Greenstick fracture
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Mohammadmain Rezazadehsaatlou[2].
A greenstick fracture, as an incomplete fracture of long bones, defined as a partial thickness fracture which just the cortex and periosteum are interrupted only on one side of the affected bone. The greenstick fracture usually are seen in young children commonly younger than 10 years old. It is usually from falling or blow to one side of the body.
Historical Perspective[2]
The term greenstick is originates from an analogy between the pliable bones and the flexible nature of a young twig.
In 1822, Sir Astley Cooper worked on the dislocations and Fracture of human body.
In 1930–2000, John Nevil Insall, An american-British orthopedic surgeon discovered the green-stick fracture.
Causes[2]
The main etiology of the greenstick fracture is thought to be a loading may be placed on a forearm during falling onto an outstretched hand (FOOSH) with an extended wrist and hyperpronated forearm. Because at this posture the energy from the radius fracture transmitted towards the radioulnar joint cause the dislocation of the DRUJ. The main cause of greenstick fracture is trauma. Such as the most fractures the greenstick fracture is caused by a falling or automobile accident. Meanwhile, the normal healthy bones are extremely tough and resilient and can withstand most powerful impacts. As a person age, two factors cause higher risk of fractures:
- Weaker bones
- Greater risk of falling
Stress fractures as a common causes of fractures can be found due to the repeated stresses and strains. Importantly children having more physically active lifestyles than adults, are also prone to fractures. People with any underlying diseases such as osteoporosis, infection, or a tumor affecting their bones having a higher risk of fractures. As mentioned in previous chapters, this type of fracture is known as a pathological fracture. Stress fractures, which result from repeated stresses and strains, commonly found among professional sports people, are also common causes of fractures.
Life-threatening Causes
- There are no life-threatening causes of greenstick fracture, however complications resulting from greenstick fracture is common.
Common Causes
Common causes of greenstick fracturemay include:
- Trauma (Fall on an outstretched hand)
Less Common Causes
Less common causes of greenstick fracture include conditions that predisposes to fracture:
Causes by Organ System
| Cardiovascular | No underlying causes |
| Chemical/Poisoning | No underlying causes |
| Dental | No underlying causes |
| Dermatologic | No underlying causes |
| Drug Side Effect | No underlying causes |
| Ear Nose Throat | No underlying causes |
| Endocrine | No underlying causes |
| Environmental | No underlying causes |
| Gastroenterologic | No underlying causes |
| Genetic | No underlying causes |
| Hematologic | No underlying causes |
| Iatrogenic | No underlying causes |
| Infectious Disease | No underlying causes |
| Musculoskeletal/Orthopedic | Osteoporosis and osteopenia. |
| Neurologic | No underlying causes |
| Nutritional/Metabolic | Osteoporosis and osteopenia. |
| Obstetric/Gynecologic | No underlying causes |
| Oncologic | No underlying causes |
| Ophthalmologic | No underlying causes |
| Overdose/Toxicity | No underlying causes |
| Psychiatric | No underlying causes |
| Pulmonary | No underlying causes |
| Renal/Electrolyte | No underlying causes |
| Rheumatology/Immunology/Allergy | No underlying causes |
| Sexual | No underlying causes |
| Trauma | Fall on an outstretched hand. |
| Urologic | No underlying causes |
| Miscellaneous | No underlying causes |
Causes in Alphabetical Order
List the causes of the disease in alphabetical order:
Mechanism
The greenstick fracture is caused by a fall on the outstretched hands with the wrist in dorsiflexion position. The form and severity of this fracture depends on the position of the wrist at the moment of hitting the ground. The width of this mentioned angle affects the localization of the fracture. Pronation, supination and abduction positions leads the direction of the force and the compression of carpus and different appearances of injury. Pathophysiology Its known that the greenstick fracture in normal healthy adults can be caused due to the high-energy trauma (e.g., motor vehicle accidents), sport related injuries, falling from height. But it should be noted that the most important Risk factors for insufficiency fractures is chronic metabolic disease such as steoporosis, osteopenia, eating-disordered behavior, higher age, prolonged corticosteroid usage, female gender, lower BMI, history of a recent falling, and prior fracture.
Pathophysiology
- The pattern of bone fracture and severity of injury depends on variety of factors such as:
- Patients age
- Patients Weight
- Patients past medical history specifically any bone diseases affecting the quality of bone (such as osteoporosis, malignancies)
- Energy of trauma
- Bone quality
- Position of the specific organ during the trauma
- The below-mentioned processes cause decreased bone mass density:
- Autophagy is the mechanism through which osteocytes evade oxidative stress.
- The capability of autophagy in cells decreases as they age, a major factor of aging.
- As osteocytes grow, viability of cells decrease thereby decreasing the bone mass density
Differentiating greenstick fracture from other Diseases[2]
In the orthopedic medicine its important to know that the forearm fracture should be evaluated using radiography for both confirming diagnosis and also for evaluating the surrounding tissues. In the orthopedic medicine its important to know that the forearm fracture should be evaluated using radiography for both confirming diagnosis and also for evaluating the surrounding tissues. Other injuries such as possible olecranon fracture-dislocation; radial head or coronoid fractures or lateral collateral ligament injury, might be seen in Monteggia fracture. If the mechanism of injury suggests particularly low energy then the Osteoporosis should be considered. The pathological Fractures occurring in a bone with a tumor or Paget's disease) are rare but possible[3].
Also it should be noted that the both bone fractures can be complicated by acute compartment syndrome of the forearm. Signs suggesting compartment syndrome are pain on extension of digits, and marked edema[3].
As another important fact in orthopedic fracture is if both-bone fractures were found in pediatric which is common after accidental trauma, but it may also be the due to the of child abuse; and in these cases a careful attention and evaluation should be considered if a child abuse is suspected.
- Salter-Harris fracture
- torus fracture
- toddler fracture (non-displaced spiral fracture of the distal tibia)
- spiral fracture
- non-accidental fracture open fracture
- athologic fracture
- non-displaced fracture
- plastic deformities
In the United States the frequency of the musculoskeletal injuries in pediatric was 12% of all emergency department visits due to this type of injuries. Greenstick fracture can be found in any age group but it is common in pediatric population under 10 years. Meanwhile,it has an equal incidence rate in both genders.
There are different risk factors that presidpose patient for the Greenstick fracture that include::
- High-risk contact sports
- Higher age (elderly adults are higher prone to such fractures)
- Osteoporosis
- Direct trauma
- Road / traffic accidents
- Falling
- Gunshot wounds
- Domestic violence
- Falling on an outstretched hand with the forearm pronated
- Glucocorticoid use
- Anabolic steroid use
- Paget disease of the bone
Screening [2]
Osteoporosis is an important risk factor for human affecting human bone especially in men with the age of older than 50 years old and postmenopausal and women.
Based on the US Preventive Services Task Force (USPSTF) there are three groups of patients need to be screened for the osteoporosis:
- · Men with no history of osteoporosis
- · Women with the age of 65≤ year old, with no previous history of pathological fracture due to the osteoporosis
- · Women with the age of <65 years, with 10-year fracture risk of not less than a 65-year-old white woman (who has not any other risk factor)
Accordingly women older than age of 50 are the main target for the osteoporosis screening. There is no specific recommendation to screen men for the osteoporosis.
The USPSTF recommendations from 2002 included:
Meanwhile, there are two major modalities for the osteoporosis screening:
- · Dual energy x-ray absorptiometry (DXA) of the hip and lumbar spine bones
- · Quantitative ultrasonography of the calcaneus
*It should be noted of the two above mentioned modalities for screening the ultrasonograhy is preferred to the DXA due to its lower cost, lower ionizing radiation, more availability.
After the primary evaluation of the osteoporosis, the further evaluation are required in some cases such as:
· Women with normal bone density or mild osteopenia: T-score of greater than −1.50 – should have screening for 15 years.
· Women with moderate osteopenia: T-score of −1.50 to −1.99 – should have screening for 5 years.
· Women with advanced osteopenia: T-score of −2.00 to −2.49 - should have screening for 1 year.
Natural History
- In cases with untreated Greenstick fracture the malunion and deformity of arm can be occurred.
The type and frequency of complications of the Greenstick fracture varies. The main complication of the Greenstick fractures is the high risk of refracture due to their instability. A primary greenstick fracture in almost most o the cases can cause recurrent forearm fractures.
In general the following are the most common complications of Greenstick fracture:
- Infection of the bone
- Infection of soft tissue
- Compartment syndrome
- Non-union of the fracture
- Mal-union
- Arm shortening
- Radial nerve Damage
- Vascular injury
- Vascular bleeding
- Re-fracture
- Decreased Motion
- Painful movement
Generally, the prognosis of Greenstick fracture is good. Most of the greenstick fractures heal well with no functional or gross problems in the appearance of the injured bone. But, proper immobilized and proper orthopedic follow-up are required due to the higher risk of refracture, complete fracture and displacement of the fracture.
The related signs and symptoms include:
- Deformity
- Skin lacerations
- Weak pulse
- Open fractures
- Bruising
- Swelling
- Stiffness
- Inability to move
- Pain in touch
- Loss of function of the forearm
- Difficulties in detection of pulses
- Radial nerve damage
In the physical exam the orthopedic surgeon should check the vascular status and amount of swelling in the forearm. In MULTI-trauma patients or in comatose or obtunded patients a tense compartment with neurological signs or stretch pain should be considered as the compartment syndrome, and the compartment pressures should be measured and monitored.
The related signs and symptoms include:
- Edema of the forearm
- Most of the time the edema will be a non-pitting edema
- Depends on the edema extent, it may even lead to compartment syndrome in the anterior and internal compartment of forearm
- Bruising
- As a manifestation of internal injury to the local vessels by trauma or fractures bone
- Decrease in range of motion
- Movement of the fractures limb will be painful if possible at all
- Tenderness
- Deformity
- Fractured bone deformity may be touchable in the internal side of the forearm if the fracture is displaced
In the physical exam the orthopedic surgeon should check the vascular status and amount of swelling in the forearm. In polytrauma patients or in comatose or obtunded patients a tense compartment with neurological signs or stretch pain should be considered as the compartment syndrome, and the compartment pressures should be measured and monitored.
Physical examination of patients with greenstick fracture is usually remarkable for swelling, tenderness, bruises, ecchymosis, deformity and restricted range of motion of the wrist.
- Patients with greenstick fracture usually appears normal unless the patients had a high energy trauma causing the open wound fracture.
Vital Signs
- Weak pulse may be seen when associated with polytrauma.
- Low blood pressure with normal pulse pressure may be present due to compound fracture with blood loss.
Skin
- Skin examination of patients with greenstick fracture includes:
HEENT
- HEENT examination of patients with greenstick fracture is usually normal.
Neck
- Neck examination of patients with greenstick fracture is normal.
Lungs
- Pulmonary examination of patients with greenstick fracture is usually normal.
Heart
- Cardiovascular examination of patients with greenstick fracture is usually normal.
Abdomen
- Abdominal examination of patients with greenstick fracture is usually normal.
Back
- Back examination of patients with greenstick fracture is usually normal.
Genitourinary
- Genitourinary examination of patients with greenstick fracture is usually normal.
Neuromuscular
- Neuromuscular examination of patients with greenstick fracture is usually normal.
- However, some patients may develop neuropraxia of the branch of the Ulnar nerve resulting in decreased sensation of thumb, index and middle finger.
There is a limited laboratory tests useful in the diagnosis of bone fractures such as greenstick fracture. Meanwhile, aged men and women may have some abnormalities in their laboratory findings suggestive of osteoporosis.
- Laboratory tests for the diagnosis of osteoporosis are:
- Complete blood count (CBC)
- Serum total calcium level
- Serum Ionized calcium level
- Serum phosphate level
- Serum alkaline phosphatase level
- Serum 25-(OH)-vitamin D level
X Ray[6]
The orthopedic surgeon should consider to have at least two radiographic projections (ie, anteroposterior [AP] and lateral) of the forearm. These show the fracture, the extent of displacement, and the extent of comminution. The orthopedic surgeon should pay serious attention toward finding any foreign bodies in open fractures and gunshot injuries. Also imperative is to include the elbow and wrist joint in the radiographs of greenstick fracture to ensure that the distal radioulnar joint injuries are not missed
A tuberosity view is helpfull ascertain the rotational displacement of the fracture. Also, it would be helpful for the orthopedic surgeon in planning how much supination or pronation is needed to achieve accurate anatomic reduction. The ulna is laid flat on the cassette with its subcutaneous border in contact with the cassette; the x-ray tube is tilted toward the olecranon by 20°. This radiograph is then compared with a standard set of diagrams that show the prominence of the radial tuberosity in various degrees of pronation and supination in order to determine the scope of the rotational deformity
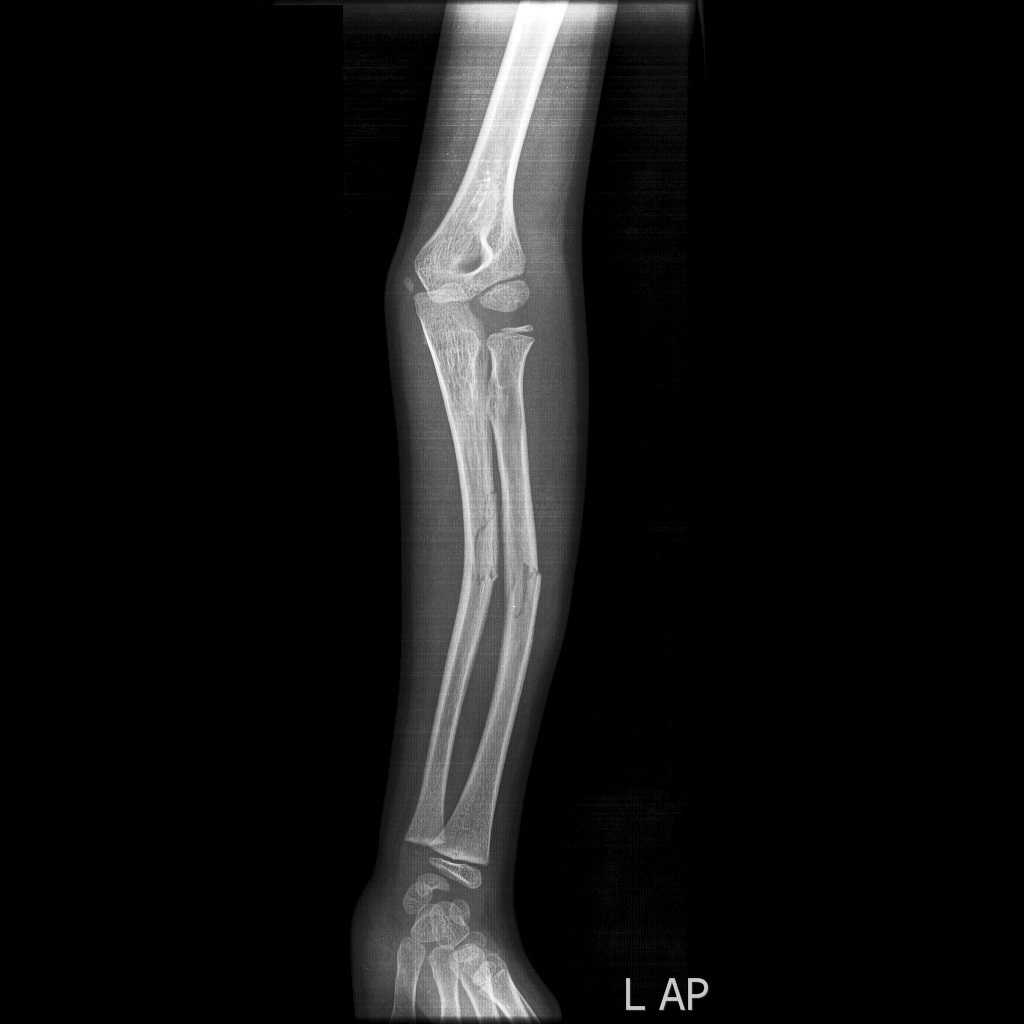
-
Radius and ulna greenstick fractures - AP view
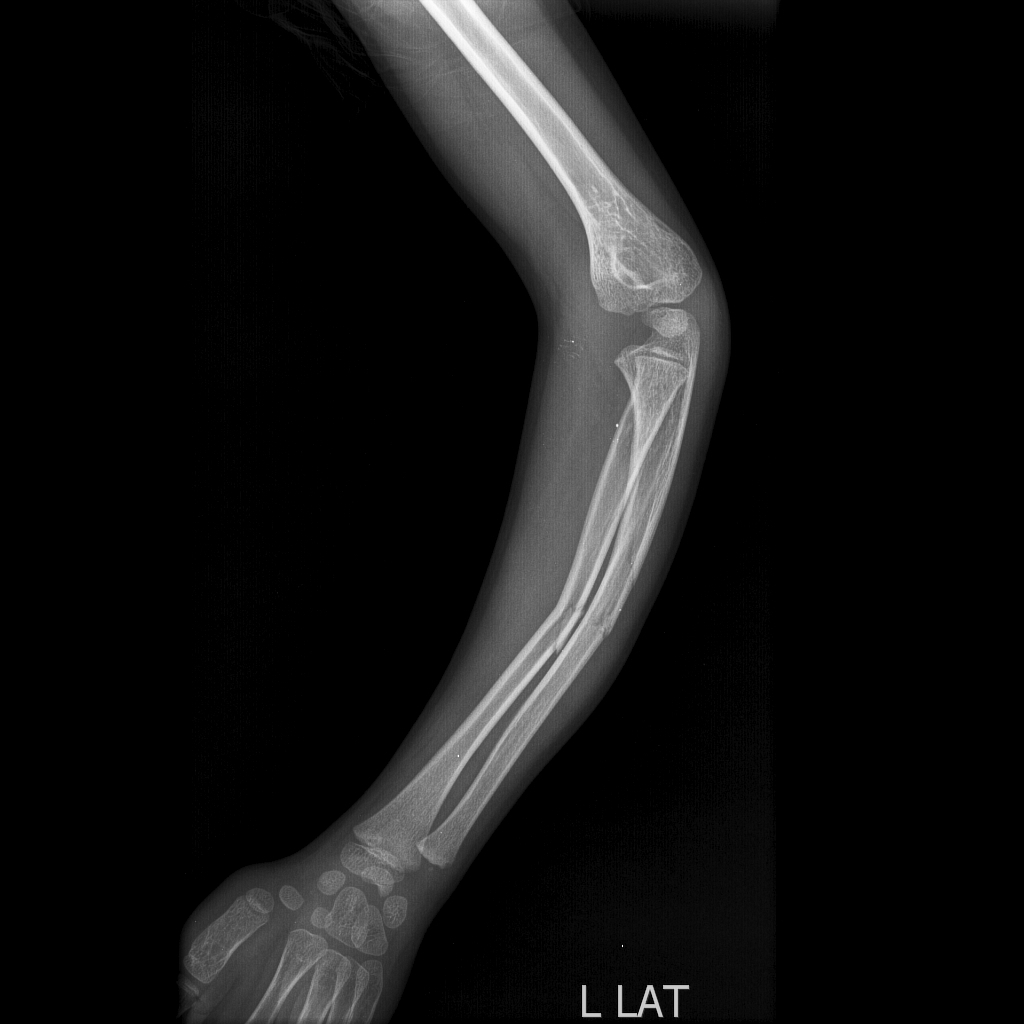
-
Radius and ulna greenstick fractures - Lateral view
CT[6]
- CT-scan in the case of greenstick fracture is the best modality if you can not have an exclusive diagnosis by X-ray itself can not be made.
- Its been reported that the articular fractures of the distal radius were statistically more likely to occur at the intervals between the ligament attachments than at the ligament attachments.
- The most common fracture sites were the center of the sigmoid notch, between the short and long radiolunate ligaments, and the central and ulnar aspects of the scaphoid fossa dorsally. These results suggest that CT may be used to identify the subsequent propagation of the fracture and the likely site of the impaction of the carpus on the distal radius articular surface
Magnetic resonance imaging (MRI) is an expensive technique that should not be used routinely. MRI is a powerful diagnostic tool to assess the abnormalities of the bone, ligaments and soft tissues associated with the Greenstick fractures, but it is known as a limited utility in radioulnar injuries and is not indicated in uncomplicated forearm fractures[1][2][3]. Meanwhile, the MRI can be useful in in following mentioned evaluations: Evaluation of occult fractures Evaluation of the post-traumatic or avascular necrosis of carpal bones Evaluation of tendons Evaluation of nerve Evaluation of carpal tunnel syndrome
Other Imaging Finding[13]s
There are no other imaging findings associated with Greenstick fracture.
Other Diagnostic Studies[13]
There are no other imaging findings associated with Greenstick fracture.
Treatment[13]
The first step in managing a patient with a fracture is to stabilize the patient if he/she is unstable due to blood loss, etc by giving them intravenous fluids and giving them some painkillers if the pain is severe. If only one bone is broken, using cast or brace might be a possible treatment option.
- The first step in managing a patient with a fracture is to stabilize the patient if he/she is unstable due to blood loss, etc by giving them intravenous fluids and giving them some painkillers if the pain is severe.
- In children, the usual plan is to attempt closed reduction followed by cast immobilization. In adults, treatment with immobilization in a molded long arm cast can be used in those rare occasions of a non-displaced fracture of both bones of the forearm. If the fracture shifts in position, it may require surgery to put the bones back together.
- Rigid immobilization is suggested in preference to removable splints in nonoperative treatment for the management of Greenstick bone fractures.
- For all patients with Greenstick fractures, a post-reduction true lateral radiograph is suggested .
- Operative fixation is suggested in preference to cast fixation for fractures with post-reduction radial shortening greater than 3 mm, dorsal tilt greater than 10º, or intra-articular displacement or step-off greater than 2 mm.
- Patients probably do not need to begin early wrist motion routinely after stable fracture fixation.
- Adjuvant treatment of Greenstick fractures with vitamin C is suggested for the prevention of disproportionate pain.
Complications of Non-surgical therapy
Failure of non-surgical therapy is common:
- Re-displacement to its original position even in a cast
- Stiffness
- Post traumatic osteoarthritis leading to wrist pain and loss of function
- Other risks specific to cast treatment include:
- Compression of the swollen arm causing compartment syndrome or carpal tunnel syndrome
- Reflex sympathetic dystrophy is a serious complication
- Stiffness is universal following a prolonged period of immobilization and swelling
Surgery
- There are a variety of methods and implants useful to stabilize the Greenstick fracture, ranging from closed reduction and percutaneous pin fixation to the use of intra-medullary devices.
- However, the most common fixation methods to treat complex Greenstick fracture include external fixation, and open reduction and internal fixation.
External Fixation With or Without Percutaneous Pin Fixation
- Wrist spanning external fixation employs ligamentotaxis to restore and maintain length, alignment, and rotation of ulnar bone.
- Reduction is typically obtained through closed or minimally open methods and preserves the fracture biology.
- The addition of percutaneous pins enhances the ability to reduce and stabilize fracture fragments.
Complications of External Fixation
- Pin tract infection
- Injury to the superficial branch of the nerve
- Complex regional pain syndrome
Open reduction and internal fixation with plates and screws
- This is the most common type of surgical repair for Greenstick fracture
- During this type of procedure, the bone fragments are first repositioned (reduced) into their normal alignment.
- The bones held together with special screws and metal plates attached to the outer surface of the bone.
Complications of open reduction and internal fixation with plates and screws
- Infection
- Damage to nerves and blood vessels
- Synostosis
- Nonunion
Pain after an injury or surgery is a natural part of the healing process.
Medications are often prescribed for short-term pain relief after surgery or an injurysuch as:
- opioids
- non-steroidal anti-inflammatory drugs (NSAIDs)
- local anesthetics
Be aware that although opioids help relieve pain after surgery or an injury, they are a narcotic and can be addictive. It is important to use opioids only as directed by doctor.
Interventions [17]
The following options can be helpful for patients to rehabilitate after their fracture :
- Joints mobilization
- compression bandage
- Soft tissue massage
- Exercises and Activity modification
- Forearm taping
- Forearm bracing
- Complex Greenstick fracture warrant individualized immobilization and rehabilitation strategies.
- Similarly, the addition of a thumb spica cast or orthosis with positioning of the wrist in slight ulnar deviation for management of a comminuted radial column fracture may prevent loss of reduction.
- Because some Greenstick fractures are the result of high-energy injuries, a prolonged period of wrist immobilization and soft-tissue rest may be beneficial and has not been shown to affect clinical outcomes.
- The wrist is typically immobilized for 2 weeks post-operatively in a sugar tong splint with neutral forearm rotation.
- At 6 weeks post-operatively, the wrist is placed into a removable orthosis, and active and passive range of motion (ROM) is initiated.
- Full weight bearing commences at approximately 3 months post-operatively after consolidation of the fracture is noted on radiographs.
- The presence of varying degrees of hand, wrist, and elbow stiffness is inevitable and may result from poor pain control, lack of effort in controlled mobilization, edema, concomitant ipsilateral upper extremity fractures, or peripheral nerve injuries.
- Early stretching and mobilization of the intrinsic and extrinsic tendons of the hand is important to prevent finger stiffness.
- Edema control can be initiated with compression gloves, digital massage, and active and passive ROM of the hand.
- A home exercise program or outpatient occupational therapy is started immediately post-operatively to maintain full range of motion of the hand and limit the development of intrinsic muscle tightness
Operation[20]
The most common surgical techniques include:
Open reduction internal fixation (ORIF)
External fixation
Percutaneous pinning
Combination of the above-mentioned techniques
The proper operative choice is often depends on the type of fracture and it can be categorized into three groups:
partial articular fractures
displaced articular fractures
metaphyseal unstable extra- or metaphyseal minimal articular involvement.
When both bones of the forearm (radius and ulna) are fractured, they are both exposed and provisionally reduced before fixation of either bone is completed. The fracture with the least comminution (usually the ulna) is fixed first. After reduction and provisional fixation of both bones, pronation and supination are examined; if normal, definitive fixation is performed. The general rule is that bone grafting is recommended when more than one third of the circumference of the bone is comminuted.
The common therapeutic options in orthopedic medicine for ulnar fractures are:
- Open reduction and internal fixation with plates and screws
Known as the most common type of surgical repair for forearm fractures.
- Open reduction and internal fixation with rods
- External fixation
The indications for intramedullary nailing are :
- Segmental fractures
- Poor skin condition
- Selected nonunions or failed compression platings
- Multiple injuries
- Diaphyseal fractures in osteopenic patients
Prevention of fracture is an important factor in orthopedic medicine and could cause significant effect on the patients life and healthcare system.Since there are no reliable method for the primary prevention of Greenstick fracture; some routine work ups such as regular exercises and Healthy diet can reduce the chances of fracture.
There are various preventive options to reduce the incidence of fractures:
- Using forearm and wrist guards during practicing sports (skating, biking)
- Using forearm and wrist guards during driving motorbikes
- Avoid falls in elderly individuals
- Prevention and/or treatment of osteoporosis
- Healthy diet
It should be noted that the Post-menopausal women specially older than the age of 65 are at the higher risk of osteoporosis consequently these type of patients at greater risk for the pathological fractures .
So the Calcium and vitamin D supplementation play important role in increasing the bone mineral density (BMD) consequently decrease the risk of fracture in these type of patients. Also, avoiding excessive alcohol and quitting smoking play important role in this regard.
Detecting osteoporosis:
- DEXA(dual-energy x-ray absorptiometry) scan
- Serum calcium and vitamin D levels
- Ultrasonography of the calcaneus
- The primary goal for the treatment of osteoporosis is to reduce longtime fracture risk in patients. Increasing bone mineral density (BMD) in response to the treatment is far less important than improvement of clinical aspects of osteoporosis, i.e., osteoporotic fracture. Therefore, most of the drugs efficacy is measured by the extent they improve the fracture risk instead of increasing BMD.
- During the treatment, if a single fracture happens, it does not necessarily indicate treatment failure or the need to be started on an alternative treatment or patient referral to a specialist.
- Calcium and vitamin D supplementation have been found to be effective in reducing the long term fracture risk, significantly. In order to suggest the people to use vitamin D and calcium supplements, the physician needs to make sure that patient is not able to obtain the nutrients through the daily intake. The available supplemental ions of calcium include calcium carbonate, calcium citrate, and vitamin D3 in various dosage forms.
- Exercise: Exercise promotes the mineralization of bone and bone accumulation particularly during growth. High impact exercise, in particular, has been shown to prevent the development of osteoporosis. However, it can have a negative effect on bone mineralization in cases of poor nutrition, such as anorexia nervosa and celiac disease.
- Nutrition: A diet high in calcium and vitamin D prevents bone loss. Patients at risk for osteoporosis, such as persons with chronic steroid use are generally treated with vitamin D and calcium supplementation. In renal disease, more active forms of vitamin D, such as 1,25-dihydroxycholecalciferol or calcitriol are used; as the kidney cannot adequately generate calcitriol from calcidiol (25-hydroxycholecalciferol), which is the storage form of vitamin D.
- By quitting smoking, osteoporosis as well as other diseases can be prevented.
- Avoiding excessive alcohol intake or drinking only in moderation (1–2 alcoholic beverages/day).
- Taking least possible dosages of certain medications that are associated with osteoporosis (anticonvulsants or corticosteroids).
Related Chapters
External links
- Greenstick Fractures of the Forearm Wheeless' Textbook of Orthopaedics
- Forearm Fractures in Children Patient Information from AAOS
- Fractures Patient Information from AAOS
References
- ↑ 1.0 1.1 Coban YK, Bekircan K (June 2017). "Greenstick Fracture of the Mandible in a Child". J Craniofac Surg. 28 (4): 1116–1117. doi:10.1097/SCS.0000000000003642. PMID 28277480.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 2.7 Atanelov Z, Bentley TP. PMID 30020651. Missing or empty
|title=(help) - ↑ 3.0 3.1 3.2 Cho SM, Kim HG, Yoon SH, Chang KH, Park MS, Park YH, Choi MS (January 2018). "Reappraisal of Neonatal Greenstick Skull Fractures Caused by Birth Injuries: Comparison of 3-Dimensional Reconstructed Computed Tomography and Simple Skull Radiographs". World Neurosurg. 109: e305–e312. doi:10.1016/j.wneu.2017.09.168. PMID 28989045.
- ↑ NADAL R, RUBENS-DUVAL A, VILLIAUMEY J, VIGNEAU J (April 1957). "[Greenstick fractures in pagetic bone]". Rev Rhum Mal Osteoartic (in French). 24 (4): 279–87. PMID 13466785.
- ↑ 5.0 5.1 5.2 5.3 5.4 Berteau JP, Gineyts E, Pithioux M, Baron C, Boivin G, Lasaygues P, Chabrand P, Follet H (October 2015). "Ratio between mature and immature enzymatic cross-links correlates with post-yield cortical bone behavior: An insight into greenstick fractures of the child fibula". Bone. 79: 190–5. doi:10.1016/j.bone.2015.05.045. PMID 26079997.
- ↑ 6.0 6.1 6.2 6.3 6.4 Ting BL, Kalish LA, Waters PM, Bae DS (December 2016). "Reducing Cost and Radiation Exposure During the Treatment of Pediatric Greenstick Fractures of the Forearm". J Pediatr Orthop. 36 (8): 816–820. doi:10.1097/BPO.0000000000000560. PMID 26057068.
- ↑ 7.0 7.1 7.2 7.3 7.4 Schmuck T, Altermatt S, Büchler P, Klima-Lange D, Krieg A, Lutz N, Muermann J, Slongo T, Sossai R, Hasler C (September 2010). "Greenstick fractures of the middle third of the forearm. A prospective multi-centre study". Eur J Pediatr Surg. 20 (5): 316–20. doi:10.1055/s-0030-1255038. PMID 20577951.
- ↑ 8.0 8.1 Aydinli U, Karaeminoğullari O, Tişkaya K, Oztürk C (September 2001). "Dural tears in lumbar burst fractures with greenstick lamina fractures". Spine. 26 (18): E410–5. PMID 11547211.
- ↑ Gierer P, Wichelhaus A, Rotter R (April 2017). "[Fractures of the olecranon]". Oper Orthop Traumatol (in German). 29 (2): 107–114. doi:10.1007/s00064-017-0490-z. PMID 28303286.
- ↑ Siebenlist S, Braun KF (July 2017). "[Elbow dislocation fractures]". Unfallchirurg (in German). 120 (7): 595–610. doi:10.1007/s00113-017-0373-7. PMID 28664232.
- ↑ Levine DG, Aitken MR (August 2017). "Physeal Fractures in Foals". Vet. Clin. North Am. Equine Pract. 33 (2): 417–430. doi:10.1016/j.cveq.2017.03.008. PMID 28687098.
- ↑ Dürr HR, Lienemann A, Stäbler A, Küehne J, Refior HJ (1997). "MRI of posttraumatic cyst-like lesions of bone after a greenstick fracture". Eur Radiol. 7 (8): 1218–20. PMID 9377504.
- ↑ 13.0 13.1 13.2 Elhassan Y, Mahon J, Kiernan D, O Brien T (May 2013). "A greenstick fracture of the patella: a unique fracture in CP crouch gait". BMJ Case Rep. 2013. doi:10.1136/bcr-2013-009717. PMC 3669938. PMID 23704454.
- ↑ Kropman RH, Bemelman M, Segers MJ, Hammacher ER (February 2010). "Treatment of impacted greenstick forearm fractures in children using bandage or cast therapy: a prospective randomized trial". J Trauma. 68 (2): 425–8. doi:10.1097/TA.0b013e3181a0e70e. PMID 19935115.
- ↑ Dancel R, Liles EA, Fiore D (2017). "Acute Pain Management in Hospitalized Children". Rev Recent Clin Trials. 12 (4): 277–283. doi:10.2174/1574887112666170816151232. PMID 28814263.
- ↑ Sanzone AG (May 2016). "Current Challenges in Pain Management in Hip Fracture Patients". J Orthop Trauma. 30 Suppl 1: S1–5. doi:10.1097/BOT.0000000000000562. PMID 27101319.
- ↑ Proubasta IR, De Sena L, Cáceres EP (1999). "Entrapment of the median nerve in a greenstick forearm fracture. A case report and review of the literature". Bull Hosp Jt Dis. 58 (4): 220–3. PMID 10711374.
- ↑ Cheatham SW, Enseki KR, Kolber MJ (November 2015). "Postoperative Rehabilitation After Hip Arthroscopy: A Search for the Evidence". J Sport Rehabil. 24 (4): 413–8. doi:10.1123/JSR.2014-0208a. PMID 26633589.
- ↑ Cheatham SW, Mokha M, Lee M (May 2016). "Postoperative Rehabilitation After Hip Resurfacing: A Systematic Review". J Sport Rehabil. 25 (2): 181–9. doi:10-1123/jsr.2014-0270 Check
|doi=value (help). PMID 25611202. - ↑ Ho-Fung VM, Zapala MA, Lee EY (July 2017). "Musculoskeletal Traumatic Injuries in Children: Characteristic Imaging Findings and Mimickers". Radiol. Clin. North Am. 55 (4): 785–802. doi:10.1016/j.rcl.2017.02.011. PMID 28601180.
- ↑ 21.0 21.1 Christianson MS, Shen W (December 2013). "Osteoporosis prevention and management: nonpharmacologic and lifestyle options". Clin Obstet Gynecol. 56 (4): 703–10. doi:10.1097/GRF.0b013e3182a9d15a. PMID 24047936.
- ↑ 22.0 22.1 22.2 22.3 Compston J (July 2015). "Obesity and fractures in postmenopausal women". Curr Opin Rheumatol. 27 (4): 414–9. doi:10.1097/BOR.0000000000000182. PMID 26002034.
- ↑ 23.0 23.1 Tella SH, Gallagher JC (July 2014). "Prevention and treatment of postmenopausal osteoporosis". J. Steroid Biochem. Mol. Biol. 142: 155–70. doi:10.1016/j.jsbmb.2013.09.008. PMC 4187361. PMID 24176761.
- ↑ 24.0 24.1 Black DM, Rosen CJ (January 2016). "Clinical Practice. Postmenopausal Osteoporosis". N. Engl. J. Med. 374 (3): 254–62. doi:10.1056/NEJMcp1513724. PMID 26789873.