PCI complications: vessel perforation
|
Percutaneous coronary intervention Microchapters |
|
PCI Complications |
|---|
|
PCI in Specific Patients |
|
PCI in Specific Lesion Types |
|
PCI complications: vessel perforation On the Web |
|
American Roentgen Ray Society Images of PCI complications: vessel perforation |
|
Directions to Hospitals Treating Percutaneous coronary intervention |
|
Risk calculators and risk factors for PCI complications: vessel perforation |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor-In-Chief: Cafer Zorkun, M.D., Ph.D. [2]
Overview
Coronary perforations are uncommon (<1%) complications of percutaneous coronary intervention (PCI) and are associated with significant morbidity and mortality rates.[1][2][3][4][5] Coronary perforations are infrequent in patients undergoing balloon angioplasty (0.1%) compared with patients undergoing atheroablative therapy (1.3%; p<0.001).[6][7] Perforation due to coronary guidewires may present late after the procedure.
Classification
Coronary artery perforation has been classified by Ellis et al. based on its angiographic appearance:[8]
| Type | Definition |
|---|---|
| Type I | A crater extending outside of the lumen only and in the absence of linear staining angiographically suggestive of a dissection. |
| Type II | Pericardial or myocardial blush without a ≥1 mm exit hole. |
| Type III | Frank streaming of contrast through a ≥1 mm exit hole. |
| Cavity Spilling | Contrast flow from the site of perforation into an anatomic cavity (eg, cardiac chamber or coronary sinus) as opposed to into the pericardium or myocardium. |
Ellis Type II Perforation
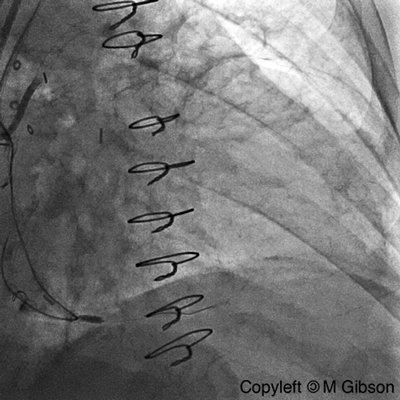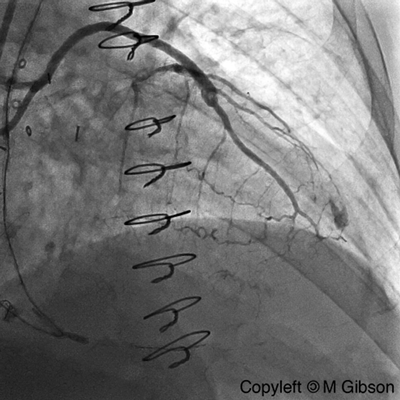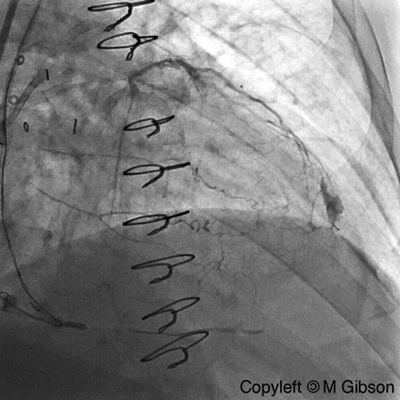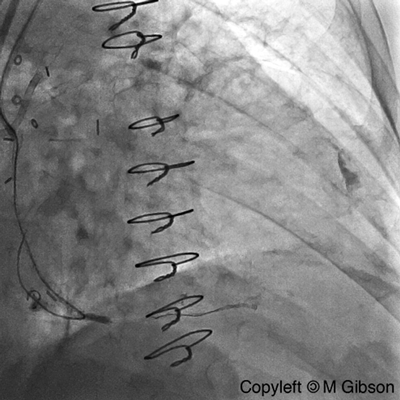 |
Ellis Type III Perforation
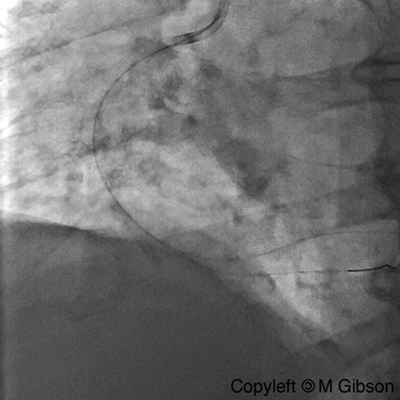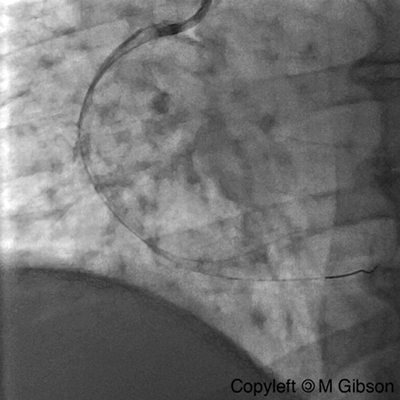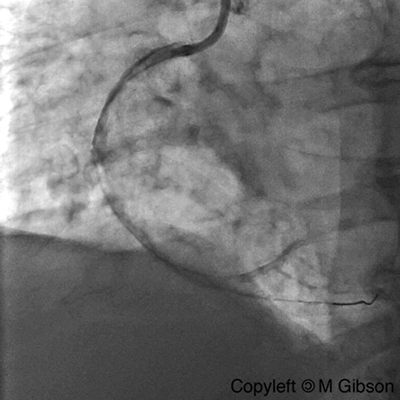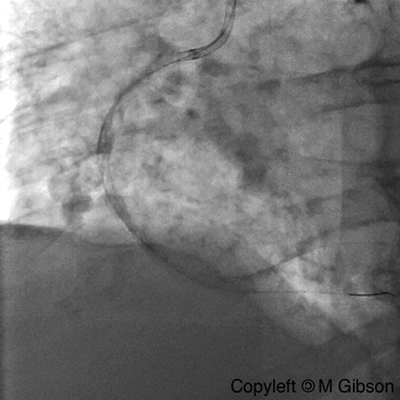 |
Risk Factors
PCI Equipment
- The use of stiff guidewires, hydrophilic guidewires and guidewires in which the core extends to the tip of the guidewire are associated with perforation.
PCI Technique
- Balloon to artery ratio > 1.1
- Over expansion of a stent at high pressures
- Use of debulking procedure such as rotational atherectomy
Lesion Risk Factors
Complex coronary anatomy including:
Natural History, Complications and Prognosis
Complications
Complications of vessel perforation include cardiac tamponade, myocardial infarction (MI) and death. It is important to maintain hemodynamic stability. Should tamponade occur, it is important to detect and treat it immediately.
Hemodynamic assessment with right heart pressure monitoring should be considered with particular attention being paid to a sudden rise in right atrial filling pressures. Also, it is important to monitor heart borders on fluoroscopy to detect signs of tamponade, as signified by a lack of movement of the heart borders.
Urgent echocardiography should be performed to evaluate for the presence of pericardial effusion and tamponade physiology. Immediate notification of the cardiothoracic surgical team is important so as to facilitate drainage of an effusion and urgent surgery to close the perforation if needed.
Prognosis
The prognosis based upon the Ellis Classification is as follows[8]:
- Type I - No deaths or myocardial infarction, tamponade incidence 8%
- Type II - No deaths, myocardial infarction incidence 14%, tamponade incidence 13%
- Type III - Mortality incidence 19%, cardiac tamponade incidence 63%, the need for urgent bypass surgery 63%
- Type III "cavity spilling" (CS) - No deaths, myocardial infarction or tamponade, but sample limited in size
Diagnosis
Perforation is an angiographic diagnosis. It appears as a small extraluminal extravasation of blush in the distribution of the target vessel. Care should be taken to routinely visualize the distal extent of the vessel following PCI to exclude the presence of a wire perforation. Emergency echocardiography should be performed to rule out the presence of a pericardial effusion or pericardial tamponade.
Treatment
Initial management strategies include:
Reversal of Anticoagulation
One is the initial steps is to reverse the anticoagulation. This includes the administration of protamine to reverse heparin. Protamine will also partially reverse the antithrombotic effect of enoxaparin if this antithrombin was used. Administration of platelets can be considered if abciximab has been administered. If it is greater than four hours after a maintenance dose of prasugrel or greater than six hours after a loading dose of prasugrel, then a platelet infusion should also be considered.
Prolonged Balloon Inflation
Inflations up to 20 minutes may be needed to achieve hemostasis. For this reason it is often wise for a cardiac catheterization laboratory to have perfusion balloons in a range of sizes available.
Covered Stent
In refractory cases, polytetrafluoroethylene covered stents (stent grafts) can be used to seal the perforation[9][10]. They can be used for most coronary perforations, but small, excessively angulated or tortuous vessels may not be amenable to them.
Other Techniques
Other techniques include coil embolization, the injection of clotted blood, the use of gel foam and the injection of thrombin at the site of the perforation. Coil embolization is suitable for small side branch perforations, but it will lead to tissue infarction and may not be available in all catheterization laboratories. Coil embolization is suited for small vessels, distal locations, arteries that supply limited viable myocardium, or situations where surgery is contraindicated.
Surgery
Approximately one third of cases of PCI-associated coronary artery perforation require emergent cardiac surgery. Surgical closure is necessary for perforations that demonstrate continued bleeding despite minimal invasive therapy, refractory ischemia, or recurrent hemorrhage. Incomplete closure is signified by persistent dye extravasation, while pericardial fluid collection and impending cardiac tamponade is signified by increasing right atrial pressure. Peristent fluid accumulation or pericardial drain output (>24 h) should prompt surgical repair.
Echocardiographic Monitoring
Serial echocardiography should be performed q 6-12h to detect the presence of an expanding pericardial effusion or cardiac tamponade physiology.
References
- ↑ Fasseas P, Orford JL, Panetta CJ, Bell MR, Denktas AE, Lennon RJ, Holmes DR, Berger PB. Incidence, correlates, management, and clinical outcome of coronary perforation: analysis of 16,298 procedures. Am Heart J. 2004 Jan; 147 (1):140-5. PMID 14691432
- ↑ Dippel EJ, Kereiakes DJ, Tramuta DA, Broderick TM, Shimshak TM, Roth EM, Hattemer CR, Runyon JP, Whang DD, Schneider JF, Abbottsmith CW. Coronary perforation during percutaneous coronary intervention in the era of abciximab platelet glycoprotein IIb/IIIa blockade: an algorithm for percutaneous management. Catheter Cardiovasc Interv. 2001 Mar; 52 (3):279-86. PMID 11246236
- ↑ Javaid A, Buch AN, Satler LF, Kent KM, Suddath WO, Lindsay J Jr, Pichard AD, Waksman R. Management and outcomes of coronary artery perforation during percutaneous coronary intervention. Am J Cardiol. 2006 Oct 1; 98 (7):911-4. Epub 2006 Aug 7. PMID 16996872
- ↑ Klein LW. Coronary artery perforation during interventional procedures. Catheter Cardiovasc Interv. 2006 Nov; 68 (5):713-7.PMID 17039517
- ↑ Stankovic G, Orlic D, Corvaja N, Airoldi F, Chieffo A, Spanos V, Montorfano M, Carlino M, Finci L, Sangiorgi G, Colombo A. Incidence, predictors, in-hospital, and late outcomes of coronary artery perforations. Am J Cardiol. 2004 Jan 15; 93 (2): 213-6. PMID 14715351
- ↑ Dippel EJ, Kereiakes DJ, Tramuta DA, Broderick TM, Shimshak TM, Roth EM, Hattemer CR, Runyon JP, Whang DD, Schneider JF, Abbottsmith CW. Coronary perforation during percutaneous coronary intervention in the era of abciximab platelet glycoprotein IIb/IIIa blockade: an algorithm for percutaneous management. Catheter Cardiovasc Interv. 2001 Mar; 52 (3):279-86. PMID 11246236
- ↑ Ellis SG, Ajluni S, Arnold AZ, Popma JJ, Bittl JA, Eigler NL, Cowley MJ, Raymond RE, Safian RD, Whitlow PL. Increased coronary perforation in the new device era. Incidence, classification, management, and outcome. Circulation. 1994 Dec; 90 (6): 2725-30. PMID 7994814
- ↑ 8.0 8.1 Ellis SG, Ajluni S, Arnold AZ, Popma JJ, Bittl JA, Eigler NL; et al. (1994). "Increased coronary perforation in the new device era. Incidence, classification, management, and outcome". Circulation. 90 (6): 2725–30. PMID 7994814.
- ↑ Ly H, Awaida JP, Lespérance J, Bilodeau L. Angiographic and clinical outcomes of polytetrafluoroethylene-covered stent use in significant coronary perforations. Am J Cardiol. 2005 Jan 15; 95 (2): 244-6. PMID 15642559
- ↑ Gercken U, Lansky AJ, Buellesfeld L, Desai K, Badereldin M, Mueller R, Selbach G, Leon MB, Grube E. Results of the Jostent coronary stent graft implantation in various clinical settings: procedural and follow-up results. Catheter Cardiovasc Interv. 2002 Jul; 56 (3): 353-60. PMID 12112888