease 2019, SARS-CoV-2, COVID-19, COVID-19, 2019-nCoV, 2019 novel coronavirus, heart failure, acute heart failure, de novo acute heart failure, chronic heart failure, acute decompensated heart failure, HFrEF, HFpEF, heart failure with reduced ejection fraction, heart failure with a preserved ejection fraction
Overview
Both de novo acute heart failure and acute decompensation of chronic heart failure can occur in patients with COVID-19. Patients with chronic heart failure may be at higher risk of developing severe COVID-19 infection due to the advanced age and the presence of multiple comorbidities.
Historical perspective
- In late December 2019, the novel coronavirus, SARS-CoV-2, originated from Wuhan, China. [1]
- The World Health Organization(WHO) declared the outbreak a Public Health Emergency of International Concern On January 30, 2020, [2] and a pandemic on March 12, 2020. [3]
- On March 27, 2020, Inciardi et al. reported the first case of acute myopericarditis complicated by heart failure in an otherwise healthy 53-year-old woman one week after the onset of symptoms of COVID-19. [4]
Classification
- Heart Failure ((HF) in COVID-19 may be classified similarly to heart failure from other causes.
- In general, heart failure can be classified based on:
- The pathophysiology of heart failure:
- The duration of symptoms:
- Acute HF (AHF) vs chronic HF (CHF)
- The underlying physiology based on left ventricular ejection fraction (LVEF):
- The severity of heart failure (i.e., the New York Heart Association Class I-IV)
- The stage of congestive heart failure (i.e., AHA Class A, B, C, D)
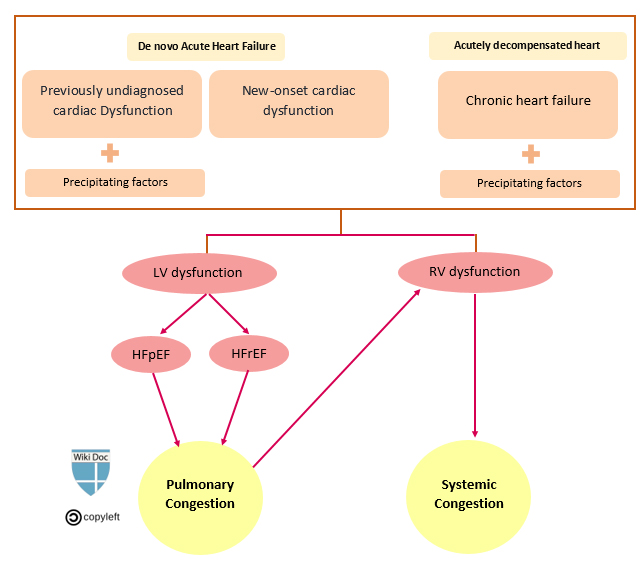
- Acute heart failure has two forms:
- Newly-arisen (“de novo”) acute heart failure
- Acutely decompensated chronic heart failure (ADCHF)
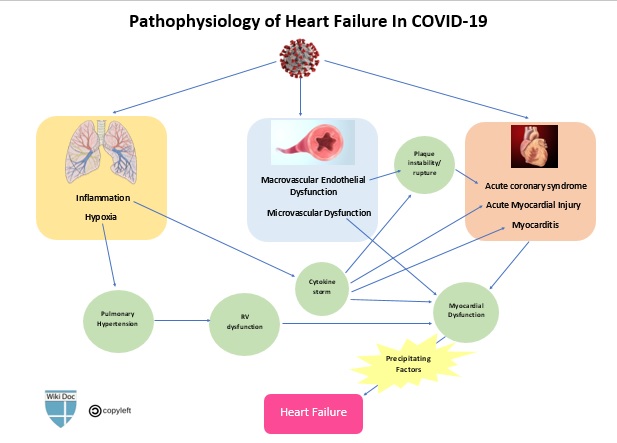
Pathophysiology
- Presumed pathophysiologic mechanisms for the development of new or decompensated heart failure in patients with COVID-19 include:[5] [6] [7] [8] [9]
- Acute exacerbation of chronic heart failure caused by precipitating factors
- Acute myocardial injury (which in turn can be caused by several mechanisms)
- Stress cardiomyopathy (i.e., Takotsubo cardiomyopathy) [10] [11]
- Impaired myocardial relaxation resulting in diastolic dysfunction [i.e., Heart failure with preserved ejection fraction (HFpEF) ]
- Right-sided heart failure, secondary to pulmonary hypertension caused by hypoxia and acute respiratory distress syndrome (ARDS)
| Common Precipitating factors in COVID-19 patients |
| Cardiac |
|
|
| Pressure overload |
|
| Volume overload |
|
|
| Pulmonary |
| Increased systemic metabolic demand |
| Iatrogenic |
|
|
| Others |
|
CausesAcute heart failure in COVID-19 patients may be caused by: [10] [11]
Differentiating (COVID-19 associated heart failure)) from other DiseasesIn patients with COVID-19 infection, acute heart failure should be differentiated from other diseases presenting with dyspnea and/or tachypnea. The differentials include the following:
Epidemiology and Demographics
Risk Factors
To read more on the risk factors of congestive heart failure, click here. Screening
Natural History, Complications, and Prognosis
DiagnosisHistory and Symptoms
Physical Examination
Laboratory Findings
Electrocardiogram
X-ray
Echocardiography or Ultrasound
CT scan
In patients with cardiogenic pulmonary edema, caused by increased pulmonary vasculature hydrostatic pressure, bilateral pleural effusions are also frequently seen. CMR
TreatmentMedical Therapy
Interventional therapy
Surgery
Primary Prevention
Secondary Prevention
References
|