Non ST elevation myocardial infarction pathophysiology: Difference between revisions
No edit summary |
No edit summary |
||
| Line 8: | Line 8: | ||
[[Image:Plaque rupture and coronary thrombosis in the left anterior descending artery with distal embolization.gif]] | [[Image:Plaque rupture and coronary thrombosis in the left anterior descending artery with distal embolization.gif]] | ||
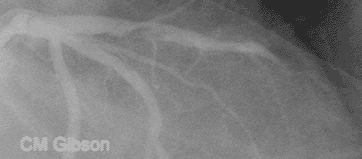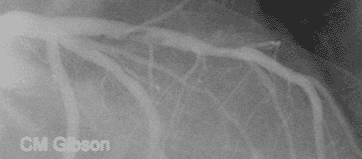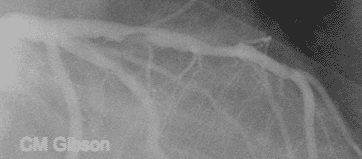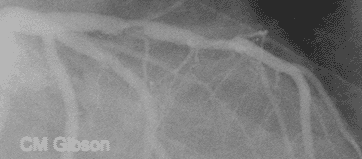
This video shows plaque rupture or disruption of the atherosclerotic plaque in the mid LAD. As is often the case, the plaque has torn at its edge, a location where the fibrous cap covering the atherosclerotic plaque is the thinnest. Clot has formed and it is embolizing downstream. The most common preceding pathophysiologic event in NSTEMI is the disruption of an [[Atherosclerosis|atherosclerotic]] [[Atheroma|plaque]] in an epicardial coronary artery such as that shown here. Exposure of the atherosclerotic plaque contents to the blood stream leads to activation of the [[clotting cascade]], local thrombus formation, and | This video shows plaque rupture or disruption of the atherosclerotic plaque in the mid LAD. As is often the case, the plaque has torn at its edge, a location where the fibrous cap covering the atherosclerotic plaque is the thinnest. Clot has formed and it is embolizing downstream. The most common preceding pathophysiologic event in NSTEMI is the disruption of an [[Atherosclerosis|atherosclerotic]] [[Atheroma|plaque]] in an epicardial coronary artery such as that shown here. Exposure of the atherosclerotic plaque contents to the blood stream leads to activation of the [[clotting cascade]], local thrombus formation, and incomplete occlusion of the epicardial artery in NSTEMI. This artery is open, in NSTEMI unlike STEMI where the artery is closed. The downstream microvasculature is occluded by the clot that has embolized, and this accounts for the [[troponin]] elevation in this patient. | ||
As opposed to the original hypothesis that acute coronary syndrome (ACS) is caused by gradual progression of coronary atherosclerosis to the point of a severe, fixed lesion, it has become clear that, in fact, ACS is usually caused by atherosclerotic plaque rupture at a site that previously had only mild to moderate stenosis.<ref>Martinez-Rumayor A, Januzzi JL Jr. Non-ST segment elevation acute coronary syndromes: A comprehensive review. South Med J. 2006 Oct;99(10):1103-10. PMID 17100031</ref> This plaque rupture exposes ligands (including collagen) for platelet adhesion which causes platelet aggregation and subsequent platelet activation. <ref>Patrono C, Renda G. Platelet activation and inhibition in unstable coronary syndromes. Am J Cardiol. 1997 Sep 4;80(5A):17E-20E. PMID 9296464 </ref> Platelets are activated by thrombin (found in blood clots), adenosine diphosphate (found in platelet granules), serotonin (also found in platelet granules) and thromboxane-A2. <ref>Patrono C, Renda G. Platelet activation and inhibition in unstable coronary syndromes. Am J Cardiol. 1997 Sep 4;80(5A):17E-20E. PMID 9296464 </ref> Upon activation, the glycoprotein IIb/IIIa receptor that in a non-active state is found in the cytosol is exteriorized and modified which enables additional platelet aggregation and cross-linking.<ref>Martinez-Rumayor A, Januzzi JL Jr. Non-ST segment elevation acute coronary syndromes: A comprehensive review. South Med J. 2006 Oct;99(10):1103-10. PMID 17100031</ref> The prothrombinase complex then binds to the activated platelet and starts to coagulation cascade.<ref>Martinez-Rumayor A, Januzzi JL Jr. Non-ST segment elevation acute coronary syndromes: A comprehensive review. South Med J. 2006 Oct;99(10):1103-10. PMID 17100031</ref> This entire process results in a thrombus which coalesces over the ruptured plaque. | As opposed to the original hypothesis that acute coronary syndrome (ACS) is caused by gradual progression of coronary atherosclerosis to the point of a severe, fixed lesion, it has become clear that, in fact, ACS is usually caused by atherosclerotic plaque rupture at a site that previously had only mild to moderate stenosis.<ref>Martinez-Rumayor A, Januzzi JL Jr. Non-ST segment elevation acute coronary syndromes: A comprehensive review. South Med J. 2006 Oct;99(10):1103-10. PMID 17100031</ref> This plaque rupture exposes ligands (including collagen) for platelet adhesion which causes platelet aggregation and subsequent platelet activation. <ref>Patrono C, Renda G. Platelet activation and inhibition in unstable coronary syndromes. Am J Cardiol. 1997 Sep 4;80(5A):17E-20E. PMID 9296464 </ref> Platelets are activated by thrombin (found in blood clots), adenosine diphosphate (found in platelet granules), serotonin (also found in platelet granules) and thromboxane-A2. <ref>Patrono C, Renda G. Platelet activation and inhibition in unstable coronary syndromes. Am J Cardiol. 1997 Sep 4;80(5A):17E-20E. PMID 9296464 </ref> Upon activation, the glycoprotein IIb/IIIa receptor that in a non-active state is found in the cytosol is exteriorized and modified which enables additional platelet aggregation and cross-linking.<ref>Martinez-Rumayor A, Januzzi JL Jr. Non-ST segment elevation acute coronary syndromes: A comprehensive review. South Med J. 2006 Oct;99(10):1103-10. PMID 17100031</ref> The prothrombinase complex then binds to the activated platelet and starts to coagulation cascade.<ref>Martinez-Rumayor A, Januzzi JL Jr. Non-ST segment elevation acute coronary syndromes: A comprehensive review. South Med J. 2006 Oct;99(10):1103-10. PMID 17100031</ref> This entire process results in a thrombus which coalesces over the ruptured plaque. | ||
Revision as of 22:33, 10 February 2009
| Cardiology Network |
 Discuss Non ST elevation myocardial infarction pathophysiology further in the WikiDoc Cardiology Network |
| Adult Congenital |
|---|
| Biomarkers |
| Cardiac Rehabilitation |
| Congestive Heart Failure |
| CT Angiography |
| Echocardiography |
| Electrophysiology |
| Cardiology General |
| Genetics |
| Health Economics |
| Hypertension |
| Interventional Cardiology |
| MRI |
| Nuclear Cardiology |
| Peripheral Arterial Disease |
| Prevention |
| Public Policy |
| Pulmonary Embolism |
| Stable Angina |
| Valvular Heart Disease |
| Vascular Medicine |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]
Please Take Over This Page and Apply to be Editor-In-Chief for this topic: There can be one or more than one Editor-In-Chief. You may also apply to be an Associate Editor-In-Chief of one of the subtopics below. Please mail us [2] to indicate your interest in serving either as an Editor-In-Chief of the entire topic or as an Associate Editor-In-Chief for a subtopic. Please be sure to attach your CV and or biographical sketch.
Plaque rupture, thrombus formation, and embolization underly the pathophysiology of NSTEMI
This video shows plaque rupture or disruption of the atherosclerotic plaque in the mid LAD. As is often the case, the plaque has torn at its edge, a location where the fibrous cap covering the atherosclerotic plaque is the thinnest. Clot has formed and it is embolizing downstream. The most common preceding pathophysiologic event in NSTEMI is the disruption of an atherosclerotic plaque in an epicardial coronary artery such as that shown here. Exposure of the atherosclerotic plaque contents to the blood stream leads to activation of the clotting cascade, local thrombus formation, and incomplete occlusion of the epicardial artery in NSTEMI. This artery is open, in NSTEMI unlike STEMI where the artery is closed. The downstream microvasculature is occluded by the clot that has embolized, and this accounts for the troponin elevation in this patient.
As opposed to the original hypothesis that acute coronary syndrome (ACS) is caused by gradual progression of coronary atherosclerosis to the point of a severe, fixed lesion, it has become clear that, in fact, ACS is usually caused by atherosclerotic plaque rupture at a site that previously had only mild to moderate stenosis.[1] This plaque rupture exposes ligands (including collagen) for platelet adhesion which causes platelet aggregation and subsequent platelet activation. [2] Platelets are activated by thrombin (found in blood clots), adenosine diphosphate (found in platelet granules), serotonin (also found in platelet granules) and thromboxane-A2. [3] Upon activation, the glycoprotein IIb/IIIa receptor that in a non-active state is found in the cytosol is exteriorized and modified which enables additional platelet aggregation and cross-linking.[4] The prothrombinase complex then binds to the activated platelet and starts to coagulation cascade.[5] This entire process results in a thrombus which coalesces over the ruptured plaque.
Although less common, ACS may also occur by other mechanisms. These include
- coronary artery spasm as in Prinzmetal's angina,
- severe narrowing alone without plaque rupture, as in the case of restenosis after percutaneous coronary intervention (PCI) or as with progressive atherosclerosis,
- coronary artery dissection,
- secondary ischemia in cases in which there is either increased myocardial oxygen demand as in tachycardia from fever, anemia, hypoxemia, thyrotoxicosis, or in cases of decreased supply such as in hypotension or anemia from hemorrhage.
Genetics
To date, there does not appear to be any single genetic marker predictive acute coronary syndrome (ACS).[6] In a recent validation study of genetic variants associated with (which includes ST-elevation myocardial infarction (STEMI), NSTEMI and UA) none of the 85 genetic variants tested were shown to be correlated with ACS. The study chose the polymorphic genetic variants based on statistically significant findings of prior studies. [7] Nonetheless, although no individual marker is likely to be predictive, in the future it is possible that a panel of markers may be used to assess risk.[8] [9]
Complete List of (known) Underlying Mechanisms of NSTEMI
- Inflammation
- Leukocytes, platelets
- Plaque disruption or plaque erosion
- Thrombosis
List of Factors may Effect Development and Complications of NSTEMI
(In alphabetical order)
- Blood lipid levels
- Catecholamine levels (smoking, cocaine, stress)
- Degree of coronary vasoconstriction
- Endothelial function
- Extent of collaterals
- Extent of plaque rupture or erosion
- Inflammatory substrate
- Location of the culprit coronary lesion
- Microembolization and microvascular obstruction
- Stenosis morphology and severity
- Systemic factors
- Heart rate and blood pressure
- Thrombotic factors
- Blood viscosity
- Intrinsic clotting activity
- Leukocyte activation
- Level of fibrinolytic activity
- Plaque tissue factor levels
- Platelet aggregability and reactivity
References
- ↑ Martinez-Rumayor A, Januzzi JL Jr. Non-ST segment elevation acute coronary syndromes: A comprehensive review. South Med J. 2006 Oct;99(10):1103-10. PMID 17100031
- ↑ Patrono C, Renda G. Platelet activation and inhibition in unstable coronary syndromes. Am J Cardiol. 1997 Sep 4;80(5A):17E-20E. PMID 9296464
- ↑ Patrono C, Renda G. Platelet activation and inhibition in unstable coronary syndromes. Am J Cardiol. 1997 Sep 4;80(5A):17E-20E. PMID 9296464
- ↑ Martinez-Rumayor A, Januzzi JL Jr. Non-ST segment elevation acute coronary syndromes: A comprehensive review. South Med J. 2006 Oct;99(10):1103-10. PMID 17100031
- ↑ Martinez-Rumayor A, Januzzi JL Jr. Non-ST segment elevation acute coronary syndromes: A comprehensive review. South Med J. 2006 Oct;99(10):1103-10. PMID 17100031
- ↑ Anwaruddin S, Askari AT, Topol EJ. Redefining risk in acute coronary syndromes using molecular medicine. J Am Coll Cardiol. 2007 Jan 23;49(3):279-89. Epub 2007 Jan 4. PMID 17239708
- ↑ Morgan TM, Krumholz HM, Lifton RP, Spertus JA.Nonvalidation of reported genetic risk factors for acute coronary syndrome in a large-scale replication study. JAMA. 2007 Apr 11;297(14):1551-61. PMID 17426274 Erratum in JAMA. 2007 Sep 5;298(9):973.
- ↑ Anwaruddin S, Askari AT, Topol EJ. Redefining risk in acute coronary syndromes using molecular medicine. J Am Coll Cardiol. 2007 Jan 23;49(3):279-89. Epub 2007 Jan 4. PMID 17239708
- ↑ Wilcken DE. Overview of inherited metabolic disorders causing cardiovascular disease. J Inherit Metab Dis. 2003;26(2-3):245-57. PMID 12889664