Sargramostim: Difference between revisions
No edit summary |
No edit summary |
||
| Line 107: | Line 107: | ||
| molecular_weight = 14434.5 g/mol | | molecular_weight = 14434.5 g/mol | ||
}} | }} | ||
|PD=====In vitro Studies of LEUKINE in Human Cells==== | |||
*The biological activity of [[GM-CSF]] is species-specific. Consequently, in vitro studies have been performed on human cells to characterize the pharmacological activity of LEUKINE. In vitro exposure of human [[bone marrow]] cells to LEUKINE at concentrations ranging from 1–100 ng/mL results in the proliferation of hematopoietic progenitors and in the formation of pure [[granulocyte]], pure [[macrophage]] and mixed [[granulocytemacrophage colonies]]. Chemotactic, anti-fungal and anti-parasitic activities of [[granulocytes]] and [[monocytes]] are increased by exposure to LEUKINE in vitro. LEUKINE increases the cytotoxicity of [[monocytes]] toward certain neoplastic cell lines and activates [[polymorphonuclear neutrophils]] to inhibit the growth of [[tumor cells]]. | |||
|PK=====General==== | |PK=====General==== | ||
*[[GM-CSF]] belongs to a group of growth factors termed colony stimulating factors which support survival, clonal expansion, and differentiation of hematopoietic progenitor cells. [[GM-CSF]] induces partially committed progenitor cells to divide and differentiate in the granulocyte-macrophage pathways which include [[neutrophils]], [[monocytes]]/[[macrophages]] and [[myeloid]]-derived [[dendritic cells]]. | *[[GM-CSF]] belongs to a group of growth factors termed colony stimulating factors which support survival, clonal expansion, and differentiation of hematopoietic progenitor cells. [[GM-CSF]] induces partially committed progenitor cells to divide and differentiate in the granulocyte-macrophage pathways which include [[neutrophils]], [[monocytes]]/[[macrophages]] and [[myeloid]]-derived [[dendritic cells]]. | ||
*[[GM-CSF]] is also capable of activating mature [[granulocytes]] and [[macrophages]]. [[GM-CSF]] is a multilineage factor and, in addition to dose-dependent effects on the myelomonocytic lineage, can promote the proliferation of [[megakaryocytic]] and [[erythroid progenitors]]. However, other factors are required to induce complete maturation in these two lineages. The various cellular responses (i.e., division, maturation, activation) are induced through [[GM-CSF]] binding to specific receptors expressed on the cell surface of target cells.2 | |||
====In vivo Primate Studies of LEUKINE==== | |||
*Pharmacology/toxicology studies of LEUKINE were performed in cynomolgus monkeys. An acute toxicity study revealed an absence of treatment-related toxicity following a single IV bolus injection at a dose of 300 mcg/kg. Two subacute studies were performed using IV injection (maximum dose 200 mcg/kg/day × 14 days) and subcutaneous injection (SC) (maximum dose 200 mcg/kg/day × 28 days). No major visceral organ toxicity was documented. Notable histopathology findings included increased cellularity in hematologic organs and heart and lung tissues. A dose-dependent increase in leukocyte count, which consisted primarily of segmented neutrophils, occurred during the dosing period; increases in [[monocytes]], [[basophils]], [[eosinophils]] and [[lymphocytes]] were also noted. [[Leukocyte]] counts decreased to pretreatment values over a 1–2 week recovery period. | |||
====Pharmacokinetics==== | |||
*Pharmacokinetic profiles have been analyzed in controlled studies of 24 normal male volunteers. Liquid and lyophilized LEUKINE, at the recommended dose of 250 mcg/m2, have been determined to be bioequivalent based on the statistical evaluation of AUC.5 | *Pharmacokinetic profiles have been analyzed in controlled studies of 24 normal male volunteers. Liquid and lyophilized LEUKINE, at the recommended dose of 250 mcg/m2, have been determined to be bioequivalent based on the statistical evaluation of AUC.5 | ||
*When LEUKINE (either liquid or lyophilized) was administered IV over two hours to normal volunteers, the mean beta half-life was approximately 60 minutes. Peak concentrations of GM-CSF were observed in blood samples obtained during or immediately after completion of LEUKINE infusion. For liquid LEUKINE, the mean maximum concentration (Cmax) was 5.0 ng/mL, the mean clearance rate was approximately 420 mL/min/m2 and the mean AUC (0–inf) was 640 ng/mL•min. Corresponding results for lyophilized LEUKINE in the same subjects were mean Cmax of 5.4 ng/mL, mean clearance rate of 431 mL/min/m2, and mean AUC (0–inf) of 677 ng/mL•min. GM-CSF was last detected in blood samples obtained at three or six hours. | *When LEUKINE (either liquid or lyophilized) was administered IV over two hours to normal volunteers, the mean beta half-life was approximately 60 minutes. Peak concentrations of GM-CSF were observed in blood samples obtained during or immediately after completion of LEUKINE infusion. For liquid LEUKINE, the mean maximum concentration (Cmax) was 5.0 ng/mL, the mean clearance rate was approximately 420 mL/min/m2 and the mean AUC (0–inf) was 640 ng/mL•min. Corresponding results for lyophilized LEUKINE in the same subjects were mean Cmax of 5.4 ng/mL, mean clearance rate of 431 mL/min/m2, and mean AUC (0–inf) of 677 ng/mL•min. GM-CSF was last detected in blood samples obtained at three or six hours. | ||
*When LEUKINE (either liquid or lyophilized) was administered SC to normal volunteers, GM-CSF was detected in the serum at 15 minutes, the first sample point. The mean beta half-life was approximately 162 minutes. Peak levels occurred at one to three hours post injection, and LEUKINE remained detectable for up to six hours after injection. The mean Cmax was 1.5 ng/mL. For liquid LEUKINE, the mean clearance was 549 mL/min/m2 and the mean AUC (0–inf) was 549 ng/mL•min. For lyophilized LEUKINE, the mean clearance was 529 mL/min/m2 and the mean AUC (0–inf) was 501 ng/mL•min | *When LEUKINE (either liquid or lyophilized) was administered SC to normal volunteers, GM-CSF was detected in the serum at 15 minutes, the first sample point. The mean beta half-life was approximately 162 minutes. Peak levels occurred at one to three hours post injection, and LEUKINE remained detectable for up to six hours after injection. The mean Cmax was 1.5 ng/mL. For liquid LEUKINE, the mean clearance was 549 mL/min/m2 and the mean AUC (0–inf) was 549 ng/mL•min. For lyophilized LEUKINE, the mean clearance was 529 mL/min/m2 and the mean AUC (0–inf) was 501 ng/mL•min | ||
|clinicalStudies=====Acute Myelogenous Leukemia==== | |||
*The safety and efficacy of LEUKINE in patients with AML who are younger than 55 years of age have not been determined. Based on Phase II data suggesting the best therapeutic effects could be achieved in patients at highest risk for severe infections and mortality while [[neutropenic]], the Phase III clinical trial was conducted in older patients. The safety and efficacy of LEUKINE in the treatment of AML were evaluated in a multi-center, randomized, double-blind placebo-controlled trial of 99 newly diagnosed adult patients, 55–70 years of age, receiving induction with or without consolidation. A combination of standard doses of [[daunorubicin]] (days 1–3) and [[ara-C]] (days 1–7) was administered during induction and high dose [[ara-C]] was administered days 1–6 as a single course of consolidation, if given. [[Bone marrow]] evaluation was performed on day 10 following induction chemotherapy. If [[hypoplasia] with <5% blasts was not achieved, patients immediately received a second cycle of induction chemotherapy. If the [[bone marrow]] was hypoplastic with <5% blasts on day 10 or four days following the second cycle of induction chemotherapy, LEUKINE (250 mcg/m2/day) or placebo was given IV over four hours each day, starting four days after the completion of chemotherapy. Study drug was continued until an ANC ≥1500/mm3 for three consecutive days was attained or a maximum of 42 days. LEUKINE or placebo was also administered after the single course of consolidation chemotherapy if delivered ([[ara-C]] 3–6 weeks after induction following [[neutrophil]] recovery). Study drug was discontinued immediately if leukemic regrowth occurred. | |||
*LEUKINE significantly shortened the median duration of [[ANC]] <500/mm3 by 4 days and <1000/mm3 by 7 days following induction (see TABLE 1). 75% of patients receiving LEUKINE achieved [[ANC]] >500/mm3 by day 16, compared to day 25 for patients receiving [[placebo]]. The proportion of patients receiving one cycle (70%) or two cycles (30%) of induction was similar in both treatment groups; LEUKINE significantly shortened the median times to [[neutrophil]] recovery whether one cycle (12 versus 15 days) or two cycles (14 versus 23 days) of induction chemotherapy was administered. Median times to [[platelet]] (>20,000/mm3) and RBC transfusion independence were not significantly different between treatment groups. | |||
[[file:Sargramostim CS1.png|none|350px]] | |||
*During the consolidation phase of treatment, LEUKINE did not shorten the median time to recovery of [[ANC]] to 500/mm3 (13 days) or 1000/mm3 (14.5 days) compared to placebo. There were no significant differences in time to platelet and [[RBC]] transfusion independence. | |||
*The incidence of severe infections and deaths associated with infections was significantly reduced in patients who received LEUKINE. During induction or consolidation, 27 of 52 patients receiving LEUKINE and 35 of 47 patients receiving [[placebo]] had at least one grade 3, 4 or 5 infection (p=0.02). Twenty-five patients receiving LEUKINE and 30 patients receiving placebo experienced severe and fatal infections during induction only. There were significantly fewer deaths from infectious causes in the LEUKINE arm (3 versus 11, p=0.02). The majority of deaths in the placebo group were associated with fungal infections with [[pneumonia]] as the primary infection. | |||
*Disease outcomes were not adversely affected by the use of LEUKINE. The proportion of patients achieving complete remission (CR) was higher in the LEUKINE group (69% as compared to 55% for the placebo group), but the difference was not significant (p=0.21). There was no significant difference in relapse rates; 12 of 36 patients who received LEUKINE and five of 26 patients who received placebo relapsed within 180 days of documented CR (p=0.26). The overall median survival was 378 days for patients receiving LEUKINE and 268 days for those on placebo (p=0.17). The study was not sized to assess the impact of LEUKINE treatment on response or survival. | |||
====Mobilization and Engraftment of PBPC==== | |||
A retrospective review was conducted of data from patients with cancer undergoing collection of peripheral blood progenitor cells (PBPC) at a single transplant center. Mobilization of PBPC and myeloid reconstitution post-transplant were compared between four groups of patients (n=196) receiving LEUKINE for mobilization and a historical control group who did not receive any mobilization treatment [progenitor cells collected by leukapheresis without mobilization (n=100)]. Sequential cohorts received LEUKINE. The cohorts differed by dose (125 or 250 mcg/m2/day), route (IV over 24 hours or SC) and use of LEUKINE post-transplant. Leukaphereses were initiated for all mobilization groups after the WBC reached 10,000/mm3. Leukaphereses continued until both a minimum number of mononucleated cells (MNC) were collected (6.5 or 8.0 × 108/kg body weight) and a minimum number of phereses (5–8) were performed. Both minimum requirements varied by treatment cohort and planned conditioning regimen. If subjects failed to reach a WBC of 10,000 cells/mm3 by day five, another cytokine was substituted for LEUKINE; these subjects were all successfully leukapheresed and transplanted. The most marked mobilization and post-transplant effects were seen in patients administered the higher dose of LEUKINE (250 mcg/m2) either IV (n=63) or SC (n=41). | |||
PBPCs from patients treated at the 250 mcg/m2/day dose had significantly higher number of granulocyte-macrophage colony-forming units (CFU-GM) than those collected without mobilization. The mean value after thawing was 11.41 × 104 CFU-GM/kg for all LEUKINE-mobilized patients, compared to 0.96 × 104/kg for the non-mobilized group. A similar difference was observed in the mean number of erythrocyte burst-forming units (BFU-E) collected (23.96 × 104/kg for patients mobilized with 250 mcg/m2 doses of LEUKINE administered SC vs. 1.63 × 104/kg for non-mobilized patients). | |||
After transplantation, mobilized subjects had shorter times to myeloid engraftment and fewer days between transplantation and the last platelet transfusion compared to non-mobilized subjects. Neutrophil recovery (ANC >500/mm3) was more rapid in patients administered LEUKINE following PBPC transplantation with LEUKINE-mobilized cells (see TABLE 2). Mobilized patients also had fewer days to the last platelet transfusion and last RBC transfusion, and a shorter duration of hospitalization than did non-mobilized subjects. | |||
|alcohol=Alcohol-Sargramostim interaction has not been established. Talk to your doctor about the effects of taking alcohol with this medication. | |alcohol=Alcohol-Sargramostim interaction has not been established. Talk to your doctor about the effects of taking alcohol with this medication. | ||
}} | }} | ||
Revision as of 16:56, 16 February 2015
{{DrugProjectFormSinglePage |authorTag=Alberto Plate [1] |genericName=Sarramostin |aOrAn=a |drugClass=colony stimulating factor |indicationType=treatment |indication=granulocytopnia following induction chemotherapy in acute myelogenous leukemia, mobilization and following transplantation of autologous peripheral blood progentior cells, myeloid reconstitution after autologous bone marrow transplantation, myeloid reconstitution after allogeneic bone marrow transplantation and bone marrow transplantation failure or engraftment delay |adverseReactions=chest pain, peripheral edema, pruritus, rash, hypercholesterolemia, hypomagnesemia, weight loss, abdominal pain, diarrhea, dysphagia, GI hemorrhage, hematemesis, nausea, vomiting, acute myelogenous leukemia, increased bilirrubin, arthralgia, bone pain, myalgia, asthenia, intraocular hemorrhage, anxiety, elevated BUN, pharyngitis, fever, malaise and rigor |blackBoxWarningTitle=TITLE |blackBoxWarningBody=Condition Name: (Content) |offLabelAdultGuideSupport=There is limited information regarding Off-Label Guideline-Supported Use of Sargramostim in adult patients. |offLabelAdultNoGuideSupport=There is limited information regarding Off-Label Non–Guideline-Supported Use of Sargramostim in adult patients. |offLabelPedGuideSupport=There is limited information regarding Off-Label Guideline-Supported Use of Sargramostim in pediatric patients. |offLabelPedNoGuideSupport=There is limited information regarding Off-Label Non–Guideline-Supported Use of Sargramostim in pediatric patients. |contraindications=LEUKINE is contraindicated:
- in patients with excessive leukemic myeloid blasts in the bone marrow or peripheral blood (≥ 10%);
- in patients with known hypersensitivity to GM-CSF, yeast-derived products or any component of the product;
- for concomitant use with chemotherapy and radiotherapy.
Due to the potential sensitivity of rapidly dividing hematopoietic progenitor cells, LEUKINE should not be administered simultaneously with cytotoxic chemotherapy or radiotherapy or within 24 hours preceding or following chemotherapy or radiotherapy. In one controlled study, patients with small cell lung cancer received LEUKINE and concurrent thoracic radiotherapy and chemotherapy or the identical radiotherapy and chemotherapy without LEUKINE. The patients randomized to LEUKINE had significantly higher incidence of adverse events, including higher mortality and a higher incidence of grade 3 and 4 infections and grade 3 and 4 thrombocytopenia. |warnings=====Pediatric Use====
- Benzyl alcohol is a constituent of liquid LEUKINE and Bacteriostatic Water for Injection diluent. Benzyl alcohol has been reported to be associated with a fatal "Gasping Syndrome" in premature infants. Liquid solutions containing benzyl alcohol (including liquid LEUKINE) or lyophilized LEUKINE reconstituted with Bacteriostatic Water for Injection, USP (0.9% benzyl alcohol) should not be administered to neonates.
Fluid Retention
- Edema, capillary leak syndrome, pleural effusion and/or pericardial effusion have been reported in patients after LEUKINE administration. In 156 patients enrolled in placebo-controlled studies using LEUKINE at a dose of 250 mcg/m2/day by 2-hour IV infusion, the reported incidences of fluid retention (LEUKINE vs. placebo) were as follows: peripheral edema, 11% vs. 7%; pleural effusion, 1% vs. 0%; and pericardial effusion, 4% vs. 1%. Capillary leak syndrome was not observed in this limited number of studies; based on other uncontrolled studies and reports from users of marketed LEUKINE, the incidence is estimated to be less than 1%. In patients with preexisting pleural and pericardial effusions, administration of LEUKINE may aggravate fluid retention; however, fluid retention associated with or worsened by LEUKINE has been reversible after interruption or dose reduction of LEUKINE with or without diuretic therapy. LEUKINE should be used with caution in patients with preexisting fluid retention, pulmonary infiltrates or congestive heart failure.
Respiratory Symptoms
- Sequestration of granulocytes in the pulmonary circulation has been documented following LEUKINE infusion and dyspnea has been reported occasionally in patients treated with LEUKINE. Special attention should be given to respiratory symptoms during or immediately following LEUKINE infusion, especially in patients with preexisting lung disease. In patients displaying dyspnea during LEUKINE administration, the rate of infusion should be reduced by half. If respiratory symptoms worsen despite infusion rate reduction, the infusion should be discontinued. Subsequent IV infusions may be administered following the standard dose schedule with careful monitoring. LEUKINE should be administered with caution in patients with hypoxia.
Cardiovascular Symptoms
- Occasional transient supraventricular arrhythmia has been reported in uncontrolled studies during LEUKINE administration, particularly in patients with a previous history of cardiac arrhythmia. However, these arrhythmias have been reversible after discontinuation of LEUKINE. LEUKINE should be used with caution in patients with preexisting cardiac disease.
Renal and Hepatic Dysfunction
- In some patients with preexisting renal dysfunction or hepatic dysfunction enrolled in uncontrolled clinical trials, administration of LEUKINE has induced elevation of serum creatinine or bilirubin and hepatic enzymes. Dose reduction or interruption of LEUKINE administration has resulted in a decrease to pretreatment values. However, in controlled clinical trials the incidences of renal dysfunction and hepatic dysfunction were comparable between LEUKINE (250 mcg/m2/day by 2-hour IV infusion) and placebo-treated patients. Monitoring of renal function and hepatic function in patients displaying renal or hepatic dysfunction prior to initiation of treatment is recommended at least every other week during LEUKINE administration.
|clinicalTrials=====Autologous and Allogeneic Bone Marrow Transplantation====
- LEUKINE is generally well tolerated. In three placebo-controlled studies enrolling a total of 156 patients after autologous BMT or peripheral blood progenitor cell transplantation, events reported in at least 10% of patients who received IV LEUKINE or placebo were as reported in TABLE 6.
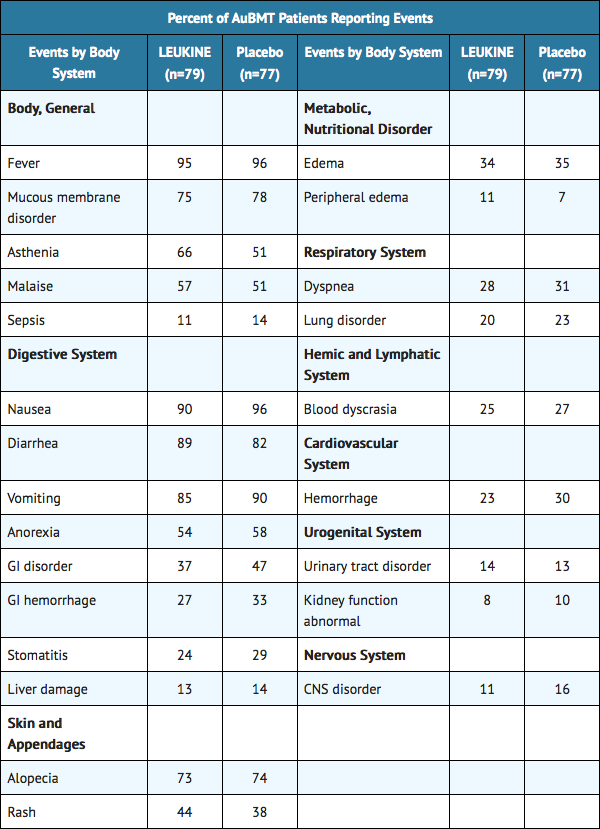
- No significant differences were observed between LEUKINE and placebo-treated patients in the type or frequency of laboratory abnormalities, including renal and hepatic parameters. In some patients with preexisting renal or hepatic dysfunction enrolled in uncontrolled clinical trials, administration of LEUKINE has induced elevation of serum creatinine or bilirubin and hepatic enzymes (see WARNINGS). In addition, there was no significant difference in relapse rate and 24 month survival between the LEUKINE and placebo-treated patients.
- In the placebo-controlled trial of 109 patients after allogeneic BMT, events reported in at least 10% of patients who received IV LEUKINE or placebo were as reported in TABLE 7.

- There were no significant differences in the incidence or severity of GVHD, relapse rates and survival between the LEUKINE and placebo-treated patients. Adverse events observed for the patients treated with LEUKINE in the historically-controlled BMT failure study were similar to those reported in the placebo-controlled studies. In addition, headache (26%), pericardial effusion (25%), arthralgia (21%) and myalgia (18%) were also reported in patients treated with LEUKINE in the graft failure study.
- In uncontrolled Phase I/II studies with LEUKINE in 215 patients, the most frequent adverse events were fever, asthenia, headache, bone pain, chills and myalgia. These systemic events were generally mild or moderate and were usually prevented or reversed by the administration of analgesics and antipyretics such as acetaminophen. In these uncontrolled trials, other infrequent events reported were dyspnea, peripheral edema, and rash.
- Reports of events occurring with marketed LEUKINE include arrhythmia, fainting, eosinophilia, dizziness, hypotension, injection site reactions, pain (including abdominal, back, chest, and joint pain), tachycardia, thrombosis, and transient liver function abnormalities.
- In patients with preexisting edema, capillary leak syndrome, pleural effusion and/or pericardial effusion, administration of LEUKINE may aggravate fluid retention. Body weight and hydration status should be carefully monitored during LEUKINE administration.
- Adverse events observed in pediatric patients in controlled studies were comparable to those observed in adult patients.
Acute Myelogenous Leukemia
Adverse events reported in at least 10% of patients who received LEUKINE or placebo were as reported in TABLE 8.
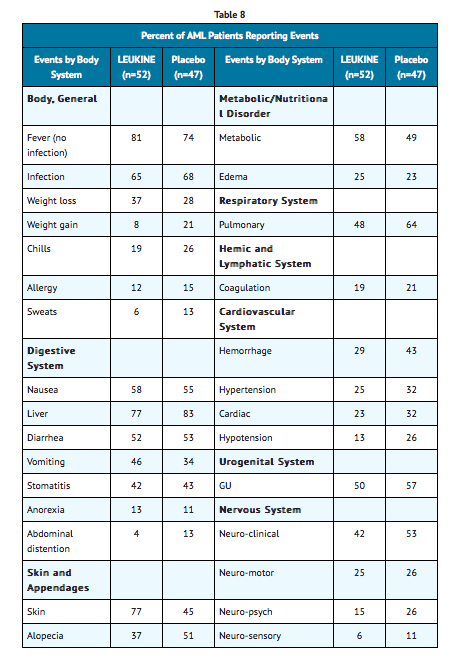
- Nearly all patients reported leukopenia, thrombocytopenia and anemia. The frequency and type of adverse events observed following induction were similar between LEUKINE and placebo groups. The only significant difference in the rates of these adverse events was an increase in skin associated events in the LEUKINE group (p=0.002). No significant differences were observed in laboratory results, renal or hepatic toxicity. No significant differences were observed between the LEUKINE and placebo-treated patients for adverse events following consolidation. There was no significant difference in response rate or relapse rate.
- In a historically-controlled study of 86 patients with acute myelogenous leukemia (AML), the LEUKINE treated group exhibited an increased incidence of weight gain (p=0.007), low serum proteins and prolonged prothrombin time (p=0.02) when compared to the control group. Two LEUKINE treated patients had progressive increase in circulating monocytes and promonocytes and blasts in the marrow which reversed when LEUKINE was discontinued. The historical control group exhibited an increased incidence of cardiac events (p=0.018), liver function abnormalities (p=0.008), and neurocortical hemorrhagic events (p=0.025).15
Antibody Formation
- Serum samples collected before and after LEUKINE treatment from 214 patients with a variety of underlying diseases have been examined for immunogenicity based on the presence of antibodies. Neutralizing antibodies were detected in five of 214 patients (2.3%) after receiving LEUKINE by continuous IV infusion (three patients) or subcutaneous injection (SC) (two patients) for 28 to 84 days in multiple courses. All five patients had impaired hematopoiesis before the administration of LEUKINE and consequently the effect of the development of anti-GM-CSF antibodies on normal hematopoiesis could not be assessed. Antibody studies of 75 patients with Crohn's disease receiving LEUKINE by subcutaneous injection with normal hematopoiesis and no other immunosuppressive drugs showed one patient (1.3%) with detectable neutralizing antibodies. The clinical relevance of the presence of these antibodies are unknown. Drug-induced neutropenia, neutralization of endogenous GM-CSF activity and diminution of the therapeutic effect of LEUKINE secondary to formation of neutralizing antibody remain a theoretical possibility. Serious allergic and anaphylactoid reactions have been reported with LEUKINE but the rate of occurrence of antibodies in such patients has not been assessed.
Overdosage
- The maximum amount of LEUKINE that can be safely administered in single or multiple doses has not been determined. Doses up to 100 mcg/kg/day (4,000 mcg/m2/day or 16 times the recommended dose) were administered to four patients in a Phase I uncontrolled clinical study by continuous IV infusion for 7 to 18 days. Increases in WBC up to 200,000 cells/mm3 were observed. Adverse events reported were dyspnea, malaise, nausea, fever, rash, sinus tachycardia, headache and chills. All these events were reversible after discontinuation of LEUKINE.
- In case of overdosage, LEUKINE therapy should be discontinued and the patient carefully monitored for WBC increase and respiratory symptoms.
To report SUSPECTED ADVERSE REACTIONS, contact Genzyme Corporation at 1-888-4RX-LEUKINE or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch |drugInteractions=*Interactions between LEUKINE and other drugs have not been fully evaluated. Drugs which may potentiate the myeloproliferative effects of LEUKINE, such as lithium and corticosteroids, should be used with caution. |FDAPregCat=C |useInPregnancyFDA=Animal reproduction studies have not been conducted with LEUKINE. It is not known whether LEUKINE can cause fetal harm when administered to a pregnant woman or can affect reproductive capability. LEUKINE should be given to a pregnant woman only if clearly needed. |useInNursing=*It is not known whether LEUKINE is excreted in human milk. Because many drugs are excreted in human milk, LEUKINE should be administered to a nursing woman only if clearly needed. |useInPed=*Safety and effectiveness in pediatric patients have not been established; however, available safety data indicate that LEUKINE does not exhibit any greater toxicity in pediatric patients than in adults. A total of 124 pediatric subjects between the ages of 4 months and 18 years have been treated with LEUKINE in clinical trials at doses ranging from 60–1,000 mcg/m2/day intravenously and 4–1,500 mcg/m2/day subcutaneously. In 53 pediatric patients enrolled in controlled studies at a dose of 250 mcg/m2/day by 2-hour IV infusion, the type and frequency of adverse events were comparable to those reported for the adult population. Liquid solutions containing benzyl alcohol (including liquid LEUKINE) or lyophilized LEUKINE reconstituted with Bacteriostatic Water for Injection, USP (0.9% benzyl alcohol) should not be administered to neonates |useInGeri=*In the clinical trials, experience in older patients (age ≥65 years), was limited to the acute myelogenous leukemia (AML) study. Of the 52 patients treated with LEUKINE in this randomized study, 22 patients were age 65–70 years and 30 patients were age 55–64 years. The number of placebo patients in each age group were 13 and 33 patients respectively. This was not an adequate database from which determination of differences in efficacy endpoints or safety assessments could be reliably made and this clinical study was not designed to evaluate difference between these two age groups. Analyses of general trends in safety and efficacy were undertaken and demonstrate similar patterns for older (65–70 yrs) vs younger patients (55–64 yrs). Greater sensitivity of some older individuals cannot be ruled out. |overdose=T*he maximum amount of LEUKINE that can be safely administered in single or multiple doses has not been determined. Doses up to 100 mcg/kg/day (4,000 mcg/m2/day or 16 times the recommended dose) were administered to four patients in a Phase I uncontrolled clinical study by continuous IV infusion for 7 to 18 days. Increases in WBC up to 200,000 cells/mm3 were observed. Adverse events reported were dyspnea, malaise, nausea, fever, rash, sinus tachycardia, headache and chills. All these events were reversible after discontinuation of LEUKINE.
- In case of overdosage, LEUKINE therapy should be discontinued and the patient carefully monitored for WBC increase and respiratory symptoms.
|drugBox=
Sargramostim
| |
| Systematic (IUPAC) name | |
| Human granulocyte macrophage colony stimulating factor | |
| Identifiers | |
| CAS number | |
| ATC code | L03 |
| PubChem | ? |
| DrugBank | |
| Chemical data | |
| Formula | Template:OrganicBox atomTemplate:OrganicBox atomTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBox atomTemplate:OrganicBoxTemplate:OrganicBox atomTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBox atomTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBox |
| Mol. mass | 14434.5 g/mol |
| Pharmacokinetic data | |
| Bioavailability | ? |
| Metabolism | ? |
| Half life | ? |
| Excretion | ? |
| Therapeutic considerations | |
| Pregnancy cat. |
? |
| Legal status |
Rx only |
| Routes | ? |
|PD=====In vitro Studies of LEUKINE in Human Cells====
- The biological activity of GM-CSF is species-specific. Consequently, in vitro studies have been performed on human cells to characterize the pharmacological activity of LEUKINE. In vitro exposure of human bone marrow cells to LEUKINE at concentrations ranging from 1–100 ng/mL results in the proliferation of hematopoietic progenitors and in the formation of pure granulocyte, pure macrophage and mixed granulocytemacrophage colonies. Chemotactic, anti-fungal and anti-parasitic activities of granulocytes and monocytes are increased by exposure to LEUKINE in vitro. LEUKINE increases the cytotoxicity of monocytes toward certain neoplastic cell lines and activates polymorphonuclear neutrophils to inhibit the growth of tumor cells.
|PK=====General====
- GM-CSF belongs to a group of growth factors termed colony stimulating factors which support survival, clonal expansion, and differentiation of hematopoietic progenitor cells. GM-CSF induces partially committed progenitor cells to divide and differentiate in the granulocyte-macrophage pathways which include neutrophils, monocytes/macrophages and myeloid-derived dendritic cells.
- GM-CSF is also capable of activating mature granulocytes and macrophages. GM-CSF is a multilineage factor and, in addition to dose-dependent effects on the myelomonocytic lineage, can promote the proliferation of megakaryocytic and erythroid progenitors. However, other factors are required to induce complete maturation in these two lineages. The various cellular responses (i.e., division, maturation, activation) are induced through GM-CSF binding to specific receptors expressed on the cell surface of target cells.2
In vivo Primate Studies of LEUKINE
- Pharmacology/toxicology studies of LEUKINE were performed in cynomolgus monkeys. An acute toxicity study revealed an absence of treatment-related toxicity following a single IV bolus injection at a dose of 300 mcg/kg. Two subacute studies were performed using IV injection (maximum dose 200 mcg/kg/day × 14 days) and subcutaneous injection (SC) (maximum dose 200 mcg/kg/day × 28 days). No major visceral organ toxicity was documented. Notable histopathology findings included increased cellularity in hematologic organs and heart and lung tissues. A dose-dependent increase in leukocyte count, which consisted primarily of segmented neutrophils, occurred during the dosing period; increases in monocytes, basophils, eosinophils and lymphocytes were also noted. Leukocyte counts decreased to pretreatment values over a 1–2 week recovery period.
Pharmacokinetics
- Pharmacokinetic profiles have been analyzed in controlled studies of 24 normal male volunteers. Liquid and lyophilized LEUKINE, at the recommended dose of 250 mcg/m2, have been determined to be bioequivalent based on the statistical evaluation of AUC.5
- When LEUKINE (either liquid or lyophilized) was administered IV over two hours to normal volunteers, the mean beta half-life was approximately 60 minutes. Peak concentrations of GM-CSF were observed in blood samples obtained during or immediately after completion of LEUKINE infusion. For liquid LEUKINE, the mean maximum concentration (Cmax) was 5.0 ng/mL, the mean clearance rate was approximately 420 mL/min/m2 and the mean AUC (0–inf) was 640 ng/mL•min. Corresponding results for lyophilized LEUKINE in the same subjects were mean Cmax of 5.4 ng/mL, mean clearance rate of 431 mL/min/m2, and mean AUC (0–inf) of 677 ng/mL•min. GM-CSF was last detected in blood samples obtained at three or six hours.
- When LEUKINE (either liquid or lyophilized) was administered SC to normal volunteers, GM-CSF was detected in the serum at 15 minutes, the first sample point. The mean beta half-life was approximately 162 minutes. Peak levels occurred at one to three hours post injection, and LEUKINE remained detectable for up to six hours after injection. The mean Cmax was 1.5 ng/mL. For liquid LEUKINE, the mean clearance was 549 mL/min/m2 and the mean AUC (0–inf) was 549 ng/mL•min. For lyophilized LEUKINE, the mean clearance was 529 mL/min/m2 and the mean AUC (0–inf) was 501 ng/mL•min
|clinicalStudies=====Acute Myelogenous Leukemia====
- The safety and efficacy of LEUKINE in patients with AML who are younger than 55 years of age have not been determined. Based on Phase II data suggesting the best therapeutic effects could be achieved in patients at highest risk for severe infections and mortality while neutropenic, the Phase III clinical trial was conducted in older patients. The safety and efficacy of LEUKINE in the treatment of AML were evaluated in a multi-center, randomized, double-blind placebo-controlled trial of 99 newly diagnosed adult patients, 55–70 years of age, receiving induction with or without consolidation. A combination of standard doses of daunorubicin (days 1–3) and ara-C (days 1–7) was administered during induction and high dose ara-C was administered days 1–6 as a single course of consolidation, if given. Bone marrow evaluation was performed on day 10 following induction chemotherapy. If [[hypoplasia] with <5% blasts was not achieved, patients immediately received a second cycle of induction chemotherapy. If the bone marrow was hypoplastic with <5% blasts on day 10 or four days following the second cycle of induction chemotherapy, LEUKINE (250 mcg/m2/day) or placebo was given IV over four hours each day, starting four days after the completion of chemotherapy. Study drug was continued until an ANC ≥1500/mm3 for three consecutive days was attained or a maximum of 42 days. LEUKINE or placebo was also administered after the single course of consolidation chemotherapy if delivered (ara-C 3–6 weeks after induction following neutrophil recovery). Study drug was discontinued immediately if leukemic regrowth occurred.
- LEUKINE significantly shortened the median duration of ANC <500/mm3 by 4 days and <1000/mm3 by 7 days following induction (see TABLE 1). 75% of patients receiving LEUKINE achieved ANC >500/mm3 by day 16, compared to day 25 for patients receiving placebo. The proportion of patients receiving one cycle (70%) or two cycles (30%) of induction was similar in both treatment groups; LEUKINE significantly shortened the median times to neutrophil recovery whether one cycle (12 versus 15 days) or two cycles (14 versus 23 days) of induction chemotherapy was administered. Median times to platelet (>20,000/mm3) and RBC transfusion independence were not significantly different between treatment groups.

- During the consolidation phase of treatment, LEUKINE did not shorten the median time to recovery of ANC to 500/mm3 (13 days) or 1000/mm3 (14.5 days) compared to placebo. There were no significant differences in time to platelet and RBC transfusion independence.
- The incidence of severe infections and deaths associated with infections was significantly reduced in patients who received LEUKINE. During induction or consolidation, 27 of 52 patients receiving LEUKINE and 35 of 47 patients receiving placebo had at least one grade 3, 4 or 5 infection (p=0.02). Twenty-five patients receiving LEUKINE and 30 patients receiving placebo experienced severe and fatal infections during induction only. There were significantly fewer deaths from infectious causes in the LEUKINE arm (3 versus 11, p=0.02). The majority of deaths in the placebo group were associated with fungal infections with pneumonia as the primary infection.
- Disease outcomes were not adversely affected by the use of LEUKINE. The proportion of patients achieving complete remission (CR) was higher in the LEUKINE group (69% as compared to 55% for the placebo group), but the difference was not significant (p=0.21). There was no significant difference in relapse rates; 12 of 36 patients who received LEUKINE and five of 26 patients who received placebo relapsed within 180 days of documented CR (p=0.26). The overall median survival was 378 days for patients receiving LEUKINE and 268 days for those on placebo (p=0.17). The study was not sized to assess the impact of LEUKINE treatment on response or survival.
Mobilization and Engraftment of PBPC
A retrospective review was conducted of data from patients with cancer undergoing collection of peripheral blood progenitor cells (PBPC) at a single transplant center. Mobilization of PBPC and myeloid reconstitution post-transplant were compared between four groups of patients (n=196) receiving LEUKINE for mobilization and a historical control group who did not receive any mobilization treatment [progenitor cells collected by leukapheresis without mobilization (n=100)]. Sequential cohorts received LEUKINE. The cohorts differed by dose (125 or 250 mcg/m2/day), route (IV over 24 hours or SC) and use of LEUKINE post-transplant. Leukaphereses were initiated for all mobilization groups after the WBC reached 10,000/mm3. Leukaphereses continued until both a minimum number of mononucleated cells (MNC) were collected (6.5 or 8.0 × 108/kg body weight) and a minimum number of phereses (5–8) were performed. Both minimum requirements varied by treatment cohort and planned conditioning regimen. If subjects failed to reach a WBC of 10,000 cells/mm3 by day five, another cytokine was substituted for LEUKINE; these subjects were all successfully leukapheresed and transplanted. The most marked mobilization and post-transplant effects were seen in patients administered the higher dose of LEUKINE (250 mcg/m2) either IV (n=63) or SC (n=41).
PBPCs from patients treated at the 250 mcg/m2/day dose had significantly higher number of granulocyte-macrophage colony-forming units (CFU-GM) than those collected without mobilization. The mean value after thawing was 11.41 × 104 CFU-GM/kg for all LEUKINE-mobilized patients, compared to 0.96 × 104/kg for the non-mobilized group. A similar difference was observed in the mean number of erythrocyte burst-forming units (BFU-E) collected (23.96 × 104/kg for patients mobilized with 250 mcg/m2 doses of LEUKINE administered SC vs. 1.63 × 104/kg for non-mobilized patients).
After transplantation, mobilized subjects had shorter times to myeloid engraftment and fewer days between transplantation and the last platelet transfusion compared to non-mobilized subjects. Neutrophil recovery (ANC >500/mm3) was more rapid in patients administered LEUKINE following PBPC transplantation with LEUKINE-mobilized cells (see TABLE 2). Mobilized patients also had fewer days to the last platelet transfusion and last RBC transfusion, and a shorter duration of hospitalization than did non-mobilized subjects. |alcohol=Alcohol-Sargramostim interaction has not been established. Talk to your doctor about the effects of taking alcohol with this medication. }}