Left main coronary artery
|
Coronary Angiography | |
|
General Principles | |
|---|---|
|
Anatomy & Projection Angles | |
|
Normal Anatomy | |
|
Anatomic Variants | |
|
Projection Angles | |
|
Epicardial Flow & Myocardial Perfusion | |
|
Epicardial Flow | |
|
Myocardial Perfusion | |
|
Lesion Complexity | |
|
ACC/AHA Lesion-Specific Classification of the Primary Target Stenosis | |
|
Lesion Morphology | |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1] Associate Editor(s)-in-Chief: Arzu Kalayci, M.D. [2]
Synonyms and keywords: LM, LMCA
Overview
The origin of the left main coronary artery (LMCA) is from the left sinus valsalva (LSV). Prior to entry into the coronary sulcus, it travels between the left auricle and the main pulmonary artery (PA). The left circumflex (LCX) and left anterior descending (LAD) arteries arise from the bifurcation of the LMCA, which does not have any significant branches. It is 1 to 25 mm long, and is normally 3 to 5 mm wide. Severe narrowing of the left main coronary artery can result in death due to coronary ischemia, and is an indication for coronary artery bypass grafting or coronary stenting.
Anatomy
Left main artery bifurcates into the left anterior descending artery and the left circumflex artery.
Shown below is an image depicting the left main artery.
<figure-inline><figure-inline><figure-inline>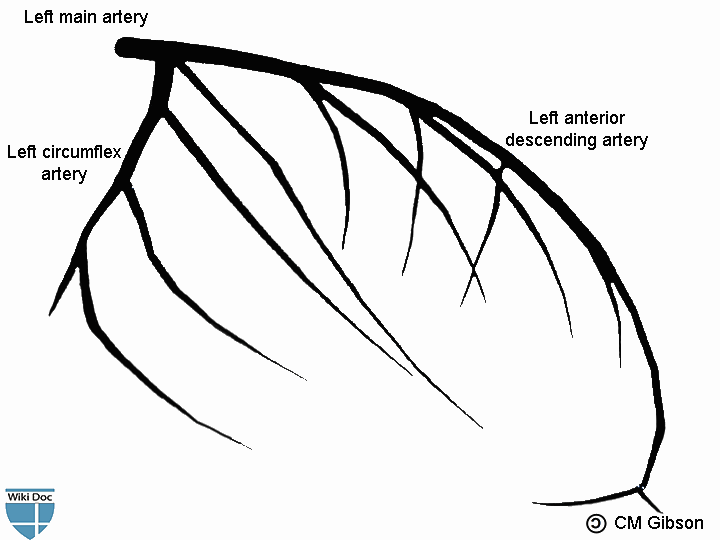 </figure-inline></figure-inline></figure-inline>
</figure-inline></figure-inline></figure-inline>
Congenital Anomalous of the Left Main Coronary Artery
LMCA from PA (anomalous origin of LCA from PA)
- Anomalous origin of LCA from PA (ALCAPA) is also known as Bland-White-Garland syndrome was described in 1956.
- ALCAPA is a very rare and a serious congenital coronary artery anomaly (0.008%).
- In this anomaly RCA is often dilated and provides an extensive collateral circulation to the LMCA territory.
- The specific findings are dilated collateral arteries and coronary veins in imaging.
- Additional components have been demonstrated in this syndrome as aortic coarctation and patent ductus arteriosus.[1]
- The suggested method of the treatment is reimplantation surgery of LMCA onto the aorta.[1][2][3]
Absence of LMCA (separate origin of LAD and LCX)
- This anomaly is characterized by the absence of LMCA. In this case, the LCX and LAD are normal in their distribution pattern but arise from adjacent, separate ostia in the LSV.
- Absent LMCA is a common benign anomaly, occurring in 0.41%-0.67% of cases.
- Cases of left system dominance and aortic valve disease have been found to have increased incidence.
- This condition is associated with no hemodynamic impairment. However, lack of identification of this anomaly may lead to clinical consequences during coronary catheterization or surgery.[3][4]
LMCA atresia
- There are often prominent right-to-left collateral vessels between the coronary arteries, although these vessels are usually inadequate to meet the oxygen requirements of left ventricle.
- A large conus collateral branch supplying the LAD may mimic a pre-pulmonic vessel.[2]
- Atresia of the LMCA is associated with formation of a fibrous connection between the left sinus valsalva and the LCX-LAD arterial junction.
- It usually affects patients in first year of life, but has also been described in elderly patients. [5]
- The lumen may not be identifiable or may be abnormal and nearly obliterated. Right-to-left collateral circulation may exist between coronary arteries to compensate for oxygen requirements, but may still be inadequate to meet the oxygen demand. A large conus collateral branch supplying the LAD may resemble a pre pulmonic vessel.[2]
Coronary Angiography
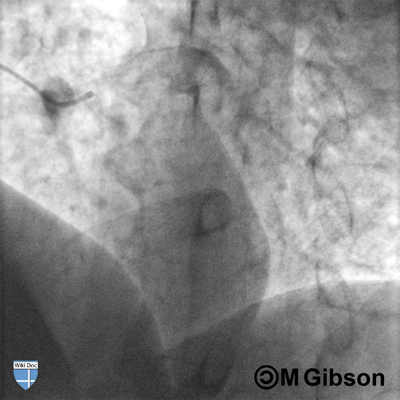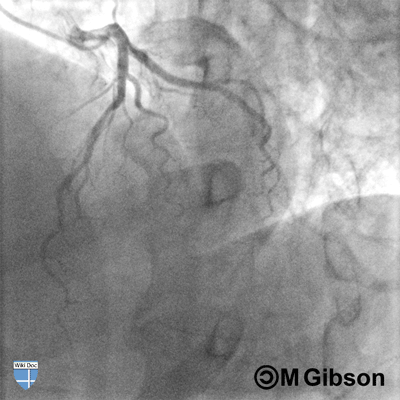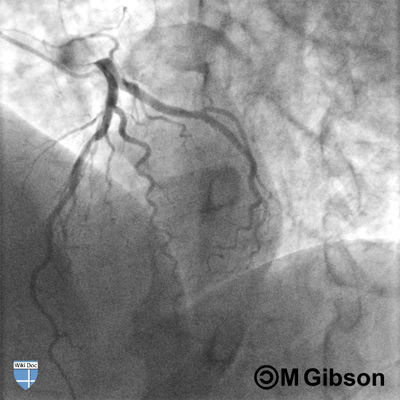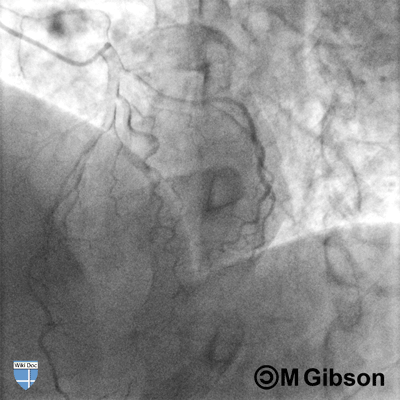
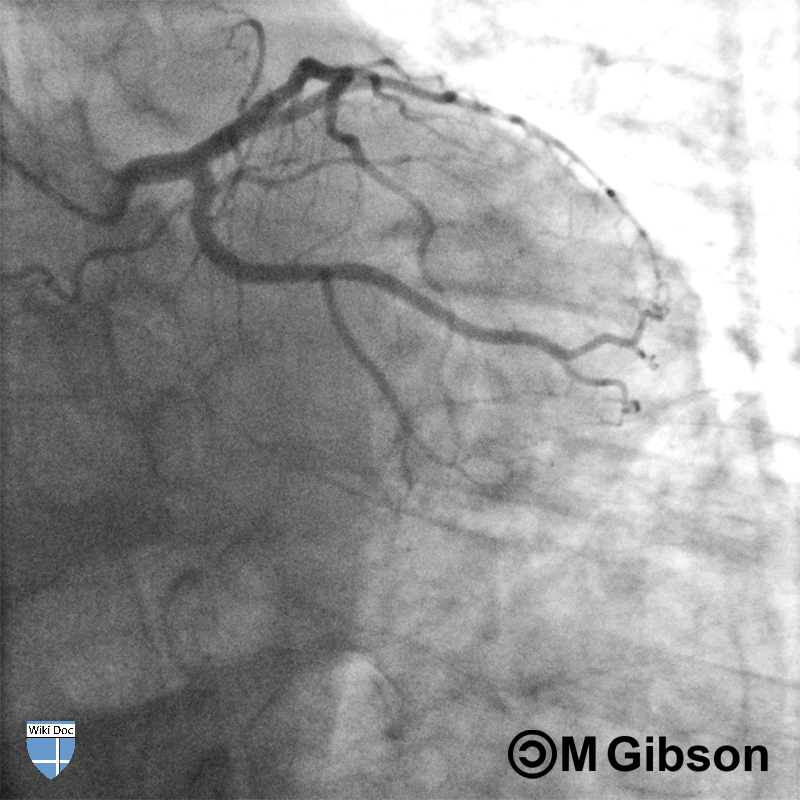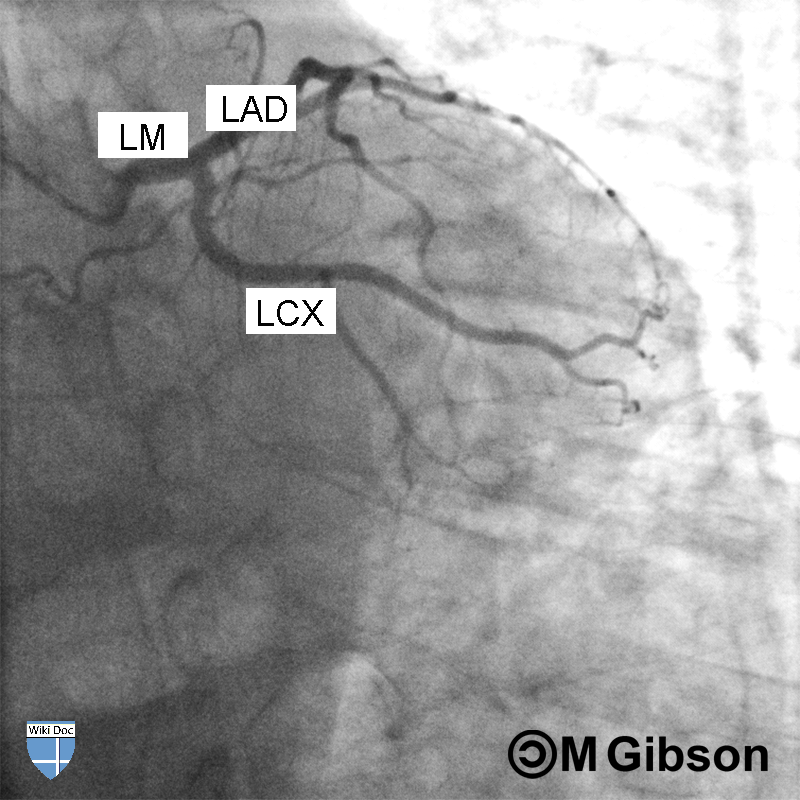
Shown below are an animated and a static angiography images depicting the left main artery in the RAO caudal view.
LAD= Left anterior descending artery; LCX= Left circumflex artery; LM= Left main artery.
Shown below are an animated and a static angiography images depicting the left main artery in the LAO cranial view.
LAD= Left anterior descending artery; LCX= Left circumflex artery; LM= Left main artery.
Shown below are an animated and a static angiography images depicting the left main artery in the LAO caudal view.
LAD= Left anterior descending artery; LCX= Left circumflex artery; LM= Left main artery.
Coronary Angiography
Shown below are an animated and a static angiography images depicting the left main artery in the RAO caudal view.
LAD= Left anterior descending artery; LCX= Left circumflex artery; LM= Left main artery.
Shown below are an animated and a static angiography images depicting the left main artery in the LAO cranial view.
LAD= Left anterior descending artery; LCX= Left circumflex artery; LM= Left main artery.
Shown below are an animated and a static angiography images depicting the left main artery in the LAO caudal view.
LAD= Left anterior descending artery; LCX= Left circumflex artery; LM= Left main artery.
PCI in the Left Main Patient
In carefully selected patients, percutaneous left main intervention can safely and effectively treat patients in whom coronary artery bypass graft surgery is a suboptimal option. Data from the SYNTAX trial supports such an approach.
Patient Selection
- Careful selection of patients for PCI is critical.
- Fractional Flow Reserve (FFR) may be helpful in determining if a lesion is critical.
- Mortality and procedural results vary depending upon whether the lesion is ostial and/or in the shaft versus distal and involves the bifurcation.
- Thus, careful and meticulous angiography in multiple views is critical to fully assess the left main at it's ostium and bifurcation. Optimal views include but are not limited to the AP caudal and the LAO Caudal.
- Coronary Artery Bypass Grafting (CABG) is currently the standard of care for patients with left main disease. However, this recommendation may be modified as data emerge regarding:
- Very low in-hospital mortality among patients treated with left main stenting
- Comparable or better MACE-free survival rates vs CABG in some registries
- Low restenosis rate with drug eluting stent use
Appropriate Candidate for Left Main PCI
- Nonoperative candidates
- Low-risk patients who decline CABG
- A patient who is both able and willing to take life long aspirin and clopidogrel (dual antiplatelet therapy)
High Risk Candidate for Left Main PCI
- High-risk features in patients undergoing left main disease PCI include:
- Absence of saphenous vein or internal mammary artery grafts distally
- Concomitant RCA disease
- Lack of collaterals from RCA
- Distal bifurcation involvement
- LV dysfunction
- Presence of clot
- Extensive calcification
Technique
Pre-interventional Preparation
- The anatomy should be well characterized before the PCI.
- Evaluation of the potential to occlude or 'snowplow' a ramus is critical.
Hemodynamic Monitoring and Support
- Hemodynamic support with intra aortic balloon pump (IABP) placement is not mandatory, but should be considered for high-risk patients.
- If an Intra aortic balloon pump is not placed, consideration should be given to placement of a 4 or 5 French sheath in the contralateral groin in case one needs to be placed urgently.
- Percutaneous cardiopulmonary support (CPS) is an option for very-high-risk patient.
- Pulmonary artery line monitoring may be helpful.
IVUS Use
- Characterizes extent of plaque
- Characterizes extent of calcification
- Can be used to calculate the MLD/MLA (minimal lumen diameter/area) accurately and ascertain the significance of stenosis
- QCA alone may not be adequate to determine the physiologic significance of an often eccentric LM stenosis
- IVUS may assist in sizing the stent appropriately to avoid stent malaposition and consequent higher risk of stent thrombosis and restenosis
- In the presence of bifurcation disease you can use IVUS to determine the degree of plaque extent in the circumflex and use Murray's Law to calculate the stent size (diameter of the proximal main branch (diameter of distal main branch + diameter of distal side branch) X 0.67
Guiding Catheter Selection
- Use of larger guiding catheters (i.e.: 7 or 8 French) in case distal bifurcation intervention is necessary.
- Select a guide that provides good support, but which can be backed out of the ostium if you are dealing with an ostial stenosis.
- Do not occlude ostium with the guide.
- Make side holes with an 18 gauge needle if necessary.
Balloon Technique
- Short occlusion/inflation times are critical to reduce ischemic time.
- Consideration should be given to a perfusion balloon in a very high risk patient and the distal tip should be placed in the LAD.
- Select equipment in advance.
- Use a rapid exchange system.
- Dilute contrast in the indeflator to allow faster deflation.
Stent Technique
- Adequate stent sizing and post-dilation cannot be understated.
- Stent selection:
- Consider using a drug eluting stent especially if the vessel is less than 4.5 mm
- Good radial strength (larger Taxus stents tend to recoil)
- High visibility for ostial or bifurcation placement
- Assure that aorto-ostial region covered by stent if there is ostial lesion (stent positioning in two orthogonal views is particularly important)
New Device Approaches to High Risk Lesion Morphologies
- Calcified lesions:
- Bulky plaque:
- Directional atherectomy + stenting
- Stenting alone
- Distal bifurcation involvement:
- Similar to other bifurcation therapies but higher risk
- DCA alone
- DCA + stenting of principal vessel
- Stenting of principal vessel (usually LAD) & rescuing circumflex
- Bifurcation stenting (V stenting with kissing balloons, crush or reverse crush, T stenting, or Y, Culotte; in double barrel V or crush stenting LCX limb is often the site of restenosis and re-crossing into the barrel is often challenging )
Pharmacotherapy
- Antiplatelet regimen:
- ASA 325 mg PO prior to the procedure, use non-enteric coated to assure rapid absorption
- Clopidogrel at a loading dose of 600 mg at least 2 hours prior to the intervention
- Glycoprotein IIb/IIIa inhibitor administration is typical for this high risk lesion morphology
- If unfractionated heparin (UFH) is used as an antithrombin, then UFH should be dosed to achieve an activated clotting time (ACT) of 250 seconds in the presence of a Glycoprotein IIb/IIIa inhibitor or 300 seconds in the absence of a Glycoprotein IIb/IIIa inhibitor
Sheath Removal
- A bad vagal reaction in a freshly implanted stent or in a patient awaiting PCI who has a significant LM lesion can be very hazardous (risk of thrombosis, or a downward spiral of poor perfusion leading to subendocardial ischemia leading to poorer LV function, leading to poorer forward output).
- Some operators will preemptively administer an ampule of atropine prior to the sheath pull or will have a low threshold to administer a full ampule of atropine.
Stenting versus Bypass Surgery for Left Main Coronary Artery Stenosis
- In patients with LMCA disease, CABG is known to have high efficacy and safety.
- In patients who were not candidates for CABG, performing PCI with stenting to the left main coronary artery was adopted.
- Evidence from literature has shown that these two techniques of revascularization have equivalent outcomes in patients with LMCA disease.
- The complexity of coronary artery disease can be evaluated by using the SYNTAX score or by determining the number of vessels requiring revascularization.
- With increasing complexity of coronary artery disease (CAD), CABG is preferred over PCI with stenting.
- CABG has been found to have a higher incidence of adverse in-hospital outcomes, including stroke, MI and death.
- PCI with stenting has a higher incidence of repeat (usually target vessel) revascularization at long-term follow up. (OR 1.85, 95% CI 1.53-2.23). There is no significant difference in the long term rates of stroke, MI and death.
- Outcomes may be better in CABG depending on CAD severity and follow-up duration.
Data Regarding The Efficacy and Safety of Left Main Stenting with Drug Eluting Stents
- A retrospective multicenter registry study has demonstrated favorable long-term outcomes after the implantation of drug eluting stents (DES) in non-bifurcation lesions involving unprotected left main coronary arteries[6].
- The study, which was published in the online edition of Circulation, examined registry data among 147 patients who were electively treated with percutaneous coronary intervention (PCI) with DES in unprotected left main coronary artery lesions.
- At a median follow-up of 886 days, the major adverse cardiac event rate was 7.4% with a cumulative cardiac mortality of 2.7%. Only seven patients required target vessel revascularization.
- The restenosis rate at six-month angiographic follow-up was 0.9% with a late loss of -0.01 mm.
- Additionally, there were no angiographically proven cases of stent thrombosis, although stent thrombosis could not be excluded in the four patients who died of unknown causes.
- While the results of the study suggest that the use of drug eluting stents in nonbifurcation unprotected left main coronary artery stenosis is both safe and effective, Dr. Alaide Chieffo and colleagues note that the results are from a retrospective registry with a relatively small number of patients due to the low occurrence of this anatomical subset.
- Currently there is no randomized data comparing PCI with DES implantation versus coronary artery bypass graft surgery. The ongoing SYNTAX trial will evaluate 710 patients with left main disease who have been randomized to either a DES or CABG.
- Unprotected left main stem PCI with drug eluting stents is associated with favorable long-term outcomes.
- Among patients with significant left main stem stenosis, coronary artery bypass surgery is still the favored method of revascularization.
- However, previous observational studies suggest favorable outcomes with percutaneous intervention using drug eluting stents (DES). But the use of DES however is associated with an increase in late stent thrombosis.
- Meliga and colleagues determine the long term (3 years) clinical outcomes with left main PCI using DES.
- Their study is an international, multicenter, retrospective registry design consisting of real world population recruited between April 2002 and April 2004 from Europe and United States.
- 358 patients underwent PCI with sirolimus eluting and paclitaxel eluting stents for de novo lesions located in the ostium, shaft and distal segments of the unprotected left main stem.
- Patients with EuroSCORE >6 were considered high risk and >9 were considered very high risk.
- The mean age of study patients was 66.1±11.2 and 30.2% of patients had diabetes mellitus (IDDM 16.2%, NIDDM 14%), 18.9% had prior coronary artery bypass surgery, the mean left ventricular ejection fraction was 48.6±12.8% and the mean EuroSCORE was 6.4±4.1.
- The most common admission diagnosis was stable angina (44.1%), unstable angina (41.9%), acute myocardial infarction (8.4%), cardiogenic shock (2.8%) and silent ischemia (2.8%).
- 19.6% of cases underwent emergent PCI.
- The lesion was located in the ostium/shaft in 26.3% of cases and the remaining lesions were located in the distal segment of the left main stem.
- Multiple stents were used in 43.3% of cases. Cypher and Taxus stents were used in almost equal proportions (54.5% and 45.5%).
- Provisional stenting was adopted in majority of the cases (56.7%) and crush stenting was used in 26.5% of cases. Intra-aortic balloon pump was used in 13.9% of cases.
- Technical procedural success was achieved in all patients (100%).
- The overall in-hospital major adverse cardiac event (MACE-cardiac death, nonfatal myocardial infarction, or target vessel revascularization) rate was 11.1%, which occurred more frequently following emergency PCI than elective PCI (22.8% vs. 8.3%, p<0.001).
- Likewise the in-hospital cardiac death was more frequent in the emergency cases (12.8% vs. 0.7%, p<0.001).
- At one year, the overall MACE rate was 24.3% (elective: 22.2% vs. emergency: 32.9%, p=0.046).
- The difference in MACE at one year between elective and emergent cases was attributed to an increase in cardiac death in the emergency group (18.6% vs. 3.8%, p<0.001).
- At 3 years, the overall MACE rate was 32.1%, with no difference in MACE between elective and emergency cases (p=0.126).
- However, at 3 years, the elective group underwent more target vessel revascularization compared with the emergency group (16% vs. 7.1%, p=0.037).
- Beyond 3 years, the overall incidence of cardiac death was 10.6% (elective: 6.9% vs. emergency 25.7%, p<0.001) and the overall MACE rate was 34.9% (elective: 31.6% vs. emergency: 48.5%, p=0.006).
- In total, stent thrombosis according to the ARC definition occurred in 6.1% of cases (acute 0.6%, subacute 0.6%, late 2.2% and very late stent thrombosis in 10 cases).
- In a multivariate analysis, age [HR 1.06 (95% CI 1.01 to 1.11, p=0.010)], shock [HR 11.0 (1.88 to 63.9), p=0.008], and EuroSCORE [HR 1.15 (1.01 to 1.31), p=0.046] were identified as independent predictors of cardiac death. The IDDM [HR 2.85 (1.29 to 6.17), p=0.009] and EuroSCORE [HR 1.10 (1.02 to 1.19), p=0.014] were predictors of MACE whereas, impaired ejection fraction [HR 1.03 (1.01 to 1.05), p=0.050], IDDM [HR 2.92 (1.60 to 5.30), p<0.001] and multiple stenting [HR 4.51 (1.07 to 19.0), p=0.040] were independent predictors of the need for target vessel revascularization.
- The investigators concluded that PCI to unprotected left main stem using DES is associated with “a satisfactory rate in both single and composite outcomes”.
- Beneficial effects were more frequently observed in elective population compared with the emergency cases over a 3 year period with lower rates of stent thrombosis.[7]
Follow-up of the Patient with a DES in the Left Main
- Left main restenosis may present as sudden death rather than recurrent angina.
- Screen aggressively for restenosis (with either angiography or Multi Detector CT for ostial disease).
- Some operators perform platelet inhibition testing to confirm that the patient is not a clopidogrel non-responder.
- Some operators dose the patient with 150 mg of clopidogrel per day in case the patient is a clopidogrel non-responder.
- Relook angiography recommended even in absence of sx at 2-3 months post-procedure to catch early restenosis and some operators recommend additional angiography at 6 months to identify late restenosis
- Angioscopy may aid in determining if clot is present at the end of the procedure, and if clot is present on repeat evaluation.
ACC/AATS/AHA/ASE/ASNC/SCAI/SCCT/ STS 2017 Appropriate Use Criteria for Coronary Revascularization in Patients With Stable Ischemic Heart Disease[8]
Left Main Coronary Artery Stenosis
| Appropriate Use Score (1-9) | ||||||||
|---|---|---|---|---|---|---|---|---|
| Left Main Disease | Asymptomatic | Ischemic Symptoms | ||||||
| Left Main Disease | Not on AA Therapy or With AA Therapy | Not on AA Therapy | On 1 AA Drug (BB Preferred) | On ≥2 AA Drugs | ||||
| Indication | PCI | CABG | PCI | CABG | PCI | CABG | PCI | CABG |
| Isolated LMCA disease - Ostial or midshaft stenosis | M (6) | A (8) | A (7) | A (8) | A (7) | A (9) | A (7) | A (9) |
| Isolated LMCA disease - Bifurcation involvement | M (5) | A (8) | M (5) | A (8) | M (5) | A (9) | M (6) | A (9) |
| LMCA disease - Ostial or mid shaft stenosis - Concurrent multi vessel disease - Low disease burden (e.g., 1–2 additional focal stenoses, SYNTAX score ≤22) | M (6) | A (8) | M (6) | A (9) | A (7) | A (9) | A (7) | A (9) |
| Ostial or mid shaft stenosis - Concurrent multi vessel disease - Intermediate or high disease burden (e.g., 1–2 additional bifurcation stenosis, long stenoses, SYNTAX score >22) | M (4) | A (9) | M (4) | A (9) | M (4) | A (9) | M (4) | A (9) |
| Ostial or mid shaft stenosis - Concurrent multi vessel disease - Intermediate or high disease burden (e.g., 1–2 additional bifurcation stenosis, long stenoses, SYNTAX score >22) | M (4) | A (9) | M (4) | A (9) | M (4) | A (9) | M (4) | A (9) |
| LMCA disease - Bifurcation involvement - Low disease burden in other vessels (e.g., 1–2 additional focal stenosis, SYNTAX score ≤22) | M (4) | A (8) | M (5) | A (8) | M (5) | A (9) | M (6) | A (9) |
| LMCA disease - Bifurcation involvement - Intermediate or high disease burden in other vessels (e.g., 1–2 additional bifurcation stenosis, long stenoses, SYNTAX score >22) | R (3) | A (8) | R (3) | A (9) | R (3) | A (9) | R (3) | A (9) |
| A indicates appropriate; AA, antianginal; BB, beta blockers; CABG, coronary artery bypass graft; LMCA, left main coronary artery; M, may be appropriate; PCI, percutaneous coronary intervention; R, rarely appropriate; and SYNTAX, Synergy between PCI with Taxus and Cardiac Surgery trial. A separate, independent rating panel scored the clinical scenarios on a scale of 1 to 9. Scores of 7 to 9 indicate that revascularization is considered appropriate for the clinical scenario presented. Scores of 1 to 3 indicate that revascularization is considered rarely appropriate for the clinical scenario, whereas scores in the mid-range of 4 to 6 indicate that coronary revascularization may be appropriate for the clinical scenario. | ||||||||
References
- ↑ 1.0 1.1 ALEXANDER RW, GRIFFITH GC (1956). "Anomalies of the coronary arteries and their clinical significance". Circulation. 14 (5): 800–5. PMID 13374855.
- ↑ 2.0 2.1 2.2 Shriki JE, Shinbane JS, Rashid MA, Hindoyan A, Withey JG, DeFrance A; et al. (2012). "Identifying, characterizing, and classifying congenital anomalies of the coronary arteries". Radiographics. 32 (2): 453–68. doi:10.1148/rg.322115097. PMID 22411942.
- ↑ 3.0 3.1 Yamanaka O, Hobbs RE (1990). "Coronary artery anomalies in 126,595 patients undergoing coronary arteriography". Cathet Cardiovasc Diagn. 21 (1): 28–40. PMID 2208265.
- ↑ Roberts WC (1986). "Major anomalies of coronary arterial origin seen in adulthood". Am Heart J. 111 (5): 941–63. PMID 3518378.
- ↑ Musiani A, Cernigliaro C, Sansa M, Maselli D, De Gasperis C (1997). "Left main coronary artery atresia: literature review and therapeutical considerations". Eur J Cardiothorac Surg. 11 (3): 505–14. PMID 9105816.
- ↑ Chieffo A, Park SJ, Valgimigli M, Kim YH, Daemen J, Sheiban I et al. (2007) Favorable long-term outcome after drug-eluting stent implantation in nonbifurcation lesions that involve unprotected left main coronary artery: a multicenter registry. Circulation 116 (2):158-62. DOI:10.1161/CIRCULATIONAHA.107.692178 PMID: 17576862
- ↑ Meliga E, Garcia-Garcia HM, Valgimigli M, Chieffo A, Biondi-Zoccai G, Maree AO; et al. (2008). "Longest available clinical outcomes after drug-eluting stent implantation for unprotected left main coronary artery disease: the DELFT (Drug Eluting stent for LeFT main) Registry". J Am Coll Cardiol. 51 (23): 2212–9. doi:10.1016/j.jacc.2008.03.020. PMID 18534266.
- ↑ Abu Daya H, Hage FG (2017). "Guidelines in review: ACC/AATS/AHA/ASE/ASNC/SCAI/SCCT/STS 2017 appropriate use criteria for coronary revascularization in patients with stable ischemic heart disease". J Nucl Cardiol. 24 (5): 1793–1799. doi:10.1007/s12350-017-1017-6. PMID 28836156.