Mitral regurgitation resident survival guide
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Mugilan Poongkunran M.B.B.S [2]
| Mitral Regurgitation Resident Survival Guide Microchapters |
|---|
| Overview |
| Causes |
| FIRE |
| Complete Diagnostic Approach |
| Treatment |
| Do's |
| Don'ts |
Overview
Mitral regurgitation (MR) is a disorder of the heart characterized by failure of the mitral valve to close properly during systole leading to blood leakage from the left ventricle to the left atrium during systole. Individuals with acute mitral regurgitation may present with significant hemodynamic instability due to the sudden drop in cardiac output, leading to acute pulmonary edema, hypotension and possible cardiogenic shock. Individuals with chronic compensated mitral regurgitation may be asymptomatic, with a normal exercise tolerance and no evidence of heart failure, or may present with fatigue, dyspnea on exertion, orthopnea, and paroxysmal nocturnal dyspnea.[1] The management of MR includes afterload reduction with careful monitoring of fluid status, management of the underlying disease (CAD, mitral valve prolapse, rheumatic heart disease), and early surgical intervention in severe cases. Ultimately, the management of MR depends on the anatomy of the mitral valve, the acuteness of the disease process, and the severity of presentation. [2]
Causes
Life Threatening Causes
Life-threatening causes include conditions which may result in death or permanent disability within 24 hours if left untreated.
Common Causes
Acute Mitral Regurgitation
- Papillary muscle rupture:
- Ruptured mitral chordae tendinae:
- Acute rheumatic fever[3]
- Chest trauma[4]
- Mitral valve prolapse[5]
- Infective endocarditis
- Spontaneous rupture
Chronic Primary Mitral Regurgitation
Chronic Secondary Mitral Regurgitation
Click here for the complete list of causes.
FIRE: Focused Initial Rapid Evaluation
A Focused Initial Rapid Evaluation (FIRE) should be performed to identify patients in need of immediate intervention.
Boxes in red color signify that an urgent management is needed.
Abbreviations: ARBs: Angiotensin II receptor antagonist; CABG: Coronary artery bypass surgery; HF: Heart failure; IE: Infective endocarditis; LVEF: Left ventricular ejection fraction; LV: Left ventricle; MR: Mitral regurgitation; S1: First heart sound; S2: Second heart sound
Identify cardinal findings that increase the pretest probability of mitral regurgitation: ❑ Murmur:
❑ Heart sounds: | |||||||||||||||||||||||||||||||||||||||
Does the patient have any of the following findings of acute mitral regurgitation with instability? ❑ Sudden onset and rapid progression of pulmonary edema:
| |||||||||||||||||||||||||||||||||||||||
| Yes | No | ||||||||||||||||||||||||||||||||||||||
| Continue with complete diagnostic approach below | |||||||||||||||||||||||||||||||||||||||
Initiate resuscitative measures: ❑ Secure airway Order imaging and blood tests (urgent): | |||||||||||||||||||||||||||||||||||||||
| Does the patient has any evidence of MR in TTE? | |||||||||||||||||||||||||||||||||||||||
| Yes | No | ||||||||||||||||||||||||||||||||||||||
Stabilize the patient:
❑ Establish intra-aortic balloon pump:
Initiate treatment for specific etiologies: | Consider other possible diagnosis: | ||||||||||||||||||||||||||||||||||||||
Does the patient have any findings on TTE that require mitral valve surgery? ❑ Flail mitral leaflet (papillary muscle or chordal rupture)
| |||||||||||||||||||||||||||||||||||||||
| Yes | No | ||||||||||||||||||||||||||||||||||||||
Perform mitral valve surgery:
| Perform reperfusion or revascularization: ❑ In patients with acute coronary syndrome, CABG or coronary angioplasty should be performed | ||||||||||||||||||||||||||||||||||||||
Perform reperfusion or revascularization: ❑ Perform CABG or coronary angioplasty at the time of mitral valve surgery in patients with myocardial infarction Consider cardiac transplantation: | |||||||||||||||||||||||||||||||||||||||
Complete Diagnostic Approach to Mitral Regurgitation
A complete diagnostic approach should be carried out after a focused initial rapid evaluation is conducted and following initiation of any urgent intervention.[2].
Abbreviations: AF: Atrial fibrillation; MR: Mitral regurgitation; EKG: Electrocardiogram; EF: Ejection fraction; S1: First heart sound; S2: Second heart sound; S3: Third heart sound; LV: Left ventricle; MVP: Mitral valve prolapse
Characterize the symptoms: Acute mitral regurgitation:
❑ Symptoms of shock and pulmonary edema:
❑ Symptoms suggestive of precipitating events:
Chronic mitral regurgitation: ❑ Asymptomatic
❑ Symptoms associated with decreased forward flow and increased backflow across mitral valve (left ventricular failure):
❑ Symptoms associated with complications:
| |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Obtain a detailed history: ❑ Past medical history:
❑ Family history: ❑ Medications: | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Examine the patient: Vital signs:
Skin: Cardiovascular system:
❑ Thrill (in acute MR and severe chronic MR)
Auscultation:
❑ Murmur
Respiratory system: Abdominal system: Neurological system: | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Order electrocardiogram (urgent):
❑ In acute MR
❑ In chronic MR
 Order chest X-ray (urgent):
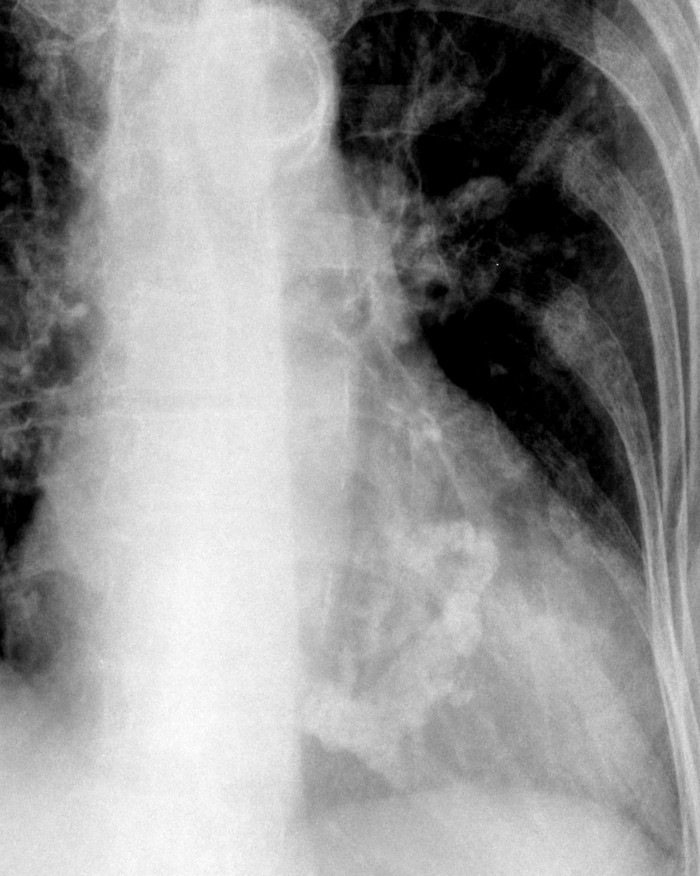 Order transthoracic echocardiography (TTE) (urgent): Order lab tests: Other tests:
❑ Exercise testing:
| |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Does the patient has acute or chronic MR? | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Acute MR (Cardinal findings suggestive of acute mitral regurgitation) ❑ Sudden onset and rapid progression of pulmonary edema
| Chronic MR (cardinal findings suggestive of chronic mitral regurgitation) ❑ Asymptomatic to chronic symptoms
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Does the mitral valve anatomy appear normal in TTE? | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Yes | No | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Chronic secondary mitral regurgitation | Chronic primary mitral regurgitation | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Treatment
Treatment of Acute Mitral Regurgitation
Shown below is an algorithm summarizing the approach to the management of acute mitral regurgitation.[1][2].
Abbreviations: IE: Infective endocarditis; LV: Left ventricle; LVEF: Left ventricular ejection fraction; MR: Mitral regurgitation
Does the patient has any signs of hemodynamic instability? ❑ Hypotension | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Yes | No | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Initiate resuscitative measures: ❑ Secure airway Stabilize the patient:
❑ Establish intra-aortic balloon pump:
| Initiate resuscitative measures: ❑ Administer O2 Initiate medical therapy: | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| MR due to IE (organic MR) | Ischemic mitral regurgitation | MR due to heart failure exacerbation(functional MR) | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Initiate IE medical therapy: ❑ Click here for infective endocarditis resident survival guide and antimicrobial treatment | Perform reperfusion or revascularization surgery: ❑ CABG or coronary angioplasty should be done to treat acute coronary syndrome | Initiate treatment for heart failure: ❑ Click here for acute heart failure resident survival guide
| |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Does the patient has any indications for mitral valve surgery? ❑ Hemodynamic instability | Does the patient has any indications for mitral valve surgery? ❑ Papillary muscle rupture | Does the patient show any hemodynamic improvement to medical therapy? | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Yes | No | Yes | No | Yes | No | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Perform mitral valve surgery:
|
❑ Continue with medical management | Perform mitral valve surgery: ❑ Done at the time of reperfusion
❑ Mitral valve replacement: Preferred in the following groups | Consider medical therapy: Consider cardiac transplantation: | Continue with the heart failure management and have appropriate follow ups to assess the severity of MR | Consider mitral valve surgery:
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Initiate anticoagulation therapy: ❑ For patients undergoing mitral valve replacement Educate the patient about IE prophylaxis: | Initiate anticoagulation therapy: ❑ For patients undergoing mitral valve replacement Educate the patient about IE prophylaxis: | Initiate anticoagulation therapy: ❑ For patients undergoing mitral valve replacement Educate the patient about IE prophylaxis: | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Treatment of Chronic Mitral Regurgitation
Chronic Primary Mitral Regurgitation
Shown below is an algorithm summarizing the approach to the management of chronic primary mitral regurgitation.[2].
Abbreviations: AF: Atrial fibrillation; IE: Infective endocarditis; LVEF: Left ventricular ejection fraction; LVESD: Left ventricular end systolic dimension; MR: Mitral regurgitation; MVP: Mitral valve proplapse; PASP: Pulmonary artery systolic pressure; RHD: Rheumatic heart disease
| Determine the severity of MR on TTE | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Severe MR: ❑ Severe MVP with loss of coaptation | Progressive MR (Stage B): ❑ Severe MVP with normal coaptation | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Symptomatic (Stage D) | Asymptomatic (Stage C) | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Does the patient has any indications for mitral valve surgery? ❑ LVEF 30 to ≤60% OR LVESD ≥ 40mm (Stage C2)
❑ New onset AF OR PASP > 50mmHg (Stage C1)
| |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Yes | No | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Initiate medical therapy:
❑ Beta blocker Perform mitral valve surgery:
Perform revascularisation: | Perform mitral valve surgery:
Perform revascularization: | Periodic monitoring:
❑ Clinical evaluation:
| |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Initiate anticoagulation therapy: ❑ Indications:
❑ Warfarin:
❑ Aspirin:
Educate the patient about IE prophylaxis: | Initiate anticoagulation therapy: ❑ Indications:
❑ Warfarin:
❑ Aspirin:
Educate the patient about IE prophylaxis: | Initiate anticoagulation therapy: ❑ Indications:
❑ Warfarin:
❑ Aspirin:
| |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Chronic Secondary Mitral Regurgitation
Shown below is an algorithm summarizing the approach to the management of chronic secondary mitral regurgitation.[2].
Abbreviations: AF: Atrial fibrillation; CAD: Coronary artery disease; HF: Heart failure; IE: Infective endocarditis; LV: Left ventricle; MR: Mitral regurgitation
| Determine the etiology and initiate specific treatment | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Heart failure: ❑ Click here for heart failure resident survival guide
| Coronary artery disease: ❑ Click here for coronary artery disease medical therapy ❑ Coronary angiography | Functional MR with ventricular dyssynchrony: ❑ Cardiac resynchronization therapy with biventricular pacing:
| |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Assess the severity of MR on TTE | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Severe MR: ❑ Regional wall motion abnormalities with severe tethering of mitral leaflet | Progressive MR: ❑ Regional wall motion abnormalities with mild tethering of mitral leaflets | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Does the HF symptoms due to MR persist even after revascularization and medical therapy? | HF and coronary ischemia symptoms respond to revascularization and medical herapy | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Yes (Stage D) | No (Stage C) | Stage B | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Perform mitral valve surgery:
| Periodic monitoring: ❑ Clinical evaluation:
Consider mitral valve surgery: | Periodic monitoring: ❑ Clinical evaluation:
Consider mitral valve surgery: | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Initiate anticoagulation therapy: ❑ Indications:
❑ Warfarin:
❑ Aspirin:
Educate the patient about IE prophylaxis: | Initiate anticoagulation therapy: ❑ Indications:
❑ Warfarin:
❑ Aspirin:
Educate the patient about IE prophylaxis: | Initiate anticoagulation therapy: ❑ Indications:
❑ Warfarin:
❑ Aspirin:
Educate the patient about IE prophylaxis: | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Do's
- Always consult a multidisciplinary heart valve team for patients with acute MR, severe chronic MR and with multiple comorbidities.
- Consider vasodilator therapy in patients with chronic MR based upon the presence or absence of symptoms and the functional state of the left ventricle.
- Always consider patients with chronic MR who become symptomatic to be candidates for corrective mitral surgery.
- Perform mitral valve repair for patients with chronic severe primary MR limited to the posterior leaflet.
Don'ts
- Don't initiate vasodilator therapy for normotensive asymptomatic patients with chronic primary MR (stages B and C1) and normal systolic LV function.
- Don't recommend cardiovascular magnetic resonance (CMR) for routine diagnosis of MR.
- Don't prefer mitral valve repair to replacement to chronic severe primary MR patients involving the anterior leaflet or both leaflets when a successful and durable repair cannot be accomplished.
- Don't perform mitral valve replacement in patients with isolated severe primary MR limited to less than one half of the posterior leaflet unless mitral valve repair has been attempted and was unsuccessful.
- Don't perform coronary angiography before valve surgery in patients who are hemodynamically unstable.
- Avoid coronary angiography in patients of acute coronary syndrome complicated by severe acute mitral regurgitation.
References
- ↑ 1.0 1.1 Stout KK, Verrier ED (2009). "Acute valvular regurgitation". Circulation. 119 (25): 3232–41. doi:10.1161/CIRCULATIONAHA.108.782292. PMID 19564568.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 Nishimura RA, Otto CM, Bonow RO, Carabello BA, Erwin JP, Guyton RA; et al. (2014). "2014 AHA/ACC Guideline for the Management of Patients With Valvular Heart Disease: Executive Summary: A Report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines". Circulation. doi:10.1161/CIR.0000000000000029. PMID 24589852.
- ↑ Anderson Y, Wilson N, Nicholson R, Finucane K (2008). "Fulminant mitral regurgitation due to ruptured chordae tendinae in acute rheumatic fever". J Paediatr Child Health. 44 (3): 134–7. doi:10.1111/j.1440-1754.2007.01214.x. PMID 17854408.
- ↑ Grinberg AR, Finkielman JD, Piñeiro D, Festa H, Cazenave C (1998). "Rupture of mitral chorda tendinea following blunt chest trauma". Clin Cardiol. 21 (4): 300–1. PMID 9580528.
- ↑ Grenadier E, Alpan G, Keidar S, Palant A (1983). "The prevalence of ruptured chordae tendineae in the mitral valve prolapse syndrome". Am Heart J. 105 (4): 603–10. PMID 6837414.
- ↑ Otto CM (2001). "Clinical practice. Evaluation and management of chronic mitral regurgitation". N Engl J Med. 345 (10): 740–6. doi:10.1056/NEJMcp003331. PMID 11547744.