Mitral regurgitation pathophysiology
| https://https://www.youtube.com/watch?v=nY4aaBezu9o%7C350}} |
| Resident Survival Guide |
|
Mitral Regurgitation Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Mitral regurgitation pathophysiology On the Web |
|
American Roentgen Ray Society Images of Mitral regurgitation pathophysiology |
|
Risk calculators and risk factors for Mitral regurgitation pathophysiology |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Varun Kumar, M.B.B.S., Lakshmi Gopalakrishnan, M.B.B.S., Mohammed A. Sbeih, M.D. [2], Rim Halaby, M.D. [3] Khizer Yaseen, M.B.B.S.[4]
Overview
Regardless of the underlying etiology of mitral regurgitation (MR), a decrease in the coaptation between the leaflets of the valve commonly characterizes all cases of MR. Acute MR occurs when there is sudden disruption of one or more of the components of the mitral valve, as occurs in leaflet perforation, rupture of a chordae tendineae, or rupture of the papillary muscle. In the acute phase, the volume and pressure overload in the left atrium is transmitted backward into the pulmonary vasculature to cause an elevation of the pulmonary capillary wedge pressure which causes dyspnea, orthopnea, and rales. In addition, there is decreased forward stroke volume.Mitral regurgitation results in chronic volume overload of the left ventricle and left atrium, leading initially to increased preload and reduced afterload that produce compensatory eccentric left ventricular hypertrophy and chamber dilation[1]. Chronic MR can be either primary or secondary. Chronic primary MR results from chronic disruption of one or more component of the mitral valve (papillary muscles, chordae tendineae, or valve leaflets), whereas chronic secondary MR results from the dysfunction and dilatation of the left ventricle rather than an intrinsic abnormality in one of the components of the mitral valve. If the chronic MR develops slowly over months to years or if the acute phase is successfully managed with medical therapy, the patient enters the chronic compensated phase of MR that can eventually deteriorate into a decompensated phase as the left ventricular systolic function worsens.This compensated phase is characterized by preserved left ventricular systolic function despite progressive chamber enlargement and increased stroke volume[1]. The markers of MR decompensation are as follows: left ventricular end-diastolic dimension greater than 70 mm, left ventricular end-systolic dimension greater than 45 to 47 mm, and left ventricular ejection fraction (LVEF) less than 50 to 55 percent. Over time, persistent volume overload increases myocardial wall stress and leads to progressive myocardial dysfunction, eventually resulting in symptomatic heart failure if untreated[1].
Anatomy
- The mitral valve is composed of the valve leaflets, the mitral valve annulus (which forms a ring around the valve leaflets), the papillary muscles (which tether the valve leaflets to the left ventricle, preventing them from prolapsing into the left atrium), and the chordae tendineae (which connect the valve leaflets to the papillary muscles).
- A dysfunction of any of these portions of the mitral valve apparatus can cause MR.
- The mitral annulus changes in shape and size during the cardiac cycle. It is smaller at the end of atrial systole due to the contraction of the left atrium around it, like a sphincter.
- This reduction in annulus size at the end of atrial systole may be important for the proper coapting of the leaflets of the mitral valve when the left ventricle contracts and pumps blood.[2][3]
Mechanical Basis of Mitral Regurgitation
The mechanical basis underlying MR includes the following:
- Anterior mitral leaflet prolapse
- Posterior mitral leaflet prolapse
- Bileaflet prolapse
- Restricted mitral leaflets
- Apical tethering
- Papillary muscle rupture
- Ischemic papillary muscle rupture
- Mitral leaflet perforation
- Rupture or tear of the chordae tendineae
- Dilation of the mitral annulus
- "Functional MR" due to dilation of the heart itself
Shown below is an image depicting the abnormal flow of blood from the left ventricle, through the mitral valve, and into the left atrium during systole.

During systole, contraction of the left ventricle causes abnormal backflow (arrow) into the left atrium.
1 Mitral valve
2 Left Ventricle
3 Left Atrium
4 Aorta
In mitral regurgitation, the presence of a low-resistance pathway into the left atrium reduces effective left ventricular afterload, which contributes to preservation of left ventricular ejection fraction during the early stages of disease despite ongoing myocardial injury[1].
Factors Affecting the Regurgitant Volume
The volume of the regurgitant flow determines the severity of MR. The factors that affect the regurgitant volume are:
- The effective regurgitant orifice (principle factor)[4]
- The gradient of pressure between the left ventricle and the left atrium (principle factor)[4]
- The compliance of the left atrium[4]
- The left ventricular function[4]
- The duration of systole[4]
- Left ventricular afterload
Pathophysiology of Acute Mitral Regurgitation
- Acute MR occurs when there is sudden disruption of one or more of the components of the mitral valve, such as leaflet perforation, rupture of a chordae tendineae, or rupture of the papillary muscle.
- The sudden disruption of the mitral valve may occur in the context of infective endocarditis, degenerative mitral valve disease, or acute ST elevation myocardial infarction.
- In the acute setting, the total stroke volume (i.e. the forward plus the regurgitant volume) is increased, but the forward cardiac output into the aorta is decreased because a proportion of the blood is going backward into the left atrium.
- Consequently, acute MR causes a sudden volume overload of both the left atrium and the left ventricle. As a result, pulmonary congestion and hypoxia occur following the elevation of the pressure in the left atrium.
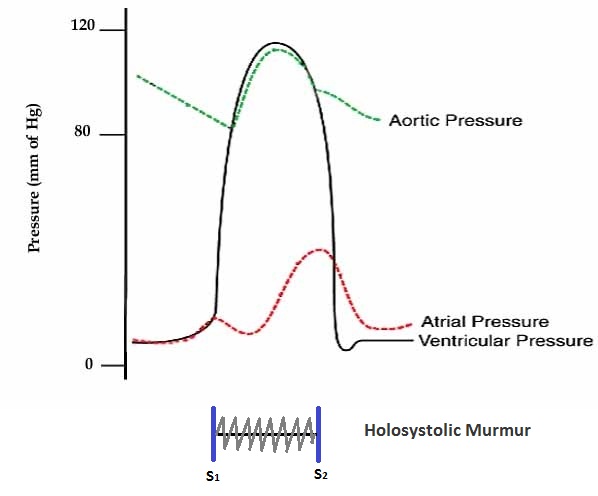
Shown below is an image depicting the pressures in the left atrium, left ventricle, and aorta in acute MR.
Pathophysiology of Chronic Mitral Regurgitation
Chronic Primary Mitral Regurgitation
Chronic primary MR results from chronic disruption of one or more component of the mitral valve (papillary muscles, chordae, and valve leaflets). This may occur among patients with:[5]
- Mitral valve prolapse
- Myxomatous degeneration (young patients)
- Fibroelastic deficiency disease (old patients)
- Infective endocarditis
- Connective tissue disease
- Rheumatic heart disease
- Radiation heart disease
Chronic Compensated Phase
- If the MR develops slowly over months to years or if the acute phase is successfully managed with medical therapy, the patient enters the chronic compensated phase of MR.
- In this phase, the left ventricle develops eccentric hypertrophy to reduce the wall stress associated with the rise in total stroke volume (i.e. the forward plus the regurgitant volume) .
- The eccentric hypertrophy and the increased diastolic volume combine to increase the total stroke volume to levels well above normal, so that the forward stroke volume (forward cardiac output) is maintained.
- In the left atrium, the chronic volume overload causes left atrial enlargement, which serves as an adaptive mechanism that accommodates the regurgitant volume and helps reduce left atrial filling pressure[1].
- Chronic mitral regurgitation leads to progressive left atrial remodeling due to persistent volume overload, resulting in atrial enlargement, increased wall stress, and activation of neurohumoral pathways that promote atrial fibrosis and dysfunction[6]. These structural and functional alterations in the left atrium are associated with atrial fibrillation, increased pulmonary pressures, and adverse clinical outcomes independent of left ventricular size and function[6]
- This dilation of the left atrium reduces the pulmonary capillary wedge pressure, and is associated with an improvement in the signs (e.e. rales) and symptoms (dyspnea, PND, and orthopnea) of pulmonary congestion.
- These compensatory changes in the left ventricle and left atrium maintain the forward cardiac output of the left ventricle, and minimize the signs and symptoms of pulmonary congestion that occur in the acute phase of the disease.
- Individuals in the chronic compensated phase may be asymptomatic and have normal exercise tolerance.
- In the compensated stage; the left ventricular (LV) end-diastolic dimension is less than 60 mm, and the end-systolic dimension is less than 40 mm on echocardiography.
Transitional phase
A transitional phase follows the compensated stage and is characterized by increasing myocardial wall stress and early myocardial dysfunction despite preserved left ventricular ejection fraction[1]. During this stage, structural myocardial changes may already be present before symptoms develop, emphasizing the importance of early recognition and timely intervention[7].
Chronic Decompensated Phase
- Patients with mitral regurgitation may remain in a compensated phase for years; however, if untreated, progressive left ventricular dysfunction develops, marking transition to the chronic decompensated phase characterized by irreversible systolic dysfunction and clinical manifestations of heart failure[1].
- It is currently unclear what causes an individual to enter the decompensated phase of this disease. However, the decompensated phase is characterized by calcium overload within the cardiac myocytes.
- In this phase, the ventricular myocardium is no longer able to contract adequately to compensate for the volume overload of MR, and the stroke volume of the left ventricle begins to decrease. The reduced stroke volume causes a decrease in the forward cardiac output and an increase in the end-systolic volume.
- The increased left ventricular end-systolic volume in turn causes increased left ventricular end diastolic pressures and increased pulmonary capillary wedge pressures.
- As the wedge pressure rises, the patient may develop symptoms of congestive heart failure such as dyspnea, PND and orthopnea and signs of congestive heart failure including rales.
- With the rise in wall stress that accompanies the rise in pressure and volume in the left ventricle, the left ventricle begins to dilate during this phase.
- This causes a dilatation of the mitral valveannulus, which may further worsen the degree of MR. While the ejection fraction is less in the chronic decompensated phase than in the acute phase or the chronic compensated phase of MR, it may still be in the normal range (i.e: > 50 percent), and may not decrease until late in the disease course.
- A decreased ejection fraction in an individual with MR and no other cardiac abnormality should alert the physician that the disease may be in its decompensated phase.
- Among asymptomatic patients with severe primary mitral regurgitation, those with left ventricular ejection fraction of 60% or less have increased mortality if untreated[7]
- The decompensated stage defined on the basis of decompensated ventricular function. At this stage; the patients are at risk for a poor results of valve replacement.
- It is helpful to classify the stage of the patient's disease so as to recognize signs that may indicate that the patient is transitioning into the decompensated phase of the disease.
- The goal is to perform mitral valve surgery before the patient transitions into the decompensated phase.
- Once the patient transitions into the decompensated phase, (left ventricular enlargement and a low left ventricular ejection fraction) there may not be recovery of left ventricular function following operative repair or replacement of the mitral valve.
- Right ventricular enlargement and dysfunction in primary mitral regurgitation often represent downstream consequences of chronic left ventricular remodeling and pulmonary hypertension resulting from long-standing volume overload. Pulmonary hypertension may develop as compensatory mechanisms of the left ventricle and left atrium fail, eventually leading to right ventricular dilation and functional tricuspid regurgitation[8]
Markers of Decompensated Ventricular Function in Mitral Regurgitaiton
- Left ventricular end-diastolic dimension greater than 70 mm
- Left ventricular end-systolic dimension greater than 45 to 47 mm
- Left ventricular ejection fraction (LVEF) less than 50 to 55 percent
Chronic Secondary Mitral Regurgitation
Chronic secondary MR results from the dysfunction and dilatation of the left ventricle rather than an intrinsic abnormality in one of the components of the mitral valve. Chronic secondary MR may occur in the setting of:[5]
- Coronary artery disease (ischemic), or
- Any disease causing left ventricular dysfunction and dilatation (functional)
- In secondary MR, the left ventricular dysfunction precedes the valvular abnormality.
- MR may be the result of an enlargement in the annular component of the mitral valve secondary to the dilatation of the left ventricle and/or the displacement of the papillary muscle following remodeling of the left ventricle.
- Ischemic heart disease causes mitral regurgitation by the combination of ischemic dysfunction of the papillary muscles, the abnormal motion of the underlying wall, and the dilatation of the left ventricle that is present in ischemic heart disease, with the subsequent displacement of the papillary muscles and the dilatation of the mitral valve annulus.
- Secondary mitral regurgitation due to the dilatation of the left ventricle is caused by stretching of the mitral valve annulus and displacement of the papillary muscles.
- This dilatation of the left ventricle can be due to any cause of dilated cardiomyopathy, including aortic insufficiency, nonischemic dilated cardiomyopathy and noncompaction cardiomyopathy.
- It is also called functional mitral regurgitation, because the papillary muscles, chordae, and valve leaflets are usually normal.
- When MR is present, the regurgitant flow into the left atrium increases the pressure in this chamber which compensates by dilatation leading to an increase in the preload.
- In addition, the decrease in the afterload causes a series of adaptation in the left ventricle in order to increase the stroke volume.
- The left ventricle adaptation mechanisms to increase the stroke volume include an increment in the preload and the ventricular wall tension.
- The long term overload on the left ventricle contributes to its further dilatation, which by itself leads to a worsening of the MR and subsequent deterioration of the heart failure.[4]
Summary Chart Distinguishing Acute and Chronic Mitral Regurgitation
| Acute mitral regurgitation | Chronic mitral regurgitation | |
|---|---|---|
| Electrocardiogram | Normal unless there are findings related to the etiology of the MR, such as STEMI | P mitrale, atrial fibrillation, left ventricular hypertrophy |
| Heart size | Normal | Cardiomegaly, left atrial enlargement |
| Systolic murmur | Heard at the base, radiates to the neck, spine, or top of head | Heard at the apex, radiates to the axilla |
| Apical thrill | May be absent | Present |
| Jugular venous distension | Present | Absent |
References
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 Gaasch WH, Meyer TE. Left ventricular response to mitral regurgitation: implications for management. Circulation. 2008 Nov 25;118(22):2298-303. doi: 10.1161/CIRCULATIONAHA.107.755942. PMID: 19029478.
- ↑ Pai RG, Varadarajan P, Tanimoto M (2003). "Effect of atrial fibrillation on the dynamics of mitral annular area". J Heart Valve Dis. 12 (1): 31–7. PMID 12578332.
- ↑ Weinrauch, LA (2008-05-12). "Mitral regurgitation - chronic". Medline Plus Encyclopedia. U.S. National Library of Medicine and National Institutes of Health. Retrieved 2009-12-04.
- ↑ 4.0 4.1 4.2 4.3 4.4 4.5 Ciarka A, Van de Veire N (2011). "Secondary mitral regurgitation: pathophysiology, diagnosis, and treatment". Heart. 97 (12): 1012–23. doi:10.1136/hrt.2010.219170. PMID 21586426.
- ↑ 5.0 5.1 Nishimura RA, Otto CM, Bonow RO, Carabello BA, Erwin JP, Guyton RA; et al. (2014). "2014 AHA/ACC guideline for the management of patients with valvular heart disease: executive summary: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines". J Am Coll Cardiol. 63 (22): 2438–88. doi:10.1016/j.jacc.2014.02.537. PMID 24603192.
- ↑ 6.0 6.1 van Wijngaarden AL, Kruithof BPT, Vinella T, Barge-Schaapveld DQCM, Ajmone Marsan N. Characterization of Degenerative Mitral Valve Disease: Differences between Fibroelastic Deficiency and Barlow's Disease. J Cardiovasc Dev Dis. 2021 Feb 22;8(2):23. doi: 10.3390/jcdd8020023. PMID: 33671724; PMCID: PMC7926852.
- ↑ 7.0 7.1 Enriquez-Sarano M, Avierinos JF, Messika-Zeitoun D, Detaint D, Capps M, Nkomo V, Scott C, Schaff HV, Tajik AJ. Quantitative determinants of the outcome of asymptomatic mitral regurgitation. N Engl J Med. 2005 Mar 3;352(9):875-83. doi: 10.1056/NEJMoa041451. PMID: 15745978.
- ↑ Patel H, Desai M, Tuzcu EM, Griffin B, Kapadia S. Pulmonary hypertension in mitral regurgitation. J Am Heart Assoc. 2014 Aug 7;3(4):e000748. doi: 10.1161/JAHA.113.000748. PMID: 25103202; PMCID: PMC4310359.