Diabetes mellitus type 1 natural history, complications, and prognosis: Difference between revisions
No edit summary |
No edit summary |
||
| Line 89: | Line 89: | ||
==Prognosis== | ==Prognosis== | ||
* [[Diabetes]] is a lifelong disease and there is no cure. Tight control of [[Blood sugar|blood glucose]] can prevent or delay [[diabetes]] [[Complication (medicine)|complications]]. But these problems can occur, even in people with good [[diabetes]] control.<ref>{{Cite web|url=http://www.diabetesincontrol.com/life-expectancy-for-type-1-diabetes/|title=Diabetes in control|last=|first=|date=|website=|publisher=|access-date=}}</ref> | * [[Diabetes]] is a lifelong disease and there is no cure. Tight control of [[Blood sugar|blood glucose]] can prevent or delay [[diabetes]] [[Complication (medicine)|complications]]. But these problems can occur, even in people with good [[diabetes]] control.<ref>{{Cite web|url=http://www.diabetesincontrol.com/life-expectancy-for-type-1-diabetes/|title=Diabetes in control|last=|first=|date=|website=|publisher=|access-date=}}</ref> | ||
* When [[Diabetes mellitus type 1|type 1 diabetes mellitus]] left untreated it can be fetal due to [[Complication (medicine)|complications]] like [[diabetic ketoacidosis]]. | |||
* [[Prognosis]] of [[Diabetes mellitus type 1|type 1 diabetes mellitus]] is effected by factors such as [[Blood sugar|blood glucose]] concentration, [[Glycosylated hemoglobin|hemoglobin A1c]] ([[Glycosylated hemoglobin|HbA1c), [[lipid|lipids]], [[blood pressure]], and weight. | |||
* There is a direct relationship between [[Glycosylated hemoglobin|hemoglobin A1c]] level and long-term [[Cognition|cognitive]] decline.<ref name="ZhengYan2018">{{cite journal|last1=Zheng|first1=Fanfan|last2=Yan|first2=Li|last3=Yang|first3=Zhenchun|last4=Zhong|first4=Baoliang|last5=Xie|first5=Wuxiang|title=HbA1c, diabetes and cognitive decline: the English Longitudinal Study of Ageing|journal=Diabetologia|volume=61|issue=4|year=2018|pages=839–848|issn=0012-186X|doi=10.1007/s00125-017-4541-7}}</ref> | |||
* The following factors have been related to longer life expectancy in patients with [[Diabetes mellitus type 1|type 1 diabetes]]:<ref name="pmid24936249">{{cite journal| author=Distiller LA| title=Why do some patients with type 1 diabetes live so long? | journal=World J Diabetes | year= 2014 | volume= 5 | issue= 3 | pages= 282-7 | pmid=24936249 | doi=10.4239/wjd.v5.i3.282 | pmc=4058732 | url=https://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=24936249 }} </ref> | |||
** Proper (not necessarily optimal) glycaemic control | |||
** High [[High density lipoprotein|HDL-cholesterol]] levels | |||
** Low insulin requirements (insulin sensitive) | |||
** Normal [[body mass index]] ([[Body mass index|BMI]]) | |||
** Proper [[blood pressure]] control | |||
** Patients who do not smoke | |||
** Absence of microalbuminuria after 15-20 years of [[Diabetes mellitus type 1|type 1 diabetes]] onset | |||
** Familial history of long life | |||
==References== | ==References== | ||
Revision as of 09:22, 30 August 2020
|
Diabetes mellitus type 1 Microchapters |
|
Differentiating Diabetes mellitus type 1 from other Diseases |
|
Diagnosis |
|
Treatment |
|
Cardiovascular Disease and Risk Management |
|
Case Studies |
|
Diabetes mellitus Main page |
|
Patient Information |
|---|
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]Associate Editor(s)-in-Chief: Vishal Devarkonda, M.B.B.S[2]
Overview
If left untreated, patients with [type 1 DM] may progress to develop complications of the hyperglycemia state, which commonly include diabetes ketoacidosis and hyperglycemia hyperosmolar state. Prognosis is generally good with compliance with medications.
Natural History
- The symptoms of type 1 diabetes usually develop in the first decade of life, and start with non-specific symptoms of classic new onset type 1 diabetes or acute symptoms with diabetic ketoacidosis. Without treatment, the patient will develop complications of type 1 diabetes.[1]
Complications
- Complications for type 1 diabetes include:[2][3][4][5]
| Complications of Diabetes | |
|---|---|
| Acute Complications due to hyperglycemia | |
| Microvascular complications | Eye disease
Neuropathy Sensory and motor (mono- and polyneuropathy) and Autonomic neuropathy Nephropathy (albuminuria and declining renal function) |
| Macrovascular complications | Coronary heart disease |
| Other | Gastrointestinal (gastroparesis, diarrhea)
Genitourinary (uropathy/sexual dysfunction) Cheiroarthropathy (thickened skin and reduced joint mobility) Fatty liver disease Low testosterone in men |
- In a control study patients with type 1 diabetes had significantly lower total body bone mineral density (BMD) z-score values. Lower levels of osteocalcin, C-terminal telopeptide, calcium, phosphorus, and magnesium have been found in patients with type 1 diabetes compared to control group.[6]
- A study demonstrated that children with type 1 diabetes mentioned barriers for physical activity (eg, fear of hypoglycemia, loss of control of diabetes and low fitness). This study report significant improvement with parental support. [7]
- Based on a systematic review, type 1 diabetic patients have worse executive function performance, working memory and task switching, compared to the control group.[8]
- The followings are some related dermatological consequences of type 1 diabetes:[9]
- Scleroderma-like skin changes: Pathogenesis is not fully understood, nevertheless advanced glycosylation end products and sugar alcohols buildup in the upper dermis is believed to effect the strengthening of collagen.
- Cheiroarthropathy (thickened skin and reduced joint mobility)
- Scleredema diabeticorum
- Necrobiosis lipoidica
- Bullosis diabeticorum
- Xerosis
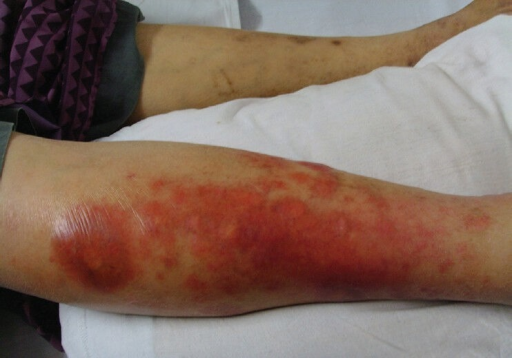
- Eruptive xanthomas: Although xanthomas are routinely related to hypertriglyceridemia, type 1 diabetic patients may develop eruptive xanthomas with normal levels of triglyceride. Prevelance of Eruptive xanthomas in type 1 diabetes is approximately 1%.
Prognosis
- Diabetes is a lifelong disease and there is no cure. Tight control of blood glucose can prevent or delay diabetes complications. But these problems can occur, even in people with good diabetes control.[11]
- When type 1 diabetes mellitus left untreated it can be fetal due to complications like diabetic ketoacidosis.
- Prognosis of type 1 diabetes mellitus is effected by factors such as blood glucose concentration, hemoglobin A1c ([[Glycosylated hemoglobin|HbA1c), lipids, blood pressure, and weight.
- There is a direct relationship between hemoglobin A1c level and long-term cognitive decline.[12]
- The following factors have been related to longer life expectancy in patients with type 1 diabetes:[13]
- Proper (not necessarily optimal) glycaemic control
- High HDL-cholesterol levels
- Low insulin requirements (insulin sensitive)
- Normal body mass index (BMI)
- Proper blood pressure control
- Patients who do not smoke
- Absence of microalbuminuria after 15-20 years of type 1 diabetes onset
- Familial history of long life
References
- ↑ Achenbach P, Bonifacio E, Koczwara K, Ziegler AG (2005). "Natural history of type 1 diabetes". Diabetes. 54 Suppl 2: S25–31. PMID 16306336.
- ↑ "ADA".
- ↑ Type 1 Diabetes mellitus "Dennis Kasper, Anthony Fauci, Stephen Hauser, Dan Longo, J. Larry Jameson, Joseph Loscalzo"Harrison's Principles of Internal Medicine, 19e Accessed on December 27th,2016
- ↑ Type 1 Diabetes mellitus "Dennis Kasper, Anthony Fauci, Stephen Hauser, Dan Longo, J. Larry Jameson, Joseph Loscalzo"Harrison's Principles of Internal Medicine, 19e Accessed on December 27th,2016
- ↑ Teng, Zhi-Pan; Tian, Rui; Xing, Fen-Li; Tang, Hui; Xu, Jin-Jing; Zhang, Bing-Wen; Qi, Jian-Wei (2017). "An association of type 1 diabetes mellitus with auditory dysfunction: A systematic review and meta-analysis". The Laryngoscope. 127 (7): 1689–1697. doi:10.1002/lary.26346. ISSN 0023-852X.
- ↑ Leão, Andreia Araújo Porchat; Fritz, Camilla Kapp; Dias, Marcia Regina Messaggi Gomes; Carvalho, Julienne Angela Ramires; Mascarenhas, Luis Paulo Gomes; Cat, Mônica Nunes Lima; Radominski, Rosana; Nesi-França, Suzana (2020). "Bone mass and dietary intake in children and adolescents with type 1 diabetes mellitus". Journal of Diabetes and its Complications. 34 (6): 107573. doi:10.1016/j.jdiacomp.2020.107573. ISSN 1056-8727.
- ↑ Jabbour, Georges; Henderson, Mélanie; Mathieu, Marie-Eve (2016). "Barriers to Active Lifestyles in Children with Type 1 Diabetes". Canadian Journal of Diabetes. 40 (2): 170–172. doi:10.1016/j.jcjd.2015.12.001. ISSN 1499-2671.
- ↑ Broadley, Melanie M.; White, Melanie J.; Andrew, Brooke (2017). "A Systematic Review and Meta-analysis of Executive Function Performance in Type 1 Diabetes Mellitus". Psychosomatic Medicine. 79 (6): 684–696. doi:10.1097/PSY.0000000000000460. ISSN 0033-3174.
- ↑ Feingold KR, Anawalt B, Boyce A, Chrousos G, de Herder WW, Dungan K; et al. (2000). "Endotext". PMID 29465926.
- ↑ https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3987274/. Missing or empty
|title=(help) - ↑ "Diabetes in control".
- ↑ Zheng, Fanfan; Yan, Li; Yang, Zhenchun; Zhong, Baoliang; Xie, Wuxiang (2018). "HbA1c, diabetes and cognitive decline: the English Longitudinal Study of Ageing". Diabetologia. 61 (4): 839–848. doi:10.1007/s00125-017-4541-7. ISSN 0012-186X.
- ↑ Distiller LA (2014). "Why do some patients with type 1 diabetes live so long?". World J Diabetes. 5 (3): 282–7. doi:10.4239/wjd.v5.i3.282. PMC 4058732. PMID 24936249.