Dolutegravir
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Alberto Plate [2]
WikiDoc MAKES NO GUARANTEE OF VALIDITY. WikiDoc is not a professional health care provider, nor is it a suitable replacement for a licensed healthcare provider. WikiDoc is intended to be an educational tool, not a tool for any form of healthcare delivery. The educational content on WikiDoc drug pages is based upon the FDA package insert, National Library of Medicine content and practice guidelines / consensus statements. WikiDoc does not promote the administration of any medication or device that is not consistent with its labeling. Please read our full disclaimer here.
Overview
Dolutegravir is a antiviral that is FDA approved for the treatment of HIV-1 infection. Common adverse reactions include hyperglycemia, increased serum lipase level, headache, insomnia.
Adult Indications and Dosage
FDA-Labeled Indications and Dosage (Adult)
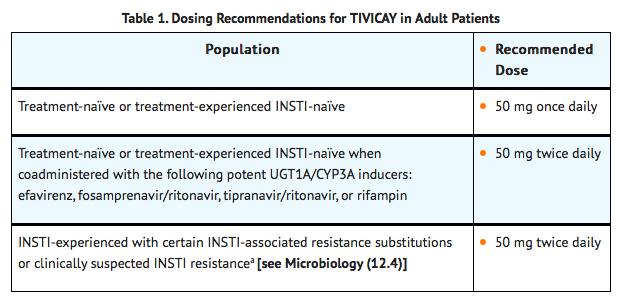
Off-Label Use and Dosage (Adult)
Guideline-Supported Use
There is limited information regarding Off-Label Guideline-Supported Use of Dolutegravir in adult patients.
Non–Guideline-Supported Use
There is limited information regarding Off-Label Non–Guideline-Supported Use of Dolutegravir in adult patients.
Pediatric Indications and Dosage
FDA-Labeled Indications and Dosage (Pediatric)
Treatment-naïve or Treatment-experienced INSTI-naïve
- The recommended dose of Dolutegravir in pediatric patients aged 12 years and older and weighing at least 40 kg is 50 mg administered orally once daily.
- If efavirenz, fosamprenavir/ritonavir, tipranavir/ritonavir, or rifampin are coadministered, the recommended dose of Dolutegravir is 50 mg twice daily.
- Safety and efficacy of Dolutegravir have not been established in pediatric patients younger than 12 years or weighing less than 40 kg, or in pediatric patients who are INSTI-experienced with documented or clinically suspected resistance to other INSTIs (raltegravir, elvitegravir).
Off-Label Use and Dosage (Pediatric)
Guideline-Supported Use
There is limited information regarding Off-Label Guideline-Supported Use of Dolutegravir in pediatric patients.
Non–Guideline-Supported Use
There is limited information regarding Off-Label Non–Guideline-Supported Use of Dolutegravir in pediatric patients.
Contraindications
Dolutegravir is contraindicated in patients:
- With previous hypersensitivity reaction to dolutegravir
- Receiving dofetilide due to the potential for increased dofetilide plasma concentrations and the risk for serious and/or life-threatening events.
Warnings
Hypersensitivity Reactions
- Hypersensitivity reactions have been reported and were characterized by rash, constitutional findings, and sometimes organ dysfunction, including liver injury. The events were reported in less than 1% of subjects receiving Dolutegravir in Phase 3 clinical trials. Discontinue Dolutegravir and other suspect agents immediately if signs or symptoms of hypersensitivity reactions develop (including, but not limited to, severe rash or rash accompanied by fever, general malaise, fatigue, muscle or joint aches, blisters or peeling of the skin, oral blisters or lesions, conjunctivitis, facial edema, hepatitis, eosinophilia, angioedema, difficulty breathing). Clinical status, including liver aminotransferases, should be monitored and appropriate therapy initiated. Delay in stopping treatment with Dolutegravir or other suspect agents after the onset of hypersensitivity may result in a life-threatening reaction. Dolutegravir is contraindicated in patients who have experienced a previous hypersensitivity reaction to dolutegravir.
Effects on Serum Liver Biochemistries in Patients with Hepatitis B or C Coinfection
- Patients with underlying hepatitis B or hepatitis C may be at increased risk for worsening or development of transaminase elevations with use of Dolutegravir In some cases the elevations in transaminases were consistent with immune reconstitution syndrome or hepatitis B reactivation particularly in the setting where anti-hepatitis therapy was withdrawn. Appropriate laboratory testing prior to initiating therapy and monitoring for hepatotoxicity during therapy with Dolutegravir are recommended in patients with underlying hepatic disease such as hepatitis B or hepatitis C.
Fat Redistribution
- Redistribution/accumulation of body fat, including central obesity, dorsocervical fat enlargement (buffalo hump), peripheral wasting, facial wasting, breast enlargement, and “cushingoid appearance” have been observed in patients receiving antiretroviral therapy. The mechanism and long-term consequences of these events are currently unknown. A causal relationship has not been established.
Immune Reconstitution Syndrome
- Immune reconstitution syndrome has been reported in patients treated with combination antiretroviral therapy, including Dolutegravir During the initial phase of combination antiretroviral treatment, patients whose immune systems respond may develop an inflammatory response to indolent or residual opportunistic infections (such as Mycobacterium avium infection, cytomegalovirus, Pneumocystis jirovecii pneumonia PCP, or tuberculosis), which may necessitate further evaluation and treatment.
- Autoimmune disorders (such as Graves’ disease, polymyositis, and Guillain-Barré syndrome) have also been reported to occur in the setting of immune reconstitution; however, the time to onset is more variable and can occur many months after initiation of treatment.
Adverse Reactions
Clinical Trials Experience
Treatment in Adult Subjects
Treatment‑emergent Adverse Drug Reactions (ADRs)
Treatment-naïve Subjects
- The safety assessment of Dolutegravir in HIV‑1‑infected treatment-naïve subjects is based on the analyses of 96-week data from 2 international, multicenter, double-blind trials, SPRING-2 (ING113086) and SINGLE (ING114467) and 48-week data from the international, multicenter, open-label FLAMINGO (ING114915) trial.
- In SPRING-2, 822 subjects were randomized and received at least 1 dose of either Dolutegravir 50 mg once daily or raltegravir 400 mg twice daily, both in combination with fixed-dose dual nucleoside reverse transcriptase inhibitor (NRTI) treatment (either abacavir sulfate and lamivudine [EPZICOM®] or emtricitabine/tenofovir TRUVADA®). There were 808 subjects included in the efficacy and safety analyses. Through 96 weeks, the rate of adverse events leading to discontinuation was 2% in both treatment arms.
- In SINGLE, 833 subjects were randomized and received at least 1 dose of either Dolutegravir 50 mg with fixed-dose abacavir sulfate and lamivudine (EPZICOM) once daily or fixed-dose efavirenz/emtricitabine/tenofovir once daily. Through 96 weeks, the rates of adverse events leading to discontinuation were 3% in subjects receiving Dolutegravir 50 mg once daily + EPZICOM and 12% in subjects receiving once daily.
- Treatment-emergent ADRs of moderate to severe intensity observed in at least 2% of subjects in either treatment arm in SPRING-2 and SINGLE trials are provided in Table 2. Side-by-side tabulation is to simplify presentation; direct comparisons across trials should not be made due to differing trial designs.
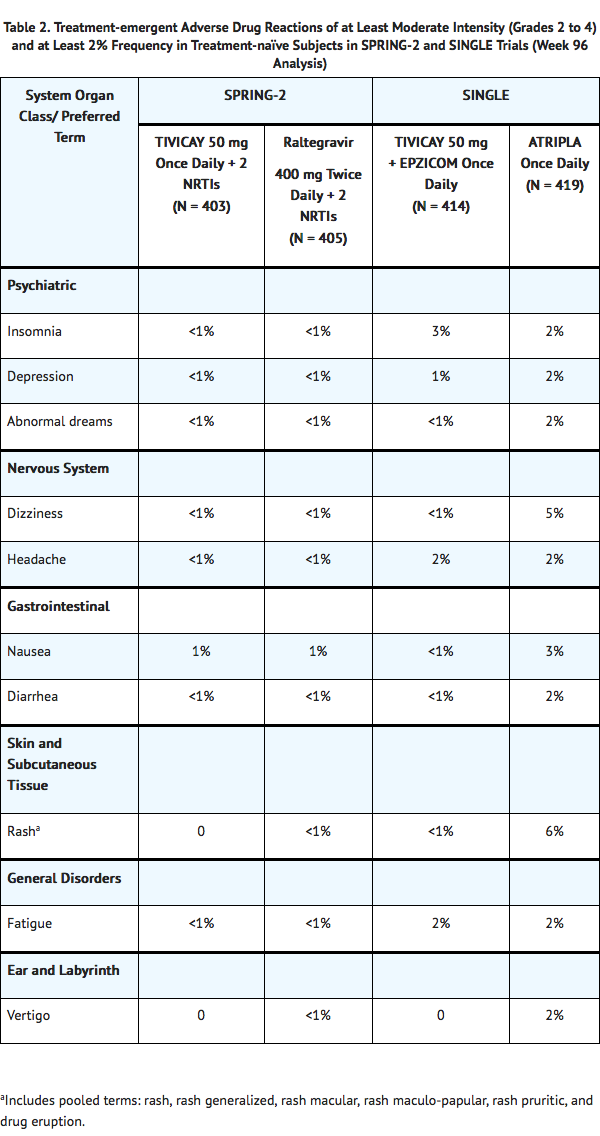
- In addition, Grade 1 insomnia was reported by 1% and less than 1% of subjects receiving Dolutegravir and raltegravir, respectively, in SPRING-2; whereas in SINGLE the rates were 7% and 4% for Dolutegravir and , respectively. These events were not treatment limiting.
- In a multicenter, open-label trial (FLAMINGO), 243 subjects received Dolutegravir 50 mg once daily versus 242 subjects who received darunavir 800 mg/ritonavir 100 mg once daily, both in combination with investigator-selected NRTI background regimen (either EPZICOM or TRUVADA). There were 484 subjects included in the efficacy and safety analyses. Through 48 weeks, the rates of adverse events leading to discontinuation were 2% in subjects receiving Dolutegravir and 4% in subjects receiving darunavir/ritonavir. The ADRs observed in FLAMINGO were generally consistent with those seen in SPRING-2 and SINGLE.
- Treatment-experienced, Integrase Strand Transfer Inhibitor-naïve Subjects: In an international, multicenter, double-blind trial (ING111762, SAILING), 719 HIV‑1‑infected, antiretroviral treatment-experienced adults were randomized and received either Dolutegravir 50 mg once daily or raltegravir 400 mg twice daily with investigator-selected background regimen consisting of up to 2 agents, including at least one fully active agent. At 48 weeks, the rates of adverse events leading to discontinuation were 3% in subjects receiving Dolutegravir 50 mg once daily + background regimen and 4% in subjects receiving raltegravir 400 mg twice daily + background regimen.
- The only treatment-emergent ADR of moderate to severe intensity with at least 2% frequency in either treatment group was diarrhea, 2% (6 of 354) in subjects receiving Dolutegravir 50 mg once daily + background regimen and 1% (5 of 361) in subjects receiving raltegravir 400 mg twice daily + background regimen.
- Treatment-experienced, Integrase Strand Transfer Inhibitor-experienced Subjects: In a multicenter, open-label, single-arm trial (ING112574, VIKING-3), 183 HIV‑1‑infected, antiretroviral treatment-experienced adults with virological failure and current or historical evidence of raltegravir and/or elvitegravir resistance received Dolutegravir 50 mg twice daily with the current failing background regimen for 7 days and with optimized background therapy from Day 8. The rate of adverse events leading to discontinuation was 4% of subjects at Week 48.
- Treatment-emergent ADRs in VIKING-3 were generally similar compared with observations with the 50-mg once-daily dose in adult Phase 3 trials.
Less Common Adverse Reactions Observed in Treatment-naïve and Treatment-experienced Trials
The following ADRs occurred in less than 2% of treatment-naïve or treatment-experienced subjects receiving Dolutegravir in a combination regimen in any one trial. These events have been included because of their seriousness and assessment of potential causal relationship.
- Gastrointestinal Disorders: Abdominal pain, abdominal discomfort, flatulence, vomiting.
- General Disorders: Fatigue.
- Hepatobiliary Disorders: Hepatitis.
- Musculoskeletal Disorders: Myositis.
- Psychiatric Disorders: Suicidal ideation, attempt, behavior, or completion. These events were observed primarily in subjects with a pre-existing history of depression or other psychiatric illness.
- Renal and Urinary Disorders: Renal impairment.
Skin and Subcutaneous Tissue Disorders: Pruritus.
Laboratory Abnormalities
- Treatment-naïve Subjects: Selected laboratory abnormalities (Grades 2 to 4) with a worsening grade from baseline and representing the worst-grade toxicity in at least 2% of subjects are presented in Table 3. The mean change from baseline observed for selected lipid values is presented in Table 4. Side-by-side tabulation is to simplify presentation; direct comparisons across trials should not be made due to differing trial designs.
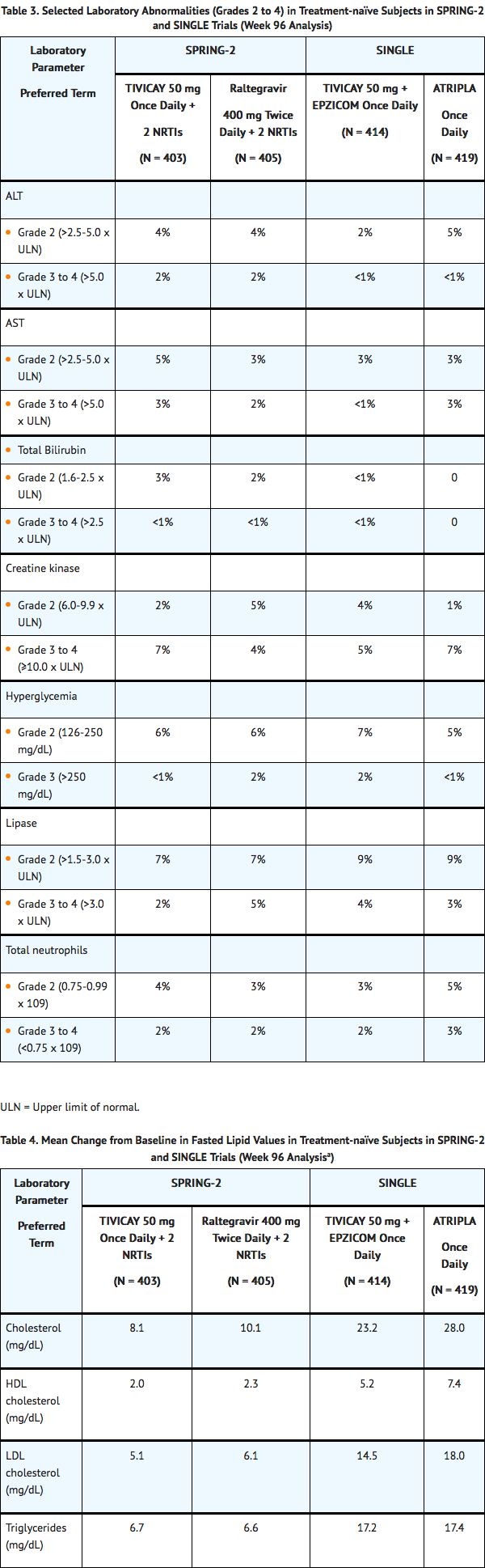
- Laboratory abnormalities observed in the FLAMINGO trial were generally consistent with observations in SPRING-2 and SINGLE. Treatment-experienced, Integrase Strand Transfer Inhibitor-naïve Subjects: Laboratory abnormalities observed in SAILING were generally similar compared with observations seen in the treatment-naïve (SPRING-2 and SINGLE) trials.
Treatment-experienced, Integrase Strand Transfer Inhibitor-experienced Subjects
- The most common treatment-emergent laboratory abnormalities (greater than 5% for Grades 2 to 4 combined) observed in VIKING-3 at Week 48 were elevated ALT (9%), AST (8%), cholesterol (10%), creatine kinase (6%), hyperglycemia (14%), and lipase (10%). Two percent (4 of 183) of subjects had a Grade 3 to 4 treatment-emergent hematology laboratory abnormality, with neutropenia (2% [3 of 183]) being the most frequently reported.
Hepatitis B and/or Hepatitis C Virus Co-infection
- In Phase 3 trials, subjects with hepatitis B and/or hepatitis C virus co-infection were permitted to enroll provided that baseline liver chemistry tests did not exceed 5 times the upper limit of normal. Overall, the safety profile in subjects with hepatitis B and/or hepatitis C virus co-infection was similar to that observed in subjects without hepatitis B or hepatitis C co-infection, although the rates of AST and ALT abnormalities were higher in the subgroup with hepatitis B and/or hepatitis C virus co-infection for all treatment groups. Grades 2 to 4 ALT abnormalities in hepatitis B and/or hepatitis C co-infected compared with HIV mono-infected subjects receiving Dolutegravir were observed in 18% vs. 3% with the 50-mg once-daily dose and 13% vs. 8% with the 50-mg twice-daily dose. Liver chemistry elevations consistent with immune reconstitution syndrome were observed in some subjects with hepatitis B and/or hepatitis C at the start of therapy with Dolutegravir, particularly in the setting where anti-hepatitis therapy was withdrawn.
Changes in Serum Creatinine
- Dolutegravir has been shown to increase serum creatinine due to inhibition of tubular secretion of creatinine without affecting renal glomerular function. Increases in serum creatinine occurred within the first 4 weeks of treatment and remained stable through 48 to 96 weeks. In treatment-naïve subjects, a mean change from baseline of 0.15 mg per dL (range: -0.32 mg per dL to 0.65 mg per dL) was observed after 96 weeks of treatment. Creatinine increases were comparable by background NRTIs and were similar in treatment-experienced subjects.
Clinical Trials Experience in Pediatric Subjects
- IMPAACT P1093 is an ongoing multicenter, open-label, non-comparative trial of approximately 160 HIV‑1‑infected pediatric subjects aged 6 weeks to less than 18 years, of which 23 treatment-experienced, INSTI-naïve subjects aged 12 to less than 18 years were enrolled.
- The adverse reaction profile was similar to that for adults. Grade 2 ADRs reported in at least 1 subject were rash (n = 1), abdominal pain (n = 1), and diarrhea (n = 1). No Grade 3 or 4 ADRs were reported. The Grade 3 laboratory abnormalities were elevated total bilirubin and lipase reported in 1 subject each. No Grade 4 laboratory abnormalities were reported. The changes in mean serum creatinine were similar to those observed in adults.
Postmarketing Experience
There is limited information regarding Dolutegravir Postmarketing Experience in the drug label.
Drug Interactions
Effect of Dolutegravir on the Pharmacokinetics of Other Agents
- In vitro, dolutegravir inhibited the renal organic cation transporters, OCT2 (IC50 = 1.93 µM) and multidrug and toxin extrusion transporter (MATE) 1 (IC50 = 6.34 µM). In vivo, dolutegravir inhibits tubular secretion of creatinine by inhibiting OCT2 and potentially MATE1. Dolutegravir may increase plasma concentrations of drugs eliminated via OCT2 or MATE1 (dofetilide and metformin). In vitro, dolutegravir inhibited the basolateral renal transporters, organic anion transporter (OAT) 1 (IC50 = 2.12 µM) and OAT3 (IC50 = 1.97 µM). However, in vivo, dolutegravir did not alter the plasma concentrations of tenofovir or para-amino hippurate, substrates of OAT1 and OAT3.
- In vitro, dolutegravir did not inhibit (IC50 greater than 50 μM) the following: cytochrome P450 (CYP)1A2, CYP2A6, CYP2B6, CYP2C8, CYP2C9, CYP2C19, CYP2D6, CYP3A, uridine diphosphate (UDP)-glucuronosyl transferase 1A1 (UGT1A1), UGT2B7, P-glycoprotein (P-gp), breast cancer resistance protein (BCRP), bile salt export pump (BSEP), organic anion transporter polypeptide (OATP)1B1, OATP1B3, OCT1, multidrug resistance protein (MRP)2, or MRP4. In vitro, dolutegravir did not induce CYP1A2, CYP2B6, or CYP3A4. Based on these data and the results of drug interaction trials, dolutegravir is not expected to affect the pharmacokinetics of drugs that are substrates of these enzymes or transporters.
- In drug interaction trials, dolutegravir did not have a clinically relevant effect on the pharmacokinetics of the following drugs: tenofovir, methadone, midazolam, rilpivirine, and oral contraceptives containing norgestimate and ethinyl estradiol. Using cross-study comparisons to historical pharmacokinetic data for each interacting drug, dolutegravir did not appear to affect the pharmacokinetics of the following drugs: atazanavir, darunavir, efavirenz, etravirine, fosamprenavir, lopinavir, ritonavir, boceprevir, and telaprevir.
Effect of Other Agents on the Pharmacokinetics of Dolutegravir
- Dolutegravir is metabolized by UGT1A1 with some contribution from CYP3A. Dolutegravir is also a substrate of UGT1A3, UGT1A9, BCRP, and P-gp in vitro. Drugs that induce those enzymes and transporters may decrease dolutegravir plasma concentration and reduce the therapeutic effect of dolutegravir. Coadministration of dolutegravir and other drugs that inhibit these enzymes may increase dolutegravir plasma concentration.
- Etravirine significantly reduced plasma concentrations of dolutegravir, but the effect of etravirine was mitigated by coadministration of lopinavir/ritonavir or darunavir/ritonavir, and is expected to be mitigated by atazanavir/ritonavir. Darunavir/ritonavir, lopinavir/ritonavir, rilpivirine, tenofovir, boceprevir, telaprevir, prednisone, rifabutin, and omeprazole had no clinically significant effect on the pharmacokinetics of dolutegravir.
Established and Other Potentially Significant Drug Interactions
- Table 5 provides clinical recommendations as a result of drug interactions with Dolutegravir These recommendations are based on either drug interaction trials or predicted interactions due to the expected magnitude of interaction and potential for serious adverse events or loss of efficacy.

Use in Specific Populations
Pregnancy
Pregnancy Category (FDA): B There are no adequate and well-controlled studies in pregnant women. Because animal reproduction studies are not always predictive of human response, and dolutegravir was shown to cross the placenta in animal studies, this drug should be used during pregnancy only if clearly needed.
Antiretroviral Pregnancy Registry
- To monitor maternal-fetal outcomes of pregnant women with HIV exposed to Dolutegravir and other antiretroviral agents, an Antiretroviral Pregnancy Registry has been established. Physicians are encouraged to register patients by calling 1-800-258-4263.
Animal Data
- Reproduction studies have been performed in rats and rabbits at doses up to 27 times the human dose of 50 mg twice daily and have revealed no evidence of impaired fertility or harm to the fetus due to Dolutegravir.
- Oral administration of dolutegravir to pregnant rats at doses up to 1,000 mg per kg daily, approximately 27 times the 50-mg twice-daily human clinical exposure based on AUC, from days 6 to 17 of gestation did not elicit maternal toxicity, developmental toxicity, or teratogenicity.
- Oral administration of dolutegravir to pregnant rabbits at doses up to 1,000 mg per kg daily, approximately 0.4 times the 50‑mg twice-daily human clinical exposure based on AUC, from days 6 to 18 of gestation did not elicit developmental toxicity or teratogenicity. In rabbits, maternal toxicity (decreased food consumption, scant/no feces/urine, suppressed body weight gain) was observed at 1,000 mg per kg.
Pregnancy Category (AUS):
There is no Australian Drug Evaluation Committee (ADEC) guidance on usage of Dolutegravir in women who are pregnant.
Labor and Delivery
There is no FDA guidance on use of Dolutegravir during labor and delivery.
Nursing Mothers
- The Centers for Disease Control and Prevention recommend that HIV‑1‑infected mothers in the United States not breastfeed their infants to avoid risking postnatal transmission of HIV-1 infection. Studies in lactating rats and their offspring indicate that dolutegravir was present in rat milk. It is not known whether dolutegravir is excreted in human milk.
- Because of both the potential for HIV transmission and the potential for adverse reactions in nursing infants, instruct mothers not to breastfeed.
Pediatric Use
- Safety and efficacy of Dolutegravir have not been established in pediatric patients younger than 12 years, weighing less than 40 kg, or in any pediatric patients who are INSTI-experienced with documented or clinically suspected resistance to other INSTIs (raltegravir, elvitegravir).
- The safety, virologic, and immunologic responses in subjects who received Dolutegravir were evaluated in 23 treatment-experienced, INSTI-naïve, HIV‑1–infected subjects aged 12 to less than 18 years in an open-label, multicenter, dose-finding clinical trial, IMPAACT P1093. Pharmacokinetic parameters, evaluated in 9 subjects weighing at least 40 kg receiving 50 mg daily and 1 subject (weighing 37 kg) receiving 35 mg once daily, were similar to adults receiving 50 mg once daily. Frequency, type, and severity of adverse drug reactions in pediatric subjects were comparable to those observed in adults.
Geriatic Use
- Clinical trials of Dolutegravir did not include sufficient numbers of subjects aged 65 and older to determine whether they respond differently from younger subjects. In general, caution should be exercised in the administration of Dolutegravir in elderly patients reflecting the greater frequency of decreased hepatic, renal, or cardiac function, and of concomitant disease or other drug therapy.
Gender
There is no FDA guidance on the use of Dolutegravir with respect to specific gender populations.
Race
There is no FDA guidance on the use of Dolutegravir with respect to specific racial populations.
Renal Impairment
- Dolutegravir plasma concentrations were decreased in subjects with severe renal impairment compared with those in matched healthy controls. However, no dosage adjustment is necessary for treatment-naïve or treatment-experienced and INSTI-naïve patients with mild, moderate, or severe renal impairment or for INSTI-experienced patients (with certain INSTI-associated resistance substitutions or clinically suspected INSTI resistance) with mild or moderate renal impairment. Caution is warranted for INSTI-experienced patients (with certain INSTI-associated resistance substitutions or clinically suspected INSTI resistance with severe renal impairment, as the decrease in dolutegravir concentrations may result in loss of therapeutic effect and development of resistance to Dolutegravir or other coadministered antiretroviral agents. Dolutegravir has not been studied in patients on dialysis.
Hepatic Impairment
- No clinically important pharmacokinetic differences between subjects with moderate hepatic impairment and matching healthy subjects were observed. No dosage adjustment is necessary for patients with mild to moderate hepatic impairment (Child-Pugh Score A or B). The effect of severe hepatic impairment (Child-Pugh Score C) on the pharmacokinetics of dolutegravir has not been studied. Therefore, Dolutegravir is not recommended for use in patients with severe hepatic impairment.
Females of Reproductive Potential and Males
There is no FDA guidance on the use of Dolutegravir in women of reproductive potentials and males.
Immunocompromised Patients
There is no FDA guidance one the use of Dolutegravir in patients who are immunocompromised.
Administration and Monitoring
Administration
There is limited information regarding Dolutegravir Administration in the drug label.
Monitoring
There is limited information regarding Dolutegravir Monitoring in the drug label.
IV Compatibility
There is limited information regarding the compatibility of Dolutegravir and IV administrations.
Overdosage
- There is no known specific treatment for overdose with Dolutegravir If overdose occurs, the patient should be monitored and standard supportive treatment applied as required. As dolutegravir is highly bound to plasma proteins, it is unlikely that it will be significantly removed by dialysis.
Pharmacology
Mechanism of Action
- Dolutegravir inhibits HIV integrase by binding to the integrase active site and blocking the strand transfer step of retroviral deoxyribonucleic acid (DNA) integration which is essential for the HIV replication cycle. Strand transfer biochemical assays using purified HIV-1 integrase and pre-processed substrate DNA resulted in IC50 values of 2.7 nM and 12.6 nM.
Structure
- The empirical formula is C20H18F2N3NaO5 and the molecular weight is 441.36 g per mol. It has the following structural formula:
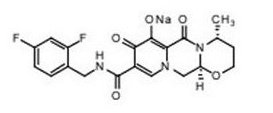
Pharmacodynamics
- In a randomized, dose-ranging trial, HIV‑1‑infected subjects treated with dolutegravir monotherapy demonstrated rapid and dose-dependent antiviral activity with mean declines from baseline to Day 11 in HIV-1 RNA of 1.5, 2.0, and 2.5 log10 for dolutegravir 2 mg, 10 mg, and 50 mg once daily, respectively. This antiviral response was maintained for 3 to 4 days after the last dose in the 50-mg group.
Effects on Electrocardiogram
- In a randomized, placebo-controlled, cross-over trial, 42 healthy subjects received single-dose oral administrations of placebo, dolutegravir 250-mg suspension (exposures approximately 3–fold of the 50-mg once-daily dose at steady state), and moxifloxacin 400 mg (active control) in random sequence. After baseline and placebo adjustment, the maximum mean QTc change based on Fridericia correction method (QTcF) for dolutegravir was 2.4 msec (1-sided 95% upper CI: 4.9 msec). Dolutegravir did not prolong the QTc interval over 24 hours postdose.
Effects on Renal Function
- The effect of dolutegravir on renal function was evaluated in an open-label, randomized, 3‑arm, parallel, placebo-controlled trial in healthy subjects (n = 37) who received dolutegravir 50 mg once daily (n = 12), dolutegravir 50 mg twice daily (n = 13), or placebo once daily (n = 12) for 14 days. A decrease in creatinine clearance, as determined by 24-hour urine collection, was observed with both doses of dolutegravir after 14 days of treatment in subjects who received 50 mg once daily (9% decrease) and 50 mg twice daily (13% decrease). Neither dose of dolutegravir had a significant effect on the actual glomerular filtration rate (determined by the clearance of probe drug, iohexol) or effective renal plasma flow (determined by the clearance of probe drug, para-amino hippurate) compared with the placebo.
Pharmacokinetics
- The pharmacokinetic properties of dolutegravir have been evaluated in healthy adult subjects and HIV‑1–infected adult subjects. Exposure to dolutegravir was generally similar between healthy subjects and HIV‑1–infected subjects. The non-linear exposure of dolutegravir following 50 mg twice daily compared with 50 mg once daily in HIV‑1–infected subjects (Table 6) was attributed to the use of metabolic inducers in the background antiretroviral regimens of subjects receiving dolutegravir 50 mg twice daily in clinical trials. Dolutegravir was administered without regard to food in these trials.
Table 6. Dolutegravir Steady-state Pharmacokinetic Parameter Estimates in HIV‑1–Infected Adults Parameter
Absorption
- Following oral administration of dolutegravir, peak plasma concentrations were observed 2 to 3 hours postdose. With once-daily dosing, pharmacokinetic steady state is achieved within approximately 5 days with average accumulation ratios for AUC, Cmax, and C24 h ranging from 1.2 to 1.5.
- Dolutegravir plasma concentrations increased in a less than dose-proportional manner above 50 mg. Dolutegravir is a P‑gp substrate in vitro. The absolute bioavailability of dolutegravir has not been established.
Effects of Food on Oral Absorption
- Dolutegravir may be taken with or without food. Food increased the extent of absorption and slowed the rate of absorption of dolutegravir. Low-, moderate-, and high-fat meals increased dolutegravir AUC(0-∞) by 33%, 41%, and 66%; increased Cmax by 46%, 52%, and 67%; and prolonged Tmax to 3, 4, and 5 hours from 2 hours under fasted conditions, respectively.
Distribution
- Dolutegravir is highly bound (greater than or equal to 98.9%) to human plasma proteins based on in vivo data and binding is independent of plasma concentration of dolutegravir. The apparent volume of distribution (Vd/F) following 50-mg once-daily administration is estimated at 17.4 L based on a population pharmacokinetic analysis.
- Cerebrospinal Fluid (CSF): In 12 treatment-naïve subjects on dolutegravir 50 mg daily plus abacavir/lamivudine, the median dolutegravir concentration in CSF was 13.2 ng per mL (range: 3.74 ng per mL to 18.3 ng per mL) 2 to 6 hours postdose after 16 weeks of treatment. The clinical relevance of this finding has not been established.
Metabolism and Elimination
- Dolutegravir is primarily metabolized via UGT1A1 with some contribution from CYP3A. After a single oral dose of [14C] dolutegravir, 53% of the total oral dose was excreted unchanged in feces. Thirty-one percent of the total oral dose was excreted in urine, represented by an ether glucuronide of dolutegravir (18.9% of total dose), a metabolite formed by oxidation at the benzylic carbon (3.0% of total dose), and its hydrolytic N-dealkylation product (3.6% of total dose). Renal elimination of unchanged drug was low (less than 1% of the dose).
- Dolutegravir has a terminal half-life of approximately 14 hours and an apparent clearance (CL/F) of 1.0 L per hour based on population pharmacokinetic analyses.
- Polymorphisms in Drug‑metabolizing Enzymes: In a meta-analysis of healthy subject trials, subjects with UGT1A1 (n = 7) genotypes conferring poor dolutegravir metabolism had a 32% lower clearance of dolutegravir and 46% higher AUC compared with subjects with genotypes associated with normal metabolism via UGT1A1 (n = 41).
Nonclinical Toxicology
Carcinogenesis, Mutagenesis, Impairment of Fertility
Carcinogenesis
- Two-year carcinogenicity studies in mice and rats were conducted with dolutegravir. Mice were administered doses of up to 500 mg per kg, and rats were administered doses of up to 50 mg per kg. In mice, no significant increases in the incidence of drug-related neoplasms were observed at the highest doses tested, resulting in dolutegravir AUC exposures approximately 14-fold higher than those in humans at the recommended dose of 50 mg twice daily. In rats, no increases in the incidence of drug-related neoplasms were observed at the highest dose tested, resulting in dolutegravir AUC exposures 10-fold and 15-fold higher in males and females, respectively, than those in humans at the recommended dose of 50 mg twice daily.
Mutagenesis
- Dolutegravir was not genotoxic in the bacterial reverse mutation assay, mouse lymphoma assay, or in the in vivo rodent micronucleus assay.
Impairment of Fertility
- In a study conducted in rats, there were no effects on mating or fertility with dolutegravir up to 1,000 mg per kg per day. This dose is associated with an exposure that is approximately 24 times higher than the exposure in humans at the recommended dose of 50 mg twice daily.
Clinical Studies
The efficacy of Dolutegravir is based on analyses of data from 3 trials, SPRING-2 (ING113086), SINGLE (ING114467), and FLAMINGO (ING114915), in treatment-naïve, HIV‑1‑infected subjects (n = 2,125); one trial, SAILING (ING111762), in treatment-experienced, INSTI-naïve HIV‑1‑infected subjects (n = 715); and from VIKING-3 (ING112574) trial in INSTI-experienced HIV‑1‑infected subjects (n = 183). The use of Dolutegravir in pediatric patients aged 12 years and older is based on evaluation of safety, pharmacokinetics, and efficacy through 24 weeks in a multicenter, open-label trial in subjects (n = 23) without INSTI resistance.
Adult Subjects
Treatment-naïve Subjects
- In SPRING-2, 822 subjects were randomized and received at least 1 dose of either Dolutegravir 50 mg once daily or raltegravir 400 mg twice daily, both in combination with fixed-dose dual NRTI treatment (either abacavir sulfate and lamivudine EPZICOM or emtricitabine/tenofovir TRUVADA). There were 808 subjects included in the efficacy and safety analyses. At baseline, the median age of subjects was 36 years, 13% female, 15% non-white, 11% had hepatitis B and/or hepatitis C virus co-infection, 2% were CDC Class C (AIDS), 28% had HIV-1 RNA greater than 100,000 copies per mL, 48% had CD4+ cell count less than 350 cells per mm3, and 39% received EPZICOM; these characteristics were similar between treatment groups.
- In SINGLE, 833 subjects were randomized and received at least 1 dose of either Dolutegravir 50 mg once daily with fixed-dose abacavir sulfate and lamivudine (EPZICOM) or fixed-dose efavirenz/emtricitabine/tenofovir. At baseline, the median age of subjects was 35 years, 16% female, 32% non-white, 7% had hepatitis C co-infection (hepatitis B virus co-infection was excluded), 4% were CDC Class C (AIDS), 32% had HIV-1 RNA greater than 100,000 copies per mL, and 53% had CD4+ cell count less than 350 cells per mm3; these characteristics were similar between treatment groups.
Week 96 outcomes for SPRING-2 and SINGLE are provided in Table 12. Side-by-side tabulation is to simplify presentation; direct comparisons across trials should not be made due to differing trial designs.
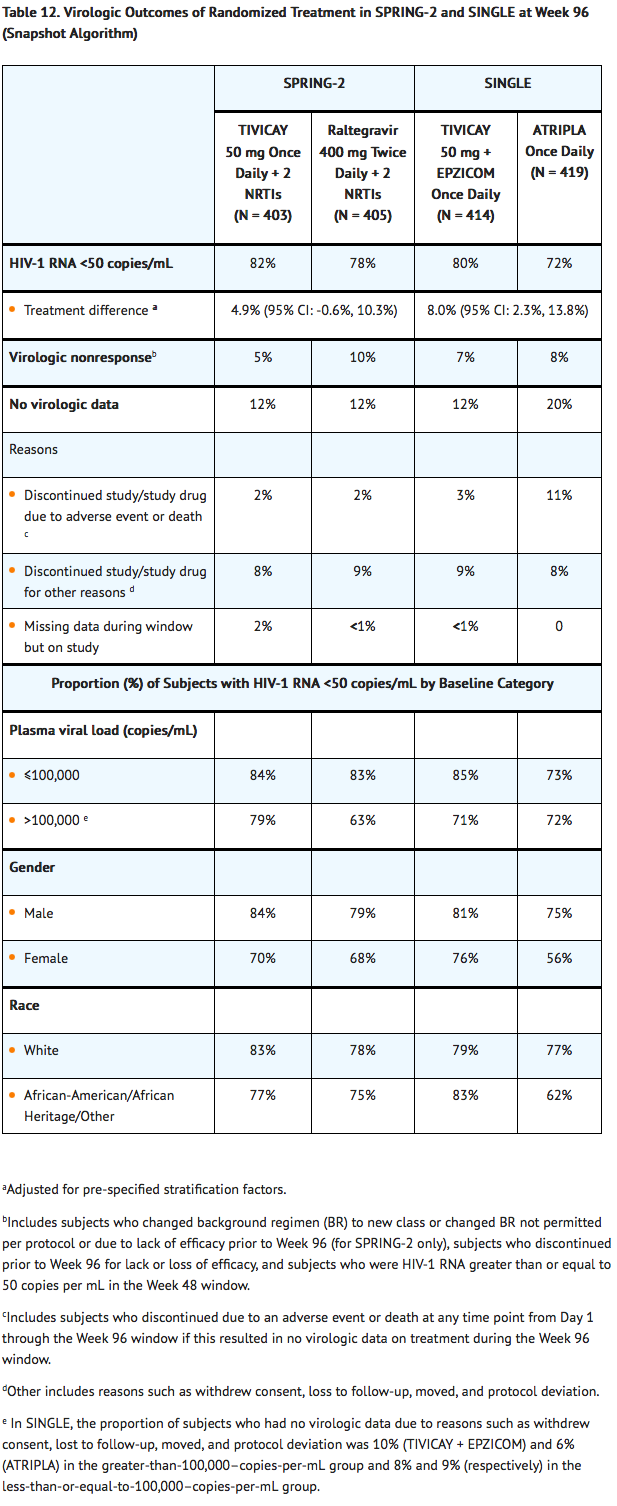
SPRING-2
- Virologic outcomes were also comparable across baseline characteristics including CD4+ cell count, age, and use of EPZICOM or TRUVADA as NRTI background regimen. The median change in CD4+ cell counts from baseline were 276 cells per mm3 in the group receiving Dolutegravir and 264 cells per mm3 for the raltegravir group at 96 weeks.
- There was no treatment-emergent resistance to dolutegravir or to the NRTI background.
SINGLE
- Treatment differences were maintained across baseline characteristics including CD4+ cell count, age, gender, and race.
- The adjusted mean changes in CD4+ cell counts from baseline were 325 cells per mm3 in the group receiving Dolutegravir + EPZICOM and 281 cells per mm3 for the group at 96 weeks. The adjusted difference between treatment arms and 95% CI was 44.0 cells per mm3 (14.3 cells per mm3, 73.6 cells per mm3) (adjusted for pre-specified stratification factors: baseline HIV-1 RNA, baseline CD4+ cell count, and multiplicity).
- There was no treatment-emergent resistance to dolutegravir, abacavir, or lamivudine.
FLAMINGO
- In FLAMINGO, 485 subjects were randomized and received at least 1 dose of either Dolutegravir 50 mg once daily (n = 243) or darunavir + ritonavir 800 mg/100 mg once daily (n = 242), both in combination with investigator-selected NRTI background regimen (either fixed-dose abacavir and lamivudine [EPZICOM] or fixed-dose emtricitabine/tenofovir disoproxil fumarate [TRUVADA]). There were 484 subjects included in the efficacy and safety analyses. At baseline, the median age of subjects was 34 years, 15% female, 28% non-white, 10% had hepatitis B and/or C virus co-infection, 3% were CDC Class C (AIDS), 25% had HIV‑1 RNA greater than 100,000 copies per mL, and 35% had CD4+ cell count less than 350 cells per mm3; these characteristics were similar between treatment groups. Overall response rates by Snapshot algorithm through Week 48 were 90% for Dolutegravir and 83% for darunavir/ritonavir. The adjusted difference in proportion and 95% CI was 7.1% (0.9%, 13.2%). No treatment-emergent primary resistance substitutions were observed in either treatment group.
Treatment-experienced, Integrase Strand Transfer Inhibitor-naïve Subjects
- In the international, multicenter, double-blind trial (SAILING), 719 HIV‑1‑ infected, antiretroviral treatment-experienced adults were randomized and received either Dolutegravir 50 mg once daily or raltegravir 400 mg twice daily with investigator-selected background regimen consisting of up to 2 agents, including at least 1 fully active agent. There were 715 subjects included in the efficacy and safety analyses. At baseline, the median age was 43 years, 32% were female, 50% non-white, 16% had hepatitis B and/or hepatitis C virus co-infection, 46% were CDC Class C (AIDS), 20% had HIV-1 RNA greater than 100,000 copies per mL, and 72% had CD4+ cell count less than 350 cells per mm3; these characteristics were similar between treatment groups. All subjects had at least 2-class antiretroviral treatment resistance, and 49% of subjects had at least 3-class antiretroviral treatment resistance at baseline. Week 48 outcomes for SAILING are shown in Table 13.
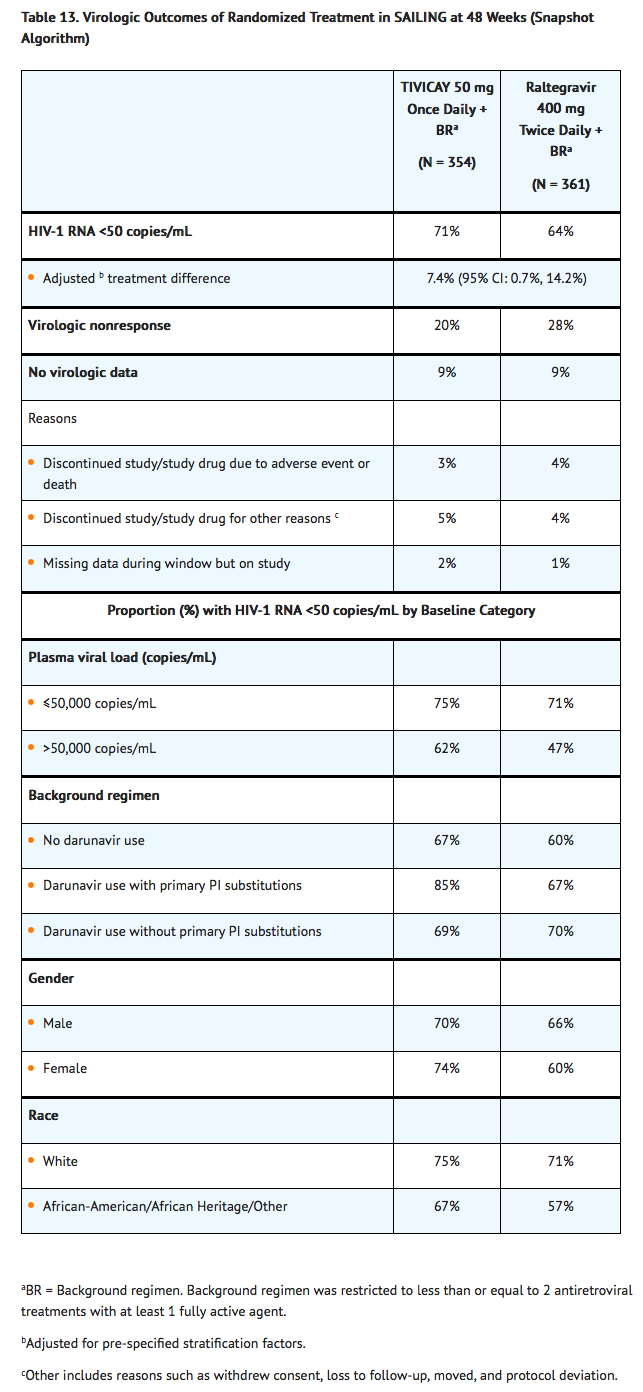
Treatment-experienced, Integrase Strand Transfer Inhibitor-experienced Subjects
- VIKING-3 examined the effect of Dolutegravir 50 mg twice daily over 7 days of functional monotherapy, followed by optimized background therapy (OBT) with continued treatment of Dolutegravir 50 mg twice daily.
- In the multicenter, open-label, single-arm VIKING-3 trial, 183 HIV‑1‑infected, antiretroviral treatment-experienced adults with virological failure and current or historical evidence of raltegravir and/or elvitegravir resistance received Dolutegravir 50 mg twice daily with the current failing background regimen for 7 days, then received Dolutegravir with OBT from Day 8. A total of 183 subjects enrolled: 133 subjects with INSTI resistance at screening and 50 subjects with only historical evidence of resistance (and not at screening). At baseline, median age of subjects was 48 years; 23% were female, 29% non-white, and 20% had hepatitis B and/or hepatitis C virus co-infection. Median baseline CD4+ cell count was 140 cells per mm3, median duration of prior antiretroviral treatment was 13 years, and 56% were CDC Class C. Subjects showed multiple-class antiretroviral treatment resistance at baseline: 79% had greater than or equal to 2 NRTI, 75% greater than or equal to 1 NNRTI, and 71% greater than or equal to 2 PI major substitutions; 62% had non-R5 virus.
- Mean reduction from baseline in HIV-1 RNA at Day 8 (primary endpoint) was 1.4 log10 (95% CI: 1.3 log10, 1.5 log10). Response at Week 48 was affected by baseline INSTI substitutions.
- After the functional monotherapy phase, subjects had the opportunity to re-optimize their background regimen when possible. Week 48 virologic outcomes for VIKING-3 are shown in Table 14.
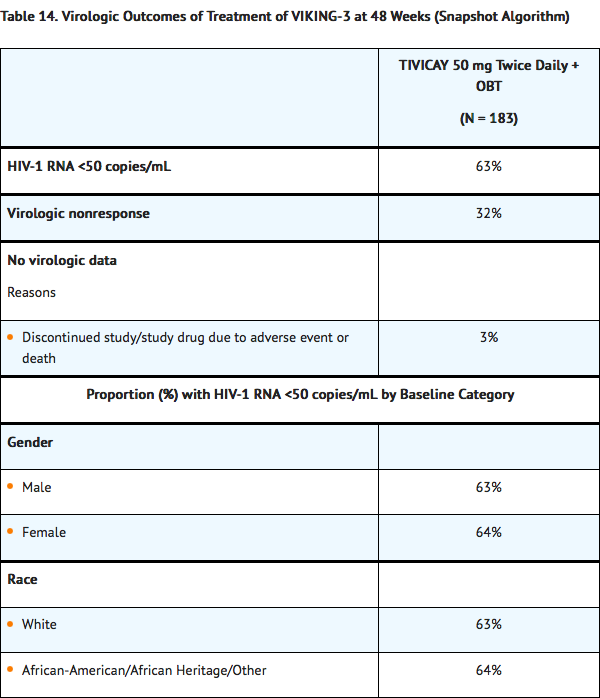
How Supplied
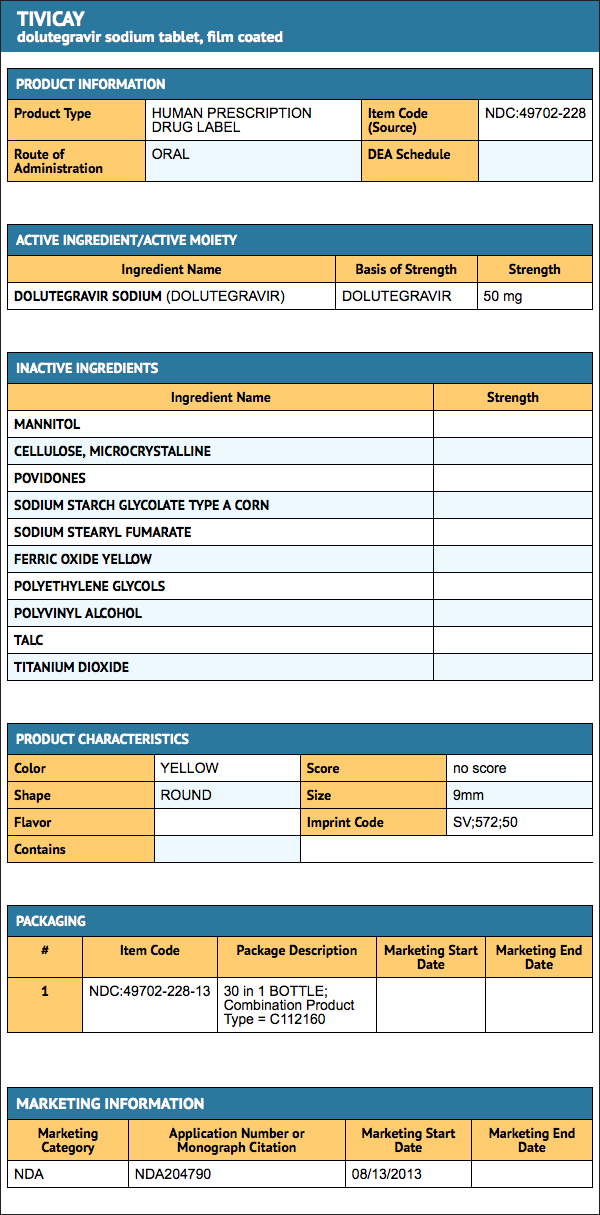
- Dolutegravir Tablets, 50 mg, are yellow, round, film-coated, biconvex tablets debossed with SV 572 on one side and 50 on the other side.
- Bottle of 30 tablets with child-resistant closure NDC 49702-228-13.
Storage
- Store at 25°C (77°F); excursions permitted 15° to 30°C (59° to 86°F)
Images
Drug Images
{{#ask: Page Name::Dolutegravir |?Pill Name |?Drug Name |?Pill Ingred |?Pill Imprint |?Pill Dosage |?Pill Color |?Pill Shape |?Pill Size (mm) |?Pill Scoring |?NDC |?Drug Author |format=template |template=DrugPageImages |mainlabel=- |sort=Pill Name }}
Package and Label Display Panel
{{#ask: Label Page::Dolutegravir |?Label Name |format=template |template=DrugLabelImages |mainlabel=- |sort=Label Page }}
Patient Counseling Information
There is limited information regarding Dolutegravir Patient Counseling Information in the drug label.
Precautions with Alcohol
Alcohol-Dolutegravir interaction has not been established. Talk to your doctor about the effects of taking alcohol with this medication.
Brand Names
Look-Alike Drug Names
There is limited information regarding Dolutegravir Look-Alike Drug Names in the drug label.
Price
References
The contents of this FDA label are provided by the National Library of Medicine.
- ↑ "Dolutegravir® (dolutegravir) Tablets for Oral Use. Full Prescribing Information" (PDF). ViiV Healthcare, 2013. Retrieved 9 February 2014.
{{#subobject:
|Label Page=Dolutegravir |Label Name=Dolutegravir Package2a.png
}}