The Physical Examination in Cardiovascular Disease: The Pulse
| The Pulse | |
 | |
|---|---|
| Palpation of the right radial artery. (Image courtesy of Charlie Goldberg, M.D., UCSD School of Medicine and VA Medical Center, San Diego, CA) |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]
Overview
The pulse can be measured at any place where there is a large artery (e.g. carotid, femoral, or simply by listening over the heart), though for the sake of convenience it is generally done by palpating the radial artery's impulse. You may find it helpful to feel both radial arteries simultaneously, doubling the sensory input and helping to insure the accuracy of your measurements. Place the tips of your index and middle fingers just proximal to the patients wrist on the thumb side, orienting them so that they are both over the length of the vessel.
The pulse can be characterized by
- The rate: Measure the rate of the pulse (recorded in beats per minute). Count for 30 seconds and multiply by 2 (or 15 seconds x 4). If the rate is particularly slow or fast, it is probably best to measure for a full 60 seconds in order to minimize the impact of any error in recording over shorter periods of time. Normal is between 60 and 100.
- The rhythm or regularity: Is the time between beats constant? In the normal setting, the heart rate should appear metronomic. Irregular rhythms, however, are quite common. If the pattern is entirely chaotic with no discernable pattern, it is referred to as irregularly irregular and likely represents atrial fibrillation. Extra beats can also be added into the normal pattern, in which case the rhythm is described as regularly irregular. This may occur, for example, when impulses originating from the ventricle are interposed at regular junctures on the normal rhythm. If the pulse is irregular, it's a good idea to verify the rate by listening over the heart. This is because certain rhythm disturbances do not allow adequate ventricular filling with each beat. The resultant systole may generate a rather small stroke volume whose impulse is not palpable in the periphery.
- The strength: Does the pulse volume (i.e. the subjective sense of fullness) feel normal? This reflects changes in stroke volume. In the setting of hypovolemia, for example, the pulse volume is relatively low (aka weak or thready). There may even be beat to beat variation in the volume, occurring occasionally with systolic heart failure.
- The symmetry
Rate
Rate, expressed in beats per minute (bpm), is measured by counting over a timed period of 60 seconds. In patients with atrial fibrillation the rate should be measured by auscultation at the cardiac apex, because beats that follow very short diastolic intervals may create a 'pulse deficit' by not generating sufficient pressure to be palpable at the radial artery.
This is generally defined as a pulse rate > 100 beats per minute.
This is generally defined as a pulse rate < 60 beats per minute.
Rhythm
Normal sinus rhythm is regular, but in youngs may show phasic variation in rate during respiration (sinus arrhythmia). An irregular rhythm usually indicates atrial fibrillation, but may also be caused by frequent ectopic beats or self-limiting paroxysmal arrhythmias.
Irregulary Irregular
An irregularly irrgular pulse suggests atrial fibrillation or premature atrial contractions PAC.
Strength
A collapsing pulse is a pulse with a fast upstroke and fast downstroke.
Alternating pulse
An alternating pulse (pulsus alternans) is a pulse with alternating high and low systolic peaks, that occurs in severe left ventricular failure but the mechanism of this clinical situation is unknown.
A paradoxical pulse is a pulse with an inspiratory decline in systolic pressure >10 mmHg and occurs in cardiac tamponade, less frequently in constrictive pericarditis and obstructive pulmonary disease. It represents an exaggeration of the normal inspiratory decline in systolic pressure and therefore is not a truly paradoxical pulse.
Symmetry
Symmetry of the palpable arteries (radial, brachial, carotid, femoral, popliteal and pedal) should be confirmed. A reduced or absent pulse indicates an obstruction more proximally in the arterial tree. Coarctation of the aorta causes symmetrical reduction and delay of the femoral artery pulses compared with the radial artery pulses.
Palpation of the radial artery
(Images courtesy of Charlie Goldberg, M.D., UCSD School of Medicine and VA Medical Center, San Diego, CA)
-
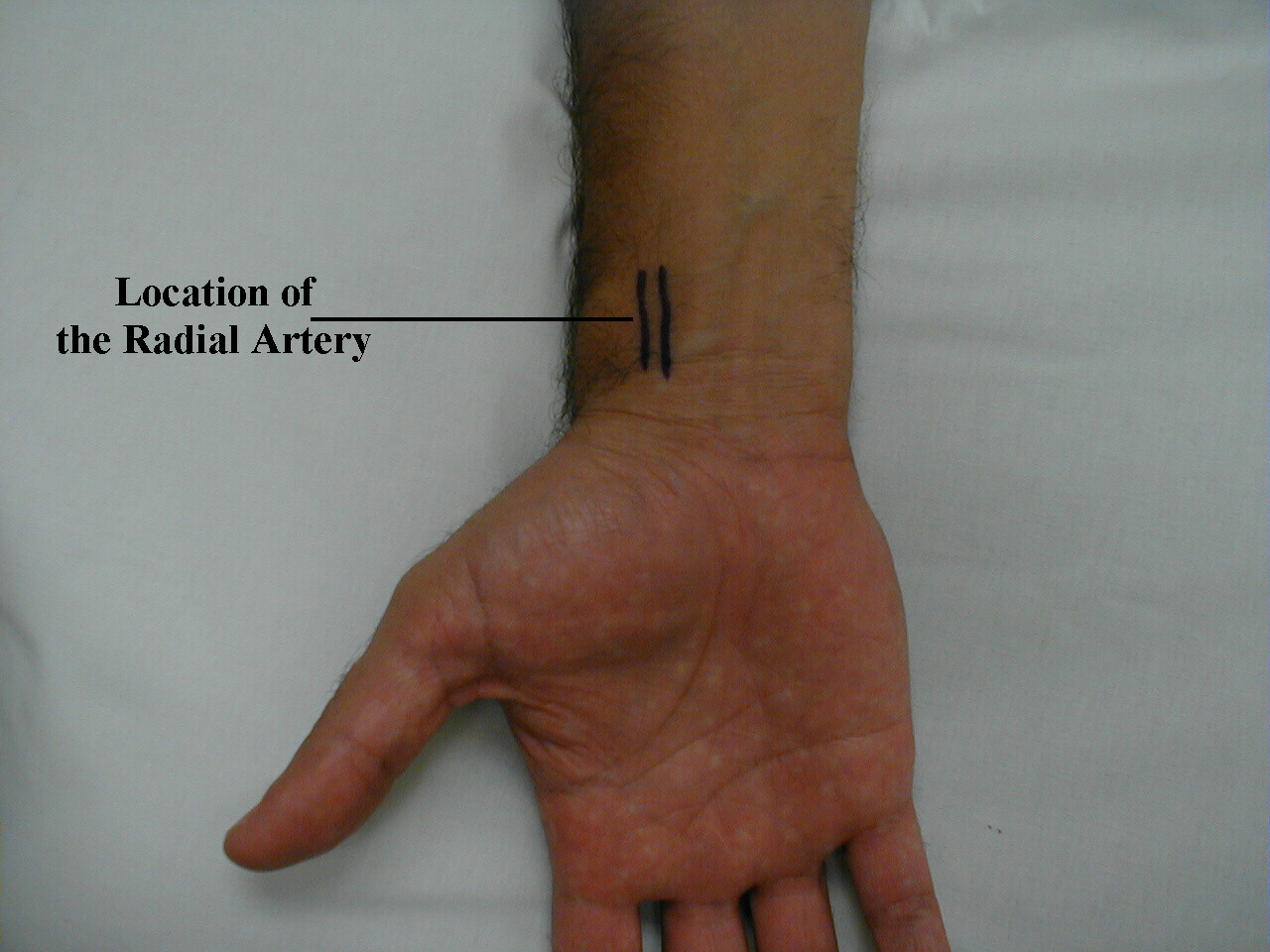
Location of the radial artery: Surface anatomy
-
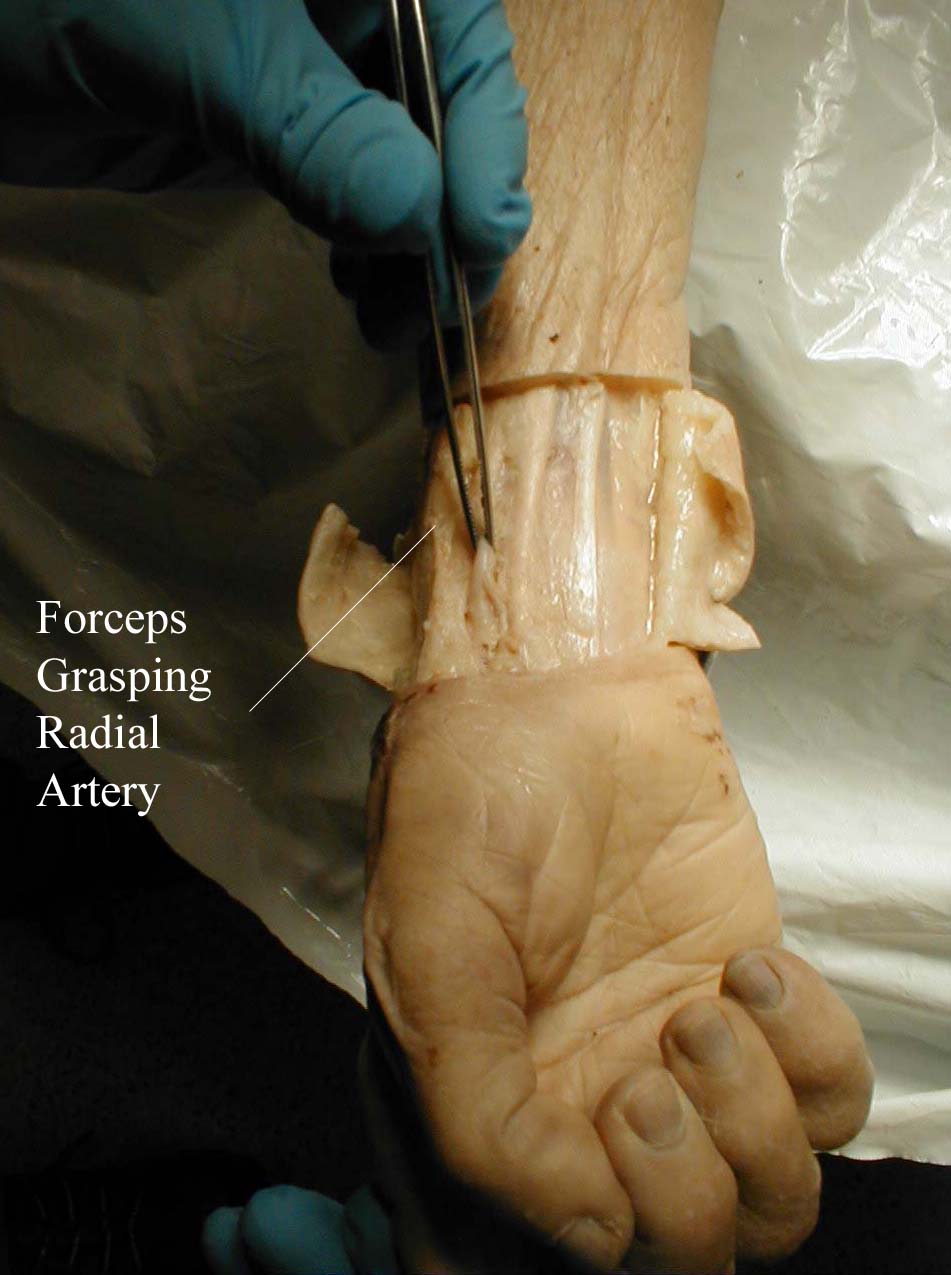
Location of the radial artery: Gross anatomy
-
Palpation of the right radial artery