Gonadotropin-releasing hormone agonist
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]
Overview
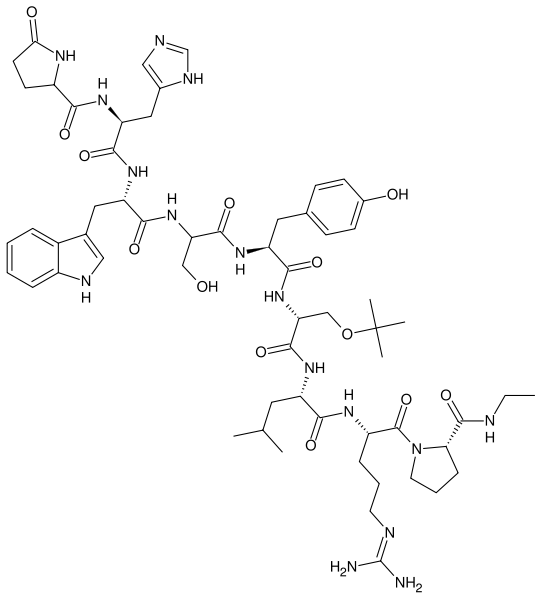
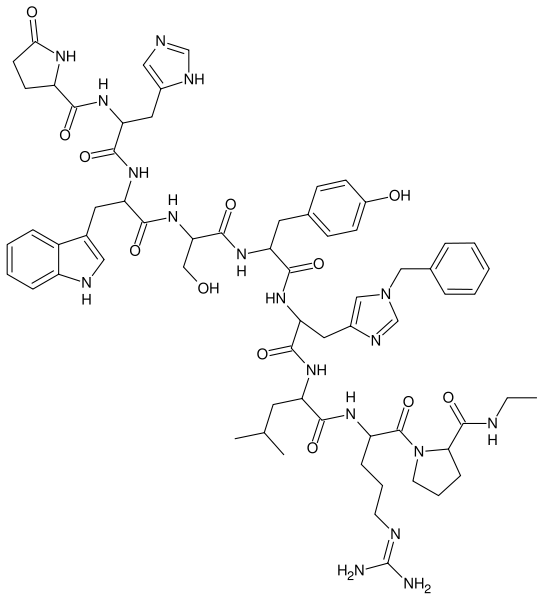
A gonadotropin-releasing hormone agonist (GnRH agonist) is a synthetic peptide modeled after the hypothalamic neurohormone GnRH that interacts with the gonadotropin-releasing hormone receptor to elicit its biologic response, the release of the pituitary hormones FSH and LH.
GnRH agonists are pregnancy category X drugs.
Flare effect and downregulation
Agonists do not quickly dissociate from the GnRH receptor. As a result initially there is an increase in FSH and LH secretion (so-called "flare effect").
However after about ten days a profound hypogonadal effect is achieved through receptor downregulation. Generally this induced and reversible hypogonadism is the therapeutic goal.
Agonists with double and single substitutions
GnRH agonists are synthetically modeled after the natural GnRH decapeptide with specific amino acid substitutions typically in position 6 and 10. These substitutions inhibit rapid degradation. Agonists with 2 substitutions include:
- leuprolide (Lupron, Eligard)
- buserelin (Suprefact, Suprecor)
- nafarelin (Synarel)
- histrelin (Supprelin)
- goserelin (Zoladex)
- deslorelin
Triptorelin is an agonist with only a single substitution at position 6.
Administration
These medications can be administered intranasally, by injection, or by implant. Injectables have been formulated for daily, monthly, and quarterly use; and implants can last from 1 to 3 months.
Uses
GnRH agonists are useful in:
- Treatment of cancers that are hormonally sensitive and where a hypogonadal state decreases the chances of a recurrence. Thus they are commonly employed in the medical management of prostate cancer and have been used in patients with breast cancer.
- Treatment of delaying puberty in individuals with precocious puberty.
- Management of female disorders that are dependent on estrogen productions. Women with menorrhagia, endometriosis. adenomyosis, or uterine fibroids may receive GnRH agonists to suppress ovarian activity and induce a hypoestrogenic state.
- IVF therapy: they allow for better control of ovarian stimulation during the administration of exogenous FSH. Typically, after GnRH agonists have induced a state of hypoestrogenism, exogenous FSH is given to stimulate ovarian follicle, followed by human chorionic gonadotropins (hCG) to trigger ovulation.
Women of reproductive age who undergo cytotoxic chemotherapy have been pretreated with GnRH agonists to reduce the risk of oocyte loss during such therapy and preserve ovarian function. Further studies are necessary to prove that this approach is useful.
Side effects
Side effects of the GnRH agonists are signs and symptoms of hypoestrogenism, including hot flashes, headaches, and osteoporosis. In patients under long-term therapy, small amounts of estrogens could be given back (“add-back regimen”) to combat such side effects.
See also