Clonazepam
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Sophia Saad, Associate Editor - WikiDoc [2];Aparna Vuppala, M.B.B.S. [3]
WikiDoc MAKES NO GUARANTEE OF VALIDITY. WikiDoc is not a professional health care provider, nor is it a suitable replacement for a licensed healthcare provider. WikiDoc is intended to be an educational tool, not a tool for any form of healthcare delivery. The educational content on WikiDoc drug pages is based upon the FDA package insert, National Library of Medicine content and practice guidelines / consensus statements. WikiDoc does not promote the administration of any medication or device that is not consistent with its labeling. Please read our full disclaimer here.
Overview
Clonazepam is a benzodiazepine that is FDA approved for the treatment of lennox-gastaut syndrome, (petit mal variant), akinetic and myoclonic seizures, panic disorder, with or without agoraphobia. Common adverse reactions include ataxia, coordination problem, dizziness, somnolence, behavior problem, upper respiratory infection, fatigue.
Adult Indications and Dosage
FDA-Labeled Indications and Dosage (Adult)
Seizure Disorders
- Dosing information
- Adults
- Initial dose: not exceed 1.5 mg PO tid. Dosage may be increased in increments of 0.5 mg to 1 mg every 3 days until seizures are adequately controlled or until side effects preclude any further increase. Maintenance dosage must be individualized for each patient depending upon response. Maximum recommended daily dose is 20 mg.
- The use of multiple anticonvulsants may result in an increase of depressant adverse effects. This should be considered before adding clonazepam tablets to an existing anticonvulsant regimen.
- Geriatric Patients
- There is no clinical trial experience with clonazepam tablets in seizure disorder patients 65 years of age and older. In general, elderly patients should be started on low doses of clonazepam tablets and observed closely
Panic disorder
- Dosing införmation
- Adults
- Initial dose: 0.25 mg bid. An increase to the target dose for most patients of 1 mg/day may be made after 3 days.
- Recommended dose: 1 mg/day is based on the results from a fixed dose study in which the optimal effect was seen at 1 mg/day. Higher doses of 2 mg/day, 3 mg/day and 4 mg/day in that study were less effective than the 1 mg/day dose and were associated with more adverse effects.
- Maximum dosage: 4 mg/day, and in those instances, the dose may be increased in increments of 0.125 mg to 0.25 mg bid every 3 days until panic disorder is controlled or until side effects make further increases undesired. To reduce the inconvenience of somnolence, administration of one dose at bedtime may be desirable.
- Treatment should be discontinued gradually, with a decrease of 0.125 mg bid every 3 days, until the drug is completely withdrawn.
- There is no body of evidence available to answer the question of how long the patient treated with clonazepam should remain on it. Therefore, the physician who elects to use clonazepam tablets for extended periods should periodically reevaluate the long-term usefulness of the drug for the individual patient.
- Geriatric Patients
- There is no clinical trial experience with clonazepam tablets in panic disorder patients 65 years of age and older. In general, elderly patients should be started on low doses of clonazepam tablets and observed closely.
Off-Label Use and Dosage (Adult)
Guideline-Supported Use
There is limited information regarding Off-Label Guideline-Supported Use of clonazepam in adult patients.
Non–Guideline-Supported Use
Restless Leg Syndrome
- Dosing information
- 0.5 to 2 mg at bedtime[1]
Sleep Walking Disorder
- Dosing information
- 0.25 to 2 mg at bedtime[2]
Social Phobia
- Dosing information
- 1 to 2.5 mg daily [3]
Pediatric Indications and Dosage
FDA-Labeled Indications and Dosage (Pediatric)
Seizure Disorder
- Dosing information
- Lonazepam tablets are administered orally. In order to minimize drowsiness, the initial dose for infants and children (up to 10 years of age or 30 kg of body weight) should be between 0.01 mg/kg/day and 0.03 mg/kg/day but not to exceed 0.05 mg/kg/day given in two or three divided doses. Dosage should be increased by no more than 0.25 mg to 0.5 mg every third day until a daily maintenance dose of 0.1 mg/kg to 0.2 mg/kg of body weight has been reached, unless seizures are controlled or side effects preclude further increase. Whenever possible, the daily dose should be divided into three equal doses. If doses are not equally divided, the largest dose should be given before retiring.
Panic Disorder
- Dosing information
- There is no clinical trial experience with clonazepam tablets in panic disorder patients under 18 years of age.
Off-Label Use and Dosage (Pediatric)
Guideline-Supported Use
There is limited information regarding Off-Label Guideline-Supported Use of clonazepam in pediatric patients.
Non–Guideline-Supported Use
There is limited information regarding Off-Label Non–Guideline-Supported Use of clonazepam in pediatric patients.
Contraindications
Clonazepam should not be used in patients with a history of sensitivity to benzodiazepines, nor in patients with clinical or biochemical evidence of significant liver disease. It may be used in patients with open angle glaucoma who are receiving appropriate therapy but is contraindicated in acute narrow angle glaucoma.
Warnings
Interference with Cognitive and Motor Performance
Since clonazepam produces CNS depression, patients receiving this drug should be cautioned against engaging in hazardous occupations requiring mental alertness, such as operating machinery or driving a motor vehicle. They should also be warned about the concomitant use of alcohol or other CNS-depressant drugs during clonazepam therapy.
Suicidal Behavior and Ideation
Antiepileptic drugs (AEDs), including clonazepam, increase the risk of suicidal thoughts or behavior in patients taking these drugs for any indication. Patients treated with any AED for any indication should be monitored for the emergence or worsening of depression, suicidal thoughts or behavior, and/or any unusual changes in mood or behavior. Pooled analyses of 199 placebo-controlled clinical trials (mono- and adjunctive therapy) of 11 different AEDs showed that patients randomized to one of the AEDs had approximately twice the risk (adjusted Relative Risk 1.8, 95% CI:1.2, 2.7) of suicidal thinking or behavior compared to patients randomized to placebo. In these trials, which had a median treatment duration of 12 weeks, the estimated incidence rate of suicidal behavior or ideation among 27,863 AED-treated patients was 0.43% compared to 0.24% among 16,029 placebo-treated patients, representing an increase of approximately one case of suicidal thinking or behavior for every 530 patients treated. There were four suicides in drug-treated patients in the trials and none in placebo-treated patients, but the number is too small to allow any conclusion about drug effect on suicide. The increased risk of suicidal thoughts or behavior with AEDs was observed as early as one week after starting drug treatment with AEDs and persisted for the duration of treatment assessed. Because most trials included in the analysis did not extend beyond 24 weeks, the risk of suicidal thoughts or behavior beyond 24 weeks could not be assessed. The risk of suicidal thoughts or behavior was generally consistent among drugs in the data analyzed. The finding of increased risk with AEDs of varying mechanisms of action and across a range of indications suggests that the risk applies to all AEDs used for any indication. The risk did not vary substantially by age (5 to 100 years) in the clinical trials analyzed. Table 1 shows absolute and relative risk by indication for all evaluated AEDs.

The relative risk for suicidal thoughts or behavior was higher in clinical trials for epilepsy than in clinical trials for psychiatric or other conditions, but the absolute risk differences were similar for the epilepsy and psychiatric indications. Anyone considering prescribing clonazepam or any other AED must balance the risk of suicidal thoughts or behavior with the risk of untreated illness. epilepsy and many other illnesses for which AEDs are prescribed are themselves associated with morbidity and mortality and an increased risk of suicidal thoughts and behavior. Should suicidal thoughts and behavior emerge during treatment, the prescriber needs to consider whether the emergence of these symptoms in any given patient may be related to the illness being treated. Patients, their caregivers, and families should be informed that AEDs increase the risk of suicidal thoughts and behavior and should be advised of the need to be alert for the emergence or worsening of the signs and symptoms of depression, any unusual changes in mood or behavior, or the emergence of suicidal thoughts, behavior, or thoughts about self-harm. Behaviors of concern should be reported immediately to healthcare providers.
Pregnancy Risks
Data from several sources raise concerns about the use of clonazepam during pregnancy.
Animal Findings
In three studies in which clonazepam was administered orally to pregnant rabbits at doses of 0.2 mg/kg/day, 1 mg/kg/day, 5 mg/kg/day or 10 mg/kg/day (low dose approximately 0.2 times the maximum recommended human dose of 20 mg/day for seizure disorders and equivalent to the maximum dose of 4 mg/day for panic disorder, on a mg/m2 basis) during the period of organogenesis, a similar pattern of malformations (cleft palate, open eyelid, fused sternebrae and limb defects) was observed in a low, non-dose-related incidence in exposed litters from all dosage groups. Reductions in maternal weight gain occurred at dosages of 5 mg/kg/day or greater and reduction in embryo-fetal growth occurred in one study at a dosage of 10 mg/kg/day. No adverse maternal or embryo-fetal effects were observed in mice and rats following administration during organogenesis of oral doses up to 15 mg/kg/day or 40 mg/kg/day, respectively (4 and 20 times the maximum recommended human dose of 20 mg/day for seizure disorders and 20 and 100 times the maximum dose of 4 mg/day for panic disorder, respectively, on a mg/m2 basis).
General Concerns and Considerations about Anticonvulsants
Recent reports suggest an association between the use of anticonvulsant drugs by women with epilepsy and an elevated incidence of birth defects in children born to these women. Data are more extensive with respect to diphenylhydantoin and phenobarbital, but these are also the most commonly prescribed anticonvulsants; less systematic or anecdotal reports suggest a possible similar association with the use of all known anticonvulsant drugs. In children of women treated with drugs for epilepsy, reports suggesting an elevated incidence of birth defects cannot be regarded as adequate to prove a definite cause and effect relationship. There are intrinsic methodologic problems in obtaining adequate data on drug teratogenicity in humans; the possibility also exists that other factors, (e.g., genetic factors or the epileptic condition itself), may be more important than drug therapy in leading to birth defects. The great majority of mothers on anticonvulsant medication deliver normal infants. It is important to note that anticonvulsant drugs should not be discontinued in patients in whom the drug is administered to prevent seizures because of the strong possibility of precipitating status epilepticus with attendant hypoxia and threat to life. In individual cases where the severity and frequency of the seizure disorder are such that the removal of medication does not pose a serious threat to the patient, discontinuation of the drug may be considered prior to and during pregnancy; however, it cannot be said with any confidence that even mild seizures do not pose some hazards to the developing embryo or fetus.
General Concerns about Benzodiazepines
An increased risk of congenital malformations associated with the use of benzodiazepine drugs has been suggested in several studies. There may also be non-teratogenic risks associated with the use of benzodiazepines during pregnancy. There have been reports of neonatal flaccidity, respiratory and feeding difficulties, and hypothermia in children born to mothers who have been receiving benzodiazepines late in pregnancy. In addition, children born to mothers receiving benzodiazepines late in pregnancy may be at some risk of experiencing withdrawal symptoms during the postnatal period. Advice Regarding the use of Clonazepam in Women of Childbearing Potential In general, the use of clonazepam in women of childbearing potential, and more specifically during known pregnancy, should be considered only when the clinical situation warrants the risk to the fetus. The specific considerations addressed above regarding the use of anticonvulsants for epilepsy in women of childbearing potential should be weighed in treating or counseling these women. Because of experience with other members of the benzodiazepine class, clonazepam is assumed to be capable of causing an increased risk of congenital abnormalities when administered to a pregnant woman during the first trimester. Because use of these drugs is rarely a matter of urgency in the treatment of panic disorder, their use during the first trimester should almost always be avoided. The possibility that a woman of childbearing potential may be pregnant at the time of institution of therapy should be considered. If this drug is used during pregnancy, or if the patient becomes pregnant while taking this drug, the patient should be apprised of the potential hazard to the fetus. Patients should also be advised that if they become pregnant during therapy or intend to become pregnant, they should communicate with their physician about the desirability of discontinuing the drug.
Withdrawal Symptoms
Withdrawal symptoms of the barbiturate type have occurred after the discontinuation of benzodiazepines
PRECAUTIONS
General
Worsening of Seizures
When used in patients in whom several different types of seizure disorders coexist, clonazepam may increase the incidence or precipitate the onset of generalized tonic-clonic seizures (grand mal). This may require the addition of appropriate anticonvulsants or an increase in their dosages. The concomitant use of valproic acid and clonazepam may produce absence status.
Laboratory Testing during Long-Term Therapy
Periodic blood counts and liver function tests are advisable during long-term therapy with clonazepam.
Risks of Abrupt Withdrawal
The abrupt withdrawal of clonazepam, particularly in those patients on long-term, high-dose therapy, may precipitate status epilepticus. Therefore, when discontinuing clonazepam, gradual withdrawal is essential. While clonazepam is being gradually withdrawn, the simultaneous substitution of another anticonvulsant may be indicated.
Caution in Renally Impaired Patients
Metabolites of clonazepam are excreted by the kidneys; to avoid their excess accumulation, caution should be exercised in the administration of the drug to patients with impaired renal function.
Clonazepam may produce an increase in salivation. This should be considered before giving the drug to patients who have difficulty handling secretions. Because of this and the possibility of respiratory depression, clonazepam should be used with caution in patients with chronic respiratory diseases.
Adverse Reactions
Clinical Trials Experience
The adverse experiences for clonazepam are provided separately for patients with seizure disorders and with panic disorder.
Seizure Disorders
The most frequently occurring side effects of clonazepam are referable to CNS depression. Experience in treatment of seizures has shown that drowsiness has occurred in approximately 50% of patients and ataxia in approximately 30%. In some cases, these may diminish with time; behavior problems have been noted in approximately 25% of patients. Others, listed by system, are:
Neurologic: abnormal eye movements, aphonia, choreiform movements, coma, diplopia, dysarthria, dysdiadochokinesis, “glassy-eyed” appearance, headache, hemiparesis, hypotonia, nystagmus, respiratory depression, slurred speech, tremor, vertigo
Psychiatric: confusion, depression, amnesia, hallucinations, hysteria, increased libido, insomnia, psychosis (the behavior effects are more likely to occur in patients with a history of psychiatric disturbances).
The following paradoxical reactions have been observed: excitability, irritability, aggressive behavior, agitation, nervousness, hostility, anxiety, sleep disturbances, nightmares and vivid dreams
Respiratory: chest congestion, rhinorrhea, shortness of breath, hypersecretion in upper respiratory passages
Cardiovascular: palpitations
Dermatologic: hair loss, hirsutism, skin rash, ankle and facial edema
Gastrointestinal: anorexia, coated tongue, constipation, diarrhea, dry mouth, encopresis, gastritis, increased appetite, nausea, sore gums
Genitourinary: dysuria, enuresis, nocturia, urinary retention
Musculoskeletal: muscle weakness, pains
Miscellaneous: dehydration, general deterioration, fever, lymphadenopathy, weight loss or gain
Hematopoietic: anemia, leukopenia, thrombocytopenia, eosinophilia
Hepatic: hepatomegaly, transient elevations of serum transaminases and alkaline phosphatase
Panic disorder
Adverse events during exposure to clonazepam were obtained by spontaneous report and recorded by clinical investigators using terminology of their own choosing. Consequently, it is not possible to provide a meaningful estimate of the proportion of individuals experiencing adverse events without first grouping similar types of events into a smaller number of standardized event categories. In the tables and tabulations that follow, CIGY dictionary terminology has been used to classify reported adverse events, except in certain cases in which redundant terms were collapsed into more meaningful terms, as noted below. The stated frequencies of adverse events represent the proportion of individuals who experienced, at least once, a treatment-emergent adverse event of the type listed. An event was considered treatment-emergent if it occurred for the first time or worsened while receiving therapy following baseline evaluation.
Adverse Findings Observed in Short-Term, Placebo Controlled Trials
Adverse Events Associated With Discontinuation of Treatment Overall, the incidence of discontinuation due to adverse events was 17% in clonazepam compared to 9% for placebo in the combined data of two 6- to 9-week trials. The most common events (≥1%) associated with discontinuation and a dropout rate twice or greater for clonazepam than that of placebo included the following:

Adverse Events Occurring at an Incidence of 1% or More Among Clonazepam-Treated Patients:
Table 3 enumerates the incidence, rounded to the nearest percent, of treatment-emergent adverse events that occurred during acute therapy of panic disorder from a pool of two 6- to 9-week trials. Events reported in 1% or more of patients treated with clonazepam (doses ranging from 0.5 mg/day to 4 mg/day) and for which the incidence was greater than that in placebo-treated patients are included. The prescriber should be aware that the figures in Table 3 cannot be used to predict the incidence of side effects in the course of usual medical practice where patient characteristics and other factors differ from those that prevailed in the clinical trials. Similarly, the cited frequencies cannot be compared with figures obtained from other clinical investigations involving different treatments, uses and investigators. The cited figures, however, do provide the prescribing physician with some basis for estimating the relative contribution of drug and non drug factors to the side effect incidence in the population studied.
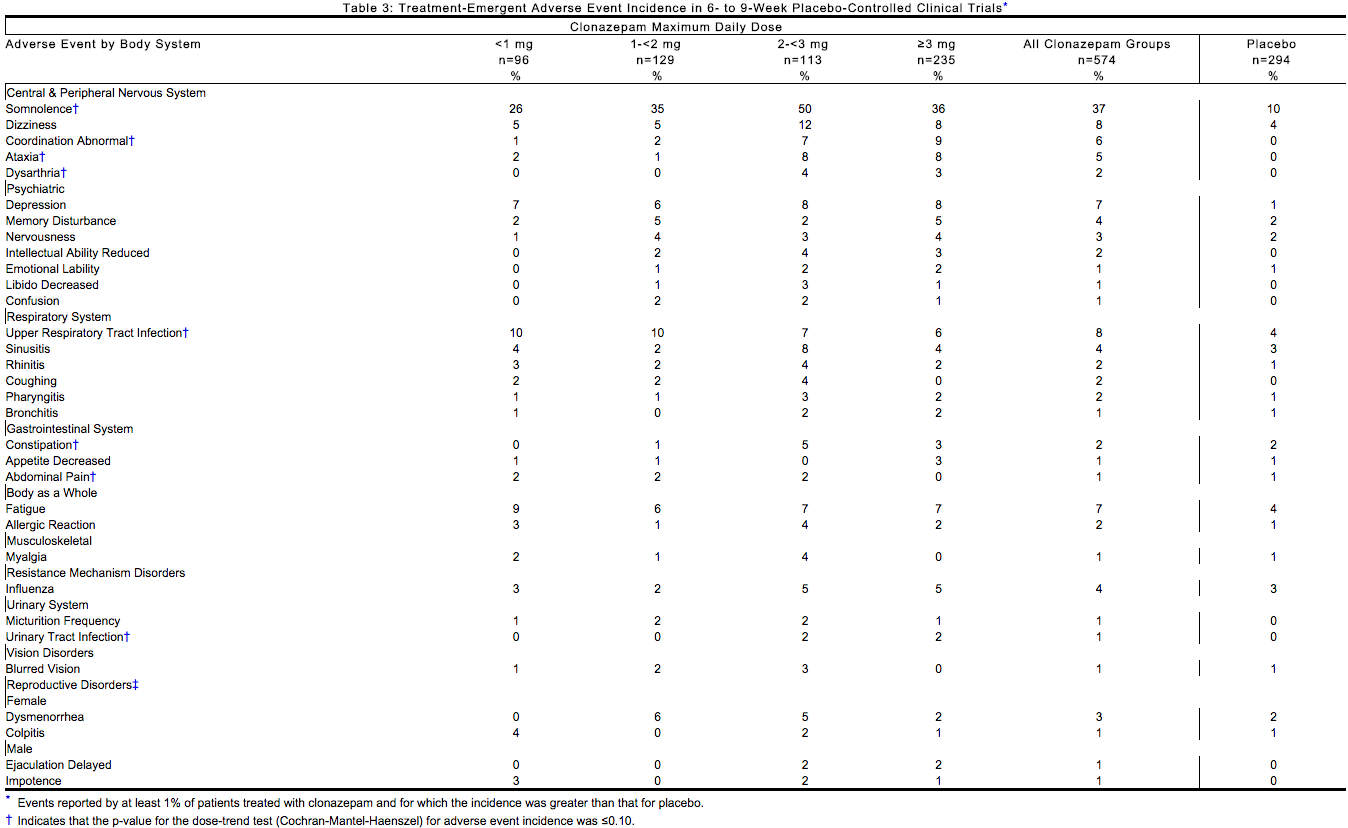
Treatment-Emergent Depressive Symptoms
In the pool of two short-term placebo-controlled trials, adverse events classified under the preferred term “depression” were reported in 7% of clonazepam-treated patients compared to 1% of placebo-treated patients, without any clear pattern of dose relatedness. In these same trials, adverse events classified under the preferred term “depression” were reported as leading to discontinuation in 4% of clonazepam-treated patients compared to 1% of placebo-treated patients. While these findings are noteworthy, Hamilton Depression Rating Scale (HAM-D) data collected in these trials revealed a larger decline in HAM-D scores in the clonazepam group than the placebo group suggesting that clonazepam-treated patients were not experiencing a worsening or emergence of clinical depression. Other Adverse Events Observed During the Pre marketing Evaluation of Clonazepam in panic disorder Following is a list of modified CIGY terms that reflect treatment-emergent adverse events reported by patients treated with clonazepam at multiple doses during clinical trials. All reported events are included except those already listed in Table 3 or elsewhere in labeling, those events for which a drug cause was remote, those event terms which were so general as to be uninformative, and events reported only once and which did not have a substantial probability of being acutely life-threatening. It is important to emphasize that, although the events occurred during treatment with clonazepam, they were not necessarily caused by it. Events are further categorized by body system and listed in order of decreasing frequency. These adverse events were reported infrequently, which is defined as occurring in 1/100 to 1/1,000 patients.
Body as a Whole: weight increase, accident, weight decrease, wound, edema, fever, shivering, abrasions, ankle edema, edema foot, edema periorbital, injury, malaise, pain, cellulitis, inflammation localized
Cardiovascular Disorders: chest pain, hypotension postural
Central and Peripheral Nervous System Disorders: migraine, paresthesia, drunkenness, feeling of enuresis, paresis, tremor, burning skin, falling, head fullness, hoarseness, hyperactivity, hypoesthesia, tongue thick, twitching
Gastrointestinal System Disorders: abdominal discomfort, gastrointestinal inflammation, stomach upset, toothache, flatulence, pyrosis, saliva increased, tooth disorder, bowel movements frequent, pain pelvic, dyspepsia, hemorrhoids
Hearing and Vestibular Disorders: vertigo, otitis, earache, motion sickness
Heart Rate and Rhythm Disorders: palpitation
Metabolic and Nutritional Disorders: thirst, gout
Musculoskeletal System Disorders: back pain, fracture traumatic, sprains and strains, pain leg, pain nape, cramps muscle, cramps leg, pain ankle, pain shoulder, tendinitis, arthralgia, hypertonia, lumbago, pain feet, pain jaw, pain knee, swelling knee
Platelet, Bleeding and Clotting Disorders: bleeding dermal
Psychiatric Disorders: insomnia, organic disinhibition, anxiety, depersonalization, dreaming excessive, libido loss, appetite increased, libido increased, reactions decreased, aggressive reaction, apathy, attention lack, excitement, feeling mad, hunger abnormal, illusion, nightmares, sleep disorders, suicide ideation, yawning
Reproductive Disorders, Female: breast pain, menstrual irregularity
Reproductive Disorders, Male: ejaculation decreased
Resistance Mechanism Disorders: infection mycotic, infection viral, infection streptococcal, herpes simplex infection, infectious mononucleosis, moniliasis
Respiratory System Disorders: sneezing excessive, asthmatic attack, dyspnea, nosebleed, pneumonia, pleurisy
Skin and Appendages Disorders: acne flare, alopecia, xeroderma, dermatitis contact, flushing, pruritus, pustular reaction, skin burns, skin disorder
Special Senses Other, Disorders: taste loss
Urinary System Disorders: dysuria, cystitis, polyuria, urinary incontinence, bladder dysfunction, urinary retention, urinary tract bleeding, urine discoloration
Vascular (Extracardiac) Disorders: thrombophlebitis leg
Vision Disorders: eye irritation, visual disturbance, diplopia, eye twitching, styes, visual field defect, xerophthalmia
Postmarketing Experience
FDA package insert for clonazepam contains no information regarding post marketing experience.
Drug Interactions
There is limited information regarding Clonazepam Drug Interactions in the drug label.
Use in Specific Populations
Pregnancy
Pregnancy Category (FDA): D
To provide information regarding the effects of in utero exposure to clonazepam, physicians are advised to recommend that pregnant patients taking clonazepam enroll in the NAAED Pregnancy Registry. This can be done by calling the toll free number 1-888-233-2334, and must be done by patients themselves. Information on this registry can also be found at the website http://www.aedpregnancyregistry.org/.
Pregnancy Category (AUS):
There is no Australian Drug Evaluation Committee (ADEC) guidance on usage of Clonazepam in women who are pregnant.
Labor and Delivery
The effect of clonazepam on labor and delivery in humans has not been specifically studied; however, perinatal complications have been reported in children born to mothers who have been receiving benzodiazepines late in pregnancy, including findings suggestive of either excess benzodiazepine exposure or of withdrawal phenomena.
Nursing Mothers
Mothers receiving clonazepam should not breastfeed their infants.
Pediatric Use
Because of the possibility that adverse effects on physical or mental development could become apparent only after many years, a benefit-risk consideration of the long-term use of clonazepam is important in pediatric patients being treated for seizure disorder . Safety and effectiveness in pediatric patients with panic disorder below the age of 18 have not been established.
Geriatic Use
Clinical studies of clonazepam did not include sufficient numbers of subjects aged 65 and over to determine whether they respond differently from younger subjects. Other reported clinical experience has not identified differences in responses between the elderly and younger patients. In general, dose selection for an elderly patient should be cautious, usually starting at the low end of the dosing range, reflecting the greater frequency of decreased hepatic, renal, or cardiac function, and of concomitant disease or other drug therapy. Because clonazepam undergoes hepatic metabolism, it is possible that liver disease will impair clonazepam elimination. Metabolites of clonazepam are excreted by the kidneys; to avoid their excess accumulation, caution should be exercised in the administration of the drug to patients with impaired renal function. Because elderly patients are more likely to have decreased hepatic and/or renal function, care should be taken in dose selection, and it may be useful to assess hepatic and/or renal function at the time of dose selection. Sedating drugs may cause confusion and over-sedation in the elderly; elderly patients generally should be started on low doses of clonazepam and observed closely.
Gender
There is no FDA guidance on the use of Clonazepam with respect to specific gender populations.
Race
There is no FDA guidance on the use of Clonazepam with respect to specific racial populations.
Renal Impairment
There is no FDA guidance on the use of Clonazepam in patients with renal impairment.
Hepatic Impairment
There is no FDA guidance on the use of Clonazepam in patients with hepatic impairment.
Females of Reproductive Potential and Males
There is no FDA guidance on the use of Clonazepam in women of reproductive potentials and males.
Immunocompromised Patients
There is no FDA guidance one the use of Clonazepam in patients who are immunocompromised.
Administration and Monitoring
Administration
Oral
Monitoring
FDA package insert for clonazepam contains no information regarding drug monitoring.
IV Compatibility
There is limited information about the IV compatibility.
Overdosage
FDA package insert for clonazepam contains no information regarding Overdose.
Pharmacology
| |
| |
Clonazepam
| |
| Systematic (IUPAC) name | |
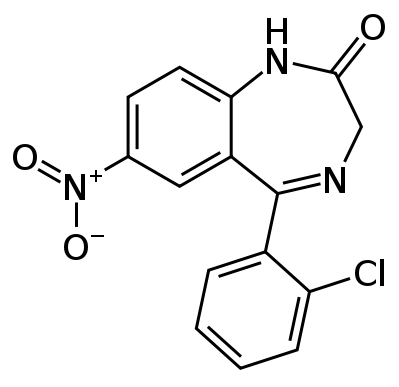
| 5-(2-chlorophenyl)-7-nitro-2,3-dihydro-1,4-benzodiazepin-2-one | |
| Identifiers | |
| CAS number | |
| ATC code | N03 |
| PubChem | |
| DrugBank | |
| Chemical data | |
| Formula | Template:OrganicBox atomTemplate:OrganicBox atomTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBox atomTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBox atomTemplate:OrganicBoxTemplate:OrganicBox atomTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBox |
| Mol. mass | 315.715 |
| SMILES | & |
| Pharmacokinetic data | |
| Bioavailability | 90% |
| Protein binding | ~85% |
| Metabolism | Hepatic CYP3A4 |
| Half life | 18–50 hours |
| Excretion | Renal |
| Therapeutic considerations | |
| Licence data |
|
| Pregnancy cat. | |
| Legal status |
Prescription Only (S4)(AU) Schedule IV(CA) ?(UK) Schedule IV(US) |
| Dependence Liability | Moderate[4] |
| Routes | Oral, I.M., I.V, sublingual |
Mechanism of Action
The precise mechanism by which clonazepam exerts its antiseizure and antipanic effects is unknown, although it is believed to be related to its ability to enhance the activity of gamma aminobutyric acid (GABA), the major inhibitory neurotransmitter in the central nervous system.
Structure
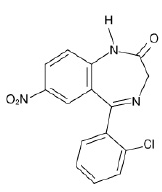
Clonazepam tablets USP, for oral administration, contain 0.5 mg, 1 mg or 2 mg clonazepam. In addition, each tablet also contains the following inactive ingredients: corn starch, lactose anhydrous, magnesium stearate and microcrystalline cellulose with the following colorants: 0.5 mg - D&C yellow No. 10 aluminum lake; 1 mg - FD&C blue No. 1 aluminum lake. Chemically, clonazepam is 5-(2-chlorophenyl)-1,3-dihydro-7-nitro-2H-1,4-benzodiazepin-2-one. It is a light yellow crystalline powder. It has a molecular weight of 315.72 and the following structural formula:
Pharmacodynamics
The precise mechanism by which clonazepam exerts its antiseizure and antipanic effects is unknown, although it is believed to be related to its ability to enhance the activity of gamma aminobutyric acid (GABA), the major inhibitory neurotransmitter in the central nervous system. Convulsions produced in rodents by pentylenetetrazol or, to a lesser extent, electrical stimulation are antagonized, as are convulsions produced by photic stimulation in susceptible baboons. A taming effect in aggressive primates, muscle weakness and hypnosis are also produced. In humans, clonazepam is capable of suppressing the spike and wave discharge in absence seizures (petit mal) and decreasing the frequency, amplitude, duration and spread of discharge in minor motor seizures.
Pharmacokinetics
Clonazepam is rapidly and completely absorbed after oral administration. The absolute bioavailability of clonazepam is about 90%. Maximum plasma concentrations of clonazepam are reached within 1 to 4 hours after oral administration. Clonazepam is approximately 85% bound to plasma proteins. Clonazepam is highly metabolized, with less than 2% unchanged clonazepam being excreted in the urine. Biotransformation occurs mainly by reduction of the 7-nitro group to the 4-amino derivative. This derivative can be acetylated, hydroxylated and glucuronidated. Cytochrome P-450, including CYP3A, may play an important role in clonazepam reduction and oxidation. The elimination half-life of clonazepam is typically 30 to 40 hours. Clonazepam pharmacokinetics are dose-independent throughout the dosing range. There is no evidence that clonazepam induces its own metabolism or that of other drugs in humans. Pharmacokinetics in Demographic Subpopulations and in Disease States
Controlled studies examining the influence of gender and age on clonazepam pharmacokinetics have not been conducted, nor have the effects of renal or liver disease on clonazepam pharmacokinetics been studied. Because clonazepam undergoes hepatic metabolism, it is possible that liver disease will impair clonazepam elimination. Thus, caution should be exercised when administering clonazepam to these patients.
Nonclinical Toxicology
Carcinogenesis, Mutagenesis, Impairment of Fertility
Carcinogenicity studies have not been conducted with clonazepam. The data currently available are not sufficient to determine the genotoxic potential of clonazepam. In a two-generation fertility study in which clonazepam was given orally to rats at 10 mg/kg/day and 100 mg/kg/day (low dose approximately 5 times and 24 times the maximum recommended human dose of 20 mg/day for seizure disorder and 4 mg/day for panic disorder, respectively, on a mg/m2 basis), there was a decrease in the number of pregnancies and in the number of offspring surviving until weaning.
Clinical Studies
FDA package insert for clonazepam contains no information regarding Clinical studies.
How Supplied
Clonazepam Tablets USP for oral administration are available as: 0.5 mg: Round, light yellow, biconvex tablet, debossed “E” over “63” on one side and bisected on the other side and supplied as: NDC 0185-0063-01 bottles of 100 NDC 0185-0063-05 bottles of 500 NDC 0185-0063-10 bottles of 1000 1 mg: Round, light blue, biconvex tablet, debossed “E” over “64” on one side and bisected on the other side and supplied as: NDC 0185-0064-01 bottles of 100 NDC 0185-0064-05 bottles of 500 NDC 0185-0064-10 bottles of 1000 2 mg: Round, white, biconvex tablet, debossed “E” over “65” on one side and bisected on the other side and supplied as: NDC 0185-0065-01 bottles of 100 NDC 0185-0065-05 bottles of 500 NDC 0185-0065-10 bottles of 1000
Storage
Store at 20° to 25°C (68° to 77°F) [see USP Controlled Room Temperature]. Dispense in a tight, light-resistant container as defined in the USP, with a child-resistant closure, as required.
Images
Drug Images
{{#ask: Page Name::Clonazepam |?Pill Name |?Drug Name |?Pill Ingred |?Pill Imprint |?Pill Dosage |?Pill Color |?Pill Shape |?Pill Size (mm) |?Pill Scoring |?NDC |?Drug Author |format=template |template=DrugPageImages |mainlabel=- |sort=Pill Name }}
Package and Label Display Panel
{{#ask: Label Page::Clonazepam |?Label Name |format=template |template=DrugLabelImages |mainlabel=- |sort=Label Page }}
Patient Counseling Information
A clonazepam medication guide must be given to the patient each time clonazepam is dispensed, as required by law. Patients should be instructed to take clonazepam only as prescribed. Physicians are advised to discuss the following issues with patients for whom they prescribe clonazepam.
Precautions with Alcohol
Patients should be advised to avoid alcohol while taking clonazepam.
Brand Names
- Klonopin
- Klonopin Wafers
Look-Alike Drug Names
clonazepam - cloBAZam clonazepam - cloNIDine clonazepam - cloNIDine hydrochloride clonazepam - cloZApine clonazepam - LORazepam Klonopin - cloNIDine hydrochloride Klonopin - cloNIDine[5]
Price
References
The contents of this FDA label are provided by the National Library of Medicine.
- ↑ Peled R, Lavie P (1987). "Double-blind evaluation of clonazepam on periodic leg movements in sleep". J Neurol Neurosurg Psychiatry. 50 (12): 1679–81. PMC 1032613. PMID 3437302.
- ↑ Schenck CH, Milner DM, Hurwitz TD, Bundlie SR, Mahowald MW (1989). "A polysomnographic and clinical report on sleep-related injury in 100 adult patients". Am J Psychiatry. 146 (9): 1166–73. PMID 2764174.
- ↑ Connor KM, Davidson JR, Potts NL, Tupler LA, Miner CM, Malik ML; et al. (1998). "Discontinuation of clonazepam in the treatment of social phobia". J Clin Psychopharmacol. 18 (5): 373–8. PMID 9790154.
- ↑ Saunders Nursing Drug Handbook 2014
- ↑ "https://www.ismp.org". External link in
|title=(help)
{{#subobject:
|Page Name=Clonazepam |Pill Name=No_image.jpg |Drug Name=Clonazepam 0.5 MG Oral Tablet |Pill Ingred=starch, corn, d&c yellow no. 10, anhydrous lactose, magnesium stearate, cellulose, microcrystalline|+sep=; |Pill Imprint=E;63 |Pill Dosage=0.5 mg |Pill Color=Yellow|+sep=; |Pill Shape=Round |Pill Size (mm)=7.00 |Pill Scoring=2 |Pill Image= |Drug Author=Eon Labs, Inc. |NDC=0185-0063
}}
{{#subobject:
|Page Name=Clonazepam |Pill Name=No_image.jpg |Drug Name=Clonazepam 1 MG Oral Tablet |Pill Ingred=starch, corn, d&c yellow no. 10, anhydrous lactose, magnesium stearate, cellulose, microcrystalline|+sep=; |Pill Imprint=E;64 |Pill Dosage=1 mg |Pill Color=Blue|+sep=; |Pill Shape=Round |Pill Size (mm)=7.00 |Pill Scoring=2 |Pill Image= |Drug Author=Eon Labs, Inc. |NDC=0185-0063
}}
{{#subobject:
|Page Name=Clonazepam |Pill Name=No_image.jpg |Drug Name=Clonazepam 2 MG Oral Tablet |Pill Ingred=starch, corn, d&c yellow no. 10, anhydrous lactose, magnesium stearate, cellulose, microcrystalline|+sep=; |Pill Imprint=E;65 |Pill Dosage=1 mg |Pill Color=White|+sep=; |Pill Shape=Round |Pill Size (mm)=7.00 |Pill Scoring=2 |Pill Image= |Drug Author=Eon Labs, Inc. |NDC=0185-0063
}}
{{#subobject:
|Label Page=Clonazepam |Label Name=Clonazepam_label_01.jpg
}}
{{#subobject:
|Label Page=Clonazepam |Label Name=Clonazepam_label_02.jpg
}}
{{#subobject:
|Label Page=Clonazepam |Label Name=Clonazepam_label_03.jpg
}}
{{#subobject:
|Label Page=Clonazepam |Label Name=Clonazepam_panel_01.png
}}
{{#subobject:
|Label Page=Clonazepam |Label Name=Clonazepam_panel_02.png
}}
{{#subobject:
|Label Page=Clonazepam |Label Name=Clonazepam_panel_03.png
}}