Multi-drug-resistant tuberculosis epidemiology and demographics
|
Multi-drug-resistant tuberculosis Microchapters |
|
Differentiating Multi-drug-resistant tuberculosis from other Diseases |
|---|
|
Diagnosis |
|
Treatment |
|
Case Studies |
|
Multi-drug-resistant tuberculosis epidemiology and demographics On the Web |
|
American Roentgen Ray Society Images of Multi-drug-resistant tuberculosis epidemiology and demographics |
|
FDA on Multi-drug-resistant tuberculosis epidemiology and demographics |
|
CDC on Multi-drug-resistant tuberculosis epidemiology and demographics |
|
Multi-drug-resistant tuberculosis epidemiology and demographics in the news |
|
Blogs on Multi-drug-resistant tuberculosis epidemiology and demographics |
|
Directions to Hospitals Treating Multi-drug-resistant tuberculosis |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [2]
Overview
Multi drug resistant tuberculosis has been emerging as an alarming threat due to the drug resistance developed due to inadequate treatment as well as slow gradual genetic mutations. People who are immunosupressed with diseases like HIV has a high chance of developing infection with multi drug resistant tuberculosis. The incidence of MDR varies substantially among countries. Prisons have a high incidence of multi drug resistant tuberculosis as well as people from soviet union have a high incidence of MDR TB
Epidemiology and Demographics
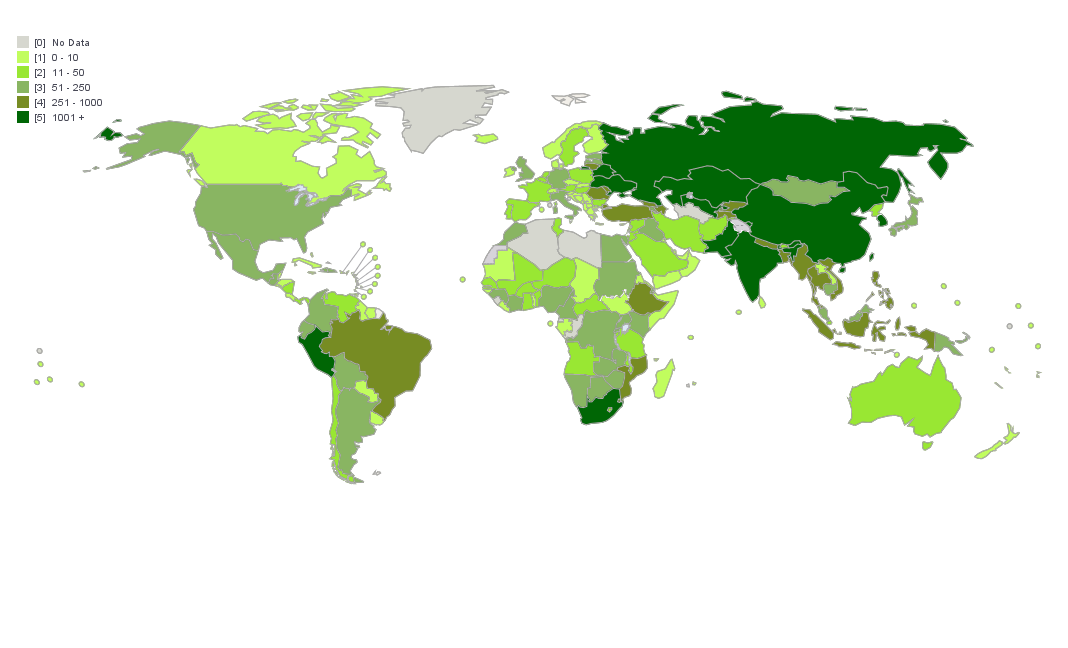
A 1997 survey of 35 countries found rates above 2% in about a third of the countries surveyed. The highest rates were in the former USSR, the Baltic states, Argentina, India and China, and was associated with poor or failing national Tuberculosis Control programmes. Likewise, the appearance of high rates of MDR-TB in New York city in the early 1990s was associated with the dismantling of public health programmes by the Reagan administration.[1][2]
MDR-TB can develop in the course of the treatment of fully sensitive TB and this is always the result of patients missing doses or failing to complete a course of treatment.
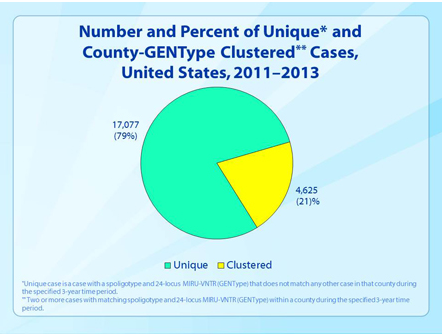
Thankfully, MDR-TB strains appear to be less fit and less transmissible. It has been known for many years that INH-resistant TB is less virulent in guinea pigs, and the epidemiological evidence is that MDR strains of TB do not dominate naturally. A study in Los Angeles found that only 6% of cases of MDR-TB were clustered. This should not be a cause for complacency: it must be remembered that MDR-TB has a mortality rate comparable to lung cancer. It must also be remembered that people who have weakened immune systems (because of diseases such as HIV or because of drugs) are more susceptible to catching TB.
A 1997 survey of 35 countries found mortality rates above 2% in about a third of the countries surveyed. The highest rates were in the former USSR, Argentina, India and China, and was associated with poor or failing national tuberculosis control programs. Likewise, the appearance of high rates of MDR-TB in New York city in the early 1990s was associated with the dismantling of public health programmes.[3][4]
MDR-TB strains appear to be less fit and less transmissible.[5] It has been known for many years that INH-resistant TB is less virulent in guinea pigs, and the epidemiological evidence is that MDR strains of TB do not dominate naturally. A study in Los Angeles found that only 6% of cases of MDR-TB were clustered. MDR-TB has a mortality rate comparable to lung cancer. People who have weakened immune systems (because of diseases such as HIV or because of drugs) are more susceptible to catching TB.
South African epidemic
Since late 2006, there has been an epidemic of XDR-TB in South Africa. The outbreak was first reported as a cluster of 53 patients in a rural hospital in KwaZulu-Natal of whom 52 died.[6] What was particularly worrisome was that the median survival from sputum specimen collection to death was only 16 days and that the majority of patients had never previously received treatment for tuberculosis. This is the epidemic for which the acronym XDR-TB was first used, and although TB strains that fulfill the current definition have been identified retrospectively,[7][8] this was the largest group of linked cases ever found. Since the initial report in September 2006,[9] cases have now been reported in most provinces in South Africa. As of 16 March 2007, there were 314 cases reported, with 215 deaths.[10] It is clear that the spread of this strain of TB is closely associated with a high prevalence of Aids and poor infection control; in other countries where XDR-TB strains have arisen, drug resistance has arisen from mismanagement of cases or poor patient compliance with drug treatment instead of being transmitted from person to person.[11] This strain of TB does not respond to any of the drugs currently available in South Africa for first- or second-line treatment. It is now clear that the problem has been around for much longer than health department officials have suggested, and is far more extensive.[12] By 23 November 2006, 303 cases of XDR-TB had been reported, of which 263 were in KwaZulu-Natal.[13] Serious thought has been put to isolation procedures that may deny some patients their mobility. This has been seen as unconstitutional by the government and patients come and go as they see fit. The few that do get quarantined start riots and stone security guards. Quarantining patients is necessary to prevent further spread of this strain of TB.
Incidence
- 3.6 % of the new tubercular cases have multi drug resistant strains.
- About 20% of the previously treated strains have drug resistance.
- The frequency of MDR TB varies substantially among countries.
- 10 % of MDR- TB cases are also resistant to two second line drug classes or XDR (Extensively drug resistant TB)
- 92 countries have reported at least oe XDR case by September 2013.
- About 450 000 people developed MDR-TB in the world in 2012. More than half of these cases were in India, China and the Russian Federation.
- It is estimated that about 9.6% of MDR-TB cases had XDR-TB.
Race
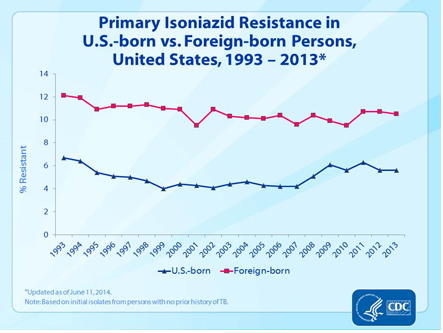
The highest amount of MDR-TB and resistance in United States is found in foreign born population especially from Soviet Union with 8.5 % and 33.5% of any resistance of TB in 2000.
Tuberculosis in prison
A rise in multi drug resistant strains of tuberculosis infection is found in prisons of developing countries as well as spanish prison and outbreaks in some prisons in New york city. [14]
 |
 |
 |
 |
 |
References
- ↑ Frieden TR, Sterling T, Pablos-Mendez A; et al. (1993). "The emergence of drug-resistant tuberculosis in New York City". N Engl J Med. 328 (8): 521&ndash, 56. PMID 8381207.
- ↑ Laurie Garrett (2000). Betrayal of trust: the collapse of global public health. New York: Hyperion. pp. 268ff. ISBN 0786884407 Check
|isbn=value: checksum (help). - ↑ Frieden TR, Sterling T, Pablos-Mendez A; et al. (1993). "The emergence of drug-resistant tuberculosis in New York City". N Engl J Med. 328 (8): 521&ndash, 56. PMID 8381207.
- ↑ Laurie Garrett (2000). Betrayal of trust: the collapse of global public health. New York: Hyperion. pp. 268ff. ISBN 0786884407 Check
|isbn=value: checksum (help). - ↑ Iseman MD (1994). "Evolution of drug-resistant tuberculosis: a tale of two species". Proc. Natl. Acad. Sci. U.S.A. 91 (7): 2428–9. PMID 8146134. Free Full Text.
- ↑ Invalid
<ref>tag; no text was provided for refs namedReuters2006 - ↑ Shah NS, Wright A, Drobniewski F; et al. (2005). "Extreme drug resistance in tuberculosis (XDR-TB): global survey of supranational reference laboratories for _Mycobacterium tuberculosis_ with resistance to second-line drugs". Int J Tuberc Lung Dis. 9(Suppl 1): S77.
- ↑ Centers for Diseases Control (2006). "Emergence of Mycobacterium tuberculosis with extensive resistance to second-line drugs-worldwide, 2000-2004". Morb Mort Wkly Rep. 55: 301&ndash, 5.
- ↑ Gandhi NR, Moll A, Sturm AW; et al. (2006). "Extensively drug-resistant tuberculosis as a cause of death in patients co-infected with
tuberculosis and HIV in a rural area of South Africa". Lancet. 368: 1575&ndash, 80. line feed character in
|title=at position 90 (help) - ↑ Angela Quintal. "314 XDR-TB cases reported in SA". Cape Times. Retrieved 2007-04-04.
- ↑ Migliori GB, Ortmann J, Girardi E; et al. (2007). "Extensively drug-resistant tuberculosis, Italy and Germany". 13 (5).
- ↑ Sidley P. (2006). "South Africa acts to curb spread of lethal strain of TB". Brit Med J. 333: 825.
- ↑ News24. "300+ cases of killer TB in SA". Retrieved 2006-11-23.
- ↑ "Strategies against multidrug-resistant tuberculosis". Invalid parameter "against" in
<ref>tag. The supported parameters are: dir, follow, group, name. - ↑ "World health organization (WHO)".
- ↑ 16.0 16.1 "Center for Disease Control and Prevention (CDC)".
- ↑ 17.0 17.1 17.2 "Public Health Image Library (PHIL), Centers for Disease Control and Prevention".