Intravenous therapy
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]
Overview
Intravenous therapy or IV therapy is the giving of liquid substances directly into a vein. It can be intermittent or continuous; continuous administration is called an intravenous drip. The word intravenous simply means "within a vein", but is most commonly used to refer to IV therapy. Therapies administered intravenously are often called specialty pharmaceuticals.
Compared with other routes of administration, the intravenous route is the fastest way to deliver fluids and medications throughout the body. Some medications, as well as blood transfusions and lethal injections, can only be given intravenously.
Intravenous access devices
Needle and syringe
The simplest form of intravenous access is a syringe with an attached hollow needle. The needle is inserted through the skin into a vein, and the contents of the syringe are injected through the needle into the bloodstream. This is most easily done with an arm vein, especially one of the metacarpal veins. Usually it is necessary to use a constricting band first to make the vein bulge; once the needle is in place, it is common to draw back slightly on the syringe to aspirate blood, thus verifying that the needle is really in a vein; then the constricting band is removed before injecting.
This is the most common method of intravenous drug use for euphoriants such as heroin, or in any case where a person must self-administer intravenous medication at home. It is also a convenient way to deliver life-saving medications in an emergency. However, in a controlled health-care setting, direct injection is rarely used since it only allows delivery of a single dose of medication.
Peripheral IV lines
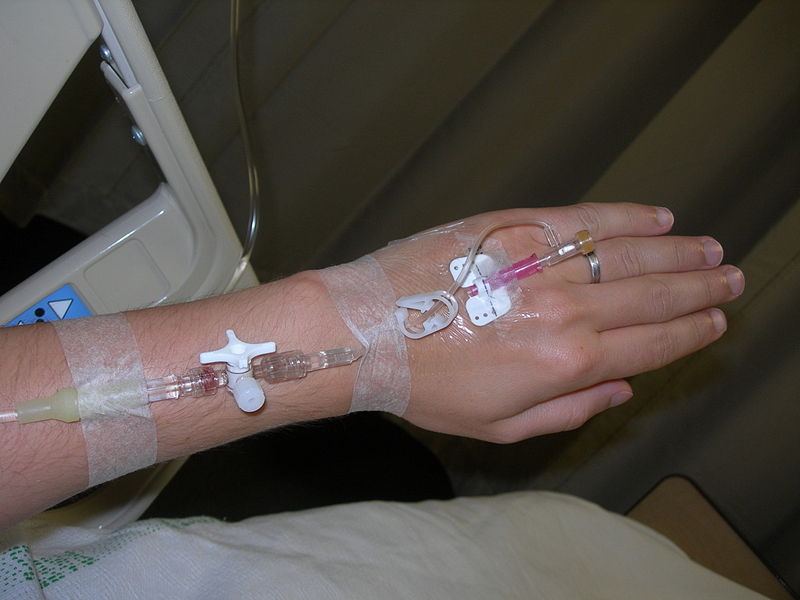
This is the most common intravenous access method in both hospitals and pre-hospital services. A peripheral IV line consists of a short catheter (a few centimeters long) inserted through the skin into a peripheral vein, any vein that is not in the chest or abdomen. Arm and hand veins are typically used although leg and foot veins are occasionally used. Veins in the hands are the common site in emergency settings, commonly performed by paramedics and emergency physicians. On infants the scalp veins are sometimes used. Part of the catheter remains outside the skin is called the connecting hub, that can be connected to a syringe or an intravenous infusion line, or capped with a bung between treatments. Ported cannula have an injection port on the top that is often used to administer medicine. The caliber of cannulae is commonly indicated in gauge, with 14 being a very large cannula (used in resuscitation settings) and 24-26 the smallest. The most common sizes are 16-gauge (midsize line used for blood donation and transfusion), 18- and 20-gauge (all-purpose line for infusions and blood draws), and 22-gauge (all-purpose pediatric line). 12- and 14-gauge peripheral lines actually deliver equivalent volumes of fluid faster than central lines, accounting for their popularity in emergency medicine; these lines are frequently called "large bores" or "trauma lines".
Blood can be drawn from a peripheral IV if necessary, but only if it is in a relatively large vein and only if the IV is newly inserted. Blood draws are typically taken with specialized IV access sets known as phlebotomy kits, and once the draw is complete, the needle is removed and the site is not used again. If a patient needs frequent venous access, the veins may scar and narrow, making any future access extremely difficult or impossible; this situation is known as a "blown vein," and the person attempting to obtain the access must find a new access site proximal to the "blown" area.
Originally, a peripheral IV was simply a needle that was taped in place and connected to tubing rather than to a syringe; this system is still used for blood donation sets, as the IV access will only be needed for a few minutes and the donor may not move while the needle is in place. Today, hospitals use a safer system in which the catheter is a flexible plastic tube that originally contains a needle to allow it to pierce the skin; the needle is then removed and discarded, while the soft catheter stays in the vein. This method is a variation of the Seldinger technique. The external portion of the catheter, which is usually taped in place or secured with a self-adhesive dressing, consists of an inch or so of flexible tubing and a locking hub. For centrally placed IV lines, sets and flushes contain a small amount of the anticoagulant heparin to keep the line from clotting off, and frequently are called "heparin locks" or "hep-locks". However, heparin is no longer recommended as a locking solution for peripheral IVs; saline is now the solution of choice for a "vac lock".
A peripheral IV cannot be left in the vein indefinitely, because of the risk of insertion-site infection leading to phlebitis, cellulites and bacterias. The CDC updated their guidelines and now advise the cannula need to be replaced every 48-72 hours. This was based on studies organised to identify causes of Methicilline Resistant Staphylococcus aureus MRSA infection in hospitals. In the United Kingdom, the UK Department of health published their finding about risk factors associated with increased MRSA infection, now include intravenous cannula, central venous catheters and urinary catheters as the main factors increasing the risk of spreading antibiotic resistant starin bacteria in hospitals.
Central IV lines
Central IV lines flow through a catheter with its tip within a large vein, usually the superior vena cava or inferior vena cava, or within the right atrium of the heart. This has several advantages over a peripheral IV:
- It can deliver fluids and medications that would be overly irritating to peripheral veins because of their concentration or chemical composition. These include some chemotherapy drugs and total parenteral nutrition.
- Medications reach the heart immediately, and are quickly distributed to the rest of the body.
- There is room for multiple parallel compartments (lumen) within the catheter, so that multiple medications can be delivered at once even if they would not be chemically compatible within a single tube.
- Caregivers can measure central venous pressure and other physiological variables through the line.
Central IV lines carry risks of bleeding, bacterial infection, and gas embolism (see Risks below).
There are several types of central IVs, depending on the route that the catheter takes from the outside of the body to the vein.
Peripherally inserted central catheter
PICC lines are used when intravenous access is required over a prolonged period of time, as in the case of long chemotherapy regimens, extended antibiotic therapy, or total parenteral nutrition.
The PICC line is inserted into a peripheral vein using the Seldinger technique under ultrasound guidance, usually in the arm, and then carefully advanced upward until the catheter is in the superior vena cava or the right atrium. This is usually done by feel and estimation; an X-ray then verifies that the tip is in the right place.
A PICC may have two parallel compartments, each with its own external connector (double-lumen), or a single tube and connector (single-lumen). From the outside, a single-lumen PICC resembles a peripheral IV, except that the tubing is slightly wider.
The insertion site must be covered by a larger sterile dressing than would be required for a peripheral IV, due to the higher risk of infection if bacteria travel up the catheter. However, a PICC poses less of a systemic infection risk than other central IVs, because bacteria would have to travel up the entire length of the narrow catheter before spreading through the bloodstream.
The chief advantage of a PICC over other types of central lines is that it is easy to insert, poses a relatively low risk of bleeding, is externally unobtrusive, and can be left in place for months to years for patients who require extended treatment. The chief disadvantage is that it must travel through a relatively small peripheral vein and is therefore limited in diameter, and also somewhat vulnerable to occlusion or damage from movement or squeezing of the arm.
Central venous lines
There are several types of catheters that take a more direct route into central veins. These are collectively called central venous lines.
In the simplest type of central venous access, a catheter is inserted into a subclavian, internal jugular, or (less commonly) a femoral vein and advanced toward the heart until it reaches the superior vena cava or right atrium. Because all of these veins are larger than peripheral veins, central lines can deliver a higher volume of fluid and can have multiple lumens.
Another type of central line, called a Hickman line or Broviac catheter, is inserted into the target vein and then "tunneled" under the skin to emerge a short distance away. This reduces the risk of infection, since bacteria from the skin surface are not able to travel directly into the vein; these catheters are also made of materials that resist infection and clotting.
Implantable ports
A port (often referred to by brand names such as Port-a-Cath or MediPort) is a central venous line that does not have an external connector; instead, it has a small reservoir that is covered with silicone rubber and is implanted under the skin. Medication is administered intermittently by placing a small needle through the skin, piercing the silicone, into the reservoir. When the needle is withdrawn the reservoir cover reseals itself. The cover can accept hundreds of needle sticks during its lifetime. It is possible to leave the ports in the patient's body for years, if this is done however, the port must be accessed monthly and flushed with an anti-coagulant, or the patient risks it getting plugged up. If it is plugged it becomes a hazard as a thrombosis will eventually form with an accompanying risk of embolisation. Removal of a port is usually a simple outpatient procedure, however installation is more complex and a good implant is fairly dependent on the skill of the Radiologist. Ports cause less inconvenience and have a lower risk of infection than PICCs, and are therefore commonly used for patients on long-term intermittent treatment.
Forms of intravenous therapy
Intravenous drip
An intravenous drip is the continuous infusion of fluids, with or without medications, through an IV access device. This may be to correct dehydration or an electrolyte imbalance, to deliver medications, or for blood transfusion.
IV fluids
There are two types of fluids that are used for intravenous drips; crystalloids and colloids. Crystalloids are aqueous solutions of mineral salts or other water-soluble molecules. Colloids contain larger insoluble molecules, such as gelatin; blood itself is a colloid.
The most commonly used crystalloid fluid is normal saline, a solution of sodium chloride at 0.9% concentration, which is close to the concentration in the blood (isotonic). Ringer's lactate or Ringer's acetate (ASERING, patented brandname of Otsuka Indonesia) is another isotonic solution often used for large-volume fluid replacement. A solution of 5% dextrose in water, sometimes called D5W, is often used instead if the patient is at risk for having low blood sugar or high sodium. The choice of fluids may also depend on the chemical properties of the medications being given.
Intravenous fluids must always be sterile.
| Solution | Other Name | [Na+](mmol/L) | [Cl-](mmol/L) | [Glucose](mmol/L) | [Glucose](mg/dl) |
|---|---|---|---|---|---|
| D5W | 5% Dextrose | 0 | 0 | 278 | 5000 |
| 2/3D & 1/3S | 3.3% Dextrose / 0.3% saline | 51 | 51 | 185 | 3333 |
| Half-normal saline | 0.45% NaCl | 77 | 77 | 0 | 0 |
| Normal saline | 0.9% NaCl | 154 | 154 | 0 | 0 |
| Ringer's lactate | Lactated Ringer | 130 | 109 | 0 | 0 |
Ringer's lactate also has 28 mmol/L lactate, 4 mmol/L K+ and 3 mmol/L Ca2+. Ringer's acetate (ASERING) also has 28 mmol/L acetate, 4 mmol/L K+ and 3 mmol/L Ca2+.
| Solution | Change in ECF | Change in ICF |
|---|---|---|
| D5W | 333 mL | 667 mL |
| 2/3D & 1/3S | 556 mL | 444 mL |
| Half-normal saline | 667 mL | 333 mL |
| Normal saline | 1000 mL | 0 mL |
| Ringer's lactate | 900 mL | 100 mL |
Choice of fluid
Solutions lower in chlorides such as Hartmann's solution and Lactated Ringer's solution, may cause less acute kidney injury when administered to adults in intensive care.[1] Likewise hydroxyethyl starch should be avoided.[2]
Infusion equipment
A standard IV infusion set consists of a pre-filled, sterile container (glass bottle, plastic bottle or plastic bag) of fluids with an attached drip chamber which allows the fluid to flow one drop at a time, making it easy to see the flow rate (and also reducing air bubbles); a long sterile tube with a clamp to regulate or stop the flow; a connector to attach to the access device; and connectors to allow "piggybacking" of another infusion set onto the same line, e.g., adding a dose of antibiotics to a continuous fluid drip.
An infusion pump allows precise control over the flow rate and total amount delivered, but in cases where a change in the flow rate would not have serious consequences, or if pumps are not available, the drip is often left to flow simply by placing the bag above the level of the patient and using the clamp to regulate the rate; this is a gravity drip.
A rapid infuser can be used if the patient requires a high flow rate and the IV access device is of a large enough diameter to accommodate it. This is either an inflatable cuff placed around the fluid bag to force the fluid into the patient or a similar electrical device that may also heat the fluid being infused.
Intermittent infusion
Intermittent infusion is used when a patient requires medications only at certain times, and does not require additional fluid. It can use the same techniques as an intravenous drip (pump or gravity drip), but after the complete dose of medication has been given, the tubing is disconnected from the IV access device. Some medications are also given by IV push, meaning that a syringe is connected to the IV access device and the medication is injected directly (slowly, if it might irritate the vein or cause a too-rapid effect). Once a medicine has been injected into the fluid stream of the IV tubing there must be some means of ensuring that it gets from the tubing to the patient. Usually this is accomplished by allowing the fluid stream to flow normally and thereby carry the medicine into the bloodstream; however, a second fluid injection is sometimes used, a "flush", following the injection to push the medicine into the bloodstream more quickly.
Risks of intravenous therapy
Intravenous therapy has many risks and should therefore only be performed by trained personnel under medical supervision, using proper equipment.
Infection
Any break in the skin carries a risk of infection. Although IV insertion is a sterile procedure, skin-dwelling organisms such as Coagulase-negative Staphylococcus or Candida albicans may enter through the insertion site around the catheter, or bacteria may be accidentally introduced inside the catheter from contaminated equipment. Moisture introduced to unprotected IV sites through washing or bathing substantially increases the infection risks.
Infection of IV sites is usually local, causing easily visible swelling, redness, and fever. If bacteria do not remain in one area but spread through the bloodstream, the infection is called septicemia and can be rapid and life-threatening. An infected central IV poses a higher risk of septicemia, as it can deliver bacteria directly into the central circulation.
Phlebitis
Phlebitis is irritation of a vein that is not caused by infection, but from the mere presence of a foreign body (the IV catheter) or the fluids or medication being given. Symptoms are swelling, pain, and redness around the vein. The IV device must be removed and if necessary re-inserted into another extremity.
Due to frequent injections and recurring phlebitis, the peripheral veins of intravenous drug addicts, and of cancer patients undergoing chemotherapy, become hardened and difficult to access over time.
Fluid overload
This occurs when fluids are given at a higher rate or in a larger volume than the system can absorb or excrete. Possible consequences include hypertension, heart failure, weight gain and pulmonary edema.
Electrolyte imbalance
Administering a too-dilute or too-concentrated solution can disrupt the patient's balance of sodium, potassium, magnesium, and other electrolytes. Hospital patients usually receive blood tests to monitor these levels.
Embolism
A blood clot or other solid mass, or an air bubble, can be delivered into the circulation through an IV and end up blocking a vessel; this is called embolism. Peripheral IVs have a low risk of embolism, since large solid masses cannot travel through a narrow catheter, and it is nearly impossible to inject air through a peripheral IV at a dangerous rate. The risk is greater with a central IV.
Air bubbles of less than 30 milliliters generally dissolve into the circulation harmlessly. A larger amount of air, if delivered all at once, can cause life-threatening damage to pulmonary circulation, or, if extremely large (3-8 milliliters per kilogram of body weight), can stop the heart.
One reason veins are preferred over arteries for intravascular administration is because the flow will pass through the lungs before passing through the body. Air bubbles can leave the blood through the lungs. A patient with a heart defect causing a right-to-left shunt is vulnerable to embolism from smaller amounts of air.
Fatality by air embolism is vanishingly rare, in part because it is also difficult to diagnose.
Extravasation
Extravasation is the accidental administration of IV infused medicinal drugs into the surrounding tissue, either by leakage (e.g. because of brittle veins in very elderly patients), or directly (e.g. because the needle has punctured the vein and the infusion goes directly into the arm tissue).
See also
External links
cs:Intravenózní aplikace da:Drop de:Infusion it:Fleboclisi he:עירוי nl:Infuus no:Intravenøs sl:Intravenska aplikacija fi:Infuusio sv:Dropp th:การฉีดเข้าเส้น
Template:WikiDoc Sources
Template:Jb1
- ↑ Yunos N, Bellomo R (2012-10-17). "ASsociation between a chloride-liberal vs chloride-restrictive intravenous fluid administration strategy and kidney injury in critically ill adults". JAMA: The Journal of the American Medical Association. 308 (15): 1566–1572. doi:10.1001/jama.2012.13356. ISSN 0098-7484. Retrieved 2012-10-17.
- ↑ Myburgh, John A. (2012). "Hydroxyethyl Starch or Saline for Fluid Resuscitation in Intensive Care". New England Journal of Medicine. 367 (20): 1901–1911. doi:10.1056/NEJMoa1209759. ISSN 0028-4793. Retrieved 2012-11-20. Unknown parameter
|coauthors=ignored (help)