Torsades de pointes overview
| https://https://www.youtube.com/watch?v=oFUZeNCox8Q%7C350}} |
|
Torsades de pointes Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Torsades de pointes overview On the Web |
|
American Roentgen Ray Society Images of Torsades de pointes overview |
|
Risk calculators and risk factors for Torsades de pointes overview |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Charmaine Patel, M.D. [2]
Overview
Torsade de pointes, in French means "Twisting of the Points". It is characterized by a polymorphic ventricular tachycardia and can occur in the congenital long QT syndromes, electrolyte abnormalities (hypomagnesemia, hypokalemia), usage of certain drugs like antiarrhythmic (quinidine), nonsedating antihistamines (terfenadine); antibiotics (erythromycin) and neuroleptics (thioridazine).
Historical Perspective
The term "torsade de pointes" was first described by Dessertenne in 1966, based on the characteristic "twisting" pattern of ventricular tachycardia seen on EKG.
Pathophysiology
Torsades de pointes is defined as the presence of polymorphic ventricular tachycardia with a prolonged QT segment on EKG. It is characterized by a constantly changing rhythm amplitude which comes from the ventricular depolarizing waves constantly shifting its axis. The underlying mechanism is thought to be triggered activity arising as a consequence of early after-depolarizations. During Torsade de pointes the ventricles depolarize in a circular fashion resulting in QRS complexes with a continuously turning heart axis around the baseline (hence the name Torsade de Pointes).
Causes
Common causes for torsades de pointes include hypomagnesemia and hypokalemia. It is commonly seen in malnourished individuals and chronic alcoholics. Drug interactions such as erythromycin or Avelox, taken concomitantly with inhibitors like nitroimidazole, diarrhea, dietary supplements, and various medications like methadone, lithium, tricyclic antidepressants or phenothiazines may also contribute to causing torsades de pointes.
Differentiating Torsades de pointes from other Conditions
Torsades de pointes should be differentiated from other conditions or disorders that may present in a similar way, such as other arrhythmias, drug toxicity, syncope and other cardiac conditions.
Risk Factors
Long QT syndrome is a risk factor for developing torsades de pointes, and can either be inherited as congenital mutations of ion channels carrying the cardiac impulse/action potential, or acquired as a result of drugs that block these cardiac ion currents. Other risk factors include electrolyte abnormalities, heart failure, left ventricular hypertrophy, female gender or renal and liver failure. Being on certain medications also pose a risk for developing torsades de pointes.
Natural History, Complications and Prognosis
Although Torsades de Pointes (TdP) is a rare ventricular arrhythmia, it can degenerate into ventricular fibrillation, leading to death without rapid medical intervention.
Diagnosis
History and Symptoms
Patients who are being evaluated for torsades de pointes should be asked about a history of syncope, and family history of long QT syndrome, sudden cardiac death, or sudden infant death syndrome. Torsades de pointes is associated with a fall in blood pressure, which often gives rise to syncopal symptoms. The patient may experience nausea, shortness of breath, dizziness,chest pain, and possibly ventricular fibrillation and sudden cardiac death.
Physical Examination
The physical exam during or directly after an episode of torsade de pointes, may reveal pallor and diaphoresis, loss of consciousness, and bradycardia followed by tachycardia.
Laboratory Findings
Laborotory tests obtained in a person with torsade de pointes will vary depending on the most likely etiology for their arrhythmia. Cardiac enzymes and levels of potassium, magnesium and calcium should be obtained.
Electrocardiogram
The EKG is the main diagnostic tool for torsades de pointes. EKG will show that the QRS complexes seem to twist around the horizontal isoelectric axis. Polymorphic ventricular tachycardia is distinguished from torsades de pointes by the absence of prolongation of the QT segment.
The ECG below is the characteristic tracing showing the "twisting" (blue line) of Torsade de pointes
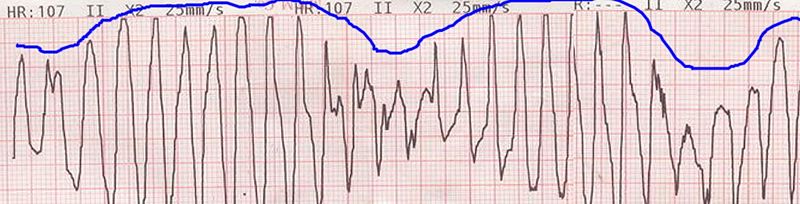
Treatment
An understanding of the pathophysiology has led to development of treatment modalities like pacing, isoproterenol and drugs like magnesium and beta blockers.If the episode of does not terminate on its own and degenerates into ventricular fibrillation, cardioversion is required.