Nummular dermatitis
Template:DiseaseDisorder infobox
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1];Associate Editor(s)-in-Chief: Kiran Singh, M.D. [2]
Overview
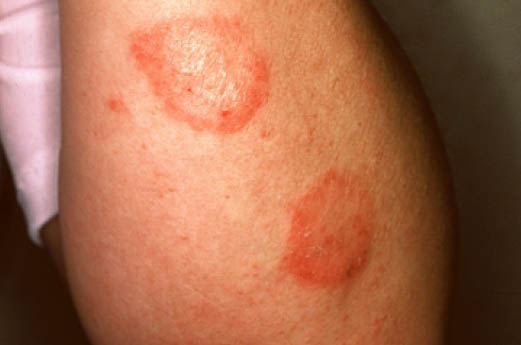
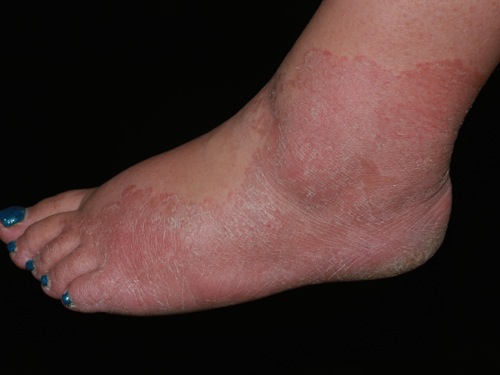
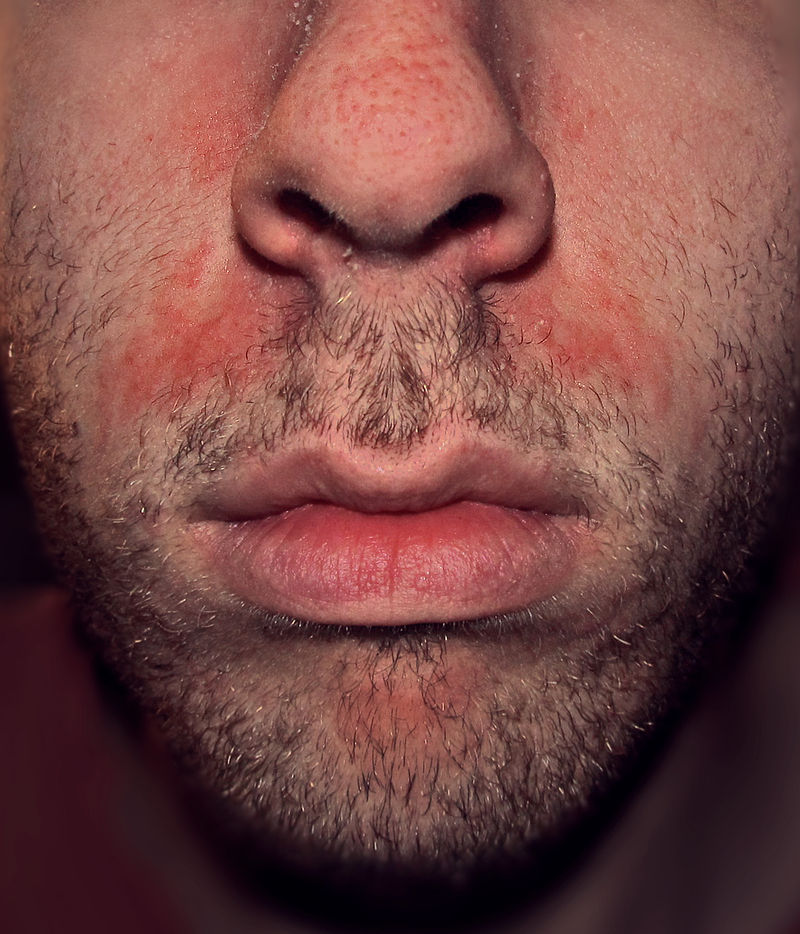
Nummular dermatitis is one of the many forms of dermatitis. Also known as discoid dermatitis, it is characterized by round or oval-shaped itchy lesions. (The name comes from the Latin word "nummus," which means "coin.")
Presentation
The disorder is recurrent and chronic, and may appear at any age, although it is most common in people in their 60's. Nummular dermatitis does not appear to be a genetic condition, is not related to food allergies, and is not contagious.
The coin-shaped patches can affect any part of the body, but the legs and buttocks are the most common areas. Flare-ups are associated with dry skin, so the winter season is a particularly bad time for those with this condition.
Other forms of dermatitis are at risk of developing.[1]
Diagnosis
Physical Examination
Skin
Extremities
-
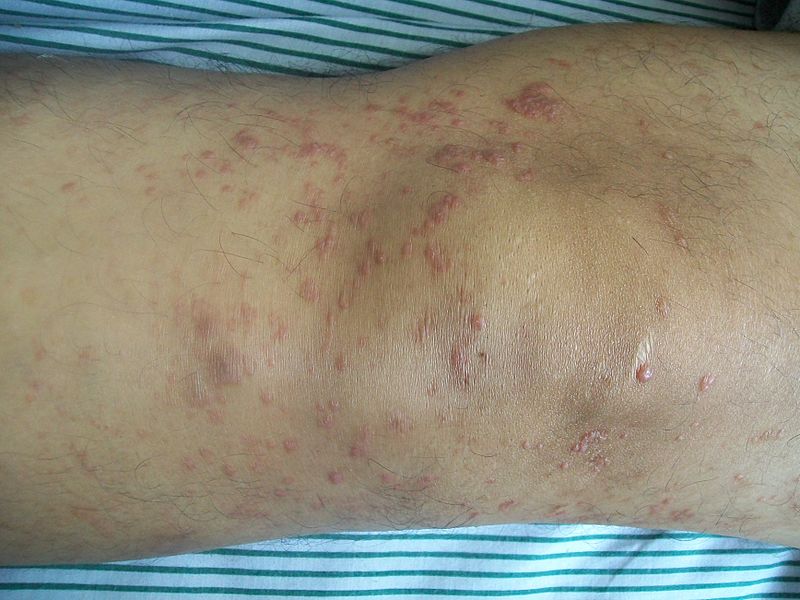
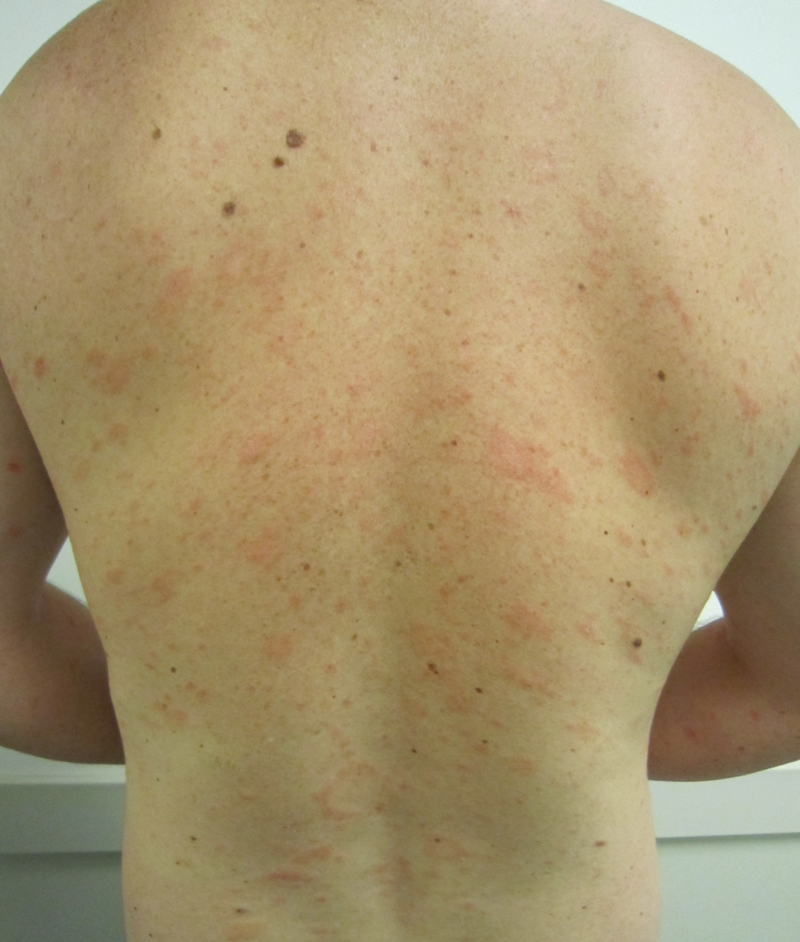
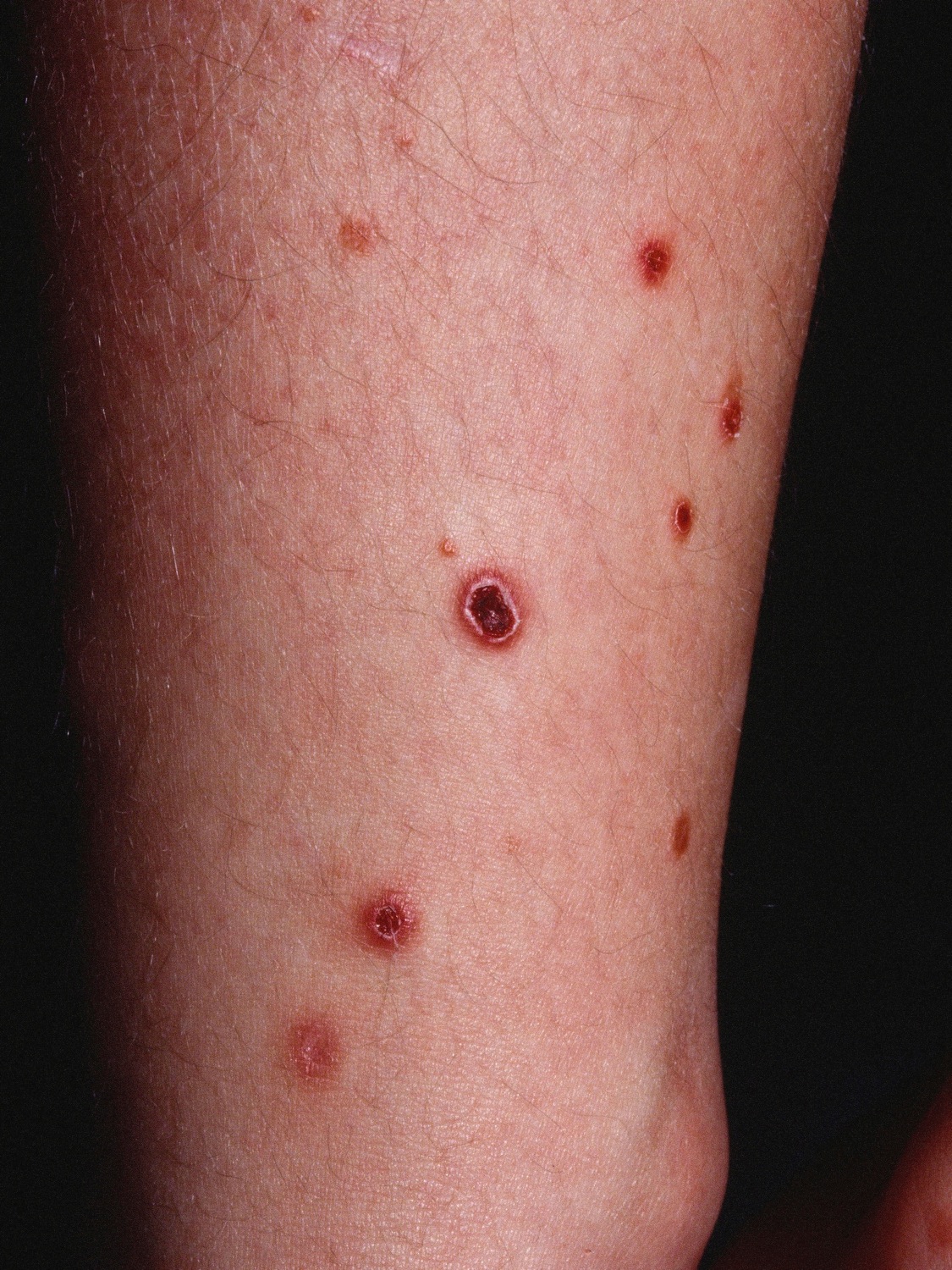
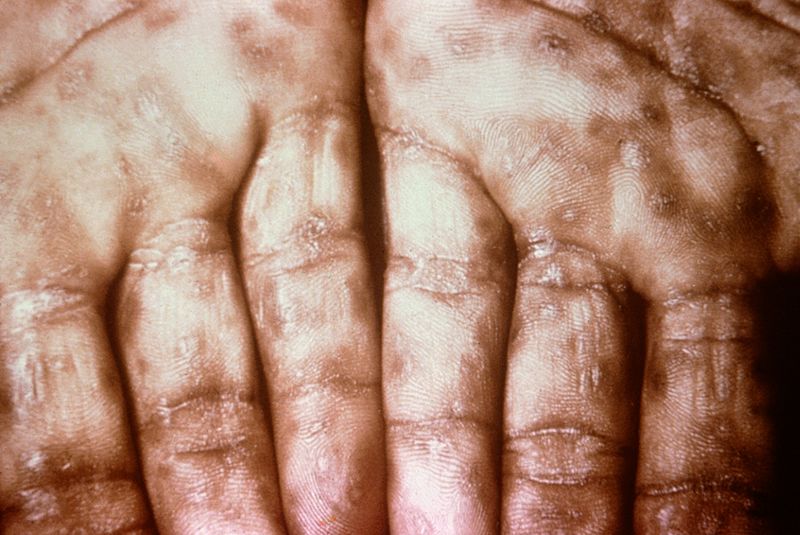
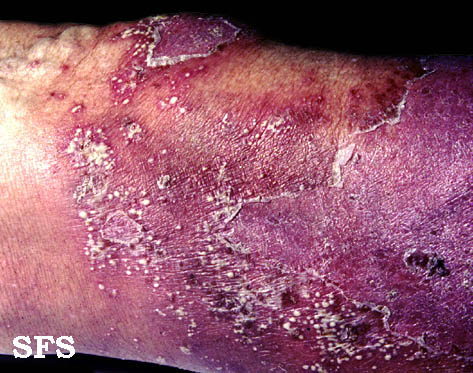
Eczema microbic. Adapted from Dermatology Atlas.[2]
-
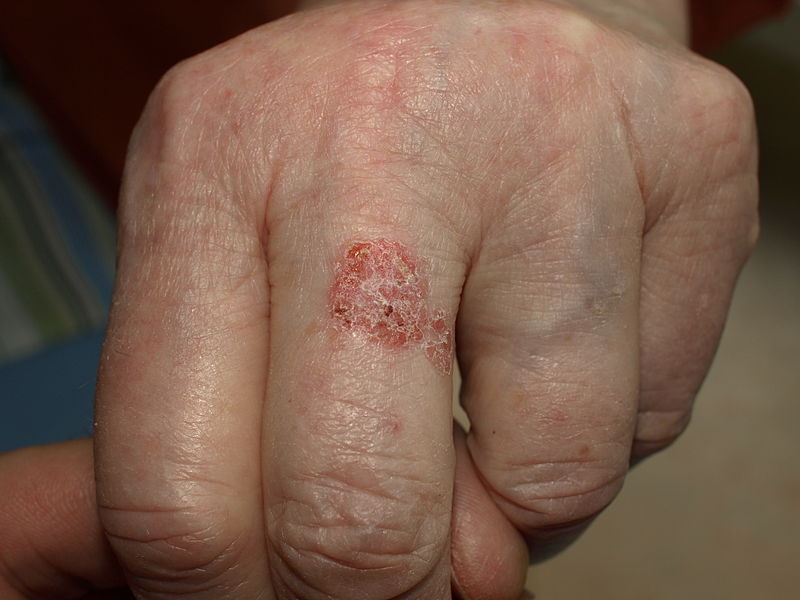
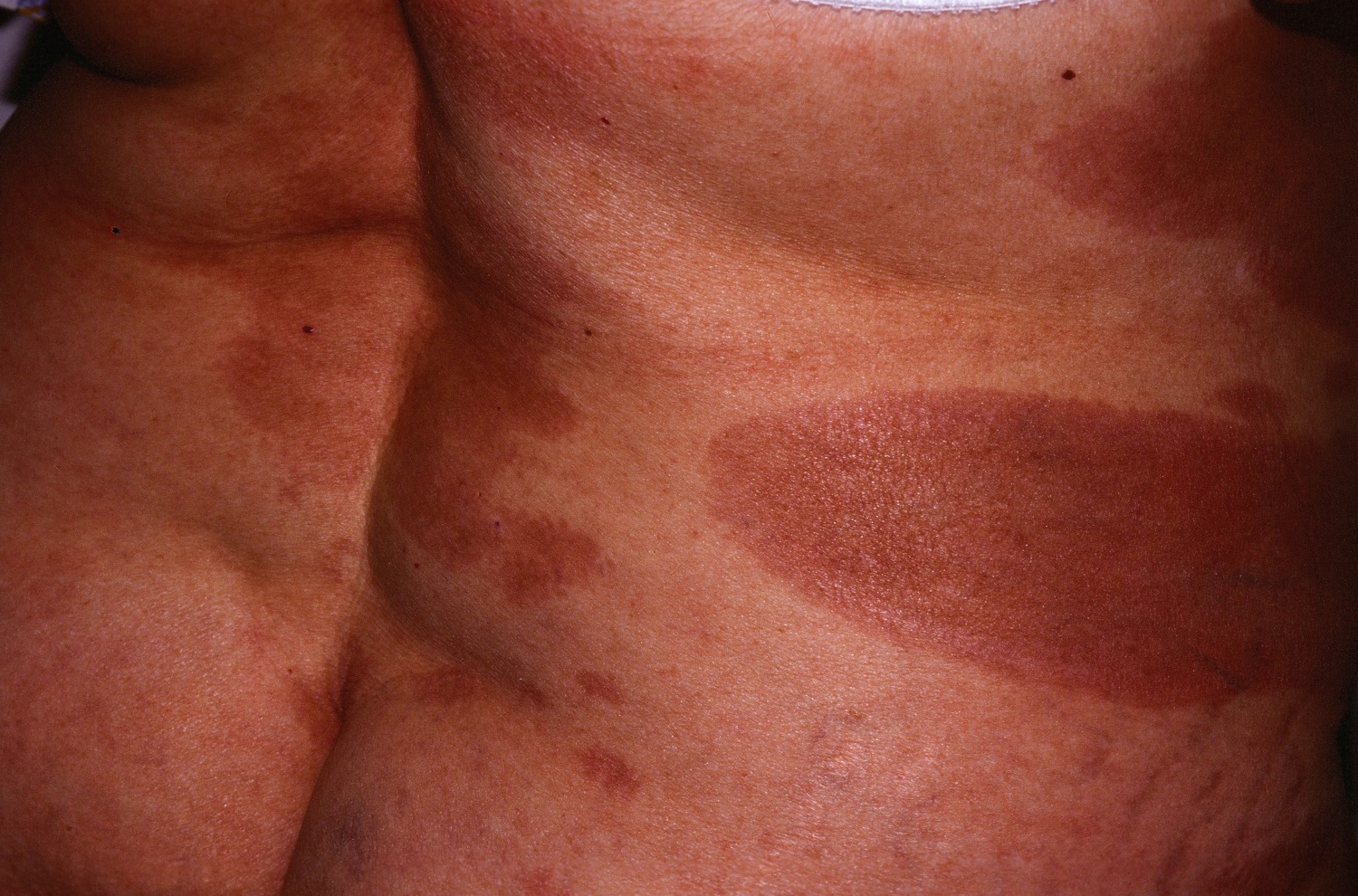
Eczema microbic. Adapted from Dermatology Atlas.[2]
-
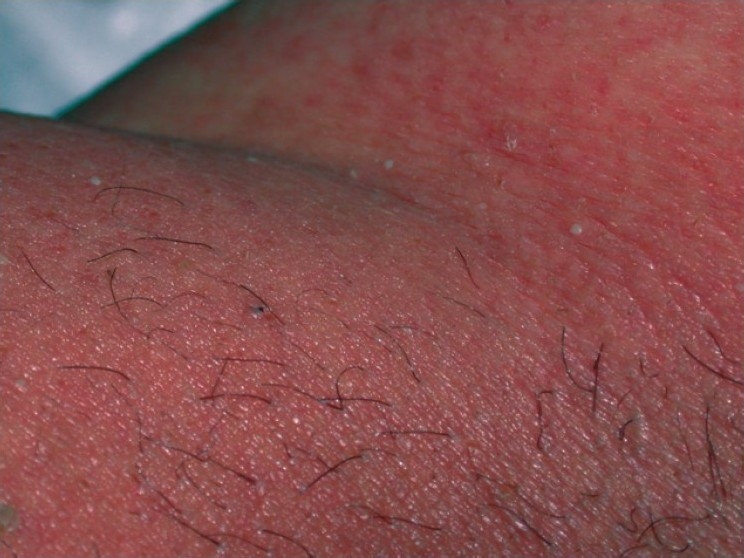
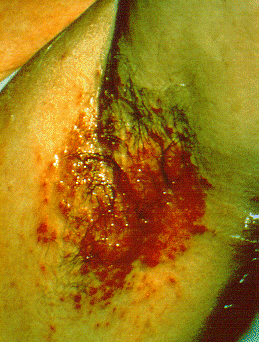
Eczema microbic. Adapted from Dermatology Atlas.[2]
-
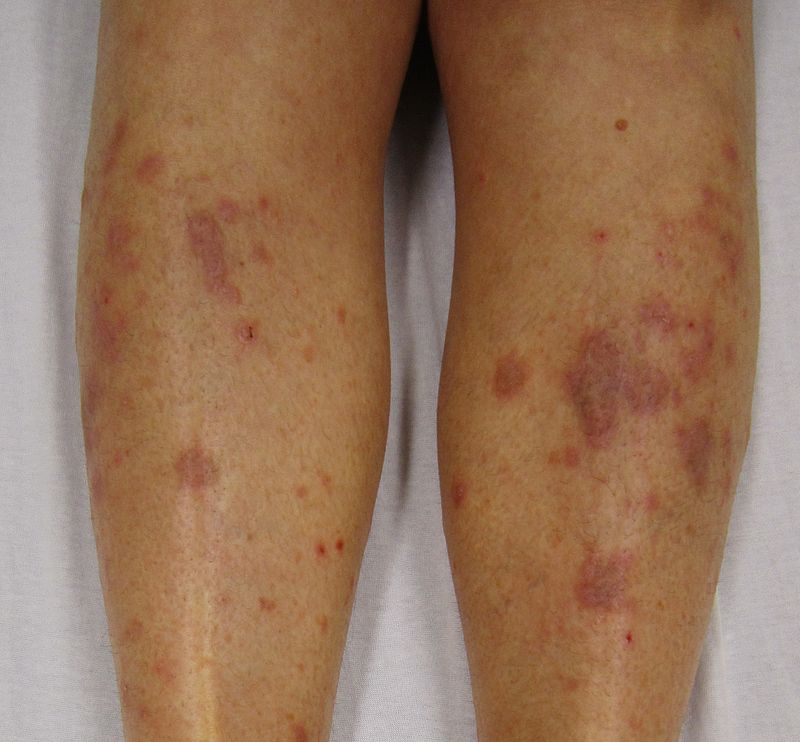
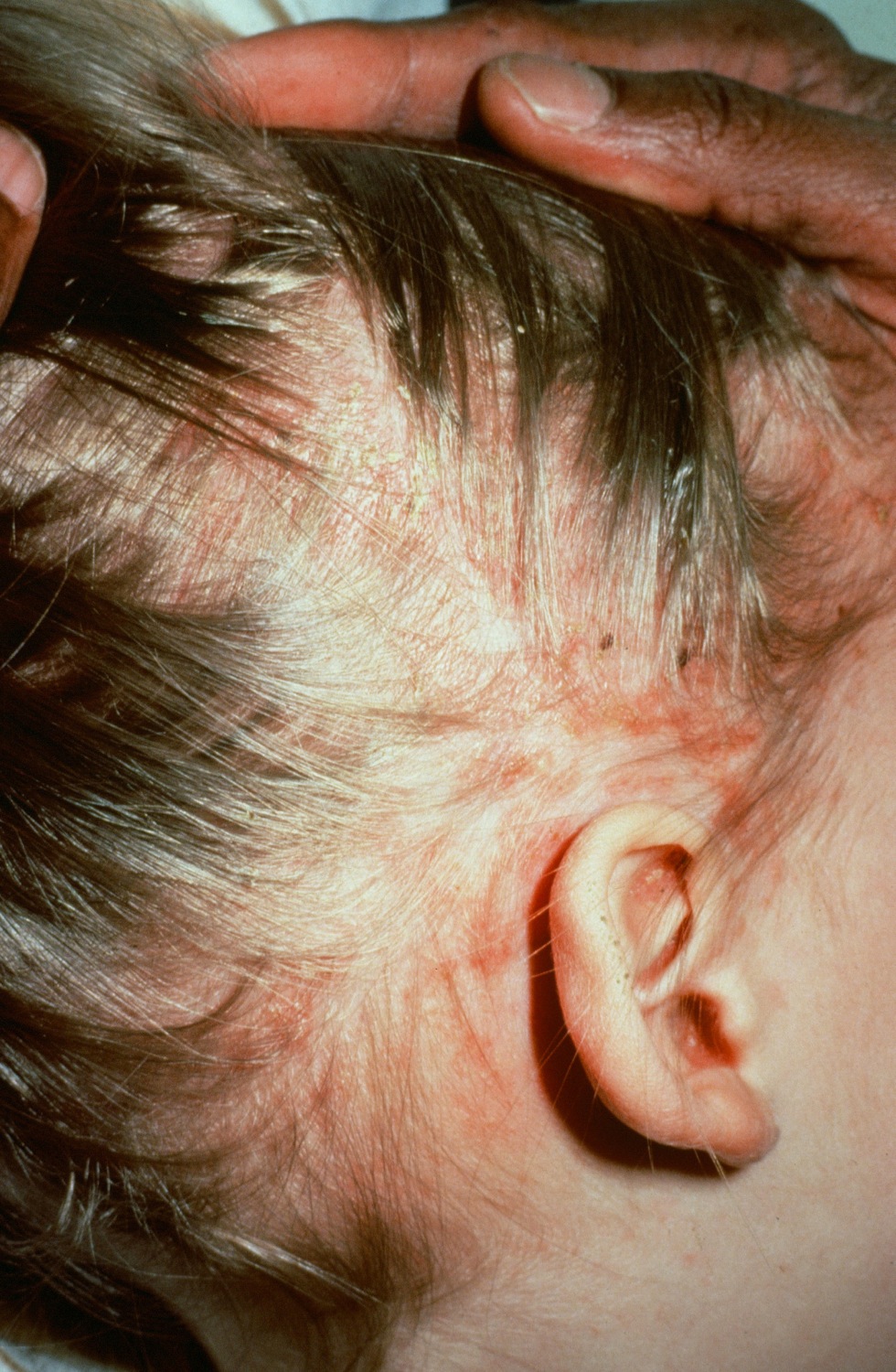
Eczema microbic. Adapted from Dermatology Atlas.[2]
-
Eczema microbic. Adapted from Dermatology Atlas.[2]
Differentiating nummular dermatitis from other diseases
Nummulrar dermatitis should be differentiated from other diseases causing papulosquamous or erythmatosquamous rash. The differentials include the following:
| Disease | Rash Characteristics | Signs and Symptoms | Associated Conditions | Images |
|---|---|---|---|---|
| Cutaneous T cell lymphoma/Mycosis fungoides[3] |
|
|
||
| Pityriasis rosea[4] |
|
|
||
| Pityriasis lichenoides chronica |
|
|
||
| Nummular dermatitis[7] |
|
|
|
|
| Secondary syphilis[8] |
|
|||
| Bowen’s disease[9] |
|
|
||
| Exanthematous pustulosis[11] |
|
|
||
| Hypertrophic lichen planus[13] |
|
|
|
|
| Sneddon–Wilkinson disease[15] |
|
|
||
| Small plaque parapsoriasis[19] |
|
|
|
|
| Intertrigo[21] |
|
|
||
| Langerhans cell histiocytosis[22] |
|
|
|
|
| Tinea manuum/pedum/capitis[26] |
|
|
|
|
| Seborrheic dermatitis |
|
|
Treatment
One of the keys to treatment and prevention involves keeping the skin moisturized. Lotions, creams, and bath oils may help prevent an outbreak. If the condition flares up, a common treatment involves the application of topical corticosteroids. Oral antihistamines may help lessen itching. More severe cases sometimes respond to ultraviolet light treatment.
References
- ↑ Krupa Shankar DS, Shrestha S (2005). "Relevance of patch testing in patients with nummular dermatitis". Indian journal of dermatology, venereology and leprology. 71 (6): 406–8. PMID 16394482.
- ↑ 2.0 2.1 2.2 2.3 2.4 "Dermatology Atlas".
- ↑ "Mycosis Fungoides and the Sézary Syndrome Treatment (PDQ®)—Patient Version - National Cancer Institute".
- ↑ Mahajan K, Relhan V, Relhan AK, Garg VK (2016). "Pityriasis Rosea: An Update on Etiopathogenesis and Management of Difficult Aspects". Indian J Dermatol. 61 (4): 375–84. doi:10.4103/0019-5154.185699. PMC 4966395. PMID 27512182.
- ↑ Prantsidis A, Rigopoulos D, Papatheodorou G, Menounos P, Gregoriou S, Alexiou-Mousatou I, Katsambas A (2009). "Detection of human herpesvirus 8 in the skin of patients with pityriasis rosea". Acta Derm. Venereol. 89 (6): 604–6. doi:10.2340/00015555-0703. PMID 19997691.
- ↑ Smith KJ, Nelson A, Skelton H, Yeager J, Wagner KF (1997). "Pityriasis lichenoides et varioliformis acuta in HIV-1+ patients: a marker of early stage disease. The Military Medical Consortium for the Advancement of Retroviral Research (MMCARR)". Int. J. Dermatol. 36 (2): 104–9. PMID 9109005.
- ↑ Jiamton S, Tangjaturonrusamee C, Kulthanan K (2013). "Clinical features and aggravating factors in nummular eczema in Thais". Asian Pac. J. Allergy Immunol. 31 (1): 36–42. PMID 23517392.
- ↑ "STD Facts - Syphilis".
- ↑ Neagu TP, Ţigliş M, Botezatu D, Enache V, Cobilinschi CO, Vâlcea-Precup MS, GrinŢescu IM (2017). "Clinical, histological and therapeutic features of Bowen's disease". Rom J Morphol Embryol. 58 (1): 33–40. PMID 28523295.
- ↑ Murao K, Yoshioka R, Kubo Y (2014). "Human papillomavirus infection in Bowen disease: negative p53 expression, not p16(INK4a) overexpression, is correlated with human papillomavirus-associated Bowen disease". J. Dermatol. 41 (10): 878–84. doi:10.1111/1346-8138.12613. PMID 25201325.
- ↑ Szatkowski J, Schwartz RA (2015). "Acute generalized exanthematous pustulosis (AGEP): A review and update". J. Am. Acad. Dermatol. 73 (5): 843–8. doi:10.1016/j.jaad.2015.07.017. PMID 26354880.
- ↑ Schmid S, Kuechler PC, Britschgi M, Steiner UC, Yawalkar N, Limat A, Baltensperger K, Braathen L, Pichler WJ (2002). "Acute generalized exanthematous pustulosis: role of cytotoxic T cells in pustule formation". Am. J. Pathol. 161 (6): 2079–86. doi:10.1016/S0002-9440(10)64486-0. PMC 1850901. PMID 12466124.
- ↑ Ankad BS, Beergouder SL (2016). "Hypertrophic lichen planus versus prurigo nodularis: a dermoscopic perspective". Dermatol Pract Concept. 6 (2): 9–15. doi:10.5826/dpc.0602a03. PMC 4866621. PMID 27222766.
- ↑ Shengyuan L, Songpo Y, Wen W, Wenjing T, Haitao Z, Binyou W (2009). "Hepatitis C virus and lichen planus: a reciprocal association determined by a meta-analysis". Arch Dermatol. 145 (9): 1040–7. doi:10.1001/archdermatol.2009.200. PMID 19770446.
- ↑ Lutz ME, Daoud MS, McEvoy MT, Gibson LE (1998). "Subcorneal pustular dermatosis: a clinical study of ten patients". Cutis. 61 (4): 203–8. PMID 9564592.
- ↑ Kasha EE, Epinette WW (1988). "Subcorneal pustular dermatosis (Sneddon-Wilkinson disease) in association with a monoclonal IgA gammopathy: a report and review of the literature". J. Am. Acad. Dermatol. 19 (5 Pt 1): 854–8. PMID 3056995.
- ↑ Delaporte E, Colombel JF, Nguyen-Mailfer C, Piette F, Cortot A, Bergoend H (1992). "Subcorneal pustular dermatosis in a patient with Crohn's disease". Acta Derm. Venereol. 72 (4): 301–2. PMID 1357895.
- ↑ Sauder MB, Glassman SJ (2013). "Palmoplantar subcorneal pustular dermatosis following adalimumab therapy for rheumatoid arthritis". Int. J. Dermatol. 52 (5): 624–8. doi:10.1111/j.1365-4632.2012.05707.x. PMID 23489057.
- ↑ Lambert WC, Everett MA (1981). "The nosology of parapsoriasis". J. Am. Acad. Dermatol. 5 (4): 373–95. PMID 7026622.
- ↑ Väkevä L, Sarna S, Vaalasti A, Pukkala E, Kariniemi AL, Ranki A (2005). "A retrospective study of the probability of the evolution of parapsoriasis en plaques into mycosis fungoides". Acta Derm. Venereol. 85 (4): 318–23. doi:10.1080/00015550510030087. PMID 16191852.
- ↑ Janniger CK, Schwartz RA, Szepietowski JC, Reich A (2005). "Intertrigo and common secondary skin infections". Am Fam Physician. 72 (5): 833–8. PMID 16156342.
- ↑ Satter EK, High WA (2008). "Langerhans cell histiocytosis: a review of the current recommendations of the Histiocyte Society". Pediatr Dermatol. 25 (3): 291–5. doi:10.1111/j.1525-1470.2008.00669.x. PMID 18577030.
- ↑ Stull MA, Kransdorf MJ, Devaney KO (1992). "Langerhans cell histiocytosis of bone". Radiographics. 12 (4): 801–23. doi:10.1148/radiographics.12.4.1636041. PMID 1636041.
- ↑ Sholl LM, Hornick JL, Pinkus JL, Pinkus GS, Padera RF (2007). "Immunohistochemical analysis of langerin in langerhans cell histiocytosis and pulmonary inflammatory and infectious diseases". Am. J. Surg. Pathol. 31 (6): 947–52. doi:10.1097/01.pas.0000249443.82971.bb. PMID 17527085.
- ↑ Grois N, Pötschger U, Prosch H, Minkov M, Arico M, Braier J, Henter JI, Janka-Schaub G, Ladisch S, Ritter J, Steiner M, Unger E, Gadner H (2006). "Risk factors for diabetes insipidus in langerhans cell histiocytosis". Pediatr Blood Cancer. 46 (2): 228–33. doi:10.1002/pbc.20425. PMID 16047354.
- ↑ Al Hasan M, Fitzgerald SM, Saoudian M, Krishnaswamy G (2004). "Dermatology for the practicing allergist: Tinea pedis and its complications". Clin Mol Allergy. 2 (1): 5. doi:10.1186/1476-7961-2-5. PMC 419368. PMID 15050029.
- ↑ Schwartz RA, Janusz CA, Janniger CK (2006). "Seborrheic dermatitis: an overview". Am Fam Physician. 74 (1): 125–30. PMID 16848386.
- ↑ Misery L, Touboul S, Vinçot C, Dutray S, Rolland-Jacob G, Consoli SG, Farcet Y, Feton-Danou N, Cardinaud F, Callot V, De La Chapelle C, Pomey-Rey D, Consoli SM (2007). "[Stress and seborrheic dermatitis]". Ann Dermatol Venereol (in French). 134 (11): 833–7. PMID 18033062.
External links
- Treatment details
- http://www.lib.uiowa.edu/hardin/md/dermnet/eczema6.html
- http://library.med.utah.edu/kw/derm/pages/desy_23.htm
Scheinfeld NS Circular brown-black eruptions (Nummular dermatitis and Discoid lupus erythematosus) Cortlandt Forum 2007;20(6)
- [pointer=0&tx_cortlandtmagissue_pi1[mode]=1&tx_cortlandtmagissue_pi1[showUid]=1388]
![Eczema microbic. Adapted from Dermatology Atlas.[2]](/images/b/bc/Eczema_microbic01.jpg)
![Eczema microbic. Adapted from Dermatology Atlas.[2]](/images/6/68/Eczema_microbic02.jpg)
![Eczema microbic. Adapted from Dermatology Atlas.[2]](/images/6/68/Eczema_microbic03.jpg)
![Eczema microbic. Adapted from Dermatology Atlas.[2]](/images/1/1a/Eczema_microbic04.jpg)