Small intestine cancer: Difference between revisions
| Line 17: | Line 17: | ||
==Pathophysiology== | ==Pathophysiology== | ||
Ptahophysiology of small intestinal cancers is not much studied domain as it is a rare condition. However the incidence has increased recently particularly in black males and it | Ptahophysiology of small intestinal cancers is not much studied domain as it is a rare condition. However, the incidence has increased recently particularly in black males and it is same for the females. Studies are being conducted to evaluate association with environmental risk factors. <ref name="pmid8850266">{{cite journal |vauthors=Severson RK, Schenk M, Gurney JG, Weiss LK, Demers RY |title=Increasing incidence of adenocarcinomas and carcinoid tumors of the small intestine in adults |journal=Cancer Epidemiol. Biomarkers Prev. |volume=5 |issue=2 |pages=81–4 |date=February 1996 |pmid=8850266 |doi= |url=}}</ref> | ||
===Associations=== | |||
Cancer of small intestine can arise sporadically or they are associated with genetic diseases. | |||
*[[Familial adenomatous polyposis coli]] | |||
* [[Peutz-Jeghers syndrome]] | |||
*chronic intestinal inflammatory disorders e.g., [[Crohn's disease]] or [[Celiac sprue]] | |||
These are some of the associations of small intestinal tumors.<ref name="pmid11588539">{{cite journal |vauthors=Gill SS, Heuman DM, Mihas AA |title=Small intestinal neoplasms |journal=J. Clin. Gastroenterol. |volume=33 |issue=4 |pages=267–82 |date=October 2001 |pmid=11588539 |doi= |url=}}</ref> | |||
[[Adenocarcinomas]] and [[Carcinoid tumors]] of the smalls intestine are associated with malignant tumors of the other sites. Rarely people with [[Peutz-Jeghers syndrome]] can develop malignant changes in polyps present in the small intestine.<ref name="pmid6821853">{{cite journal |vauthors=Barclay TH, Schapira DV |title=Malignant tumors of the small intestine |journal=Cancer |volume=51 |issue=5 |pages=878–81 |date=March 1983 |pmid=6821853 |doi= |url=}}</ref> | |||
Primary [[adenocarcinoma]] consists of 40% of cases of malignant tumors of small intestine and it is the most common histologic type. [[Carcinoid tumor]] is the second most common cancer of the small bowel. | Primary [[adenocarcinoma]] consists of 40% of cases of malignant tumors of small intestine and it is the most common histologic type. [[Carcinoid tumor]] is the second most common cancer of the small bowel. | ||
Revision as of 15:55, 27 December 2018
For patient information click here
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Qurrat-ul-ain Abid, M.D.[2], Parminder Dhingra, M.D. [3]
|
Small intestine cancer Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Small intestine cancer On the Web |
|
American Roentgen Ray Society Images of Small intestine cancer |
|
Risk calculators and risk factors for Small intestine cancer |
Synonyms and keywords:
Overview
Historical Perspective
Despite of
Classification
Intestinal cancers can be classified into benign tumors, malignant tumors and extra-intestinal tumors. Benign tumors are: leiomyoma, lipoma, hamartoma and desmoid tumors. Malignant tumors of small intestine are: adenocarcinoma, leiomyosarcoma, carcinoid, and lymphomas. Extra-intestinal tumors metastasize to small intestine mostly through contagious spread or through peritoneal implantation. Metastatic spread through blood supply is very uncommon and is route of spread for Melanoma.[1]
Pathophysiology
Ptahophysiology of small intestinal cancers is not much studied domain as it is a rare condition. However, the incidence has increased recently particularly in black males and it is same for the females. Studies are being conducted to evaluate association with environmental risk factors. [2]
Associations
Cancer of small intestine can arise sporadically or they are associated with genetic diseases.
- Familial adenomatous polyposis coli
- Peutz-Jeghers syndrome
- chronic intestinal inflammatory disorders e.g., Crohn's disease or Celiac sprue
These are some of the associations of small intestinal tumors.[1] Adenocarcinomas and Carcinoid tumors of the smalls intestine are associated with malignant tumors of the other sites. Rarely people with Peutz-Jeghers syndrome can develop malignant changes in polyps present in the small intestine.[3] Primary adenocarcinoma consists of 40% of cases of malignant tumors of small intestine and it is the most common histologic type. Carcinoid tumor is the second most common cancer of the small bowel.
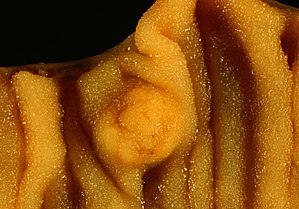
The pathophysiology of small intestinal cancers depends on the histological subtype. Duodenal tumors are more common than the tumors of jejunum and illeum.[4] Adenomas tend to occur more proximally in the duodenum while jejunum and illeum have more lymphomas.[5] Neuroendocrine tumors of small intestine originate from enterochromaffin (EC) cells and they secrete serotonin.[6]
Causes
Disease name] may be caused by [cause1], [cause2], or [cause3].
OR
Common causes of [disease] include [cause1], [cause2], and [cause3].
OR
The most common cause of [disease name] is [cause 1]. Less common causes of [disease name] include [cause 2], [cause 3], and [cause 4].
OR
The cause of [disease name] has not been identified. To review risk factors for the development of [disease name], click here.
Epidemiology and Demographics
Small intestinal cancer makes less than two percent of the gastrointestinal track cancers.[7]
The incidence/prevalence of [disease name] is approximately [number range] per 100,000 individuals worldwide.
OR
In [year], the incidence/prevalence of [disease name] was estimated to be [number range] cases per 100,000 individuals worldwide.
OR
In [year], the incidence of [disease name] is approximately [number range] per 100,000 individuals with a case-fatality rate of [number range]%.
Patients of all age groups may develop [disease name].
OR
The incidence of [disease name] increases with age; the median age at diagnosis is [#] years.
OR
[Disease name] commonly affects individuals younger than/older than [number of years] years of age.
OR
[Chronic disease name] is usually first diagnosed among [age group].
OR
[Acute disease name] commonly affects [age group].
There is no racial predilection to [disease name].
OR
[Disease name] usually affects individuals of the [race 1] race. [Race 2] individuals are less likely to develop [disease name].
[Disease name] affects men and women equally.
OR
[Gender 1] are more commonly affected by [disease name] than [gender 2]. The [gender 1] to [gender 2] ratio is approximately [number > 1] to 1.
The majority of [disease name] cases are reported in [geographical region].
OR
[Disease name] is a common/rare disease that tends to affect [patient population 1] and [patient population 2].
Risk Factors
There are no established risk factors for small intestinal cancers. Crohn disease is considered to be the most important risk factor of small intestinal cancers.[4] Other associated risk factors are: Familial Adenomatous Polyposis (FAP), Lynch syndrome, Acquired immunodeficiency syndrome (AIDS), Celiac disease, Peutz-Jeghers Syndrome and Hereditary Nonpolyposis Colorectal Cancer.[8]
Screening
Currently there are no screening protocols and rarity of condition makes it a less suspected condition.[9]
Natural History, Complications, and Prognosis
Adenocarcinoma of the duodenum is associated with low overall survival rate compared to the tumors located in Jejunum and ileum.[4]
Diagnosis
Adenocarcinoma of the small intestine is usually diagnosed late and patients present with metastasis of lymph node or distant sites. Main stay of the treatment is surgery for these tumors. [10]. Small intestinal cancers are not suspected clinically as their incidence is very low. Inaccessibility of endoscope to the small intestine can be cause of its late diagnosis. Small intestinal tumors can be diagnosed using enteroscope.[9]
History and Symptoms
The majority of patients with small Intestinal cancers are asymptomatic or have non-specific symptoms, which contributes to its late diagnosis and more investigations.[11]
Physical Examination
Patients with [disease name] usually appear [general appearance]. Physical examination of patients with [disease name] is usually remarkable for [finding 1], [finding 2], and [finding 3].
OR
Common physical examination findings of [disease name] include [finding 1], [finding 2], and [finding 3].
OR
The presence of [finding(s)] on physical examination is diagnostic of [disease name].
OR
The presence of [finding(s)] on physical examination is highly suggestive of [disease name].
CT scan
CT can help in differenting the small intestinal cancers. Adenocarcinmoa appear as ulcerative lesion, nodular or as annular lesion on CT. Non-Hodgkin lymphoma appears as bulky mass on CT that
Although the differential diagnosis for a small bowel tumor is extensive, various small bowel neoplasms have characteristic features at computed tomography (CT) that may aid in making a diagnosis. Small bowel adenocarcinoma may appear at CT as an annular lesion, a discrete nodular mass, or an ulcerative lesion. Non-Hodgkin lymphoma may appear as a segmental bulky mass that gradually merges into the normal bowel wall. Lymphoma is characteristically associated with marked luminal dilatation. Carcinoid tumor may appear as an ill-defined homogeneous mass that displaces bowel loops. Calcification and desmoplastic reaction in a mesenteric mass suggest the diagnosis of carcinoid tumor. Gastrointestinal stromal tumors (GISTs), both benign and malignant, may be submucosal, subserosal, or intraluminal. The CT appearance of a GIST may include a sharply defined mass with homogeneous attenuation, sometimes with calcification. Lipoma appears at CT as a well-circumscribed, intraluminal homogeneous mass with fat attenuation. Most malignant small bowel tumors are actually metastases that have spread intraperitoneally, hematogenously, or by local extension. Intraperitoneal seeding usually manifests at CT as multiple small nodular metastases along the small bowel serosa, mesentery, and omentum. In patients with Peutz-Jeghers syndrome, nonneoplastic lesions may mimic small bowel neoplasms.
MRI
There are no MRI findings associated with [disease name].
OR
[Location] MRI may be helpful in the diagnosis of [disease name]. Findings on MRI suggestive of/diagnostic of [disease name] include [finding 1], [finding 2], and [finding 3].
OR
There are no MRI findings associated with [disease name]. However, a MRI may be helpful in the diagnosis of complications of [disease name], which include [complication 1], [complication 2], and [complication 3].
Other Imaging Findings
There are no other imaging findings associated with [disease name].
OR
[Imaging modality] may be helpful in the diagnosis of [disease name]. Findings on an [imaging modality] suggestive of/diagnostic of [disease name] include [finding 1], [finding 2], and [finding 3].
Other Diagnostic Studies
There are no other diagnostic studies associated with [disease name].
OR
[Diagnostic study] may be helpful in the diagnosis of [disease name]. Findings suggestive of/diagnostic of [disease name] include [finding 1], [finding 2], and [finding 3].
OR
Other diagnostic studies for [disease name] include [diagnostic study 1], which demonstrates [finding 1], [finding 2], and [finding 3], and [diagnostic study 2], which demonstrates [finding 1], [finding 2], and [finding 3].
Treatment
For non-metastatic disease curative surgery gives good results when done in a tertiary care center. Adenocarcinoma of duodenum has a low 5-year disease free survival rate and requires surgery.[4] The role of adjuvant chemotherapy for small intestinal cancer is not established yet.[12]
OR
Surgery is not the first-line treatment option for patients with [disease name]. Surgery is usually reserved for patients with either [indication 1], [indication 2], and [indication 3]
OR
The mainstay of treatment for [disease name] is medical therapy. Surgery is usually reserved for patients with either [indication 1], [indication 2], and/or [indication 3].
OR
The feasibility of surgery depends on the stage of [malignancy] at diagnosis.
OR
Surgery is the mainstay of treatment for [disease or malignancy].
Primary Prevention
There are no established measures for the primary prevention of [disease name].
OR
There are no available vaccines against [disease name].
OR
Effective measures for the primary prevention of [disease name] include [measure1], [measure2], and [measure3].
OR
[Vaccine name] vaccine is recommended for [patient population] to prevent [disease name]. Other primary prevention strategies include [strategy 1], [strategy 2], and [strategy 3].
Secondary Prevention
There are no established measures for the secondary prevention of [disease name].
OR
Effective measures for the secondary prevention of [disease name] include [strategy 1], [strategy 2], and [strategy 3].
References
- ↑ 1.0 1.1 Gill SS, Heuman DM, Mihas AA (October 2001). "Small intestinal neoplasms". J. Clin. Gastroenterol. 33 (4): 267–82. PMID 11588539.
- ↑ Severson RK, Schenk M, Gurney JG, Weiss LK, Demers RY (February 1996). "Increasing incidence of adenocarcinomas and carcinoid tumors of the small intestine in adults". Cancer Epidemiol. Biomarkers Prev. 5 (2): 81–4. PMID 8850266.
- ↑ Barclay TH, Schapira DV (March 1983). "Malignant tumors of the small intestine". Cancer. 51 (5): 878–81. PMID 6821853.
- ↑ 4.0 4.1 4.2 4.3 Dabaja BS, Suki D, Pro B, Bonnen M, Ajani J (August 2004). "Adenocarcinoma of the small bowel: presentation, prognostic factors, and outcome of 217 patients". Cancer. 101 (3): 518–26. doi:10.1002/cncr.20404. PMID 15274064.
- ↑ Chow JS, Chen CC, Ahsan H, Neugut AI (August 1996). "A population-based study of the incidence of malignant small bowel tumours: SEER, 1973-1990". Int J Epidemiol. 25 (4): 722–8. PMID 8921448.
- ↑ Sei Y, Feng J, Zhao X, Forbes J, Tang D, Nagashima K, Hanson J, Quezado MM, Hughes MS, Wank SA (July 2016). "Polyclonal Crypt Genesis and Development of Familial Small Intestinal Neuroendocrine Tumors". Gastroenterology. 151 (1): 140–51. doi:10.1053/j.gastro.2016.03.007. PMC 5578471. PMID 27003604.
- ↑ North JH, Pack MS (January 2000). "Malignant tumors of the small intestine: a review of 144 cases". Am Surg. 66 (1): 46–51. PMID 10651347.
- ↑ Sarosiek T, Stelmaszuk M (February 2018). "[Small intestine neoplasms]". Pol. Merkur. Lekarski (in Polish). 44 (260): 45–48. PMID 29498365.
- ↑ 9.0 9.1 Rossini FP, Risio M, Pennazio M (January 1999). "Small bowel tumors and polyposis syndromes". Gastrointest. Endosc. Clin. N. Am. 9 (1): 93–114. PMID 9834319.
- ↑ Ogata Y, Yamaguchi K, Sasatomi T, Uchida S, Akagi Y, Shirouzu K (August 2010). "[Treatment and outcome in small bowel cancer]". Gan To Kagaku Ryoho (in Japanese). 37 (8): 1454–7. PMID 20716869.
- ↑ Williamson JM, Williamson RC (January 2014). "Small bowel tumors: pathology and management". J Med Assoc Thai. 97 (1): 126–37. PMID 24701741.
- ↑ Overman MJ, Kopetz S, Lin E, Abbruzzese JL, Wolff RA (May 2010). "Is there a role for adjuvant therapy in resected adenocarcinoma of the small intestine". Acta Oncol. 49 (4): 474–9. doi:10.3109/02841860903490051. PMID 20397775.