Ebola epidemiology and demographics
|
Ebola Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Postmortem Care |
|
Case Studies |
|
Ebola epidemiology and demographics On the Web |
|
American Roentgen Ray Society Images of Ebola epidemiology and demographics |
|
Risk calculators and risk factors for Ebola epidemiology and demographics |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]
Michael Maddaleni, B.S.;
Guillermo Rodriguez Nava, M.D. [2]
Ahmed Younes M.B.B.CH [3]
Syed Hassan A. Kazmi BSc, MD [4]
Overview
Outbreaks of Ebola have been generally restricted to Africa. Governments and individuals should quickly quarantine the area. Lack of roads and transportation help to contain the outbreak in remote areas. The potential for widespread Ebola virus disease epidemics is considered low due to the high case-fatality rate, the rapidity of the demise of patients, and the often remote areas where infections occur.
2020 Outbreak Updates
- On 31 May 2020, the World Health Organization (WHO) received information that between 18 and 30 May, 4 deaths were reported from Mbandaka Health Zone, Mbandaka city, Equateur Province, the Democratic Republic of the Congo.
- As of 2 June 2020, 8 cases, including 2 confirmed alive cases, 2 suspected cases and 4 deaths (1 confirmed and 3 probable deaths), have been reported. On June 1, 2020, the Ministry of Health (MOH) officially declared the outbreak in Equateur Province.
- This is the 11th outbreak of Ebola virus disease reported in the Democratic Republic of the Congo since the discovery of the virus in 1976.
2019 Outbreak Updates
On June 11, 2019, the Ministry of Health and the World Health Organization (WHO) confirmed a case of Ebola Virus Disease in Uganda. Although there have been numerous previous alerts, this is the first confirmed case in Uganda during the Ebola outbreak on-going in neighboring Democratic Republic of the Congo. A 5-year-old Congolese boy was diagnosed with the virus in Uganda. This is the 10th outbreak in Congo since 1976.
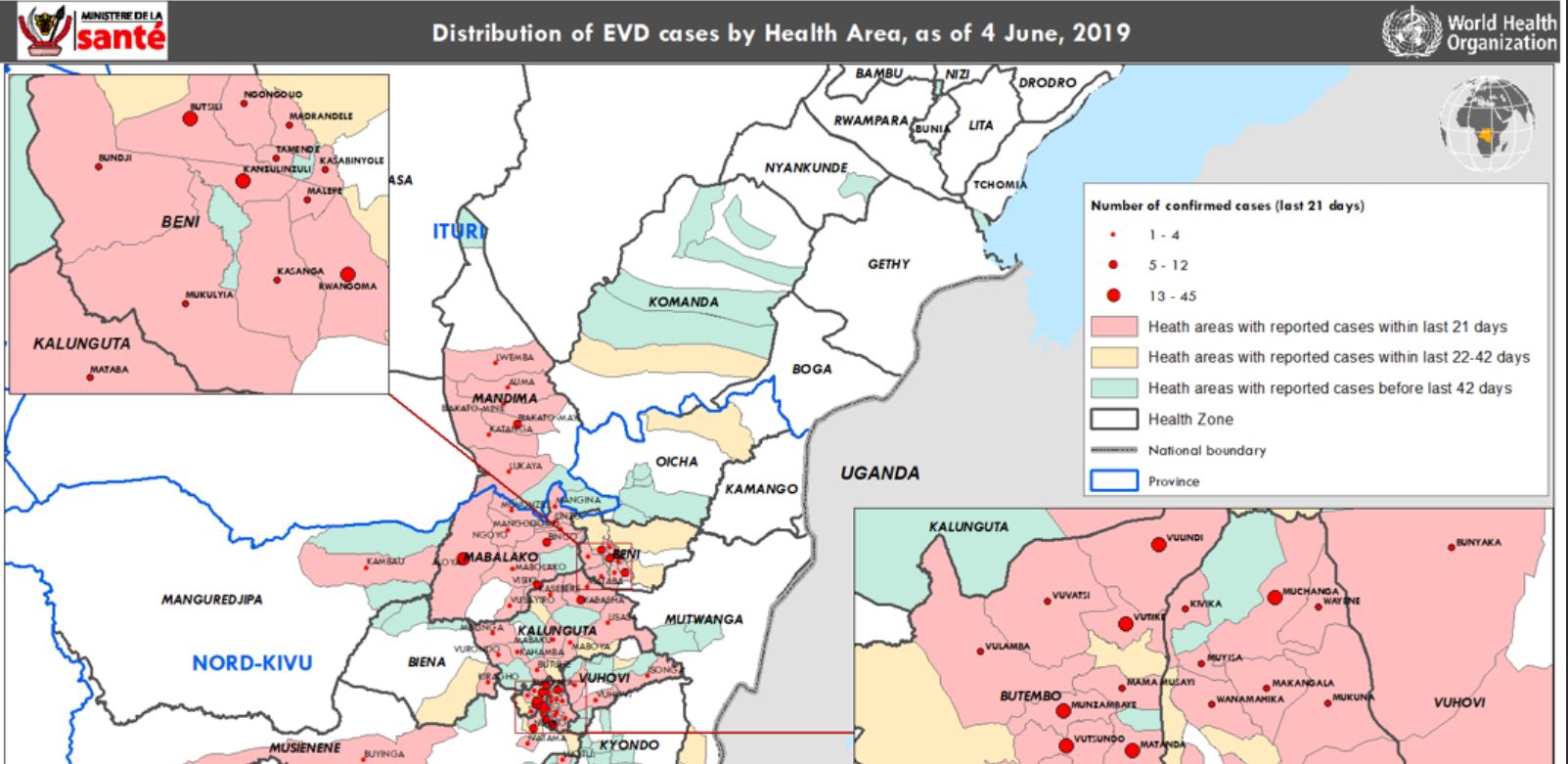
- An increase in the incidence of new cases has been reported from Mabalako Health Zone in recent weeks, and high infection rates continue within Butembo metropolitan. Times between detecting, reporting and admission of cases at Ebola treatment/transit centres (ETCs) remains too long (median 6 days, interquartile range 4–9 days in the past 3 weeks), with about a third (34% in the past 3 weeks) of cases dying outside of ETCs.
- In the 21 days between 15 May to 4 June 2019, 80 health areas within 12 health zones reported new cases, representing 12% of the 664 health areas within North Kivu and Ituri provinces. During this period, a total of 280 confirmed cases were reported, the majority of which were from the Mabalako (27%, n=75), Butembo (23%, n=63), Katwa (16%, n=44), Beni (11%, n=30), Kalunguta (8%, n=23), Mandima (7%, n=19) and Musienene (5%, n=14) health zones.
- As of 4 June 2019, a total of 2025 EVD cases, including 1931 confirmed and 94 probable cases, were reported. A total of 1357 deaths were reported (overall case fatality ratio 67%), including 1263 deaths among confirmed cases. Of the 2025 confirmed and probable cases with known age and sex, 58% (1170) were female, and 29% (589) were children aged less than 18 years. The number of healthcare workers affected has risen to 110 (5% of total cases).
2018 Outbreak Updates
In early May 2018, there was an outbreak of Ebola virus disease (EVD) in the Bikoro region of Equateur Province in the northwestern part of the Democratic Republic of Congo (DRC). The DRC government declared the outbreak on May 8 after two cases were confirmed by laboratory testing at the Institut National de Recherche Biomédicale in Kinshasa. CDC is assisting the DRC government and local and international partners, including the World Health Organization (WHO) to address the outbreak.[1]
- On August 1, 2018, the Ministry of Health of the Democratic Republic of Congo reported an outbreak of Ebola Virus Disease in North Kivu Province. The current outbreak is located in the Mabalako, Beni, Oicha, and Mandima health zones of North Kivu and Ituri provinces. The area is about 780 miles away from Equateur province, where an Ebola outbreak was reported in May 2018. Although the ebolavirus species associated with the current outbreak is the same species that caused the earlier outbreak (Zaire ebolavirus), genetic differences between the viruses suggest the two outbreaks are not linked.
- This is the 10th Ebola outbreak in the Democratic Republic of Congo since the virus was discovered in 1976 in DRC.
Map of DR Congo Affected Regions
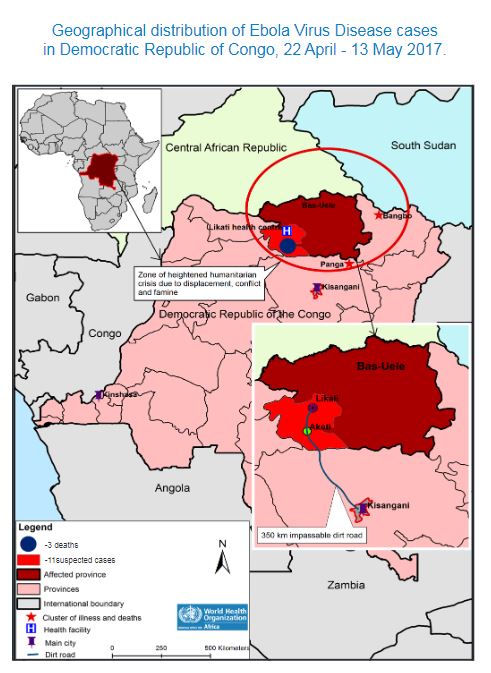
2017 Outbreak updates
| Country | Date | Cases (confirmed and suspected) | Deaths | More details |
| The Democratic Republic of Congo (DRC) | May 12th, 2017 | 9 | 1 (11.1%) |
|
| May 14th, 2017 | 11 | 3 (27%)[2] |
| |
| May 17th, 2017 | 11 | 3 (27%) |
| |
| May 18th, 2017 | 18 | 3 (17%) |
| |
| May 19th, 2017 | 29 | 3 (10%) |
| |
| May 21st, 2017 | 32 | 4 (13%) |
| |
| May 22nd, 2017 | 34 | 4 (12%) |
| |
| May 22nd, 2017 | 37 | 4 (11%) |
| |
| May 22nd, 2017 | 38 | 4 (11%) | ||
| May 25th, 2017 | 43 | 4 (9%) |
| |
| May 28th, 2017 | 43 | 4 (9%) | ||
| May 30th, 2017 | 52 | 4 (7%) |
| |
| June 3rd, 2017 | 52 | 4 (7%) |
| |
| July 2nd, 2017 | 8 (confirmed cases) | 4 (50%) |
{{#ev:youtube|tNZi8MLsMWM}} |
Map of DR Congo Affected Regions

2014 Outbreak
The first reported case of the recent outbreak was diagnosed in Guinea in December 2013. From there it spread to Liberia, Sierra Leone, Nigeria, and Senegal. The first case in the United States was confirmed on September 30, 2014.
| Country | Case definition | Cases | Deaths |
| Guinea | Confirmed | 2762 | 1704 |
| Probable | 387 | 387 | |
| Suspected | 6 | - | |
| All | 3155 | 2091 | |
| Liberia | Confirmed | 3153 | - |
| Probable | 1888 | - | |
| Suspected | 4197 | - | |
| All | 9238 | 4037 | |
| Sierra Leone | Confirmed | 8289 | 3095 |
| Probable | 287 | 208 | |
| Suspected | 2725 | 158 | |
| All | 11,301 | 3461 | |
| Nigeria | Confirmed | 19 | 7 |
| Probable | 1 | 1 | |
| Suspected | 0 | 0 | |
| All | 20 | 8 | |
| Senegal | Confirmed | 1 | 0 |
| Probable | 0 | 0 | |
| Suspected | 0 | 0 | |
| All | 1 | 0 | |
| United States | Confirmed | 3 | 1 |
| Probable | 0 | 0 | |
| Suspected | 0 | 0 | |
| All | 3 | 1 | |
| Spain | Confirmed | 1 | 0 |
| Probable | 0 | 0 | |
| Suspected | 0 | 0 | |
| All | 1 | 0 | |
| Total | 23,719 | 9,598 |
As of February 25, 2015. Data from the World Health Organization
Cases of Ebola in Africa
|
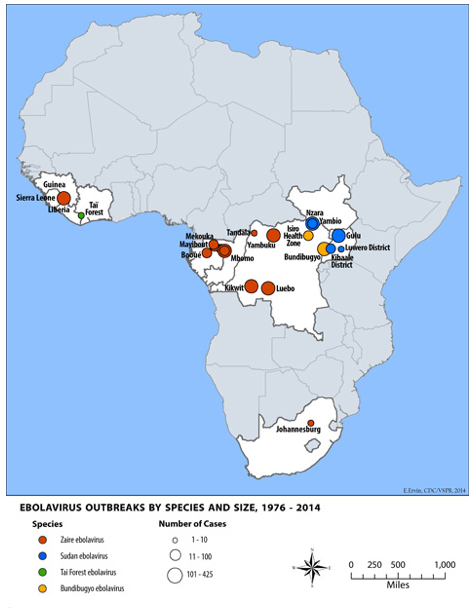 |
Major Historical Outbreaks
Until recently, Ebola outbreaks have been restricted to Africa, with the exception of Reston ebolavirus. The International Committee on Taxonomy of Viruses currently recognizes four species of the Ebola: Zaire virus (ZEBOV), Sudan ebolavirus (SEBOV), Reston ebolavirus (REBOV), and Cote d'Ivoire ebolavirus (CIEBOV).
| Year(s) | Country | Ebola subtype | Reported number of human cases | Reported number (%) of deaths among cases | Situation |
| 1976 | Zaire (Democratic Republic of the Congo - DRC) | Ebola virus | 318 | 280 (88%) | Occurred in Yambuku and surrounding area. Disease was spread by close personal contact and by use of contaminated needles and syringes in hospitals/clinics. This outbreak was the first recognition of the disease. |
| 1976 | Sudan (South Sudan) | Sudan virus | 284 | 151 (53%) | Occurred in Nzara, Maridi and the surrounding area. Disease was spread mainly through close personal contact within hospitals. Many medical care personnel were infected. |
| 1976 | England | Sudan virus | 1 | 0 | Laboratory infection by accidental stick of contaminated needle. |
| 1977 | Zaire | Ebola virus | 1 | 1 (100%) | Noted retrospectively in the village of Tandala. |
| 1979 | Sudan (South Sudan) | Sudan virus | 34 | 22 (65%) | Occured in Nzara, Maridi. Recurrent outbreak at the same site as the 1976 Sudan epidemic. |
| 1989 | USA | Reston virus | 0 | 0 | Ebola-Reston virus was introduced into quarantine facilities in Virginia and Pennsylvania by monkeys imported from the Philippines. |
| 1990 | USA | Reston virus | 4 (asymptomatic) | 0 | Ebola-Reston virus was introduced once again into quarantine facilities in Virginia, and Texas by monkeys imported from the Philippines. Four humans developed antibodies but did not get sick. |
| 1989-1990 | Philippines | Reston virus | 3 (asymptomatic) | 0 | High mortality among cynomolgus macaques in a primate facility responsible for exporting animals in the USA. Three workers in the animal facility developed antibodies but did not get sick. |
| 1992 | Italy | Reston virus | 0 | 0 | Ebola-Reston virus was introduced into quarantine facilities in Sienna by monkeys imported from the same export facility in the Philippines that was involved in the episodes in the United States. No humans were infected. |
| 1994 | Gabon | Ebola virus | 52 | 31 (60%) | Occured in Mékouka and other gold-mining camps deep in the rain forest. Initially thought to be yellow fever; identified as Ebola hemorrhagic fever in 1995. |
| 1994 | Ivory Coast | Taï Forest virus | 1 | 0 | Scientist became ill after conducting an autopsy on a wild chimpanzee in the Tai Forest. The patient was treated in Switzerland. |
| 1995 | Democratic Republic of the Congo (formerly Zaire) | Ebola virus | 315 | 250 (81%) | Occured in Kikwit and surrounding area. Traced to index case-patient who worked in forest adjoining the city. Epidemic spread through families and hospitals. |
| 1996 (January-April) | Gabon | Ebola virus | 37 | 21 (57%) | Occured in Mayibout area. A chimpanzee found dead in the forest was eaten by people hunting for food. Nineteen people who were involved in the butchery of the animal became ill; other cases occured in family members. |
| 1996-1997 (July-January) | Gabon | Ebola virus | 60 | 45 (74%) | Occurred in Booué area with transport of patients to Libreville. Index case-patient was a hunter who lived in a forest camp. Disease was spread by close contact with infected persons. A dead chimpanzee found in the forest at the time was determined to be infected. |
| 1996 | South Africa | Ebola virus | 2 | 1 (50%) | A medical professional traveled from Gabon to Johannesburg, South Africa, after having treated Ebola virus-infected patients and thus having been exposed to the virus. He was hospitalized, and a nurse who took care of him became infected and died. |
| 1996 | USA | Reston virus | 0 | 0 | Ebola-Reston virus was introduced into a quarantine facility in Texas by monkeys imported from the Philippines. No human infections were identified. |
| 1996 | Philippines | Reston virus | 0 | 0 | Ebola-Reston virus was identified in a mokey export facility in the Philippines. No human infections were identified. |
| 1996 | Russia | Ebola virus | 1 | 1 (100%) | Laboratory contamination |
| 2000-2001 | Uganda | Sudan virus | 425 | 224 (53%) | Occurred in Gulu, Masindi, and Mbarara districts of Uganda. The three most important risks associated with Ebola virus infection were attending funerals of Ebola hemorrhagic fever case-patients, having contact with case-patients in one's family, and providing medical care to Ebola case-patients without using adequate personal protective measures. |
| October 2001-March 2002 | Gabon | Ebola virus | 65 | 53 (82%) | Outbreak occured over the border of Gabon and the Republic of the Congo. |
| October 2001-March 2002 | Republic of Congo | Ebola virus | 57 | 43 (75%) | Outbreak occurred over the border of Gabon and the Republic of the Congo. This was the first time that Ebola hemorrhagic fever was reported in the Republic of the Congo. |
| December 2002-April 2003 | Republic of Congo | Ebola virus | 143 | 128 (89%) | Outbreak occurred in the districts of Mbomo and Kéllé in Cuvette Ouest Département. |
| November-December 2003 | Republic of Congo | Ebola virus | 35 | 29 (83%) | Outbreak occured in Mbomo and Mbandza villages located in Mbomo distric, Cuvette Ouest Département. |
| 2004 | Sudan (South Sudan) | Sudan virus | 17 | 7 (41%) | Outbreak occurred in Yambio county of southern Sudan. This outbreak was concurrent with an outbreak of measles in the same area, and several suspected EHF cases were later reclassified as measeles cases. |
| 2004 | Russia | Ebola virus | 1 | 1 (100%) | Laboratory contamination. |
| 2007 | Democratic Republic of Congo | Ebola virus | 264 | 187 (71%) | Outbreak occurred in Kasai Occidental Province. The outbreak was declared over November 20. Last confirmed case on October 4 and last death on October 10. |
| December 2007-January 2008 | Uganda | Bundibugyo virus | 149 | 37 (25%) | Outbreak occurred in Bundibugyo District in western Uganda. First reported occurance of a new strain. |
| November 2008 | Philippines | Reston virus | 6 (asymptomatic) | 0 | First known occurrence of Ebola-Reston in pigs. Strain closely similar to earlier strains. Six workers from the pig farm and slaughterhouse developed antibodies but did not become sick. |
| December 2008-February 2009 | Democratic Republic of the Congo | Ebola virus | 32 | 15 (47%) | Outbreak occurred in the Mweka and luebo health zones of the Province of Kasai Occidental. |
| May-11 | Uganda | Sudan virus | 1 | 1 (100%) | The Ugandan Ministry of Health informed the public that a patient with suspected Ebola Hemorrhagic fever died on May 6, 2011 in the Luwero district, Uganda. The quick diagnosis from a blood sample of Ebola virus was provided by the new CDC Viral Hemorrhagic Fever laboratory installed at the Uganda Viral Research Institute (UVRI). |
| June-October 2012 | Uganda | Sudan virus | 11* | 4* (36.4%) | Outbreak occurred in the Kibaale District of Uganda. Laboratory tests of blood samples were conducted by the UVRI and the U.S. Centers for Disease Control and Prevention (CDC). |
| June-November 2012 | Democratic Republic of the Congo | Bundibugyo virus | 36* | 13* (36.1%) | Outbreak occurred in DRC’s Province Orientale. Laboratory support was provided through CDC and the Public Health Agency of Canada (PHAC)’s field laboratory in Isiro, and through the CDC/UVRI lab in Uganda. The outbreak in DRC has no epidemiologic link to the near contemporaneous Ebola outbreak in the Kibaale district of Uganda. |
| November 2012-January 2013 | Uganda | Sudan virus | 6* | 3* (50%) | Outbreak occurred in the Luwero District. CDC assisted the Ministry of Health in the epidemiologic and diagnostic aspects of the outbreak. Testing of samples by CDC's Viral Special Pathogens Branch occurred at UVRI in Entebbe. |
| March 2014-Present | Guinea, Liberia, and Sierra Leone | Ebola virus | 9936 | 4878 (49.1%) | Outbreak across Guinea, northern Liberia, and now eastern Sierra Leone. |
West Africa outbreak (2013-2014)
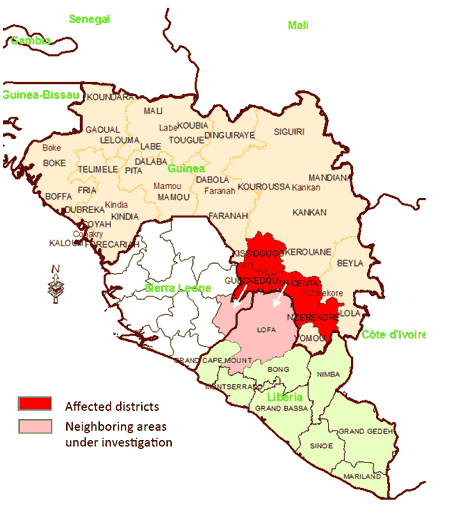
Image extracted from WHO: Ebola Hemorrhagic Fever in Guinea[8]
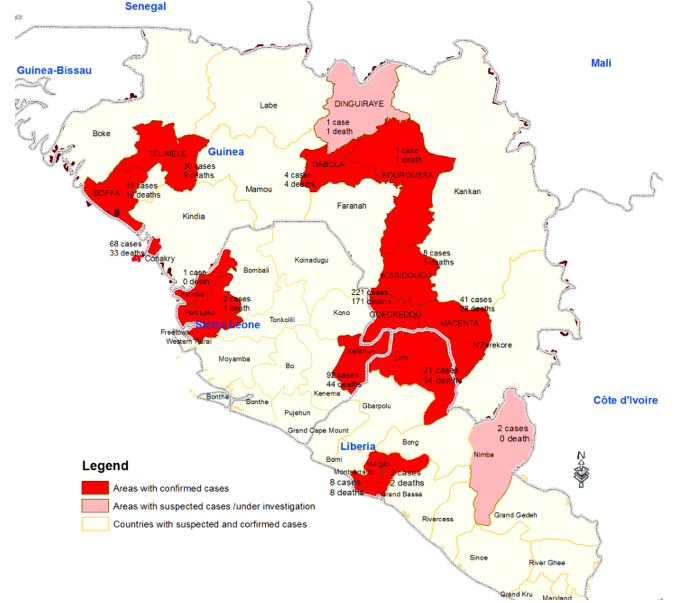
Image extracted from WHO: Ebola Virus Disease (EVD) in West Africa (situation as of 16 June 2014)[9]
On March 23, 2014, the Ministry of Health of Guinea notified the World Health Organization (WHO) of a rapidly evolving outbreak of Ebola virus disease (EVD) in forested areas south eastern Guinea: Guekedou, Macenta, Nzerekore and Kissidougou districts. As of 22 March 2014, a total of 49 cases including 29 deaths (case fatality ratio: 59%) were reported. Four health care workers were among the victims. At the same time, suspected cases in border areas of Liberia and Sierra Leone were being investigated. Six blood samples were tested at Institut Pasteur in Lyon, France, resulting positive for Ebola virus by PCR, confirming the first Ebola virus disease outbreak in Guinea. Preliminary results from sequencing of a part of the L gene showed strong homology with Zaire Ebolavirus. The ministry of health together with the WHO and other partners initiated measures to control the outbreak and prevent further spread. Médecins Sans Frontières, Switzerland (MSF-CH) started working in the affected areas and assisted with the establishment of isolation facilities, and also supported transport of the biological samples from suspected cases and contacts to international reference laboratories for urgent testing. The Emerging and Dangerous Pathogens Laboratory Network (EDPLN) worked with the Guinean VHF Laboratory in Donka, the Institut Pasteur in Lyon, the Institut Pasteur in Dakar, and the Kenema Lassa fever laboratory in Sierra Leone to make available appropriate Filovirus diagnostic capacity in Guinea and Sierra Leone.[8]
On 30 March, 2014, the Ministry of Health of Liberia provided updated details on the suspected and confirmed cases of Ebola virus disease in Liberia. As of 29 March, seven clinical samples, all from adult patients from Foya District, Lofa County, were tested by PCR using Ebola Zaire virus primers by the mobile laboratory of the Institut Pasteur (IP) Dakar in Conakry. Two of those samples tested positive for the ebolavirus. There were 2 deaths among the suspected cases; a 35-year-old woman who died on 21 March tested positive for ebolavirus while a male patient who died on 27 March tested negative. At that time, Foya was the only district in Liberia that reported confirmed or suspected cases of Ebola Hemorrhagic Fever. As of 26 March, Liberia had 27 contacts under medical follow-up. Liberia established a high-level National Task Force to lead the response. Response partners include WHO, the International Red Cross (IRC), Samaritan’s Purse (SP) Liberia, Pentecostal Mission Unlimited (PMU)-Liberia, CHF-WASH Liberia, PLAN-Liberia, UNFPA and UNICEF.[10]
On 3 April, 2014, the outbreak was confirmed to be caused by a strain of ebolavirus with very close homology (98%) to the Zaire ebolavirus. This is the first time the disease has been detected in West Africa.[11] [12]
Democratic Republic of the Congo (2007)
As of August 30, 2007, 103 people (100 adults and three children) were infected by a suspected hemorrhagic fever outbreak in the village of Mweka, Democratic Republic of the Congo (DRC). The outbreak started after the funerals of two village chiefs, and 217 people in four villages fell ill. The World Health Organization sent a team to take blood samples for analysis and confirmed that many of the cases are the result of the Ebola virus [13]. The Congo's last major Ebola epidemic killed 245 people in 1995 inKikwit, about 200 miles from the source of the Aug. 2007 outbreak.[14]
On November 30, 2007, the Uganda Ministry of Health confirmed an outbreak of Ebola in the Bundibugyo District. After confirmation of samples tested by the United States National Reference Laboratories and the Centers for Disease Control, the World Health Organization confirmed the presence of a new species of the Ebola virus.[15] The epidemic came to an official end on February 20, 2008. 149 cases of this new strain were reported and 37 of those led to deaths.
Uganda Outbreak (2000)
On October 8, 2000, an outbreak of an unusual febrile illness with occasional hemorrhage and significant mortality was reported to the Ministry of Health (MoH) in Kampala by the superintendent of St. Mary's Hospital in Lacor, and the District Director of Health Services in the Gulu District. A preliminary assessment conducted by MoH found additional cases in Gulu District and in Gulu Hospital, the regional referral hospital. On October 15, suspicion of Ebola hemorrhagic fever (EHF) was confirmed when the National Institute of Virology (NIV), Johannesburg, South Africa, identified Ebola virus infection among specimens from patients, including health-care workers at St. Mary's Hospital. This report describes surveillance and control activities related to the EHF outbreak and presents preliminary clinical and epidemiologic findings.
Control activities were organized around surveillance and epidemiology, clinical case management, social education and mobilization, and coordination and logistic support. An active EHF surveillance system was initiated to determine the extent and magnitude of the outbreak, identify foci of disease activity, and detect cases early. Ill persons were encouraged to be assessed at a hospital and, if indicated, to be hospitalized to reduce further community transmission. Targeted prevention activities included follow-up of contacts of identified cases for 21 days; establishment of trained burial teams for all potential and confirmed EHF deaths; community education; cessation of traditional healing and burial practices; cessation of large public gatherings; and updates of hospital infection-control measures, including isolation wards. Laboratory testing was performed at a field laboratory established at St. Mary's Hospital by CDC and supplemented by additional testing at CDC and NIV. Sequence analysis revealed that the virus associated with this outbreak was Ebola-Sudan and differed at the nucleotide sequence level from earlier Ebola-Sudan isolates by 3.3% and 4.2% in the polymerase (362 nucleotides sequenced) and nucleocapsid (146 nucleotides sequenced) protein encoding genes, respectively.
During the third week of October, active surveillance was established and included three case notification categories: alert, suspect, and probable. The alert category comprised persons with sudden onset of high fever, sudden death, or hemorrhage, and was used by community members to alert health-care personnel. The suspect category comprised persons with fever and contact with a potential case-patient; persons with unexplained bleeding; persons with fever and three or more specified symptoms (i.e., headache, vomiting, anorexia, diarrhea, weakness or severe fatigue, abdominal pain, body aches or joint pains, difficulty swallowing, difficulty breathing, and hiccups), and all unexplained deaths. The suspect category was used by mobile surveillance teams to determine whether a patient required transport to an isolation ward. The probable category included persons who met these criteria and were assessed and reported by a physician. Laboratory tests included virus antigen detection and antibody ELISA tests and reverse transcriptase polymerase chain reaction. Laboratory-confirmed case-patients were defined as patients who met the surveillance case definitions and were either positive for Ebola virus antigen or Ebola IgG antibody.
During October 5--November 27, among 62 persons with laboratory-confirmed EHF admitted to Gulu Hospital, symptoms included diarrhea (66%), asthenia(64%),anorexia (61%), headache (63%), nausea and vomiting (60%), abdominal pain (55%), and chest pain (48%). Patients presented for care a mean of 8 days (range: 2--20 days) after symptom onset. Bleeding occurred in 12 (20%) patients and primarily involved the gastrointestinal tract. Among the 62 confirmed case-patients, 36 (58%) died; among patients aged <15 years, four of five died (case fatality: 80%). Spontaneous abortions were reported among pregnant women infected with EHF. Patients who died usually exhibited a rapid progression of shock, increasing coagulopathy, and loss ofconsciousness.
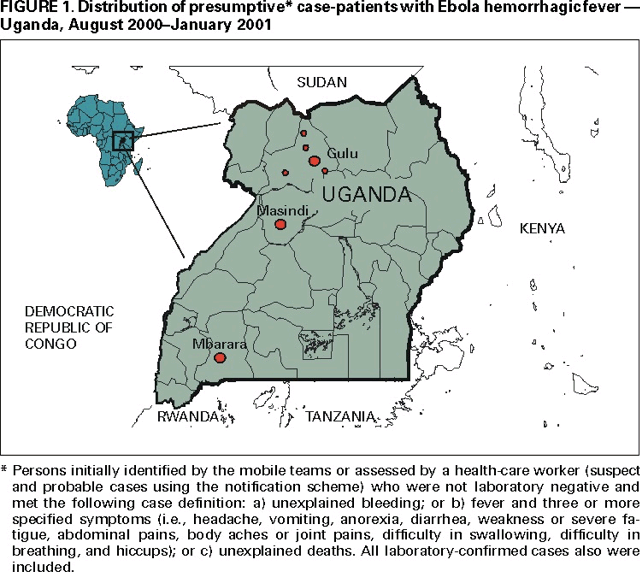
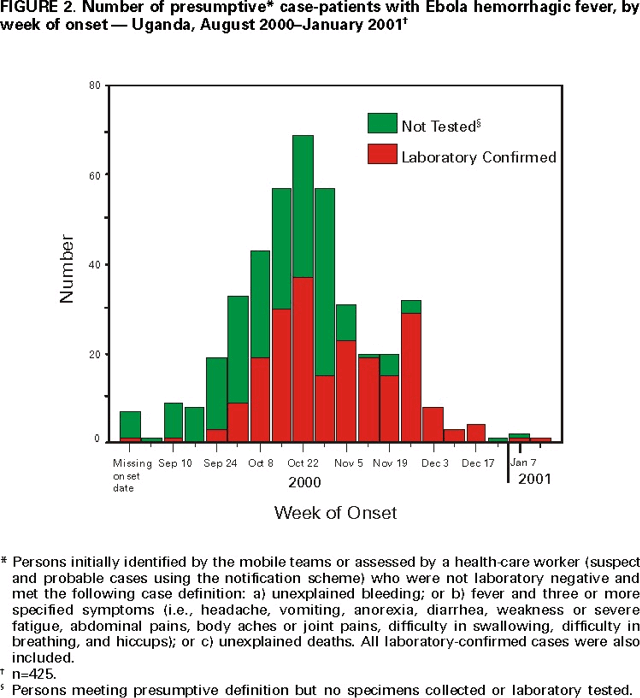
As of January 23, 2001, 425 presumptive* case-patients with 224 (53%) deaths attributed to EHF were recorded from three districts in Uganda: 393 (93%) from Gulu, 27 (6%) from Masindi, and five (1%) from Mbarara. The combined area comprises approximately 11,700 square miles (31,000 square kilometers; 2000 combined population: 1.8 million) (See the map of Uganda below) (1). Although the cluster of cases in early October triggered identification of the outbreak and response measures, investigations (i.e., case-record review and interviews with surviving patients or their surrogates) identified cases occurring in the community and patients hospitalized several weeks earlier. The onset of illness of the earliest presumptive case was August 30, 2000, and onset of last presumptive case was January 9, 2001 (See the graph below the map of Uganda). The ages of presumptive case-patients ranged from 3 days--72 years (median: 28 years); 269 (63%) were women. Mean time from symptom onset to death was 8 days (95% confidence interval=±5 days); 218 (51%) presumptive cases were laboratory confirmed.
Epidemiologic investigations identified the three most important means of transmission as attending funerals of presumptive EHF case-patients where ritual contact with the deceased occurred, and intrafamilial or nosocomial transmission. Fourteen (64%) of 22 health-care workers in Gulu were infected after establishing the isolation wards; these incidences led to the reinforcement of infection-control measures. Two distant focal outbreaks were initiated by movement of infected contacts of EHF cases from Gulu to Mbarara and Masindi districts. National notification and surveillance efforts led to the rapid identification of these foci and effective containment.
 |
 |
References
- ↑ "2018 Democratic Republic of the Congo, Bikoro | Democratic Republic of Congo | Ebola (Ebola Virus Disease) | CDC".
- ↑ 2.0 2.1 "Ebola kills 3 in Democratic Republic of Congo, WHO says - CNN.com".
- ↑ "Congo's Ebola outbreak threatens CAR – WHO - Vanguard News".
- ↑ "apps.who.int" (PDF).
- ↑ "WHO declares an end to the Ebola outbreak in the Democratic Republic of the Congo - WHO | Regional Office for Africa".
- ↑ 6.0 6.1 "CDC Ebola Hemorrhagic Fever Distribution Map".
- ↑ "CDC Chronology of Ebola Hemorrhagic Fever Outbreaks".
- ↑ 8.0 8.1 "Ebola Hemorrhagic Fever in Guinea".
- ↑ "Ebola Virus Disease (EVD) in West Africa (situation as of 16 June 2014)".
- ↑ "30 March 2014 Ebola virus disease in Liberia".
- ↑ "3 April 2014 Ebola virus disease: background and summary".
- ↑ "Ebola virus disease, West Africa (Situation as of 17 June 2014)".
- ↑ "Ebola Outbreak Confirmed in Congo". NewScientist.com. 2007-09-11. Retrieved 2008-02-25.
- ↑ "Mystery DR Congo fever kills 100". BBC News. 2007-08-31. Retrieved 2008-02-25.
- ↑ "Uganda: Deadly Ebola Outbreak Confirmed -UN". UN News Service. 2007-11-30. Retrieved 2008-02-25.
- ↑ 16.0 16.1 "Public Health Image Library (PHIL), Centers for Disease Control and Prevention".