Psychiatry
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]
Background

Psychiatry is a branch of medicine which exists to study, prevent, and treat mental disorders in humans.[1][2][3] The art and science of the clinical application of psychiatry has been considered a bridge between the social world and those who are mentally ill.[4] Both its research and clinical application are considered interdisciplinary.[5] Because of this, various subspecialties and theoretical approaches exist in psychiatric research and practice. Psychiatrists can be considered physicians who specialize in the doctor-patient relationship[6] who utilize some of medicine's newest classification schemes, diagnostic tools and treatments.[7][8][9]
Ancient psychiatry originated in the 5th century BC with the ideology that psychotic disorders were supernatural in origin.[10] At that time clergy were the individuals in society with the responsibility of "curing" mental disorders.[10] By the middle ages psychiatric hospitals were first created as custodial institutions to house those with mental disorders.[11] During the 18th century the idea arose that mental health institutions could utilize treatments.[12] As a result of these early psychiatric interventions, the 19th century saw a massive increase in patient populations.[13] This dramatic increase led to the decline of treatments offered in such institutions and hurt the reputation of psychiatry.[14] The 20th century saw a rebirth of a biological understanding of mental disorders as well an introduction into disease classification.[15][16] The shift of psychiatry to the hard sciences moved psychiatry into a different direction which resulted in an altered doctor-patient relationship.[17] These changes were seen by many in society as negative and anti-psychiatry movements emerged.[18] The shift in thinking, as well as the introduction of psychiatric medications, led to the dismantling of state psychiatric hospitals.[19] While community treatment was seen as the single solution for those suffering from mental disorders, clinician's soon realized that it was only another treatment option following the drift of disturbed populations into homelessness and prisons.[20] The dramatic changes associated with psychiatric diagnoses and treatments have pushed the field into recognizing the balance between the biological and social sciences and has called for a significant demand of research looking into the origins, classification, and treatment of mental disorders.[21][22]
Theory and focus
"Psychiatry, more than any other branch of medicine, forces its practitioners to wrestle with the nature of evidence, the validity of introspection, problems in communication, and other long-standing philosophical issues" (Psychiatry# note-Guze4|Guze, 1992, p.4).
Psychiatry, a word coined by Johann Christian Reil in 1808, has historically been seen as a specialty of medicine which acted as an intermediary between the world from a social context and the world from the perspective of those who are mentally ill.[4] Those who practice psychiatry are different than most other mental health professionals and physicians in that they must be familiar with both the social and biological sciences.[22] The discipline is interested in the operations of different organs and body systems as classified by the patient's subjective experiences and the objective physiology of the patient.[23] Psychiatry exists to treat mental disorders which are conventionally divided into three very general categories; mental illness, severe learning disability, and personality disorder.[24] While the focus of psychiatry has changed little throughout time, the diagnostic and treatment processes have evolved dramatically and continue to do so. Since the late 20th century, the field of psychiatry has continued to become more biological and less conceptually isolated from the field of medicine.[25]
Scope of practice
While the medical specialty of psychiatry utilizes research in the field of neuroscience, psychology, medicine, biology, biochemistry, and pharmacology,[5] it has generally been considered a middle ground between neurology and psychology.[6] Unlike other physicians and neurologists, psychiatrists specialize in the doctor-patient relationship and are trained in the use of psychotherapy and other therepautic communication techniques.[6] Psychiatrists also differ from psychologists in that they are physicians and the entirety of their post-graduate training is revolved around the field of medicine.[26] Psychiatrists can therefore prescribe medications, order laboratory tests, utilize neuroimaging in a clinical setting, and conduct physical examinations.[27]
Ethics
Like other professions, the World Psychiatric Association issues an ethical code to govern the conduct of psychiatrists. The psychiatric code of ethics, first set forth through the Declaration of Hawaii in 1977, has been expanded through a 1983 Vienna update and, in 1996, the broader Madrid Declaration. The code was further revised in Hamburg, 1999. The World Psychiatric Association code covers such matters as patient assessment, up-to-date knowledge, the human dignity of incapacitated patients, confidentiality, research ethics, sex selection, euthanasia,[28] organ transplantation, torture,[29][30] the death penalty, media relations, genetics, and ethnic or cultural discrimination.[31] In establishing such ethical codes, the profession has responded to a number of controversies about the practice of psychiatry.
Subspecialties
Various subspecialties and/or theoretical approaches exist which are related to the field of psychiatry. They include the following:
- Biological psychiatry; an approach to psychiatry that aims to understand mental disorder in terms of the biological function of the nervous system.
- Child and adolescent psychiatry; a branch of psychiatry that specialises in work with children, teenagers, and their families.
- Cross-cultural psychiatry; a branch of psychiatry concerned with the cultural and ethnic context of mental disorder and psychiatric services.
- Emergency psychiatry; the clinical application of psychiatry in emergency settings.
- Forensic psychiatry; the interface between law and psychiatry.
- Geriatric psychiatry; a branch of psychiatry dealing with the study, prevention, and treatment of mental disorders in humans with old age.
- Liaison psychiatry; the branch of psychiatry that specializes in the interface between other medical specialties and psychiatry.
- Neuropsychiatry; branch of medicine dealing with mental disorders attributable to diseases of the nervous system.
- Social psychiatry; a branch of psychiatry that focuses on the interpersonal and cultural context of mental disorder and mental wellbeing.
History

Ancient psychiatry
Starting in the 5th century BC, mental disorders, especially those disorders with psychotic traits, were considered supernatural in origin.[10] This view existed throughout ancient Greece and ancient Rome|Rome.[10] Early manuals written about mental disorders were created by the Greeks.[32] In 4th century BC, Hippocrates theorized that physiological abnormalities may be the root of mental disorders.[10] However further explorations of this perspective ceased shortly thereafter following the Decline of the Roman Empire|fall of the Roman Empire.[10] Religious leaders and others returned to using early versions of exorcisms to treat mental disorders which often utilized cruel, harsh, and other barbarous methods.[10]
Middle ages through the 18th century
Psychiatric hospitals have existed to treat mental disorders since the Middle Ages but were utilized only as custodial institutions and did not provide any type of treatment.[11] Founded in the 13th century, Bethlem Royal Hospital in London is one of the oldest psychiatric hospitals.[11] By 1547 the City of London acquired the hospital and continued its function until 1948.[33] In 1656, Louis XIV of France created a public system of hospitals for those suffering from mental disorders, but like in England, no real treatment was being applied.[33] In 1758 English physician William Battie wrote the Treatise on Madness which called for treatments to be utilized in asylums.[12] Thirty years later the new ruling monarch in England, George III of the United Kingdom|George III, was known to be suffering from a mental disorder.[10] Following the King's remission in 1789, mental illness was seen as something which could be treated and cured.[10] By 1792 French physician Philippe Pinel introduced Moral treatment|humane treatment approaches to those suffering from mental disorders.[10] William Tuke adopted the methods outlined by Pinel and that same year Tuke opened the The Retreat|York Retreat in England.[10] That institution became known as a model throughout the world for humane and moral treatment of patients suffering from mental disorders.[34]
19th century
In 1800 the number of individuals in asylums in all of England and France was only in the low hundreds.[35] By the late 1890s and early 1900s this number skyrocketed to the hundreds of thousands.[35] The United States housed 150,000 patients in mental hospitals by 1904.[35] German speaking countries housed more than 400 public and private sector asylums.[35] These asylums were critical to the evolution of psychiatry as they provided a universal platform of practice throughout the world.[35] Universities oftentimes played a part in the administration of the asylums.[36] Due to the relationship between the universities and asylums, scores of competitive psychiatrists were being molded in Germany.[36] Germany became known as the world leader in psychiatry during the nineteenth century.[35] The country possessed more than 20 separate universities all competing with each other for scientific advancement.[35] However, because of Germany's individual states and the lack of national regulation of asylums, the country had no organized centralization of asylums or psychiatry.[35] Britain, like Germany, also lacked a centralized organization for the administration of asylums.[37] This deficit hindered the diffusion of new ideas in medicine and psychiatry.[37] By 1838, France created a national law which regulated both the mechanisms for admission into asylums and organized asylum services across the country.[38] By 1840 asylums existing as therapeutic institutions existed throughout Europe and the United States.[13]

However, the new and dominating ideas that mental illness could be "conquered" during the mid-nineteenth century all came crashing down.[13] Psychiatrists and asylums were being pressured by an ever increasing patient population.[13] The average number of patients in asylums in the United States jumped 927%.[13] Numbers were similar in England and Germany.[13] Overcrowding was rampant in France where asylums would commonly take in double their maximum capacity.[39] Increases in asylum populations may have been a result of the transfer of care from families and poorhouses, but the specific reasons as to why the increase occurred is still debated today.[40][41] No matter the cause, the pressure on asylums from the increase was taking its toll on the asylums and psychiatry as a specialty. Asylums were once again turning into custodial institutions[42] and the reputation of psychiatry in the medical world had hit an extreme low.[14]
20th century
Disease classification and rebirth of biological psychiatry
The 20th century introduced a new psychiatry into the world. The different perspectives of looking at mental disorders began to be introduced. The career and beginnings of Emil Kraepelin somewhat model this hiatus of psychiatry between the different disciplines.[15] Kraepelin initially was very attracted to psychology and ignored the ideas of anatomical psychiatry.[15] Following his acceptance for a professorship of psychiatry, and later his work in a university psychiatric clinic, Kraepelin's insterest in pure psychology began to fade and he introduced a plan of a more comprehensive psychiatry.[43][16] Kraepelin also began to study and promote the ideas of disease classification for mental disorders, an idea introduced by Karl Ludwig Kahlbaum.[16] The initial ideas behind biological psychiatry, stating that these different disorders were all biological in nature, evolved into a new idea of "nerves" and psychiatry became a sort of rough neurology or neuropsychiatry.[44] Following Sigmund Freud's death, ideas stemming from psychoanalytic theory also began to take root.[45] The psychoanalytic theory became popular among psychiatrists because it allowed the patients to be treated in private practices instead of asylums.[45] However the progress of psychiatry by the 1970s turned psychoanalytic theory into a marginal school of thought within the field.[45]
This period of time saw the reemergence of biological psychiatry. Psychopharmacology became an integral part of psychiatry starting with Otto Loewi's discovery of the first neurotransmitter, acetylcholine.[46] Neuroimaging was first utilized as a tool for psychiatry in the 1980s.[47] The discovery of chlorpromazine's effectiveness in treating schizophrenia in 1952 revolutionized treatment of the disease, [48] as did lithium carbonate's ability to stabilize mood highs and lows in bipolar disorder in 1948.[49] While psychosocial issues were still seen as valid, psychotherapy was seen to be their "cure."[50] Genetics were once again thought to play a role in mental illness.[46] Molecular biology opened the door for specific genes causing mental disorders to be identified.[46] By 1995 genes causing schizophrenia had been identified on chromosome 6 and those genes responsible for bipolar disorder on chromosomes 18 and 21.[46]
Anti-psychiatry and deinstitutionalization
The introduction of psychiatric medications and the use of laboratory tests altered the doctor-patient relationship between psychiatrists and their patients.[17] Psychiatry's shift to the hard sciences had been interpreted as a lack of concern for patients.[17] Anti-psychiatry had become more prevalent in the late twentieth century due to this and publications in the media which conceptualized mental disorders as myths.[18] Others in the movement argued that psychiatry was a form of social control and demanded that institutionalized psychiatric care, stemming from Pinel's thereapeutic asylum, be abolished.[19] Incidents of physical abuse by psychiatrists took place during the reign of some totalitarian regimes as part of a system to enforce political control with some of the abuse even continuing to our present day.[51] Historical examples of the abuse of psychiatry took place in Nazi Germany [52], in the Soviet Union under Psikhushka, and in the apartheid system in South Africa.[53]

Electroconvulsive therapy was one treatment that the anti-psychiatry movement wanted eliminated.[54] They alleged that electroconvulsive therapy damaged the brain and it was used as a tool for discipline.[54] While there is no evidence that brain damage was a result of electronconvulsive therapy[55][56][57], there have been isolated incidents where the use of electroconvulsive therapy was threatened to keep the patients "in line."[54] The prevalence of psychiatric medication helped initiate deinstitutionalization,[58] the process of discharging patients from psychiatric hospitals to the community.[59] The pressure from the anti-psychiatry movements and the ideology of community treatment from the medical arena helped sustain deinstitutionalization.[58] A mere thirty three years after deinstitutionalization started in the United States, only 19% of the patients in state hospitals remained.[58] Mental health professionals envisioned a process wherein patients would be released into communities where they could participate in a normal life while living in a therapeutic atmosphere.[58]
Transinstitutionalization and the aftermath
In 1963, United States president John F. Kennedy introduced legislation delegating the National Institute of Mental Health to administer Community Mental Health Centers for those being discharged from state psychiatric hospitals.[58] Later, though, the Community Mental Health Center's focus was diverted to provide psychotherapy sessions for those suffering from acute and/or mild mental disorders.[58] Ultimately there were no arrangements made for actively ill patients who were being discharged from hospitals.[58] Instead of being treated by the "community," those suffering from mental disorders drifted into homelessness or ended up in prisons and jails.[58][20] Studies found that 33% of the homeless population and 14% of inmates in prisons and jails were already diagnosed with a mental illness.[58][60]
In 1972, psychologist David Rosenhan published the Rosenhan experiment, a study analyzing the validity of psychiatric diagnoses.[61] The study arranged for eight individuals with no history of psychopathology to attempt admission into psychiatric hospitals. The individuals included a graduate student, psychologists, an artist, a housewife, and two physicians, including one psychiatrist. All eight individuals were admitted with a diagnosis of schizophrenia or bipolar disorder. Psychiatrists then attempted to treat the individuals using psychiatric medication. All eight were discharged within 7 to 52 days. Rosenhan's study concluded that individuals with no presence of mental disorders could not be distinguished from those suffering from mental disorders.[61] While critics such as Robert Spitzer placed doubt on the validity and credibility of the study, they also conceded that the consistency of psychiatric diagnoses needed improvement.[62]
Psychiatry is one of the few medical specialties with a continuing, significant demand for research investigating its related diseases, classifications, origins, and treatments.[21] Psychiatry falls into biology's fundamental belief that disease and health are different elements of an individual's adaptation to an environment.[63] But psychiatry also recognizes that the environment of the human species is complex and includes physical, cultural, and relational elements.[63] In addition to external factors, the human brain must recognize or organize an individual's hopes, fears, desires, fantasies and feelings.[63] Psychiatry's difficult task is the attempt to envelop the understanding of these factors so that they can be studied both clinically and physiologically.[63]
Industry and academia
Practitioners
As with most medical specialties, all physicians can diagnose mental disorders and prescribe treatments utilizing principles of psychiatry. Psychiatrists are physicians who specialize in psychiatry and are certified in treating mental illness using the biomedical approach to mental disorders.[64] Psychiatrists may also go through significant training to conduct psychotherapy, psychoanalysis, and/or cognitive behavioral therapy, but it is their medical training, access to medical laboratories, and ability to prescribe medications that differentiates them from other mental health professionals.[64]
Research
Psychiatric research is, by its very nature, interdisciplinary. From a general perspective it studies and combines social, biological and psychological approaches and how those perspectives cause mental disorders.[65] While practicing psychiatrists and other psychiatric researchers study outcomes from such a wide variety of fields, research institutions and publications exist that are dedicated to the interdisciplinary study of mental disorders within the psychiatric context.[5][66][67][68] Under the supervision of institutional review boards, psychiatric researchers looks at a variety of topics such as neuroimaging, genetics, and psychopharmacology, which in turn help enhance diagnostic consistency, discover new treatment methods, and classify new mental disorders.[69]
Clinical application
Diagnostic systems
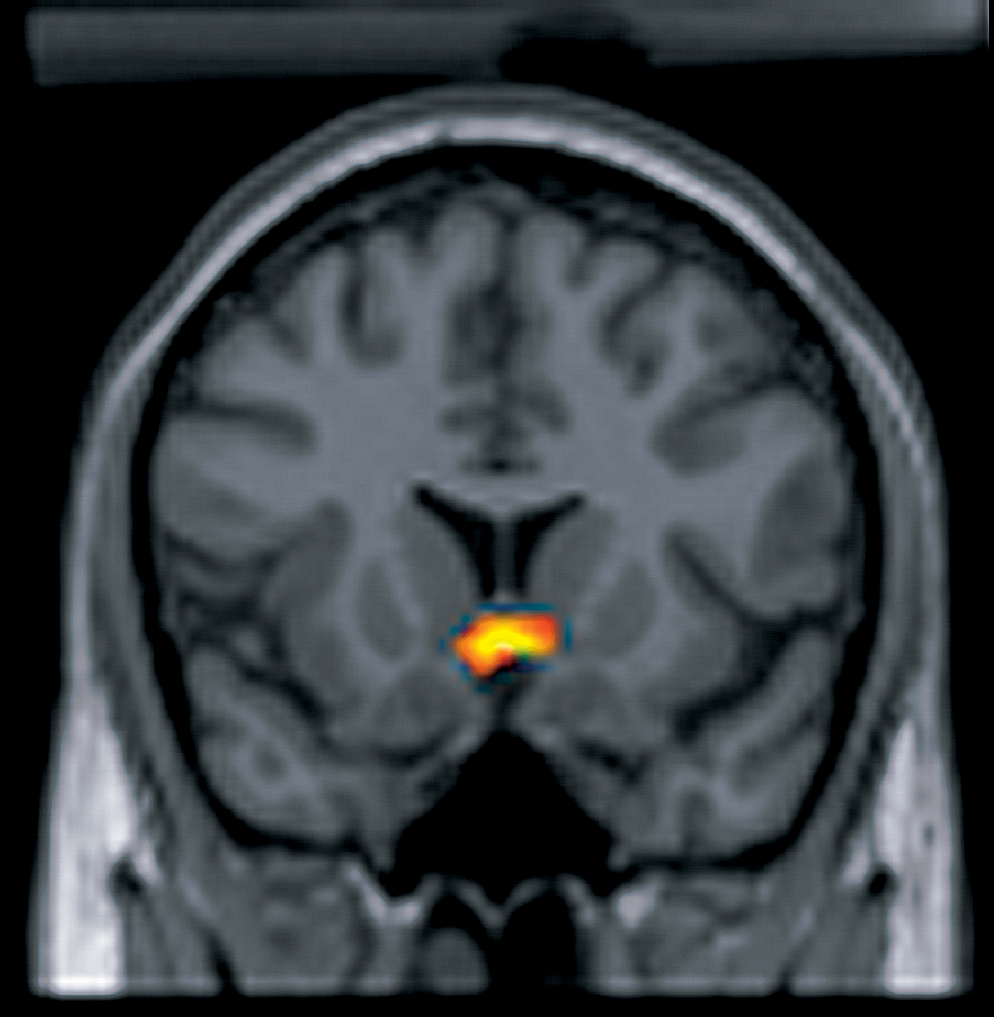
Psychiatric diagnoses take place in a wide variety of settings and are performed by many different health professionals. Therefore, the diagnostic procedure may vary greatly based upon these factors. Typically, though, a psychiatric diagnosis utilizes a differential diagnosis procedure where mental status examinations and physical examinations are conducted, pathological, psychopathological and psychosocial histories obtained, neuroimages or other neurophysiological measurements are taken, and personality tests or cognitive tests may be administered.[70][71][72][73][74][9][75] In addition psychiatrists are beginning to utilize genetics during the diagnostic process.[8] Some endophenotypes being researched may predispose certain individuals to certain conditions.[76][77]
Diangostic manuals
Three main diagnostic manuals used to classify mental health conditions are in use today. The ICD-10 is produced and published by the World Health Organisation and includes a section on psychiatric conditions, and is used worldwide.[78] The Diagnostic and Statistical Manual of Mental Disorders, produced and published by the American Psychiatric Association, is solely focused on mental health conditions and is the main classification tool in the United States.[79] It is currently in its fourth revised edition and is also used worldwide.[79] The Chinese Society of Psychiatry has also produced a diagnostic manual, the Chinese Classification of Mental Disorders.[80]
The stated intention of diagnostic manuals is typically to develop replicable and clinically useful categories and criteria, to facilitate consensus and agreed standards, whilst being atheoretical as regards etiology.[79][7] However, the categories are nevertheless based on particular psychiatric theories and data; they are broad and often specified by numerous possible combinations of symptoms, and many of the categories overlap in symptomology or typically occur together.[81] While originally intended only as a guide for experienced clinicians trained in its use, the nomenclature is now widely used by clinicians, administrators and insurance companies in many countries.[82]
Treatment settings
In general, psychiatric treatments have changed over the past several decades. In the past, psychiatric patients were often hospitalized for six months or more, with some cases involving hospitalization for many years. Today, most people receiving psychiatric treatment are seen as outpatients. If hospitalization is required, the average hospital stay is around two to three weeks, with only a small number of people receiving long-term hospitalization.
Individuals with mental health conditions are commonly referred to as patients but may also be called clients, consumers, or service recipients. They may come under the care of a psychiatric physician or other psychiatric practitioners by various paths, the two most common being self-referral or referral by a primary-care physician. Alternatively, a person may be referred by hospital medical staff, by court order, involuntary commitment, or, in the UK and Australia, by sectioning under a mental health law.
Whatever the circumstance of a person's referral, a psychiatrist first assesses a person's mental and physical condition. This usually involves interviewing the person and often obtaining information from other sources such as other health and social care professionals, relatives, associates, law enforcement and emergency medical personnel and psychiatric rating scales. A physical examination is usually performed to establish or exclude other illnesses, such as thyroid dysfunction or brain tumors, or identify any signs of self-harm; this examination may be done by someone else other than the psychiatrist, especially if blood tests and medical imaging are performed.
Like all medications, psychiatric medications can have toxic effects in patients and hence often involve ongoing therapeutic drug monitoring, for instance full blood counts or, for patients taking lithium salts, serum levels of lithium, renal and thyroid function. Electroconvulsive therapy (ECT) is sometimes administered for serious and disabling conditions, especially those unresponsive to medication.
Psychiatric inpatients are people admitted to a hospital or clinic to receive psychiatric care. Some are admitted involuntarily, perhaps committed to a secure hospital, or in some jurisdictions to a facility within the prison system. In many countries including the USA and Canada, the criteria for involuntary admission vary with local jurisdiction. They may be as broad as having a mental health condition, or as narrow as being an immediate danger to themselves and/or others. Bed availability is often the real determinant of admission decisions to hard pressed public facilities. European Human Rights legislation restricts detention to medically-certified cases of mental disorder, and adds a right to timely judicial review of detention.
Voluntary commitment is also possible, and in some cases people seeking care are offered this option if a mental health professional feels inpatient care is needed, but is unable or unwilling to seek involuntary commitment. People who are voluntarily committed have more options in ending their commitment, but procedures on leaving the facility vary greatly.
Inpatient psychiatric wards may be secure (for those thought to have a particular risk of violence or self-harm) or unlocked/open. Some wards are mixed-sex whilst same-sex wards are increasingly favored to protect women inpatients.
Once in the care of a hospital, people are assessed, monitored, and often given medication and care from a multidisciplinary team, which may include physicians, psychiatric nurse practitioners, psychiatric nurses, clinical psychologists, psychotherapists, psychiatric social workers, occupational therapists and social workers. If a person receiving treatment in a psychiatric hospital is assessed as at particular risk of harming themselves or others, they may be put on constant or intermittent one-to-one supervision, and may be physically restrained or medicated. People on inpatient wards may be allowed leave for periods of time, either accompanied or on their own.
In many developed countries there has been a massive reduction in psychiatric beds since the mid 20th century, with the growth of community care. Standards of inpatient care remain a challenge in some public and private facilities, due to levels of funding, and facilities in developing countries are typically grossly inadequate for the same reason.
People receiving psychiatric care may do so on an inpatient or outpatient basis. Outpatient treatment involves periodic visits to a clinician for consultation in his or her office, usually for an appointment lasting thirty to sixty minutes. These consultations normally involve the psychiatric practitioner interviewing the person to update their assessment of the person's condition, and to provide psychotherapy or review medication. The frequency with which a psychiatric practitioner sees people in treatment varies widely, from days to months, depending on the type, severity and stability of each person's condition, and depending on what the clinician and client decide would be best. Increasingly, psychiatrists are limiting their practice to psychopharmacology (prescribing medications) with less time devoted to psychotherapy or "talk" therapies, or behavior modification. The role of psychiatrists is changing in community psychiatry, with many assuming more leadership roles, coordinating and supervising teams of allied health professionals and junior doctors in delivery of health services.
References
General referencs
- Ford-Martin, Paula Anne Gale (2002), "Psychosis" Gale Encyclopedia of Medicine, Farmington Hills, Michigan
- Hirschfeld et al 2003, "Perceptions and impact of bipolar disorder: how far have we really come?", J. Clin. Psychiatry vol.64(2), p.161-174.
- McGorry PD, Mihalopoulos C, Henry L et al (1995) Spurious precision: procedural validity of diagnostic assessment in psychiatric disorders. American Journal of Psychiatry 152 (2) 220-223
- MedFriendly.com, Psychologist, Viewed 20 September, 2006
- Moncrieff J, Cohen D. (2005). Rethinking models of psychotropic drug action. Psychotherapy & Psychosomatics, 74, 145-153
- National Association of Cognitive-Behavioral Therapists, What is Cognitive-Behavioral Therapy?, Viewed 20 September, 2006
- van Os J, Gilvarry C, Bale R et al (1999) A comparison of the utility of dimensional and categorical representations of psychosis. Psychological Medicine 29 (3) 595-606
- Williams, J.B., Gibbon, M., First, M., Spitzer, R., Davies, M., Borus, J., Howes, M., Kane, J., Pope, H., Rounsaville, B., and Wittchen, H. (1992). The structured clinical interview for DSM-III-R (SCID) II: Multi-site test-retest reliability. Archives of General Psychiatry, 49, 630-636.
Works cited
- ↑ Storrow, H.A. (1969). Outline of Clinical Psychiatry. New York: Appleton-Century-Crofts, p. 1. ISBN 978-0-39-085075-1
- ↑ Lyness, J.M. (1997). Psychiatric Pearls. Philadelphia: F.A. Davis Company, p. 3. ISBN 978-0-80-360280-9
- ↑ Guze, S.B. (1992). Why Psychiatry Is a Branch of Medicine. New York: Oxford University Press, p. 4. ISBN 978-0-19-507420-8
- ↑ 4.0 4.1 Gask, L. (2004). A Short Introduction to Psychiatry. London: SAGE Publications Ltd., p. 7 ISBN 978-0-7619-7138-2
- ↑ 5.0 5.1 5.2 Pietrini, P. (2003). Toward a Biochemistry of Mind? American Journal of Psychiatry, 160, 1907-1908.
- ↑ 6.0 6.1 6.2 Shorter, E. (1997). A History of Psychiatry: From the Era of the Asylum to the Age of Prozac. New York: John Wiley & Sons, Inc, p. 326. ISBN 978-0-47-124531-5
- ↑ 7.0 7.1 Essen-Moller, E. (1971). On classification of mental disorders. Acta Psychiatrica Scandinavica, 37, 119-126.
- ↑ 8.0 8.1 Krebs, M.O. (2005). Future contributions on genetics. World Journal of Biological Psychiatry, 6, 49-55
- ↑ 9.0 9.1 Hampel, H.; Teipel, S.J.; Kotter, H.U.; et al. (1997). Structural magnetic resonance imaging in diagnosis and research of Alzheimer's disease. Nervenarzt, 68, 365-378.
- ↑ 10.00 10.01 10.02 10.03 10.04 10.05 10.06 10.07 10.08 10.09 10.10 Elkes, A. & Thorpe, J.G. (1967). A Summary of Psychiatry. London: Faber & Faber, p. 13.
- ↑ 11.0 11.1 11.2 Shorter, E. (1997). A History of Psychiatry: From the Era of the Asylum to the Age of Prozac. New York: John Wiley & Sons, Inc, p. 4. ISBN 978-0-47-124531-5
- ↑ 12.0 12.1 Shorter, E. (1997). A History of Psychiatry: From the Era of the Asylum to the Age of Prozac. New York: John Wiley & Sons, Inc, p. 9. ISBN 978-0-47-124531-5
- ↑ 13.0 13.1 13.2 13.3 13.4 13.5 Shorter, E. (1997). A History of Psychiatry: From the Era of the Asylum to the Age of Prozac. New York: John Wiley & Sons, Inc, p. 46. ISBN 978-0-47-124531-5
- ↑ 14.0 14.1 Shorter, E. (1997). A History of Psychiatry: From the Era of the Asylum to the Age of Prozac. New York: John Wiley & Sons, Inc, p. 65. ISBN 978-0-47-124531-5
- ↑ 15.0 15.1 15.2 Shorter, E. (1997). A History of Psychiatry: From the Era of the Asylum to the Age of Prozac. New York: John Wiley & Sons, Inc, p. 101. ISBN 978-0-47-124531-5
- ↑ 16.0 16.1 16.2 Shorter, E. (1997). A History of Psychiatry: From the Era of the Asylum to the Age of Prozac. New York: John Wiley & Sons, Inc, p. 103. ISBN 978-0-47-124531-5
- ↑ 17.0 17.1 17.2 Shorter, E. (1997). A History of Psychiatry: From the Era of the Asylum to the Age of Prozac. New York: John Wiley & Sons, Inc, p. 273. ISBN 978-0-47-124531-5
- ↑ 18.0 18.1 Shorter, E. (1997). A History of Psychiatry: From the Era of the Asylum to the Age of Prozac. New York: John Wiley & Sons, Inc, p. 274. ISBN 978-0-47-124531-5
- ↑ 19.0 19.1 Shorter, E. (1997). A History of Psychiatry: From the Era of the Asylum to the Age of Prozac. New York: John Wiley & Sons, Inc, p. 277. ISBN 978-0-47-124531-5
- ↑ 20.0 20.1 Slovenko, R. (2003). The transinstitutionalization of the mentally ill. Ohio University Law Review, 29, 641.
- ↑ 21.0 21.1 Lyness, J.M. (1997). Psychiatric Pearls. Philadelphia: F.A. Davis Company. ISBN 978-0-80-360280-9
- ↑ 22.0 22.1 Storrow, H.A. (1969). Outline of Clinical Psychiatry. New York:Appleton-Century-Crofts, p 1. ISBN 978-0-39-085075-1
- ↑ Guze, S. B. (1992). Why Psychiatry is a Branch of Medicine. New York: Oxford University Press, p 131. ISBN 978-0-19-507420-8.
- ↑ Gask, L. (2004). A Short Introduction to Psychiatry. London: SAGE Publications Ltd., p. 113 ISBN 978-0-7619-7138-2
- ↑ Gask, L. (2004). A Short Introduction to Psychiatry. London: SAGE Publications Ltd., p. 128 ISBN 978-0-7619-7138-2
- ↑ Hauser, M.J. (Unknown last update). Student Information. Retrieved September 21, 2007, from http://www.psychiatry.com/student.php
- ↑ National Institute of Mental Health. (2006, January 31). Information about Mental Illness and the Brain. Retrieved April 19, 2007, from http://science-education.nih.gov/supplements/nih5/Mental/guide/info-mental-c.htm
- ↑ López-Muñoza, Francisco (2006-12-07). "Progress in Neuro-Psychopharmacology and Biological Psychiatry : Psychiatry and political–institutional abuse from the historical perspective: The ethical lessons of the Nuremberg Trial on their 60th anniversary". Cecilio Alamoa, Michael Dudleyb, Gabriel Rubioc, Pilar García-Garcíaa, Juan D. Molinad and Ahmed Okasha. Science Direct. doi:10.1016/j.pnpbp.2006.12.007. Retrieved 2007-10-04.
These practices, in which racial hygiene constituted one of the fundamental principles and euthanasia programmes were the most obvious consequence, violated the majority of known bioethical principles. Psychiatry played a central role in these programmes, and the mentally ill were the principal victims.
- ↑ Gluzman, S.F. (1991). "Abuse of psychiatry: analysis of the guilt of medical personnel". J Med Ethics. 17: 19–20. Retrieved 2007-09-30.
Based on the generally accepted definition, we correctly term the utilisation of psychiatry for the punishment of political dissidents as torture.
- ↑ Debreu, Gerard (1988). "Part 1: Torture, Psychiatric Abuse, and the Ethics of Medicine". In Corillon, Carol. Science and Human Rights. National Academy of Sciences. Retrieved 2007-10-04.
Over the past two decades the systematic use of torture and psychiatric abuse have been sanctioned or condoned by more than one-third of the nations in the United Nations, about half of mankind.
- ↑ The WPA code of ethics.
- ↑ Shorter, E. (1997). A History of Psychiatry: From the Era of the Asylum to the Age of Prozac. New York: John Wiley & Sons, Inc, p. 1. ISBN 978-0-47-124531-5
- ↑ 33.0 33.1 Shorter, E. (1997). A History of Psychiatry: From the Era of the Asylum to the Age of Prozac. New York: John Wiley & Sons, Inc, p. 5. ISBN 978-0-47-124531-5
- ↑ Borthwick, A.; Holman, C.; Kennard, D.; McFetridge, M.; Messruther, K.; Wilkes, J. (2001). The relevance of moral treatment to contemporary mental health care. Journal of Mental Health, 10, 427-439.
- ↑ 35.0 35.1 35.2 35.3 35.4 35.5 35.6 35.7 Shorter, E. (1997). A History of Psychiatry: From the Era of the Asylum to the Age of Prozac. New York: John Wiley & Sons, Inc, p. 34. ISBN 978-0-47-124531-5
- ↑ 36.0 36.1 Shorter, E. (1997). A History of Psychiatry: From the Era of the Asylum to the Age of Prozac. New York: John Wiley & Sons, Inc, p. 35. ISBN 978-0-47-124531-5
- ↑ 37.0 37.1 Shorter, E. (1997). A History of Psychiatry: From the Era of the Asylum to the Age of Prozac. New York: John Wiley & Sons, Inc, p. 41. ISBN 978-0-47-124531-5
- ↑ Shorter, E. (1997). A History of Psychiatry: From the Era of the Asylum to the Age of Prozac. New York: John Wiley & Sons, Inc, p. 40. ISBN 978-0-47-124531-5
- ↑ Shorter, E. (1997). A History of Psychiatry: From the Era of the Asylum to the Age of Prozac. New York: John Wiley & Sons, Inc, p. 47. ISBN 978-0-47-124531-5
- ↑ Shorter, E. (1997). A History of Psychiatry: From the Era of the Asylum to the Age of Prozac. New York: John Wiley & Sons, Inc, p. 48. ISBN 978-0-47-124531-5
- ↑ Shorter, E. (1997). A History of Psychiatry: From the Era of the Asylum to the Age of Prozac. New York: John Wiley & Sons, Inc, p. 49. ISBN 978-0-47-124531-5
- ↑ Rothman, D.J. (1990). The Discovery of the Asylum: Social Order and Disorder in the New Republic. Boston: Little Brown, p. 239. ISBN 978-0-316-75745-4
- ↑ Shorter, E. (1997). A History of Psychiatry: From the Era of the Asylum to the Age of Prozac. New York: John Wiley & Sons, Inc, p. 102. ISBN 978-0-47-124531-5
- ↑ Shorter, E. (1997). A History of Psychiatry: From the Era of the Asylum to the Age of Prozac. New York: John Wiley & Sons, Inc, p. 1114. ISBN 978-0-47-124531-5
- ↑ 45.0 45.1 45.2 Shorter, E. (1997). A History of Psychiatry: From the Era of the Asylum to the Age of Prozac. New York: John Wiley & Sons, Inc, p. 145. ISBN 978-0-47-124531-5
- ↑ 46.0 46.1 46.2 46.3 Shorter, E. (1997). A History of Psychiatry: From the Era of the Asylum to the Age of Prozac. New York: John Wiley & Sons, Inc, p. 246. ISBN 978-0-47-124531-5
- ↑ Shorter, E. (1997). A History of Psychiatry: From the Era of the Asylum to the Age of Prozac. New York: John Wiley & Sons, Inc, p. 270. ISBN 978-0-47-124531-5
- ↑ Turner T. (2007). "Unlocking psychosis". Brit J Med. 334 (suppl): s7.
- ↑ Cade, JFJ; Lithium salts in the treatment of psychotic excitement. Med J Aust 1949, 36, p349-352
- ↑ Shorter, E. (1997). A History of Psychiatry: From the Era of the Asylum to the Age of Prozac. New York: John Wiley & Sons, Inc, p. 239. ISBN 978-0-47-124531-5
- ↑ Sunny Y. Lu & Viviana B. Galli, The Journal of the American Academy of Psychiatry and the Law
- ↑ http://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=12817666&dopt=Abstract
- ↑ http://www.info.gov.za/speeches/1997/06160x76497.htm
- ↑ 54.0 54.1 54.2 Shorter, E. (1997). A History of Psychiatry: From the Era of the Asylum to the Age of Prozac. New York: John Wiley & Sons, Inc, p. 282. ISBN 978-0-47-124531-5
- ↑ Weiner, R.D. (1984). Does ECT cause brain damage? Behavioral and Brain Sciences, 7, 153.
- ↑ Meldrum, B.S. (1986). Neuropathological consequences of chemically and electrically induced seizures. Annals of the New York Academy of Sciences, 462, 18693.
- ↑ Dwork, A.J.; Arango, V.; Underwood, M.; Ilievski, B.; Rosoklija, G.; Sackeim, H.A.; Lisanby, S.H. (2004). Absence of histological lesions in primate models of ECT and magnetic seizure therapy. American Journal of Psychiatry, 161, 576-578.
- ↑ 58.0 58.1 58.2 58.3 58.4 58.5 58.6 58.7 58.8 Shorter, E. (1997). A History of Psychiatry: From the Era of the Asylum to the Age of Prozac. New York: John Wiley & Sons, Inc, p. 280. ISBN 978-0-47-124531-5
- ↑ Shorter, E. (1997). A History of Psychiatry: From the Era of the Asylum to the Age of Prozac. New York: John Wiley & Sons, Inc, p. 279. ISBN 978-0-47-124531-5
- ↑ Torrey, E.F. (1988). Nowhere to Go: The Tragic Odyssey of the Homeless Mentally Ill. New York: Harper and Row, pp.25-29, 126-128. ISBN 978-0-06-015993-1
- ↑ 61.0 61.1 Rosenhan, D. (1973). On being sane in insane places. Science, 179, 250-258.
- ↑ Spitzer, R.L.; Lilienfeld, S.O.; Miller, M.B. (2005). Rosenhan revisited: The scientific credibility of Lauren Slater's pseudopatient diagnosis study. Journal of Nervous and Mental Disease, 193, 734-739.
- ↑ 63.0 63.1 63.2 63.3 Guze, S. B. (1992). Why Psychiatry is a Branch of Medicine. New York: Oxford University Press, p 130. ISBN 978-0-19-507420-8.
- ↑ 64.0 64.1 About:Psychology. (Unknown last update). Difference Between Psychologists and Psychiatrists. Retrieved March 25, 2007, from http://psychology.about.com/od/psychotherapy/f/psychvspsych.htm
- ↑ University of Manchester. (Unknown last update). Research in Psychiatry. Retrieved October 13, 2007, from http://www.manchester.ac.uk/research/areas/subareas/?a=s&id=44694
- ↑ New York State Psychiatric Institute. (2007, March 15). Psychiatric Research Institute New York State. Retrieved October 13, 2007, from http://nyspi.org/
- ↑ Canadian Psychiatric Research Foundation. (2007, July 27). Canadian Psychiatric Research Foundation. Retrieved October 13, 2007, from http://www.cprf.ca/
- ↑ Elsevier. (2007, October 08). Journal of Psychiatric Research. Retrieved October 13, 2007, from http://www.elsevier.com/wps/find/journaldescription.cws_home/241/description
- ↑ Mitchell, J.E.; Crosby, R.D.; Wonderlich, S.A.; Adson, D.E. (2000). Elements of Clinical Research in Psychiatry. Washington D.C.: American Psychiatric Press. ISBN 978-0-88-048802-0.
- ↑ Meyendorf, R. (1980). Diagnosis and differential diagnosis in psychiatry and the question of situation referred prognostic diagnosis. Schweizer Archiv Neurol Neurochir Psychiatry für Neurologie, Neurochirurgie et de psychiatrie, 126, 121-134.
- ↑ Leigh, H. (1983). Psychiatry in the practice of medicine. Menlo Park: Addison-Wesley Publishing Company, p. 15. ISBN 978-0-20-105456-9
- ↑ Leigh, H. (1983). Psychiatry in the practice of medicine. Menlo Park: Addison-Wesley Publishing Company, p. 67. ISBN 978-0-20-105456-9
- ↑ Leigh, H. (1983). Psychiatry in the practice of medicine. Menlo Park: Addison-Wesley Publishing Company, p. 17. ISBN 978-0-20-105456-9
- ↑ Lyness, J.M. (1997). Psychiatric Pearls. Philadelphia: F.A. Davis Company, p. 10. ISBN 978-0-80-360280-9
- ↑ Townsend, B.A.; Petrella, J.R.; Doraiswamy, P.M. (2002). The role of neuroimaging in geriatric psychiatry. Current Opinion in Psychiatry, 15, 427-432.
- ↑ Benes, F.M. (2007). An electrophysiological endophenotype of hypomanic and hyperthymic personality. Journal of Affective Disorders, 101, 13-26.
- ↑ Vonk, R.; van der Schot, A.C.; Kahn, R.S.; et al. (2007). Is autoimmune thyroiditis part of the genetic vulnerability (or an endophenotype) for bipolar disorder? Biological Psychiatry, 62, 135-140.
- ↑ World Health Organisation. (1992). The ICD-10 Classification of Mental and Behavioural Disorders: Clinical Descriptions and Diagnostic Guidelines. Geneva: World Health Organisation. ISBN 978-9-24-154422-1
- ↑ 79.0 79.1 79.2 American Psychiatric Association. (2000). Diagnostic and Statistical Manual of Mental Disorders (4th Edition). Washington D.C.: American Psychiatric Publishing, Inc. ISBN 978-0-89-042025-6
- ↑ Chen, Y.F. (2002) Chinese classification of mental disorders (CCMD-3): towards integration in international classification. Psychopathology, 35, 171-175
- ↑ Mezzich, J.E. (1979). Patterns and issues in multiaxial psychiatric diagnosis. Psychological Medicine, 9, 125-137.
- ↑ Guze, S.B. (1970) The need for toughmindedness in psychiatric thinking. Southern Medical Journal, 63, 662-671.
External links
See also
Related topics
af:Psigiatrie bg:Психиатрия ca:Psiquiatria cs:Psychiatrie da:Psykiatri de:Psychiatrie eo:Psikiatrio eu:Psikiatria ga:Síciatracht gl:Psiquiatría hr:Psihijatrija id:Psikiatri ia:Psychiatria it:Psichiatria he:פסיכיאטריה la:Psychiatria lt:Psichiatrija hu:Pszichiátria nl:Psychiatrie no:Psykiatri nn:Psykiatri simple:Psychiatry sk:Psychiater sl:Psihiatrija sr:Психијатрија sh:Psihijatrija fi:Psykiatria sv:Psykiatri uk:Психіатрія ur:طب نفسی yi:פסיכיאטריע