Lown-Ganong-Levine syndrome
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [2] Associate Editor(s)-in-Chief: Usman Ali Akbar, M.B.B.S.[3]
Synonyms and keywords: Lown-Ganong-Levine Syndrome, LGL syndrome, Pre-excitation syndromes, Short PR Normal QRS Complex Syndrome, Clerc-Lévy-Cristesco syndrome, Coronary nodal rhythm syndrome, Short PQ interval syndrome, Short P-R syndrome.
Overview
Lown-Ganong-Levine syndrome (LGL) is one of the pre-excitation syndromes that present with EKG findings of the short PR interval, narrow/normal QRS complex, and normal P wave. The presence of accessory bundles fibers such as James fiber leads to the development of abnormal conduction pathways. The LGL pattern was described in 1952 by Bernard Lown, William Francis Ganong, and Samual Levine. Patients present with a history of palpitations, lightheadedness, shortness of breath, and sometimes chest pain. There is an increased risk of tachyarrhythmias and syncope. EKG is the principal modality of investigation for establishing a diagnosis. Usually, antiarrhythmics are given to prevent the development of tachyarrhythmias but recently radiofrequency ablation of the accessory pathway has been the main stray of treatment with a good prognosis.
Historical Perspective
Following is timeline of of LGL syndrome with its discovery and developments of its bypass tracts.[1][2][3]
| Year | Description |
|---|---|
| 1938 | Clerc, Levy and Critesco in 1938 first reported cases in which there was occurence of frequent paroxysms of tachycardia. The EKG of such patients consist of a short PR interval and normal QRS interval |
| 1946 | Burch and Kimball hinted on existence of the atrio-Hisian pathway |
| 1952 | The Lown-Ganong-Levine (LGL) pattern was described in 1952 by Bernard Lown, William Francis Ganong, and Samual Levine. |
| 1961,1974 | In 1961 and subsequently in 1974 anatomic pathway was identified and reported by James and Brechemacher respectively. |

Classification
| Accessory Pathway | Description |
|---|---|
| James Fibers | They can be present as a normal part of AV node but these fibers have been established as an anatomic reason for LGL syndrome |
| Brechmacher fibers | These atrio-Hisian tracts are reported to have a frequency of 0.03 % and can be theoratically a cause of LGL syndrome |
| Intra-nodal bypass tracts | Intra-nodal bypass tracts would allow the conduction of rapid action potential through AV node bypassing the other slow pathways. |
Pathophysiology
- The pathophysiology of LGL syndrome has not yet been completely understood.
- Multiple theories have been proposed to suggest the mechanism of LGL. [1]
- The current theory supporting the mechanism of LGL is that it may result from numerous underlying causes that involve junctional pathways that partially or wholly bypass the AV node with subsequent normal conduction down the bundle of His.
- The three accessory pathways as discussed in classification has been proposed to be the main triggering factors for the development of LGL.
- Lown-Ganong-Levine pattern may occur include Brechenmacher fibers or intranodal bypass tracts and James Fibers. Brenchmacher fibers account for 0.03% of the patients presenting with LGL.
- The intra-nodal bypass tracts allow the conduction of rapid action potential through AV-node bypassing the other slow pathways.
Causes
Differentiating Lown-Ganong-Levine Syndrome from other Diseases
The differential diagnosis for Lown-Ganong-Levine includes
- Supraventricular tachycardia
- Atrial fibrillation or flutter with a rapid ventricular response
- AV nodal reentry tachycardia
- Wolf-Parkinson-White Syndrome
Epidemiology and Demographics
- The Lown-Ganong-Levine pattern does not show an increased incidence in one particular sex or ethnic background.
- In a retrospective study conducted by Bernard Lown, William Francis Ganong, and Samual Levine 200 electrocardiograms (EKG) of 13500 patients showed EKG findings with the prevalence of just over 1%. [1]
Age
- There is currently insufficient data regarding age predilection of LGL syndrome.
Gender
- There is currently insufficient data regarding gender predilection of LGL syndrome. However, Lown in 1952 reported 70.9% of the 34 cases in women.[1]
Race
- There is currently insufficient data regarding race predilection of LGL syndrome.
Risk Factors
- The data regarding the risk factors predisposing to LGL syndrome is insufficient. However, the following conditions or factors may lead to various pre-excitation syndromes.
- Presence of accessory bypass tracts
- High risk population for sudden cardiac death in Pre-excitation syndromes include
- Policemen
- Athletes
- Firemen
- Pilots
- Steelworkers
Natural History, Complications and Prognosis
Natural History
- LGL syndrome can be asymptomatic or can present with palpitations, lightheadedness, shortness of breath, and syncope. In the case of congenital heart disease or genetic anomaly, it can also present as paroxysms of tachycardia or chest pain.[1]
Complications
- There is an increased risk of developing tachyarrhythmias.
- Certain medications such as sympathomimetics should be used with caution in the patients of LGL syndrome. Digitalis does not have any effect in LGL syndrome but it can slow conduction via the AV-node. This can prevent AVRT in these patients.
- Beta-blockers do not affect the accessory pathway directly but can slow conduction through the AV node similar to digitalis.
Prognosis
There is an overall good prognosis in patients with LGL syndrome. Patients are usually asymptomatic but some can develop certain clinical features such as palpitations, shortness of breath, and occasional episodes of atrial fibrillation, atrial flutter, AVRT, and other tachyarrhythmias. They can also lead to the development of ventricular arrhythmias in rare cases.[1][4]
Diagnosis
Diagnostic Criteria
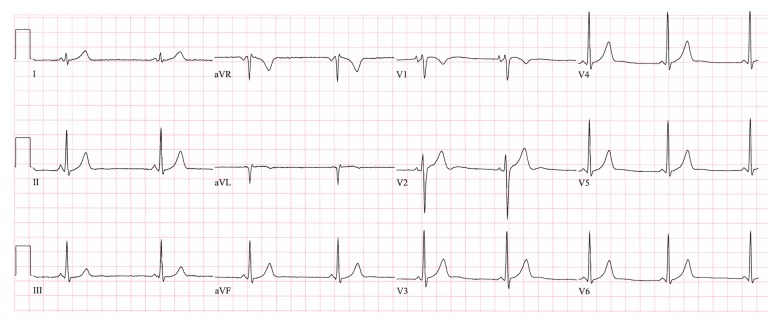
- Characteristic ECG findings of LGL syndrome are [1]
- Short PR interval (<120ms)
- Normal P wave axis
- Normal/narrow QRS morphology in the presence of paroxysmal tachyarrhythmia.
History and Symptoms
- LGL syndrome is usually asymptomatic.
- Symptoms of LGL syndrome overlap with the pre-excitation syndrome and may include the following:[1]
- Palpitations
- Dizziness
- Lightheadedness
- Shortness of breath
- Racing heart
- Syncope
- Chest pain or tachycardia {in case of an underlying cardiac structural defect)
Physical Examination
- Patients with LGL syndrome usually appear normal.
- Physical examination findings are limited in LGL syndrome.
- During cardiac auscultation or palpation of peripheral pulses, there can be irregular rhythm.
Laboratory Findings
- There are no specific laboratory findings associated with LGL syndrome.
Imaging Findings
ECG
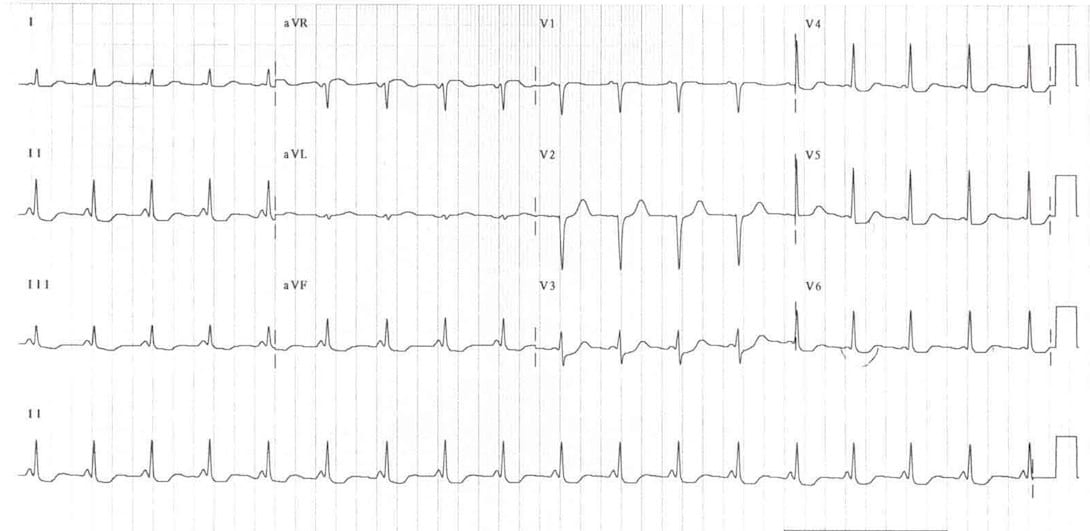
The diagnosis of LGL syndrome can be made by the use of resting EKG. EKG finding usually shows
- Short PR interval (<120ms)
- Normal P wave axis
- Normal/narrow QRS morphology in the presence of paroxysmal tachyarrhythmia.
Other Diagnostic Studies
- Holter monitors or implantable loop recorders may provide insight to the underlying conductions abnormalities.
Treatment
Medical Therapy
- The mainstay of therapy for LGL syndrome is the use of antiarrhythmic medications to prevent tachyarrhythmias.
- Medications such as digitalis, beta-blockers, calcium channel blockers and Class I and III antiarrhythmic drugs have been used to slow down AV conduction and prevent AVRT and other arrhythmias.[5] [6]
- Drugs like sotalol and amiodarone are under investigations and have promising effect in LGL syndrome but needs further studies.
Surgery
Patients refractory to medical management can be managed by the use of radiofrequency catheter ablation as it has become primary treatment in various pre-excitation syndromes. This can be further implicated by the implantation of a permanent pacemaker.
Prevention
- There are no primary preventive measures available for LGL syndrome.
References
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 1.7 1.8 LOWN, BERNARD; GANONG, WILLIAM F.; LEVINE, SAMUEL A. (1952). "The Syndrome of Short P-R Interval Normal QRS Complex and Paroxysmal Rapid Heart Action". Circulation. Ovid Technologies (Wolters Kluwer Health). 5 (5): 693–706. doi:10.1161/01.cir.5.5.693. ISSN 0009-7322. PMID 14926053.
- ↑ 2.0 2.1 Manning, G W (1978). "Lown-Ganong-Levine syndrome". Circulation. Ovid Technologies (Wolters Kluwer Health). 58 (3): 576–577. doi:10.1161/01.cir.58.3.576. ISSN 0009-7322. PMID 679452.
- ↑ DOUGLAS, JOHN E. (1972). "Lown-Ganong-Levine Syndrome". Circulation. Ovid Technologies (Wolters Kluwer Health). 45 (5): 1143–1144. doi:10.1161/01.cir.45.5.1143. ISSN 0009-7322. PMID 5020803.
- ↑ Benditt, D G; Pritchett, L C; Smith, W M; Wallace, A G; Gallagher, J J (1978). "Characteristics of atrioventricular conduction and the spectrum of arrhythmias in lown-ganong-levine syndrome". Circulation. Ovid Technologies (Wolters Kluwer Health). 57 (3): 454–465. doi:10.1161/01.cir.57.3.454. ISSN 0009-7322. PMID 624155.
- ↑ Benditt, D G; Klein, G J; Kriett, J M; Dunnigan, A; Benson, D W (1984). "Enhanced atrioventricular nodal conduction in man: electrophysiologic effects of pharmacologic autonomic blockade". Circulation. Ovid Technologies (Wolters Kluwer Health). 69 (6): 1088–1095. doi:10.1161/01.cir.69.6.1088. ISSN 0009-7322. PMID 6713613.
- ↑ Caracta, Anthony R.; Damato, Anthony N.; Gallagher, John J.; Josephson, Mark E.; Varghese, P.Jacob; Lau, Sun H.; Westura, Edwin E. (1973). "Electrophysiologic studies in the syndrome of short P-R interval, normal QRS complex". The American Journal of Cardiology. Elsevier BV. 31 (2): 245–253. doi:10.1016/0002-9149(73)91037-0. ISSN 0002-9149.