Medical ultrasonography
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]
Assistant Editor-In-Chief: Anand Patel, MD [2]
Overview
Medical ultrasonography (sonography) is an ultrasound-based diagnostic imaging technique used to visualize muscles and internal organs, their size, structures and possible pathologies or lesions. Obstetric sonography is commonly used during pregnancy and is widely recognized by the public. There are a plethora of diagnostic and therapeutic applications practiced in medicine.
In physics the term "ultrasound" applies to all acoustic energy with a frequency above human hearing (20,000 hertz or 20 kilohertz). Typical diagnostic sonographic scanners operate in the frequency range of 2 to 18 megahertz, hundreds of times greater than this limit. The choice of frequency is a trade-off between spatial resolution of the image and imaging depth: lower frequencies produce less resolution but image deeper into the body.
Diagnostic applications
Sonography (ultrasonography) is widely used in medicine. It is possible to perform diagnosis or therapeutic procedures with the guidance of sonography (for instance biopsies or drainage of fluid collections). Sonographers are medical professionals who perform scans for diagnostic purposes. Sonographers typically use a hand-held probe (called a transducer) that is placed directly on and moved over the patient. A water-based gel is used to couple the ultrasound between the transducer and patient.
Sonography is effective for imaging soft tissues of the body. Superficial structures such as muscles, tendons, testes, breast and the neonatal brain are imaged at a higher frequency (7-18 MHz), which provides better axial and lateral resolution. Deeper structures such as liver and kidney are imaged at a lower frequency 1-6 MHz with lower axial and lateral resolution but greater penetration.
Medical sonography is used in, for example:
- Cardiology; see echocardiography
- Endocrinology
- Gastroenterology
- Gynaecology; see gynecologic ultrasonography
- Obstetrics; see obstetric ultrasonography
- Ophthalmology; see A-scan ultrasonography, B-scan ultrasonography
- Urology, to determine, for example, the amount of fluid retained in a patient's bladder.
- Musculoskeletal, ligaments, tendons, muscles, and nerves; see Diagnostic musculoskeletal ultrasound
- Vascular, arteries and veins
- Intravascular ultrasound (e.g. ultrasound guided fluid aspiration, fine needle aspiration, guided injections)
- Intervenional; biopsy, emptying fluids, intrauterine transfusion (Hemolytic disease of the newborn)
- Contrast-enhanced ultrasound
A general-purpose sonographic machine may be able to be used for most imaging purposes. Usually specialty applications may be served only by use of a specialty transducer. The dynamic nature of many studies generally requires specialized features in a sonographic machine for it to be effective; such as endovaginal, endorectal, or transesophageal transducers.

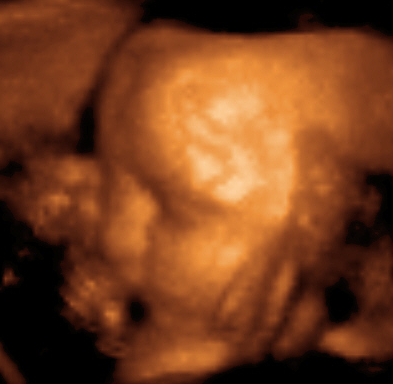
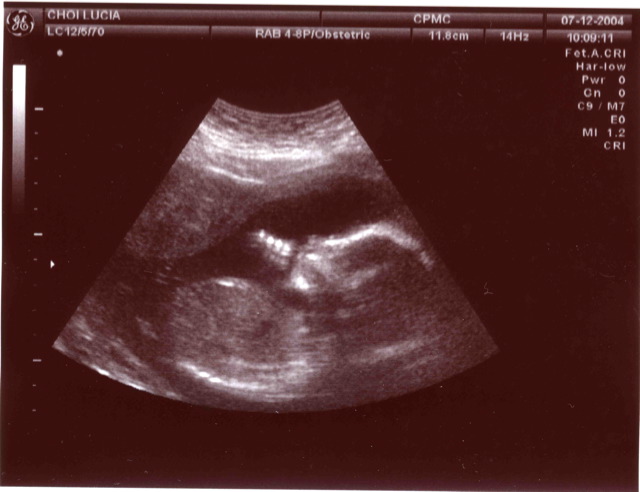
Obstetrical ultrasound is commonly used during pregnancy to check on the development of the fetus.
In a pelvic sonogram, organs of the pelvic region are imaged. This includes the uterus and ovaries or urinary bladder. Men are sometimes given a pelvic sonogram to check on the health of their bladder and prostate. There are two methods of performing a pelvic sonography - externally or internally. The internal pelvic sonogram is performed either transvaginally (in a woman) or transrectally (in a man). Sonographic imaging of the pelvic floor can produce important diagnostic information regarding the precise relationship of abnormal structures with other pelvic organs and it represents a useful hint to treat patients with symptoms related to pelvic prolapse, double incontinence and obstructed defecation.[1]
In abdominal sonography, the solid organs of the abdomen such as the pancreas, aorta, inferior vena cava, liver, gall bladder, bile ducts, kidneys, and spleen are imaged. Sound waves are blocked by gas in the bowel, therefore there are limited diagnostic capabilities in this area. The appendix can sometimes be seen when inflamed eg: appendicitis.
Therapeutic applications
Therapeutic applications use ultrasound to bring heat or agitation into the body. Therefore much higher energies are used than in diagnostic ultrasound. In many cases the range of frequencies used are also very different.
- Ultrasound may be used to clean teeth in dental hygiene.
- Ultrasound sources may be used to generate regional heating in biological tissue, e.g. in occupational therapy, physical therapy and cancer treatment.
- Focused ultrasound may be used to generate highly localized heating to treat cysts and tumors (benign or malignant), This is known as Focused Ultrasound Surgery (FUS) or High Intensity Focused Ultrasound (HIFU). These procedures generally use lower frequencies than medical diagnostic ultrasound (from 250 kHz to 2000 kHz), but significantly higher energies. HIFU treatment is often guided by MRI.
- Focused ultrasound may be used to break up kidney stones by lithotripsy.
- Ultrasound may be used for cataract treatment by phacoemulsification.
- Additional physiological effects of low-intensity ultrasound have recently been discovered, e.g. its ability to stimulate bone-growth and its potential to disrupt the blood-brain barrier for drug delivery.
From sound to image
The creation of an image from sound is done in three steps - producing a sound wave, receiving echoes, and interpreting those echoes.
Producing a sound wave
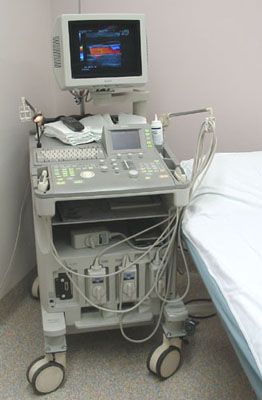
A sound wave is typically produced by a piezoelectric transducer encased in a probe. Strong, short electrical pulses from the ultrasound machine make the transducer ring at the desired frequency. The frequencies can be anywhere between 2 and 15 MHz. The sound is focused either by the shape of the transducer, a lens in front of the transducer, or a complex set of control pulses from the ultrasound scanner machine. This focusing produces an arc-shaped sound wave from the face of the transducer. The wave travels into the body and comes into focus at a desired depth.
Older technology transducers focus their beam with physical lenses. Newer technology transducers use phased array techniques to enable the sonographic machine to change the direction and depth of focus. Almost all piezoelectric transducers are made of ceramic.
Materials on the face of the transducer enable the sound to be transmitted efficiently into the body (usually seeming to be a rubbery coating, a form of impedance matching). In addition, a water-based gel is placed between the patient's skin and the probe.
The sound wave is partially reflected from the layers between different tissues. In detail, sound is reflected anywhere there are density changes in the body: e.g. blood cells in blood plasma, small structures in organs, etc. Some of the reflections return to the transducer.
Receiving the echoes
The return of the sound wave to the transducer results in the same process that it took to send the sound wave, except in reverse. The return sound wave vibrates the transducer, the transducer turns the vibrations into electrical pulses that travel to the ultrasonic scanner where they are processed and transformed into a digital image.
Forming the image
The sonographic scanner must determine three things from each received echo:
- The direction of the echo.
- How strong the echo was.
- How long it took the echo to be received from when the sound was transmitted.
Once the ultrasonic scanner determines these three things, it can locate which pixel in the image to light up and to what intensity.
Transforming the received signal into a digital image may be explained by using a blank spreadsheet as an analogy. We imagine our transducer is a long, flat transducer at the top of the sheet. We will send pulses down the 'columns' of our spreadsheet (A, B, C, etc.). We listen at each column for any return echoes. When we hear an echo, we note how long it took for the echo to return. The longer the wait, the deeper the row (1,2,3, etc.). The strength of the echo determines the brightness setting for that cell (white for a strong echo, black for a weak echo, and varying shades of grey for everything in between.) When all the echoes are recorded on the sheet, we have a greyscale image.
Sound in the body

Ultrasonography (sonography) uses a probe containing one or more acoustic transducers to send pulses of sound into a material. Whenever a sound wave encounters a material with a different density (acoustical impedance), part of the sound wave is reflected back to the probe and is detected as an echo. The time it takes for the echo to travel back to the probe is measured and used to calculate the depth of the tissue interface causing the echo. The greater the difference between acoustic impedances, the larger the echo is. If the pulse hits gases or solids, the density difference is so great that most of the acoustic energy is reflected and it becomes impossible to see deeper.
The frequencies used for medical imaging are generally in the range of 1 to 18 MHz. Higher frequencies have a correspondingly smaller wavelength, and can be used to make sonograms with smaller details. However, the attenuation of the sound wave is increased at higher frequencies, so in order to have better penetration of deeper tissues, a lower frequency (3-5 MHz) is used.
Seeing deep into the body with sonography is very difficult. Some acoustic energy is lost every time an echo is formed, but most of it (approximately <math>\textstyle 0.3 \frac{\mbox{dB}}{\mbox{cm depth}\cdot\mbox{MHz}}</math>)is lost from acoustic absorption.
The speed of sound is different in different materials, and is dependent on the acoustical impedance of the material. However, the sonographic instrument assumes that the acoustic velocity is constant at 1540 m/s. An effect of this assumption is that in a real body with non-uniform tissues, the beam become somewhat de-focused and image resolution is reduced.
To generate a 2D-image, the ultrasonic beam is swept. A transducer may be swept mechanically by rotating or swinging. Or a 1D phased array transducer may be use to sweep the beam electronically. The received data is processed and used to construct the image. The image is then a 2D representation of the slice into the body.
3D images can be generated by acquiring a series of adjacent 2D images. Commonly a specialised probe that mechanically scans a conventional 2D-image transducer is used. However, since the mechanical scanning is slow, it is difficult to make 3D images of moving tissues. Recently, 2D phased array transducers that can sweep the beam in 3D have been developed. These can image faster and can even be used to make live 3D images of a beating heart.
Doppler ultrasonography is used to study blood flow and muscle motion. The different detected speeds are represented in color for ease of interpretation, for example leaky heart valves: the leak shows up as a flash of unique color. Colors may alternatively be used to represent the amplitudes of the received echoes.
Modes of Sonography
Four different modes of ultrasound are used in medical imaging[2]. These are:
- A-mode: A-mode is the simplest type of ultrasound. A single transducer scans a line through the body with the echoes plotted on screen as a function of depth. Therapeutic ultrasound aimed at a specific tumor or calculus is also A-mode, to allow for pinpoint accurate focus of the destructive wave energy.
- B-mode: In B-mode ultrasound, a linear array of transducers simultaneously scans a plane through the body that can be viewed as a two-dimensional image on screen.
- M-mode: M stands for motion. In m-mode a rapid sequence of B-mode scans whose images follow each other in sequence on screen enables doctors to see and measure range of motion, as the organ boundaries that produce reflections move relative to the probe.
- Doppler mode: This mode makes use of the Doppler effect.
Doppler sonography



Sonography can be enhanced with Doppler measurements, which employ the Doppler effect to assess whether structures (usually blood) are moving towards or away from the probe, and its relative velocity. By calculating the frequency shift of a particular sample volume, for example a jet of blood flow over a heart valve, its speed and direction can be determined and visualised. This is particularly useful in cardiovascular studies (sonography of the vasculature system and heart) and essential in many areas such as determining reverse blood flow in the liver vasculature in portal hypertension. The Doppler information is displayed graphically using spectral Doppler, or as an image using color Doppler (directional Doppler) or power Doppler (non directional Doppler). This Doppler shift falls in the audible range and is often presented audibly using stereo speakers: this produces a very distinctive, although synthetic, pulsing sound.
Strictly speaking, most modern sonographic machines do not use the Doppler effect to measure velocity, as they rely on pulsed wave Doppler (PW). Pulsed wave machines transmit pulses of ultrasound, and then switch to receive mode. As such, the reflected pulse that they receive is not subject to a frequency shift, as the insonation is not continuous. However, by making several measurements, the phase change in subsequent measurements can be used to obtain the frequency shift (since frequency is the rate of change of phase). To obtain the phase shift between the received and transmitted signals, one of two algorithms is typically used: the Kasai algorithm or cross-correlation. Older machines, that use continuous wave (CW) Doppler, exhibit the Doppler effect as described above. To do this, they must have separate transmission and reception transducers. The major drawback of CW machines, is that no distance information can be obtained (this is the major advantage of PW systems - the time between the transmitted and received pulses can be converted into a distance with knowledge of the speed of sound).
In the sonographic community (although not in the signal processing community), the terminology "Doppler" ultrasound, has been accepted to apply to both PW and CW Doppler systems despite the different mechanisms by which the velocity is measured.
Microbubbles
The use of microbubble contrast media in medical sonography to improve ultrasound signal backscatter is known as contrast-enhanced ultrasound. This technique is currently used in echocardiography, and may have future applications in molecular imaging and drug delivery.
Strengths of sonography
- It images muscle and soft tissue very well and is particularly useful for delineating the interfaces between solid and fluid-filled spaces.
- It renders "live" images, where the operator can dynamically select the most useful section for diagnosing and documenting changes, often enabling rapid diagnoses.
- It shows the structure of organs.
- It has no known long-term side effects and rarely causes any discomfort to the patient.
- Equipment is widely available and comparatively flexible.
- Small, easily carried scanners are available; examinations can be performed at the bedside.
- Relatively inexpensive compared to other modes of investigation (e.g. computed X-ray tomography, DEXA or magnetic resonance imaging).
Weaknesses of ultrasonic imaging
- Sonographic devices have trouble penetrating bone. For example, sonography of the adult brain is very limited.
- Sonography performs very poorly when there is a gas between the transducer and the organ of interest, due to the extreme differences in acoustic impedance. For example, overlying gas in the gastrointestinal tract often makes ultrasound scanning of the pancreas difficult, and lung imaging is not possible (apart from demarcating pleural effusions).
- Even in the absence of bone or air, the depth penetration of ultrasound is limited, making it difficult to image structures deep in the body, especially in obese patients.
- The method is operator-dependent. A high level of skill and experience is needed to acquire good-quality images and make accurate diagnoses.
- There is no scout image as there is with CT and MR. Once an image has been acquired there is no exact way to tell which part of the body was imaged.
Risks and side-effects
Ultrasonography is generally considered a "safe" imaging modality.[3] However slight detrimental effects have been occasionally observed (see below).
Diagnostic ultrasound studies of the fetus are generally considered to be safe during pregnancy. This diagnostic procedure should be performed only when there is a valid medical indication, and the lowest possible ultrasonic exposure setting should be used to gain the necessary diagnostic information under the "as low as reasonably achievable" or ALARA principle.
The promotion, selling, or leasing of ultrasound equipment for making "keepsake fetal videos" is considered by the US Food and Drug Administration to be an unapproved use of a medical device. Use of a diagnostic ultrasound system for these purposes, without a physician’s order, may be in violation of state laws or regulations.
Studies on the safety of ultrasound
- A study at the Yale Medical School found a correlation between prolonged and frequent use of ultrasound and abnormal neuronal migration in mice.[4]
- A study published in 2001 by a team working at the Karolinska Institute in Stockholm found a correlation between the number of scans received by male fetuses and subsequent left-handedness. [5]
- A meta-analysis of several ultrasonography studies found no statistically significant harmful effects from ultrasonography, but mentioned that there was a lack of data on long-term substantive outcomes such as neurodevelopment.[6]
Regulation
Diagnostic sonography is regulated in the USA by the FDA, and world-wide by other national regulatory agencies. The FDA limits acoustic output using several metrics. Generally other regulatory agencies around the world accept the FDA-established guidelines.
The primary regulated metrics are MI (Mechanical Index) a metric associated with the cavitation bio-effect, and TI (Thermal Index) a metric associated with the tissue heating bio-effect. The FDA requires that the machine not exceed limits that they have established. This requires self-regulation on the part of the manufacturer in terms of the calibration of the machine. The established limits are reasonably conservative so as to maintain diagnostic ultrasound as a safe imaging modality.
History
United States
Ultrasonic energy was first applied to the human body for medical purposes by Dr. George Ludwig at the Naval Medical Research Institute, Bethesda, Maryland in the late 1940s.[7][8]
The first demonstration of color Doppler was by Geoff Stevenson, who was involved in the early developments and medical use of Doppler shifted ultrasonic energy.[9]
Sweden
Medical ultrasonography was used 1953 at Lund University by cardiologist Inge Edler and Carl Hellmuth Hertz, the son of Gustav Ludwig Hertz, who was a graduate student at the department of nuclear physics.
Edler had asked Hertz if it was possible to use radar to look into the body, but Hertz said this was impossible. However, he said, it might be possible to use ultrasonography. Hertz was familiar with using ultrasonic reflectoscopes for nondestructive materials testing, and together they developed the idea of using this method in medicine.
The first successful measurement of heart activity was made on October 29, 1953 using a device borrowed from the ship construction company Kockums in Malmö. On December 16 the same year, the method was used to generate an echo-encephalogram (ultrasonic probe of the brain). Edler and Hertz published their findings in 1954.
Scotland
Parallel developments in Glasgow, Scotland (coincidentally also a major shipbuilding centre) by Professor Ian Donald and colleagues at the Glasgow Royal Maternity Hospital (GRMH) led to the first diagnostic applications of the technique. Donald was an obstetrician with a self-confessed "childish interest in machines, electronic and otherwise", who, having treated the wife of one of the company's directors, was invited to visit the Research Department of boilermakers Babcock & Wilcox at Renfrew, Scotland where he used their industrial ultrasound equipment to conduct experiments on various morbid anatomical specimens and assess their ultrasonic characteristics. Together with the medical physicist Tom Brown and fellow obstetrician Dr John MacVicar, Donald refined the equipment to enable differentiation of pathology in live volunteer patients. These findings were reported in The Lancet on 7th June 1958 as "Investigation of Abdominal Masses by Pulsed Ultrasound" - possibly one of the most important papers ever published in the field of diagnostic medical imaging.
At GRMH, Professor Donald and Dr James Willocks then refined their techniques to obstetric applications including fetal head measurement to assess the size and growth of the foetus. With the opening of the new Queen Mother's Hospital on Yorkhill in 1964, it became possible to improve these methods even further. Dr Stuart Campbell's pioneering work on fetal cephalometry led to it acquiring long-term status as the definitive method of study of fetal growth. As the technical quality of the scans was further developed, it soon became possible to study pregnancy from start to finish and diagnose its many complications such as multiple pregnancy, fetal abnormality and placenta praevia. Diagnostic ultrasound has since been imported into practically every other area of medicine.
See also
References
- Donald I, MacVicar J, Brown TG. Investigation of abdominal masses by pulsed ultrasound. Lancet 1958;1(7032):1188-95. PMID 13550965
- Edler I, Hertz CH. The use of ultrasonic reflectoscope for the continuous recording of movements of heart walls. Kungl Fzsiogr Sallsk i Lund Forhandl. 1954;24:5. Reproduced in Clin Physiol Funct Imaging 2004;24:118-36. PMID 15165281.
- S. A. Kana (2003). Introduction to physics in modern medicine. Tsylor & Francis. ISBN 0-415-30171-8.
- C. Kasai et al. Real-time two-dimensional blood flow imaging using an autocorrelation technique. IEEE Transactions on Sonics and Ultrasonics 1985:458-464.
- Ohanyido FO,. Basic Sonology for Doctors in Low Income Settings. Healthquest 2005;3:23.
- Bushberg JT (2002). The essential physics of medical imaging. Lippincott Williams & Wilkins. ISBN 0-683-30118-7.
- ↑ Sonography of the female pelvic floor Clinical indications and techniques
- ↑ The Gale Encyclopedia of Medicine, 2nd Edition Volume 1 A-B. Page no.4
- ↑ Merritt, CR (Nov 1989). "Ultrasound safety: what are the issues?". Radiology. 173 (2): 304–306. PMID 2678243. Retrieved 2008-01-22.
- ↑ Ang ES Jr, Gluncic V, Duque A, Schafer ME, Rakic P (2006). "Prenatal exposure to ultrasound waves impacts neuronal migration in mice". Proc Natl Acad Sci U S A. 103 (34): 12903–10. PMID 16901978.
- ↑ Kieler H, Cnattingius S, Haglund B, Palmgren J, Axelsson O (2001). "Sinistrality--a side-effect of prenatal sonography: a comparative study of young men". Epidemiology (Cambridge, Mass.). 12 (6): 618–23. PMID 11679787.
- ↑ Bricker L, Garcia J, Henderson J; et al. (2000). "Ultrasound screening in pregnancy: a systematic review of the clinical effectiveness, cost-effectiveness and women's views". Health technology assessment (Winchester, England). 4 (16): i–vi, 1–193. PMID 11070816.
- ↑ "History of the AIUM". Retrieved November 15. Unknown parameter
|accessyear=ignored (|access-date=suggested) (help); Check date values in:|accessdate=(help) - ↑ "The History of Ultrasound: A collection of recollections, articles, interviews and images". www.obgyn.net. Retrieved 2006-05-11.
- ↑ "Doppler Ultrasound History". www.obgyn.net. Retrieved 2006-05-11.
External links
- American Institute of Ultrasound in Medicine Professional Association
- About the discovery of medical ultrasonography
- History of medical sonography (ultrasound)
- Procedures in Ultrasound (Sonography) for patients, from RadiologyInfo.org
- Manuals of medical ultrasound from University of Rochester Medical Center
- Ultrasound Safety Issues
- Ultrasound Can Affect Fetal Brain Development
- Sonography of the female pelvic floor:clinical indications and techniques Illustrate the clinical utility of this non-invasive diagnostic technique.
Template:Link FA ar:أشعة موجات فوق الصوتية de:Sonographie eo:Sonografio fa:سونوگرافی id:Ultrasonografi medis it:Ecografia he:בדיקת אולטרה סאונד nl:Echografie sv:Sonografi ta:மீயொலி வாருதல் uk:Ультразвукове дослідження ur:صوتی تخطیط