Emtricitabine and tenofovir disoproxil fumarate
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Alonso Alvarado, M.D. [2]
WikiDoc MAKES NO GUARANTEE OF VALIDITY. WikiDoc is not a professional health care provider, nor is it a suitable replacement for a licensed healthcare provider. WikiDoc is intended to be an educational tool, not a tool for any form of healthcare delivery. The educational content on WikiDoc drug pages is based upon the FDA package insert, National Library of Medicine content and practice guidelines / consensus statements. WikiDoc does not promote the administration of any medication or device that is not consistent with its labeling. Please read our full disclaimer here.
Black Box Warning
|
WARNING: LACTIC ACIDOSIS/SEVERE HEPATOMEGALY WITH STEATOSIS, POST TREATMENT ACUTE EXACERBATION OF HEPATITIS B, and RISK OF DRUG RESISTANCE WITH USE OF EMTRICITABINE AND TENOFOVIR DISOPROXIL FUMARATE FOR PRE-EXPOSURE PROPHYLAXIS (PrEP) IN UNDIAGNOSED EARLY HIV-1 INFECTION
See full prescribing information for complete Boxed Warning.
LACTIC ACIDOSIS/SEVERE HEPATOMEGALY WITH STEATOSIS, POST TREATMENT ACUTE EXACERBATION OF HEPATITIS B, and RISK OF DRUG RESISTANCE WITH USE OF EMTRICITABINE AND TENOFOVIR DISOPROXIL FUMARATE FOR PRE-EXPOSURE PROPHYLAXIS (PrEP) IN UNDIAGNOSED EARLY HIV-1 INFECTION: Lactic acidosis and severe hepatomegaly with steatosis, including fatal cases, have been reported with the use of nucleoside analogs, including tenofovir disoproxil fumarate, a component of emtricitabine and tenofovir disoproxil fumarate, in combination with other antiretrovirals.
Emtricitabine and tenofovir disoproxil fumarate is not approved for the treatment of chronic hepatitis B virus (HBV) infection and the safety and efficacy of emtricitabine and tenofovir disoproxil fumarate have not been established in patients coinfected with HBV and HIV-1. Severe acute exacerbations of hepatitis B have been reported in patients who are coinfected with HBV and HIV-1 and have discontinued emtricitabine and tenofovir disoproxil fumarate. Therefore, hepatic function should be monitored closely with both clinical and laboratory follow-up for at least several months in patients who are infected with HBV and discontinue emtricitabine and tenofovir disoproxil fumarate. If appropriate, initiation of anti-hepatitis B therapy may be warranted. Emtricitabine and tenofovir disoproxil fumarate used for a PrEP indication must only be prescribed to individuals confirmed to be HIV-negative immediately prior to initiating and periodically (at least every 3 months) during use. Drug-resistant HIV-1 variants have been identified with use of emtricitabine and tenofovir disoproxil fumarate for a PrEP indication following undetected acute HIV-1 infection. Do not initiate emtricitabine and tenofovir disoproxil fumarate for a PrEP indication if signs or symptoms of acute HIV-1 infection are present unless negative infection status is confirmed. |
Overview
Emtricitabine and tenofovir disoproxil fumarate is a human immunodeficiency virus 1 non-nucleoside analog reverse transcriptase inhibitor that is FDA approved for the treatment of HIV-1 Infection, pre-exposure prophylaxis to HIV-1. There is a Black Box Warning for this drug as shown here. Common adverse reactions include rash, lactic acidosis, abdominal pain, diarrhea, nausea, serum amylase raised, backache, myalgia, osteopenia, dizziness, headache, insomnia, peripheral neuropathy, depression, dream disorder, pneumonia, fatigue.
Adult Indications and Dosage
FDA-Labeled Indications and Dosage (Adult)
Recommended Dose for Treatment of HIV-1 Infection
The recommended dose of emtricitabine and tenofovir disoproxil fumarate in adults and in pediatric patients 12 years of age and older with body weight greater than or equal to 35 kg (greater than or equal to 77 lb) is one tablet (containing 200 mg of emtricitabine and 300 mg of tenofovir disoproxil fumarate) once daily taken orally with or without food.
Recommended Dose for Pre-exposure Prophylaxis
The dose of emtricitabine and tenofovir disoproxil fumarate in HIV-1 uninfected adults is one tablet (containing 200 mg of emtricitabine and 300 mg of tenofovir disoproxil fumarate) once daily taken orally with or without food.
Dose Adjustment for Renal Impairment
Treatment of HIV-1 Infection
Significantly increased drug exposures occurred when emtricitabine or tenofovir disoproxil fumarate were administered to subjects with moderate to severe renal impairment. Therefore, adjust the dosing interval of emtricitabine and tenofovir disoproxil fumarate in HIV-1 infected adult patients with baseline creatinine clearance 30–49 mL/min using the recommendations in Table 1. These dosing interval recommendations are based on modeling of single-dose pharmacokinetic data in non-HIV infected subjects. The safety and effectiveness of these dosing interval adjustment recommendations have not been clinically evaluated in patients with moderate renal impairment, therefore clinical response to treatment and renal function should be closely monitored in these patients.
No dose adjustment is necessary for HIV-1 infected patients with mild renal impairment (creatinine clearance 50–80 mL/min). No data are available to make dose recommendations in pediatric patients with renal impairment.
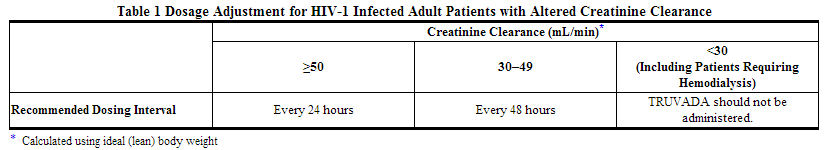
Routine monitoring of estimated creatinine clearance, serum phosphorus, urine glucose, and urine protein should be performed in all individuals with mild renal impairment.
Pre-exposure Prophylaxis
Do not use emtricitabine and tenofovir disoproxil fumarate for a PrEP indication in HIV-1 uninfected individuals with estimated creatinine clearance below 60 mL/min.
Routine monitoring of estimated creatinine clearance, serum phosphorus, urine glucose, and urine protein should be performed in all individuals with mild renal impairment. If a decrease in estimated creatinine clearance is observed in uninfected individuals while using emtricitabine and tenofovir disoproxil fumarate for PrEP, evaluate potential causes and re-assess potential risks and benefits of continued use.
Off-Label Use and Dosage (Adult)
Guideline-Supported Use
There is limited information regarding Off-Label Guideline-Supported Use of Emtricitabine and tenofovir disoproxil fumarate in adult patients.
Non–Guideline-Supported Use
There is limited information regarding Off-Label Non–Guideline-Supported Use of Emtricitabine and tenofovir disoproxil fumarate in adult patients.
Pediatric Indications and Dosage
FDA-Labeled Indications and Dosage (Pediatric)
There is limited information regarding Emtricitabine and tenofovir disoproxil fumarate FDA-Labeled Indications and Dosage (Pediatric) in the drug label.
Off-Label Use and Dosage (Pediatric)
Guideline-Supported Use
There is limited information regarding Off-Label Guideline-Supported Use of Emtricitabine and tenofovir disoproxil fumarate in pediatric patients.
Non–Guideline-Supported Use
There is limited information regarding Off-Label Non–Guideline-Supported Use of Emtricitabine and tenofovir disoproxil fumarate in pediatric patients.
Contraindications
Do not use emtricitabine and tenofovir disoproxil fumarate for pre-exposure prophylaxis in individuals with unknown or positive HIV-1 status. Emtricitabine and tenofovir disoproxil fumarate should be used in HIV-infected patients only in combination with other antiretroviral agents.
Warnings
|
WARNING: LACTIC ACIDOSIS/SEVERE HEPATOMEGALY WITH STEATOSIS, POST TREATMENT ACUTE EXACERBATION OF HEPATITIS B, and RISK OF DRUG RESISTANCE WITH USE OF EMTRICITABINE AND TENOFOVIR DISOPROXIL FUMARATE FOR PRE-EXPOSURE PROPHYLAXIS (PrEP) IN UNDIAGNOSED EARLY HIV-1 INFECTION
See full prescribing information for complete Boxed Warning.
LACTIC ACIDOSIS/SEVERE HEPATOMEGALY WITH STEATOSIS, POST TREATMENT ACUTE EXACERBATION OF HEPATITIS B, and RISK OF DRUG RESISTANCE WITH USE OF EMTRICITABINE AND TENOFOVIR DISOPROXIL FUMARATE FOR PRE-EXPOSURE PROPHYLAXIS (PrEP) IN UNDIAGNOSED EARLY HIV-1 INFECTION: Lactic acidosis and severe hepatomegaly with steatosis, including fatal cases, have been reported with the use of nucleoside analogs, including tenofovir disoproxil fumarate, a component of emtricitabine and tenofovir disoproxil fumarate, in combination with other antiretrovirals.
Emtricitabine and tenofovir disoproxil fumarate is not approved for the treatment of chronic hepatitis B virus (HBV) infection and the safety and efficacy of emtricitabine and tenofovir disoproxil fumarate have not been established in patients coinfected with HBV and HIV-1. Severe acute exacerbations of hepatitis B have been reported in patients who are coinfected with HBV and HIV-1 and have discontinued emtricitabine and tenofovir disoproxil fumarate. Therefore, hepatic function should be monitored closely with both clinical and laboratory follow-up for at least several months in patients who are infected with HBV and discontinue emtricitabine and tenofovir disoproxil fumarate. If appropriate, initiation of anti-hepatitis B therapy may be warranted. Emtricitabine and tenofovir disoproxil fumarate used for a PrEP indication must only be prescribed to individuals confirmed to be HIV-negative immediately prior to initiating and periodically (at least every 3 months) during use. Drug-resistant HIV-1 variants have been identified with use of emtricitabine and tenofovir disoproxil fumarate for a PrEP indication following undetected acute HIV-1 infection. Do not initiate emtricitabine and tenofovir disoproxil fumarate for a PrEP indication if signs or symptoms of acute HIV-1 infection are present unless negative infection status is confirmed. |
Lactic Acidosis/Severe Hepatomegaly with Steatosis
Lactic acidosis and severe hepatomegaly with steatosis, including fatal cases, have been reported with the use of nucleoside analogs, including VIREAD, a component of emtricitabine and tenofovir disoproxil fumarate, in combination with other antiretrovirals. A majority of these cases have been in women. Obesity and prolonged nucleoside exposure may be risk factors. Particular caution should be exercised when administering nucleoside analogs to any patient or uninfected individual with known risk factors for liver disease; however, cases have also been reported in HIV-1 infected patients with no known risk factors. Treatment with emtricitabine and tenofovir disoproxil fumarate should be suspended in any patient or uninfected individual who develops clinical or laboratory findings suggestive of lactic acidosis or pronounced hepatotoxicity (which may include hepatomegaly and steatosis even in the absence of marked transaminase elevations).
HBV Infection
It is recommended that all individuals be tested for the presence of chronic hepatitis B virus (HBV) before initiating emtricitabine and tenofovir disoproxil fumarate. emtricitabine and tenofovir disoproxil fumarate is not approved for the treatment of chronic HBV infection and the safety and efficacy of emtricitabine and tenofovir disoproxil fumarate have not been established in patients infected with HBV. Severe acute exacerbations of hepatitis B have been reported in patients who are coinfected with HBV and HIV-1 and have discontinued emtricitabine and tenofovir disoproxil fumarate. In some patients infected with HBV and treated with EMTRIVA, the exacerbations of hepatitis B were associated with liver decompensation and liver failure. Patients who are infected with HBV should be closely monitored with both clinical and laboratory follow-up for at least several months after stopping treatment with emtricitabine and tenofovir disoproxil fumarate. If appropriate, initiation of anti-hepatitis B therapy may be warranted. HBV -uninfected individuals should be offered vaccination.
New Onset or Worsening Renal Impairment
Emtricitabine and tenofovir are principally eliminated by the kidney. Renal impairment, including cases of acute renal failure and Fanconi syndrome (renal tubular injury with severe hypophosphatemia), has been reported with the use of VIREAD.
It is recommended that estimated creatinine clearance be assessed in all individuals prior to initiating therapy and as clinically appropriate during therapy with emtricitabine and tenofovir disoproxil fumarate. In patients at risk of renal dysfunction, including patients who have previously experienced renal events while receiving HEPSERA®, it is recommended that estimated creatinine clearance, serum phosphorus, urine glucose, and urine protein be assessed prior to initiation of emtricitabine and tenofovir disoproxil fumarate, and periodically during emtricitabine and tenofovir disoproxil fumarate therapy.
Emtricitabine and tenofovir disoproxil fumarate should be avoided with concurrent or recent use of a nephrotoxic agent (e.g., high-dose or multiple non-steroidal anti-inflammatory drugs (NSAIDs)) [See Drug Interactions (7.3)]. Cases of acute renal failure after initiation of high dose or multiple NSAIDs have been reported in HIV-infected patients with risk factors for renal dysfunction who appeared stable on tenofovir DF. Some patients required hospitalization and renal replacement therapy. Alternatives to NSAIDs should be considered, if needed, in patients at risk for renal dysfunction.
Persistent or worsening bone pain, pain in extremities, fractures and/or muscular pain or weakness may be manifestations of proximal renal tubulopathy and should prompt an evaluation of renal function in at-risk patients.
Treatment of HIV-1 Infection
Dosing interval adjustment of emtricitabine and tenofovir disoproxil fumarate and close monitoring of renal function are recommended in all patients with estimated creatinine clearance 30–49 mL/min, [See Dosage and Administration (2.3)]. No safety or efficacy data are available in patients with renal impairment who received emtricitabine and tenofovir disoproxil fumarate using these dosing guidelines, so the potential benefit of emtricitabine and tenofovir disoproxil fumarate therapy should be assessed against the potential risk of renal toxicity. Emtricitabine and tenofovir disoproxil fumarate should not be administered to patients with estimated creatinine clearance below 30 mL/min or patients requiring hemodialysis.
Pre-exposure Prophylaxis
Emtricitabine and tenofovir disoproxil fumarate for a PrEP indication should not be used if estimated creatinine clearance is less than 60 mL/min. If a decrease in estimated creatinine clearance is observed in uninfected individuals while using emtricitabine and tenofovir disoproxil fumarate for PrEP, evaluate potential causes and re-assess potential risks and benefits of continued use.
Coadministration with Other Products
Emtricitabine and tenofovir disoproxil fumarate is a fixed-dose combination of emtricitabine and tenofovir disoproxil fumarate. Do not coadminister emtricitabine and tenofovir disoproxil fumarate with ATRIPLA, COMPLERA, EMTRIVA, STRIBILD, or VIREAD. Due to similarities between emtricitabine and lamivudine, do not coadminister emtricitabine and tenofovir disoproxil fumarate with other drugs containing lamivudine, including Combivir (lamivudine/zidovudine), Epivir or Epivir-HBV (lamivudine), Epzicom (abacavir sulfate/lamivudine), or Trizivir (abacavir sulfate/lamivudine/zidovudine). Do not coadminister emtricitabine and tenofovir disoproxil fumarate with HEPSERA (adefovir dipivoxil).
Bone Effects of Tenofovir DF
Bone Mineral Density
In clinical trials in HIV-1 infected adults and in a clinical trial of HIV-1 uninfected individuals, tenofovir DF was associated with slightly greater decreases in bone mineral density (BMD) and increases in biochemical markers of bone metabolism, suggesting increased bone turnover relative to comparators. Serum parathyroid hormone levels and 1,25 Vitamin D levels were also higher in subjects receiving tenofovir DF.
Clinical trials evaluating tenofovir DF in pediatric and adolescent subjects were conducted. Under normal circumstances, BMD increases rapidly in pediatric patients. In HIV-1 infected subjects aged 2 years to less than 18 years, bone effects were similar to those observed in adult subjects and suggest increased bone turnover. Total body BMD gain was less in the tenofovir DF treated HIV-1 infected pediatric subjects as compared to the control groups. Similar trends were observed in chronic hepatitis B infected adolescent subjects aged 12 years to less than 18 years. In all pediatric trials, skeletal growth (height) appeared to be unaffected. For more information, please consult the VIREAD prescribing information.
The effects of tenofovir DF-associated changes in BMD and biochemical markers on long-term bone health and future fracture risk are unknown. Assessment of BMD should be considered for adult and pediatric patients who have a history of pathologic bone fracture or other risk factors for osteoporosis or bone loss. Although the effect of supplementation with calcium and vitamin D was not studied, such supplementation may be beneficial. If bone abnormalities are suspected then appropriate consultation should be obtained.
Mineralization Defects
Cases of osteomalacia associated with proximal renal tubulopathy, manifested as bone pain or pain in extremities and which may contribute to fractures, have been reported in association with the use of tenofovir DF. Arthralgias and muscle pain or weakness have also been reported in cases of proximal renal tubulopathy. Hypophosphatemia and osteomalacia secondary to proximal renal tubulopathy should be considered in patients at risk of renal dysfunction who present with persistent or worsening bone or muscle symptoms while receiving products containing tenofovir DF.
Fat Redistribution
Redistribution/accumulation of body fat including central obesity, dorsocervical fat enlargement (buffalo hump), peripheral wasting, facial wasting, breast enlargement, and "cushingoid appearance" have been observed in HIV-1 infected patients receiving antiretroviral therapy. The mechanism and long-term consequences of these events are currently unknown. A causal relationship has not been established.
Immune Reconstitution Syndrome
Immune reconstitution syndrome has been reported in HIV-1 infected patients treated with combination antiretroviral therapy, including emtricitabine and tenofovir disoproxil fumarate. During the initial phase of combination antiretroviral treatment, HIV-1 infected patients whose immune system responds may develop an inflammatory response to indolent or residual opportunistic infections [such as Mycobacterium avium infection, cytomegalovirus, Pneumocystis jirovecii pneumonia (PCP), or tuberculosis], which may necessitate further evaluation and treatment.
Autoimmune disorders (such as Graves' disease, polymyositis, and Guillain-Barré syndrome) have also been reported to occur in the setting of immune reconstitution, however, the time to onset is more variable, and can occur many months after initiation of treatment.
Early Virologic Failure
Clinical trials in HIV-1 infected subjects have demonstrated that certain regimens that only contain three nucleoside reverse transcriptase inhibitors (NRTI) are generally less effective than triple drug regimens containing two NRTIs in combination with either a non-nucleoside reverse transcriptase inhibitor or a HIV-1 protease inhibitor. In particular, early virological failure and high rates of resistance substitutions have been reported. Triple nucleoside regimens should therefore be used with caution. Patients on a therapy utilizing a triple nucleoside-only regimen should be carefully monitored and considered for treatment modification.
Comprehensive Management to Reduce the Risk of Acquiring HIV-1
Use emtricitabine and tenofovir disoproxil fumarate for pre-exposure prophylaxis only as part of a comprehensive prevention strategy that includes other prevention measures, such as safer sex practices, because emtricitabine and tenofovir disoproxil fumarate is not always effective in preventing the acquisition of HIV-1.
Counsel uninfected individuals about safer sex practices that include consistent and correct use of condoms, knowledge of their HIV-1 status and that of their partner(s), and regular testing for other sexually transmitted infections that can facilitate HIV-1 transmission (such as syphilis and gonorrhea). Inform uninfected individuals about and support their efforts in reducing sexual risk behavior.
Use emtricitabine and tenofovir disoproxil fumarate to reduce the risk of acquiring HIV-1 only in individuals confirmed to be HIV-negative. HIV-1 resistance substitutions may emerge in individuals with undetected HIV-1 infection who are taking only emtricitabine and tenofovir disoproxil fumarate, because emtricitabine and tenofovir disoproxil fumarate alone does not constitute a complete treatment regimen for HIV-1 treatment; therefore, care should be taken to minimize drug exposure in HIV-infected individuals.
Many HIV-1 tests, such as rapid tests, detect anti-HIV antibodies and may not identify HIV-1 during the acute stage of infection. Prior to initiating emtricitabine and tenofovir disoproxil fumarate for a PrEP indication, evaluate seronegative individuals for current or recent signs or symptoms consistent with acute viral infections (e.g., fever, fatigue, myalgia, skin rash, etc.) and ask about potential exposure events (e.g., unprotected, or condom broke during sex with an HIV-1 infected partner) that may have occurred within the last month.
If clinical symptoms consistent with acute viral infection are present and recent (<1 month) exposures are suspected, delay starting PrEP for at least one month and reconfirm HIV-1 status or use a test approved by the FDA as an aid in the diagnosis of HIV-1 infection, including acute or primary HIV-1 infection. While using emtricitabine and tenofovir disoproxil fumarate for a PrEP indication, HIV-1 screening tests should be repeated at least every 3 months. If symptoms consistent with acute HIV-1 infection develop following a potential exposure event, PrEP should be discontinued until negative infection status is confirmed using a test approved by the FDA as an aid in the diagnosis of HIV-1, including acute or primary HIV-1 infection.
Counsel uninfected individuals to strictly adhere to the recommended emtricitabine and tenofovir disoproxil fumarate dosing schedule. The effectiveness of emtricitabine and tenofovir disoproxil fumarate in reducing the risk of acquiring HIV-1 is strongly correlated with adherence as demonstrated by measurable drug levels in clinical trials
Adverse Reactions
Clinical Trials Experience
Adverse Reactions from Clinical Trials Experience in HIV-1 Infected Subjects
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
Clinical Trials in Adult Subjects
The most common adverse reactions (incidence greater than or equal to 10%, any severity) occurring in Study 934, an active-controlled clinical trial of efavirenz, emtricitabine, and tenofovir disoproxil fumarate, include diarrhea, nausea, fatigue, headache, dizziness, depression, insomnia, abnormal dreams, and rash. See also Table 2 for the frequency of treatment-emergent adverse reactions (Grades 2–4) occurring in greater than or equal to 5% of subjects treated in any treatment group in this trial.
Skin discoloration, manifested by hyperpigmentation on the palms and/or soles, was generally mild and asymptomatic. The mechanism and clinical significance are unknown. Study 934 - Treatment Emergent Adverse Reactions: In Study 934, 511 antiretroviral-naive subjects received either tenofovir disoproxil fumarate + emtricitabine administered in combination with efavirenz (N=257) or zidovudine/lamivudine administered in combination with efavirenz (N=254) for 144 weeks. Subjects had a mean age of 40 years (range 20 to 73 years) and were predominantly male (88%). Overall, 65% were White, 17% were Black, and 13% were Hispanic. Adverse reactions observed in this trial were generally consistent with those seen in other trials in treatment-experienced or treatment-naive subjects receiving tenofovir disoproxil fumarate and/or emtricitabine (Table 2).

Laboratory Abnormalities: Laboratory abnormalities observed in this trial were generally consistent with those seen in other trials of tenofovir disoproxil fumarate and/or emtricitabine (Table 3).

In addition to the events described above for Study 934, other adverse reactions that occurred in at least 5% of subjects receiving emtricitabine or tenofovir disoproxil fumarate with other antiretroviral agents in clinical trials include anxiety, arthralgia, increased cough, dyspepsia, fever, myalgia, pain, abdominal pain, back pain, paresthesia, peripheral neuropathy (including peripheral neuritis and neuropathy), pneumonia, and rhinitis.
In addition to the laboratory abnormalities described above for Study 934, Grades 3–4 laboratory abnormalities of increased bilirubin (>2.5 × ULN), increased pancreatic amylase (>2.0 × ULN), increased or decreased serum glucose (<40 or >250 mg/dL), and increased serum lipase (>2.0 × ULN) occurred in up to 3% of subjects treated with emtricitabine or tenofovir disoproxil fumarate with other antiretroviral agents in clinical trials.
Clinical Trials in Pediatric Subjects 12 Years of Age and Older
Emtricitabine: In addition to the adverse reactions reported in adults, anemia and hyperpigmentation were observed in 7% and 32%, respectively, of pediatric subjects (3 months to less than 18 years of age) who received treatment with emtricitabine in the larger of two open-label, uncontrolled pediatric trials (N=116). For additional information, please consult the emtricitabine prescribing information.
Tenofovir Disoproxil Fumarate: In a pediatric clinical trial conducted in subjects 12 to less than 18 years of age, the adverse reactions observed in pediatric subjects who received treatment with VIREAD were consistent with those observed in clinical trials of tenofovir disoproxil fumarate in adults.
Adverse Reactions from Clinical Trial Experience in HIV-1 Uninfected Adult Subjects
No new adverse reactions to TRUVADA were identified from two randomized placebo-controlled clinical trials (iPrEx, Partners PrEP) in which 2830 HIV-1 uninfected adults received TRUVADA once daily for pre-exposure prophylaxis. Subjects were followed for a median of 71 weeks and 87 weeks, respectively. These trials enrolled HIV-negative individuals ranging in age from 18 to 67 years. The iPrEx trial enrolled only males or transgender females of Hispanic/Latino (72%), White (18%), Black (9%) and Asian (5%) race. The Partners PrEP trial enrolled both males (61–64% across treatment groups) and females in Kenya and Uganda. Table 4 provides a list of all adverse events that occurred ≥2% of subjects in any treatment group in the iPrEx and Partners PrEP trials.
Laboratory Abnormalities: Table 5 provides a list of laboratory abnormalities observed in both trials. Six subjects in the TDF-containing arms of the Partners PrEP trial discontinued participation in the study due to an increase in blood creatinine compared with no discontinuations in the placebo group. One subject in the emtricitabine, and tenofovir disoproxil fumarate arm of the iPrEx trial discontinued from the study due to an increase in blood creatinine and another due to low phosphorous.
In addition to the laboratory abnormalities described above, Grade 1 proteinuria (1+) occurred in 6% of subjects receiving emtricitabine, and tenofovir disoproxil fumarate in the iPrEx trial. Grades 2–3 proteinuria (2–4+) and glycosuria (3+) occurred in less than 1% of subjects treated with emtricitabine, and tenofovir disoproxil fumarate in the iPrEx trial and Partners PrEP trial.


Changes in Bone Mineral Density
In clinical trials of HIV-1 uninfected individuals, decreases in BMD were observed. In the iPrEx trial, a substudy of 503 subjects found mean changes from baseline in BMD ranging from -0.4% to -1.0% across total hip, spine, femoral neck, and trochanter in the emtricitabine, and tenofovir disoproxil fumarate group compared with the placebo group, which returned toward baseline after discontinuation of treatment. Thirteen percent of subjects receiving emtricitabine, and tenofovir disoproxil fumarate vs. 6% of subjects receiving placebo lost at least 5% of BMD at the spine during treatment. Bone fractures were reported in 1.7% of the emtricitabine, and tenofovir disoproxil fumarate group compared with 1.4% in the placebo group. No correlation between BMD and fractures was noted. The Partners PrEP trial found similar fracture rates between treatment and placebo groups (0.8% and 0.6%, respectively). No BMD evaluations were conducted during this trial.
Postmarketing Experience
The following adverse reactions have been identified during postapproval use of tenofovir disoproxil fumarate. No additional adverse reactions have been identified during postapproval use of emtricitabine. Because postmarketing reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
- Immune System Disorders: allergic reaction, including angioedema
- Metabolism and Nutrition Disorders: lactic acidosis, hypokalemia, hypophosphatemia
- Respiratory, Thoracic, and Mediastinal Disorders: dyspnea
- Gastrointestinal Disorders: pancreatitis, increased amylase, abdominal pain
- Hepatobiliary Disorders: hepatic steatosis, hepatitis, increased liver enzymes (most commonly AST, ALT, GGT)
- Skin and Subcutaneous Tissue Disorders: rash
- Musculoskeletal and Connective Tissue Disorders: rhabdomyolysis, osteomalacia(manifested as bone pain and which may contribute to fractures), muscular weakness, myopathy
- Renal and Urinary Disorders: acute renal failure, renal failure, acute tubular necrosis, Fanconi syndrome, proximal renal tubulopathy, interstitial nephritis (including acute cases), nephrogenic diabetes insipidus, renal insufficiency, increased creatinine, proteinuria, polyuria
- General Disorders and Administration Site Conditions: asthenia
The following adverse reactions, listed under the body system headings above, may occur as a consequence of proximal renal tubulopathy: rhabdomyolysis, osteomalacia, hypokalemia, muscular weakness, myopathy, hypophosphatemia.
Drug Interactions
No drug interaction trials have been conducted using emtricitabine and tenofovir disoproxil fumarate tablets. Drug interaction trials have been conducted with emtricitabine and tenofovir disoproxil fumarate, the components of emtricitabine and tenofovir disoproxil fumarate. This section describes clinically relevant drug interactions observed with emtricitabine and tenofovir disoproxil fumarate.
Didanosine
Coadministration of emtricitabine and tenofovir disoproxil fumarate and didanosine should be undertaken with caution and patients receiving this combination should be monitored closely for didanosine-associated adverse reactions. Didanosine should be discontinued in patients who develop didanosine-associated adverse reactions.
When tenofovir disoproxil fumarate was administered with didanosine the Cmax and AUC of didanosine increased significantly. The mechanism of this interaction is unknown. Higher didanosine concentrations could potentiate didanosine-associated adverse reactions, including pancreatitis, and neuropathy. Suppression of CD4+ cell counts has been observed in patients receiving tenofovir DF with didanosine 400 mg daily.
In patients weighing greater than 60 kg, the didanosine dose should be reduced to 250 mg when it is coadministered with emtricitabine and tenofovir disoproxil fumarate. Data are not available to recommend a dose adjustment of didanosine for adult or pediatric patients weighing less than 60 kg. When coadministered, emtricitabine and tenofovir disoproxil fumarate and Videx EC may be taken under fasted conditions or with a light meal (less than 400 kcal, 20% fat).
HIV-1 Protease Inhibitors
Tenofovir decreases the AUC and Cmin of atazanavir. When coadministered with emtricitabine and tenofovir disoproxil fumarate, it is recommended that atazanavir 300 mg is given with ritonavir 100 mg. emtricitabine and tenofovir disoproxil fumarate should not be coadministered with atazanavir without ritonavir.
Lopinavir/ritonavir, atazanavir coadministered with ritonavir, and darunavir coadministered with ritonavir have been shown to increase tenofovir concentrations. Tenofovir disoproxil fumarate is a substrate of P-glycoprotein (Pgp) and breast cancer resistance protein (BCRP) transporters. When tenofovir disoproxil fumarate is co-administered with an inhibitor of these transporters, an increase in absorption may be observed. Patients receiving emtricitabine and tenofovir disoproxil fumarate concomitantly with lopinavir/ritonavir, ritonavir-boosted atazanavir, or ritonavir-boosted darunavir should be monitored for tenofovir-associated adverse reactions. Emtricitabine and tenofovir disoproxil fumarate should be discontinued in patients who develop tenofovir-associated adverse reactions.
Drugs Affecting Renal Function
Emtricitabine and tenofovir are primarily excreted by the kidneys by a combination of glomerular filtration and active tubular secretion. No drug-drug interactions due to competition for renal excretion have been observed; however, coadministration of emtricitabine and tenofovir disoproxil fumarate with drugs that are eliminated by active tubular secretion may increase concentrations of emtricitabine, tenofovir, and/or the coadministered drug. Some examples include, but are not limited to acyclovir, adefovir dipivoxil, cidofovir, ganciclovir, valacyclovir, valganciclovir, aminoglycosides (e.g., gentamicin), and high-dose or multiple NSAIDs. Drugs that decrease renal function may increase concentrations of emtricitabine and/or tenofovir.
Use in Specific Populations
Pregnancy
Pregnancy Category (FDA): B Antiretroviral Pregnancy Registry: To monitor fetal outcomes of pregnant women exposed to emtricitabine and tenofovir disoproxil fumarate, an Antiretroviral Pregnancy Registry (APR) has been established. Healthcare providers are encouraged to register patients by calling 1-800-258-4263.
Risk Summary
Emtricitabine and tenofovir disoproxil fumarate has been evaluated in a limited number of women during pregnancy and postpartum. Available human and animal data suggest that emtricitabine and tenofovir disoproxil fumarate does not increase the risk of major birth defects overall compared to the background rate. There are, however, no adequate and well-controlled trials in pregnant women. Because the studies in humans cannot rule out the possibility of harm, emtricitabine and tenofovir disoproxil fumarate should be used during pregnancy only if clearly needed. If an uninfected individual becomes pregnant while taking emtricitabine and tenofovir disoproxil fumarate for a PrEP indication, careful consideration should be given to whether use of emtricitabine and tenofovir disoproxil fumarate should be continued, taking into account the potential increased risk of HIV-1 infection during pregnancy.
Clinical Considerations=
As of July 2011, the APR has received prospective reports of 764 and 1219 exposures to emtricitabine and tenofovir containing regimens, respectively in the first trimester, 321 and 455 exposures, respectively, in second trimester, and 140 and 257 exposures, respectively, in the third trimester. Birth defects occurred in 18 of 764 (2.4%) live births for emtricitabine-containing regimens and 27 of 1219 (2.2%) live births for tenofovir-containing regimens (first trimester exposure) and 10 of 461 (2.2%) live births for emtricitabine-containing regimens and 15 of 714 (2.1%) live births for tenofovir-containing regimens (second/third trimester exposure). Among pregnant women in the U.S. reference population, the background rate of birth defects is 2.7%. There was no association between emtricitabine or tenofovir and overall birth defects observed in the APR.
Animal Data
Emtricitabine
The incidence of fetal variations and malformations was not increased in embryofetal toxicity studies performed with emtricitabine in mice at exposures (AUC) approximately 60-fold higher and in rabbits at approximately 120-fold higher than human exposures at the recommended daily dose.
Tenofovir Disoproxil Fumarate
Reproduction studies have been performed in rats and rabbits at doses up to 14 and 19 times the human dose based on body surface area comparisons and revealed no evidence of impaired fertility or harm to the fetus due to tenofovir.
Pregnancy Category (AUS):
There is no Australian Drug Evaluation Committee (ADEC) guidance on usage of Emtricitabine and tenofovir disoproxil fumarate in women who are pregnant.
Labor and Delivery
There is no FDA guidance on use of Emtricitabine and tenofovir disoproxil fumarate during labor and delivery.
Nursing Mothers
The Centers for Disease Control and Prevention recommend that HIV-1 infected mothers not breast-feed their infants to avoid risking postnatal transmission of HIV-1.
Studies in humans have shown that both tenofovir and emtricitabine are excreted in human milk. Because the risks of low level exposure to emtricitabine and tenofovir to infants are unknown, mothers should be instructed not to breast-feed if they are receiving emtricitabine and tenofovir disoproxil fumarate, whether they are taking emtricitabine and tenofovir disoproxil fumarate for treatment or to reduce the risk of acquiring HIV-1.
Emtricitabine
Samples of breast milk obtained from five HIV-1 infected mothers show that emtricitabine is secreted in human milk. Breastfeeding infants whose mothers are being treated with emtricitabine may be at risk for developing viral resistance to emtricitabine. Other emtricitabine-associated risks in infants breastfed by mothers being treated with emtricitabine are unknown.
Tenofovir Disoproxil Fumarate
Samples of breast milk obtained from five HIV-1 infected mothers show that tenofoviris secreted in human milk. Tenofovir-associated risks, including the risk of viral resistance to tenofovir, in infants breastfed by mothers being treated with tenofovir disoproxil fumarate are unknown.
Pediatric Use
Emtricitabine and tenofovir disoproxil fumarateshould only be administered to HIV-1 infected pediatric patients 12 years of age and older with body weight greater than or equal to 35 kg. Because it is a fixed-dose combination tablet, emtricitabine and tenofovir disoproxil fumarate cannot be adjusted for patients of lower age and weight. Safety and efficacy have not been established in pediatric patients less than 12 years of age or weighing less than 35 kg.
Geriatic Use
Clinical trials of emtricitabine or tenofovir disoproxil fumarate did not include sufficient numbers of subjects aged 65 and over to determine whether they respond differently from younger subjects. In general, dose selection for the elderly patients should be cautious, keeping in mind the greater frequency of decreased hepatic, renal, or cardiac function, and of concomitant disease or other drug therapy.
Gender
There is no FDA guidance on the use of Emtricitabine and tenofovir disoproxil fumarate with respect to specific gender populations.
Race
There is no FDA guidance on the use of Emtricitabine and tenofovir disoproxil fumarate with respect to specific racial populations.
Renal Impairment
Treatment of HIV-1 Infection
The dosing interval for emtricitabine or tenofovir disoproxil fumarate should be modified in HIV-infected adult patients with estimated creatinine clearance of 30–49 mL/min. Emtricitabine or tenofovir disoproxil fumarate should not be used in patients with estimated creatinine clearance below 30 mL/min and in patients with end-stage renal disease requiring dialysis.
Pre-exposure Prophylaxis
Emtricitabine or tenofovir disoproxil fumarate for a PrEP indication should not be used in HIV-1 uninfected individuals with estimated creatinine clearance below 60 mL/min. If a decrease in estimated creatinine clearance is observed in uninfected individuals while using emtricitabine or tenofovir disoproxil fumarate for PrEP, evaluate potential causes and re-assess potential risks and benefits of continued use.
Hepatic Impairment
There is no FDA guidance on the use of Emtricitabine and tenofovir disoproxil fumarate in patients with hepatic impairment.
Females of Reproductive Potential and Males
There is no FDA guidance on the use of Emtricitabine and tenofovir disoproxil fumarate in women of reproductive potentials and males.
Immunocompromised Patients
There is no FDA guidance one the use of Emtricitabine and tenofovir disoproxil fumarate in patients who are immunocompromised.
Administration and Monitoring
Administration
(Oral/Intravenous/etc)
Monitoring
Condition 1
(Description regarding monitoring, from Warnings section)
Condition 2
(Description regarding monitoring, from Warnings section)
Condition 3
(Description regarding monitoring, from Warnings section)
IV Compatibility
There is limited information regarding the compatibility of Emtricitabine and tenofovir disoproxil fumarate and IV administrations.
Overdosage
If overdose occurs, the patient must be monitored for evidence of toxicity, and standard supportive treatment applied as necessary.
Emtricitabine: Limited clinical experience is available at doses higher than the therapeutic dose of emtricitabine. In one clinical pharmacology trial, single doses of emtricitabine 1200 mg were administered to 11 subjects. No severe adverse reactions were reported.
Hemodialysis treatment removes approximately 30% of the emtricitabine dose over a 3-hour dialysis period starting within 1.5 hours of emtricitabine dosing (blood flow rate of 400 mL/min and a dialysate flow rate of 600 mL/min). It is not known whether emtricitabine can be removed by peritoneal dialysis.
Tenofovir Disoproxil Fumarate: Limited clinical experience at doses higher than the therapeutic dose of tenofovir disoproxil fumarate 300 mg is available. In one trial, 600 mg tenofovir disoproxil fumarate was administered to 8 subjects orally for 28 days, and no severe adverse reactions were reported. The effects of higher doses are not known.
Tenofovir is efficiently removed by hemodialysis with an extraction coefficient of approximately 54%. Following a single 300 mg dose of tenofovir disoproxil fumarate, a four-hour hemodialysis session removed approximately 10% of the administered tenofovir dose.
Pharmacology
Emtricitabine and tenofovir disoproxil fumarate
| |
| Systematic (IUPAC) name | |
| ? | |
| Identifiers | |
| CAS number | ? |
| ATC code | ? |
| PubChem | ? |
| Chemical data | |
| Formula | ? |
| Mol. mass | ? |
| Pharmacokinetic data | |
| Bioavailability | ? |
| Metabolism | ? |
| Half life | ? |
| Excretion | ? |
| Therapeutic considerations | |
| Pregnancy cat. |
? |
| Legal status | |
| Routes | ? |
Mechanism of Action
Emtricitabine
Emtricitabine, a synthetic nucleoside analog of cytidine, is phosphorylated by cellular enzymes to form emtricitabine 5'-triphosphate. Emtricitabine 5'-triphosphate inhibits the activity of the HIV-1 reverse transcriptase (RT) by competing with the natural substrate deoxycytidine 5'-triphosphate and by being incorporated into nascent viral DNA which results in chain termination. Emtricitabine 5'-triphosphate is a weak inhibitor of mammalian DNA polymerase α, β, ε and mitochondrial DNA polymerase γ.
Tenofovir Disoproxil Fumarate
Tenofovir disoproxil fumarate is an acyclic nucleoside phosphonate diester analog of adenosine monophosphate. Tenofovir disoproxil fumarate requires initial diester hydrolysis for conversion to tenofovir and subsequent phosphorylations by cellular enzymes to form tenofovir diphosphate. Tenofovir diphosphate inhibits the activity of HIV-1 RT by competing with the natural substrate deoxyadenosine 5'-triphosphate and, after incorporation into DNA, by DNA chain termination. Tenofovir diphosphate is a weak inhibitor of mammalian DNA polymerases α, β, and mitochondrial DNA polymerase γ.
Structure
Emtricitabine and tenofovir disoproxil fumarate tablets are fixed dose combination tablets containing emtricitabine and tenofovir disoproxil fumarate. Emtricitabine is the brand name for emtricitabine, a synthetic nucleoside analog of cytidine. Tenofovir disoproxil fumarate (tenofovir DF) is converted in vivo to tenofovir, an acyclic nucleoside phosphonate (nucleotide) analog of adenosine 5'-monophosphate. Both emtricitabine and tenofovir exhibit inhibitory activity against HIV-1 reverse transcriptase.
Emtricitabine: The chemical name of emtricitabine is 5-fluoro-1-(2R,5S)-[2-(hydroxymethyl)-1,3-oxathiolan-5-yl]cytosine. Emtricitabine is the (-) enantiomer of a thio analog of cytidine, which differs from other cytidine analogs in that it has a fluorine in the 5-position.
It has a molecular formula of C8H10FN3O3S and a molecular weight of 247.24. It has the following structural formula:
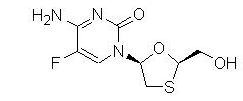
Emtricitabine is a white to off-white crystalline powder with a solubility of approximately 112 mg/mL in water at 25 °C. The partition coefficient (log p) for emtricitabine is -0.43 and the pKa is 2.65.
Tenofovir Disoproxil Fumarate: Tenofovir disoproxil fumarate is a fumaric acid salt of the bis-isopropoxycarbonyloxymethyl ester derivative of tenofovir. The chemical name of tenofovir disoproxil fumarate is 9-[(R)-2 ([bis([(isopropoxycarbonyl)oxy]- methoxy)phosphinyl]methoxy)propyl]adenine fumarate (1:1). It has a molecular formula of C19H30N5O10P ∙ C4H4O4 and a molecular weight of 635.52. It has the following structural formula:
Tenofovir disoproxil fumarate is a white to off-white crystalline powder with a solubility of 13.4 mg/mL in water at 25 °C. The partition coefficient (log p) for tenofovir disoproxil is 1.25 and the pKa is 3.75. All dosages are expressed in terms of tenofovir disoproxil fumarate except where otherwise noted.
Emtricitabine and tenofovir disoproxil fumarate tablets are for oral administration. Each film-coated tablet contains 200 mg of emtricitabine and 300 mg of tenofovir disoproxil fumarate, (which is equivalent to 245 mg of tenofovir disoproxil), as active ingredients. The tablets also include the following inactive ingredients: croscarmellose sodium, lactose monohydrate, magnesium stearate, microcrystalline cellulose, and pregelatinized starch (gluten free). The tablets are coated with Opadry II Blue Y-30-10701, which contains FD&C Blue #2 aluminum lake, hydroxypropyl methylcellulose 2910, lactose monohydrate, titanium dioxide, and triacetin.
Pharmacodynamics
Antiviral Activity
Emtricitabine and Tenofovir Disoproxil Fumarate: In combination studies evaluating the cell culture antiviral activity of emtricitabine and tenofovir together, synergistic antiviral effects were observed.
Emtricitabine
The antiviral activity of emtricitabine against laboratory and clinical isolates of HIV-1 was assessed in lymphoblastoid cell lines, the MAGI-CCR5 cell line, and peripheral blood mononuclear cells. The 50% effective concentration (EC50) values for emtricitabine were in the range of 0.0013–0.64 µM (0.0003–0.158 µg/mL). In drug combination studies of emtricitabine with nucleoside reverse transcriptase inhibitors (abacavir, lamivudine, stavudine, zalcitabine, zidovudine), non-nucleoside reverse transcriptase inhibitors (delavirdine, efavirenz, nevirapine), and protease inhibitors (amprenavir, nelfinavir, ritonavir, saquinavir), additive to synergistic effects were observed. Emtricitabine displayed antiviral activity in cell culture against HIV-1 clades A, B, C, D, E, F, and G (EC50 values ranged from 0.007–0.075 µM) and showed strain specific activity against HIV-2 (EC50 values ranged from 0.007–1.5 µM).
Tenofovir Disoproxil Fumarate
The antiviral activity of tenofovir against laboratory and clinical isolates of HIV-1 was assessed in lymphoblastoid cell lines, primary monocyte/macrophage cells and peripheral blood lymphocytes. The EC50 values for tenofovir were in the range of 0.04–8.5 µM. In drug combination studies of tenofovir with nucleoside reverse transcriptase inhibitors (abacavir, didanosine, lamivudine, stavudine, zalcitabine, zidovudine), non-nucleoside reverse transcriptase inhibitors (delavirdine, efavirenz, nevirapine), and protease inhibitors (amprenavir, indinavir, nelfinavir, ritonavir, saquinavir), additive to synergistic effects were observed. Tenofovir displayed antiviral activity in cell culture against HIV-1 clades A, B, C, D, E, F, G and O (EC50 values ranged from 0.5–2.2 µM) and showed strain specific activity against HIV-2 (EC50 values ranged from 1.6 µM to 5.5 µM).
Prophylactic Activity in a Nonhuman Primate Model of HIV Transmission
Emtricitabine and Tenofovir Disoproxil Fumarate: The prophylactic activity of the combination of daily oral emtricitabine (FTC) and tenofovir disoproxil fumarate (TDF) was evaluated in a controlled study of macaques inoculated once weekly for 14 weeks with SIV/HIV-1 chimeric virus (SHIV) applied to the rectal surface. Of the 18 control animals, 17 became infected after a median of 2 weeks. In contrast, 4 of the 6 animals treated daily with oral FTC and TDF remained uninfected and the two infections that did occur were significantly delayed until 9 and 12 weeks and exhibited reduced viremia. An M184I-expressing FTC-resistant variant emerged in 1 of the 2 macaques after 3 weeks of continued drug exposure.
Resistance
Emtricitabine and Tenofovir Disoproxil Fumarate: HIV-1 isolates with reduced susceptibility to the combination of emtricitabine and tenofovir have been selected in cell culture. Genotypic analysis of these isolates identified the M184V/I and/or K65R amino acid substitutions in the viral RT. In a clinical trial of treatment-naive subjects [Study 934, see Clinical Studies (14.1)], resistance analysis was performed on HIV-1 isolates from all confirmed virologic failure subjects with greater than 400 copies/mL of HIV-1 RNA at Week 144 or early discontinuation. Development of efavirenz resistance-associated substitutions occurred most frequently and was similar between the treatment arms. The M184V amino acid substitution, associated with resistance to emtricitabine and lamivudine, was observed in 2/19 analyzed subject isolates in the emtricitabine + tenofovir disoproxil fumarate group and in 10/29 analyzed subject isolates in the zidovudine/lamivudine group. Through 144 weeks of Study 934, no subjects have developed a detectable K65R substitution in their HIV-1 as analyzed through standard genotypic analysis.
Emtricitabine: Emtricitabine-resistant isolates of HIV-1 have been selected in cell culture and in vivo. Genotypic analysis of these isolates showed that the reduced susceptibility to emtricitabine was associated with a substitution in the HIV-1 RT gene at codon 184 which resulted in an amino acid substitution of methionine by valine or isoleucine (M184V/I).
Tenofovir Disoproxil Fumarate: HIV-1 isolates with reduced susceptibility to tenofovir have been selected in cell culture. These viruses expressed a K65R substitution in RT and showed a 2–4 fold reduction in susceptibility to tenofovir.
In treatment-naive subjects, isolates from 8/47 (17%) analyzed subjects developed the K65R substitution in the tenofovir disoproxil fumarate arm through 144 weeks; 7 occurred in the first 48 weeks of treatment and 1 at Week 96. In treatment-experienced subjects, 14/304 (5%) isolates from subjects failing tenofovir disoproxil fumarate through Week 96 showed greater than 1.4 fold (median 2.7) reduced susceptibility to tenofovir. Genotypic analysis of the resistant isolates showed a substitution in the HIV-1 RT gene resulting in the K65R amino acid substitution.
iPrEx Trial: In a clinical study of HIV-1 seronegative subjects [iPrEx Trial, see Clinical Studies (14.2)], no amino acid substitutions associated with resistance to emtricitabine or tenofovir were detected at the time of seroconversion among 48 subjects in the emtricitabine and tenofovir disoproxil fumarate group and 83 subjects in the placebo group who became infected with HIV-1 during the trial. Ten subjects were observed to be HIV-1 infected at time of enrollment. The M184V/I substitutions associated with resistance to emtricitabine were observed in 3 of the 10 subjects (2 of 2 in theemtricitabine and tenofovir disoproxil fumarate group and 1 of 8 in the placebo group). One of the two subjects in the emtricitabine and tenofovir disoproxil fumarate group harbored wild type virus at enrollment and developed the M184V substitution 4 weeks after enrollment. The other subject had indeterminate resistance at enrollment but was found to have the M184I substitution 4 weeks after enrollment.
Partners PrEP Trial: In a clinical study of HIV-1 seronegative subjects [Partners PrEP Trial, see Clinical Studies (14.3)], no variants expressing amino acid substitutions associated with resistance to emtricitabine or tenofovir were detected at the time of seroconversion among 12 subjects in the emtricitabine and tenofovir disoproxil fumarate group, 15 subjects in the tenofovir disoproxil fumarate group, and 51 subjects in the placebo group. Fourteen subjects were observed to be HIV-1 infected at the time of enrollment (3 in the emtricitabine and tenofovir disoproxil fumarate group, 5 in the tenofovir disoproxil fumarate group, and 6 in the placebo group). One of the three subjects in the emtricitabine and tenofovir disoproxil fumarate group who was infected with wild type virus at enrollment selected an M184V expressing virus by week 12. Two of the five subjects in the tenofovir disoproxil fumarate group had tenofovir-resistant viruses at the time of seroconversion; one subject infected with wild type virus at enrollment developed a K65R substitution by week 16, while the second subject had virus expressing the combination of D67N and K70R substitutions upon seroconversion at week 60, although baseline virus was not genotyped and it is unclear if the resistance emerged or was transmitted. Following enrollment, 4 subjects (2 in the tenofovir disoproxil fumarate group, 1 in the emtricitabine and tenofovir disoproxil fumarate group, and 1 in the placebo group) had virus expressing K103N or V106A substitutions, which confer high-level resistance to NNRTIs but have not been associated with tenofovir or emtricitabine and may have been present in the infecting virus.
Cross Resistance
Emtricitabine and Tenofovir Disoproxil Fumarate: Cross-resistance among certain nucleoside reverse transcriptase inhibitors (NRTIs) has been recognized. The M184V/I and/or K65R substitutions selected in cell culture by the combination of emtricitabine and tenofovir are also observed in some HIV-1 isolates from subjects failing treatment with tenofovir in combination with either lamivudine or emtricitabine, and either abacavir or didanosine. Therefore, cross-resistance among these drugs may occur in patients whose virus harbors either or both of these amino acid substitutions.
Emtricitabine: Emtricitabine-resistant isolates (M184V/I) were cross-resistant to lamivudine and zalcitabine but retained susceptibility in cell culture to didanosine, stavudine, tenofovir, zidovudine, and NNRTIs (delavirdine, efavirenz, and nevirapine). HIV-1 isolates containing the K65R substitution, selected in vivo by abacavir, didanosine, tenofovir, and zalcitabine, demonstrated reduced susceptibility to inhibition by emtricitabine. Viruses harboring substitutions conferring reduced susceptibility to stavudine and zidovudine (M41L, D67N, K70R, L210W, T215Y/F, K219Q/E), or didanosine (L74V) remained sensitive to emtricitabine. HIV-1 containing the K103N substitution associated with resistance to NNRTIs was susceptible to emtricitabine.
Tenofovir Disoproxil Fumarate: HIV-1 isolates from subjects (N=20) whose HIV-1 expressed a mean of 3 zidovudine-associated RT amino acid substitutions (M41L, D67N, K70R, L210W, T215Y/F, or K219Q/E/N) showed a 3.1-fold decrease in the susceptibility to tenofovir. Subjects whose virus expressed an L74V substitution without zidovudine resistance associated substitutions (N=8) had reduced response to tenofovir disoproxil fumarate. Limited data are available for patients whose virus expressed a Y115F substitution (N=3), Q151M substitution (N=2), or T69 insertion (N=4), all of whom had a reduced response.
Pharmacokinetics
Emtricitabine and Tenofovir Disoproxil Fumarate:: One emtricitabine and tenofovir disoproxil fumarate tablet was bioequivalent to one emtricitabine capsule (200 mg) plus one tenofovir disoproxil fumarate tablet (300 mg) following single-dose administration to fasting healthy subjects (N=39).
Emtricitabine: The pharmacokinetic properties of emtricitabine are summarized in Table 6. Following oral administration of emtricitabine, emtricitabine is rapidly absorbed with peak plasma concentrations occurring at 1–2 hours post-dose. Less than 4% of emtricitabine binds to human plasma proteins in vitro and the binding is independent of concentration over the range of 0.02–200 μg/mL. Following administration of radiolabelled emtricitabine, approximately 86% is recovered in the urine and 13% is recovered as metabolites. The metabolites of emtricitabine include 3'-sulfoxide diastereomers and their glucuronic acid conjugate. Emtricitabine is eliminated by a combination of glomerular filtration and active tubular secretion. Following a single oral dose of emtricitabine, the plasma emtricitabine half-life is approximately 10 hours.
Tenofovir Disoproxil Fumarate: The pharmacokinetic properties of tenofovir disoproxil fumarate are summarized in Table 6. Following oral administration of tenofovir disoproxil fumarate, maximum tenofovir serum concentrations are achieved in 1.0 ± 0.4 hour. Less than 0.7% of tenofovir binds to human plasma proteins in vitro and the binding is independent of concentration over the range of 0.01–25 µg/mL. Approximately 70–80% of the intravenous dose of tenofovir is recovered as unchanged drug in the urine. Tenofovir is eliminated by a combination of glomerular filtration and active tubular secretion. Following a single oral dose of tenofovir disoproxil fumarate, the terminal elimination half-life of tenofovir is approximately 17 hours.

Effects of Food on Oral Absorption
Emtricitabine and tenofovir disoproxil fumarate may be administered with or without food. Administration of emtricitabine and tenofovir disoproxil fumarate following a high fat meal (784 kcal; 49 grams of fat) or a light meal (373 kcal; 8 grams of fat) delayed the time of tenofovir Cmax by approximately 0.75 hour. The mean increases in tenofovir AUC and Cmax were approximately 35% and 15%, respectively, when administered with a high fat or light meal, compared to administration in the fasted state. In previous safety and efficacy trials, tenofovir disoproxil fumarate was taken under fed conditions. Emtricitabine systemic exposures (AUC and Cmax) were unaffected when emtricitabine and tenofovir disoproxil fumarate was administered with either a high fat or a light meal.
Special Populations
Race
Emtricitabine: No pharmacokinetic differences due to race have been identified following the administration of emtricitabine. Tenofovir Disoproxil Fumarate: There were insufficient numbers from racial and ethnic groups other than Caucasian to adequately determine potential pharmacokinetic differences among these populations following the administration of tenofovir disoproxil fumarate.
Gender
Emtricitabine and Tenofovir Disoproxil Fumarate: Emtricitabine and tenofovir pharmacokinetics are similar in male and female subjects.
Pediatric Patients
Emtricitabine and tenofovir disoproxil fumarate should not be administered to HIV-1 infected pediatric patients less than 12 years of age or weighing less than 35 kg (less than 77 lb).
Emtricitabine: The pharmacokinetics of emtricitabine at steady state were determined in 27 HIV-1-infected pediatric subjects 13 to 17 years of age receiving a daily dose of 6 mg/kg up to a maximum dose of 240 mg oral solution or a 200 mg capsule; 26 of 27 subjects in this age group received the 200 mg emtricitabine capsule. Mean (± SD) Cmax and AUC were 2.7 ± 0.9 μg/mL and 12.6 ± 5.4 μg•hr/mL, respectively. Exposures achieved in pediatric subjects 12 to less than 18 years of age were similar to those achieved in adults receiving a once daily dose of 200 mg.
Tenofovir Disoproxil Fumarate: Steady-state pharmacokinetics of tenofovir were evaluated in 8 HIV-1 infected pediatric subjects (12 to less than 18 years). Mean (± SD) Cmax and AUCtau are 0.38 ± 0.13 μg/mL and 3.39 ± 1.22 μg•hr/mL, respectively. Tenofovir exposure achieved in these pediatric subjects receiving oral daily doses of tenofovir disoproxil fumarate 300 mg was similar to exposures achieved in adults receiving once-daily doses of tenofovir disoproxil fumarate 300 mg.
Geriatric Patients
Pharmacokinetics of emtricitabine and tenofovir have not been fully evaluated in the elderly (65 years of age and older).
Patients with Impaired Renal Function
The pharmacokinetics of emtricitabine and tenofovir are altered in subjects with renal impairment. In adult subjects with creatinine clearance below 50 mL/min, Cmax, and AUC0–∞ of emtricitabine and tenofovir were increased. It is recommended that the dosing interval for emtricitabine and tenofovir disoproxil fumarate be modified in HIV-infected adult patients with estimated creatinine clearance 30–49 mL/min. No data are available to make dose recommendations in pediatric patients with renal impairment. emtricitabine and tenofovir disoproxil fumarate should not be used in patients with estimated creatinine clearance below 30 mL/min and in patients with end-stage renal disease requiring dialysis.
Emtricitabine and tenofovir disoproxil fumarate for a PrEP indication should not be used in HIV-1 uninfected individuals with estimated creatinine clearance below 60 mL/min. If a decrease in estimated creatinine clearance is observed in uninfected individuals while using emtricitabine and tenofovir disoproxil fumarate for PrEP, evaluate potential causes and re-assess potential risks and benefits of continued use.
Patients with Hepatic Impairment
The pharmacokinetics of tenofovir following a 300 mg dose of tenofovir disoproxil fumarate have been studied in non-HIV infected subjects with moderate to severe hepatic impairment. There were no substantial alterations in tenofovir pharmacokinetics in subjects with hepatic impairment compared with unimpaired subjects. The pharmacokinetics of emtricitabine and tenofovir disoproxil fumarate or emtricitabine have not been studied in subjects with hepatic impairment; however, emtricitabine is not significantly metabolized by liver enzymes, so the impact of liver impairment should be limited.
Assessment of Drug Interactions
The steady state pharmacokinetics of emtricitabine and tenofovir were unaffected when emtricitabine and tenofovir disoproxil fumarate were administered together versus each agent dosed alone.
In vitro studies and clinical pharmacokinetic drug-drug interaction trials have shown that the potential for CYP mediated interactions involving emtricitabine and tenofovir with other medicinal products is low.
No clinically significant drug interactions have been observed between emtricitabine and famciclovir, indinavir, stavudine, tenofovir disoproxil fumarate, and zidovudine (see Tables 7 and 8). Similarly, no clinically significant drug interactions have been observed between tenofovir disoproxil fumarate and efavirenz, methadone, nelfinavir, oral contraceptives, or ribavirin in trials conducted in healthy volunteers (see Tables 9 and 10).


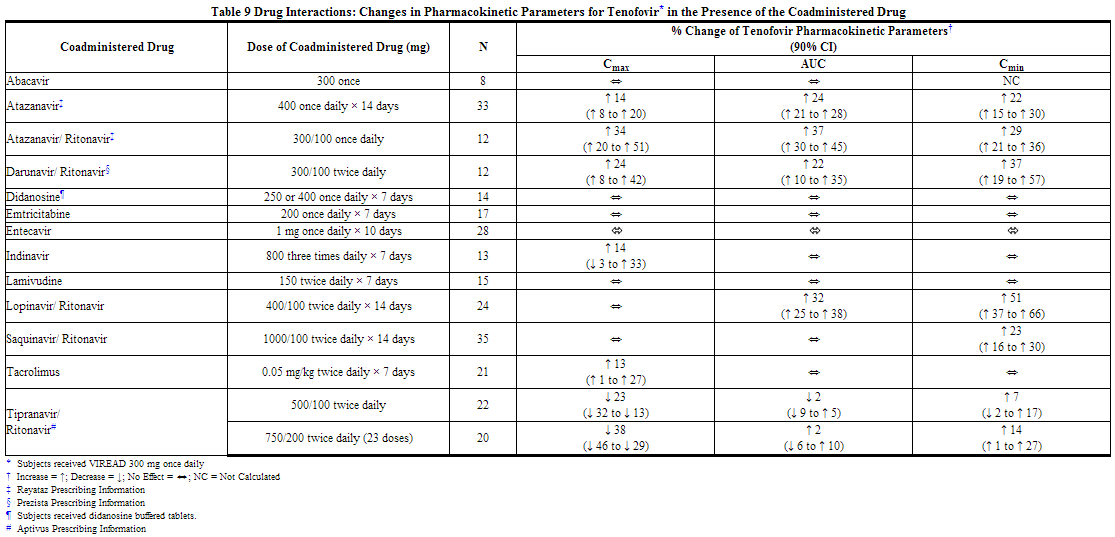

Coadministration of tenofovir disoproxil fumarate with didanosine results in changes in the pharmacokinetics of didanosine that may be of clinical significance. Concomitant dosing of tenofovir disoproxil fumarate with didanosine enteric-coated capsules significantly increases the Cmax and AUC of didanosine. When didanosine 250 mg enteric-coated capsules were administered with tenofovir disoproxil fumarate, systemic exposures of didanosine were similar to those seen with the 400 mg enteric-coated capsules alone under fasted conditions. The mechanism of this interaction is unknown. See Drug Interactions (7.1) regarding use of didanosine with tenofovir disoproxil fumarate .
Nonclinical Toxicology
Carcinogenesis, Mutagenesis, Impairment of Fertility
Emtricitabine
In long-term oral carcinogenicity studies of emtricitabine, no drug-related increases in tumor incidence were found in mice at doses up to 750 mg/kg/day (26 times the human systemic exposure at the therapeutic dose of 200 mg/day) or in rats at doses up to 600 mg/kg/day (31 times the human systemic exposure at the therapeutic dose).
Emtricitabine was not genotoxic in the reverse mutation bacterial test (Ames test), mouse lymphoma or mouse micronucleus assays.
Emtricitabine did not affect fertility in male rats at approximately 140-fold or in male and female mice at approximately 60-fold higher exposures (AUC) than in humans given the recommended 200 mg daily dose. Fertility was normal in the offspring of mice exposed daily from before birth (in utero) through sexual maturity at daily exposures (AUC) of approximately 60-fold higher than human exposures at the recommended 200 mg daily dose.
Tenofovir Disoproxil Fumarate
Long-term oral carcinogenicity studies of tenofovir disoproxil fumarate in mice and rats were carried out at exposures up to approximately 16 times (mice) and 5 times (rats) those observed in humans at the therapeutic dose for HIV-1 infection. At the high dose in female mice, liver adenomas were increased at exposures 16 times that in humans. In rats, the study was negative for carcinogenic findings at exposures up to 5 times that observed in humans at the therapeutic dose.
Tenofovir disoproxil fumarate was mutagenic in the in vitro mouse lymphoma assay and negative in an in vitro bacterial mutagenicity test (Ames test). In an in vivo mouse micronucleus assay, tenofovir disoproxil fumarate was negative when administered to male mice.
There were no effects on fertility, mating performance or early embryonic development when tenofovir disoproxil fumarate was administered to male rats at a dose equivalent to 10 times the human dose based on body surface area comparisons for 28 days prior to mating and to female rats for 15 days prior to mating through day seven of gestation. There was, however, an alteration of the estrous cycle in female rats.
Animal Toxicology and/or Pharmacology
Tenofovir and tenofovir disoproxil fumarate administered in toxicology studies to rats, dogs and monkeys at exposures (based on AUCs) greater than or equal to 6-fold those observed in humans caused bone toxicity. In monkeys the bone toxicity was diagnosed as osteomalacia. Osteomalacia observed in monkeys appeared to be reversible upon dose reduction or discontinuation of tenofovir. In rats and dogs, the bone toxicity manifested as reduced bone mineral density. The mechanism(s) underlying bone toxicity is unknown.
Evidence of renal toxicity was noted in 4 animal species. Increases in serum creatinine, BUN, glycosuria, proteinuria, phosphaturia, and/or calciuria and decreases in serum phosphate were observed to varying degrees in these animals. These toxicities were noted at exposures (based on AUCs) 2–20 times higher than those observed in humans. The relationship of the renal abnormalities, particularly the phosphaturia, to the bone toxicity is not known.
Clinical Studies
Clinical Study 934 supports the use of emtricitabine and tenofovir disoproxil fumarate tablets for the treatment of HIV-1 infection. Additional data in support of the use of emtricitabine and tenofovir disoproxil fumarate are derived from clinical Study 903, in which lamivudine and tenofovir disoproxil fumarate (tenofovir DF) were used in combination in treatment-naive adults, and clinical Study 303 in which emtricitabine and lamivudine demonstrated comparable efficacy, safety and resistance patterns as part of multidrug regimens. For additional information about these trials, please consult the prescribing information for tenofovir DF and emtricitabine. The iPrEx study and Partners PrEP study support the use of emtricitabine and tenofovir disoproxil fumarate to help reduce the risk of acquiring HIV-1.
Study 934
Data through 144 weeks are reported for Study 934, a randomized, open-label, active-controlled multicenter trial comparing emtricitabine + tenofovir DF administered in combination with efavirenz versus zidovudine/lamivudine fixed-dose combination administered in combination with efavirenz in 511 antiretroviral-naive subjects. From Weeks 96 to 144 of the trial, subjects received emtricitabine and tenofovir disoproxil fumarate with efavirenz in place of emtricitabine + tenofovir DF with efavirenz. Subjects had a mean age of 38 years (range 18–80), 86% were male, 59% were Caucasian and 23% were Black. The mean baseline CD4+ cell count was 245 cells/mm3 (range 2–1191) and median baseline plasma HIV-1 RNA was 5.01 log10 copies/mL (range 3.56–6.54). Subjects were stratified by baseline CD4+ cell count (< or ≥200 cells/mm3); 41% had CD4+ cell counts <200 cells/mm3 and 51% of subjects had baseline viral loads >100,000 copies/mL. Treatment outcomes through 48 and 144 weeks for those subjects who did not have efavirenz resistance at baseline are presented in Table 11.

Through Week 48, 84% and 73% of subjects in the emtricitabine + tenofovir DF group and the zidovudine/lamivudine group, respectively, achieved and maintained HIV-1 RNA <400 copies/mL (71% and 58% through Week 144). The difference in the proportion of subjects who achieved and maintained HIV-1 RNA <400 copies/mL through 48 weeks largely results from the higher number of discontinuations due to adverse events and other reasons in the zidovudine/lamivudine group in this open-label trial. In addition, 80% and 70% of subjects in the emtricitabine + tenofovir DF group and the zidovudine/lamivudine group, respectively, achieved and maintained HIV-1 RNA <50 copies/mL through Week 48 (64% and 56% through Week 144). The mean increase from baseline in CD4+ cell count was 190 cells/mm3 in the emtricitabine + tenofovir DF group and 158 cells/mm3 in the zidovudine/lamivudine group at Week 48 (312 and 271 cells/mm3 at Week 144).
Through 48 weeks, 7 subjects in the emtricitabine + tenofovir DF group and 5 subjects in the zidovudine/lamivudine group experienced a new CDC Class C event (10 and 6 subjects through 144 weeks).
iPrEx Trial
The iPrEx trial was a randomized double-blind placebo-controlled multinational study evaluating emtricitabine and tenofovir disoproxil fumarate in 2499 HIV-seronegative men or transgender women who have sex with men and with evidence of high risk behavior for HIV-1 infection. Evidence of high risk behavior included any one of the following reported to have occurred up to six months prior to study screening: no condom use during anal intercourse with an HIV-1 positive partner or a partner of unknown HIV status; anal intercourse with more than 3 sex partners; exchange of money, gifts, shelter or drugs for anal sex; sex with male partner and diagnosis of sexually transmitted infection; no consistent use of condoms with sex partner known to be HIV-1 positive.
All subjects received monthly HIV-1 testing, risk-reduction counseling, condoms and management of sexually transmitted infections. Of the 2499 enrolled, 1251 received emtricitabine and tenofovir disoproxil fumarate and 1248 received placebo. The mean age of subjects was 27 years, 5% were Asian, 9% Black, 18% White, and 72% Hispanic/Latino.
Subjects were followed for 4237 person-years. The primary outcome measure for the study was the incidence of documented HIV seroconversion. At the end of treatment, emergent HIV-1 seroconversion was observed in 131 subjects, of which 48 occurred in the emtricitabine and tenofovir disoproxil fumarate group and 83 occurred in the placebo group, indicating a 42% (95% CI: 18% to 60%) reduction in risk. Risk reduction was found to be higher (53%; 95% CI: 34% to 72%) among subjects who reported previous unprotected anal intercourse (URAI) at screening (732 and 753 subjects reported URAI within the last 12 weeks at screening in the emtricitabine and tenofovir disoproxil fumarate and placebo groups, respectively). In a post-hoc case control study of plasma and intracellular drug levels in about 10% of study subjects, risk reduction appeared to be the greatest in subjects with detectable intracellular tenofovir. Efficacy was therefore strongly correlated with adherence.
Partners PrEP Trial
The Partners PrEP trial was a randomized, double-blind, placebo-controlled 3 arm trial conducted in 4758 serodiscordant heterosexual couples in Kenya and Uganda to evaluate the efficacy and safety of TDF (N=1589) and FTC/TDF (N=1583) versus (parallel comparison) placebo (N=1586), in preventing HIV-1 acquisition by the uninfected partner.
All subjects received monthly HIV-1 testing, evaluation of adherence, assessment of sexual behavior, and safety evaluations. Women were also tested monthly for pregnancy. Women who became pregnant during the trial had study drug interrupted for the duration of the pregnancy and while breastfeeding. The uninfected partner subjects were predominantly male (61–64% across study drug groups), and had a mean age of 33–34 years.
Following 7827 person-years of follow up, 82 emergent HIV-1 seroconversions were reported, with an overall observed seroincidence rate of 1.05 per 100 person-years. Of the 82 seroconversions, 13 and 52 occurred in partner subjects randomized to emtricitabine and tenofovir disoproxil fumarate and placebo, respectively. Two of the 13 seroconversions in the emtricitabine and tenofovir disoproxil fumarate arm and 3 of the 52 seroconversions in the placebo arm occurred in women during treatment interruptions for pregnancy. The risk reduction for emtricitabine and tenofovir disoproxil fumarate relative to placebo was 75% (95% CI: 55% to 87%). In a post-hoc case control study of plasma drug levels in about 10% of study subjects, risk reduction appeared to be the greatest in subjects with detectable plasma tenofovir. Efficacy was therefore strongly correlated with adherence.
How Supplied
The blue, capsule-shaped, film-coated, tablets contain 200 mg of emtricitabine and 300 mg of tenofovir disoproxil fumarate (which is equivalent to 245 mg of tenofovir disoproxil), are debossed with "GILEAD" on one side and with "701" on the other side, and are available in unit of use bottles [containing a dessicant (silica gel canister or sachet) and closed with a child-resistant closure] of 30 tablets (NDC 61958-0701-1).
Storage
Store at 25 °C (77 °F), excursions permitted to 15 °C –30 °C (59 °F –86 °F) (see USP Controlled Room Temperature).
- Keep container tightly closed.
- Dispense only in original container.
- Do not use if seal over bottle opening is broken or missing.
Images
Drug Images
{{#ask: Page Name::Emtricitabine and tenofovir disoproxil fumarate |?Pill Name |?Drug Name |?Pill Ingred |?Pill Imprint |?Pill Dosage |?Pill Color |?Pill Shape |?Pill Size (mm) |?Pill Scoring |?NDC |?Drug Author |format=template |template=DrugPageImages |mainlabel=- |sort=Pill Name }}
Package and Label Display Panel
{{#ask: Label Page::Emtricitabine and tenofovir disoproxil fumarate |?Label Name |format=template |template=DrugLabelImages |mainlabel=- |sort=Label Page }}
Patient Counseling Information
As a part of patient counseling, healthcare providers must review the emtricitabine and tenofovir disoproxil fumarate Medication Guide with every uninfected individual taking emtricitabine and tenofovir disoproxil fumarate to reduce the risk of acquiring HIV.
Important Information for All Patients and Uninfected Individuals
Advise patients and uninfected individuals that:
- The long term effects of emtricitabine and tenofovir disoproxil fumarate are unknown.
- Emtricitabine and tenofovir disoproxil fumarate tablets are for oral ingestion only.
- Patients and uninfected individuals should not discontinue emtricitabine and tenofovir disoproxil fumarate without first informing their physicians.
- Patients and uninfected individuals should remain under the care of a physician when using emtricitabine and tenofovir disoproxil fumarate.
- It is important to take emtricitabine and tenofovir disoproxil fumarate on a regular dosing schedule to avoid missing doses.
- Lactic acidosis and severe hepatomegaly with steatosis, including fatal cases, have been reported. Treatment with emtricitabine and tenofovir disoproxil fumarate should be suspended in patients or uninfected individuals who develop clinical symptoms suggestive of lactic acidosis or pronounced hepatotoxicity (including nausea, vomiting, unusual or unexpected stomach discomfort, and weakness).
- Severe acute exacerbations of hepatitis B have been reported in patients who are coinfected with hepatitis B virus (HBV) and HIV-1 and have discontinued emtricitabine and tenofovir disoproxil fumarate. Before initiating emtricitabine and tenofovir disoproxil fumarate, test all patients and uninfected individuals for HBV. All patients who are infected with HBV need close medical follow-up for several months after stopping emtricitabine and tenofovir disoproxil fumarate to monitor for exacerbations of hepatitis.
- Renal impairment, including cases of acute renal failure and Fanconi syndrome, has been reported in association with the use of tenofovir disoproxil fumarate. Emtricitabine and tenofovir disoproxil fumarate should be avoided with concurrent or recent use of a nephrotoxic agent (e.g., high-dose or multiple NSAIDs). Dosing interval of emtricitabine and tenofovir disoproxil fumarate may need adjustment in HIV-1 infected patients with renal impairment. Emtricitabine and tenofovir disoproxil fumarate for a PrEP indication should not be used in HIV-1 uninfected individuals if estimated creatinine clearance is less than 60 mL/min. If a decrease in estimated creatinine clearance is observed in uninfected individuals while using emtricitabine and tenofovir disoproxil fumarate for PrEP, evaluate potential causes and re-assess potential risks and benefits of continued use.
- Do not administer emtricitabine and tenofovir disoproxil fumarate with efavirenz/emtricitabine/tenofovir disoproxil fumarate, emtricitabine/rilpivirine/tenofovir disoproxil fumarate, emtricitabine, elvitegravir/cobicistat/tenofovir/emtricitabine, or tenofovir disoproxil fumarate; or with drugs containing lamivudine, including Combivir (lamivudine/zidovudine), Epivir or Epivir-HBV (lamivudine), Epzicom (abacavir sulfate/lamivudine), or Trizivir (abacavir sulfate/lamivudine/zidovudine).
- Do not administer emtricitabine and tenofovir disoproxil fumarate with adefovir dipivoxil.
- Decreases in bone mineral density have been observed with the use of tenofovir disoproxil fumarate or emtricitabine and tenofovir disoproxil fumarate. Consider bone monitoring in patients and uninfected individuals who have a history of pathologic bone fracture or at risk for osteopenia.
- Patients and uninfected individuals should avoid doing things that can spread HIV-1 or HBV infection.
- Do not share needles or other injection equipment.
- Do not share personal items that can have blood or body fluids on them, like toothbrushes and razor blades.
- Do not have any kind of sex without protection. Always practice safer sex by using a latex or polyurethane condom to lower the chance of sexual contact with semen, vaginal secretions, or blood.
- Patients and uninfected individuals should not breastfeed because the drugs in emtricitabine and tenofovir disoproxil fumarate can be passed to the baby in breast milk, and it is not known whether they can harm the baby. HIV-positive women should also not breastfeed because of the risk of passing the HIV-1 virus to the baby.
Treatment of HIV-1 Infection
When emtricitabine and tenofovir disoproxil fumarate is used in the treatment of HIV-infection, advise patients that:
- Emtricitabine and tenofovir disoproxil fumarate is not a cure for HIV-1 infection and patients may continue to experience illnesses associated with HIV-1 infection, including opportunistic infections.
- It is important to take emtricitabine and tenofovir disoproxil fumarate in a regular dosing schedule with combination therapy to avoid missing doses.
- All patients with HIV-1 should be tested for hepatitis B virus (HBV) before initiating and monitored after discontinuing taking emtricitabine and tenofovir disoproxil fumarate.
Pre-Exposure Prophylaxis
When emtricitabine and tenofovir disoproxil fumarate is used to reduce the risk of acquiring HIV-1, advise uninfected individuals about the importance of the following:
- Confirming that they are HIV-negative before starting to take emtricitabine and tenofovir disoproxil fumarate to reduce the risk of acquiring HIV-1.
- Emtricitabine and tenofovir disoproxil fumarate should only be used as part of a complete prevention strategy including other prevention measures. In clinical trials, emtricitabine and tenofovir disoproxil fumarate only protected some subjects from acquiring HIV-1.
- Using condoms consistently and correctly to lower the chance of sexual contact with any body fluids such as semen, vaginal secretions, or blood.
- Knowing their HIV status and the status of their partner(s).
- Getting tested regularly (at least every 3 months) for HIV-1 and ask their partner(s) to get tested as well.
- HIV-1 resistance substitutions may emerge in individuals with undetected HIV-1 infection who are taking emtricitabine and tenofovir disoproxil fumarate, because emtricitabine and tenofovir disoproxil fumarate alone does not constitute a complete regimen for HIV-1 treatment.
- Reporting any symptoms of acute HIV-1 infection (flu-like symptoms) to their healthcare provider immediately.
- Signs and symptoms of acute infection include: fever, headache, fatigue, arthralgia, vomiting, myalgia, diarrhea, pharyngitis, rash, night sweats, and adenopathy (cervical and inguinal).
- Getting tested for other sexually transmitted infections such as syphilis and gonorrhea that may facilitate HIV-1 transmission.
- Learning about sexual risk behavior and getting support to help reduce sexual risk behavior.
- Taking emtricitabine and tenofovir disoproxil fumarate on a regular dosing schedule and strictly adhere to the recommended dosing schedule to reduce the risk of acquiring HIV-1. Uninfected individuals who miss doses are at greater risk of acquiring HIV-1 than those who do not miss doses.
- Women who are pregnant should learn about the risks and benefits of emtricitabine and tenofovir disoproxil fumarate to reduce the risk of acquiring HIV-1 during their pregnancy.
- Encourage use of the Agreement Form for Initiating emtricitabine and tenofovir disoproxil fumarate for PrEP of Sexually Acquired HIV-1 Infection.
Precautions with Alcohol
Alcohol-Emtricitabine and tenofovir disoproxil fumarate interaction has not been established. Talk to your doctor about the effects of taking alcohol with this medication.
Brand Names
- Truvada
Look-Alike Drug Names
There is limited information regarding Emtricitabine and tenofovir disoproxil fumarate Look-Alike Drug Names in the drug label.
Drug Shortage
Price
References
The contents of this FDA label are provided by the National Library of Medicine.
{{#subobject:
|Label Page=Emtricitabine and tenofovir disoproxil fumarate |Label Name=Emtricitabine and tenofovir disoproxil fumarate Package.png
}}