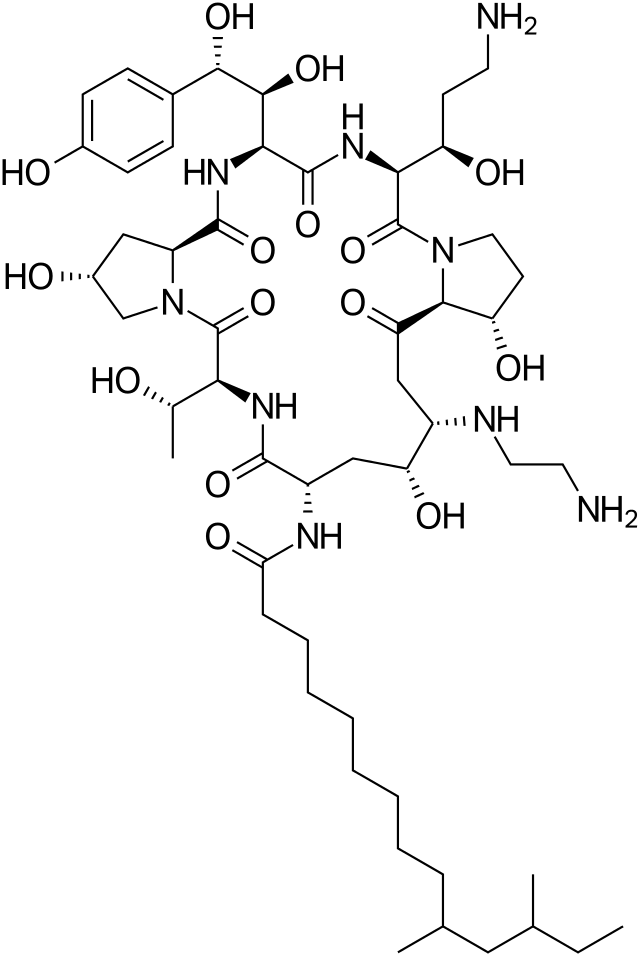
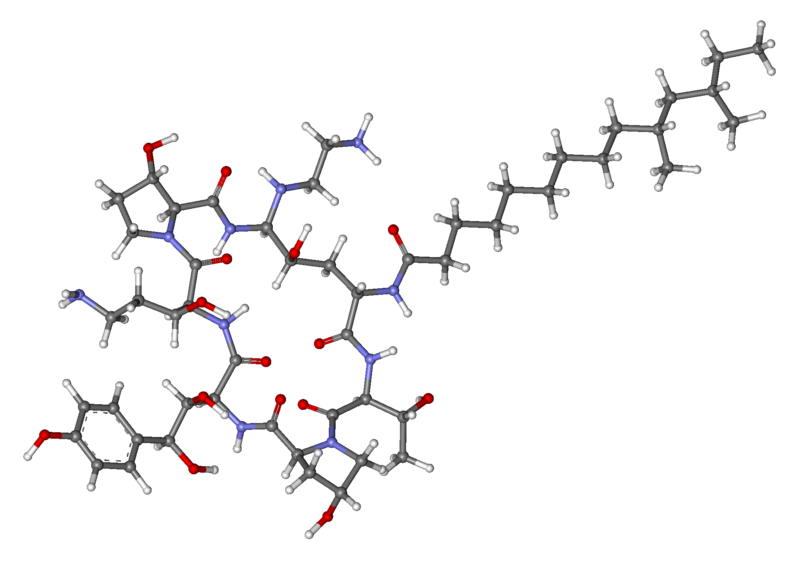
Caspofungin
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Kiran Singh, M.D. [2]
WikiDoc MAKES NO GUARANTEE OF VALIDITY. WikiDoc is not a professional health care provider, nor is it a suitable replacement for a licensed healthcare provider. WikiDoc is intended to be an educational tool, not a tool for any form of healthcare delivery. The educational content on WikiDoc drug pages is based upon the FDA package insert, National Library of Medicine content and practice guidelines / consensus statements. WikiDoc does not promote the administration of any medication or device that is not consistent with its labeling. Please read our full disclaimer here.
Overview
Caspofungin is an antifungal that is FDA approved for the treatment of fungal infections, candidemia, esophageal candidiasis, invasive aspergillosis refractory or intolerant to other therapies. Common adverse reactions include anemia, febrile neutropenia, neutropenia, thrombocytopenia, arrhythmia, atrial fibrillation, abdominal pain, bacteremia, sepsis, urinary tract infection.
Adult Indications and Dosage
FDA-Labeled Indications and Dosage (Adult)
Indications
Caspofungin® is indicated in adults and pediatric patients (3 months and older) for:
- Empirical therapy for presumed fungal infections in febrile, neutropenic patients
- Treatment of candidemia and the following Candida infections: intra-abdominal abscesses, peritonitis and pleural space infections. Caspofungin has not been studied in endocarditis, osteomyelitis, and meningitis due to Candida.
- Treatment of esophageal candidiasis.
- Treatment of invasive aspergillosis in patients who are refractory to or intolerant of other therapies (e.g., amphotericin B, lipid formulations of amphotericin B, itraconazole). Caspofungin has not been studied as initial therapy for invasive aspergillosis.
Dosage
Recommended Dosing in Adult Patients [≥18 years of age]
- The usual dose is 50 mg once daily (following a 70-mg loading dose for most indications). The safety and efficacy of a dose of 150 mg daily (range: 1 to 51 days; median: 14 days) have been studied in 100 adult patients with candidemia and other Candida infections. The efficacy of caspofungin at this higher dose was not significantly better than the efficacy of the 50-mg daily dose of caspofungin. The efficacy of doses higher than 50 mg daily in the other adult patients for whom caspofungin is indicated is not known.
Empirical Therapy
A single 70-mg loading dose should be administered on Day 1, followed by 50 mg once daily thereafter. Duration of treatment should be based on the patient's clinical response. Empirical therapy should be continued until resolution of neutropenia. Patients found to have a fungal infection should be treated for a minimum of 14 days; treatment should continue for at least 7 days after both neutropenia and clinical symptoms are resolved. If the 50-mg dose is well tolerated but does not provide an adequate clinical response, the daily dose can be increased to 70 mg.
Candidemia and Other Candida Infections
A single 70-mg loading dose should be administered on Day 1, followed by 50 mg once daily thereafter. Duration of treatment should be dictated by the patient's clinical and microbiological response. In general, antifungal therapy should continue for at least 14 days after the last positive culture. Patients who remain persistently neutropenic may warrant a longer course of therapy pending resolution of the neutropenia.
Esophageal Candidiasis
The dose is 50 mg once daily for 7 to 14 days after symptom resolution. A 70-mg loading dose has not been studied for this indication. Because of the risk of relapse of oropharyngeal candidiasis in patients with HIV infections, suppressive oral therapy could be considered.
Invasive Aspergillosis
A single 70-mg loading dose should be administered on Day 1, followed by 50 mg once daily thereafter. Duration of treatment should be based upon the severity of the patient's underlying disease, recovery from immunosuppression, and clinical response.
Patients with Hepatic Impairment
Adult patients with mild hepatic impairment (Child-Pugh score 5 to 6) do not need a dosage adjustment. For adult patients with moderate hepatic impairment (Child-Pugh score 7 to 9), caspofungin 35 mg once daily is recommended based upon pharmacokinetic data. However, where recommended, a 70-mg loading dose should still be administered on Day 1. There is no clinical experience in adult patients with severe hepatic impairment (Child-Pugh score >9) and in pediatric patients with any degree of hepatic impairment.
Patients Receiving Concomitant Inducers of Drug Clearance
- Adult patients on rifampin should receive 70 mg of caspofungin once daily. Adult patients on nevirapine, efavirenz, carbamazepine, dexamethasone, or phenytoin may require an increase in dose to 70 mg of caspofungin once daily.
Off-Label Use and Dosage (Adult)
Guideline-Supported Use
There is limited information regarding Off-Label Guideline-Supported Use of Caspofungin in adult patients.
Non–Guideline-Supported Use
There is limited information regarding Off-Label Non–Guideline-Supported Use of Caspofungin in adult patients.
Pediatric Indications and Dosage
FDA-Labeled Indications and Dosage (Pediatric)
Recommended Dosing in Pediatric Patients [3 months to 17 years of age]
- For all indications, a single 70-mg/m2 loading dose should be administered on Day 1, followed by 50 mg/m2 once daily thereafter. The maximum loading dose and the daily maintenance dose should not exceed 70 mg, regardless of the patient's calculated dose. Dosing in pediatric patients (3 months to 17 years of age) should be based on the patient's body surface area (BSA) as calculated by the Mosteller Formula

- Following calculation of the patient's BSA, the loading dose in milligrams should be calculated as BSA (m2) X 70 mg/m2. The maintenance dose in milligrams should be calculated as BSA (m2) X 50 mg/m2.
- Duration of treatment should be individualized to the indication, as described for each indication in adults. If the 50-mg/m2 daily dose is well tolerated but does not provide an adequate clinical response, the daily dose can be increased to 70 mg/m2 daily (not to exceed 70 mg).
Patients Receiving Concomitant Inducers of Drug Clearance
When caspofungin is co-administered to pediatric patients with inducers of drug clearance, such as rifampin, efavirenz, nevirapine, phenytoin, dexamethasone, or carbamazepine, a caspofungin dose of 70 mg/m2 once daily (not to exceed 70 mg) should be considered
Special Considerations for Pediatric Patients >3 Months of Age
- Follow the reconstitution procedures described above using either the 70-mg or 50-mg vial to create the reconstituted solution. From the reconstituted solution in the vial, remove the volume of drug equal to the calculated loading dose or calculated maintenance dose based on a concentration of 7 mg/mL (if reconstituted from the 70-mg vial) or a concentration of 5 mg/mL (if reconstituted from the 50-mg vial).
- The choice of vial should be based on total milligram dose of drug to be administered to the pediatric patient. To help ensure accurate dosing, it is recommended for pediatric doses less than 50 mg that 50-mg vials (with a concentration of 5 mg/mL) be used if available. The 70-mg vial should be reserved for pediatric patients requiring doses greater than 50 mg.
The maximum loading dose and the daily maintenance dose should not exceed 70 mg, regardless of the patient's calculated dose.
Off-Label Use and Dosage (Pediatric)
Guideline-Supported Use
There is limited information regarding Off-Label Guideline-Supported Use of Caspofungin in pediatric patients.
Non–Guideline-Supported Use
There is limited information regarding Off-Label Non–Guideline-Supported Use of Caspofungin in pediatric patients.
Contraindications
Caspofungin is contraindicated in patients with hypersensitivity (e.g., anaphylaxis) to any component of this product.
Warnings
Hypersensitivity
- Anaphylaxis has been reported during administration of caspofungin. If this occurs, caspofungin should be discontinued and appropriate treatment administered.
- Possible histamine-mediated adverse reactions, including rash, facial swelling, angioedema, pruritus, sensation of warmth or bronchospasm have been reported and may require discontinuation and/or administration of appropriate treatment.
Concomitant Use with Cyclosporine
- Concomitant use of caspofungin with cyclosporine should be limited to patients for whom the potential benefit outweighs the potential risk. In one clinical study, 3 of 4 healthy adult subjects who received caspofungin 70 mg on Days 1 through 10, and also received two 3 mg/kg doses of cyclosporine 12 hours apart on day 10, developed transient elevations of alanine transaminase (ALT) on day 11 that were 2 to 3 times the upper limit of normal (ULN). In a separate panel of adult subjects in the same study, 2 of 8 who received caspofungin 35 mg daily for 3 days and cyclosporine (two 3 mg/kg doses administered 12 hours apart) on day 1 had small increases in ALT (slightly above the ULN) on day 2. In both groups, elevations in aspartate transaminase (AST) paralleled ALT elevations, but were of lesser magnitude. In another clinical study, 2 of 8 healthy men developed transient ALT elevations of less than 2X ULN. In this study, cyclosporine (4 mg/kg) was administered on Days 1 and 12, and caspofungin was administered (70 mg) daily on Days 3 through 13. In one subject, the ALT elevation occurred on days 7 and 9 and, in the other subject, the ALT elevation occurred on Day 19. These elevations returned to normal by Day 27. In all groups, elevations in AST paralleled ALT elevations but were of lesser magnitude. In these clinical studies, cyclosporine (one 4 mg/kg dose or two 3 mg/kg doses) increased the AUC of caspofungin by approximately 35%.
- In a retrospective postmarketing study, 40 immunocompromised patients, including 37 transplant recipients, were treated with caspofungin and cyclosporine for 1 to 290 days (median 17.5 days). Fourteen patients (35%) developed transaminase elevations >5X upper limit of normal or >3X baseline during concomitant therapy or the 14-day follow-up period; five were considered possibly related to concomitant therapy. One patient had elevated bilirubin considered possibly related to concomitant therapy. No patient developed clinical evidence of hepatotoxicity or serious hepatic events. Discontinuations due to laboratory abnormalities in hepatic enzymes from any cause occurred in four patients. Of these, 2 were considered possibly related to therapy with caspofungin and/or cyclosporine as well as to other possible causes.
- In the prospective invasive aspergillosis and compassionate use studies, there were 4 adult patients treated with caspofungin (50 mg/day) and cyclosporine for 2 to 56 days. None of these patients experienced increases in hepatic enzymes.
- Given the limitations of these data, caspofungin and cyclosporine should only be used concomitantly in those patients for whom the potential benefit outweighs the potential risk. Patients who develop abnormal liver function tests during concomitant therapy should be monitored and the risk/benefit of continuing therapy should be evaluated.
Hepatic Effects
- Laboratory abnormalities in liver function tests have been seen in healthy volunteers and in adult and pediatric patients treated with caspofungin. In some adult and pediatric patients with serious underlying conditions who were receiving multiple concomitant medications with caspofungin, isolated cases of clinically significant hepatic dysfunction, hepatitis, and hepatic failure have been reported; a causal relationship to caspofungin has not been established.
- Patients who develop abnormal liver function tests during caspofungin therapy should be monitored for evidence of worsening hepatic function and evaluated for risk/benefit of continuing caspofungin therapy
Adverse Reactions
Clinical Trials Experience
- The following serious adverse reactions are discussed in detail in another section of the labeling:
- Hepatic effects
- Hypersensitivity
- Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in clinical trials of caspofungin cannot be directly compared to rates in clinical trials of another drug and may not reflect the rates observed in practice. The adverse reaction information from clinical trials does provide a basis for identifying adverse reactions that appear to be related to drug use and for approximating rates.
Clinical Trials Experience in Adults
The overall safety of caspofungin was assessed in 1865 adult individuals who received single or multiple doses of caspofungin: 564 febrile, neutropenic patients (empirical therapy study); 382 patients with candidemia and/or intra-abdominal abscesses, peritonitis, or pleural space infections (including 4 patients with chronic disseminated candidiasis); 297 patients with esophageal and/or oropharyngeal candidiasis; 228 patients with invasive aspergillosis; and 394 individuals in phase I studies. In the empirical therapy study patients had undergone hematopoietic stem-cell transplantation or chemotherapy. In the studies involving patients with documented Candida infections, the majority of the patients had serious underlying medical conditions (e.g., hematologic or other malignancy, recent major surgery, HIV) requiring multiple concomitant medications. Patients in the noncomparative Aspergillus studies often had serious predisposing medical conditions (e.g., bone marrow or peripheral stem cell transplants, hematologic malignancy, solid tumors or organ transplants) requiring multiple concomitant medications.
Empirical Therapy
- In the randomized, double-blinded empirical therapy study, patients received either caspofungin 50 mg/day (following a 70-mg loading dose) or AmBisome® (amphotericin B liposome for injection, 3 mg/kg/day). In this study clinical or laboratory hepatic adverse reactions were reported in 39% and 45% of patients in the caspofungin and AmBisome groups, respectively. Also reported was an isolated, serious adverse reaction of hyperbilirubinemia considered possibly related to caspofungin. Adverse reactions occurring in ≥7.5% of the patients in either treatment group are presented in Table 2
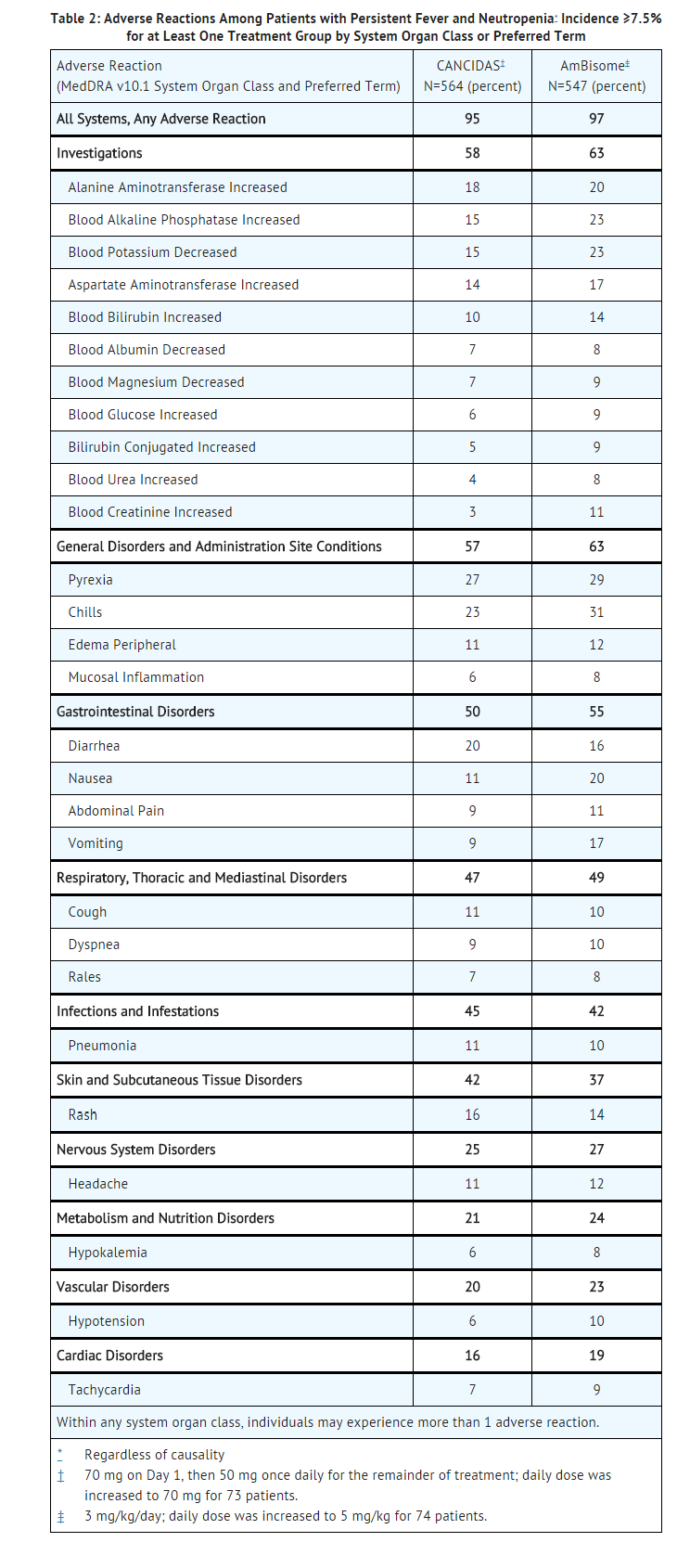
- The proportion of patients who experienced an infusion-related adverse reaction (defined as a systemic event, such as pyrexia, chills, flushing, hypotension, hypertension, tachycardia, dyspnea, tachypnea, rash, or anaphylaxis, that developed during the study therapy infusion and one hour following infusion) was significantly lower in the group treated with caspofungin (35%) than in the group treated with AmBisome (52%).
- To evaluate the effect of caspofungin and AmBisome on renal function, nephrotoxicity was defined as doubling of serum creatinine relative to baseline or an increase of ≥1 mg/dL in serum creatinine if baseline serum creatinine was above the upper limit of the normal range. Among patients whose baseline creatinine clearance was >30 mL/min, the incidence of nephrotoxicity was significantly lower in the group treated with caspofungin (3%) than in the group treated with AmBisome (12%). Clinical renal events, regardless of causality, were similar between caspofungin (75/564, 13%) and AmBisome (85/547, 16%).
Candidemia and Other Candida Infections
- In the randomized, double-blinded invasive candidiasis study, patients received either caspofungin 50 mg/day (following a 70-mg loading dose) or amphotericin B 0.6 to 1 mg/kg/day. Adverse reactions occurring in ≥10% of the patients in either treatment group are presented in Table 3.
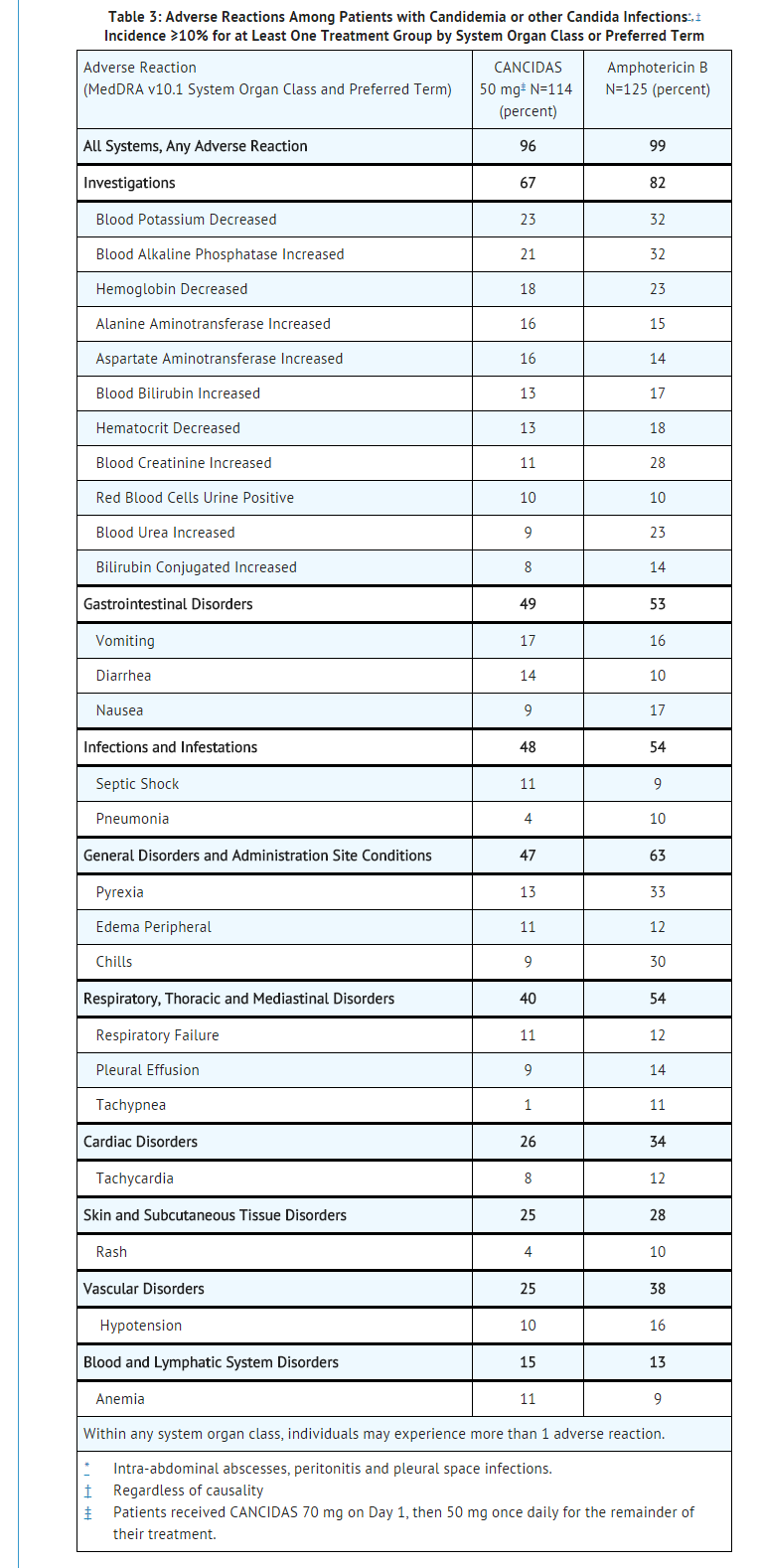
- The proportion of patients who experienced an infusion-related adverse reaction (defined as a systemic event, such as pyrexia, chills, flushing, hypotension, hypertension, tachycardia, dyspnea, tachypnea, rash, or anaphylaxis, that developed during the study therapy infusion and one hour following infusion) was significantly lower in the group treated with caspofungin (20%) than in the group treated with amphotericin B (49%).
- To evaluate the effect of caspofungin and amphotericin B on renal function, nephrotoxicity was defined as doubling of serum creatinine relative to baseline or an increase of ≥1 mg/dL in serum creatinine if baseline serum creatinine was above the upper limit of the normal range. In a subgroup of patients whose baseline creatinine clearance was >30 mL/min, the incidence of nephrotoxicity was significantly lower in the group treated with caspofungin than in the group treated with amphotericin B.
- In a second randomized, double-blinded invasive candidiasis study, patients received either caspofungin 50 mg/day (following a 70-mg loading dose) or caspofungin 150 mg/day. The proportion of patients who experienced any adverse reaction was similar in the 2 treatment groups; however, this study was not large enough to detect differences in rare or unexpected adverse events. Adverse reactions occurring in ≥5% of the patients in either treatment group are presented in Table 4.
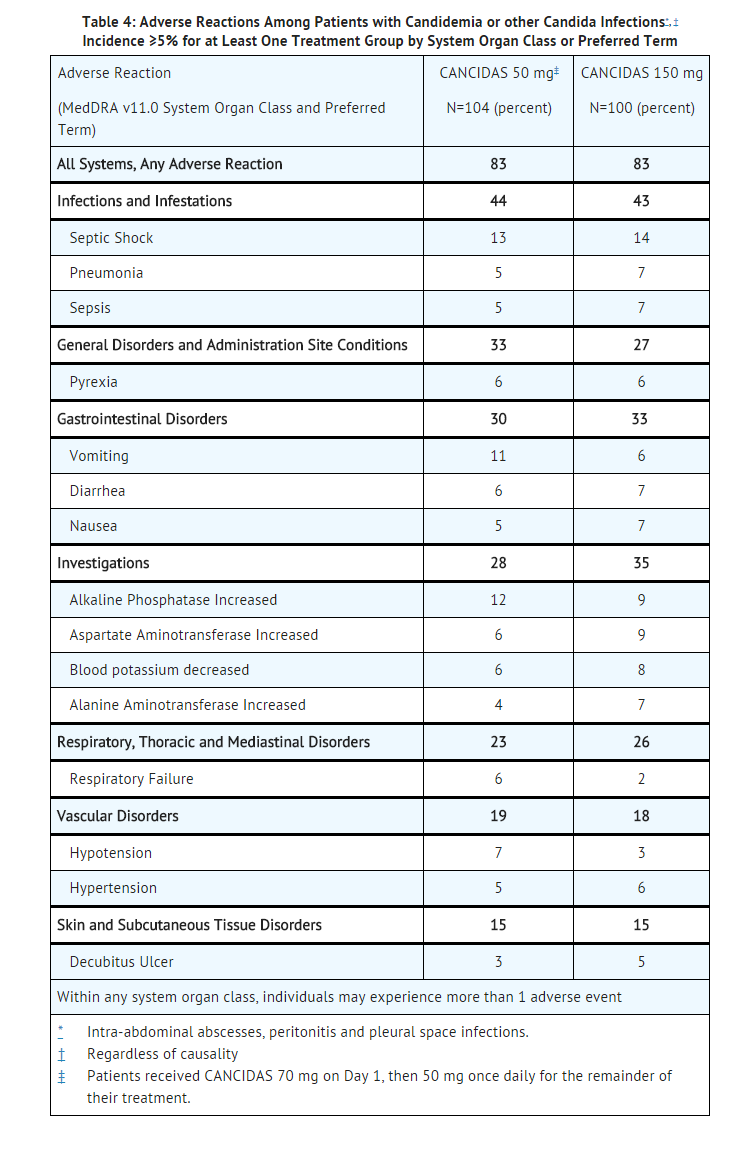
Esophageal Candidiasis and Oropharyngeal Candidiasis
Adverse reactions occurring in ≥10% of patients with esophageal and/or oropharyngeal candidiasis are presented in Table 5.
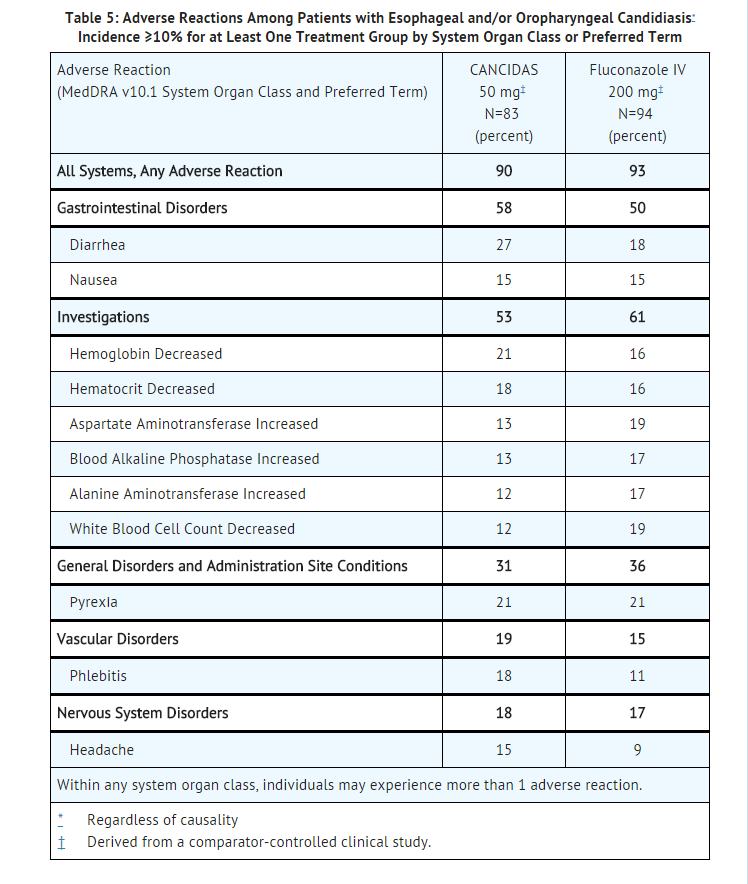
Invasive Aspergillosis
In an open-label, non comparative aspergillosis study, in which 69 patients received caspofungin (70-mg loading dose on Day 1 followed by 50 mg daily), the following treatment-emergent adverse reactions were observed with an incidence of ≥12.5%: blood alkaline phosphatase increased (22%), hypotension (20%), respiratory failure (20%), pyrexia (17%), diarrhea (15%), nausea (15%), headache (15%), rash (13%), aspergillosis (13%), alanine aminotransferase increased (13%), aspartate aminotransferase increased (13%), blood bilirubin increased (13%), and blood potassium decreased (13%). Also reported infrequently in this patient population were pulmonary edema, ARDS (adult respiratory distress syndrome), and radiographic infiltrates.
Clinical Trials Experience in Pediatric Patients (3 months to 17 years of age)
- The overall safety of caspofungin was assessed in 171 pediatric patients who received single or multiple doses of caspofungin. The distribution among the 153 pediatric patients who were over the age of 3 months was as follows: 104 febrile, neutropenic patients; 38 patients with candidemia and/or intra-abdominal abscesses, peritonitis, or pleural space infections; 1 patient with esophageal candidiasis; and 10 patients with invasive aspergillosis. The overall safety profile of caspofungin in pediatric patients is comparable to that in adult patients. Table 6 shows the incidence of adverse reactions reported in ≥7.5% of pediatric patients in clinical studies.
- One patient (0.6%) receiving caspofungin, and three patients (12%) receiving AmBisome developed a serious drug-related adverse reaction. Two patients (1%) were discontinued from caspofungin and three patients (12%) were discontinued from AmBisome due to a drug-related adverse reaction. The proportion of patients who experienced an infusion-related adverse reaction (defined as a systemic event, such as pyrexia, chills, flushing, hypotension, hypertension, tachycardia, dyspnea, tachypnea, rash, or anaphylaxis, that developed during the study therapy infusion and one hour following infusion) was 22% in the group treated with caspofungin and 35% in the group treated with AmBisome.
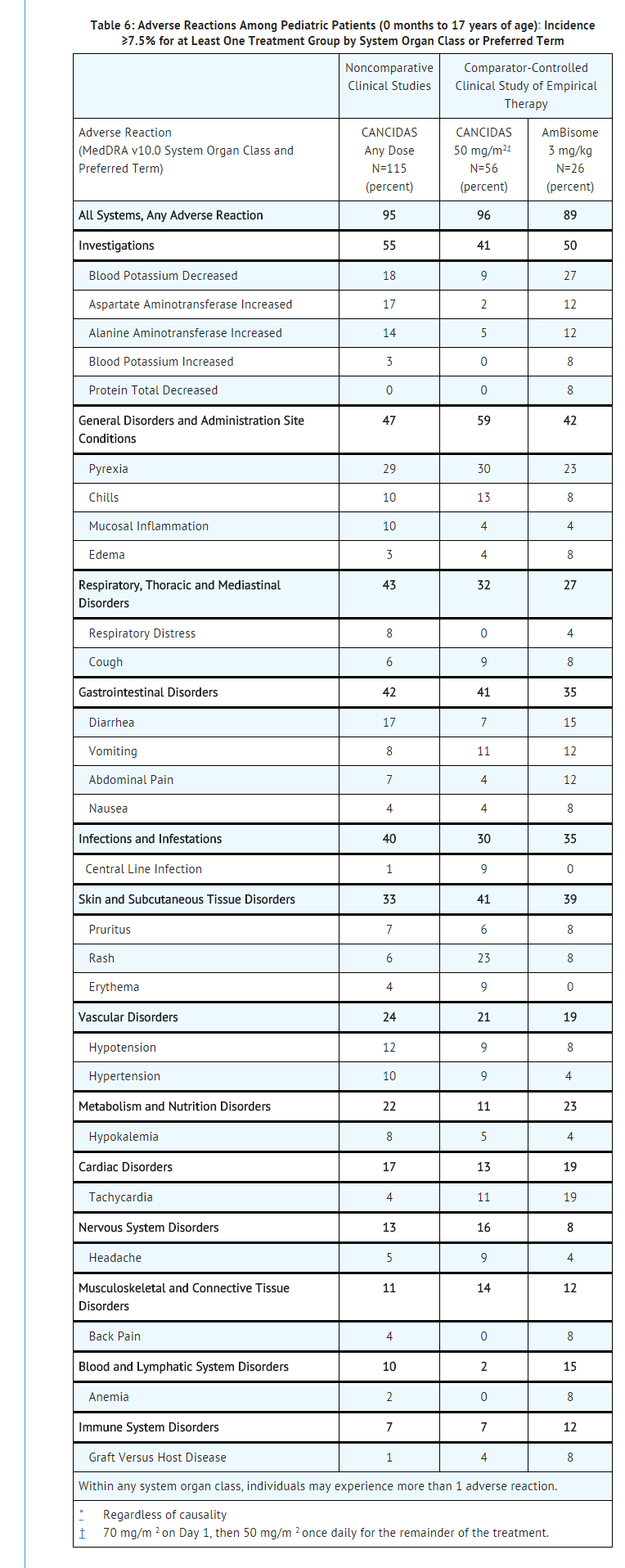
Overall Safety Experience of Caspofungin in Clinical Trials
- The overall safety of caspofungin was assessed in 2036 individuals (including 1642 adult or pediatric patients and 394 volunteers) from 34 clinical studies. These individuals received single or multiple (once daily) doses of caspofungin, ranging from 5 mg to 210 mg. Full safety data is available from 1951 individuals, as the safety data from 85 patients enrolled in 2 compassionate use studies was limited solely to serious adverse reactions. Treatment emergent adverse reactions, regardless of causality, which occurred in ≥5% of all individuals who received caspofungin in these trials, are shown in Table 7.
- Overall, 1665 of the 1951 (85%) patients/volunteers who received caspofungin experienced an adverse reaction.
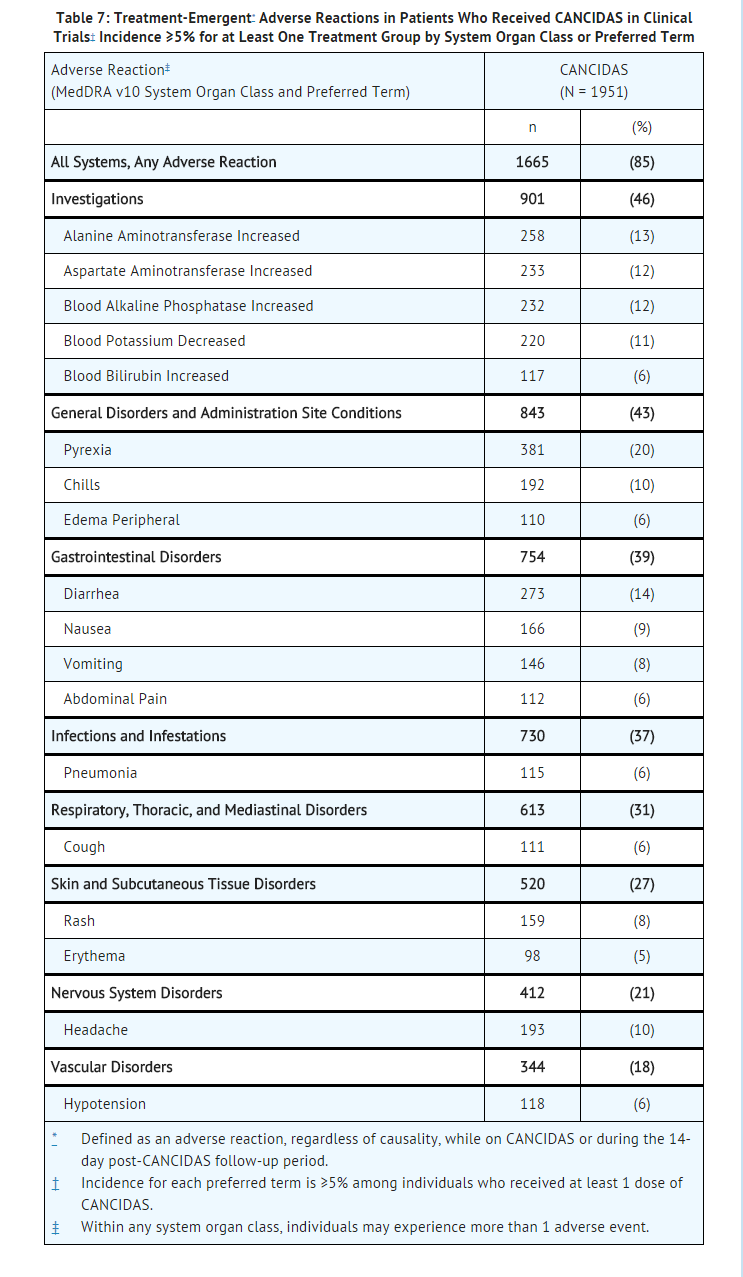
Clinically significant adverse reactions, regardless of causality or incidence which occurred in less than 5% of patients are listed below.
- Blood and lymphatic system disorders: anemia, coagulopathy, febrile neutropenia, neutropenia, thrombocytopenia
- Cardiac disorders: arrhythmia, atrial fibrillation, bradycardia, cardiac arrest, myocardial infarction, tachycardia
- Gastrointestinal disorders: abdominal distension, abdominal pain upper, constipation, dyspepsia
- General disorders and administration site conditions: asthenia, fatigue, infusion site pain/pruritus/swelling, mucosal inflammation, edema
- Hepatobiliary disorders: hepatic failure, hepatomegaly, hepatotoxicity, hyperbilirubinemia, jaundice
- Infections and infestations: bacteremia, sepsis, urinary tract infection
- Metabolic and nutrition disorders: anorexia, decreased appetite, fluid overload, hypomagnesemia, hypercalcemia, hyperglycemia, hypokalemia
- Musculoskeletal, connective tissue, and bone disorders: arthralgia, back pain, pain in extremity
- Nervous system disorders: convulsion, dizziness, somnolence, tremor
- Psychiatric disorders: anxiety, confusional state, depression, insomnia
- Renal and urinary disorders: hematuria, renal failure
- Respiratory, thoracic, and mediastinal disorders: dyspnea, epistaxis, hypoxia, tachypnea
- Skin and subcutaneous tissue disorders: erythema, petechiae, skin lesion, urticaria
- Vascular disorders: flushing, hypertension, phlebitis
Postmarketing Experience
The following additional adverse reactions have been identified during the post-approval use of caspofungin. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
- Gastrointestinal disorders: pancreatitis
- Hepatobiliary disorders: hepatic necrosis
- Skin and subcutaneous tissue disorders: erythema multiforme, Stevens-Johnson, skin exfoliation
- Renal and urinary disorders: clinically significant renal dysfunction
- General disorders and administration site conditions: swelling and peripheral edema
- Laboratory abnormalities: gamma-glutamyltransferase increased
Drug Interactions
- In clinical studies, caspofungin did not induce the CYP3A4 metabolism of other drugs. Caspofungin is not a substrate for P-glycoprotein and is a poor substrate for cytochrome P450 enzymes.
- Clinical studies in adult healthy volunteers show that the pharmacokinetics of caspofungin are not altered by itraconazole, amphotericin B, mycophenolate, nelfinavir, or tacrolimus. Caspofungin has no effect on the pharmacokinetics of itraconazole, amphotericin B, or the active metabolite of mycophenolate.
- Cyclosporine: In two adult clinical studies, cyclosporine (one 4 mg/kg dose or two 3 mg/kg doses) increased the AUC of caspofungin by approximately 35%. caspofungin did not increase the plasma levels of cyclosporine. There were transient increases in liver ALT and AST when caspofungin and cyclosporine were co-administered .
- Tacrolimus: For patients receiving caspofungin and tacrolimus, standard monitoring of tacrolimus blood concentrations and appropriate tacrolimus dosage adjustments are recommended.
- Rifampin: Adult patients on rifampin should receive 70 mg of caspofungin daily.
- Other inducers of drug clearance:
- Adults: When caspofungin is co-administered to adult patients with inducers of drug clearance, such as efavirenz, nevirapine, phenytoin, dexamethasone, or carbamazepine, use of a daily dose of 70 mg of caspofungin should be considered.
- Pediatric Patients: When caspofungin is co-administered to pediatric patients with inducers of drug clearance, such as rifampin, efavirenz, nevirapine, phenytoin, dexamethasone, or carbamazepine, a caspofungin dose of 70 mg/m2 daily (not to exceed an actual daily dose of 70 mg) should be considered.
Use in Specific Populations
Pregnancy
Pregnancy Category (FDA): Pregnancy Category C
- There are no adequate and well-controlled studies with the use of caspofungin in pregnant women. In animal studies, caspofungin caused embryofetal toxicity, including increased resorptions, increased peri-implantation loss, and incomplete ossification at multiple fetal sites. Caspofungin should be used during pregnancy only if the potential benefit justifies the potential risk to the fetus.
- In offspring born to pregnant rats treated with caspofungin at doses comparable to the human dose based on body surface area comparisons, there was incomplete ossification of the skull and torso and increased incidences of cervical rib. There was also an increase in resorptions and peri-implantation losses. In pregnant rabbits treated with caspofungin at doses comparable to 2 times the human dose based on body surface area comparisons, there was an increased incidence of incomplete ossification of the talus/calcaneus in offspring and increases in fetal resorptions. Caspofungin crossed the placenta in rats and rabbits and was detectable in fetal plasma.
Pregnancy Category (AUS):
There is no Australian Drug Evaluation Committee (ADEC) guidance on usage of Caspofungin in women who are pregnant.
Labor and Delivery
There is no FDA guidance on use of Caspofungin during labor and delivery.
Nursing Mothers
It is not known whether caspofungin is present in human milk. Caspofungin was found in the milk of lactating, drug-treated rats. Because many drugs are excreted in human milk, caution should be exercised when caspofungin is administered to a nursing woman.
Pediatric Use
- The safety and effectiveness of caspofungin in pediatric patients 3 months to 17 years of age are supported by evidence from adequate and well-controlled studies in adults, pharmacokinetic data in pediatric patients, and additional data from prospective studies in pediatric patients 3 months to 17 years of age for the following indications:
- Empirical therapy for presumed fungal infections in febrile, neutropenic patients.
- Treatment of candidemia and the following Candida infections: intra-abdominal abscesses, peritonitis, and pleural space infections.
- Treatment of esophageal candidiasis.
- Treatment of invasive aspergillosis in patients who are refractory to or intolerant of other therapies (e.g.,amphotericin B, lipid formulations of amphotericin B, itraconazole).
- The efficacy and safety of caspofungin has not been adequately studied in prospective clinical trials involving neonates and infants under 3 months of age. Although limited pharmacokinetic data were collected in neonates and infants below 3 months of age, these data are insufficient to establish a safe and effective dose of caspofungin in the treatment of neonatal candidiasis. Invasive candidiasis in neonates has a higher rate of CNS and multi-organ involvement than in older patients; the ability of caspofungin to penetrate the blood-brain barrier and to treat patients with meningitis and endocarditis is unknown.
- Caspofungin has not been studied in pediatric patients with endocarditis, osteomyelitis, and meningitis due to Candida. caspofungin has also not been studied as initial therapy for invasive aspergillosis in pediatric patients.
- In clinical trials, 171 pediatric patients (0 months to 17 years of age), including 18 patients who were less than 3 months of age, were given intravenous caspofungin. Pharmacokinetic studies enrolled a total of 66 pediatric patients, and an additional 105 pediatric patients received caspofungin in safety and efficacy studies. The majority of the pediatric patients received caspofungin at a once-daily maintenance dose of 50 mg/m2 for a mean duration of 12 days (median 9, range 1-87 days). In all studies, safety was assessed by the investigator throughout study therapy and for 14 days following cessation of study therapy. The most common adverse reactions in pediatric patients treated with caspofungin were pyrexia (29%), blood potassium decreased (15%), diarrhea (14%), increased aspartate aminotransferase (12%), rash (12%), increased alanine aminotransferase (11%), hypotension (11%), and chills (11%).
- Postmarketing hepatobiliary adverse reactions have been reported in pediatric patients with serious underlying medical conditions.
Geriatic Use
Clinical studies of caspofungin did not include sufficient numbers of patients aged 65 and over to determine whether they respond differently from younger patients. Although the number of elderly patients was not large enough for a statistical analysis, no overall differences in safety or efficacy were observed between these and younger patients. Plasma concentrations of caspofungin in healthy older men and women (≥65 years of age) were increased slightly (approximately 28% in AUC) compared to young healthy men. A similar effect of age on pharmacokinetics was seen in patients with candidemia or other Candida infections (intra-abdominal abscesses, peritonitis, or pleural space infections). No dose adjustment is recommended for the elderly; however, greater sensitivity of some older individuals cannot be ruled out.
Gender
There is no FDA guidance on the use of Caspofungin with respect to specific gender populations.
Race
There is no FDA guidance on the use of Caspofungin with respect to specific racial populations.
Renal Impairment
No dosage adjustment is necessary for patients with renal impairment. Caspofungin is not dialyzable; thus, supplementary dosing is not required following hemodialysis.
Hepatic Impairment
Adult patients with mild hepatic impairment (Child-Pugh score 5 to 6) do not need a dosage adjustment. For adult patients with moderate hepatic impairment (Child-Pugh score 7 to 9), caspofungin 35 mg once daily is recommended based upon pharmacokinetic data. However, where recommended, a 70-mg loading dose should still be administered on day 1. There is no clinical experience in adult patients with severe hepatic impairment (Child-Pugh score >9) and in pediatric patients 3 months to 17 years of age with any degree of hepatic impairment.
Females of Reproductive Potential and Males
There is no FDA guidance on the use of Caspofungin in women of reproductive potentials and males.
Immunocompromised Patients
There is no FDA guidance one the use of Caspofungin in patients who are immunocompromised.
Administration and Monitoring
Administration
Instructions for Use in All Patients
- Caspofungin should be administered by slow intravenous (IV) infusion over approximately 1 hour. Caspofungin should not be administered by IV bolus administration.
- Do not mix or co-infuse caspofungin with other medications, as there are no data available on the compatibility of caspofungin with other intravenous substances, additives, or medications. DO NOT USE DILUENTS CONTAINING DEXTROSE (α-D-GLUCOSE), as caspofungin is not stable in diluents containing dextrose.
Monitoring
There is limited information regarding Caspofungin Monitoring in the drug label.
IV Compatibility
There is limited information regarding the compatibility of Caspofungin and IV administrations.
Overdosage
- In 6 healthy subjects who received a single 210-mg dose, no significant adverse reactions were reported. Multiple doses above 150 mg daily have not been studied. Caspofungin is not dialyzable. The minimum lethal dose of caspofungin in rats was 50 mg/kg, a dose which is equivalent to 10 times the recommended daily dose based on relative body surface area comparison.
- In clinical trials, one pediatric patient (16 years of age) unintentionally received a single dose of caspofungin of 113 mg (on day 1), followed by 80 mg daily for an additional 7 days. No clinically significant adverse reactions were reported.
Pharmacology
Mechanism of Action
There is limited information regarding Caspofungin Mechanism of Action in the drug label.
Structure
- Caspofungin is a sterile, lyophilized product for intravenous (IV) infusion that contains a semisynthetic lipopeptide (echinocandin) compound synthesized from a fermentation product of Glarea lozoyensis. Caspofungin is an echinocandin that inhibits the synthesis of β (1,3)-D-glucan, an integral component of the fungal cell wall.
- CANCIDAS (caspofungin acetate) is 1-[(4R,5S)-5-[(2-aminoethyl)amino]-N2-(10,12-dimethyl-1-oxotetradecyl)-4-hydroxy-L-ornithine]-5-[(3R)-3-hydroxy-L-ornithine] pneumocandin B0 diacetate (salt). Caspofungin 50 mg also contains: 39 mg sucrose, 26 mg mannitol, glacial acetic acid, and sodium hydroxide. Caspofungin 70 mg also contains 54 mg sucrose, 36 mg mannitol, glacial acetic acid, and sodium hydroxide. Caspofungin acetate is a hygroscopic, white to off-white powder. It is freely soluble in water and methanol, and slightly soluble in ethanol. The pH of a saturated aqueous solution of caspofungin acetate is approximately 6.6. The empirical formula is C52H88N10O15•2C2H4O2 and the formula weight is 1213.42. The structural formula is:
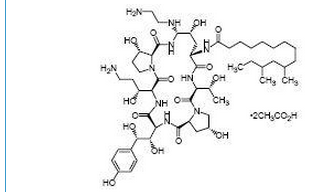
Pharmacodynamics
There is limited information regarding Caspofungin Pharmacodynamics in the drug label.
Pharmacokinetics
Adult and pediatric pharmacokinetic parameters are presented in Table 8.
Distribution
Plasma concentrations of caspofungin decline in a polyphasic manner following single 1-hour IV infusions. A short α-phase occurs immediately postinfusion, followed by a β-phase (half-life of 9 to 11 hours) that characterizes much of the profile and exhibits clear log-linear behavior from 6 to 48 hours postdose during which the plasma concentration decreases 10-fold. An additional, longer half-life phase, γ-phase, (half-life of 40-50 hours), also occurs. Distribution, rather than excretion or biotransformation, is the dominant mechanism influencing plasma clearance. Caspofungin is extensively bound to albumin (~97%), and distribution into red blood cells is minimal. Mass balance results showed that approximately 92% of the administered radioactivity was distributed to tissues by 36 to 48 hours after a single 70-mg dose of [3H] caspofungin acetate. There is little excretion or biotransformation of caspofungin during the first 30 hours after administration.
Metabolism
Caspofungin is slowly metabolized by hydrolysis and N-acetylation. Caspofungin also undergoes spontaneous chemical degradation to an open-ring peptide compound, L-747969. At later time points (≥5 days postdose), there is a low level (≤7 picomoles/mg protein, or ≤1.3% of administered dose) of covalent binding of radiolabel in plasma following single-dose administration of [3H] caspofungin acetate, which may be due to two reactive intermediates formed during the chemical degradation of caspofungin to L-747969. Additional metabolism involves hydrolysis into constitutive amino acids and their degradates, including dihydroxyhomotyrosine and N-acetyl-dihydroxyhomotyrosine. These two tyrosine derivatives are found only in urine, suggesting rapid clearance of these derivatives by the kidneys.
Excretion
Two single-dose radiolabeled pharmacokinetic studies were conducted. In one study, plasma, urine, and feces were collected over 27 days, and in the second study plasma was collected over 6 months. Plasma concentrations of radioactivity and of caspofungin were similar during the first 24 to 48 hours postdose; thereafter drug levels fell more rapidly. In plasma, caspofungin concentrations fell below the limit of quantitation after 6 to 8 days postdose, while radiolabel fell below the limit of quantitation at 22.3 weeks postdose. After single intravenous administration of [3H] caspofungin acetate, excretion of caspofungin and its metabolites in humans was 35% of dose in feces and 41% of dose in urine. A small amount of caspofungin is excreted unchanged in urine (~1.4% of dose). Renal clearance of parent drug is low (~0.15 mL/min) and total clearance of caspofungin is 12 mL/min.
Special Populations
Renal Impairment
In a clinical study of single 70-mg doses, caspofungin pharmacokinetics were similar in healthy adult volunteers with mild renal impairment (creatinine clearance 50 to 80 mL/min) and control subjects. Moderate (creatinine clearance 31 to 49 mL/min), severe (creatinine clearance 5 to 30 mL/min), and end-stage (creatinine clearance <10 mL/min and dialysis dependent) renal impairment moderately increased caspofungin plasma concentrations after single-dose administration (range: 30 to 49% for AUC). However, in adult patients with invasive aspergillosis, candidemia, or other Candida infections (intra-abdominal abscesses, peritonitis, or pleural space infections) who received multiple daily doses of caspofungin 50 mg, there was no significant effect of mild to end-stage renal impairment on caspofungin concentrations. No dosage adjustment is necessary for patients with renal impairment. Caspofungin is not dialyzable, thus supplementary dosing is not required following hemodialysis.
Hepatic Impairment
Plasma concentrations of caspofungin after a single 70-mg dose in adult patients with mild hepatic impairment (Child-Pugh score 5 to 6) were increased by approximately 55% in AUC compared to healthy control subjects. In a 14-day multiple-dose study (70 mg on Day 1 followed by 50 mg daily thereafter), plasma concentrations in adult patients with mild hepatic impairment were increased modestly (19 to 25% in AUC) on Days 7 and 14 relative to healthy control subjects. No dosage adjustment is recommended for patients with mild hepatic impairment.
Adult patients with moderate hepatic impairment (Child-Pugh score 7 to 9) who received a single 70-mg dose of caspofungin had an average plasma caspofungin increase of 76% in AUC compared to control subjects. A dosage reduction is recommended for adult patients with moderate hepatic impairment based upon these pharmacokinetic data.
There is no clinical experience in adult patients with severe hepatic impairment (Child-Pugh score >9) or in pediatric patients with any degree of hepatic impairment.
Gender
Plasma concentrations of caspofungin in healthy adult men and women were similar following a single 70-mg dose. After 13 daily 50-mg doses, caspofungin plasma concentrations in women were elevated slightly (approximately 22% in area under the curve [AUC]) relative to men. No dosage adjustment is necessary based on gender.
Race
Regression analyses of patient pharmacokinetic data indicated that no clinically significant differences in the pharmacokinetics of caspofungin were seen among Caucasians, Blacks, and Hispanics. No dosage adjustment is necessary on the basis of race.
Geriatric Patients
Plasma concentrations of caspofungin in healthy older men and women (≥65 years of age) were increased slightly (approximately 28% AUC) compared to young healthy men after a single 70-mg dose of caspofungin. In patients who were treated empirically or who had candidemia or other Candida infections (intra-abdominal abscesses, peritonitis, or pleural space infections), a similar modest effect of age was seen in older patients relative to younger patients. No dosage adjustment is necessary for the elderly.
Pediatric Patients
Caspofungin has been studied in five prospective studies involving pediatric patients under 18 years of age, including three pediatric pharmacokinetic studies [initial study in adolescents (12-17 years of age) and children (2-11 years of age) followed by a study in younger patients (3-23 months of age) and then followed by a study in neonates and infants (<3 months)].
Pharmacokinetic parameters following multiple doses of caspofungin in pediatric and adult patients are presented in Table 8
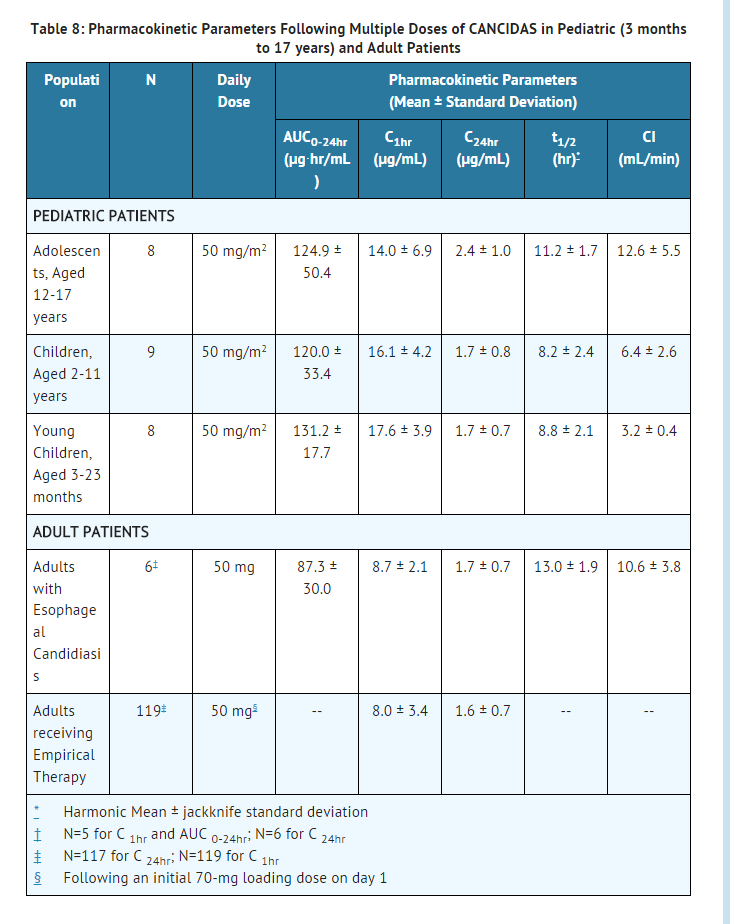
Studies in vitro show that caspofungin acetate is not an inhibitor of any enzyme in the cytochrome P450 (CYP) system. In clinical studies, caspofungin did not induce the CYP3A4 metabolism of other drugs. Caspofungin is not a substrate for P-glycoprotein and is a poor substrate for cytochrome P450 enzymes.
Clinical studies in adult healthy volunteers show that the pharmacokinetics of caspofungin are not altered by itraconazole, amphotericin B, mycophenolate, nelfinavir, or tacrolimus. Caspofungin has no effect on the pharmacokinetics of itraconazole, amphotericin B, or the active metabolite of mycophenolate.
Cyclosporine: In two adult clinical studies, cyclosporine (one 4 mg/kg dose or two 3 mg/kg doses) increased the AUC of caspofungin by approximately 35%. Caspofungin did not increase the plasma levels of cyclosporine. There were transient increases in liver ALT and AST when caspofungin and cyclosporine were co-administered.
Tacrolimus: caspofungin reduced the blood AUC0-12 of tacrolimus (FK-506, Prograf®) by approximately 20%, peak blood concentration (Cmax) by 16%, and 12-hour blood concentration (C12hr) by 26% in healthy adult subjects when tacrolimus (2 doses of 0.1 mg/kg 12 hours apart) was administered on the 10th day of caspofungin 70 mg daily, as compared to results from a control period in which tacrolimus was administered alone. For patients receiving both therapies, standard monitoring of tacrolimus blood concentrations and appropriate tacrolimus dosage adjustments are recommended.
Rifampin: A drug-drug interaction study with rifampin in adult healthy volunteers has shown a 30% decrease in caspofungin trough concentrations. Adult patients on rifampin should receive 70 mg of caspofungin daily.
Other inducers of drug clearance
Adults: In addition, results from regression analyses of adult patient pharmacokinetic data suggest that co-administration of other inducers of drug clearance (efavirenz, nevirapine, phenytoin, dexamethasone, or carbamazepine) with caspofungin may result in clinically meaningful reductions in caspofungin concentrations. It is not known which drug clearance mechanism involved in caspofungin disposition may be inducible. When caspofungin is co-administered to adult patients with inducers of drug clearance, such as efavirenz, nevirapine, phenytoin, dexamethasone, or carbamazepine, use of a daily dose of 70 mg of caspofungin should be considered.
Pediatric patients: In pediatric patients, results from regression analyses of pharmacokinetic data suggest that co-administration of dexamethasone with caspofungin may result in clinically meaningful reductions in caspofungin trough concentrations. This finding may indicate that pediatric patients will have similar reductions with inducers as seen in adults. When caspofungin is co-administered to pediatric patients with inducers of drug clearance, such as rifampin, efavirenz, nevirapine, phenytoin, dexamethasone, or carbamazepine, a caspofungin dose of 70 mg/m2 daily (not to exceed an actual daily dose of 70 mg) should be considered.
Nonclinical Toxicology
Carcinogenesis, Mutagenesis, Impairment of Fertility
- No long-term studies in animals have been performed to evaluate the carcinogenic potential of caspofungin.
- Caspofungin did not show evidence of mutagenic or genotoxic potential when evaluated in the following in vitro assays: bacterial (Ames) and mammalian cell (V79 Chinese hamster lung fibroblasts) mutagenesis assays, the alkaline elution/rat hepatocyte DNA strand break test, and the chromosome aberration assay in Chinese hamster ovary cells. Caspofungin was not genotoxic when assessed in the mouse bone marrow chromosomal test at doses up to 12.5 mg/kg (equivalent to a human dose of 1 mg/kg based on body surface area comparisons), administered intravenously.
- Fertility and reproductive performance were not affected by the intravenous administration of caspofungin to rats at doses up to 5 mg/kg. At 5 mg/kg exposures were similar to those seen in patients treated with the 70-mg dose.
Animal Toxicology and/or Pharmacology
- In one 5-week study in monkeys at doses which produced exposures approximately 4 to 6 times those seen in adult patients treated with a 70-mg dose, scattered small foci of subcapsular necrosis were observed microscopically in the livers of some animals (2/8 monkeys at 5 mg/kg and 4/8 monkeys at 8 mg/kg); however, this histopathological finding was not seen in another study of 27 weeks duration at similar doses.
- No treatment-related findings were seen in a 5-week study in infant monkeys at doses which produced exposures approximately 3 times those achieved in pediatric patients receiving a maintenance dose of 50 mg/m2 daily.
Clinical Studies
Empirical Therapy in Febrile, Neutropenic Patients
- A double-blind study enrolled 1111 febrile, neutropenic (<500 cells/mm3) patients who were randomized to treatment with daily doses of caspofungin (50 mg/day following a 70-mg loading dose on Day 1) or AmBisome (3 mg/kg/day). Patients were stratified based on risk category (high-risk patients had undergone allogeneic stem cell transplantation or had relapsed acute leukemia) and on receipt of prior antifungal prophylaxis. Twenty-four percent of patients were high risk and 56% had received prior antifungal prophylaxis. Patients who remained febrile or clinically deteriorated following 5 days of therapy could receive 70 mg/day of caspofungin or 5 mg/kg/day of AmBisome. Treatment was continued to resolution of neutropenia (but not beyond 28 days unless a fungal infection was documented).
- An overall favorable response required meeting each of the following criteria: no documented breakthrough fungal infections up to 7 days after completion of treatment, survival for 7 days after completion of study therapy, no discontinuation of the study drug because of drug-related toxicity or lack of efficacy, resolution of fever during the period of neutropenia, and successful treatment of any documented baseline fungal infection.
- Based on the composite response rates, caspofungin was as effective as AmBisome in empirical therapy of persistent febrile neutropenia (see Table 11)
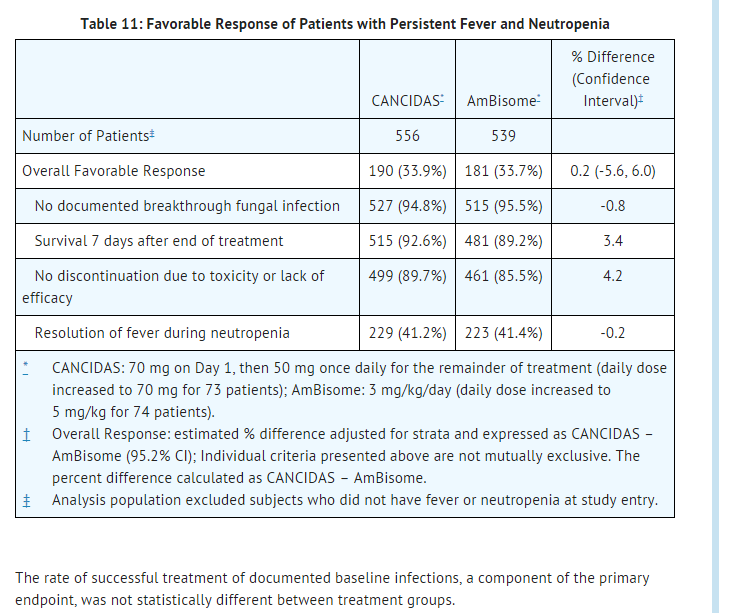
- The rate of successful treatment of documented baseline infections, a component of the primary endpoint, was not statistically different between treatment groups.
- The response rates did not differ between treatment groups based on either of the stratification variables: risk category or prior antifungal prophylaxis.
Candidemia and the Following other Candida Infections: Intra-Abdominal Abscesses, Peritonitis and Pleural Space Infections
- In a randomized, double-blind study, patients with a proven diagnosis of invasive candidiasis received daily doses of caspofungin (50 mg/day following a 70-mg loading dose on Day 1) or amphotericin B deoxycholate (0.6 to 0.7 mg/kg/day for non-neutropenic patients and 0.7 to 1 mg/kg/day for neutropenic patients). Patients were stratified by both neutropenic status and APACHE II score. Patients with Candida endocarditis, meningitis, or osteomyelitis were excluded from this study.
- Patients who met the entry criteria and received one or more doses of IV study therapy were included in the modified intention-to-treat [MITT] analysis of response at the end of IV study therapy. A favorable response at this time point required both symptom/sign resolution/improvement and microbiological clearance of the Candida infection.
- Two hundred thirty-nine patients were enrolled. Patient disposition is shown in Table 12.
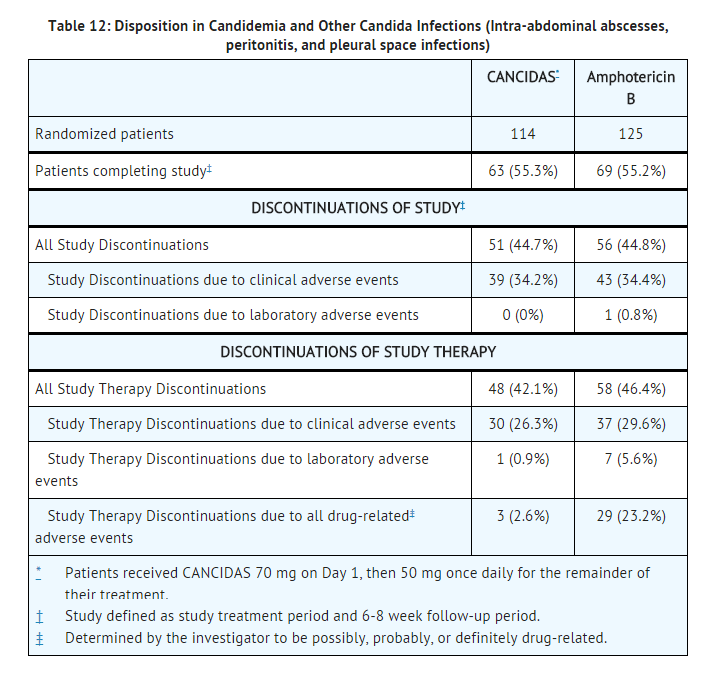
- Of the 239 patients enrolled, 224 met the criteria for inclusion in the MITT population (109 treated with caspofungin and 115 treated with amphotericin B). Of these 224 patients, 186 patients had candidemia (92 treated with caspofungin and 94 treated with amphotericin B). The majority of the patients with candidemia were non-neutropenic (87%) and had an APACHE II score less than or equal to 20 (77%) in both arms. Most candidemia infections were caused by C. albicans (39%), followed by C. parapsilosis (20%), C. tropicalis (17%), C. glabrata (8%), and C. krusei (3%).
- At the end of IV study therapy, caspofungin was comparable to amphotericin B in the treatment of candidemia in the MITT population. For the other efficacy time points (Day 10 of IV study therapy, end of all antifungal therapy, 2-week post-therapy follow-up, and 6- to 8-week post-therapy follow-up), caspofungin was as effective as amphotericin B.
- Outcome, relapse and mortality data are shown in Table 13.

- In this study, the efficacy of caspofungin in patients with intra-abdominal abscesses, peritonitis and pleural space Candida infections was evaluated in 19 non-neutropenic patients. Two of these patients had concurrent candidemia. Candida was part of a polymicrobial infection that required adjunctive surgical drainage in 11 of these 19 patients. A favorable response was seen in 9 of 9 patients with peritonitis, 3 of 4 with abscesses (liver, parasplenic, and urinary bladder abscesses), 2 of 2 with pleural space infections, 1 of 2 with mixed peritoneal and pleural infection, 1 of 1 with mixed abdominal abscess and peritonitis, and 0 of 1 with Candida pneumonia.
- Overall, across all sites of infection included in the study, the efficacy of caspofungin was comparable to that of amphotericin B for the primary endpoint.
- In this study, the efficacy data for caspofungin in neutropenic patients with candidemia were limited. In a separate compassionate use study, 4 patients with hepatosplenic candidiasis received prolonged therapy with caspofungin following other long-term antifungal therapy; three of these patients had a favorable response.
- In a second randomized, double-blind study, 197 patients with proven invasive candidiasis received caspofungin 50 mg/day (following a 70-mg loading dose on Day 1) or caspofungin 150 mg/day. The diagnostic criteria, evaluation time points, and efficacy endpoints were similar to those employed in the prior study. Patients with Candida endocarditis, meningitis, or osteomyelitis were excluded. Although this study was designed to compare the safety of the two doses, it was not large enough to detect differences in rare or unexpected adverse events. A significant improvement in efficacy with the 150-mg daily dose was not seen when compared to the 50-mg dose.
Esophageal Candidiasis (and information on oropharyngeal candidiasis)
- The safety and efficacy of caspofungin in the treatment of esophageal candidiasis was evaluated in one large, controlled, noninferiority, clinical trial and two smaller dose-response studies.
- In all 3 studies, patients were required to have symptoms and microbiological documentation of esophageal candidiasis; most patients had advanced AIDS (with CD4 counts <50/mm3).
- Of the 166 patients in the large study who had culture-confirmed esophageal candidiasis at baseline, 120 had Candida albicans and 2 had Candida tropicalis as the sole baseline pathogen whereas 44 had mixed baseline cultures containing C. albicans and one or more additional Candida species.
- In the large, randomized, double-blind study comparing caspofungin 50 mg/day versus intravenous fluconazole 200 mg/day for the treatment of esophageal candidiasis, patients were treated for an average of 9 days (range 7-21 days). Favorable overall response at 5 to 7 days following discontinuation of study therapy required both complete resolution of symptoms and significant endoscopic improvement. The definition of endoscopic response was based on severity of disease at baseline using a 4-grade scale and required at least a two-grade reduction from baseline endoscopic score or reduction to grade 0 for patients with a baseline score of 2 or less.
- The proportion of patients with a favorable overall response was comparable for caspofungin and fluconazole as shown in Table 14.
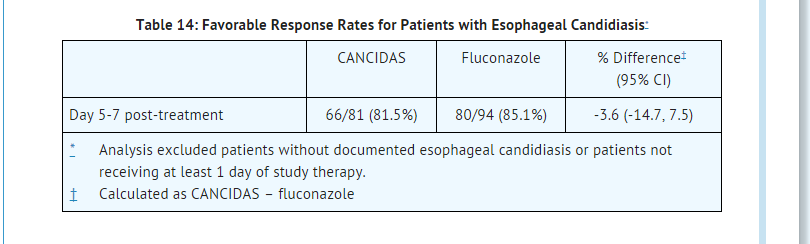
- The proportion of patients with a favorable symptom response was also comparable (90.1% and 89.4% for caspofungin and fluconazole, respectively). In addition, the proportion of patients with a favorable endoscopic response was comparable (85.2% and 86.2% for caspofungin and fluconazole, respectively).
- As shown in Table 15, the esophageal candidiasis relapse rates at the Day 14 post-treatment visit were similar for the two groups. At the Day 28 post-treatment visit, the group treated with caspofungin had a numerically higher incidence of relapse; however, the difference was not statistically significant.
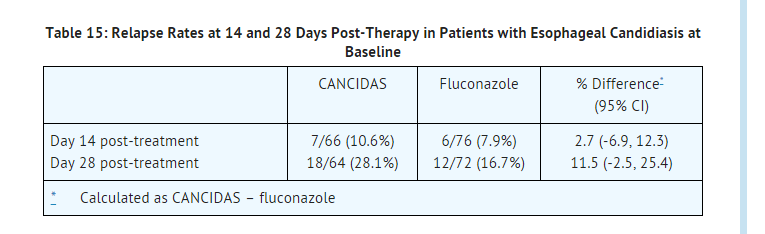
- In this trial, which was designed to establish non inferiority of caspofungin to fluconazole for the treatment of esophageal candidiasis, 122 (70%) patients also had oropharyngeal candidiasis. A favorable response was defined as complete resolution of all symptoms of oropharyngeal disease and all visible oropharyngeal lesions. The proportion of patients with a favorable oropharyngeal response at the 5- to 7-day post-treatment visit was numerically lower for caspofungin; however, the difference was not statistically significant. Oropharyngeal candidiasis relapse rates at day 14 and day 28 post-treatment visits were statistically significantly higher for caspofungin than for fluconazole. The results are shown in Table 16.
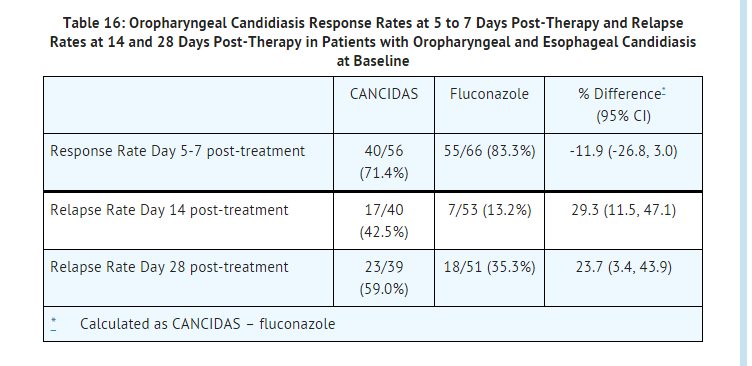
- The results from the two smaller dose-ranging studies corroborate the efficacy of caspofungin for esophageal candidiasis that was demonstrated in the larger study.
- Caspofungin was associated with favorable outcomes in 7 of 10 esophageal C. albicans infections refractory to at least 200 mg of fluconazole given for 7 days, although the in vitro susceptibility of the infecting isolates to fluconazole was not known.
Invasive Aspergillosis
- Sixty-nine patients between the ages of 18 and 80 with invasive aspergillosis were enrolled in an open-label, noncomparative study to evaluate the safety, tolerability, and efficacy of caspofungin. Enrolled patients had previously been refractory to or intolerant of other antifungal therapy(ies). Refractory patients were classified as those who had disease progression or failed to improve despite therapy for at least 7 days with amphotericin B, lipid formulations of amphotericin B, itraconazole, or an investigational azole with reported activity against Aspergillus. Intolerance to previous therapy was defined as a doubling of creatinine (or creatinine ≥2.5 mg/dL while on therapy), other acute reactions, or infusion-related toxicity. To be included in the study, patients with pulmonary disease must have had definite (positive tissue histopathology or positive culture from tissue obtained by an invasive procedure) or probable (positive radiographic or computed tomography evidence with supporting culture from bronchoalveolar lavage or sputum, galactomannan enzyme-linked immunosorbent assay, and/or polymerase chain reaction) invasive aspergillosis. Patients with extrapulmonary disease had to have definite invasive aspergillosis. The definitions were modeled after the Mycoses Study Group Criteria. Patients were administered a single 70-mg loading dose of caspofungin and subsequently dosed with 50 mg daily. The mean duration of therapy was 33.7 days, with a range of 1 to 162 days.
- An independent expert panel evaluated patient data, including diagnosis of invasive aspergillosis, response and tolerability to previous antifungal therapy, treatment course on caspofungin, and clinical outcome.
- A favorable response was defined as either complete resolution (complete response) or clinically meaningful improvement (partial response) of all signs and symptoms and attributable radiographic findings. Stable, non progressive disease was considered to be an unfavorable response.
- Among the 69 patients enrolled in the study, 63 met entry diagnostic criteria and had outcome data; and of these, 52 patients received treatment for >7 days. Fifty-three (84%) were refractory to previous antifungal therapy and 10 (16%) were intolerant. Forty-five patients had pulmonary disease and 18 had extrapulmonary disease. Underlying conditions were hematologic malignancy (N=24), allogeneic bone marrow transplant or stem cell transplant (N=18), organ transplant (N=8), solid tumor (N=3), or other conditions (N=10). All patients in the study received concomitant therapies for their other underlying conditions. Eighteen patients received tacrolimus and caspofungin concomitantly, of whom 8 also received mycophenolate mofetil.
- Overall, the expert panel determined that 41% (26/63) of patients receiving at least one dose of caspofungin had a favorable response. For those patients who received >7 days of therapy with caspofungin, 50% (26/52) had a favorable response. The favorable response rates for patients who were either refractory to or intolerant of previous therapies were 36% (19/53) and 70% (7/10), respectively. The response rates among patients with pulmonary disease and extrapulmonary disease were 47% (21/45) and 28% (5/18), respectively. Among patients with extrapulmonary disease, 2 of 8 patients who also had definite, probable, or possible CNS involvement had a favorable response. Two of these 8 patients had progression of disease and manifested CNS involvement while on therapy.
- Caspofungin is effective for the treatment of invasive aspergillosis in patients who are refractory to or intolerant of itraconazole, amphotericin B, and/or lipid formulations of amphotericin B. However, the efficacy of caspofungin for initial treatment of invasive aspergillosis has not been evaluated in comparator-controlled clinical studies
Pediatric Patients
- The safety and efficacy of caspofungin were evaluated in pediatric patients 3 months to 17 years of age in two prospective, multicenter clinical trials.
- The first study, which enrolled 82 patients between 2 to 17 years of age, was a randomized, double-blind study comparing caspofungin (50 mg/m2 IV once daily following a 70-mg/m2 loading dose on Day 1 [not to exceed 70 mg daily]) to AmBisome (3 mg/kg IV daily) in a 2:1 treatment fashion (56 on caspofungin, 26 on AmBisome) as empirical therapy in pediatric patients with persistent fever and neutropenia. The study design and criteria for efficacy assessment were similar to the study in adult patients. Patients were stratified based on risk category (high-risk patients had undergone allogeneic stem cell transplantation or had relapsed acute leukemia). Twenty-seven percent of patients in both treatment groups were high risk. Favorable overall response rates of pediatric patients with persistent fever and neutropenia are presented in Table 17.
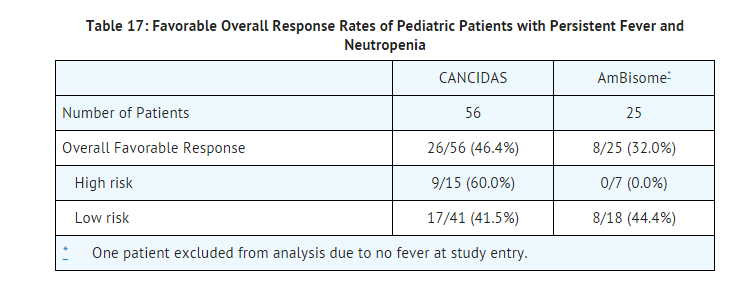
- The second study was a prospective, open-label, non-comparative study estimating the safety and efficacy of caspofungin in pediatric patients (ages 3 months to 17 years) with candidemia and other Candida infections, esophageal candidiasis, and invasive aspergillosis (as salvage therapy). The study employed diagnostic criteria which were based on established EORTC/MSG criteria of proven or probable infection; these criteria were similar to those criteria employed in the adult studies for these various indications. Similarly, the efficacy time points and endpoints used in this study were similar to those employed in the corresponding adult studies. All patients received caspofungin at 50 mg/m2 IV once daily following a 70-mg/m2 loading dose on Day 1 (not to exceed 70 mg daily). Among the 49 enrolled patients who received caspofungin, 48 were included in the efficacy analysis (one patient excluded due to not having a baseline Aspergillus or Candida infection). Of these 48 patients, 37 had candidemia or other Candida infections, 10 had invasive aspergillosis, and 1 patient had esophageal candidiasis. Most candidemia and other Candida infections were caused by C. albicans (35%), followed by C. parapsilosis (22%), C. tropicalis (14%), and C. glabrata (11%). The favorable response rate, by indication, at the end of caspofungin therapy was as follows: 30/37 (81%) in candidemia or other Candida infections, 5/10 (50%) in invasive aspergillosis, and 1/1 in esophageal candidiasis.
How Supplied
- Caspofungin 50 mg is a white to off-white powder/cake for infusion in a vial with a red aluminum band and a plastic cap.
- NDC 0006-3822-10 supplied as one single-use vial.
- Caspofungin 70 mg is a white to off-white powder/cake for infusion in a vial with a yellow/orange aluminum band and a plastic cap.
- NDC 0006-3823-10 supplied as one single-use vial.
Storage
Vials
The lyophilized vials should be stored refrigerated at 2° to 8°C (36° to 46°F).
Reconstituted Concentrate
Reconstituted caspofungin in the vial may be stored at ≤25°C (≤77°F) for one hour prior to the preparation of the patient infusion solution.
Diluted Product
The final patient infusion solution in the IV bag or bottle can be stored at ≤25°C (≤77°F) for 24 hours or at 2 to 8°C (36 to 46°F) for 48 hours.
Images
Drug Images
{{#ask: Page Name::Caspofungin |?Pill Name |?Drug Name |?Pill Ingred |?Pill Imprint |?Pill Dosage |?Pill Color |?Pill Shape |?Pill Size (mm) |?Pill Scoring |?NDC |?Drug Author |format=template |template=DrugPageImages |mainlabel=- |sort=Pill Name }}
Package and Label Display Panel
{{#ask: Label Page::Caspofungin |?Label Name |format=template |template=DrugLabelImages |mainlabel=- |sort=Label Page }}
Patient Counseling Information
Hypersensitivity
Inform patients that anaphylactic reactions have been reported during administration of caspofungin. Caspofungin can cause hypersensitivity reactions, including rash, facial swelling, angioedema, pruritus, sensation of warmth, or bronchospasm. Inform patients to report these signs or symptoms to their healthcare providers.
Hepatic Effects
- Inform patients that there have been isolated reports of serious hepatic effects from caspofungin therapy. Physicians will assess the risk/benefit of continuing caspofungin therapy if abnormal liver function tests occur during treatment.
Precautions with Alcohol
Alcohol-Caspofungin interaction has not been established. Talk to your doctor about the effects of taking alcohol with this medication.
Brand Names
CANCIDA
Look-Alike Drug Names
There is limited information regarding Caspofungin Look-Alike Drug Names in the drug label.
Price
References
The contents of this FDA label are provided by the National Library of Medicine.
{{#subobject:
|Label Page=Caspofungin |Label Name=
}}
{{#subobject:
|Label Page=Caspofungin |Label Name=Caspofungin ingredients and appearance.png
}}
{{#subobject:
|Label Page=Caspofungin |Label Name=Caspofungin fig02.jpg
}}