Sandbox/AIRSG
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Alejandro Lemor, M.D. [2]
| Aortic Regurgitation Resident Survival Guide Microchapters |
|---|
| Overview |
| Causes |
| FIRE |
| Diagnosis |
| Treatment |
| Do's |
| Don'ts |
Overview
Aortic regurgitation (AR) refers to the retrograde or backward flow of blood from the aorta into the left ventricle during diastole.[1][2][3][4] The presentation depends on the response and adaptability of the left ventricle to the increased diastolic volume, in chronic AR the left ventricle has adapted by dilatation of its walls. However, in acute AR, a rapid increase in the diastolic volume is not tolerated by a normal size ventricle and this could lead to cardiogenic shock. The most common causes of acute aortic regurgitation are aortic dissection and infective endocarditis and the preferred treatment in both cases surgical intervention. The most common cause of chronic AR is bicuspid aortic valve and the treatment will depend on the stage of the disease. Acute AR is a life-threatening condition and must be recognized and treated promptly.
Causes
Life Threatening Causes
Life-threatening causes include conditions which may result in death or permanent disability within 24 hours if left untreated.
Common Causes
- Bicuspid aortic valve
- Senile or degenerative calcific aortic valve disease[5]
- Hypertension
- Idiopathic dilatation of the aorta
- Myxomatous degeneration
- Rheumatic fever
Click here for the complete list of causes.
FIRE: Focused Initial Rapid Evaluation
A Focused Initial Rapid Evaluation (FIRE) should be performed to identify patients in need of immediate intervention. The algorithm below is based on the 2014 AHA/ACC Guideline for the Management of Patients With Valvular Heart Disease.[6][7]
Boxes in salmon color signify that an urgent management is needed.
Abbreviations: ECG: electrocardiogram; TTE: transthoracic echocardiography; TEE: transesophageal echocardiography; S1: first heart sound; P2: second heart sound, pulmonary component; S3: third heart sound
Identify cardinal findings that increase the pretest probability of aortic regurgitation Acute aortic regurgitation ❑ Low pitched early diastolic murmur
❑ Decreased or absent S1
❑ S3 ❑ Corrigan's pulse: a rapid upstroke and collapse of the carotid artery pulse | |||||||||||||||||||||||||||||||||||
Does the patient have any of the following findings that require urgent management? ❑ Tachycardia ❑ Hypotension ❑ Altered mental status ❑ Tachypnea ❑ Oliguria ❑ Cold extremities | |||||||||||||||||||||||||||||||||||
YES | NO | ||||||||||||||||||||||||||||||||||
Initiate resuscitation measures: ❑ Secure airway ❑ Administer oxygen ❑ 2 wide bore IV access ❑ ECG monitor ❑ Monitor vitals continuously ❑ ICU admission Initiate medical therapy ❑ Administer nitroprusside 0.3-0.5 υg/kg/min IV (max 10 υg/kg/min), AND ❑ Administer dobutamine 0.5 υg/kg/min IV (max 20 υg/kg/min) ❑ Administer beta blockers in high suspicion of aortic dissection
| Proceed to Complete Diagnostic Approach | ||||||||||||||||||||||||||||||||||
| What is the etiology based on clinical findings and echo? | |||||||||||||||||||||||||||||||||||
Diagnostic clues: ❑ Chest pain of the following characteristics:
❑ Syncope
❑ Aortic root dissection found on TTE | Diagnostic clues: ❑ Persistent fever ❑ New valvular regurgitation murmur ❑ Previous blood culture positive ❑ Vegetations found on TTE ❑ High risk factors:
| ||||||||||||||||||||||||||||||||||
❑ Immediate surgical intervention | ❑ Immediate surgical intervention | ||||||||||||||||||||||||||||||||||
Click here for aortic dissection resident survival guide | Click here for infective endocarditis resident survival guide | ||||||||||||||||||||||||||||||||||
Diagnosis
A complete diagnostic approach should be carried out after a focused initial rapid evaluation is conducted and following initiation of any urgent intervention.[6][7]
Abbreviations: BP: blood pressure; CXR: chest X-ray; ECG: electrocardiogram; LV: left ventricle; MI: myocardial infarction; TTE: transthoracic echocardiography; TEE: transesophageal echocardiography; TAVR: transcatheter aortic valve replacement; S1: first heart sound; S2: second heart sound; S3: third heart sound;
Acute Aortic Regurgitation
Characterize the symptoms: ❑ Sudden and severe dyspnea
❑ Syncope ❑ Weakness ❑ Myalgias | |||||||||||||||||||||||||||||||||||||||||||
Inquire about past medical history: ❑ Cardiac disease: ❑ Rheumatic fever
| |||||||||||||||||||||||||||||||||||||||||||
Examine the patient: Vitals
Cardiovascular examination
❑ Jugular venous distension
❑ Apical diastolic rumble
Respiratory examination | |||||||||||||||||||||||||||||||||||||||||||
Order labs and tests: ❑ TTE (most important test) (Class I; Level of Evidence: B)
❑ ECG
❑ Blood culture (if suspected infective endocarditis) ❑ Cardiac enzymes (Troponin, CK-MB) | |||||||||||||||||||||||||||||||||||||||||||
| Determine the etiology of the acute aortic regurgitation | |||||||||||||||||||||||||||||||||||||||||||
Diagnostic clues: ❑ Chest pain of the following characteristics:
❑ Syncope
❑ Previous history of: | Diagnostic clues: ❑ Persistent fever ❑ New valvular regurgitation murmur ❑ Positive blood culture ❑ Vegetations found on TTE ❑ High risk factors:
| Other causes | |||||||||||||||||||||||||||||||||||||||||
Click here for aortic dissection resident survival guide | Click here for infective endocarditis resident survival guide | ||||||||||||||||||||||||||||||||||||||||||
Chronic Aortic Regurgitation
Characterize the symptoms: ❑ Asymptomatic ❑ Dyspnea on exertion ❑ Orthopnea ❑ Paroxysmal nocturnal dyspnea ❑ Palpitations ❑ Chest pain ❑ Shortness of breath ❑ Cough ❑ Altered mental status ❑ Syncope ❑ Fatigue | |||||||||||||||||||||||||||||||||||||||||||||
Inquire about past medical history: ❑ Cardiac disease: ❑ Rheumatic fever ❑ Pulmonary disease ❑ Trauma ❑ Syphilis ❑ Ankylosing spondylitis ❑ Acromegaly ❑ Marfan syndrome ❑ Ehlers-Danlos syndrome ❑ Giant cell arteritis ❑ Takayasu's arteritis ❑ Previous cardiac surgery | |||||||||||||||||||||||||||||||||||||||||||||
Examine the patient: Vitals
Cardiovascular examination
❑ Search for other characteristic signs suggestive of aortic regurgitation
Respiratory examination | |||||||||||||||||||||||||||||||||||||||||||||
Order imaging studies: ❑ TTE (most important evaluation test) (Class I; Level of Evidence: B)
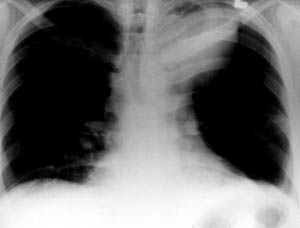
❑ ECG | |||||||||||||||||||||||||||||||||||||||||||||
| Classify aortic regurgitation based on the following findings on TTE: ❑ Vena contracta ❑ Jet/LVOT ❑ Regurgitant volume ❑ Regurgitant fraction ❑ Effective regurgitant orifice | |||||||||||||||||||||||||||||||||||||||||||||
❑ No regurgitation | Mild (Stage B) ❑ Vena contracta <0.3 cm ❑ Jet/LVOT <25% ❑ Regurgitant volume <30 mL/beat ❑ Regurgitant fraction <30% ❑ Effective regurgitant orifice <0.10 cm² | Moderate (Stage B) ❑ Vena contracta 0.3-0.6 cm ❑ Jet/LVOT 25-64% ❑ Regurgitant volume 30-59 mL/beat ❑ Regurgitant fraction 30-49% ❑ Effective regurgitant orifice 0.10-0.29 cm² | Severe ❑ Vena contracta >0.6 cm ❑ Jet/LVOT ≥ 65% ❑ Regurgitant volume ≥60 mL/beat ❑ Regurgitant fraction ≥50% ❑ Effective regurgitant orifice ≥ 0.30 cm² ❑ Holodiastolic flow reversal in the proximal abdominal aorta | ||||||||||||||||||||||||||||||||||||||||||
Asymptomatic | Symptomatic (Stage D) | ||||||||||||||||||||||||||||||||||||||||||||
Treatment
Treatment of Acute Aortic Regurgitation
Shown below is an algorithm for the treatment of acute aortic regurgitation according to the 2014 AHA/ACC Guidelines for the Management of Valvular Heart Disease[6][9] and the 2010 ACCF/AHA Guidelines for the Diagnosis and Management of Patients With Thoracic Aortic Disease[10]
Determine the etiology and the grade of regurgitation | |||||||||||||||||||||||||||||||||||
Mild or moderate regurgitation (Stage B) | Severe regurgitation (Stage C or D) | Mild or moderate regurgitation (Stage B) | Severe regurgitation (Stage C or D) | ||||||||||||||||||||||||||||||||
Does the patient has any of the following? ❑ S.aureus infection ❑ Fungal infection ❑ Large vegetation | Replacement of supra-coronary ascending aorta | Aortic root replacement, OR Valve-sparing aortic root replacement | |||||||||||||||||||||||||||||||||
No | Yes | ||||||||||||||||||||||||||||||||||
❑ Initiate antibiotic treatment
| ❑ Schedule for AVR (Class I; Level of Evidence: B) | ||||||||||||||||||||||||||||||||||
If the patient does not get better after 5-7 days: ❑ Schedule for AVR (Class I; Level of Evidence: B) | |||||||||||||||||||||||||||||||||||
Treatment of Chronic Aortic Regurgitation
Shown below is an algorithm summarizing the treatment approach to chronic aortic regurgitation according to the 2014 AHA/ACC Guidelines on the Management of Valvular Heart Disease.[6][7]
Abbreviations: TTE: transthoracic echocardiography; AVR: aortic valve replacement; CCB: calcium channel blocker; ACE: angiotensin converting enzyme; ARB: angiotensin receptor blocker
What is the stage of aortic regurgitation according to the TTE? | |||||||||||||||||||||||||||||||||||||||||||||
No regurgitation (Stage A) | Progressive regurgitation (Stage B) Mild ❑ Vena contracta <0.3 cm ❑ Jet/LVOT <25% ❑ Regurgitant volume <30 mL/beat ❑ Regurgitant fraction <30% ❑ Effective regurgitant orifice <0.10 cm² Moderate ❑ Vena contracta 0.3-0.6 cm ❑ Jet/LVOT 25-64% ❑ Regurgitant volume 30-59 mL/beat ❑ Regurgitant fraction 30-49% ❑ Effective regurgitant orifice 0.10-0.29 cm² | Severe regurgitation ❑ Vena contracta >0.6 cm ❑ Jet/LVOT ≥ 65% ❑ Regurgitant volume ≥60 mL/beat ❑ Regurgitant fraction ≥50% ❑ Effective regurgitant orifice ≥ 0.30 cm² ❑ Holodiastolic flow reversal in the proximal abdominal aorta | |||||||||||||||||||||||||||||||||||||||||||
| Is the patient symptomatic? | |||||||||||||||||||||||||||||||||||||||||||||
Asymptomatic patients ❑ Control hypertension preferably with
| NO (Stage C) | YES (Stage D) | |||||||||||||||||||||||||||||||||||||||||||
❑ No treatment is needed | ❑ Perform a periodic echo (Class I; Level of Evidence:B)
| ||||||||||||||||||||||||||||||||||||||||||||
❑ Perform a periodic echocardiogram every 6 - 12 months (Class I; Level of Evidence: B) ❑ Perform an exercise stress test | ❑ Schedule for AVR (Class I; Level of Evidence: B) ❑ Initiate medical therapy with ACE inhibitors/ARBs or beta blockers if patient has contraindications for surgery | ||||||||||||||||||||||||||||||||||||||||||||
Does the patient developed symptoms in the stress test? | |||||||||||||||||||||||||||||||||||||||||||||
YES | NO | ||||||||||||||||||||||||||||||||||||||||||||
❑ Initiate medical therapy with vasodilators
| ❑ No treatment is needed | ||||||||||||||||||||||||||||||||||||||||||||
If the patient undergoes another cardiac surgery: ❑ Schedule for AVR (Class IIa; Level of Evidence: C) | |||||||||||||||||||||||||||||||||||||||||||||
Type of Valve and Discharge Anticoagulation Therapy
Abbreviations: AVR: Aortic valve replacement; INR: International normalized ratio; TAVR Tansthoracic aortic valve replacement
Determine: ❑ Age ❑ Contraindications for anticoagulation
| |||||||||||||||||||||||||||||||||
❑ Patients ≤ 60 years old (Class IIa; Level of Evidence: B), AND ❑ No contraindication for anticoagulation | ❑ Patients 60 - 70 years old ❑ No contraindication for anticoagulation | ❑ Patients ≥ 70 years old (Class IIa; Level of Evidence: B), OR ❑ Patients with contraindications for anticoagulation therapy (Class I; Level of Evidence: C) | |||||||||||||||||||||||||||||||
| Mechanical Prosthesis Avoid the use of direct thrombin inhibitors or anti-Xa agents in patients with mechanical prosthesis (Class III; Level of Evidence: B) | Either a bioprosthesic or mechanical valve is reasonable (Class IIa; Level of Evidence: B). | Bioprosthesis | |||||||||||||||||||||||||||||||
Patient with risk factors† | Patient without risk factors† | Surgical AVR | |||||||||||||||||||||||||||||||
Do's
❑ Perform a cardiac MRI in patients with moderate or severe AR with an inconclusive TTE to assess LV systolic function, systolic and diastolic
volumes, and measurement of AR severity. (Class I; Level of Evidence: B)
❑ Exercise stress test could be useful to assess symptomatic status and functional capacity of patents with severe aortic regurgitation
❑
❑
Don'ts
❑ Do not use beta blockers in aortic regurgitation that is not caused by aortic dissection as it will block the compensatory tachycardia.
❑ Do not use intra-aortic baloon counterpulsation in severe acute AI as it will increase the aortic diastolic pressure and the regurgitant volume.
❑ Do not give antibiotics to patients with known VHD before blood cultures are obtained for unexplained fever. (Class III; Level of Evidence: C)
❑ Do not give ACE inhibitors to pregnant patients with aortic regurgitation. (Class III; Level of Evidence: B)
❑
❑
❑
❑
❑
❑
❑
References
- ↑ Connolly HM, Crary JL, McGoon MD; et al. (1997). "Valvular heart disease associated with fenfluramine-phentermine". N. Engl. J. Med. 337 (9): 581–8. doi:10.1056/NEJM199708283370901. PMID 9271479.
- ↑ Weissman NJ (2001). "Appetite suppressants and valvular heart disease". Am. J. Med. Sci. 321 (4): 285–91. doi:10.1097/00000441-200104000-00008. PMID 11307869.
- ↑ Schade R, Andersohn F, Suissa S, Haverkamp W, Garbe E (2007). "Dopamine agonists and the risk of cardiac-valve regurgitation". N. Engl. J. Med. 356 (1): 29–38. doi:10.1056/NEJMoa062222. PMID 17202453.
- ↑ Zanettini R, Antonini A, Gatto G, Gentile R, Tesei S, Pezzoli G (2007). "Valvular heart disease and the use of dopamine agonists for Parkinson's disease". N. Engl. J. Med. 356 (1): 39–46. doi:10.1056/NEJMoa054830. PMID 17202454.
- ↑ Nishimura, RA. (2002). "Cardiology patient pages. Aortic valve disease". Circulation. 106 (7): 770–2. PMID 12176943. Unknown parameter
|month=ignored (help) - ↑ 6.0 6.1 6.2 6.3 Nishimura, R. A.; Otto, C. M.; Bonow, R. O.; Carabello, B. A.; Erwin, J. P.; Guyton, R. A.; O'Gara, P. T.; Ruiz, C. E.; Skubas, N. J.; Sorajja, P.; Sundt, T. M.; Thomas, J. D. (2014). "2014 AHA/ACC Guideline for the Management of Patients With Valvular Heart Disease: A Report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines". Circulation. doi:10.1161/CIR.0000000000000031. ISSN 0009-7322.
- ↑ 7.0 7.1 7.2 Bonow, R. O.; Carabello, B. A.; Chatterjee, K.; de Leon, A. C.; Faxon, D. P.; Freed, M. D.; Gaasch, W. H.; Lytle, B. W.; Nishimura, R. A.; O'Gara, P. T.; O'Rourke, R. A.; Otto, C. M.; Shah, P. M.; Shanewise, J. S. (2008). "2008 Focused Update Incorporated Into the ACC/AHA 2006 Guidelines for the Management of Patients With Valvular Heart Disease: A Report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Writing Committee to Revise the 1998 Guidelines for the Management of Patients With Valvular Heart Disease): Endorsed by the Society of Cardiovascular Anesthesiologists, Society for Cardiovascular Angiography and Interventions, and Society of Thoracic Surgeons". Circulation. 118 (15): e523–e661. doi:10.1161/CIRCULATIONAHA.108.190748. ISSN 0009-7322.
- ↑ Williams BR, Steinberg JP (2006). "Images in clinical medicine. Müller's sign". The New England Journal of Medicine. 355 (3): e3. doi:10.1056/NEJMicm050642. PMID 16855259. Retrieved 2012-04-15. Unknown parameter
|month=ignored (help) - ↑ Hamirani, Y. S.; Dietl, C. A.; Voyles, W.; Peralta, M.; Begay, D.; Raizada, V. (2012). "Acute Aortic Regurgitation". Circulation. 126 (9): 1121–1126. doi:10.1161/CIRCULATIONAHA.112.113993. ISSN 0009-7322.
- ↑ Hiratzka, L. F.; Bakris, G. L.; Beckman, J. A.; Bersin, R. M.; Carr, V. F.; Casey, D. E.; Eagle, K. A.; Hermann, L. K.; Isselbacher, E. M.; Kazerooni, E. A.; Kouchoukos, N. T.; Lytle, B. W.; Milewicz, D. M.; Reich, D. L.; Sen, S.; Shinn, J. A.; Svensson, L. G.; Williams, D. M. (2010). "2010 ACCF/AHA/AATS/ACR/ASA/SCA/SCAI/SIR/STS/SVM Guidelines for the Diagnosis and Management of Patients With Thoracic Aortic Disease: A Report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines, American Association for Thoracic Surgery, American College of Radiology, American Stroke Association, Society of Cardiovascular Anesthesiologists, Society for Cardiovascular Angiography and Interventions, Society of Interventional Radiology, Society of Thoracic Surgeons, and Society for Vascular Medicine". Circulation. 121 (13): e266–e369. doi:10.1161/CIR.0b013e3181d4739e. ISSN 0009-7322.