Retroperitoneal abscess
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1];Associate Editor(s)-in-Chief: Ahmed Younes M.B.B.CH [2]
Synonyms and keywords: RP abscess
Overview
Retroperitoneal abscess is an unusual type of abscess in surgical practice. It is often underdiagnosed due to the insidious onset of symptoms and its location in the retroperitoneal space making it hard to be assessed via the regular abdominal examination. It is most often due to Genitourinary infection (Pyelonephritis) or gastrointestinal cause (i.e Inflammatory Bowel Syndrome). CT & MRI are the cornerstones for diagnosis. Treatment is usually focused on surgical drainage either through open or percutaneous approaches usually accompanied with the use of IV antibiotics.
Historical perspective
- Retroperitoneal abscess was first described by Grassi and Serge in 1887.
- Dr. Hugh Cabbot presented the first case of retroperitoneal abscess in a case report in 1922.
Classification
Retroperitoneal abscess may be classified according to the location in the retroperitoneal space into 5 categories [1] :
- Perinephric abscess
- Upper retroperitoneal abscess
- Pelvic abscess
- Combined retroperitoneal and pelvic abscess
- Lٍٍocalized musculoskeletal abscess
Pathophysiology
 |
Pathogenesis
- A retroperitoneal abscess is usually secondary to spread from other primary site either through hematogenous or by contiguous spread.
- The bacteria causing the abscess depends on the primary site. When the bacteria invades the retroperitoneal tissue, toxins released from it destroy the tissues and trigger an inflammatory response.
- As a result of the inflammatory response, white blood cells get recruited. They phagocytose the invading bacteria but at the same time they break down the infected tissue.
- The healthy tissues around enclose the area with a membrane surrounding the abscess.
- After pus evacuation, the membrane grows in to fill the cavity.
Microscopic findings
- The Abscess consists of a mixture of inflammatory cells together with debris tissue.
- From the surrounding wall grows some capillaries to form granulation tissue.
- If the body defenses are successful in eliminating the infection, the granulation tissue continues to grow and the abscess continues to shrink in size until it is only a scar.
- If the offending pathogen is not cleared, the process goes on and may eventually spread.
Causes
Retroperitoneal Abscess may be caused by :[2]
- E. Coli or Proteus spp (if the primary site is the urinary tract)
- Multibacterial & anaerobes (if gastrointestinal tract (GIT) is the primary source)
- Staphylococcus aureus (if from distant septic focus)
- Tuberculosis (if secondary to Pott’s disease)
Differentiating retroperitoneal abscess from other Diseases
| Disease | Clinical feature | Laboratory findings | Imaging findings | ||
|---|---|---|---|---|---|
| Fever | Weight loss | Abdominal pain | |||
| Retroperitoneal abscess | ✔ | ✔ | Leukocytosis and positive inflammatory markers | MRI is the best radiologic tool to differentiate between retroperitoneal masses. | |
| Retroperitoneal hematoma | ✔ | Anemia | |||
| Retroperitoneal tumors (.e.g. liposarcoma) | ✔ | ✔ | ✔ | Positive tumor marker | |
| Chronic pancreatitis | ✔ | ✔ | Elevated blood sugar (due to diabetes mellitus), amylase and lipase levels may be slightly elevated | ||
Epidemiology and demographics
Retroperitoneal abscess is far less common than intraperitoneal abscesses.[3]
- Males are slightly more susceptible than females.
- Increased incidence between third and sixth decades.
- Most common cause in developing countries is spread from distant septic focus.
- Most common causes in developed countries are Renal and GI causes. [2]
Risk Factors
Any septic focus can theoretically lead to retroperitoneal abscess. These are the primary foci in order of frequency of causing retroperitoneal abscess.
- Renal infections:
- Spread from the urinary tract is the most common cause.
- Gastrointestinal diseases:
- Spread from the gastrointestinal tract is the second common cause (e.g. perforated appendix, perforated colon cancer, diverticulitis ,and cohn’s disease.)
- Bone infection:
- e.g. pott's disease or osteomyelitis
- Hematogenous spread:
- From distant septic foci.
Any condition compromising the immune system is a risk factor for developing retroperitoneal abscess. The following were the risk factors in observed patients. [1]
- Diabetes Mellitus
- Cirrhosis
- Malignancy
- Remote infection
- Glucocorticoids administration
- Chronic renal failure
Screening
According to the USPSTF, screening for retroperitoneal abscess is not recommended.
Natural History, Complications and Prognosis:
Natural history
If left untreated, retroperitoneal abscess may cause septicemia with very high incidence of morbidity and mortality.
Complications :
Most complications result from septicemia which presents late in the disease.[1]
- Pneumonia and respiratory failure type 1 is the most common complication with very high mortality.
- Recurrent Abscess after drainage.
- Renal Failure
- DVT
- Small Bowel Obstruction
- Arterial Thrombosis
- UTI
- Brain abscess
- Empyema
- Osteomyelitis
Prognosis
Depending on the extent of the abscess at the time of diagnosis, the prognosis may vary. However, with the presence of the mentioned factors below, the prognosis is generally regarded poor.[1]
- Septicemia (Positive Blood Culture) : Not presenting in every patient but when present, it is a very poor prognostic sign.
- Number of days for fever to fade away after drainage: Persistence of fever more than 4 days carries a mortality more than 70%.
Diagnosis
History
- A detailed history should be obtained from the patient presenting with insidious onset of abdominal pain.
- Common causes should be investigated (Kidney and gastrointestinal diseases) especially in the presence of any of the risk factors (e.g. DM and corticosteroid administration).
Symptoms [1]:
Given that the presentation is usually insidious, nonspecific beside that it’s an unusual condition .. the diagnosis is usually delayed.
Common symptoms:
- Fever is the most common complaint and usually it is more than 101 F.
- Constitutional symptoms : chills, malaise, anorexia and weight loss.
- Abdominal pain : Not localized due to the unusual site of the abscess.
Less common symptoms:
- Gastrointestinal complaints which varies from case to case
- If abscess involves psoas major muscle, pain is usually referred to the hip, groin and knee.
Physical Exam
General Appearance
The patient is usually fatigued & looking ill due to the preexisting risk factor. In advanced cases with septicemia, the patient may be drowsy with decreased level of consciousness.[1]
Vital signs
- Fever
- Tachycardia
- Tachypnea
- Hypotension (if patient is presenting with shock)
Abdominal Examination
- Abdominal tenderness is often present (localized).
- Positive psoas sign if the psoas muscle is involved.
- The classic signs of peritonitis is absent (making the diagnosis more difficult).
Lab Findings
- Classic lab findings of inflammation as leukocytosis, high ESR, high CRP ,etc, ...Leukocytosis is usually not extremely high (between 10,000 and 20,000 in most cases)
- Blood culture is not always positive (but carries a grave prognosis if positive).Organism depends on the source of abscess as mentioned above in pathophysiology.
Radiological Findings
CT & MRI are the 2 most important radiological diagnostic tools.
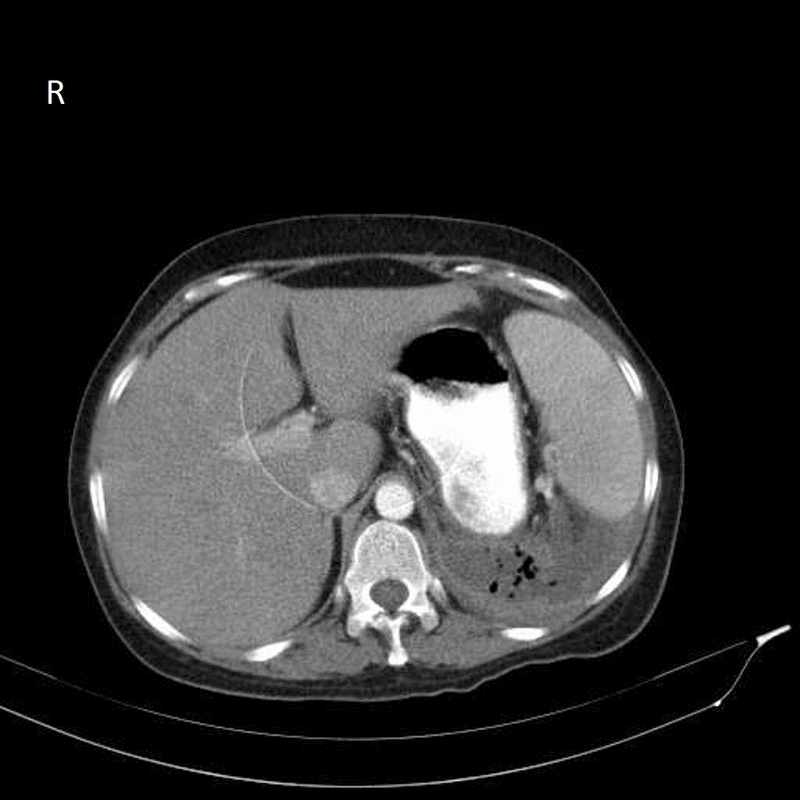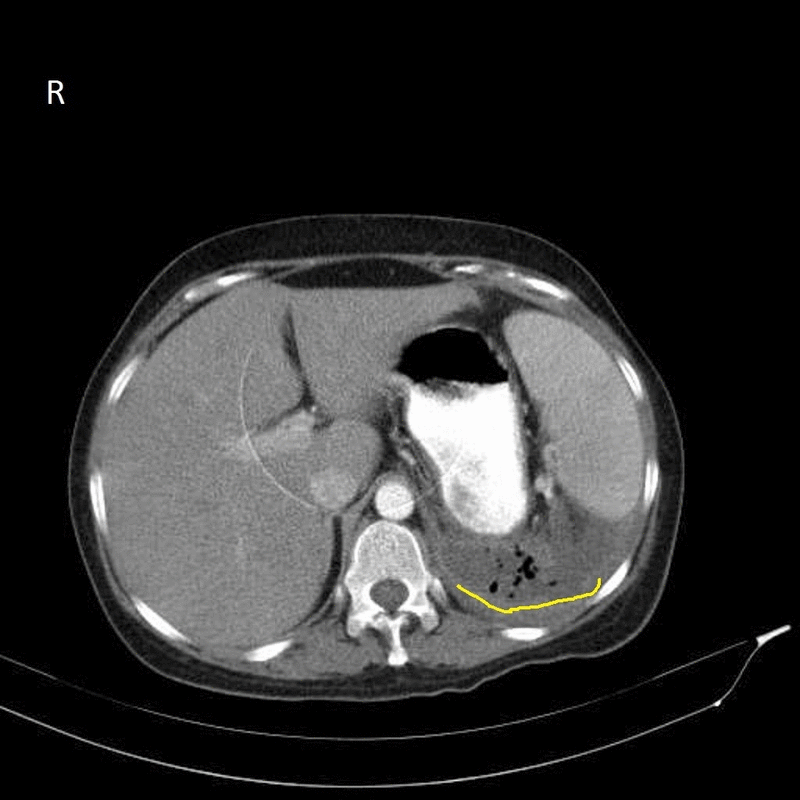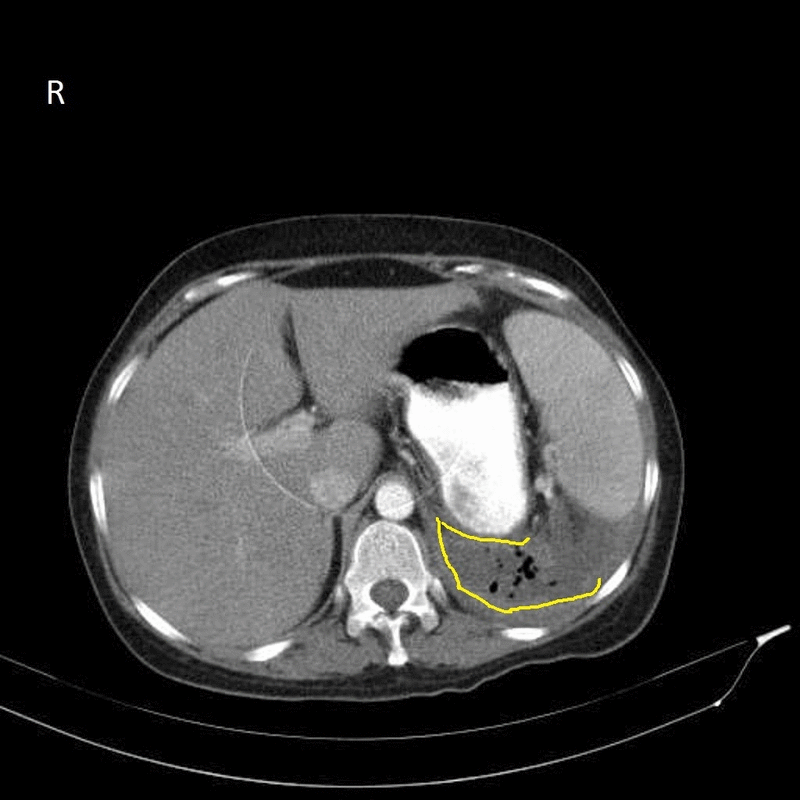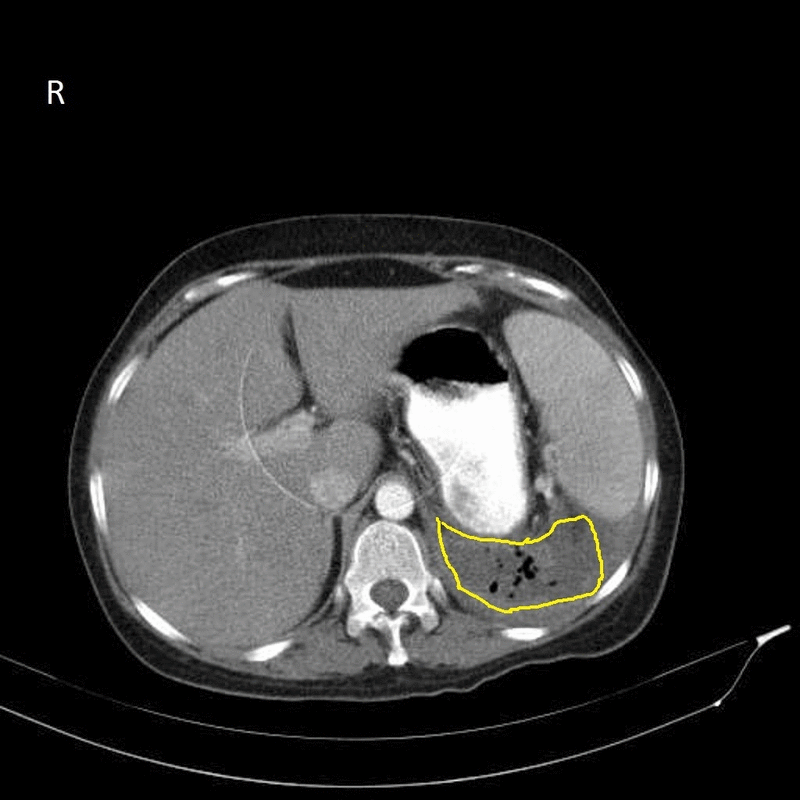
- The image shows retroperitoneal abscess in left side with gas bubbles inside (circled area)
CT
- CT shows fluid collection in the retroperitoneal space and may also show gas bubbles. It is also helpful in determining the primary source of the abscess.
MRI
- Shows the same findings as CT, but more sensitive.
Ultrasonography
- Not the preferred diagnostic tool because of the remote site of the abscess.
Treatment
Overview
Surgery is the mainstay of treatment together with the proper use of antibiotics.
Medical Treatment
- Intravenous empiric antibiotics should be started till results of the cultures are available.[1]
| Regimen | Pediatrics | Adults | |
|---|---|---|---|
| Mild - Moderate infection | Severe infection | ||
| Single agent | Ertapenem, meropenem, imipenem, cilastatin, ticarcillin-clavulanate, and piperacillin-tazobactam | Cefoxitin, ertapenem, moxifloxacin, tigecycline, and ticarcillin-clavulanic acid | Imipenem-cilastatin, meropenem, doripenem, and piperacillin-tazobactam |
| Combination | Ceftriaxone, cefotaxime, cefepime, or ceftazidime, each in combination with metronidazole; gentamicin or tobramycin, each in combination with metronidazole or clindamycin, and with or without ampicillin | Cefepime, ceftazidime, ciprofloxacin, or levofloxacin, each in combination with metronidazole. | Cefepime, ceftazidime, ciprofloxacin, or levofloxacin, each in combination with metronidazole. |
| Organisms that are common in health care facility | Regimen | ||||
|---|---|---|---|---|---|
| Carbapenem | Aminoglycoside | Ceftazidime or cefepime, each with metronidazole | Piperacillin-tazobactam | Vancomycin | |
| <20% Resistant Pseudomonas aeruginosa, extended-spectrum b-lactamase-producing Enterobacteriaceae, Acinetobacter, or other multidrug resistant gram-negative bacilli | Recommended | Not recommended | Recommended | Recommended | Not recommended† |
| Extended-spectrum b-lactamase-producing Enterobacteriaceae | Recommended | Recommended | Not recommended | Recommended | Not recommended |
| P. aeruginosa 120% resistant to ceftazidime | Recommended | Recommended | Not recommended | Recommended | Not recommended |
| Methicillin-resistant Staphylococcus aureus | Not recommended | Not recommended | Not recommended | Not recommended | Recommended |
- Drainage of the abscess is a must and using medical treatment alone carries a mortality rate approaching 100 % in some studies.
Surgical Treatment :
- Operative treatment is usually preferred unless there is a special condition for which surgery is contraindicated.[1]
- Retroperitoneal or pelvic approaches are much more preferred than transperitoneal approach due to better outcomes and decreased probability of intraperitoneal spread.
References
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 1.7 Grollier G, Burucoa C, Bonnin M, de Rautlin de La Roy Y (1992). "Identification and susceptibility testing for obligate anaerobic bacteria using a semi-automated API ATB plus system". Ann Biol Clin (Paris). 50 (6–7): 393–7. PMID 1492717.
- ↑ 2.0 2.1 Winter BM, Gajda M, Grimm MO (2016). "[Diagnosis and treatment of retroperitoneal abscesses]". Urologe A. 55 (6): 741–7. doi:10.1007/s00120-016-0118-1. PMID 27220893.
- ↑ Vitale L, Kiss A, Drago GW (1994). "[Retroperitoneal abscesses: clinical and therapeutical aspects]". Minerva Chir. 49 (3): 163–5. PMID 8028724.
- ↑ 4.0 4.1 "www.idsociety.org" (PDF).