Hyperlipoproteinemia type 5: Difference between revisions
| Line 250: | Line 250: | ||
inducibility | inducibility | ||
|Fat tolerance | |Fat tolerance | ||
|Electrophoresis | |||
|Cholesterol/TG ratio | |||
|LDL/HDL ratio | |||
|- | |- | ||
|Hyperlipoproteinemia type 5 | |Hyperlipoproteinemia type 5 | ||
| Line 261: | Line 264: | ||
|May be abnormal | |May be abnormal | ||
|Markedly abnormal | |Markedly abnormal | ||
|Pre-beta band ↑↑,beta and alpha ↓ | |||
|>0.15 and <0.6 | |||
|↓ | |||
|} | |} | ||
#LIPID ANALYSIS | #LIPID ANALYSIS | ||
Revision as of 15:33, 30 November 2016
|
Hyperlipoproteinemia Microchapters |
|
ACC/AHA Guideline Recommendations |
|
Intensity of statin therapy in primary and secondary prevention |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1] ;Associate Editor(s)-in-Chief: Shivani Chaparala M.B.B.S [2] Venkata Sivakrishna Kumar Pulivarthi M.B.B.S [3]
Synonyms and keywords: : Hyperchylomicronemia, Late-Onset Hyperchylomicronemia With Hyperprebetalipoproteinemia, Familial mixed hyperlipidemia, Type V hyperlipemia, Hyperlipidemia type V, Type 5 hyperlipoproteinemia, Type 5 hyperlipemia, Type 5 HLP, Type V HLP, Combined fat and carbohydrate Induced hyperlipidemia, Mixed hypertriglyceridemia, Endogenous hypertriglyceridemia.
Overview
Type 5 Hyperlipoproteinemia (HLP V) is a rare disorder of lipo-protein metabolism characterized by fasting chylomicronemia and elevated levels of cholesterol in the very low density (VLD) lipoprotein fraction. The triglyceride(TG) levels are invariably greater than 1000mg/dl thereby increasing the risk of pancreatitis.It has been postulated that HLP V is the result of a defective clearance of TG-rich lipoproteins(VLDLs and Chylomicrons),although lipoprotein lipase is not absent. Another suggested mechanism is of VLDL TG's overproduction. Some patients seem to have "Primary" HLP V which usually appears first in adulthood,this phenotype is often associated with secondary factors,almost always Diabetes Mellitus.May be associated with Eruptive Xanthomas and Hyperuricemia. The primary goal of therapy is to reduce the TG level to <500mg/dl for the intent of reducing the risk of pancreatitis.
Historical Perspective
- In 1967, Dr. Fredrickson classified lipoprotein disorders using paperelectrophoresis.[1]
Classification
Classification based on etiologyAlthough the exact etiology of HLP V remains unclear till date,it has been postulated that its largely due to a combination of genetic and acquired factors.
❑ Secondary/Acquired/Environmental
|
Classification by Severity of TriglyceridesHypertriglyceridemia may be classified according to the concentration of triglycerides on the lipid profile. More marked elevations are usually seen in cases of hypertriglyceridemia resulting from secondary causes.[2] ❑ Normal triglycerides: <150 mg/dL, To view the ATPIII guidelines for classification of triglyceride levels click here. |
Classification by Severity of MutationsHLP V may be classified according to the severity of the mutation involving the APOA5 gene. |
Pathophysiology
The two main sources of plasma triglycerides (also known as triacylglycerol) are exogenous (i.e., from dietary fat) and carried in chylomicrons, and endogenous (from the liver) and carried in very-low-density lipoprotein (VLDL) particles. In capillaries within fat and muscle tissue, these lipoproteins and chylomicrons are hydrolyzed by lipoprotein lipase into free fatty acids. After a meal, over 90% of the circulating triglycerides originate in the intestine and are secreted in chylomicrons, whereas during periods of fasting, endogenous triglycerides secreted by the liver as VLDL predominate. The increase in plasma of triglyceride-rich lipoproteins results from increased production from the liver and intestine (by means of upregulated synthetic and secretory pathways) or through decreased peripheral catabolism (mainly from reduced lipoprotein lipase activity).
Pathogenesis
The pathogenesis of type V is not fully understood. However; VLDL appears to be the most affected lipoprotein fraction in type V and there is three-fold increase in synthesis rate as well as decreased fractional catabolism of VLDL.The molecular basis for Type V HLP is not clearly understood.[3] In patients with type V HLP, the presence of underlying diseases or contributing factors such as Diabetes and alcohol abuse occurs in ~67% of patients and the remaining patients usually show type IV HLP and have hypertriglyceridemia in the family.Transiently impaired LPL activity with no defect in LPL enzyme induced severe hypertriglyceridemia in infants. The transient occurrence of inhibitor(s) for LPL was proposed.[3]
Genetics
Precise genetic patterns have not been determined for type V HLP and it has been suggested that type V may be due to number of genetic defects. Among them, the apo E and its isoforms may have an important clinical significance in type V HLP and may affect the catabolism of triglyceride rich lipoproteins. The presence of apo E4 allele may be the genetic factor that predisposes to the development of type V due to delayed lipoprotein clearance.
Associated Conditions
- diabetes mellitus
- alcohol abuse
- glycogen storage disease type I
- Hyperuricemia
- Pancreatitis
- Eruptive xanthomas.
Causes
Type V hyperlipoproteinemia is more complicated and more closely related to acquired environmental factors. It rarely shows familial occurrence, but its inheritance is variable. Therefore, type V HLP is usually considered to be triggered by acquired environmental factors in individuals with some congenital susceptibility to altered triglyceride metabolism (genetic factors). While the involved environmental factors vary, involvement of heavy drinking, type 2 Diabetes, hormonal therapy and medications are frequently observed.[3]
Causes by Pathophysiology
| Congenital (Genetic) Factors | Secondary causes of Dyslipidemia[4] | |
|---|---|---|
|
Due to disordered metabolism or disease | Due to drugs |
| Common Clinical Causes : Increased body fat with adiposopathy, Metabolic syndrome, Insulin resistance, Nutritional content, Limited physical activity, Cigarette smoking, Acute or substantial alcohol consumption, especially in patients with fatty liver, Pregnancy, Anorexia nervosa, Post solid organ transplantation, especially with marked medical stress and use of high dose immunosuppressants (e.g. corticosteroids).
Endocrine Diseases: Inadequately controlled diabetes mellitus, Untreated hypothyroidism, Lipodystrophy, Polycystic ovarian syndrome, Chronic kidney disease, Nephrotic syndrome. Liver Disease: Hepatitis with fatty liver, Cholestasis, Biliary cirrhosis, Primary sclerosing cholangitis (cholesterol levels may be mildly increased with low rate of ASCVD; cholesterol levels are decreased with cirrhosis), Narrowed and malformed bile ducts (Alagille syndrome) Pancreatic Disease: If acute pancreatitis results in insulinopenia, hyperglycemia, and systemic stress, then acute pancreatitis can potentially contribute to hypertriglyceridemia (e.g. triglyceride-induced pancreatitis can potentially worsen triglyceride levels) Infections: Human immunodeficiency virus infection, especially if treated with highly active anti-retroviral therapy Inflammatory Diseases: Systemic lupus erythematosus, Rheumatoid arthritis Storage Diseases: Glycogen storage disease, Gaucher’s disease, Cystine storage disease, Juvenile Tay-Sachs disease, Niemann-Pick disease Others: Progeria, Idiopathic hypercalcemia, Klinefelter syndrome, Werner’s syndrome, Kawasakis disease, Acute intermittent porphyria. |
Hormones or hormone- like agents:
Cariometabolic pharmacotherapies: Recreational drugs: Immuno-active agents: Anti-neoplastic agents: Anti psychotic drugs: Other pharmacotherapies: | |
Differentiating HLP type 5 from other conditions associated with raised triglycerides
HLP type 5 must be differentiated from other diseases that cause abnormal increase in triglycerides in the blood.
- Familial hyperchylomicronemia
- Familial hypercholesterolemia/ Familial combined hyperlipidemia
- Dysbetalipoprotenemia
- Primary hypertriglyceridemia/ Primary hypertriglyceridemia
- Drugs Causing high triglyceride levels:[5]
- Atypical antipsychotic drugs(Fluperlapine, Clozapine, Olanzapine), Beta-blockers (especially non-beta 1-selective), Bile acid sequestrants, Cyclophosphamide, Glucocorticoids, Immunosuppressive drugs (Cyclosporine, Sirolimus), Interferon, L-asparaginase, Oral estrogens, Protease inhibitors, Raloxifene, Retinoids, Rosiglitazone, Tamoxifen, Thiazide diuretics.
Epidemiology and Demographics
Prevalence/Incidence
It is difficult to accurately estimate the prevalence of HLP V in the general population,although the estimated incidence being <1/1,000,000. but a survey of about 40,000 people by the Lipid Research Clinic reported the frequency of individuals with a plasma TG level of 2,000 mg/dl or higher to be about 0.018%.
Age
Average triglyceride levels in type V hyperlipoproteinemia were lower for women than for men before age 50.[6]
Gender
- Average triglyceride levels in type V hyperlipoproteinemia were lower for women than for men before age 50.
Race
In Western population, LPL gene abnormalities were observed in 10% of patients with type V HLP.
Risk Factors
- Family history of dyslipoproteinemia
- Diabetes
- Alcohol abuse
- Obesity
Screening
- First-degree relatives should be screened for hyperlipidemia.
Natural History, Complications and Prognosis
Natural History
Mixed hyperlipidemia—a common disorder that becomes more prevalent with increasing age.A history of acute pancreatitis was observed in about 17% of the patients, demonstrating that hyperlipidemia is frequently complicated by pancreatitis also in Japanese, in whom the fat intake is lower than in Western people, and stressing the importance of its prevention and management.
- Restriction of dietary fat eliminates chylomicrons and the lipoprotein panel changes to type 4 hyperlipoproteinemia.
Complications
Prognosis
The prognosis is uncertain due to the risk of Pancreatitis.Increased fat intake may cause recurrent bouts of illness possibly leading to pseudocyst formation,hemorrhage and death.
Diagnosis
Diagnostic Criteria
- I. Demonstration of an increase in VLDL in addition to hyperchylomicronemia.
- II. The absence of LPL deficiency, Apolipoprotein C-II deficiency, Apo E deficiency.
Definitely diagnosed if both I and II are fulfilled.
- Fasting chylomicronemia can be diagnosed by confirming the presence of chylomicrons and excess VLDL on agarose gel electrophoresis or ultracentrifugal analysis. A simple technique is to refrigerate plasma overnight and examine the specimen for a creamy supernatant from chylomicrons and a turbid VLDL-rich infranatant.This latter finding of a turbid infranatant is not seen in patients with type I hyperlipoproteinemia, in which only chylomicrons accumulate and the infranatant is clear.
- Also,the identification of other primary relatives with dyslipidemias is useful in making the diagnosis.
History and Symptoms
HTGemia is usually asymptomatic until TG levels are greater than 1000-2000 mg/dl. Signs and symptoms may include the following.
- GI : Pain in the mid-epigastric, chest, or back regions; nausea, vomiting.
- Respiratory: Dyspnea
- Dermatologic: Xanthomas xanthomas
- Ophthalmologic: Lipemia Retinalis
- Neurological:Recent memory loss
Always enquire about family history of Diabetes.
Physical Examination
Physical examination of patients with HLP V is usually normal.
The additional findings may be subjective and include:
- ABDOMEN: Hepato-Splenomegaly.
- SKIN:Eruptive Xanthomas.
Laboratory Findings
Laboratory studies used to evaluate hypertriglyceridemia include the following:
| Laboratory finding | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Phenotype | Lipoprotein(s)
Elevated |
Serum total
cholesterol |
HDL | Serum
triglycerides |
Plasma
appearance
|
Glucose
tolerance |
Carbohydrate
inducibility |
Fat tolerance | Electrophoresis | Cholesterol/TG ratio | LDL/HDL ratio |
| Hyperlipoproteinemia type 5 | Chylomicrons and VLDL ↑ | ↑↑ | ↓↓↓ | ↑↑↑ | Creamy top and Turbid bottom | Impaired | May be abnormal | Markedly abnormal | Pre-beta band ↑↑,beta and alpha ↓ | >0.15 and <0.6 | ↓ |
- LIPID ANALYSIS
-Measurement of plasma lipid and lipoprotein levels after an overnight fast.
- Elevated triglycerides are determined by direct laboratory analysis of serum or plasma,however determining which lipoprotein abnormality is the cause of hypertriglyceridemia is less straightforward.
- Both VLDL and chylomicrons are usually highly elevated.
- Tests to rule out secondary causes of hypertriglyceridemia include:
fasting or random glucose levels thyroid-stimulating hormone [TSH] levels urinalysis, creatinine, and micro albumin If the diagnosis of eruptive xanthomas is in doubt, obtaining a biopsy of the suspicious lesions will reveal accumulations of fat (not cholesterol). The only procedure that reliably distinguishes between a mixed hyperlipoproteinemia (increased LDL cholesterol and triglycerides) and type III hyperlipoproteinemia (increased IDL) is beta quantification (lipoprotein electrophoresis) Chylomicron Determination If the triglyceride levels are greater than 1000 mg/dL and the presence of chylomicrons must be confirmed, the simplest and most cost-effective test involves overnight refrigeration of an upright tube of plasma or serum. If a creamy supernatant is seen the next day, chylomicrons are present. If the infranatant is cloudy, high levels of very low-density lipoprotein (VLDL) are present (type V hyperlipidemia)
Imaging Findings
Other Diagnostic Studies
Treatment
The evaluation and treatment decisions for HLP V should be based on patient-centered and individual circumstances. Lifestyle therapies, such as appropriate nutrition and physical activity, are important elements of ASCVD risk reduction, with or without lipid-altering drug therapy. For patients in whom lipid-altering drug therapy is indicated, statin treatment is the primary pharmacologic modality for reducing ASCVD risk.
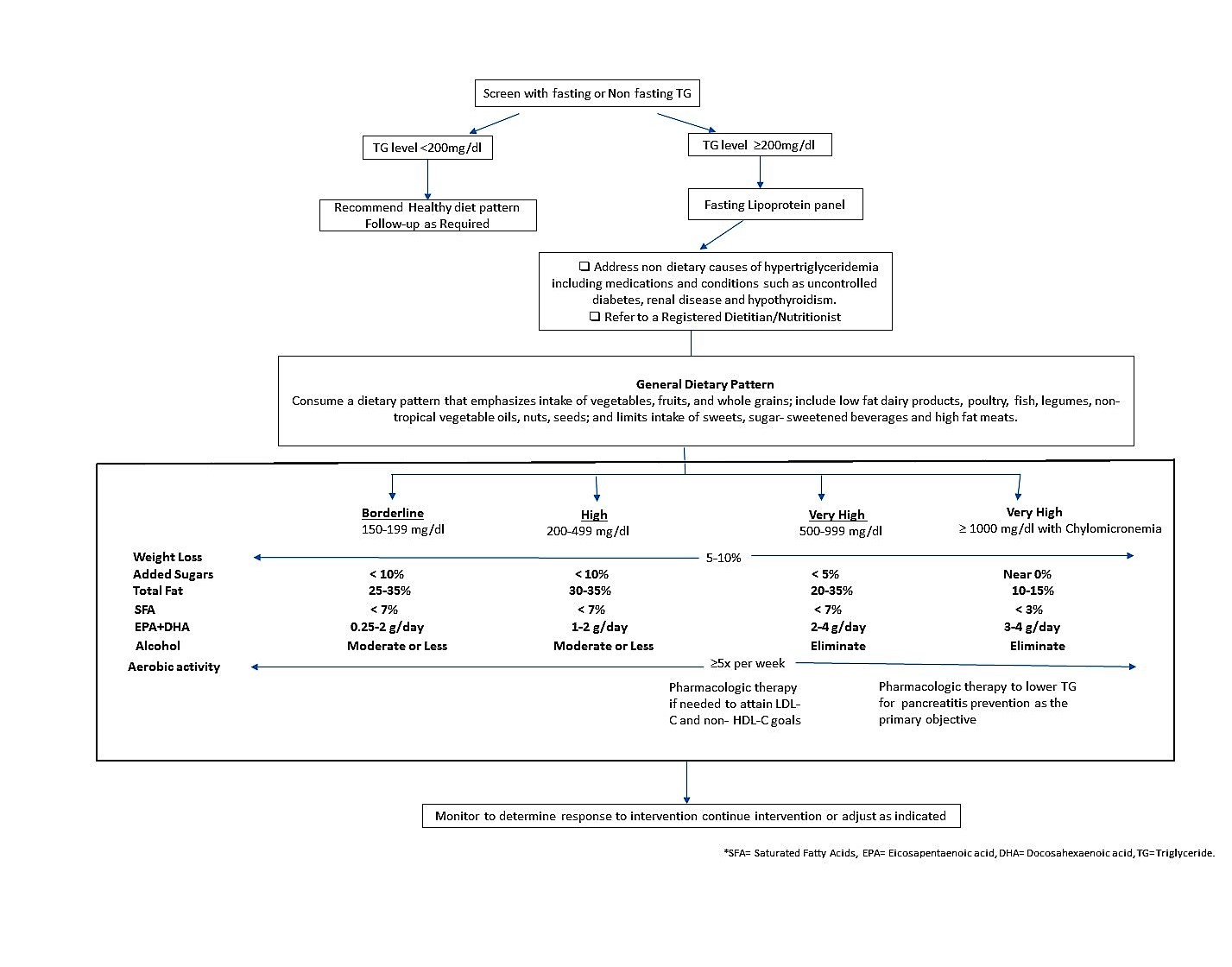
Clinical algorithm for screening and management of elevated TG[10]
Medical Therapy
When the triglyceride concentration is very high (≥500 mg/dL, and especially if ≥1000 mg/dL), the primary goal of therapy is to reduce the triglyceride level to <500 mg/dL for the intent of reducing the risk of pancreatitis.
| Triglyceride concentration | First line of therapy |
|---|---|
| ≥1000mg/dl | Triglyceride lowering agents such as ❑ Fibric acids ❑ High-dose [2 to 4 g/d] long-chain omega-3 fatty acids ❑ Nicotinic acid |
| 500-999mg/dl | ❑ Triglyceride lowering agents, ❑ Statins |
| 200-499mg/dl | Statin will generally be first-line drug therapy.If maximum tolerated statin therapy does not lower non-HDL-C below goal levels in patients with triglycerides 200 to 499 mg/dL, adding an agent that primarily lowers triglycerides may help to achieve atherogenic cholesterol goals. |
When triglycerides are between 200 and 499mg/dL, the primary targets of lipid therapy are non–HDL-C and LDL-C for the purpose of reducing ASCVD risk.
| Lipid treatment goals to reduce ASCVD risk[10] | ||
|---|---|---|
| Risk of ASCVD | Indication for drug therapy | Goal of drug therapy |
| Low ASCVD risk | Non HDL- C* level ≥190mg/dl LDL-C level ≥160mg/dl |
Non HDL- C level <130mg/dl LDL-C level <100mg/dl |
| Moderate ASCVD risk | Non HDL- C* level ≥160mg/dl LDL-C level ≥130mg/dl |
Non HDL- C level <130mg/dl LDL-C level <100mg/dl |
| High ASCVD risk | Non HDL- C level ≥130mg/dl LDL-C level ≥100mg/dl |
Non HDL- C level <130mg/dl LDL-C level <100mg/dl |
| Very high ASCVD risk | Non HDL- C level ≥100mg/dl LDL-C level ≥70mg/dl |
Non HDL- C level <100mg/dl LDL-C level <70mg/dl |
Non–HDL-C comprises the cholesterol carried by all atherogenic particles, including LDL, intermediatedensity lipoproteins, very low-density lipoproteins (VLDL) and VLDL remnants, chylomicron remnants, and lipoprotein.[4]
Surgery
The effect of bariatric surgery on lipid levels is variable and dependent upon the type of bariatric surgical procedure (e.g., gastric bypass, gastric sleeve, adjustable gastric banding).Gastric bypass procedures generally produce greater improvements in lipid and other metabolic parameters because of greater reductions in body fat, alterations in gut and other hormones, and improvements in inflammatory factors.[4]Bariatric surgery significantly improved multiple metabolic parameters, and reduced overall mortality.Regarding lipids, compared with conventional therapy, bariatric surgery significantly reduced the incidence of hypertriglyceridemia (defined as ≥150 mg/dL) and the incidence of low HDL-C (defined as <39 mg/dL) but no significant reduction in hypercholesterolemia (defined as ≥200 mg/dL).[11]
Primary Prevention
There is no way to prevent the genetic disease.Although,there is a lot of scope to control the Environmental factors,especially in those with a family history of Dyslipidemia.
Secondary Prevention
- Lifestyle interventions are a key to reduce triglycerides that includes[10]
- weight loss if overweight or obese
- physical activity (≥ 150 minutes per week of moderate or higher intensity activity)
- Restriction of alcohol
- Restriction of sugar/refined carbohydrate intakes
- For patients with very high TG level (≥500 mg/dL),chylomicronemia will generally be present. For such patients, a low-fat diet (,15% of energy) may be helpful to reduce entry of new chylomicron particles into the circulation.[10]
- For patients with triglycerides <500 mg/dL, partial replacement of dietary carbohydrate (especially sugars and other refined carbohydrates) with a combination of unsaturated fats and proteins may help to reduce the triglyceride and non-HDL-C concentrations.
References
[12] [13] [14] [3] [15] [16] [17] [16] [18] [19] [[[20]]] [21]
- ↑ Culliton BJ (1987) Fredrickson's bitter end at Hughes. Science 236 (4807):1417-8. PMID: 3296193
- ↑ National Cholesterol Education Program (NCEP) Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults (Adult Treatment Panel III) (2002). "Third Report of the National Cholesterol Education Program (NCEP) Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults (Adult Treatment Panel III) final report". Circulation. 106 (25): 3143–421. PMID 12485966.
- ↑ 3.0 3.1 3.2 3.3 Gotoda T, Shirai K, Ohta T, Kobayashi J, Yokoyama S, Oikawa S et al. (2012) Diagnosis and management of type I and type V hyperlipoproteinemia. J Atheroscler Thromb 19 (1):1-12. PMID: 22129523
- ↑ 4.0 4.1 4.2 Bays HE, Jones PH, Orringer CE, Brown WV, Jacobson TA (2016) National Lipid Association Annual Summary of Clinical Lipidology 2016. J Clin Lipidol 10 (1 Suppl):S1-43. DOI:10.1016/j.jacl.2015.08.002 PMID: 26891998
- ↑ Jacobson TA, Ito MK, Maki KC, Orringer CE, Bays HE, Jones PH et al. (2014) National Lipid Association recommendations for patient-centered management of dyslipidemia: part 1 - executive summary. J Clin Lipidol 8 (5):473-88. DOI:10.1016/j.jacl.2014.07.007 PMID: 25234560
- ↑ Greenberg BH, Blackwelder WC, Levy RI (1977) Primary type V hyperlipoproteinemia. A descriptive study in 32 families. Ann Intern Med 87 (5):526-34. PMID: 200162
- ↑
- ↑
- ↑
- ↑ 10.0 10.1 10.2 10.3 Jacobson TA, Ito MK, Maki KC, Orringer CE, Bays HE, Jones PH et al. (2015) National lipid association recommendations for patient-centered management of dyslipidemia: part 1--full report. J Clin Lipidol 9 (2):129-69. DOI:10.1016/j.jacl.2015.02.003 PMID: 25911072
- ↑ Sjöström L, Narbro K, Sjöström CD, Karason K, Larsson B, Wedel H et al. (2007) Effects of bariatric surgery on mortality in Swedish obese subjects. N Engl J Med 357 (8):741-52. DOI:10.1056/NEJMoa066254 PMID: 17715408
- ↑ Park JR, Jung TS, Jung JH, Lee GW, Kim MA, Park KJ et al. (2005) A case of hypothyroidism and type 2 diabetes associated with type V hyperlipoproteinemia and eruptive xanthomas. J Korean Med Sci 20 (3):502-5. DOI:10.3346/jkms.2005.20.3.502 PMID: 15953878
- ↑ Nagasaka H, Kikuta H, Chiba H, Murano T, Harashima H, Ohtake A et al. (2003) Two cases with transient lipoprotein lipase (LPL) activity impairment: evidence for the possible involvement of an LPL inhibitor. Eur J Pediatr 162 (3):132-8. DOI:10.1007/s00431-002-1133-3 PMID: 12655414
- ↑ Calandra S, Priore Oliva C, Tarugi P, Bertolini S (2006) APOA5 and triglyceride metabolism, lesson from human APOA5 deficiency. Curr Opin Lipidol 17 (2):122-7. DOI:10.1097/01.mol.0000217892.00618.54 PMID: 16531747
- ↑ Marçais C, Verges B, Charrière S, Pruneta V, Merlin M, Billon S et al. (2005) Apoa5 Q139X truncation predisposes to late-onset hyperchylomicronemia due to lipoprotein lipase impairment. J Clin Invest 115 (10):2862-9. DOI:10.1172/JCI24471 PMID: 16200213
- ↑ 16.0 16.1 Ghiselli G, Schaefer EJ, Zech LA, Gregg RE, Brewer HB (1982) Increased prevalence of apolipoprotein E4 in type V hyperlipoproteinemia. J Clin Invest 70 (2):474-7. PMID: 7096573
- ↑ Dallongeville J (2000) Apolipoprotein E mutations, type V hyperlipoproteinaemia and diet. Br J Nutr 83 (6):573-4. PMID: 10911764
- ↑ Piolot A, Nadler F, Cavallero E, Coquard JL, Jacotot B (1996) Prevention of recurrent acute pancreatitis in patients with severe hypertriglyceridemia: value of regular plasmapheresis. Pancreas 13 (1):96-9. PMID: 8783340
- ↑ Titanji R, Paz-Guevara A (1992) Hypertriglyceridemia: severe type V hyperlipidemia in a young woman. Md Med J 41 (3):231-3. PMID: 1602929
- ↑ Stuyt PM, Stalenhoef AF, Demacker PN, van't Laar A (1982) Hyperlipoproteinemia type V and apolipoprotein E4. Lancet 2 (8304):934. PMID: 6126778
- ↑ Fallat RW, Glueck CJ (1976) Familial and acquired type V hyperlipoproteinemia. Atherosclerosis 23 (1):41-62. PMID: 1078394