Sinusitis in children
(Redirected from Sinusitis in kids)
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1] Associate Editor(s)-in-Chief: Archana Vajjala, M.B.B.S
Synonyms and keywords: Sinusitis in Children, Pediatric Rhinosinusitis, Pediatric Sinusitis, Sinusitis in Kids
Overview
- Rhinosinusitis is an inflammation of the paranasal and nasal sinus mucosae which is a very common condition encountered in children.
Historical Perspective
- The term Rhinosinusitis was first coined by Task Force of Rhinology and Paranasal Sinus Committee in 1997 as sinusitis is invariably accompanied by rhinitis.
Classification
- Anatomically paranasal sinuses are classified in to [four] paired sinuses, divided into subgroups that are named according to the bones within which the sinuses lie. The paranasal air sinuses are lined with ciliated pseudostratified columnar epithelium also known as respiratory epithelium.
- Maxillary Sinuses, the largest of the paranasal sinuses, are under the eyes, in the maxillary bones. They are innervated by the trigeminal nerve (CN Vb)
- Frontal Sinuses, superior to the eyes, in the frontal bone, which forms the hard part of the forehead. They are also innervated by the trigeminal nerve (CN Va)
- Ethmoidal Sinuses, which are formed from several discrete air cells within the ethmoid bone between the nose and the eyes. They are innervated by the ethmoidal nerves, which branch from the nasociliary nerve of the trigeminal nerve (CN Va)
- Sphenoidal Sinus, in the sphenoid bone. They are innervated by the trigeminal nerve (CN Va & Vb)
- Sinusitis is classified into four subtypes/groups:
- Acute Rhinosinusitis: Sudden onset, lasting less than 4 weeks with complete resolution.
- Subacute Rhinosinusitis: A continuum of acute rhinosinusitis but less than 12 weeks.
- Recurrent Acute Rhinosinusitis: Four or more episodes of acute, lasting at least 7 days each, in any 1-year period.
- Chronic Rhinosinusitis: Signs of symptoms persist 12 weeks or longer.
Pathophysiology
- Most commonly a viral upper respiratory infection causes rhinosinusitis secondary to edema and inflammation of the nasal lining and production of thick mucus that obstructs the paranasal sinuses and allows a secondary bacterial overgrowth. Allergic rhinitis can lead to sinusitis also due to ostial obstruction. Ciliary immobility can lead to increased mucus viscosity, further blocking drainage. Bacteria are introduced into the sinuses by coughing and nose blowing. Bacterial sinusitis usually occurs after a viral upper respiratory infection and worsening symptoms after 5 days, or persistent symptoms after 10 days. A key concept in understanding the pathogenesis of acute bacterial sinusitis is that the nasal and nasopharyngeal mucosae are continuous with the paranasal sinus mucosa. Any process that affects the nasal mucosa may also affect the sinus mucosa; The mucosa consists of mucus secreting goblet cells and pseudo-stratified ciliated columnar epithelium. The role of the mucus covering the mucosa is to catch the dust, stimulating particles and microorganisms. The drainage of mucus is by active mucociliary transport, and not by gravity. Nasal secretions originate from goblet cells, epithelial cells, epithelial cell proteins, vascular transudation and lacrimal fluid. The essential protein parts of these secretions are mucin glycoproteins composed of oligosaccharide side chains and a peptide core structure. Those glycoproteins affect the composition of the mucus and facilitate the interaction between microorganisms and host. Mucin binds surface adhesins on microorganisms therefore inhibiting their ability to colonize the epithelium. Mucociliary movement transports mucus from the paranasal sinuses to the nasal cavity and pharynx where it is swallowed. The large nasal mucosal surface consists of a mucus layer that moistens the air flowing over it and filters the air particles. In the nasal submucosa, vascular plexi swell and produce nasal congestion after exposure to certain stimuli such as noxious or allergic triggers, and temperature changes.
Causes
The most common causes of [sinusitis] include conditions that interferes with normal sinus drainage predisposes to the development of infection.
- Obstruction of the sinus outflow tract may be due to mucosal swelling (allergic rhinitis, viral URI)
- Mechanical obstruction (nasal polyp, foreign body, tumor, anatomic abnormality).
- Instrumentation (with nasotracheal, nasogastric, orotracheal, or orogastric tubes) is an essential risk factor for ABRS.
Differentiating [Sinusitis] from other Diseases
- Differential diagnosis include
- Adenoid hypertrophy
- Adenoiditis
- Benign tumors of the nasal cavity
- Benign tumors of the sinuses
- Ciliary dyskinesia
- Congenital malformations of the sinuses
- Immune deficiency
- Upper respiratory infection
For further information about the differential diagnosis, click here.
Epidemiology and Demographics
Frequency
- Although the exact incidence of sinusitis in the pediatric population in united states is unclear, it is diagnosed commonly, most often following a viral URTI. The number of URTIs that an individual has per year may be as high as 25 (children will have on average 6-8 per year); the number depends on a several factors, including age, day care attendance, and number of siblings
Age
- Patients of all age groups may develop [sinusitis].
- [Sinusitis] is more commonly observed among children younger than 15 years of age and adults aged [25 to 64] years.
Gender
- There is no sex predilection for [sinusitis].
Race
- There is no racial predilection for [sinusitis].
Risk Factors
- Local predisposing factors
- Allergic rhinitis
- URI
- Anatomic abnormality
- Deviated septum
- Concha bullosa
- Enlarged adenoid
- Nasal polyps
- Tumor
- Foreign body
- Trauma
- Barotrauma
- Diving, swimming
- Smoke
- Topical decongestant abuse
- Nasal intubation, Nasogastric tube
- Systemic predisposing factors
- Immune deficiency
- IgA deficiency
- Pan-hypogammaglobulinemia
- IgG subclass deficiency
- HIV
- Cystic fibrosis
- Ciliary disorder
- Immune deficiency
Natural History, Complications and Prognosis
- Early clinical features include [rhinorrhoea] and [headache]
- If left untreated, many patients with [rhinosinusitis] may progress to develop [chronic rhinosinusitis].
- Common complications of [sinusitis] include
- Orbit (optic neuritis, orbital and periorbital cellulitis, Orbital and subperiosteal abscess)
- Central nervous system (meningitis, subdural and epidural empyema, brain abscess and venous sinus thrombosis)
- Bone (maxillary osteitis, frontal osteitis (Pott puffy tumor))
Diagnosis
Diagnostic Criteria
- The IDSA guidelines suggest that ABRS can be diagnosed with each of the following clinical scenarios:
- URI symptoms lasting more than 10 days without any improvement;
- Severe onset of signs and symptoms lasting more than 3-4 consecutive days, like high grade fever (>39°C),facial pain or purulent nasal discharge;
- Worsening of signs and symptoms following a typical viral URI that lasted 5-6 days and were initially improving, like new onset of fever, headache, or increase in nasal discharge “double-sickening”.
Symptoms
- Symptoms of [Sinusitis] may include the following:
- Common symptoms include:
- Daytime cough and rhinorrhea
- Nasal congestion
- Infrequent low-grade fever
- Otitis media (50-60% of patients)
- Irritability
- Headache
- Common symptoms include:
- Signs and symptoms of severe infection include:
- Purulent rhinorrhea
- High fever (ie, >39°C)
- Periorbital edema
- Signs and symptoms of severe infection include:
Physical Examination
- Physical examination may be remarkable for:
- Anterior rhinoscopy
- Examine the middle turbinate and middle meatus for evidence of purulence or sinus discharge.
- Polyps, if present, should prompt an evaluation for cystic fibrosis.
- Anterior rhinoscopy
- Nasal endoscopy
- Provides an excellent look at the middle meatus with accurate examination results outside the operating room.
Laboratory Findings
- There are no specific laboratory findings associated with [sinusitis] that can help in making the diagnosis. However, they can be essential in determining whether associated conditions such as allergic rhinitis, cystic fibrosis, or immunodeficiency are present. In addition, in patients with suppurative complications or in very sick children, some blood work and cultures may be helpful for determining treatment.
X-ray
- An x-ray may not be helpful in the diagnosis of [sinusitis] as 75% of them are either underestimate or overestimate the disease. Inaccuracies are compounded by mucosal tears, asymmetric facial or sinus development, overlying soft tissue, multiple septal walls, sinus overlap, improper exposure, and head rotation.
Ultrasonography
- There are no ultrasound findings associated with [Sinusitis]. However, an ultrasound may be helpful in the diagnosis of [maxillary sinusitis], but results have been somewhat inconsistent.
CT scan
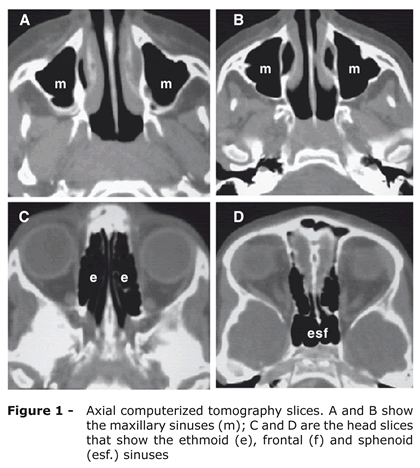
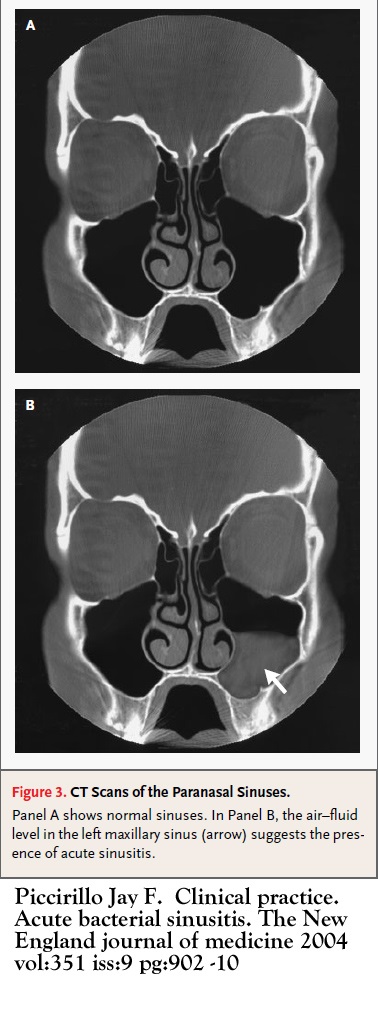
- [Sinuses] CT scan is helpful in the diagnosis of [sinusitis]. It helps detect mucosal inflammation and anatomic abnormalities in the paranasal sinuses. CT scanning provides a reliable picture of the ostiomeatal complex in a noninvasive fashion.
- CT scanning demonstrates exceptional diagnostic accuracy for the diagnosis of pediatric sinusitis with excellent sensitivity and specificity.
- Findings on CT scan suggestive of/diagnostic of [Sinusitis] include [Mucosal inflammation/sinus opacification], [Anatomic abnormalities].
- CT scanning is mandatory before endoscopic sinus surgery and very valuable when an impending complication of sinusitis such as periorbital or intracranial involvement exists.
- Note anatomic abnormalities, hypoplastic maxillary sinuses, concha bullosa, and changes consistent with cystic fibrosis (eg, medial displacement of the lateral nasal wall) on review of CT scans.
- A thinning of the surrounding bone with wispy areas of calcium density may be observed in patients with allergic fungal sinusitis.
MRI
- MRI may be helpful in the diagnosis of complications of [sinusitis] like [Intracranial complications], [allergic fungal sinusitis]
Treatment
Medical Therapy
- An acute attack of rhinosinusitis is usually self-limiting and recovers with symptomatic treatment and with minimal intervention. Steam inhalation, adequate hydration, instillation of topical decongestants, warm facial packs application, and saline nasal drops are useful. Nasal steroidal or cromolyn drops or sprays improve symptoms in children with concurrent nasal allergy. Environmental pollutants worsen the situation, and hence avoidance of them tends to improve rhinosinusitis. Antibiotics are usually not warranted. A “wait-and-watch” policy for 7–10 days is fruitful and cost-effective. About 90% recover without antibiotics in a week. [1]
- Antibiotics
- Antibiotics are reserved for children with severe acute sinusitis, Persistent acute sinusitis, Toxic child with suspected complications or persistence of symptoms. Choice of antibiotics should be guided by local susceptibility studies, safety profile, and child's age. Usual preferred are amoxicillin, coamoxiclav, oral cephalosporins, and macrolide group of antibiotics. Treat for 10-14 days or for 1 week beyond symptom resolution. 2 weeks course is usually required. Associated conditions should be simultaneously and individually addressed as follows.
- Irrigation
- Saline sinus irrigation has demonstrated efficacy in the treatment of acute and chronic sinusitis as It increases mucociliary flow rates and aids in vasoconstriction. It mechanically clears secretions, decreases bacterial counts, and clears allergens and environmental irritants from the nose.
- Steroids
- Nasal steroids are essential for patients with concurrent allergic rhinitis. Of patients with allergic rhinitis, 90% report improvement in symptoms, including nasal congestion. Short bursts of systemic steroids can be helpful for patients with allergies. Many otolaryngologists also give patients with nasal polyposis a short burst before surgical intervention to decrease intraoperative blood loss.
- Decongestants and antihistamines
- Nasal decongestants are variably effective. Topical decongestants may improve patients' level of comfort. Restricting use to the first 4-5 days of medical treatment is best in order to avoid rebound vasodilatation.
- Mucolytics are variably effective. No controlled studies have demonstrated efficacy. Antihistamines are most useful in patients with atopy.
- Immunotherapy
- Immunotherapy is effective for patients with known specific allergies who have symptoms not responsive to other forms of traditional medical therapy.
- Optimization of associated medical conditions
- Allergic rhinitis - Measures include allergen avoidance, optimal environment, nasal steroids, a second-generation antihistamine, and possible immunotherapy.
- Gastroesophageal reflux - Treat in consultation with a pediatrician or GI specialist. Conservative measures include elevating the head of the bed, not feeding immediately before bedtime, and thickening feeds. Medical therapy includes H-2 blockers, prokinetic agents, and hydrogen ion pump inhibitors.
- Immune deficiency - Treat in consultation with an immunologist and possibly an infectious-disease specialist. Treatment involves aggressive routine medical therapy and possibly intravenous gamma-globulin injections. This is an expensive type of therapy with many possible associated complications.
- Asthma - Measures include avoidance of exacerbating factors and use of bronchodilators and inhaled steroids.
- Cystic fibrosis - Aggressive nasal toilet with saline irrigations, nasal steroids, and antibiotic irrigations for pseudomonad colonization may help optimize this condition, although antibiotic irrigations have never been prospectively studied effectively.
- Immotile cilia syndromes - Mechanical clearance of secretions with daily irrigations is helpful in reducing the number of infections.
- Chronic sinusitis - For patients with chronic rhinosinusitis, administer at least 4 weeks of a broad-spectrum beta-lactamase–resistant second-line antibiotic therapy. Consider changing antibiotics if no significant response has occurred within 1 week. A culture may be required at that point to more appropriately adjust antibiotic coverage.
- All of the above medical adjuncts may play a role, especially nasal steroids and saline irrigations. Excluding or maximally treating all associated conditions is essential
Surgery
- When appropriate, maximal medical therapy fails or with associated anatomic aberrations, surgical interventions are contemplated in rhinosinusitis.
- Adenoidectomy
- [Adenoidectomy] is usually the first surgical intervention considered for children with CRS. A significant symptom overlap exists between adenoiditis and chronic sinusitis. The adenoids are niduses for infection and sources of obstruction. With adenoidectomy alone, symptom improvement occurs for more than 50% of patients.
- Functional endoscopic sinus surgery
- Consider surgery as a last resort in the pediatric population. Uncinate removal, anterior ethmoidectomy, and maxillary antrostomy are the most common forms of surgery.
- Balloon sinuplasty
- This new procedure should be considered prior to endoscopic sinus surgery. It is helpful for children, especially those children with minimal findings on CT scan but with significant symptoms and a failure to respond to continued medical therapy.
- Adenoidectomy
Management of complications
- Intra orbital and intracranial complications are common in chronic sinusitis, and fungal sinusitis with cystic fibrosis and immunodeficient states. Meningitis, abscess, and cavernous sinus thrombosis may occur. Sinusitis may extend to adjacent tissues and cause adenoiditis, serous or purulent otitis media, laryngitis, and dacryocystitis. Osteomyelitis and mucocele formation are also noted. Hospitalization and intravenous antibiotics may be required for treatment of these complications. Prolonged course of antibiotics for 4–6 weeks may be necessitated in some. Cerebral venous thrombosis needs anticoagulation. Nasal decongestants and steroids and nasal saline irrigation may be required for a longer time in such patients even after cessation of antimicrobial therapy. Pollutants, irritants, and allergens in the environment increase symptoms and avoidance of them is of benefit.
- Sinusitis involving the orbit is potentially life threatening and has a high risk of rapid visual loss. Manage orbital involvement closely, even in early cases, because visual changes may be permanent. Orbital involvement requires intravenous antibiotics and possible endoscopic or open surgical management by physicians with expertise in treating these patients.
- Intracranial involvement in sinusitis usually occurs subsequent to direct spread from sphenoid or frontal sinus disease. Subdural and frontal lobe abscesses are most common and meningitis may occur. Administer intravenous antibiotics with good cerebrospinal fluid (CSF) penetration, such as third-generation cephalosporins. Obtain empiric broad-spectrum intravenous antibiotic coverage while awaiting more specific culture and sensitivity results.
Prognosis
- Prognosis is excellent for acute rhinosinusitis. Chronic sinusitis can be much more difficult to manage, but with optimal treatment of associated conditions and full medical treatment, high cure rates are probable. Only rarely is surgery required.
Prevention
- Effective measures for the primary prevention of [Sinusitis] include prevention of risk factors that can help avoid development of rhinosinusitis. These include environmental pollutants including tobacco smoke, repeated colds and upper airway infections, daycare centre attendance, nasal allergies, and anatomical aberrations.
- Acute attacks of rhinosinusitis should be optimally managed to prevent progress to chronicity. Influenza and pneumococcal vaccines could also lead to fall in upper airway infections and hence rhinosinusitis.
- Finally good nasal hygiene and use of saline irrigations may be critical for the prevention of exacerbations of acute or chronic sinusitis. Maximize control of associated conditions and warn patients to avoid exposure to environmental irritants such as cigarette smoke.
Conclusion
- Rhinosinusitis is an upper airway infection with chronic implications. Prompt management would prevent cases slipping into chronicity with resistant polymicrobial infections. Management of chronic rhinosinusitis is an expensive, long-term affair with high likelihood of complications. Hence prevention and control of rhinosinusitis will assist in decreasing morbidity and lessen the burden on healthcare expenditure. Achieving sinonasal eutrophism and efficient mucociliary transport is the keystone to sinus health and reduction of recurrences.
References
- ↑ Badr, Dana T.; Gaffin, Jonathan M.; Phipatanakul, Wanda (2016). "Pediatric Rhinosinusitis". Current Treatment Options in Allergy. 3 (3): 268–281. doi:10.1007/s40521-016-0096-y. ISSN 2196-3053.