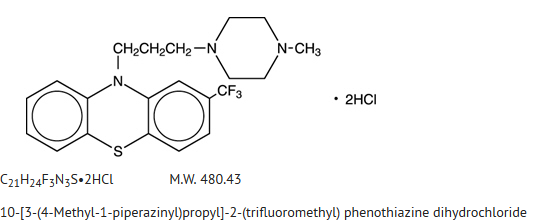
Trifluoperazine
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Vignesh Ponnusamy, M.B.B.S. [2]
WikiDoc MAKES NO GUARANTEE OF VALIDITY. WikiDoc is not a professional health care provider, nor is it a suitable replacement for a licensed healthcare provider. WikiDoc is intended to be an educational tool, not a tool for any form of healthcare delivery. The educational content on WikiDoc drug pages is based upon the FDA package insert, National Library of Medicine content and practice guidelines / consensus statements. WikiDoc does not promote the administration of any medication or device that is not consistent with its labeling. Please read our full disclaimer here.
Black Box Warning
|
WARNING
See full prescribing information for complete Boxed Warning.
|
Overview
Trifluoperazine is an antipsychotic that is FDA approved for the {{{indicationType}}} of schizophrenia and non-psychotic anxiety. There is a Black Box Warning for this drug as shown here. Common adverse reactions include hypotension, orthostatic hypotension, constipation, xerostomia, akathisia, dizziness, dystonia, extrapyramidal disease, parkinsonian, somnolence, and tardive dyskinesia.
Adult Indications and Dosage
FDA-Labeled Indications and Dosage (Adult)
Schizophrenia
- Usual starting dosage is 2 mg to 5 mg b.i.d. (Small or emaciated patients should always be started on the lower dosage.)
- Most patients will show optimum response on 15 mg or 20 mg daily, although a few may require 40 mg a day or more. Optimum therapeutic dosage levels should be reached within 2 or 3 weeks.
Non-Psychotic Anxiety
- Usual dosage is 1 mg or 2 mg twice daily. Do not administer at doses of more than 6 mg per day or for longer than 12 weeks.
Off-Label Use and Dosage (Adult)
Guideline-Supported Use
There is limited information regarding Off-Label Guideline-Supported Use of Trifluoperazine in adult patients.
Non–Guideline-Supported Use
There is limited information regarding Off-Label Non–Guideline-Supported Use of Trifluoperazine in adult patients.
Pediatric Indications and Dosage
FDA-Labeled Indications and Dosage (Pediatric)
Schizophrenia
- Dosage should be adjusted to the weight of the child and severity of the symptoms. These dosages are for children, ages 6 to 12, who are hospitalized or under close supervision.
- The starting dosage is 1 mg administered once a day or b.i.d. Dosage may be increased gradually until symptoms are controlled or until side effects become troublesome.
- While it is usually not necessary to exceed dosages of 15 mg daily, some older children with severe symptoms may require higher dosages.
Off-Label Use and Dosage (Pediatric)
Guideline-Supported Use
There is limited information regarding Off-Label Guideline-Supported Use of Trifluoperazine in pediatric patients.
Non–Guideline-Supported Use
There is limited information regarding Off-Label Non–Guideline-Supported Use of Trifluoperazine in pediatric patients.
Contraindications
- A known hypersensitivity to phenothiazines, comatose or greatly depressed states due to central nervous system depressants and, in cases of existing blood dyscrasias, bone marrow depression and preexisting liver damage.
Warnings
|
WARNING
See full prescribing information for complete Boxed Warning.
|
- Tardive Dyskinesia
- Tardive dyskinesia, a syndrome consisting of potentially irreversible, involuntary, dyskinetic movements, may develop in patients treated with antipsychotic drugs. Although the prevalence of the syndrome appears to be highest among the elderly, especially elderly women, it is impossible to rely upon prevalence estimates to predict, at the inception of antipsychotic treatment, which patients are likely to develop the syndrome. Whether antipsychotic drug products differ in their potential to cause tardive dyskinesia is unknown.
- Both the risk of developing the syndrome and the likelihood that it will become irreversible are believed to increase as the duration of treatment and the total cumulative dose of antipsychotic drugs administered to the patient increase. However, the syndrome can develop, although much less commonly, after relatively brief treatment periods at low doses.
- There is no known treatment for established cases of tardive dyskinesia, although the syndrome may remit, partially or completely, if antipsychotic treatment is withdrawn. Antipsychotic treatment itself, however, may suppress (or partially suppress) the signs and symptoms of the syndrome and thereby may possibly mask the underlying disease process. The effect that symptomatic suppression has upon the long-term course of the syndrome is unknown.
- Given these considerations, antipsychotics should be prescribed in a manner that is most likely to minimize the occurrence of tardive dyskinesia. Chronic antipsychotic treatment should generally be reserved for patients who suffer from a chronic illness that 1) is known to respond to antipsychotic drugs, and, 2) for whom alternative, equally effective, but potentially less harmful treatments are not available or appropriate. In patients who do require chronic treatment, the smallest dose and the shortest duration of treatment producing a satisfactory clinical response should be sought. The need for continued treatment should be reassessed periodically.
- If signs and symptoms of tardive dyskinesia appear in a patient on antipsychotics, drug discontinuation should be considered. However, some patients may require treatment despite the presence of the syndrome.
- Neuroleptic Malignant Syndrome (NMS)
- A potentially fatal symptom complex sometimes referred to as Neuroleptic Malignant Syndrome (NMS) has been reported in association with antipsychotic drugs. Clinical manifestations of NMS are hyperpyrexia, muscle rigidity, altered mental status and evidence of autonomic instability (irregular pulse or blood pressure, tachycardia, diaphoresis, and cardiac dysrhythmias).
- The diagnostic evaluation of patients with this syndrome is complicated. In arriving at a diagnosis, it is important to identify cases where the clinical presentation includes both serious medical illness (e.g., pneumonia, systemic infection, etc.) and untreated or inadequately treated extrapyramidal signs and symptoms (EPS). Other important considerations in the differential diagnosis include central anticholinergic toxicity, heat stroke, drug fever and primary central nervous system (CNS) pathology.
- The management of NMS should include 1) immediate discontinuation of antipsychotic drugs and other drugs not essential to concurrent therapy, 2) intensive symptomatic treatment and medical monitoring, and 3) treatment of any concomitant serious medical problems for which specific treatments are available. There is no general agreement about specific pharmacological treatment regimens for uncomplicated NMS.
- If a patient requires antipsychotic drug treatment after recovery from NMS, the potential reintroduction of drug therapy should be carefully considered. The patient should be carefully monitored, since recurrences of NMS have been reported.
- An encephalopathic syndrome (characterized by weakness, lethargy, fever, tremulousness and confusion, extrapyramidal symptoms, leukocytosis, elevated serum enzymes, BUN and FBS) has occurred in a few patients treated with lithium plus an antipsychotic. In some instances, the syndrome was followed by irreversible brain damage. Because of a possible causal relationship between these events and the concomitant administration of lithium and antipsychotics, patients receiving such combined therapy should be monitored closely for early evidence of neurologic toxicity and treatment discontinued promptly if such signs appear. This encephalopathic syndrome may be similar to or the same as neuroleptic malignant syndrome (NMS).
- Patients who have demonstrated a hypersensitivity reaction (e.g., blood dyscrasias, jaundice) with a phenothiazine should not be reexposed to any phenothiazine, including trifluoperazine hydrochloride, unless in the judgment of the physician the potential benefits of treatment outweigh the possible hazard.
- Trifluoperazine hydrochloride may impair mental and/or physical abilities, especially during the first few days of therapy. Therefore, caution patients about activities requiring alertness (e.g., operating vehicles or machinery).
- If agents such as sedatives, narcotics, anesthetics, tranquilizers or alcohol are used either simultaneously or successively with the drug, the possibility of an undesirable additive depressant effect should be considered.
- Usage in Pregnancy
- Safety for the use of trifluoperazine hydrochloride during pregnancy has not been established. Therefore, it is not recommended that the drug be given to pregnant patients except when, in the judgment of the physician, it is essential. The potential benefits should clearly outweigh possible hazards. There are reported instances of prolonged jaundice, extrapyramidal signs, hyperreflexia or hyporeflexia in newborn infants whose mothers received phenothiazines.
- Reproductive studies in rats given over 600 times the human dose showed an increased incidence of malformations above controls and reduced litter size and weight linked to maternal toxicity. These effects were not observed at half this dosage. No adverse effect on fetal development was observed in rabbits given 700 times the human dose nor in monkeys given 25 times the human dose.
Precautions
General
- Given the likelihood that some patients exposed chronically to antipsychotics will develop tardive dyskinesia, it is advised that all patients in whom chronic use is contemplated be given, if possible, full information about this risk. The decision to inform patients and/or their guardians must obviously take into account the clinical circumstances and the competency of the patient to understand the information provided.
- Thrombocytopenia and anemia have been reported in patients receiving the drug. Agranulocytosis and pancytopenia have also been reported-warn patients to report the sudden appearance of sore throat or other signs of infection. If white blood cell and differential counts indicate cellular depression, stop treatment and start antibiotic and other suitable therapy.
- Jaundice of the cholestatic type of hepatitis or liver damage has been reported. If fever with grippe-like symptoms occurs, appropriate liver studies should be conducted. If tests indicate an abnormality, stop treatment.
- One result of therapy may be an increase in mental and physical activity. For example, a few patients with angina pectoris have complained of increased pain while taking the drug. Therefore, angina patients should be observed carefully and, if an unfavorable response is noted, the drug should be withdrawn.
- Because hypotension has occurred, large doses and parenteral administration should be avoided in patients with impaired cardiovascular systems. To minimize the occurrence of hypotension after injection, keep patient lying down and observe for at least 1/2 hour. If hypotension occurs from parenteral or oral dosing, place patient in head-low position with legs raised. If a vasoconstrictor is required, norepinephrine bitartrate and phenylephrine hydrochloride are suitable. Other pressor agents, including epinephrine, should not be used as they may cause a paradoxical further lowering of blood pressure.
- Since certain phenothiazines have been reported to produce retinopathy, the drug should be discontinued if ophthalmoscopic examination or visual field studies should demonstrate retinal changes.
- An antiemetic action of trifluoperazine hydrochloride may mask the signs and symptoms of toxicity or overdosage of other drugs and may obscure the diagnosis and treatment of other conditions such as intestinal obstruction, brain tumor and Reye’s syndrome.
- With prolonged administration at high dosages, the possibility of cumulative effects, with sudden onset of severe central nervous system or vasomotor symptoms, should be kept in mind.
- Antipsychotic drugs elevate prolactin levels; the elevation persists during chronic administration. Tissue culture experiments indicate that approximately 1/3 of human breast cancers are prolactin-dependent in vitro, a factor of potential importance if the prescribing of these drugs is contemplated in a patient with a previously detected breast cancer. Although disturbances such as galactorrhea, amenorrhea, gynecomastia and impotence have been reported, the clinical significance of elevated serum prolactin levels is unknown for most patients. An increase in mammary neoplasms has been found in rodents after chronic administration of antipsychotic drugs. Neither clinical nor epidemiologic studies conducted to date, however, have shown an association between chronic administration of these drugs and mammary tumorigenesis; the available evidence is considered too limited to be conclusive at this time.
- Chromosomal aberrations in spermatocytes and abnormal sperm have been demonstrated in rodents treated with certain antipsychotics.
- Because phenothiazines may interfere with thermoregulatory mechanisms, use with caution in persons who will be exposed to extreme heat.
- The presence of phenothiazines may produce false-positive phenylketonuria (PKU) test results.
- Long-Term Therapy
- To lessen the likelihood of adverse reactions related to cumulative drug effect, patients with a history of long-term therapy with trifluoperazine hydrochloride and/or other antipsychotics should be evaluated periodically to decide whether the maintenance dosage could be lowered or drug therapy discontinued.
- Leukopenia, Neutropenia and Agranulocytosis
- In clinical trial and post-marketing experience, events of leukopenia/neutropenia and agranulocytosis have been reported temporally related to antipsychotic agents.
- Possible risk factors for leukopenia/neutropenia include preexisting low white blood cell count (WBC) and history of drug induced leukopenia/neutropenia. Patients with a preexisting low WBC or a history of drug induced leukopenia/neutropenia should have their complete blood count (CBC) monitored frequently during the first few months of therapy and should discontinue Trifluoperazine Hydrochloride Tablets, USP at the first sign of a decline in WBC in the absence of other causative factors.
- Patients with neutropenia should be carefully monitored for fever or other symptoms or signs of infection and treated promptly if such symptoms occur. Patients with severe neutropenia (absolute neutrophil count < 1000/mm3) should discontinue Trifluoperazine Hydrochloride Tablets, USP and have their WBC followed until recovery.
Adverse Reactions
Clinical Trials Experience
- Drowsiness, dizziness, skin reactions, rash, dry mouth, insomnia, amenorrhea, fatigue, muscular weakness, anorexia, lactation, blurred vision and neuromuscular (extrapyramidal) reactions.
Neuromuscular (Extrapyramidal) Reactions
- These symptoms are seen in a significant number of hospitalized mental patients. They may be characterized by motor restlessness, be of the dystonic type, or they may resemble parkinsonism.
- Depending on the severity of symptoms, dosage should be reduced or discontinued. If therapy is reinstituted, it should be at a lower dosage. Should these symptoms occur in children or pregnant patients, the drug should be stopped and not reinstituted. In most cases, barbiturates by suitable route of administration will suffice. (Or, injectable diphenhydramine hydrochloride may be useful.) In more severe cases, the administration of an antiparkinsonism agent, except levodopa, usually produces rapid reversal of symptoms. Suitable supportive measures such as maintaining a clear airway and adequate hydration should be employed.
- Motor Restlessness
- Symptoms may include agitation or jitteriness and sometimes insomnia. These symptoms often disappear spontaneously. At times these symptoms may be similar to the original neurotic or psychotic symptoms. Dosage should not be increased until these side effects have subsided.
- If this phase becomes too troublesome, the symptoms can usually be controlled by a reduction of dosage or change of drug. Treatment with antiparkinsonism agents, benzodiazepines or propranolol may be helpful.
- Dystonia
- Class Effect
- Symptoms of dystonia, prolonged abnormal contractions of muscle groups, may occur in susceptible individuals during the first few days of treatment. Dystonic symptoms include: spasm of the neck muscles, sometimes progressing to tightness of the throat, swallowing difficulty, difficulty breathing, and/or protrusion of the tongue. While these symptoms can occur at low doses, they occur more frequently and with greater severity with high potency and at higher doses of first generation antipsychotic drugs. An elevated risk of acute dystonia is observed in males and younger age groups.
- Class Effect
- Pseudoparkinsonism
- Symptoms may include: mask-like facies; drooling; tremors; pill-rolling motion; cogwheel rigidity; and shuffling gait. Reassurance and sedation are important. In most cases these symptoms are readily controlled when an antiparkinsonism agent is administered concomitantly. Antiparkinsonism agents should be used only when required. Generally, therapy of a few weeks to 2 or 3 months will suffice. After this time, patients should be evaluated to determine their need for continued treatment. (Note: Levodopa has not been found effective in pseudoparkinsonism.) Occasionally it is necessary to lower the dosage of trifluoperazine hydrochloride or to discontinue the drug.
- Tardive Dyskinesia
- As with all antipsychotic agents, tardive dyskinesia may appear in some patients on long-term therapy or may appear after drug therapy has been discontinued. The syndrome can also develop, although much less frequently, after relatively brief treatment periods at low doses. This syndrome appears in all age groups. Although its prevalence appears to be highest among elderly patients, especially elderly women, it is impossible to rely upon prevalence estimates to predict at the inception of antipsychotic treatment which patients are likely to develop the syndrome. The symptoms are persistent and in some patients appear to be irreversible. The syndrome is characterized by rhythmical involuntary movements of the tongue, face, mouth or jaw (e.g., protrusion of tongue, puffing of cheeks, puckering of mouth, chewing movements). Sometimes these may be accompanied by involuntary movements of extremities. In rare instances, these involuntary movements of the extremities are the only manifestations of tardive dyskinesia. A variant of tardive dyskinesia, tardive dystonia, has also been described.
- There is no known effective treatment for tardive dyskinesia; antiparkinsonism agents do not alleviate the symptoms of this syndrome. If clinically feasible, it is suggested that all antipsychotic agents be discontinued if these symptoms appear. Should it be necessary to reinstitute treatment, or increase the dosage of the agent, or switch to a different antipsychotic agent, the syndrome may be masked.
- It has been reported that fine vermicular movements of the tongue may be an early sign of the syndrome and if the medication is stopped at that time the syndrome may not develop.
Adverse Reactions Reported with Trifluoperazine Hydrochloride or Other Phenothiazine Derivatives
- Adverse effects with different phenothiazines vary in type, frequency, and mechanism of occurrence, i.e., some are dose related, while others involve individual patient sensitivity. Some adverse effects may be more likely to occur, or occur with greater intensity, in patients with special medical problems, e.g., patients with mitral insufficiency or pheochromocytoma have experienced severe hypotension following recommended doses of certain phenothiazines.
- Neuroleptic Malignant Syndrome (NMS) has been reported in association with antipsychotic drugs.
- Not all of the following adverse reactions have been observed with every phenothiazine derivative, but they have been reported with one or more and should be borne in mind when drugs of this class are administered: extrapyramidal symptoms (opisthotonos, oculogyric crisis, hyperreflexia, dystonia, akathisia, dyskinesia, parkinsonism) some of which have lasted months and even years–particularly in elderly patients with previous brain damage; grand mal and petit mal convulsions, particularly in patients with EEG abnormalities or history of such disorders; altered cerebrospinal fluid proteins; cerebral edema; intensification and prolongation of the action of central nervous system depressants (opiates, analgesics, antihistamines, barbiturates, alcohol), atropine, heat, organophosphorus insecticides; autonomic reactions (dryness of mouth, nasal congestion, headache, nausea, constipation, obstipation, adynamic ileus, ejaculatory disorders/impotence, priapism, atonic colon, urinary retention, miosis and mydriasis); reactivation of psychotic processes, catatonic-like states; hypotension (sometimes fatal); cardiac arrest; blood dyscrasias (pancytopenia, thrombocytopenic purpura, leukopenia, agranulocytosis, eosinophilia, hemolytic anemia, aplastic anemia); liver damage (jaundice, biliary stasis); endocrine disturbances (hyperglycemia, hypoglycemia, glycosuria, lactation, galactorrhea, gynecomastia, menstrual irregularities, false-positive pregnancy tests); skin disorders (photosensitivity, itching, erythema, urticaria, eczema up to exfoliative dermatitis); other allergic reactions (asthma, laryngeal edema, angioneurotic edema, anaphylactoid reactions); peripheral edema; reversed epinephrine effect; hyperpyrexia; increased appetite; increased weight; a systemic lupus erythematosus-like syndrome; pigmentary retinopathy; with prolonged administration of substantial doses, skin pigmentation, epithelial keratopathy, and lenticular and corneal deposits.
- EKG changes-particularly nonspecific, usually reversible Q and T wave distortions-have been observed in some patients receiving phenothiazine antipsychotics. Although phenothiazines cause neither psychic nor physical dependence, sudden discontinuance in long-term psychiatric patients may cause temporary symptoms, e.g., nausea and vomiting, dizziness, tremulousness.
- Note: There have been occasional reports of sudden death in patients receiving phenothiazines. In some cases, the cause appeared to be cardiac arrest or asphyxia due to failure of the cough reflex.
Postmarketing Experience
There is limited information regarding Postmarketing Experience of Trifluoperazine in the drug label.
Drug Interactions
- As with all drugs which exert an anticholinergic effect, and/or cause mydriasis, trifluoperazine should be used with caution in patients with glaucoma.
- Phenothiazines may diminish the effect of oral anticoagulants.
- Phenothiazines can produce alpha-adrenergic blockade.
- Concomitant administration of propranolol with phenothiazines results in increased plasma levels of both drugs.
- Antihypertensive effects of guanethidine and related compounds may be counteracted when phenothiazines are used concurrently.
- Thiazide diuretics may accentuate the orthostatic hypotension that may occur with phenothiazines.
- Phenothiazines may lower the convulsive threshold; dosage adjustments of anticonvulsants may be necessary. Potentiation of anticonvulsant effects does not occur. However, it has been reported that phenothiazines may interfere with the metabolism of phenytoin and thus precipitate phenytoin toxicity.
- Drugs which lower the seizure threshold, including phenothiazine derivatives, should not be used with metrizamide. As with other phenothiazine derivatives, trifluoperazine hydrochloride should be discontinued at least 48 hours before myelography, should not be resumed for at least 24 hours post procedure and should not be used for the control of nausea and vomiting occurring either prior to myelography or post procedure with metrizamide.
Use in Specific Populations
Pregnancy
- Pregnancy Category C
- Nonteratogenic Effects
- Neonates exposed to antipsychotic drugs, during the third trimester of pregnancy are at risk for extrapyramidal and/or withdrawal symptoms following delivery. There have been reports of agitation, hypertonia, hypotonia, tremor, somnolence, respiratory distress and feeding disorder in these neonates. These complications have varied in severity; while in some cases symptoms have been self-limited, in other cases neonates have required intensive care unit support and prolonged hospitalization.
- Trifluoperazine hydrochloride should be used during pregnancy only if the potential benefit justifies the potential risk to the fetus.
- Australian Drug Evaluation Committee (ADEC) Pregnancy Category
There is no Australian Drug Evaluation Committee (ADEC) guidance on usage of Trifluoperazine in women who are pregnant.
Labor and Delivery
There is no FDA guidance on use of Trifluoperazine during labor and delivery.
Nursing Mothers
- There is evidence that phenothiazines are excreted in the breast milk of nursing mothers. Because of the potential for serious adverse reactions in nursing infants from trifluoperazine, a decision should be made whether to discontinue nursing or to discontinue the drug, taking into account the importance of the drug to the mother.
Pediatric Use
There is no FDA guidance on the use of Trifluoperazine with respect to pediatric patients.
Geriatic Use
There is no FDA guidance on the use of Trifluoperazine with respect to geriatric patients.
Gender
There is no FDA guidance on the use of Trifluoperazine with respect to specific gender populations.
Race
There is no FDA guidance on the use of Trifluoperazine with respect to specific racial populations.
Renal Impairment
There is no FDA guidance on the use of Trifluoperazine in patients with renal impairment.
Hepatic Impairment
There is no FDA guidance on the use of Trifluoperazine in patients with hepatic impairment.
Females of Reproductive Potential and Males
There is no FDA guidance on the use of Trifluoperazine in women of reproductive potentials and males.
Immunocompromised Patients
There is no FDA guidance one the use of Trifluoperazine in patients who are immunocompromised.
Administration and Monitoring
Administration
- Oral
Monitoring
There is limited information regarding Monitoring of Trifluoperazine in the drug label.
IV Compatibility
There is limited information regarding IV Compatibility of Trifluoperazine in the drug label.
Overdosage
Acute Overdose
Signs and Symptoms
- Primarily involvement of the extrapyramidal mechanism producing some of the dystonic reactions described above. Symptoms of central nervous system depression to the point of somnolence or coma. Agitation and restlessness may also occur. Other possible manifestations include convulsions, EKG changes and cardiac arrhythmias, fever and autonomic reactions such as hypotension, dry mouth and ileus.
Management
- It is important to determine other medications taken by the patient since multiple dose therapy is common in overdosage situations. Treatment is essentially symptomatic and supportive. Early gastric lavage is helpful. Keep patient under observation and maintain an open airway, since involvement of the extrapyramidal mechanism may produce dysphagia and respiratory difficulty in severe overdosage. Do not attempt to induce emesis because a dystonic reaction of the head or neck may develop that could result in aspiration of vomitus. Extrapyramidal symptoms may be treated with antiparkinsonism drugs, barbiturates, or diphenhydramine hydrochloride. See prescribing information for these products. Care should be taken to avoid increasing respiratory depression. If administration of a stimulant is desirable, amphetamine, dextroamphetamine, or caffeine with sodium benzoate is recommended. Stimulants that may cause convulsions (e.g., picrotoxin or pentylenetetrazol) should be avoided.
- If hypotension occurs, the standard measures for managing circulatory shock should be initiated. If it is desirable to administer a vasoconstrictor, norepinephrine bitartrate and phenylephrine hydrochloride are most suitable. Other pressor agents, including epinephrine, are not recommended because phenothiazine derivatives may reverse the usual elevating action of these agents and cause a further lowering of blood pressure.
- Limited experience indicates that phenothiazines are not dialyzable.
Chronic Overdose
There is limited information regarding Chronic Overdose of Trifluoperazine in the drug label.
Pharmacology
| |
| |
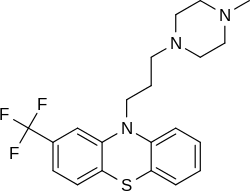
Trifluoperazine
| |
| Systematic (IUPAC) name | |
| 10-[3-(4-methylpiperazin-1-yl)propyl]- 2-(trifluoromethyl)-10H-phenothiazine | |
| Identifiers | |
| CAS number | |
| ATC code | N05 |
| PubChem | |
| DrugBank | |
| Chemical data | |
| Formula | Template:OrganicBox atomTemplate:OrganicBox atomTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBox atomTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBox atomTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBox atomTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBox |
| Mol. mass | 407.497 |
| SMILES | & |
| Pharmacokinetic data | |
| Bioavailability | ? |
| Metabolism | Hepatic |
| Half life | 10–20 hours |
| Excretion | ? |
| Therapeutic considerations | |
| Pregnancy cat. | |
| Legal status |
POM(UK) [[Prescription drug|Template:Unicode-only]](US) |
| Routes | oral, IM |
Mechanism of Action
- Trifluoperazine hydrochloride is a phenothiazine that has anticholinergic and alpha-adrenergic inhibiting properties.
Structure
- Each film-coated tablet, for oral administration, contains trifluoperazine hydrochloride, USP equivalent to 1 mg, 2 mg, 5 mg, or 10 mg trifluoperazine.
- The structural formula is:
- In addition, each tablet contains the following inactive ingredients: colloidal silicon dioxide, croscarmellose sodium, hypromellose, lactose monohydrate, magnesium stearate, microcrystalline cellulose, polydextrose, polyethylene glycol, pregelatinized starch, sodium lauryl sulfate, titanium dioxide, and triacetin. The 5 mg and 10 mg tablets contain the following coloring agents: D&C Red No. 30 Aluminum Lake, FD&C Blue No. 2 Aluminum Lake, and FD&C Yellow No. 6 Aluminum Lake.
Pharmacodynamics
There is limited information regarding Pharmacodynamics of Trifluoperazine in the drug label.
Pharmacokinetics
There is limited information regarding Pharmacokinetics of Trifluoperazine in the drug label.
Nonclinical Toxicology
There is limited information regarding Nonclinical Toxicology of Trifluoperazine in the drug label.
Clinical Studies
There is limited information regarding Clinical Studies of Trifluoperazine in the drug label.
How Supplied
- Trifluoperazine Hydrochloride Tablets, USP are available containing trifluoperazine hydrochloride, USP equivalent to 1 mg, 2 mg, 5 mg or 10 mg of trifluoperazine.
- The 1 mg tablets are white film-coated, round, unscored tablets debossed with T3 on one side of the tablet and M on the other side. They are available as follows:
- NDC 51079-572-20 - Unit dose blister packages of 100 (10 cards of 10 tablets each).
- The 2 mg tablets are white film-coated, round, unscored tablets debossed with T4 on one side of the tablet and M on the other side. They are available as follows:
- NDC 51079-573-20 - Unit dose blister packages of 100 (10 cards of 10 tablets each).
- For psychiatric patients who are hospitalized under close supervision.
- The 5 mg tablets are lavender film-coated, round, unscored tablets debossed with T5 on one side of the tablet and M on the other side. They are available as follows:
- NDC 51079-574-20 - Unit dose blister packages of 100 (10 cards of 10 tablets each).
- The 10 mg tablets are lavender film-coated, round, unscored tablets debossed with T6 on one side of the tablet and M on the other side. They are available as follows:
- NDC 51079-575-20 - Unit dose blister packages of 100 (10 cards of 10 tablets each).
- Store at 20° to 25°C (68° to 77°F). [See USP Controlled Room Temperature.]
- Protect from light.
Storage
There is limited information regarding Trifluoperazine Storage in the drug label.
Images
Drug Images
{{#ask: Page Name::Trifluoperazine |?Pill Name |?Drug Name |?Pill Ingred |?Pill Imprint |?Pill Dosage |?Pill Color |?Pill Shape |?Pill Size (mm) |?Pill Scoring |?NDC |?Drug Author |format=template |template=DrugPageImages |mainlabel=- |sort=Pill Name }}
Package and Label Display Panel
{{#ask: Label Page::Trifluoperazine |?Label Name |format=template |template=DrugLabelImages |mainlabel=- |sort=Label Page }}
Patient Counseling Information
There is limited information regarding Patient Counseling Information of Trifluoperazine in the drug label.
Precautions with Alcohol
- Alcohol-Trifluoperazine interaction has not been established. Talk to your doctor about the effects of taking alcohol with this medication.
Brand Names
- TRIFLUOPERAZINE HYDROCHLORIDE®[1]
Look-Alike Drug Names
There is limited information regarding Trifluoperazine Look-Alike Drug Names in the drug label.
Price
References
The contents of this FDA label are provided by the National Library of Medicine.
{{#subobject:
|Page Name=Trifluoperazine |Pill Name=No image.jpg |Drug Name= |Pill Ingred=|+sep=; |Pill Imprint= |Pill Dosage= |Pill Color=|+sep=; |Pill Shape= |Pill Size (mm)= |Pill Scoring= |Pill Image= |Drug Author= |NDC=
}}
{{#subobject:
|Label Page=Trifluoperazine |Label Name=Trifluoperazine02.png
}}
{{#subobject:
|Label Page=Trifluoperazine |Label Name=Trifluoperazine03.png
}}
{{#subobject:
|Label Page=Trifluoperazine |Label Name=Trifluoperazine04.png
}}
{{#subobject:
|Label Page=Trifluoperazine |Label Name=Trifluoperazine05.png
}}
{{#subobject:
|Label Page=Trifluoperazine |Label Name=Trifluoperazine06.png
}}