Vesicoureteral reflux
| https://https://www.youtube.com/watch?v=7OqqtSlW9sA&t=75s |350}} |
Template:DiseaseDisorder infobox Template:Search infobox Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1], Steven C. Campbell, M.D., Ph.D.
Overview
Vesicoureteral reflux (VUR) is an abnormal movement of urine from the bladder into ureters or kidneys. Urine normally travels from the kidneys via the ureters to the bladder. In vesicoureteral reflux the direction of urine flow is reversed (retrograde). In the majority of cases, it occurs as a result of a primary maturation abnormality of the vesicoureteral junction or a short distal ureteric submucosal tunnel in the bladder that alters the function of the valve mechanism. VUR may be an isolated anomaly or associated with other congenital anomalies such as posterior urethral valves or complete duplication of the urinary tract.
Symptoms
- Prenatal hydronephrosis.[1]
- Abnormal widening of the ureter .
- Urinary tract infection.
- Acute pyelonephritis .
- Symptoms such as painful urination or renal colic / flank pain are not symptoms associated with vesicoureteral reflux.
- Newborns may be lethargic with failure to thrive, while infants and young children typically present with pyrexia, dysuria, frequent urination, malodorous urine and GIT symptoms, but only when urinary tract infection is present as the initial presentation of VUR.
Causes
Vesicoureteral reflux has two type ; primary and secondary
Primary VUR
- Is due to incompetent or inadequate closure of the ureterovesical junction (UVJ).
- Usually reflux is prevented during bladder contraction by completely compressing the intravesical ureter and sealing it with surrounding bladder muscle.
- Failure of anti-reflux mechanism is due to shortening of the intravesical ureter.
Secondary VUR
- Is due to abnormally high pressure in the bladder which cause failure of the closure of the ureterovesical junction during bladder contraction.
- Secondary VUR is related with anatomic ( eg , posterior urethral valves) or
- Functional bladder obstruction (eg , dysfunctional voiding and neurogenic bladder)
Prevalence
VUR is present in more than 10% of the population. In children without urinary tract infections 17.2-18.5% have VUR, whereas in those with urinary tract infections the incidence may be as high as 70%.
Age
Younger children are more prone to VUR because of the relative shortness of the submucosal ureters. This susceptibility decreases with age as the length of the ureters increases as the children grow. In children under the age of 1 year with a urinary tract infection, 70% will have VUR. This number decreases to 15% by the age of 12.
Sex
Although VUR is more common in males antenatally, in later life there is a definite female preponderance with 85% of cases being female.
International Classification of Vesicoureteral Reflux
- Grade I – Reflux only fills the ureter without dilation.
- Grade II – Reflux into the renal pelvis and calyces without dilatation
- Grade III – Reflux fills and mildly dilates the ureter and the collecting system with mild blunting of the calyces.
- Grade IV – Dilation of the renal pelvis and calyces with moderate ureteral tortuosity
- Grade V – Gross dilatation of the ureter, pelvis and calyces; ureteral tortuosity; papillary impressions
Almost 85% of grade I & II cases of VUR will resolve spontaneously. Approximately 50% of grade III cases and a lower percentage of higher grades will also resolve spontaneously.[2]
Diagnosis
The following procedures may be used to diagnose VUR:
- Nuclear cystogram (RNC)
- Fluoroscopic voiding cystourethrogram (VCUG)
- Ultrasonic cystography
- Abdominal ultrasound
- if ureteral dilation is seen during abdominal ultrasound it suggest VUR
- In children suspected of having VUR presenting with prenatal hydronephrosis or UTI
-
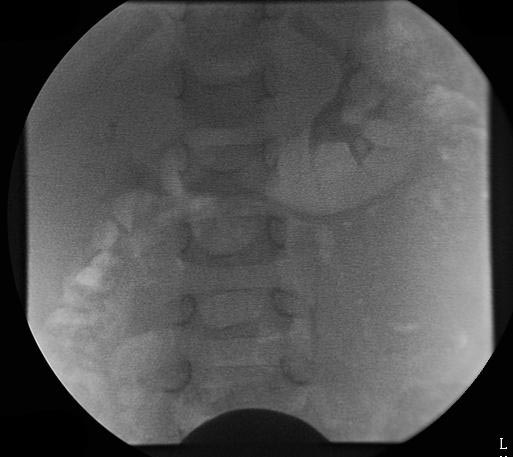
VCUG demonstrating bilateral Grade III vesicoureteral reflux
-
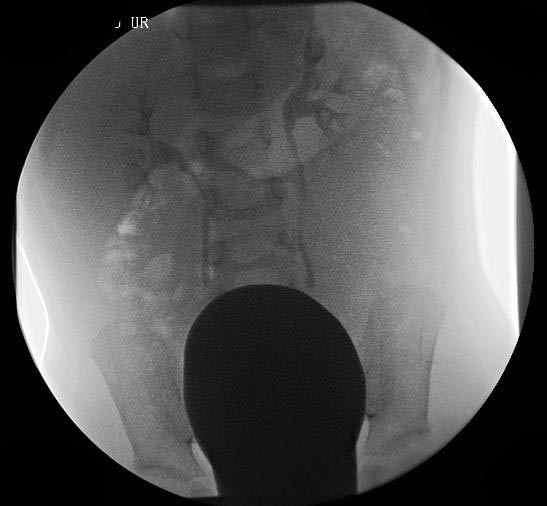
VCUG demonstrating bilateral Grade III vesicoureteral reflux
-
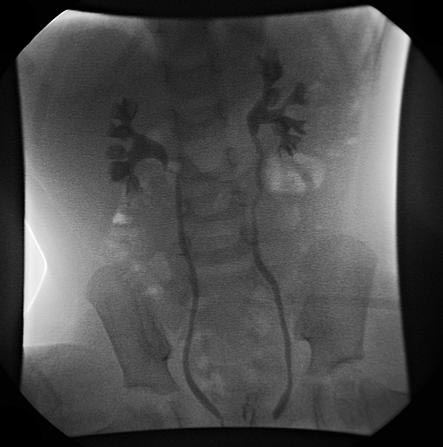
VCUG demonstrating bilateral Grade III vesicoureteral reflux
Treatment
Medical treatment is the preferred mode of management but surgical interventions may be necessary. Medical management is recommended in children with Grade I-III VUR as most cases will resolve spontaneously. A trial of medical treatment is indicated in patients with Grade IV VUR especially in younger patients or those with unilateral disease. Of the patients with Grade V VUR only infants are trialed on a medical approach before surgery is indicated, in older patients surgery is the only option.
Medical Treatment
start with low dose antibiotic prophylaxis until resolution of VUR occurs. Antibiotics are give nightly at half the normal dose.
- Amoxicillin or ampicillin infants younger than 6 weeks. [3]
- Trimethoprim - Sulfamethoxazole (co-trimoxazole) - 6 weeks to 2 months
After 2 months the following antibiotics are suitable:
- Nitrofurantoin (5-7mg/kg/24hrs )
- Nalidixic acid
- Bactrim
- Trimethoprim
- Cephalosporins
Surgical Management
surgical treatment is needed in case of
- Antibiotic treatment is not effective.
- if VUR is severe ( Grade IV and V ).
- In case of pyelonephritic changes and congenital abnormalities
- Failure of renal growth or formation of new renal scars.[4]
open surgical reimplantation
Is surgical correction and highly successful procedure with correction rate of 95 to 99 %.
In this procedure bladder is opened ( intravesical approach ) and the ureters are reimplanted by tunneling a ureteral segment through the detrusor muscle which is creating submucosal tunnel.
Endoscopic correction
Also called STING procedure is surgical correction.
In procedure injecting a copolymer ( dextranomer / hyaluronic acid ) under the mucosa of the UVJ through a cystoscope as result of this injection change the angle and fixation of the intravesical ureter.
References
- Atala. A, Keating. M, in Campbells Urology 8th ed. Pgs 2053-2094
- Bailey RR: The relationship of VUR to UTI and chronic pyelonephritis-reflux nephropathy. Clin Nephrol 1973;1:132
- Baker et al, Relation of age, sex and infection to reflux: Data indicating high spontaneous cure rate in paediatric patients. J Urol 1966;95:27
- Duckett JW: VUR a "conservative analysis." Am J Kidney Dis 1983;3:139
- Hodson CJ, Edwards D: Chronic Pyelonephritis and VUR. Clin Radiol 1960;11:219
- King et al: Natural history of VUR: Outcome of a trial of non-operative therapy. Urol Clin North Am 1974;1:144
- Ring E et al: Primary VUR in infants with a dilated fetal urinary tract. Eur J Pediatr 1993;152:523
- Sargent MA: what is the normal prevalence of VUR? Pediatr Radiol 2000;9;587
- Smellie JM, Normand ICS: The clinical features and significance of UTIs in children. Proc R Soc London 1966;59:415
- Walker et al: Screening schoolchildren for urologic disease. Pediatrics 1977;60:239
- ↑ Yeung CK, Godley ML, Dhillon HK, Gordon I, Duffy PG, Ransley PG (August 1997). "The characteristics of primary vesico-ureteric reflux in male and female infants with pre-natal hydronephrosis". Br J Urol. 80 (2): 319–27. PMID 9284209.
- ↑ Mattoo TK (September 2011). "Vesicoureteral reflux and reflux nephropathy". Adv Chronic Kidney Dis. 18 (5): 348–54. doi:10.1053/j.ackd.2011.07.006. PMC 3169795. PMID 21896376.
- ↑ Doganis D, Siafas K, Mavrikou M, Issaris G, Martirosova A, Perperidis G, Konstantopoulos A, Sinaniotis K (October 2007). "Does early treatment of urinary tract infection prevent renal damage?". Pediatrics. 120 (4): e922–8. doi:10.1542/peds.2006-2417. PMID 17875650.
- ↑ Shaikh N, Ewing AL, Bhatnagar S, Hoberman A (December 2010). "Risk of renal scarring in children with a first urinary tract infection: a systematic review". Pediatrics. 126 (6): 1084–91. doi:10.1542/peds.2010-0685. PMID 21059720.