Osteoclast
|
WikiDoc Resources for Osteoclast |
|
Articles |
|---|
|
Most recent articles on Osteoclast |
|
Media |
|
Evidence Based Medicine |
|
Clinical Trials |
|
Ongoing Trials on Osteoclast at Clinical Trials.gov Clinical Trials on Osteoclast at Google
|
|
Guidelines / Policies / Govt |
|
US National Guidelines Clearinghouse on Osteoclast
|
|
Books |
|
News |
|
Commentary |
|
Definitions |
|
Patient Resources / Community |
|
Patient resources on Osteoclast Discussion groups on Osteoclast Patient Handouts on Osteoclast Directions to Hospitals Treating Osteoclast Risk calculators and risk factors for Osteoclast
|
|
Healthcare Provider Resources |
|
Causes & Risk Factors for Osteoclast |
|
Continuing Medical Education (CME) |
|
International |
|
|
|
Business |
|
Experimental / Informatics |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]
Overview
An osteoclast (from the Greek words for "bone" and "broken") is a type of bone cell that removes bone tissue by removing the bone's mineralized matrix. This process is known as bone resorption. Osteoclasts and osteoblasts are instrumental in controlling the amount of bone tissue. Osteoblasts form bone; osteoclasts resorb bone. Osteoclasts are formed by the fusion of cells of the monocyte-macrophage cell line.[1] Osteoclasts are characterized by high expression of tartrate resistant acid phosphatase (TRAP) and cathepsin K.
Morphology


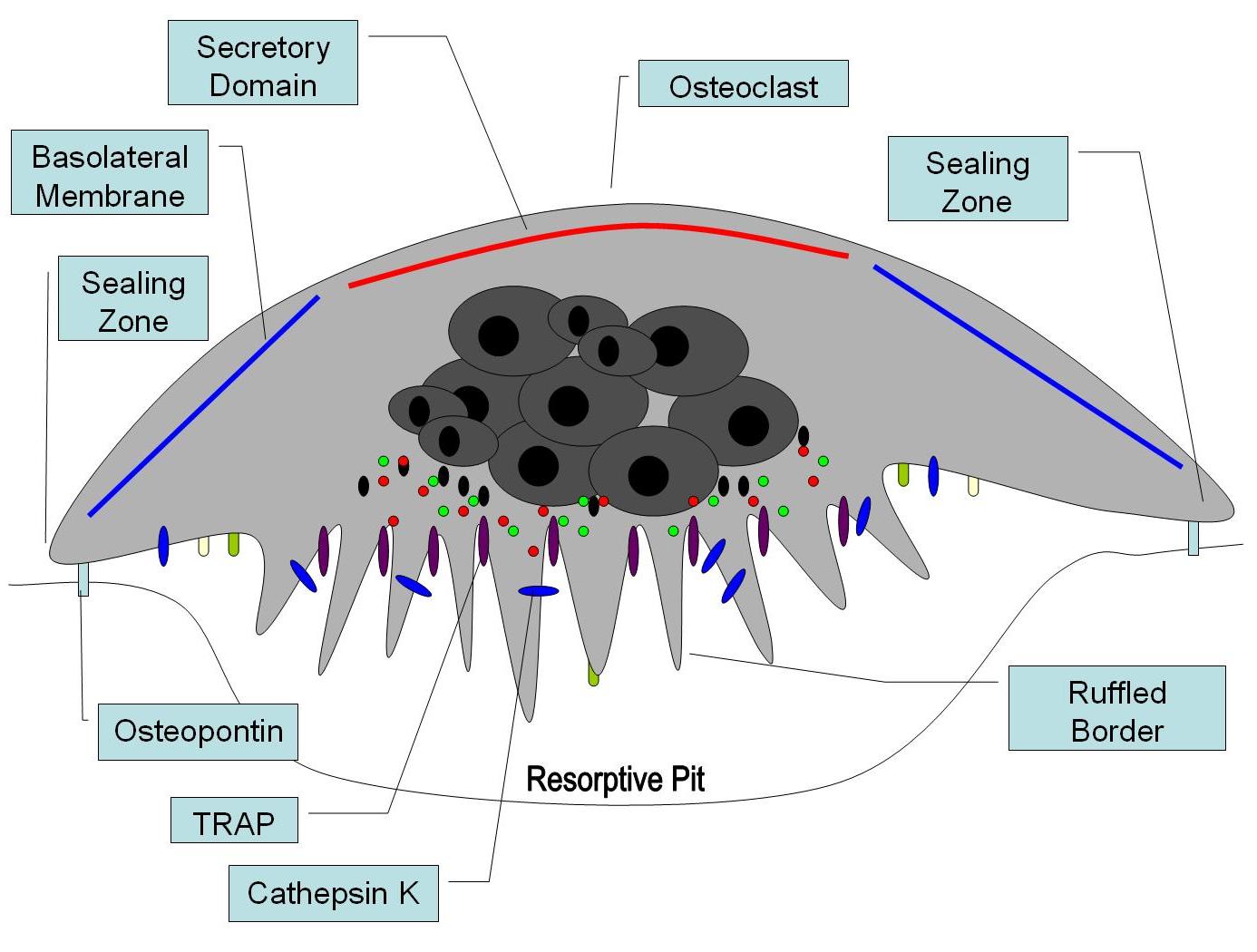
An osteoclast is a large cell that is characterized by multiple nuclei and a cytoplasm with a homogeneous, "foamy" appearance. This appearance is due to a high concentration of vesicles and vacuoles.[2][3] At a site of active bone resorption, the osteoclast forms a specialized cell membrane, the "ruffled border", which touches the surface of the bone tissue.[1] The ruffled border, which facilitates removal of the bony matrix, is a morphologic characteristic of an osteoclast that is actively resorbing bone. The ruffled border increases surface area interface for bone resorption. The mineral portion of the matrix (called hydroxyapatite) includes calcium and phosphate ions. These ions are absorbed into small vesicles (see endocytosis) which move across the cell and eventually are released into the extracellular fluid, thus increasing levels of the ions in the blood.
Formation
Osteoclasts formation requires the presence of RANK ligand (receptor activator of nuclear factor κβ) and M-CSF (Macrophage colony-stimulating factor). These membrane bound proteins are produced by neighbouring stromal cells and osteoblasts; thus requiring direct contact between these cells and osteoclast precursors.
M-CSF acts through its receptor on the osteoclast, c-fms (colony stimulating factor 1 receptor), a transmembrane tyrosine kinase-receptor, leading to secondary messenger activation of tyrosine kinase Src. Both of these molecules are necessary for osteoclastogenesis and are widely involved in the differentiation of monocyte/macrophage derived cells.
RANKL is a member of the tumour necrosis family (TNF), and is essential in osteoclastogenesis. RANKL knockout mice exhibit a phenotype of osteopetrosis and defects of tooth eruption, along with an absence or deficiency of osteoclasts. RANKL activates NF-κβ (nuclear factor-κβ) and NFATc1 (nuclear factor of activated t cells, cytoplasmic, calcineurin-dependent 1) through RANK. NF-κβ activation is stimulated almost immediately after RANKL-RANK interaction occurs, and is not upregulated. NFATc1 stimulation, however, begins ~24-48 hours after binding occurs and its expression has been shown to be RANKL dependent.
Osteoclast differentiation is inhibited by osteoprotegerin (OPG), which binds to RANKL thereby preventing interaction with RANK.
Function
Once activated, they move to areas of microfracture in the bone by chemotaxis. Osteoclasts lie in a small cavity called Howship's lacuna, formed from the digestion of the underlying bone. The sealing zone is the attachment of the osteoclast's plasmalemma to the underlying bone. Sealing zones are bounded by belts of specilized adhesion structures called podosomes. Attachment to the bone matrix is facilitated by integrin receptors, such as αvβ3, via the specific amino acid motif Arg-Gly-Asp in bone matrix proteins, such as osteopontin. The osteoclast releases hydrogen ions (H2O + CO2 → HCO3- + H+) through the ruffled border into the cavity, acidifying and dissolving the mineralized bone matrix into Ca2+, H3PO4, H2CO3 and water. Hydrogen ions are pumped against a high concentration gradient by proton pumps, specifically a unique vacuolar-ATPase. This enzyme has been targeted in the prevention of osteoporosis. In addition, several hydrolytic enzymes, such as members of the cathepsin and matrix metalloprotease(MMP) groups , are released to digest the organic components of the matrix. These enzymes are released into the compartment by lysosomes. Of these hydrolytic enzymes, cathepsin K is of most importance.
Cathepsin K and other cathepsins
Cathepsin K is a collagenolytic, papain-like, cysteine protease that is mainly expressed in osteoclasts, and is secreted into the resorptive pit. Mutations in the cathepsin K gene are associated with pycnodysostosis, a hereditary osteopetrotic disease, characterised by lack of functional cathepsin K expression. Knockout studies of cathepsin K in mice lead to an osteopetrotic phenotype, which, is partially compensated by increased expression of proteases other that cathepsin K and enhanced osteoclastogenesis.
Cathepsin K has an optimal enzymatic activity in acidic conditions. It is synthesized as a proenzyme with a molecular weight of 37kDa, and upon activation by autocatalytic cleavage, is transformed into the mature, active form with a molecular weight of ~27kDa.
In the osteoclast, cathepsin K functions in the resorptive process. Upon polarization of the osteoclast over the site of resorption, cathepsin K is secreted from the ruffled border into the resorptive pit. Here, it is the major protease involved in the degradation of type I collagen and other noncollagenous proteins, which have been demineralized by the acidic environment of the resorptive pit. From the resorptive pit, cathepsin K transmigrates across the ruffled border, through the osteoclast via intercellular vesicles and is then released by the functional secretory domain. Within these intercellular vesicles, cathepsin K, along with ROS generation by TRAP further degrades bone resorption products.
Numerous other cathepsins are expressed in osteoclasts. These include cathepsin B, C, D, E, G, and L. The function of these cysteine and aspartic proteases is generally unknown within bone, and they are expressed at much lower levels that cathepsin K.
Studies on cathepsin L knockout mice have been mixed, with a report of reduced trabecular bone in homozygous and heterozygous cathepsin L knockout mice compared to wild-type and another report finding no skeletal abnormalities.
Matrix metalloproteinases
The matrix metalloproteinases (MMPs) comprise a family of more that 20 zinc-dependent endopeptidases. The role of matrix metalloproteinases (MMPs) in osteoclast biology is ill-defined, but in other tissue they have been linked with tumor promoting activities, such as activation of growth factors and are required for tumor metastasis and angiogenesis.
MMP-9 is associated with the bone microenvironment. It is expressed by osteoclasts, and is known to be required for osteoclast migration and is a powerful gelatinase. Transgenic mice lacking MMP-9 develop defects in bone development, intraosseous angiogenesis, and fracture repair.
MMP-13 is believed to be involved in bone resorption and in osteoclast differentiation, as knockout mice revealed decreased osteoclast numbers, osteopetrosis, and decreased bone resorption.
MMPs expressed by the osteoclast include MMP-9, -10, -12, and -14. apart from MMP-9, little is know about their relevance to the osteoclast, however, high levels of MMP-14 are found at the sealing zone.
Regulation
Osteoclasts are regulated by several hormones, including parathyroid hormone (PTH) from the parathyroid gland, calcitonin from the thyroid gland, and growth factor interleukin 6 (IL-6). This last hormone, IL-6, is one of the factors in the disease osteoporosis, which is an imbalance between bone resorption and bone formation. Osteoclast activity is also mediated by the interaction of two molecules produced by osteoblasts, namely osteoprotegerin and RANK ligand. Note that these molecules also regulate differentiation of the osteoclast.[4]
Alternate use of term
An osteoclast can also be an instrument used to fracture and reset bones (the origin is Greek osteon:bone and klastos:broken). To avoid confusion, the cell was originally termed osotoclast. When the surgical instrument went out of use, the cell became known by its present name.
References
- ↑ 1.0 1.1 Netter, Frank H. (1987), Musculoskeletal system: anatomy, physiology, and metabolic disorders. Summit, New Jersey: Ciba-Geigy Corporation. Page 169.
- ↑ Holtrop, M. E. and G. J. King (1977). "The ultrastructure of the osteoclast and its functional implications". Clin Orthop Relat Res. 123: 177–196. PMID 856515.
- ↑ Väänänen H, Zhao H, Mulari M, Halleen J. "The cell biology of osteoclast function". J Cell Sci. 113 ( Pt 3): 377–81. PMID 10639325. p. 378
- ↑ Schoppet M, Preissner K, Hofbauer L (2002). "RANK ligand and osteoprotegerin: paracrine regulators of bone metabolism and vascular function". Arterioscler Thromb Vasc Biol. 22 (4): 549–53. PMID 11950689.
External link
- MedicineNet
- Osteoclasts at the US National Library of Medicine Medical Subject Headings (MeSH)
Template:Blood Template:Bone and cartilage
ca:Osteoclast
de:Osteoklast
it:Osteoclasto
nl:Osteoclast
sk:Osteoklast
sl:Osteoklast
fi:Osteoklasti
sv:Osteoklast