Azathioprine
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Vignesh Ponnusamy, M.B.B.S. [2]
WikiDoc MAKES NO GUARANTEE OF VALIDITY. WikiDoc is not a professional health care provider, nor is it a suitable replacement for a licensed healthcare provider. WikiDoc is intended to be an educational tool, not a tool for any form of healthcare delivery. The educational content on WikiDoc drug pages is based upon the FDA package insert, National Library of Medicine content and practice guidelines / consensus statements. WikiDoc does not promote the administration of any medication or device that is not consistent with its labeling. Please read our full disclaimer here.
Black Box Warning
|
WARNING - MALIGNANCY
See full prescribing information for complete Boxed Warning.
MALIGNANCY
|
Overview
Azathioprine is a purine antimetabolite that is FDA approved for the treatment of renal homotransplantation, rheumatoid arthritis. There is a Black Box Warning for this drug as shown here. Common adverse reactions include nausea and vomiting.
Adult Indications and Dosage
FDA-Labeled Indications and Dosage (Adult)
Renal Homotransplantation
- Dosing Information
- Azathioprine tablets are indicated as an adjunct for the prevention of rejection in renal homotransplantation. Experience with over 16,000 transplants shows a 5-year patient survival of 35% to 55%, but this is dependent on donor, match for HLA antigens, anti-donor or anti-B-cell alloantigen antibody, and other variables. The effect of azathioprine tablets on these variables has not been tested in controlled trials.
- The dose of azathioprine tablets required to prevent rejection and minimize toxicity will vary with individual patients; this necessitates careful management. The initial dose is usually 3 to 5 mg/kg daily, beginning at the time of transplant. Azathioprine tablets are usually given as a single daily dose on the day of, and in a minority of cases 1 to 3 days before, transplantation. Dose reduction to maintenance levels of 1 to 3 mg/kg daily is usually possible. The dose of azathioprine tablets should not be increased to toxic levels because of threatened rejection. Discontinuation may be necessary for severe hematologic or other toxicity, even if rejection of the homograft may be a consequence of drug withdrawal.
Rheumatoid Arthritis
- Dosing Information
- Azathioprine tablets are indicated for the treatment of active rheumatoid arthritis (RA) to reduce signs and symptoms. Aspirin, non-steroidal anti-inflammatory drugs and/or low dose glucocorticoids may be continued during treatment with azathioprine tablets. The combined use of azathioprine tablets with disease modifying anti-rheumatic drugs (DMARDs) has not been studied for either added benefit or unexpected adverse effects. The use of azathioprine tablets with these agents cannot be recommended.
- Azathioprine tablets are usually given on a daily basis. The initial dose should be approximately 1 mg/kg (50 mg to 100 mg) given as a single dose or on a twice-daily schedule. The dose may be increased, beginning at 6 to 8 weeks and thereafter by steps at 4-week intervals, if there are no serious toxicities and if initial response is unsatisfactory. Dose increments should be 0.5 mg/kg daily, up to a maximum dose of 2.5 mg/kg per day. Therapeutic response occurs after several weeks of treatment, usually 6 to 8; an adequate trial should be a minimum of 12 weeks. Patients not improved after 12 weeks can be considered refractory. Azathioprine tablets may be continued long-term in patients with clinical response, but patients should be monitored carefully, and gradual dosage reduction should be attempted to reduce risk of toxicities.
- Maintenance therapy should be at the lowest effective dose, and the dose given can be lowered decrementally with changes of 0.5 mg/kg or approximately 25 mg daily every 4 weeks while other therapy is kept constant. The optimum duration of maintenance azathioprine tablets has not been determined. Azathioprine tablets can be discontinued abruptly, but delayed effects are possible.
Off-Label Use and Dosage (Adult)
Guideline-Supported Use
There is limited information regarding Off-Label Guideline-Supported Use of Azathioprine in adult patients.
Non–Guideline-Supported Use
Actinic dermatitis
- Dosing Information
- Oral azathioprine 100 to 200 milligrams daily for a mean of 11.5 months.
Atopic dermatitis
- Dosing Information
- Azathioprine (2.5 milligrams per kilogram per day (mg/kg/d) as a single daily dose).
Bullous pemphigoid - Psoriasis
- Dosing Information
- Azathioprine 50 to 150 milligrams (mg) daily.
Giant cell myocarditis
- Dosing Information
- Azathioprine 2 mg/kg/day was then introduced in conjunction with a reduction in prednisone to a dose of 0.33 mg/kg/day.
Idiopathic pulmonary fibrosis
- Dosing Information
- Azathioprine 3 mg/kg/day (not to exceed 200 mg/day.
Inflammatory bowel disease
- Dosing Information
- Azathioprine 1.4 to 2.5 milligrams/kilogram/day.
Lichen planus
- Dosing Information
- oral azathioprine 50 milligrams (mg) twice daily (approximately 2 mg/kilogram/day) for a mean of 5 months.
Liver transplant rejection; Prophylaxis
- Dosing Information
- Azathioprine (1 to 2 mg/kg) were started within 24 hours posttransplant.
Lymphocytic hypopituitarism
- Dosing Information
- Azathioprine (150 milligrams per day).
Myasthenia gravis
- Dosing Information
- Azathioprine (initial dose 50 mg titrated to a maximum dose of 2.5 mg/kg).
Neuromyelitis optica
- Dosing Information
- Oral azathioprine 2 mg/kg/day beginning at week 3.
Radiation pneumonitis
- Dosing Information
- Azathioprine 50 milligrams daily.
Pediatric Indications and Dosage
FDA-Labeled Indications and Dosage (Pediatric)
There is limited information regarding FDA-Labeled Use of Azathioprine in pediatric patients.
Off-Label Use and Dosage (Pediatric)
Guideline-Supported Use
There is limited information regarding Off-Label Guideline-Supported Use of Azathioprine in pediatric patients.
Non–Guideline-Supported Use
There is limited information regarding Off-Label Non–Guideline-Supported Use of Azathioprine in pediatric patients.
Contraindications
- Azathioprine tablets should not be given to patients who have shown hypersensitivity to the drug. Azathioprine tablets should not be used for treating rheumatoid arthritis in pregnant women. Patients with rheumatoid arthritis previously treated with alkylating agents (cyclophosphamide, chlorambucil, melphalan, or others) may have a prohibitive risk of maligancy if treated with azathioprine tablets.
Warnings
|
WARNING - MALIGNANCY
See full prescribing information for complete Boxed Warning.
MALIGNANCY
|
Precautions
- Malignancy
- Patients receiving immunosuppressants, including azathioprine tablets, are at increased risk of developing lymphoma and other malignancies, particularly of the skin. Physicians should inform patients of the risk of malignancy with azathioprine tablets. As usual for patients with increased risk for skin cancer, exposure to sunlight and ultraviolet light should be limited by wearing protective clothing and using a sunscreen with a high protection factor.
- Post-transplant
- Renal transplant patients are known to have an increased risk of malignancy, predominantly skin cancer and reticulum cell or lymphomatous tumors. The risk of post-transplant lymphomas may be increased in patients who receive aggressive treatment with immunosuppressive drugs, including azathioprine tablets. Therefore, immunosuppressive drug therapy should be maintained at the lowest effective levels.
- Rheumatoid Arthritis
- Information is available on the risk of malignancy with the use of azathioprine tablets in rheumatoid arthritis. It has not been possible to define the precise risk of malignancy due to azathioprine tablets. The data suggest the risk may be elevated in patients with rheumatoid arthritis, though lower than for renal transplant patients. However, acute myelogenous leukemia as well as solid tumors have been reported in patients with rheumatoid arthritis who have received azathioprine tablets.
- Inflammatory Bowel Disease
- Postmarketing cases of hepatosplenic T-cell lymphoma (HSTCL), a rare type of T-cell lymphoma, have been reported in patients treated with azathioprine tablets. These cases have had a very aggressive disease course and have been fatal. The majority of reported cases have occurred in patients with Crohn's disease or ulcerative colitis and the majority were in adolescent and young adult males. Some of the patients were treated with azathioprine tablets as monotherapy and some had received concomitant treatment with a TNFα blocker at or prior to diagnosis. The safety and efficacy of azathioprine tablets for the treatment of Crohn's disease and ulcerative colitis have not been established.
- Cytopenias
- Severe leukopenia, thrombocytopenia, anemias including macrocytic anemia, and/or pancytopenia may occur in patients being treated with azathioprine tablets. Severe bone marrow suppression may also occur. Patients with intermediate thiopurine S-methyl transferase (TPMT) activity may be at an increased risk of myelotoxicity if receiving conventional doses of azathioprine tablets. Patients with low or absent TPMT activity are at an increased risk of developing severe, life-threatening myelotoxicity if receiving conventional doses of azathioprine tablets. TPMT genotyping or phenotyping can help identify patients who are at an increased risk for developing azathioprine tablets toxicity.2-9 (See PRECAUTIONS: Laboratory Tests.) Hematologic toxicities are dose-related and may be more severe in renal transplant patients whose homograft is undergoing rejection. It is suggested that patients on azathioprine tablets have complete blood counts, including platelet counts, weekly during the first month, twice monthly for the second and third months of treatment, then monthly or more frequently if dosage alterations or other therapy changes are necessary. Delayed hematologic suppression may occur. Prompt reduction in dosage or temporary withdrawal of the drug may be necessary if there is a rapid fall in or persistently low leukocyte count, or other evidence of bone marrow depression. Leukopenia does not correlate with therapeutic effect; therefore the dose should not be increased intentionally to lower the white blood cell count.
- Serious Infections
- Patients receiving immunosuppressants, including azathioprine tablets, are at increased risk for bacterial, viral, fungal, protozoal, and opportunistic infections, including reactivation of latent infections. These infections may lead to serious, including fatal outcomes.
- Progressive Multifocal Leukoencephalopathy
- Cases of JC virus-associated infection resulting in progressive multifocal leukoencephalopathy (PML), sometimes fatal, have been reported in patients treated with immunosuppressants, including azathioprine tablets. Risk factors for PML include treatment with immunosuppressant therapies and impairment of immune function. Consider the diagnosis of PML in any patient presenting with new-onset neurological manifestations and consider consultation with a neurologist as clinically indicated. Consider reducing the amount of immunosuppression in patients who develop PML. In transplant patients, consider the risk that the reduced immunosuppression represents to the graft.
- Effect on Sperm in Animals
- Azathioprine tablets has been reported to cause temporary depression in spermatogenesis and reduction in sperm viability and sperm count in mice at doses 10 times the human therapeutic dose;10 a reduced percentage of fertile matings occurred when animals received 5 mg/kg.
- Laboratory Tests
- Complete Blood Count (CBC) Monitoring
- Patients on azathioprine tablets should have complete blood counts, including platelet counts, weekly during the first month, twice monthly for the second and third months of treatment, then monthly or more frequently if dosage alterations or other therapy changes are necessary.
- TPMT Testing
- It is recommended that consideration be given to either genotype or phenotype patients for TPMT. Phenotyping and genotyping methods are commercially available. The most common non-functional alleles associated with reduced levels of TPMT activity are TPMT*2, TPMT*3A and TPMT*3C. Patients with two non-functional alleles (homozygous) have low or absent TPMT activity and those with one non-functional allele (heterozygous) have intermediate activity. Accurate phenotyping (red blood cell TPMT activity) results are not possible in patients who have received recent blood transfusions. TPMT testing may also be considered in patients with abnormal CBC results that do not respond to dose reduction. Early drug discontinuation in these patients is advisable.
Adverse Reactions
Clinical Trials Experience
- The principal and potentially serious toxic effects of azathioprine tablets are hematologic and gastrointestinal. The risks of secondary infection and malignancy are also significant (see WARNINGS). The frequency and severity of adverse reactions depend on the dose and duration of azathioprine tablets as well as on the patient’s underlying disease or concomitant therapies. The incidence of hematologic toxicities and neoplasia encountered in groups of renal homograft recipients is significantly higher than that in studies employing azathioprine tablets for rheumatoid arthritis. The relative incidences in clinical studies are summarized below:
- Hematologic
- Leukopenia and/or thrombocytopenia are dose-dependent and may occur late in the course of therapy with azathioprine tablets. Dose reduction or temporary withdrawal may result in reversal of these toxicities. Infection may occur as a secondary manifestation of bone marrow suppression or leukopenia, but the incidence of infection in renal homotransplantation is 30 to 60 times that in rheumatoid arthritis. Anemias, including macrocytic anemia, and/or bleeding have been reported.
- TPMT genotyping or phenotyping can help identify patients with low or absent TPMT activity (homozygous for non-functional alleles) who are at increased risk for severe, life-threatening myelosuppression from azathioprine tablets. Death associated with pancytopenia has been reported in patients with absent TPMT activity receiving azathioprine.
- Gastrointestinal
- Nausea and vomiting may occur within the first few months of therapy with azathioprine tablets and occurred in approximately 12% of 676 rheumatoid arthritis patients. The frequency of gastric disturbance often can be reduced by administration of the drug in divided doses and/or after meals. However, in some patients, nausea and vomiting may be severe and may be accompanied by symptoms such as diarrhea, fever, malaise, and myalgias (see PRECAUTIONS). Vomiting with abdominal pain may occur rarely with a hypersensitivity pancreatitis. Hepatotoxicity manifest by elevation of serum alkaline phosphatase, bilirubin, and/or serum transaminases is known to occur following azathioprine use, primarily in allograft recipients. Hepatotoxicity has been uncommon (less than 1%) in rheumatoid arthritis patients. Hepatotoxicity following transplantation most often occurs within 6 months of transplantation and is generally reversible after interruption of azathioprine tablets. A rare, but life-threatening hepatic veno-occlusive disease associated with chronic administration of azathioprine has been described in transplant patients and in one patient receiving azathioprine tablets for panuveitis. Periodic measurement of serum transaminases, alkaline phosphatase, and bilirubin is indicated for early detection of hepatotoxicity. If hepatic veno-occlusive disease is clinically suspected, azathioprine tablets should be permanently withdrawn.
- Others
- Additional side effects of low frequency have been reported. These include skin rashes, alopecia, fever, arthralgias, diarrhea, steatorrhea, negative nitrogen balance, reversible interstitial pneumonitis, hepatosplenic T-cell lymphoma, and Sweet’s Syndrome (acute febrile neutrophilic dermatosis).
Postmarketing Experience
There is limited information regarding Postmarketing Experience of Azathioprine in the drug label.
Drug Interactions
- Use with Allopurinol
- One of the pathways for inactivation of azathioprine is inhibited by allopurinol. Patients receiving azathioprine tablets and allopurinol concomitantly should have a dose reduction of azathioprine tablets, to approximately 1/3 to 1/4 the usual dose. It is recommended that a further dose reduction or alternative therapies be considered for patients with low or absent TPMT activity receiving azathioprine tablets and allopurinol because both TPMT and XO inactivation pathways are affected.
- Use with Aminosalicylates
- There is in vitro evidence that aminosalicylate derivatives (e.g., sulphasalazine, mesalazine, or olsalazine) inhibit the TPMT enzyme. Concomitant use of these agents with azathioprine tablets should be done with caution.
- Use with Other Agents Affecting Myelopoesis
- Drugs which may affect leukocyte production, including co-trimoxazole, may lead to exaggerated leukopenia, especially in renal transplant recipients.
- Use with Angiotensin-Converting Enzyme Inhibitors
- The use of angiotensin-converting enzyme inhibitors to control hypertension in patients on azathioprine has been reported to induce anemia and severe leukopenia.
- Use with Warfarin
- Azathioprine tablets may inhibit the anticoagulant effect of warfarin.
- Use with Ribavirin
- The use of ribavirin for hepatitis C in patients receiving azathioprine has been reported to induce severe pancytopenia and may increase the risk of azathioprine-related myelotoxicity. Inosine monophosphate dehydrogenase (IMDH) is required for one of the metabolic pathways of azathioprine. Ribavirin is known to inhibit IMDH, thereby leading to accumulation of an azathioprine metabolite, 6-methylthioionosine monophosphate (6-MTITP), which is associated with myelotoxicity (neutropenia, thrombocytopenia, and anemia). Patients receiving azathioprine with ribavirin should have complete blood counts, including platelet counts, monitored weekly for the first month, twice monthly for the second and third months of treatment, then monthly or more frequently if dosage or other therapy changes are necessary.
Use in Specific Populations
Pregnancy
- Pregnancy Category D
- Azathioprine tablets can cause fetal harm when administered to a pregnant woman. Azathioprine tablets should not be given during pregnancy without careful weighing of risk versus benefit. Whenever possible, use of azathioprine tablets in pregnant patients should be avoided. This drug should not be used for treating rheumatoid arthritis in pregnant women.
- Azathioprine tablets are teratogenic in rabbits and mice when given in doses equivalent to the human dose (5 mg/kg daily). Abnormalities included skeletal malformations and visceral anomalies.
- Limited immunologic and other abnormalities have occurred in a few infants born of renal allograft recipients on azathioprine tablets. In a detailed case report, 13 documented lymphopenia, diminished IgG and IgM levels, CMV infection, and a decreased thymic shadow were noted in an infant born to a mother receiving 150 mg azathioprine and 30 mg prednisone daily throughout pregnancy. At 10 weeks most features were normalized. DeWitte et al reported pancytopenia and severe immune deficiency in a preterm infant whose mother received 125 mg azathioprine and 12.5 mg prednisone daily. 14 There have been two published reports of abnormal physical findings. Williamson and Karp described an infant born with preaxial polydactyly whose mother received azathioprine 200 mg daily and prednisone 20 mg every other day during pregnancy. 15 Tallent et al described an infant with a large myelomeningocele in the upper lumbar region, bilateral dislocated hips, and bilateral talipes equinovarus. The father was on long-term azathioprine therapy.
- Benefit versus risk must be weighed carefully before use of azathioprine tablets in patients of reproductive potential. There are no adequate and well-controlled studies in pregnant women. If this drug is used during pregnancy or if the patient becomes pregnant while taking this drug, the patient should be apprised of the potential hazard to the fetus. Women of childbearing age should be advised to avoid becoming pregnant.
- Australian Drug Evaluation Committee (ADEC) Pregnancy Category
There is no Australian Drug Evaluation Committee (ADEC) guidance on usage of Azathioprine in women who are pregnant.
Labor and Delivery
There is no FDA guidance on use of Azathioprine during labor and delivery.
Nursing Mothers
- The use of azathioprine tablets in nursing mothers is not recommended. Azathioprine or its metabolites are transferred at low levels, both transplacentally and in breast milk. Because of the potential for tumorigenicity shown for azathioprine, a decision should be made whether to discontinue nursing or discontinue the drug, taking into account the importance of the drug to the mother.
Pediatric Use
- Safety and efficacy of azathioprine in pediatric patients have not been established.
Geriatic Use
There is no FDA guidance on the use of Azathioprine with respect to geriatric patients.
Gender
There is no FDA guidance on the use of Azathioprine with respect to specific gender populations.
Race
There is no FDA guidance on the use of Azathioprine with respect to specific racial populations.
Renal Impairment
There is no FDA guidance on the use of Azathioprine in patients with renal impairment.
Hepatic Impairment
There is no FDA guidance on the use of Azathioprine in patients with hepatic impairment.
Females of Reproductive Potential and Males
There is no FDA guidance on the use of Azathioprine in women of reproductive potentials and males.
Immunocompromised Patients
There is no FDA guidance one the use of Azathioprine in patients who are immunocompromised.
Administration and Monitoring
Administration
- Oral
Monitoring
There is limited information regarding Monitoring of Azathioprine in the drug label.
IV Compatibility
There is limited information regarding IV Compatibility of Azathioprine in the drug label.
Overdosage
Acute Overdose
Signs and Symptoms
- The oral LD50s for single doses of azathioprine tablets in mice and rats are 2500 mg/kg and 400 mg/kg, respectively. Very large doses of this antimetabolite may lead to marrow hypoplasia, bleeding, infection, and death. A single case has been reported of a renal transplant patient who ingested a single dose of 7500 mg azathioprine tablets. The immediate toxic reactions were nausea, vomiting, and diarrhea, followed by mild leukopenia and mild abnormalities in liver function. The white blood cell count, SGOT, and bilirubin returned to normal 6 days after the overdose.
Management
- About 30% of azathioprine tablets are bound to serum proteins, but approximately 45% is removed during an 8-hour hemodialysis.
Chronic Overdose
There is limited information regarding Chronic Overdose of Azathioprine in the drug label.
Pharmacology
Mechanism of Action
- The use of azathioprine for inhibition of renal homograft rejection is well established, the mechanism(s) for this action are somewhat obscure. The drug suppresses hypersensitivities of the cell-mediated type and causes variable alterations in antibody production. Suppression of T-cell effects, including ablation of T-cell suppression, is dependent on the temporal relationship to antigenic stimulus or engraftment. This agent has little effect on established graft rejections or secondary responses.
- Alterations in specific immune responses or immunologic functions in transplant recipients are difficult to relate specifically to immunosuppression by azathioprine. These patients have subnormal responses to vaccines, low numbers of T-cells, and abnormal phagocytosis by peripheral blood cells, but their mitogenic responses, serum immunoglobulins, and secondary antibody responses are usually normal.
- Azathioprine suppresses disease manifestations as well as underlying pathology in animal models of autoimmune disease. For example, the severity of adjuvant arthritis is reduced by azathioprine.
- The mechanisms whereby azathioprine affects autoimmune diseases are not known. Azathioprine is immunosuppressive, delayed hypersensitivity and cellular cytotoxicity tests being suppressed to a greater degree than are antibody responses. In the rat model of adjuvant arthritis, azathioprine has been shown to inhibit the lymph node hyperplasia, which precedes the onset of the signs of the disease. Both the immunosuppressive and therapeutic effects in animal models are dose-related. Azathioprine is considered a slow-acting drug and effects may persist after the drug has been discontinued.
Structure
- Azathioprine tablets USP, an immunosuppressive antimetabolite, is available in tablet form for oral administration. Each scored tablet contains 50 mg azathioprine, USP and the inactive ingredients corn starch, lactose monohydrate, magnesium stearate, povidone, and stearic acid.
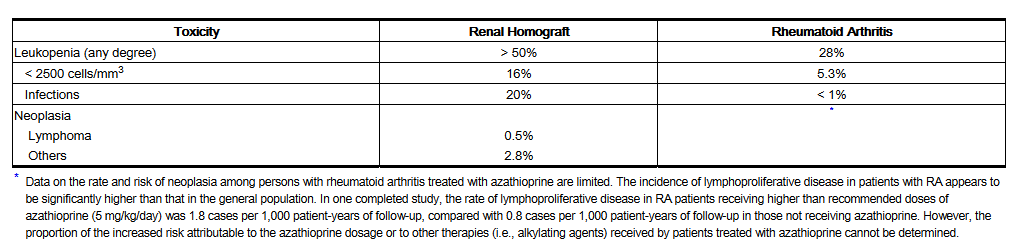
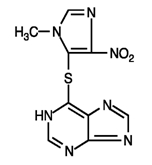
- Azathioprine is chemically 6-[(1-Methyl-4-nitro-1H-imidazol-5-yl)thio]-1H-purine.
- The structural formula of azathioprine is:
- It is an imidazolyl derivative of 6-mercaptopurine and many of its biological effects are similar to those of the parent compound.
- Azathioprine is insoluble in water, but may be dissolved with addition of one molar equivalent of alkali. The sodium salt of azathioprine is sufficiently soluble to make a 10 mg/mL water solution which is stable for 24 hours at 59° to 77°F (15° to 25°C). Azathioprine is stable in solution at neutral or acid pH but hydrolysis to mercaptopurine occurs in excess sodium hydroxide (0.1N), especially on warming. Conversion to mercaptopurine also occurs in the presence of sulfhydryl compounds such as cysteine, glutathione, and hydrogen sulfide.
Pharmacodynamics
There is limited information regarding Pharmacodynamics of Azathioprine in the drug label.
Pharmacokinetics
- Azathioprine is well absorbed following oral administration. Maximum serum radioactivity occurs at 1 to 2 hours after oral 35S-azathioprine and decays with a half-life of 5 hours. This is not an estimate of the half-life of azathioprine itself, but is the decay rate for all 35S-containing metabolites of the drug. Because of extensive metabolism, only a fraction of the radioactivity is present as azathioprine. Usual doses produce blood levels of azathioprine, and of mercaptopurine derived from it, which are low (< 1 mcg/mL). Blood levels are of little predictive value for therapy since the magnitude and duration of clinical effects correlate with thiopurine nucleotide levels in tissues rather than with plasma drug levels. Azathioprine and mercaptopurine are moderately bound to serum proteins (30%) and are partially dialyzable.
- Azathioprine is metabolized to 6-mercaptopurine (6-MP). Both compounds are rapidly eliminated from blood and are oxidized or methylated in erythrocytes and liver; no azathioprine or mercaptopurine is detectable in urine after 8 hours. Activation of 6-mercaptopurine occurs via hypoxanthine-guanine phosphoribosyltransferase (HGPRT) and a series of multi-enzymatic processes involving kinases to form 6-thioguanine nucleotides (6-TGNs) as major metabolites (See Metabolism Scheme in Figure 1). The cytotoxicity of azathioprine is due, in part, to the incorporation of 6-TGN into DNA.
- 6-MP undergoes two major inactivation routes (Figure 1). One is thiol methylation, which is catalyzed by the enzyme thiopurine S-methyltransferase (TPMT), to form the inactive metabolite methyl-6-MP (6-MeMP). TPMT activity is controlled by a genetic polymorphism. For Caucasians and African Americans, approximately 10% of the population inherit one non-functional TPMT allele (heterozygous) conferring intermediate TPMT activity, and 0.3% inherit two TPMT non-functional alleles (homozygous) for low or absent TPMT activity. Non-functional alleles are less common in Asians. TPMT activity correlates inversely with 6-TGN levels in erythrocytes and presumably other hematopoietic tissues, since these cells have negligible xanthine oxidase (involved in the other inactivation pathway) activities, leaving TPMT methylation as the only inactivation pathway. Patients with intermediate TPMT activity may be at increased risk of myelotoxicity if receiving conventional doses of azathioprine tablets. Patients with low or absent TPMT activity are at an increased risk of developing severe, life-threatening myelotoxicity if receiving conventional doses of azathioprine tablets. 4-9 TPMT genotyping or phenotyping (red blood cell TPMT activity) can help identify patients who are at an increased risk for developing azathioprine toxicity. Accurate phenotyping (red blood cell TPMT activity) results are not possible in patients who have received recent blood transfusions.
- GMPS: Guanosine monophosphate synthetase; HGPRT: Hypoxanthine-guanine-phosphoribosyl-transferase; IMPD: Inosine monophosphate dehydrogenase; MeMP: Methylmercaptopurine; MeMPN: Methylmercaptopurine nucleotide; TGN: Thioguanine nucleotides; TIMP: Thioinosine monophosphate; TPMT: Thiopurine S-methyltransferase; TU: Thiouric acid; XO: Xanthine oxidase.
- Another inactivation pathway is oxidation, which is catalyzed by xanthine oxidase (XO) to form 6-thiouric acid. The inhibition of xanthine oxidase in patients receiving allopurinol is the basis for the azathioprine dosage reduction required in these patients (see PRECAUTIONS: Drug Interactions). Proportions of metabolites are different in individual patients, and this presumably accounts for variable magnitude and duration of drug effects. Renal clearance is probably not important in predicting biological effectiveness or toxicities, although dose reduction is practiced in patients with poor renal function.
Nonclinical Toxicology
There is limited information regarding Nonclinical Toxicology of Azathioprine in the drug label.
Clinical Studies
There is limited information regarding Clinical Studies of Azathioprine in the drug label.
How Supplied
- Azathioprine Tablets USP, 50 mg are round, yellow, flat faced tablets debossed with A to the left of the score and Z to the right of the score on one side of the tablet and blank on the other side. They are available as follows:
- NDC 0378-1005-01
- bottles of 100 tablets
- Store at 20° to 25°C (68° to 77°F). [See USP Controlled Room Temperature.] in a dry place and protect from light.
- Dispense in a tight, light-resistant container as defined in the USP using a child-resistant closure.
Storage
There is limited information regarding Azathioprine Storage in the drug label.
Images
Drug Images
{{#ask: Page Name::Azathioprine |?Pill Name |?Drug Name |?Pill Ingred |?Pill Imprint |?Pill Dosage |?Pill Color |?Pill Shape |?Pill Size (mm) |?Pill Scoring |?NDC |?Drug Author |format=template |template=DrugPageImages |mainlabel=- |sort=Pill Name }}
Package and Label Display Panel
{{#ask: Label Page::Azathioprine |?Label Name |format=template |template=DrugLabelImages |mainlabel=- |sort=Label Page }}
Patient Counseling Information
- Patients being started on azathioprine tablets should be informed of the necessity of periodic blood counts while they are receiving the drug and should be encouraged to report any unusual bleeding or bruising to their physician. They should be informed of the danger of infection while receiving azathioprine tablets and asked to report signs and symptoms of infection to their physician. Careful dosage instructions should be given to the patient, especially when azathioprine tablets are being administered in the presence of impaired renal function or concomitantly with allopurinol (see DOSAGE AND ADMINISTRATION and PRECAUTIONS: Drug Interactions). Patients should be advised of the potential risks of the use of azathioprine tablets during pregnancy and during the nursing period. The increased risk of malignancy following therapy with azathioprine tablets should be explained to the patient.
Precautions with Alcohol
- Alcohol-Azathioprine interaction has not been established. Talk to your doctor about the effects of taking alcohol with this medication.
Brand Names
- Azathioprine®[1]
Look-Alike Drug Names
- azaTHIOprine® — azaCITIDine®[2]
Price
References
The contents of this FDA label are provided by the National Library of Medicine.
- ↑ "AZATHIOPRINE tablet [Mylan Pharmaceuticals Inc.]".
- ↑ "http://www.ismp.org". External link in
|title=(help)
{{#subobject:
|Page Name=Azathioprine |Pill Name=Azathioprine_NDC_00544084.jpg |Drug Name=Azathioprine |Pill Ingred=AZATHIOPRINE[AZATHIOPRINE]|+sep=; |Pill Imprint=54;043 |Pill Dosage=50 mg |Pill Color=Yellow|+sep=; |Pill Shape=Round |Pill Size (mm)=1 |Pill Scoring=2 |Pill Image= |Drug Author=Roxane Laboratories, Inc |NDC=00544084
}}
{{#subobject:
|Page Name=Azathioprine |Pill Name=Azathioprine_NDC_00548084.jpg |Drug Name=Azathioprine |Pill Ingred=AZATHIOPRINE[AZATHIOPRINE]|+sep=; |Pill Imprint=54;043 |Pill Dosage=50 mg |Pill Color=Yellow|+sep=; |Pill Shape=Round |Pill Size (mm)=1 |Pill Scoring=2 |Pill Image= |Drug Author=Roxane Laboratories, Inc |NDC=00548084
}}
{{#subobject:
|Page Name=Azathioprine |Pill Name=Azathioprine_NDC_433530686.jpg |Drug Name=Azathioprine |Pill Ingred=AZATHIOPRINE[AZATHIOPRINE]|+sep=; |Pill Imprint=54;043 |Pill Dosage=50 mg |Pill Color=Yellow|+sep=; |Pill Shape=Round |Pill Size (mm)=1 |Pill Scoring=2 |Pill Image= |Drug Author=Aphena Pharma Solutions - Tennessee, Inc. |NDC=433530686
}}
{{#subobject:
|Page Name=Azathioprine |Pill Name=IMURAN_NDC_654830590.jpg |Drug Name=IMURAN |Pill Ingred=azathioprine[azathioprine]|+sep=; |Pill Imprint=IMURAN;50 |Pill Dosage=50 mg |Pill Color=Yellow|+sep=; |Pill Shape=DoubleCircle |Pill Size (mm)=11 |Pill Scoring=2 |Pill Image= |Drug Author=Prometheus Laboratories Inc. |NDC=654830590
}}
{{#subobject:
|Page Name=Azathioprine |Pill Name=Azathioprine_NDC_683820003.jpg |Drug Name=Azathioprine |Pill Ingred=AZATHIOPRINE[AZATHIOPRINE]|+sep=; |Pill Imprint=ZC;59 |Pill Dosage=50 mg |Pill Color=Yellow|+sep=; |Pill Shape=Round |Pill Size (mm)=8 |Pill Scoring=2 |Pill Image= |Drug Author=Zydus Pharmaceuticals (USA) Inc. |NDC=683820003
}}
{{#subobject:
|Page Name=Azathioprine |Pill Name=Azathioprine_NDC_03781005.jpg |Drug Name=Azathioprine |Pill Ingred=AZATHIOPRINE[AZATHIOPRINE]|+sep=; |Pill Imprint=A;Z |Pill Dosage=50 mg |Pill Color=Yellow|+sep=; |Pill Shape=Round |Pill Size (mm)=8 |Pill Scoring=2 |Pill Image= |Drug Author=Mylan Pharmaceuticals Inc. |NDC=03781005
}}
{{#subobject:
|Label Page=Azathioprine |Label Name=Azathioprine02.png
}}
{{#subobject:
|Label Page=Azathioprine |Label Name=Azathioprine03.png
}}