Anaplastic large cell lymphoma pathophysiology: Difference between revisions
No edit summary |
No edit summary |
||
| Line 3: | Line 3: | ||
{{CMG}};{{AE}}{{SM}}{{AS}} | {{CMG}};{{AE}}{{SM}}{{AS}} | ||
==Overview== | ==Overview== | ||
On microscopic histopathological analysis, medium sized cells, abundant cytoplasm, kidney shaped nuclei, and paranuclear eosinophilic region are characteristic findings of anaplastic large cell lymphoma. | |||
==Genetics== | ==Genetics== | ||
ALK negative anaplastic large cell lymphoma is characterized by a translocation T(6;7)(p25.3;q32.3), which inactivates the DUSP22 gene and leads to a higher proliferation rate.<ref name="pmid21030553">{{cite journal| author=Feldman AL, Dogan A, Smith DI, Law ME, Ansell SM, Johnson SH et al.| title=Discovery of recurrent t(6;7)(p25.3;q32.3) translocations in ALK-negative anaplastic large cell lymphomas by massively parallel genomic sequencing. | journal=Blood | year= 2011 | volume= 117 | issue= 3 | pages= 915-9 | pmid=21030553 | doi=10.1182/blood-2010-08-303305 | pmc=PMC3035081 | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=21030553 }} </ref> In healthy people, the product of the DUSP22 gene, the DUSP22 protein (also known as the <i>JNK pathway-associated phosphatase</i> or <i>JKAP</i>), inactivates the LCK tyrosine kinase protein during T-cell receptor signaling.<ref>{{cite web|url=http://www.nature.com/ncomms/2014/140409/ncomms4618/full/ncomms4618.html|title=The phosphatase JKAP/DUSP22 inhibits T-cell receptor signalling and autoimmunity by inactivating Lck}}</ref> | ALK negative anaplastic large cell lymphoma is characterized by a translocation T(6;7)(p25.3;q32.3), which inactivates the ''DUSP22 ''gene and leads to a higher proliferation rate.<ref name="pmid21030553">{{cite journal| author=Feldman AL, Dogan A, Smith DI, Law ME, Ansell SM, Johnson SH et al.| title=Discovery of recurrent t(6;7)(p25.3;q32.3) translocations in ALK-negative anaplastic large cell lymphomas by massively parallel genomic sequencing. | journal=Blood | year= 2011 | volume= 117 | issue= 3 | pages= 915-9 | pmid=21030553 | doi=10.1182/blood-2010-08-303305 | pmc=PMC3035081 | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=21030553 }} </ref> In healthy people, the product of the ''DUSP22'' gene, the DUSP22 protein (also known as the <i>JNK pathway-associated phosphatase</i> or <i>JKAP</i>), inactivates the LCK [[tyrosine kinase]] protein during T-cell receptor signaling.<ref>{{cite web|url=http://www.nature.com/ncomms/2014/140409/ncomms4618/full/ncomms4618.html|title=The phosphatase JKAP/DUSP22 inhibits T-cell receptor signalling and autoimmunity by inactivating Lck}}</ref> | ||
DUSP22 mutations are also associated with breast cancer (the UDSMP22 protein can also block [[estrogen receptors]]).<ref>{{cite web|url=http://www.bloodjournal.org/content/117/3/915?sso-checked=true|title=Discovery of recurrent t(6;7)(p25.3;q32.3) translocations in ALK-negative anaplastic large cell lymphomas by massively parallel genomic sequencing}}</ref> and primary cutaneous | DUSP22 mutations are also associated with breast cancer (the UDSMP22 protein can also block [[estrogen receptors]]).<ref>{{cite web|url=http://www.bloodjournal.org/content/117/3/915?sso-checked=true|title=Discovery of recurrent t(6;7)(p25.3;q32.3) translocations in ALK-negative anaplastic large cell lymphomas by massively parallel genomic sequencing}}</ref> and primary cutaneous anaplastic large cell lymphoma.<ref name="pmid25461779">{{cite journal| author=Xing X, Feldman AL| title=Anaplastic large cell lymphomas: ALK positive, ALK negative, and primary cutaneous. | journal=Adv Anat Pathol | year= 2015 | volume= 22 | issue= 1 | pages= 29-49 | pmid=25461779 | doi=10.1097/PAP.0000000000000047 | pmc= | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=25461779}} </ref> | ||
=== Molecular biology === | ===Molecular biology=== | ||
The majority of cases, greater than 90%, contain a clonal rearrangement of the [[T-cell receptor]]. This may be identified using [[PCR]] techniques, such as T-gamma multiplex PCR. Oncogeneic potential is conferred by | The majority of anaplastic large cell lymphoma cases, greater than 90%, contain a clonal rearrangement of the [[T-cell receptor]]. This may be identified using [[PCR]] techniques, such as T-gamma multiplex PCR. Oncogeneic potential is conferred by up regulation of a [[tyrosine kinase]] gene on [[chromosome]] 2. Several different translocations involving this gene have been identified in different cases of this lymphoma. The most common is a [[chromosomal translocation]] involving the nucleophosmin gene on chromosome 5. The translocation may be identified by analysis of giemsa-banded metaphase spreads of tumor cells and is characterised by t(2;5)(p23;q35). The product of this [[Gene fusion|fusion]] [[gene]] may be identified by [[immunohistochemistry]] using antiserum to [[Anaplastic_lymphoma_kinase|ALK protein]]. Probes are available to identify the translocation by fluorescent in situ hybridization ([[FISH]]). The nucleophosmin component associated with the common translocation results in nuclear positivity as well as cytoplasmic positivity. Positivity with the other translocations may be confined to the cytoplasm. Mutagenesis and functional studies have identified a plethora of [[NPM1]]–[[Anaplastic_lymphoma_kinase|ALK]] interacting molecules which ultimately lead to the activation of key pathways including [[Extracellular signal-regulated kinases|Erk]], PLC-γ, [[PI3K]], and [[Janus kinase|Jak]]/signal transducers and activators of [[transcription]] (STAT) path- ways, which in turn control cell proliferation and survival and cytoskeletal rearrangements.<ref name="pmid22649787">{{cite journal |author=Tabbó F, Barreca A, Piva R, Inghirami G; European T-Cell Lymphoma Study Group |title=ALK Signaling and Target Therapy in Anaplastic Large Cell Lymphoma |journal=Front Oncol |volume=2 |pages=41 |year=2012 |pmid=22649787 |doi= 10.3389/fonc.2012.00041|url=http://www.frontiersin.org/Cancer_Molecular_Targets_and_Therapeutics/10.3389/fonc.2012.00041/abstract |pmc=3355932}}</ref> | ||
Other gene mutations include:<ref>{{cite web|url=http://www.nature.com/nrc/journal/v8/n1/abs/nrc2291.html|title=The anaplastic lymphoma kinase in the pathogenesis of cancer}}</ref> | Other gene mutations include:<ref>{{cite web|url=http://www.nature.com/nrc/journal/v8/n1/abs/nrc2291.html|title=The anaplastic lymphoma kinase in the pathogenesis of cancer}}</ref> | ||
* T(1;2), encoding a tropomyosin3 (TPM3)/ALK fusion protein (10 to 20%) | * T(1;2), encoding a tropomyosin3 (TPM3)/ALK fusion protein (10 to 20%) | ||
| Line 23: | Line 19: | ||
* T(2;22), encoding a non-muscle myosin (MYH9)/ALK fusion protein (<1%) | * T(2;22), encoding a non-muscle myosin (MYH9)/ALK fusion protein (<1%) | ||
===Immunophenotype=== | ===Immunophenotype=== | ||
* The hallmark cells (and variants) show immunopositivity for [[CD30]] (also known as Ki-1) | * The hallmark cells (and variants) of anaplastic large cell lymphoma show immunopositivity for [[CD30]] (also known as Ki-1) | ||
* Nuclear negativity for the [[PAX5]] transcription factor (usually expressed in [[Hodgkin’s lymphoma]] classic variant) | * Nuclear negativity for the [[PAX5]] transcription factor (usually expressed in [[Hodgkin’s lymphoma]] classic variant) | ||
* Negativity for the [[EBV]] markers EBER and LMP1 (which may be expressed in [[Hodgkin’s lymphoma]] classic variant) | * Negativity for the [[EBV]] markers EBER and LMP1 (which may be expressed in [[Hodgkin’s lymphoma]] classic variant) | ||
* Presence of clonal [[T-cell receptor]] rearrangements (usually absent in [[Hodgkin’s lymphoma]] classic variant) | * Presence of clonal [[T-cell receptor]] rearrangements (usually absent in [[Hodgkin’s lymphoma]] classic variant) | ||
Revision as of 18:29, 19 October 2015
|
Anaplastic large cell lymphoma Microchapters |
|
Differentiating Anaplastic large cell lymphoma from other Diseases |
|---|
|
Diagnosis |
|
Treatment |
|
Case Studies |
|
Anaplastic large cell lymphoma pathophysiology On the Web |
|
American Roentgen Ray Society Images of Anaplastic large cell lymphoma pathophysiology |
|
Directions to Hospitals Treating Anaplastic large cell lymphoma |
|
Risk calculators and risk factors for Anaplastic large cell lymphoma pathophysiology |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1];Associate Editor(s)-in-Chief: Shivali Marketkar, M.B.B.S. [2]Sowminya Arikapudi, M.B,B.S. [3]
Overview
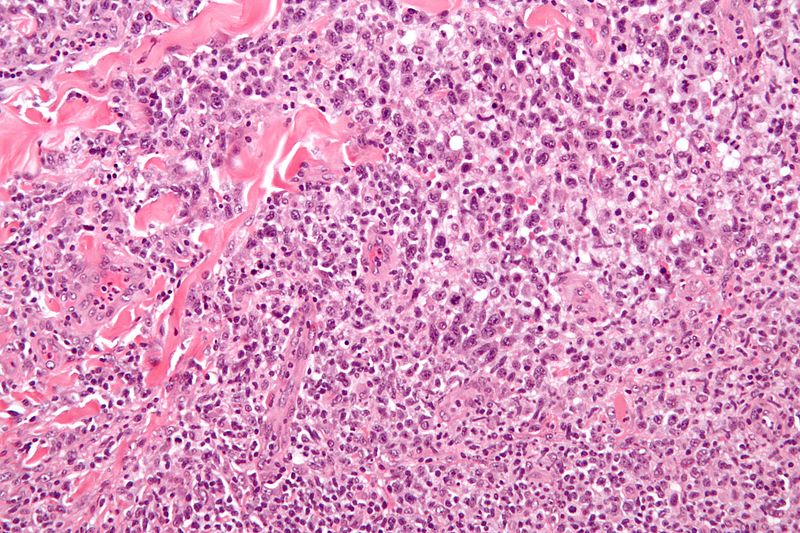
On microscopic histopathological analysis, medium sized cells, abundant cytoplasm, kidney shaped nuclei, and paranuclear eosinophilic region are characteristic findings of anaplastic large cell lymphoma.
Genetics
ALK negative anaplastic large cell lymphoma is characterized by a translocation T(6;7)(p25.3;q32.3), which inactivates the DUSP22 gene and leads to a higher proliferation rate.[1] In healthy people, the product of the DUSP22 gene, the DUSP22 protein (also known as the JNK pathway-associated phosphatase or JKAP), inactivates the LCK tyrosine kinase protein during T-cell receptor signaling.[2] DUSP22 mutations are also associated with breast cancer (the UDSMP22 protein can also block estrogen receptors).[3] and primary cutaneous anaplastic large cell lymphoma.[4]
Molecular biology
The majority of anaplastic large cell lymphoma cases, greater than 90%, contain a clonal rearrangement of the T-cell receptor. This may be identified using PCR techniques, such as T-gamma multiplex PCR. Oncogeneic potential is conferred by up regulation of a tyrosine kinase gene on chromosome 2. Several different translocations involving this gene have been identified in different cases of this lymphoma. The most common is a chromosomal translocation involving the nucleophosmin gene on chromosome 5. The translocation may be identified by analysis of giemsa-banded metaphase spreads of tumor cells and is characterised by t(2;5)(p23;q35). The product of this fusion gene may be identified by immunohistochemistry using antiserum to ALK protein. Probes are available to identify the translocation by fluorescent in situ hybridization (FISH). The nucleophosmin component associated with the common translocation results in nuclear positivity as well as cytoplasmic positivity. Positivity with the other translocations may be confined to the cytoplasm. Mutagenesis and functional studies have identified a plethora of NPM1–ALK interacting molecules which ultimately lead to the activation of key pathways including Erk, PLC-γ, PI3K, and Jak/signal transducers and activators of transcription (STAT) path- ways, which in turn control cell proliferation and survival and cytoskeletal rearrangements.[5] Other gene mutations include:[6]
- T(1;2), encoding a tropomyosin3 (TPM3)/ALK fusion protein (10 to 20%)
- T(2;3), encoding a TRK fusion gene (TFP)/ALK fusion protein (2 to 5%)
- Inv(2), encoding a ATIC (Pur H gene)/ALK fusion protein (2 to 5%)
- T(2;17), encoding a clathrin heavy (CLTC)/ALK fusion protein (2 to 5%)
- T(2;17), encoding a ALO17/ALK fusion protein (2 to 5 percent of cases)
- T(2;19), encoding a tropomyosin 4 (TPM4)/ALK fusion protein (<1%)
- T(2;22), encoding a non-muscle myosin (MYH9)/ALK fusion protein (<1%)
Immunophenotype
- The hallmark cells (and variants) of anaplastic large cell lymphoma show immunopositivity for CD30 (also known as Ki-1)
- Nuclear negativity for the PAX5 transcription factor (usually expressed in Hodgkin’s lymphoma classic variant)
- Negativity for the EBV markers EBER and LMP1 (which may be expressed in Hodgkin’s lymphoma classic variant)
- Presence of clonal T-cell receptor rearrangements (usually absent in Hodgkin’s lymphoma classic variant)
- Another useful marker which helps to differentiate this lesion from Hodgkin lymphoma is Clusterin
- The neoplastic cells have a golgi staining pattern (hence paranuclear staining), which is characteristic of this lymphoma
- The cells are also typically positive for a subset of markers of T-cell lineage
- However, as with other T-cell lymphomas, they are usually negative for the pan T-cell marker CD3
- Occasional examples are of null (neither T nor B) cell type
- These lymphomas show immunopositivity for ALK protein in 70% of cases
- They are also typically positive for EMA
Microscopic Pathology
The histologic features of anaplastic large cell lymphoma are variable. The hallmark cells are of medium size and feature abundant cytoplasm (which may be clear, amphophilic or eosinophilic), kidney shaped nuclei, and a paranuclear eosinophilic region. Occasional cells may be identified in which the plane of section passes through the nucleus in such a way that it appears to enclose a region of cytoplasm within a ring; such cells are called "doughnut" cells.
| Name | Description | ||||
|---|---|---|---|---|---|
| Classical Variants | |||||
| Common pattern |
| ||||
| Atypical Variants | |||||
| Small cell | |||||
| Lymphohistiocytic |
| ||||
| Giant cell |
| ||||
| Hodgkin's like |
| ||||
| Rare Variants | |||||
| Sarcomatoid |
| ||||
Video
{{#ev:youtube|3-ajNCAGP4Y}}
References
- ↑ Feldman AL, Dogan A, Smith DI, Law ME, Ansell SM, Johnson SH; et al. (2011). "Discovery of recurrent t(6;7)(p25.3;q32.3) translocations in ALK-negative anaplastic large cell lymphomas by massively parallel genomic sequencing". Blood. 117 (3): 915–9. doi:10.1182/blood-2010-08-303305. PMC 3035081. PMID 21030553.
- ↑ "The phosphatase JKAP/DUSP22 inhibits T-cell receptor signalling and autoimmunity by inactivating Lck".
- ↑ "Discovery of recurrent t(6;7)(p25.3;q32.3) translocations in ALK-negative anaplastic large cell lymphomas by massively parallel genomic sequencing".
- ↑ Xing X, Feldman AL (2015). "Anaplastic large cell lymphomas: ALK positive, ALK negative, and primary cutaneous". Adv Anat Pathol. 22 (1): 29–49. doi:10.1097/PAP.0000000000000047. PMID 25461779.
- ↑ Tabbó F, Barreca A, Piva R, Inghirami G; European T-Cell Lymphoma Study Group (2012). "ALK Signaling and Target Therapy in Anaplastic Large Cell Lymphoma". Front Oncol. 2: 41. doi:10.3389/fonc.2012.00041. PMC 3355932. PMID 22649787.
- ↑ "The anaplastic lymphoma kinase in the pathogenesis of cancer".
- ↑ The anaplastic lymphoma kinase in the pathogenesis of cancer. http://go.galegroup.com/ps/retrieve.dosgHitCountType=None&sort=RELEVANCE&inPS=true&prodId=HRCA&userGroupName=mlin_b_bethidmc&tabID=T002&searchId=R1&resultListType=RESULT_LIST&contentSegment=&searchType=AdvancedSearchForm¤tPosition=1&contentSet=GALE%7CA188154738&&docId=GALE Accessed on October 8, 2015
- ↑ 8.0 8.1 8.2 Swerdlow, Steven (2008). WHO classification of tumours of haematopoietic and lymphoid tissues. Lyon, France: International Agency for Research on Cancer. ISBN 9789283224310.
- ↑ Falini B, Bigerna B, Fizzotti M, Pulford K, Pileri SA, Delsol G; et al. (1998). "ALK expression defines a distinct group of T/null lymphomas ("ALK lymphomas") with a wide morphological spectrum". Am J Pathol. 153 (3): 875–86. doi:10.1016/S0002-9440(10)65629-5. PMC 1853018. PMID 9736036.
- ↑ Kinney MC, Collins RD, Greer JP, Whitlock JA, Sioutos N, Kadin ME (1993). "A small-cell-predominant variant of primary Ki-1 (CD30)+ T-cell lymphoma". Am J Surg Pathol. 17 (9): 859–68. PMID 8394652.
- ↑ "Frequent Expression ofthe NPM-ALK Chimeric Fusion Protein inAnaplastic Large-Cell Lymphoma, Lympho-Histiocytic Type" (PDF).
- ↑ 12.0 12.1 Vassallo J, Lamant L, Brugieres L, Gaillard F, Campo E, Brousset P; et al. (2006). "ALK-positive anaplastic large cell lymphoma mimicking nodular sclerosis Hodgkin's lymphoma: report of 10 cases". Am J Surg Pathol. 30 (2): 223–9. PMID 16434897.