Tinea corporis
| Tinea corporis | |
 | |
|---|---|
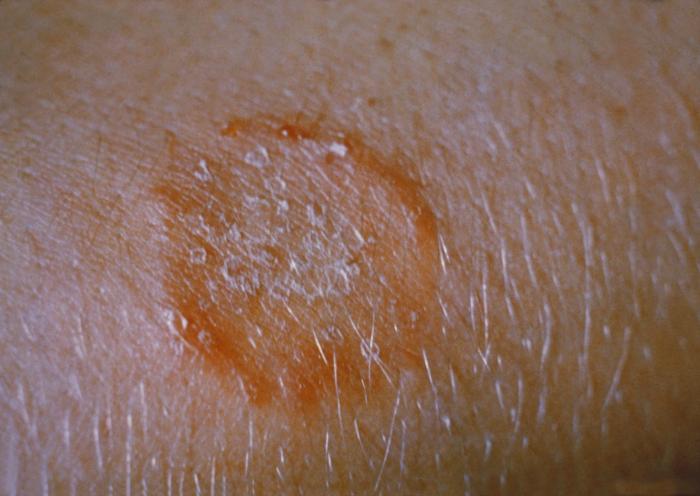
| This patient presented with ringworm on the arm, or tinea corporis due to Trichophyton mentagrophytes. | |
| ICD-10 | B35.4 |
| ICD-9 | 110.5 |
| DiseasesDB | 29138 |
| MedlinePlus | 000877 |
| eMedicine | derm/421 |
|
Dermatophytosis Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Tinea corporis On the Web |
|
American Roentgen Ray Society Images of Tinea corporis |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Kiran Singh, M.D. [2]
Overview
Tinea corporis (also known as ringworm,[1] tinea circinata,[2] and tinea glabrosa[1]) is a superficial fungal infection (dermatophytosis) of the arms and legs, especially on glabrous skin; however, it may occur on any part of the body.
Symptoms
It may have a variety of appearances; most easily identifiable are the enlarging raised red rings with a central area of clearing (ringworm).[3] The same appearances of ringworm may also occur on the scalp (tinea capitis), beard area (tinea barbae) or the groin (tinea cruris, known as jock itch or dhobi itch).
Other classic features of tinea corporis include:
- The edge of the rash appears elevated and is scaly to touch.
- Sometimes the skin surrounding the rash may be dry and flaky.
- Almost invariably, there will be hair loss in areas of the infection.[4]
Causes
Tinea corporis is caused by a tiny fungus known as dermatophyte. These tiny organisms normally live on the superficial skin surface, and when the opportunity is right, they can induce a rash or infection.[5]
The disease can also be acquired by person-to-person transfer usually via direct skin contact with an infected individual.[3] Animal-to-human transmission is also common. Ringworm commonly occurs on pets (dogs, cats) and the fungus can be acquired while petting or grooming an animal. Ringworm can also be acquired from other animals such as horses, pigs, ferrets and cows. The fungus can also be spread by touching inanimate objects like personal care products, bed linen, combs, athletic gear, or hair brushes contaminated by an affected person.[3]
Individuals at high risk of acquiring ringworm include those who:
- Live in crowded, humid conditions.
- Sweat excessively, as sweat can produce a humid wet environment where the pathogenic fungi can thrive. This is most common in the armpits, groin creases and skin folds of the abdomen.
- Participate in close contact sports like soccer, rugby, or wrestling.
- Wear tight, constrictive clothing with poor aeration.
- Have a weakened immune system (e.g., those infected with HIV or taking immunosuppressive drugs).
Diagnosis and testing
Once a fungus is suspected, your physician will examine the skin and take scrapings. These superficial scraps of skin are examined underneath the microscope which quickly reveal the presence of a fungus. If the skin scrapings are negative and a fungus is still suspected, the scrapings are sent for culture. Because the fungus grows slowly, the culture results do take several days to become positive. Other methods of diagnosis include Potassium Hydroxide(KOH) tests.
Physical Examination
Skin
Trunk
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
Extremities
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
Gluteal Region
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
-
Tinea corporis. Adapted from Dermatology Atlas.[6]
Prevention
Because fungi prefer warm, moist environments, preventing ringworm involves keeping skin dry and avoiding contact with infectious material. Basic prevention measures include:
- Washing hands after handling animals, soil, and plants.
- Avoiding touching characteristic lesions on other people.
- Wearing loose-fitting clothing.
- Practicing good hygiene when participation in sports involves physical contact with other people.[5]
Treatment
Most cases are treated by application of topical antifungal creams to the skin, but in extensive or difficult to treat cases systemic treatment with oral medication may be required.
In general, ringworm responds well to topical treatment. Topical antifungals are applied to the lesion twice a day for at least 3 weeks. The lesion usually resolves within 2 weeks, but therapy should be continued for another week to ensure the fungus is completely eradicated. The most commonly used antifungal creams are clotrimazole, ketoconazole, miconazole, terbinafine, tolnaftate, and butenafine.
If there are several ringworm lesions, the lesions are extensive, complications such as secondary infection exist, or the patient is immunocompromised, oral antifungal medications can be used. Oral medications are taken once a day for 7 days and result in higher clinical cure rates. The antifungal medications most commonly used are itraconazole and terbinafine.[5][7]
Antimicrobial Regimen
- Tinea corporis[8]
- Small, well-defined lesions
- Preferred regimen: Topical cream/ointment Terbinafine OR Miconazole OR Econazole OR Clotrimazole
- Larger lesionss
- Preferred regimen: Terbinafine 250 mg/day PO for 2 weeks OR Itraconazole 200 mg/day PO for 1 wk OR Fluconazole 250 mg PO weekly for 2-4 weeks
Prognosis
Tinea corporis is moderately contagious and can affect both humans and pets. If a person acquires it, the proper measures must be taken to prevent it from spreading. Young children in particular should be educated about the infection and preventive measures: avoid skin to skin contact with infected persons and animals, wear clothing that allows the skin to breath, and don't share towels, clothing or combs with others. If pets are kept in the household or premises, they should get the animal checked for tinea,[9] especially if hair loss in patches is noticed or the pet is scratching excessively. The majority of people who have acquired tinea know how uncomfortable the infection can be. However, the fungus can easily be treated and prevented in individuals with a healthy immune system.[4][7]
See also
References
- ↑ 1.0 1.1 Bolognia, Jean; Jorizzo, Joseph L.; Rapini, Ronald P. (2007). Dermatology (2nd ed.). St. Louis, Mo.: Mosby Elsevier. p. 1135. ISBN 978-1-4160-2999-1. OCLC 212399895.
- ↑ James, William D.; Berger, Timothy G.; Elston, Dirk M.; Odom, Richard B. (2006). Andrews' Diseases of the Skin: Clinical Dermatology (10th ed.). Philadelphia: Saunders Elsevier. p. 302. ISBN 978-0-8089-2351-0. OCLC 62736861.
- ↑ 3.0 3.1 3.2 Likness, LP (June 2011). "Common dermatologic infections in athletes and return-to-play guidelines". The Journal of the American Osteopathic Association. 111 (6): 373–379. PMID 21771922.
- ↑ 4.0 4.1 Berman, Kevin (2008-10-03). "Tinea corporis - All Information". Multi Media Medical Encyclopedia. University of Maryland Medical Center. Retrieved 2011-07-19.
- ↑ 5.0 5.1 5.2 Brannon, Heather (2010-03-08). "Ringworm - Tinea Corporis". About.com Dermatology. About.com. Retrieved 2011-07-19.
- ↑ 6.000 6.001 6.002 6.003 6.004 6.005 6.006 6.007 6.008 6.009 6.010 6.011 6.012 6.013 6.014 6.015 6.016 6.017 6.018 6.019 6.020 6.021 6.022 6.023 6.024 6.025 6.026 6.027 6.028 6.029 6.030 6.031 6.032 6.033 6.034 6.035 6.036 6.037 6.038 6.039 6.040 6.041 6.042 6.043 6.044 6.045 6.046 6.047 6.048 6.049 6.050 6.051 6.052 6.053 6.054 6.055 6.056 6.057 6.058 6.059 6.060 6.061 6.062 6.063 6.064 6.065 6.066 6.067 6.068 6.069 6.070 6.071 6.072 6.073 6.074 6.075 6.076 6.077 6.078 6.079 6.080 6.081 6.082 6.083 6.084 6.085 6.086 6.087 6.088 6.089 6.090 6.091 6.092 6.093 6.094 6.095 6.096 6.097 6.098 6.099 6.100 6.101 6.102 6.103 "Dermatology Atlas".
- ↑ 7.0 7.1 Gupta, Aditya K.; Chaudhry, Maria; Elewski, Boni (July 2003). "Tinea corporis, tinea cruris, tinea nigra, and piedra". Dermatologic Clinics. Philadelphia: Elsevier Health Sciences Division. 21 (3): 395&ndash, 400. doi:10.1016/S0733-8635(03)00031-7. ISSN 0733-8635. OCLC 8649114. PMID 12956194.
|access-date=requires|url=(help) - ↑ Bennett, John (2015). Mandell, Douglas, and Bennett's principles and practice of infectious diseases. Philadelphia, PA: Elsevier/Saunders. ISBN 978-1455748013.
- ↑ "Fungus Infections: Tinea". Dermatologic Disease Database. American Osteopathic College of Dermataology. Retrieved 2011-07-19.
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/9/97/Tinea_corporis01.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/8/81/Tinea_corporis03.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/1/12/Tinea_corporis08.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/2/21/Tinea_corporis09.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/5/5b/Tinea_corporis11.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/1/19/Tinea_corporis12.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/8/8b/Tinea_corporis13.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/4/45/Tinea_corporis14.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/6/66/Tinea_corporis16.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/6/66/Tinea_corporis17.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/f/fd/Tinea_corporis18.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/f/ff/Tinea_corporis19.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/6/6d/Tinea_corporis28.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/a/ae/Tinea_corporis33.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/6/65/Tinea_corporis34.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/9/9f/Tinea_corporis35.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/c/cc/Tinea_corporis41.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/0/06/Tinea_corporis42.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/7/7c/Tinea_corporis45.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/e/eb/Tinea_corporis46.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/1/15/Tinea_corporis47.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/d/d9/Tinea_corporis48.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/0/08/Tinea_corporis49.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/0/05/Tinea_corporis50.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/9/99/Tinea_corporis51.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/7/75/Tinea_corporis52.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/3/32/Tinea_corporis53.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/4/4c/Tinea_corporis54.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/6/6a/Tinea_corporis55.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/8/8b/Tinea_corporis56.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/9/9f/Tinea_corporis60.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/a/a5/Tinea_corporis62.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/5/5a/Tinea_corporis81.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/9/96/Tinea_corporis82.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/1/10/Tinea_corporis83.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/1/1f/Tinea_corporis97.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/7/7c/Tinea_corporis98.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/0/00/Tinea_corporis99.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/f/f5/Tinea_corporis100.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/9/9e/Tinea_corporis101.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/e/e1/Tinea_corporis102.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/6/6f/Tinea_corporis103.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/6/6f/Tinea_corporis104.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/f/fd/Tinea_corporis02.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/3/33/Tinea_corporis04.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/f/f5/Tinea_corporis05.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/5/5c/Tinea_corporis06.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/5/54/Tinea_corporis15.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/9/98/Tinea_corporis20.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/2/2d/Tinea_corporis22.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/3/3e/Tinea_corporis23.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/b/be/Tinea_corporis26.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/9/94/Tinea_corporis27.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/b/bd/Tinea_corporis29.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/f/f9/Tinea_corporis30.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/9/91/Tinea_corporis31.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/f/f7/Tinea_corporis32.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/a/a7/Tinea_corporis38.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/0/08/Tinea_corporis39.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/5/5f/Tinea_corporis40.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/5/5e/Tinea_corporis43.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/3/3e/Tinea_corporis44.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/c/c5/Tinea_corporis57.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/c/c8/Tinea_corporis58.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/4/4c/Tinea_corporis59.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/6/68/Tinea_corporis61.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/2/22/Tinea_corporis63.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/d/d1/Tinea_corporis64.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/c/c2/Tinea_corporis65.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/2/21/Tinea_corporis66.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/8/81/Tinea_corporis67.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/8/88/Tinea_corporis68.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/a/ad/Tinea_corporis69.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/0/02/Tinea_corporis70.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/4/4d/Tinea_corporis71.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/8/8a/Tinea_corporis72.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/2/2f/Tinea_corporis73.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/b/b9/Tinea_corporis74.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/7/77/Tinea_corporis75.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/9/9c/Tinea_corporis76.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/0/0d/Tinea_corporis77.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/c/c0/Tinea_corporis78.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/f/f5/Tinea_corporis79.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/8/85/Tinea_corporis80.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/0/0b/Tinea_corporis84.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/4/4a/Tinea_corporis85.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/9/9c/Tinea_corporis86.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/b/b9/Tinea_corporis87.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/8/88/Tinea_corporis88.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/8/82/Tinea_corporis89.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/3/3b/Tinea_corporis90.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/d/d2/Tinea_corporis91.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/9/9c/Tinea_corporis92.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/6/6d/Tinea_corporis93.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/0/00/Tinea_corporis94.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/7/7f/Tinea_corporis95.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/a/a9/Tinea_corporis96.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/2/29/Tinea_corporis07.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/5/5f/Tinea_corporis10.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/9/9d/Tinea_corporis21.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/7/7f/Tinea_corporis24.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/7/7e/Tinea_corporis25.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/1/16/Tinea_corporis36.jpg)
![Tinea corporis. Adapted from Dermatology Atlas.[6]](/images/1/1d/Tinea_corporis37.jpg)