Congestive heart failure laboratory tests: Difference between revisions
(/* 2017 ACC/AHA/HFSA Focused Update of the 2013 ACCF/AHA Guideline for the Management of Heart Failure/2013 ACCF/AHA Guideline for the Management of Heart Failure/2009 ACC/AHA Focused Update and 2005 Guidelines for the Diagnosis and Management of Chron...) |
|||
| Line 55: | Line 55: | ||
|} | |} | ||
===Biomarkers indications for use=== | |||
<span style="font-size:85%">'''Abbreviations:''' | |||
'''ACC:''' American College of Cardiology, '''AHA:''' American Heart Association, '''ADHF:''' acute decompensated | |||
heart failure, '''BNP:''' B-type natriuretic peptide, '''COR:''' Class of Recommendation, '''ED:''' emergency department, '''HF:''' heart failure, '''NT-proBNP:''' N-terminal pro-B-type natriuretic peptide, '''NYHA:''' New York Heart Association, '''pts:''' patients | |||
</span> | |||
<br> | |||
[[image:BNP.jpg|center|]] | |||
(*)Other biomarkers of injury or fibrosis include soluble ST2 receptor, galectin-3, and high-sensitivity troponin. | |||
===Biomarkers of Myocardial Injury: Cardiac Troponin T or I=== | ===Biomarkers of Myocardial Injury: Cardiac Troponin T or I=== | ||
Even without obvious myocardial ischemic injury, troponin level may be increased in heart failure which means undergoing myocyte injury.<ref name="pmid14999208">{{cite journal |vauthors=Hudson MP, O'Connor CM, Gattis WA, Tasissa G, Hasselblad V, Holleman CM, Gaulden LH, Sedor F, Ohman EM |title=Implications of elevated cardiac troponin T in ambulatory patients with heart failure: a prospective analysis |journal=Am. Heart J. |volume=147 |issue=3 |pages=546–52 |year=2004 |pmid=14999208 |doi=10.1016/j.ahj.2003.10.014 |url=}}</ref> Elevated levels of troponin is associated with impaired hemodynamics, progressive LV dysfunction and increased mortality rates.<ref name="pmid12912820">{{cite journal |vauthors=Horwich TB, Patel J, MacLellan WR, Fonarow GC |title=Cardiac troponin I is associated with impaired hemodynamics, progressive left ventricular dysfunction, and increased mortality rates in advanced heart failure |journal=Circulation |volume=108 |issue=7 |pages=833–8 |year=2003 |pmid=12912820 |doi=10.1161/01.CIR.0000084543.79097.34 |url=}}</ref> | Even without obvious myocardial ischemic injury, troponin level may be increased in heart failure which means undergoing myocyte injury.<ref name="pmid14999208">{{cite journal |vauthors=Hudson MP, O'Connor CM, Gattis WA, Tasissa G, Hasselblad V, Holleman CM, Gaulden LH, Sedor F, Ohman EM |title=Implications of elevated cardiac troponin T in ambulatory patients with heart failure: a prospective analysis |journal=Am. Heart J. |volume=147 |issue=3 |pages=546–52 |year=2004 |pmid=14999208 |doi=10.1016/j.ahj.2003.10.014 |url=}}</ref> Elevated levels of troponin is associated with impaired hemodynamics, progressive LV dysfunction and increased mortality rates.<ref name="pmid12912820">{{cite journal |vauthors=Horwich TB, Patel J, MacLellan WR, Fonarow GC |title=Cardiac troponin I is associated with impaired hemodynamics, progressive left ventricular dysfunction, and increased mortality rates in advanced heart failure |journal=Circulation |volume=108 |issue=7 |pages=833–8 |year=2003 |pmid=12912820 |doi=10.1161/01.CIR.0000084543.79097.34 |url=}}</ref> | ||
Revision as of 16:33, 1 May 2017
| Resident Survival Guide |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-In-Chief: Lakshmi Gopalakrishnan, M.B.B.S. [2]; Seyedmahdi Pahlavani, M.D. [3]; Tarek Nafee, M.D. [4]
Overview
BNP levels may be useful in the initial establishment of the diagnosis of heart failure in the patient with dyspnea of unclear etiology. In a meta-analysis, BNP was superior N-terminal pro-BNP (NTproBNP) and was associated with a sensitivity of 85% and specificity of 84% in the diagnosis of heart failure in the primary care setting.[1] Once the diagnosis of heart failure is made, subsequent laboratory studies should be directed toward the identification of an underlying cause of heart failure.
Laboratory Tests
Renal Function
Renal function should be assessed as a rough guide to the patient's intravascular volume status and renal perfusion. A urinalysis is helpful in the assessment of the patient's volume status. Electrolyte assessment and the correction of electrolyte disturbances such as hypokalemia, hyperkalemia and hypomagnesemia is critical in those patients treated with diuretics. Hyponatremia (due to poor stimulation of the baroreceptors and appropriate ADH release and free water retention) is associated with a poor prognosis.
Hematologic Studies
A complete blood count should be obtained to assess for the presence of anemia which may exacerbate heart failure and to assess the patients coagulation status which may be impaired due to hepatic congestion.
Thyroid Studies
The assessment of thyroid function tests is particularly important in the patient who is being treated with concomitant therapy with an agent such as amiodarone.
Biomarkers
Biomarkers are going to play a great role in diagnosis of heart failure. In addition to routine laboratory tests, they are gaining attention in heart failure management.
Natriuretic Peptides: BNP or NT-proBNP
BNP or its amino-terminal cleavage equivalent (NT-proBNP) is generated by cardiomyocytes in the context of numerous triggers, most notably myocardial stretch. Their measurement is helpful for diagnosis or ruling out heart failure especially in acute setting.[2]
| Cardiac cause | Non cardiac causes | |
|---|---|---|
| Elevated BNP |
|
|
Biomarkers indications for use
Abbreviations:
ACC: American College of Cardiology, AHA: American Heart Association, ADHF: acute decompensated
heart failure, BNP: B-type natriuretic peptide, COR: Class of Recommendation, ED: emergency department, HF: heart failure, NT-proBNP: N-terminal pro-B-type natriuretic peptide, NYHA: New York Heart Association, pts: patients
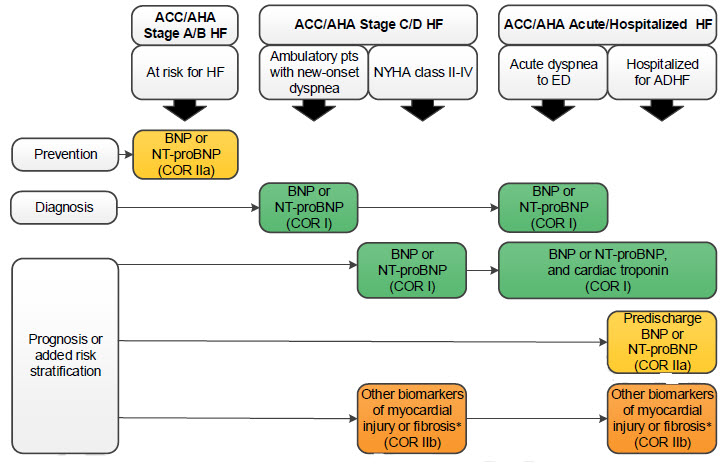
(*)Other biomarkers of injury or fibrosis include soluble ST2 receptor, galectin-3, and high-sensitivity troponin.
Biomarkers of Myocardial Injury: Cardiac Troponin T or I
Even without obvious myocardial ischemic injury, troponin level may be increased in heart failure which means undergoing myocyte injury.[3] Elevated levels of troponin is associated with impaired hemodynamics, progressive LV dysfunction and increased mortality rates.[4]
Carbohydrate Antigen 125
CA-125 is an emerging, highly sensitive biomarker for heart failure.[5] Although it is not yet used in clinical practice, the CHANCE-HF trial has demonstrated utility in using CA-125 to guide diuretic therapy and for determining short-term prognosis.[6] CA-125 is a non-specific antigen that is most strongly associated with ovarian cancer. In patients with acute heart failure, ambulatory follow-up care aimed at titrating diuretic use according to CA-125 levels has demonstrated ~50% reduction in rehospitalizations.[6] CA-125 was first associated with heart failure in 1999 by Nagele et al.[5][7]
2017 ACC/AHA/HFSA Focused Update of the 2013 ACCF/AHA Guideline for the Management of Heart Failure/2013 ACCF/AHA Guideline for the Management of Heart Failure/2009 ACC/AHA Focused Update and 2005 Guidelines for the Diagnosis and Management of Chronic Heart Failure in the Adult (DO NOT EDIT)[8][9]
Initial Clinical Assessment of Patients Presenting With Heart Failure (DO NOT EDIT)[8][9]
| Class I |
| "1. Initial laboratory evaluation of patients presenting with heart failure should include complete blood count, urinalysis, serum electrolytes (including calcium and magnesium), blood urea nitrogen, serum creatinine, fasting blood glucose (glycohemoglobin), lipid profile, liver function tests, and thyroid-stimulating hormone. (Level of Evidence: C) " |
| "2. Serial monitoring, when indicated, should include serum electrolytes and renal function. (Level of Evidence: C) " |
| "3. A 12-lead ECG should be performed initially on all patients presenting with HF. (Level of Evidence: C) " |
| "4. In ambulatory patients with dyspnea, measurement of BNP or N-terminal pro-B-type natriuretic peptide (NT-proBNP) is useful to support clinical decision making regarding the diagnosis of HF, especially in the setting of clinical uncertainty.[10][11] (Level of Evidence: A) " |
| "5. In hospitalized patients/acute setting, measurement of BNP or NT-proBNP is useful to support clinical judgment for the diagnosis of acutely decompensated HF, especially in the setting of uncertainty for the diagnosis.[12][13] (Level of Evidence: A) " |
| "6. In hospitalized patients/acute setting, Measurement of BNP or NT-proBNP and/or cardiac troponin is useful for establishing prognosis or disease severity in acutely decompensated HF.[14][15] (Level of Evidence: A) " |
| "7. Measurement of BNP or NT-proBNP is useful for establishing prognosis or disease severity in chronic HF.[16][17][18](Level of Evidence: A) " |
| Class III (No Benefit) |
| "1. Routine measurement of circulating levels of neurohormones (e.g., norepinephrine or endothelin) is not recommended for patients presenting with heart failure. (Level of Evidence: C) " |
| Class IIa |
| "1. BNP- or NT-proBNP–guided HF therapy can be useful to achieve optimal dosing of GDMT in select clinically euvolemic patients followed in a well-structured HF disease management program. (Level of Evidence: B) " |
| "2. Screening for hemochromatosis or HIV is reasonable in selected patients who present with HF (Level of Evidence: C) " |
| "3. Diagnostic tests for rheumatologic diseases, amyloidosis, or pheochromocytoma are reasonable in patients presenting with heart failure in whom there is a clinical suspicion of these diseases. (Level of Evidence: C) " |
Serial Clinical Assessment of Patients Presenting With Heart Failure (DO NOT EDIT)[8][9]
| Class IIb |
| "1. The usefulness of serial measurement of BNP or NT-proBNP to reduce hospitalization or mortality in patients with HF is not well established. (Level of Evidence: B) " |
| "2. The usefulness of BNP- or NT-proBNP–guided therapy for acutely decompensated HF is not well established. (Level of Evidence: C) " |
| "3. Measurement of other clinically available tests such as biomarkers of myocardial injury or fibrosis may be considered for additive risk stratification in patients with acutely decompensated HF. (Level of Evidence: A) " |
| "4. Measurement of other clinically available tests such as biomarkers of myocardial injury or fibrosis may be considered for additive risk stratification in patients with chronic HF. (Level of Evidence: B) " |
Biomarkers for Prevention (DO NOT EDIT)
| Class IIa |
| "1. For patients at risk of developing HF, natriuretic peptide biomarker–based screening followed by team-based care, including a cardiovascular specialist optimizing GDMT, can be useful to prevent the development of left ventricular dysfunction (systolic or diastolic) or new-onset HF.[19][20] (Level of Evidence: B-R) " |
Biomarkers for Diagnosis (DO NOT EDIT)
| Class I |
| "1. In patients presenting with dyspnea, measurement of natriuretic peptide biomarkers is useful to support a diagnosis or exclusion of HF.[21][16][22] (Level of Evidence: A) " |
Biomarkers for Prognosis or Added Risk Stratification (DO NOT EDIT)
| Class I |
| "1. Measurement of BNP or NT-proBNP is useful for establishing prognosis or disease severity in chronic HF.[16][23] (Level of Evidence: A) " |
| "2. Measurement of baseline levels of natriuretic peptide biomarkers and/or cardiac troponin on admission to the hospital is useful to establish a prognosis in acutely decompensated HF.[14][15][24][25] (Level of Evidence: A) " |
| Class IIa |
| "1. During a HF hospitalization, a predischarge natriuretic peptide level can be useful to establish a postdischarge prognosis.[15][26][27] (Level of Evidence: B-NR) " |
| Class IIb |
| "1. In patients with chronic HF, measurement of other clinically available tests, such as biomarkers of myocardial injury or fibrosis, may be considered for
additive risk stratification.[24][28][25] (Level of Evidence: B-NR) " Vote on and Suggest Revisions to the Current GuidelinesSources
References
|