Breast pump
|
WikiDoc Resources for Breast pump |
|
Articles |
|---|
|
Most recent articles on Breast pump Most cited articles on Breast pump |
|
Media |
|
Powerpoint slides on Breast pump |
|
Evidence Based Medicine |
|
Clinical Trials |
|
Ongoing Trials on Breast pump at Clinical Trials.gov Clinical Trials on Breast pump at Google
|
|
Guidelines / Policies / Govt |
|
US National Guidelines Clearinghouse on Breast pump
|
|
Books |
|
News |
|
Commentary |
|
Definitions |
|
Patient Resources / Community |
|
Patient resources on Breast pump Discussion groups on Breast pump Patient Handouts on Breast pump Directions to Hospitals Treating Breast pump Risk calculators and risk factors for Breast pump
|
|
Healthcare Provider Resources |
|
Causes & Risk Factors for Breast pump |
|
Continuing Medical Education (CME) |
|
International |
|
|
|
Business |
|
Experimental / Informatics |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1] Associate Editor(s)-in-Chief: Tarek Nafee, M.D. [2]
Overview
A breast pump is a mechanical device (powered manually or by electricity) that extracts milk from the breasts of a woman who is lactating. The breast pump was invented and patented by Edward Lasker. Mechanically, a breast pump is directly analogous to a milking machine used in commercial dairy production. A misconception is that the breast pump suctions milk out of the breast. A breast pump's job is to trigger the milk-ejection response or let-down. Most pumps achieve this goal by using suction to pull the nipple into the tunnel of the breast shield or flange then release, which counts as one cycle. Thirty to sixty cycles per minute can be expected with better quality electric breast pumps. It is important to note that in most cases the breast pump is not as efficient at removing milk from the breast as the nursing baby.
The expressed breast milk (EBM) may be stored and later fed to a baby by bottle. Expressed milk may be kept at room temperature for up to ten hours (at 66-72 degrees Fahrenheit, around 20 degrees Celsius), refrigerated for up to 8 days, or frozen for six months in a deep freeze separate from a refrigerator maintained at a temperature of 0 degrees Fahrenheit or −18 degrees Celsius. Expressed milk may be donated to milk banks, which provide human breast milk to premature infants and other high-risk children whose mothers cannot provide for them.
Women use breast pumps for many reasons. Many women use breast pumps to continue breastfeeding after they return to work. They use the pump to express breast milk which is later bottle fed to their child by a caregiver. A breast pump may also be used to stimulate lactation for women with a low milk supply, or who have not just given birth. A breast pump may be used to relieve engorgement, a painful condition whereby the breasts are overfull, possibly preventing a proper latch by the infant. If an infant does not latch properly for direct breastfeeding, and the mother still desires the benefits of breast milk, she may choose to pump exclusively. If the mother needs to take medication that affects the breast milk and may be harmful to the infant, the mother may "pump and dump" the breast milk to keep up her milk supply during the time period that she is on the medication and may resume nursing after the course of medication is completed. Finally, pumping may be desirable to continue lactation and its associated hormonal benefits to aid in recovery from pregnancy even if the pumped milk is not used. [1]
Types of Breast Pumps
Manual breast pumps are operated by squeezing a handle in a repetitive fashion, allowing the user to directly control the pressure and frequency of pumps. Though manual pumps are small and inexpensive, they can require significant effort and can be tiring because the user provides all the power. This style is recommended for infrequent usage such as when a woman is away from her baby for a single feeding. It is recommended that "bicycle horn" style manual pumps not be used. Though cheap, they can damage breast tissue and harbor bacteria in the rubber suction bulb, which is difficult to clean.[2]
 |
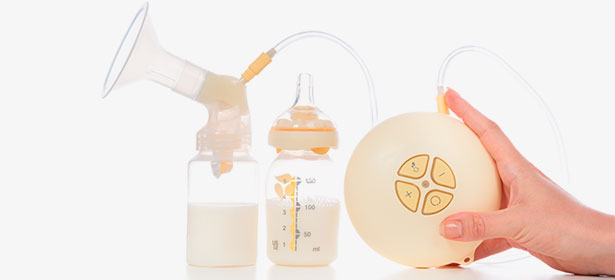
Personal electric pumps are powered by a small motor which supplies suction through plastic tubing to a breast shield (or flange) that fits over the nipple. The portions of the pump that come into direct contact with the expressed milk must be sterilized to prevent contamination. This style provides a lot more suction, making pumping significantly faster, and allows pumping of both breasts at the same time. Electric breast pumps are ideal for when a mother will be pumping daily or more than once daily. Electric breast pumps are larger than manual ones, but portable models are available (e.g. in a backpack or shoulder bag) that allow the mother to transport the pump.
Personal electric breast pumps may have different power supplies including:
- AC Adapter
- Batteries
- Portable charging adapters
- Rechargeable pumps
 |
 |
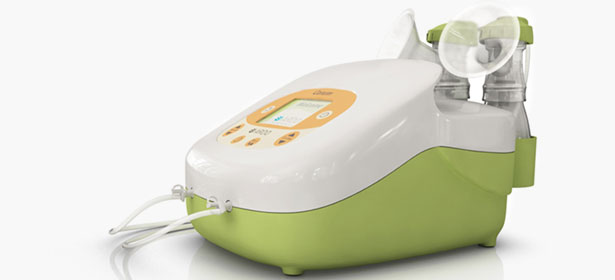
Hospital-grade electric pumps have larger motors which provide more suction. They are relatively silent and provide more efficient, quicker expression of breast milk. Hospital-grade breast pumps are FDA-approved for multiple users as long as the collection system is changed between users. They are often used at hospitals for milk donations or for mothers who have trouble breast feeding (due to trouble latching or painful engorgement). Hospital-grade electric pumps are generally rented for personal use due to the high cost, however, they may be a good purchase option for mothers who can afford them and either have a need for them or prefer them for the convenience and speed of milk expression.
 |
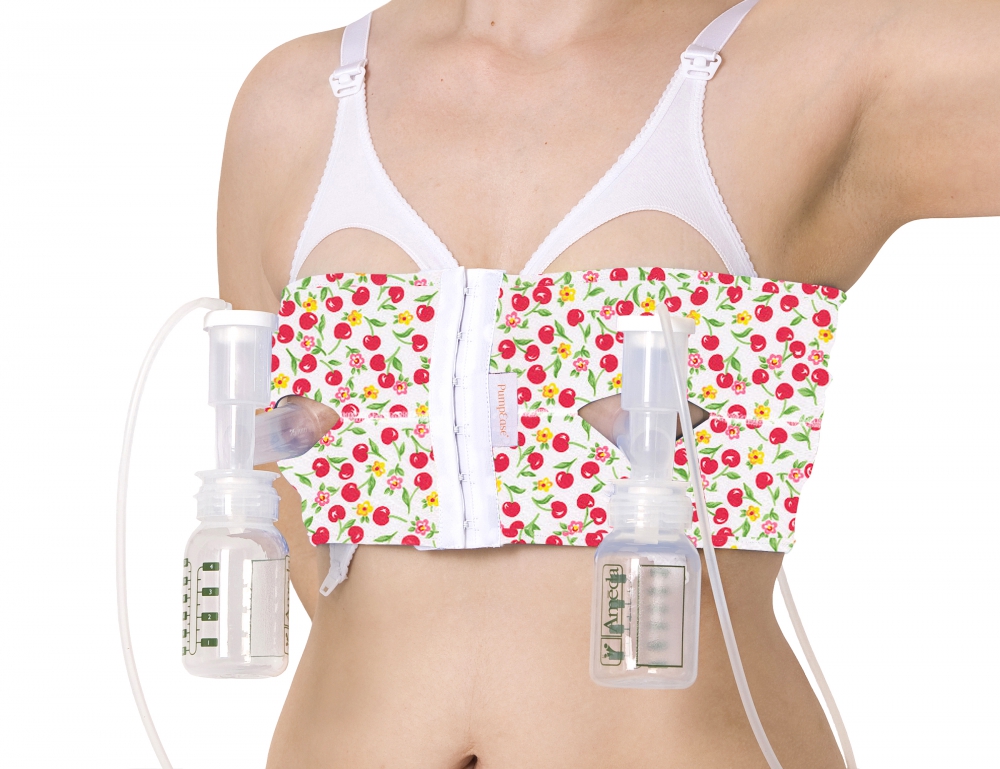
Hands-free electric pumps have been on the market for several years in the form of a fitted undergarment with breast pump attachments on the areolae to allow for hands-free breastmilk pumping. Recently, new models have become available that have a self-contained collection system with no tubing or visible containers. They use ergonomic designs to cup the breast under the garments and collect breast milk while the mother goes about her daily activities.
 |
 |
Open Collection Systems vs. Closed Collection Systems
The plastic tubing and breast shield (or flange) of an electric breast pump are commonly referred to as the collection system. When this style of breast pump was originally developed, the pump’s suction was supplied through the collection system tubing. This type of collection system design is now referred to as an open system.
Today most electric breast pumps feature a closed collection system. A closed collection system has a barrier or diaphragm that separates the pump tubing from the breast shield. In this design, the suction of the pump motor lifts the diaphragm to create a vacuum within the collection system to extract milk.
When an open collection system is used, the pump’s suction can cause milk to overflow into the collection system tubing, which may lead to milk particles being drawn into the pump motor. If milk leaks into the pump’s tubing, the tubes should be washed, sterilized and air-dried prior to using the pump again. Failure to thoroughly clean collection tubing may lead to mold growth within the tubing.
The diaphragm in a closed system eliminates the possibility of milk being able to overflow into the pump tubing. Because milk is unable to be exposed to the pump motor, closed collection systems are considered more hygienic than open collection systems. The barrier in a closed collection system breast pump also prevents outside air from contaminating the expressed breast milk in the collection bottle, which preserves the milk’s purity.
Breast Milk Storage, Thawing, and Warming
Some breast pumps are designed to be part of a "feeding system" so that the milk storage portion of the pump is the baby bottle used to feed the infant. Additionally, expressed milk may be collected in bags that are designed for freezing and storage.
The following table serves as a general guideline for storage of breast milk:[3][4][5][6][7][8][9]
| Location of Storage | Temperature | Maximum Recommended Storage Duration | Additional Advice |
|---|---|---|---|
| Room Temperature | 16-29°C (60-85°F) | 3-4 hours (optimal) | Insulated coolers/ ice packs may extend storage duration up to 24 hours. |
| Refrigerator | ≤4°C (39°C) | 72 hours (optimal) | Store at the back - away from the door. |
| Freezer | ≤-17°C (0°F) | 6 months (optimal) | Store at the back, away from the door. Do not re-freeze thawed breast milk. |
Directions for Thawing
Frozen breast milk should be thawed in the refrigerator for 12-24 hours. For expedited thawing, keep the storage container under cool running water.
Directions for Warming
It is recommended to warm milk by placing in a bowl of warm water, or using a bottle warmer. It is NOT recommended to microwave breast milk or heat it on the stove top.
Re-freezing
It is not safe to re-freeze thawed breast milk which was previously frozen or refrigerated. If the baby does not finish the milk in one feeding, it is recommended to refrigerate and attempt another feed within 2 hours. It is very important to refrigerate the remaining breast milk between feeds if it is intended to be fed to the baby at a later time.
Insurance coverage in the United States
In 2010, the Affordable Care Act (ACA), also known as "Obamacare" was passed. The ACA requires insurers to cover breast pumps and lactation support.[10] Insurers usually require a mother to go through a durable medical equipment supplier in their network. Mothers interested in getting access to lactation support, counseling and getting a free breast pump must contact their health insurance provider and request a list of in-network durable medical equipment supplier.[11] Some of the most well known suppliers include:
- Aeroflow Breastpumps
- McKesson
- Byram Healthcare
- Edgepark
- Acelleron
- Pumping Essentials
- Yummy Mummy
- Better Living Now
- MedSource
- A Breast Pump and More
- A Med Supplies
- Mommy Express
- 1 Natural Way
Related Pages
References
- ↑ Breastfeeding - Pumping and Equipment, http://kellymom.com/category/bf/pumpingmoms/, Accessed on: April 21, 2017
- ↑ Breastfeeding - womenshealth.gov
- ↑ Pardou A, Serruys E, Mascart-Lemone F, Dramaix M, Vis HL (1994). "Human milk banking: influence of storage processes and of bacterial contamination on some milk constituents". Biol Neonate. 65 (5): 302–9. PMID 8054398.
- ↑ Igumbor EO, Mukura RD, Makandiramba B, Chihota V (2000). "Storage of breast milk: effect of temperature and storage duration on microbial growth". Cent Afr J Med. 46 (9): 247–51. PMID 11320771.
- ↑ Lavine M, Clark RM (1987). "Changing patterns of free fatty acids in breast milk during storage". J Pediatr Gastroenterol Nutr. 6 (5): 769–74. PMID 3694370.
- ↑ Bertino E, Giribaldi M, Baro C, Giancotti V, Pazzi M, Peila C; et al. (2013). "Effect of prolonged refrigeration on the lipid profile, lipase activity, and oxidative status of human milk". J Pediatr Gastroenterol Nutr. 56 (4): 390–6. doi:10.1097/MPG.0b013e31827af155. PMID 23149807.
- ↑ Rechtman DJ, Lee ML, Berg H (2006). "Effect of environmental conditions on unpasteurized donor human milk". Breastfeed Med. 1 (1): 24–6. doi:10.1089/bfm.2006.1.24. PMID 17661557.
- ↑ Academy of Breastfeeding Medicine Protocol Committee (2010). "ABM clinical protocol #8: human milk storage information for home use for full-term infants (original protocol March 2004; revision #1 March 2010)". Breastfeed Med. 5 (3): 127–30. PMID 20524226.
- ↑ Hamosh M, Ellis LA, Pollock DR, Henderson TR, Hamosh P (1996). "Breastfeeding and the working mother: effect of time and temperature of short-term storage on proteolysis, lipolysis, and bacterial growth in milk". Pediatrics. 97 (4): 492–8. PMID 8632934.
- ↑ "Healthcare.gov Breastfeeding benefits".
- ↑ "How To Get A Free Breast Pump".