Progesterone (oral): Difference between revisions
No edit summary |
Gerald Chi- (talk | contribs) mNo edit summary |
||
| (22 intermediate revisions by 3 users not shown) | |||
| Line 5: | Line 5: | ||
|drugClass=hormone | |drugClass=hormone | ||
|indicationType=treatment | |indicationType=treatment | ||
|indication=[[secondary amenorrhea]], and the prevention of [[endometrial hyperplasia]] in nonhysterectomized postmenopausal women who are receiving conjugated estrogens tablets | |||
|hasBlackBoxWarning=Yes | |hasBlackBoxWarning=Yes | ||
|adverseReactions= | |adverseReactions=[[abdominal pain]], [[constipation]], [[nausea]], swollen abdomen,viral disease, [[cramp]], [[musculoskeletal pain]], [[dizziness]], [[headache]], sleep disorder, [[somnolence]], [[depression]], mood swings, [[nocturia]], breast tenderness, large breast, [[pain]], post-oocyte retrieval , pain of breast, [[perineal pain]], [[vaginal discharge]], and [[fatigue]] | ||
|blackBoxWarningTitle=<span style="color:#FF0000;">WARNING: CARDIOVASCULAR DISORDERS, BREAST CANCER and PROBABLE DEMENTIA FOR ESTROGEN PLUS PROGESTIN THERAPY</span> | |blackBoxWarningTitle=<span style="color:#FF0000;">WARNING: CARDIOVASCULAR DISORDERS, BREAST CANCER and PROBABLE DEMENTIA FOR ESTROGEN PLUS PROGESTIN THERAPY</span> | ||
|blackBoxWarningBody=<i><span style="color:#FF0000;">Cardiovascular Disorders and Probable Dementia: </span></i> | |blackBoxWarningBody=<i><span style="color:#FF0000;">Cardiovascular Disorders and Probable Dementia: </span></i> | ||
*Estrogens plus progestin therapy should not be used for the prevention of cardiovascular disease or dementia. | *Estrogens plus progestin therapy should not be used for the prevention of cardiovascular disease or dementia. | ||
The Women's Health Initiative (WHI) estrogen plus progestin substudy reported increased risks of deep vein thrombosis, pulmonary embolism, stroke and myocardial infarction in postmenopausal women (50 to 79 years of age) during 5.6 years of treatment with daily oral conjugated estrogens (CE) [0.625 mg] combined with medroxyprogesterone acetate (MPA) [2.5 mg], relative to placebo. | *The Women's Health Initiative (WHI) estrogen plus progestin substudy reported increased risks of deep vein thrombosis, pulmonary embolism, stroke and myocardial infarction in postmenopausal women (50 to 79 years of age) during 5.6 years of treatment with daily oral conjugated estrogens (CE) [0.625 mg] combined with medroxyprogesterone acetate (MPA) [2.5 mg], relative to placebo. | ||
*The WHI Memory Study (WHIMS) estrogen plus progestin ancillary study of the WHI reported an increased risk of developing probable dementia in postmenopausal women 65 years of age or older during 4 years of treatment with daily CE (0.625 mg) combined with MPA (2.5 mg), relative to placebo. It is unknown whether this finding applies to younger postmenopausal women. | |||
<i><span style="color:#FF0000;">Breast Cancer: </span></i> | <i><span style="color:#FF0000;">Breast Cancer: </span></i> | ||
The WHI estrogen plus progestin substudy also demonstrated an increased risk of invasive breast cancer. | *The WHI estrogen plus progestin substudy also demonstrated an increased risk of invasive breast cancer. | ||
In the absence of comparable data, these risks should be assumed to be similar for other doses of CE and MPA, and other combinations and dosage forms of estrogens and progestins. | *In the absence of comparable data, these risks should be assumed to be similar for other doses of CE and MPA, and other combinations and dosage forms of estrogens and progestins. | ||
Progestins with estrogens should be prescribed at the lowest effective doses and for the shortest duration consistent with treatment goals and risks for the individual woman. | *Progestins with estrogens should be prescribed at the lowest effective doses and for the shortest duration consistent with treatment goals and risks for the individual woman. | ||
<!--Adult Indications and Dosage--> | <!--Adult Indications and Dosage--> | ||
<!--FDA-Labeled Indications and Dosage (Adult)--> | <!--FDA-Labeled Indications and Dosage (Adult)--> | ||
|fdaLIADAdult=Progesterone intrauterine insert (Progestasert(R)) was discontinued on 06/01/2001 | |fdaLIADAdult=====Progesterone intrauterine insert (Progestasert(R)) was discontinued on 06/01/2001)==== | ||
*Important Notes: | |||
*Before insertion of the intrauterine device containing progesterone, the patient must read and initial each section of the Patient Information Leaflet supplied with the system. The intrauterine system should be inserted only by physicians familiar with the instructions. Prior to insertion, a cervical Pap smear, tests for [[Neisseria gonorrhoeae]] and [[Chlamydia]], and a pelvic exam should be conducted. | |||
*One system containing 38 mg of progesterone should be inserted into the uterus using the inserter provided. The system should be removed and replaced every 12 months for continued effectiveness. | |||
*Patients should be advised that this product will not protect them from HIV infection or other sexually transmitted diseases. | |||
*The patient should return for a check up 3 months after insertion and at 12 months for removal and replacement of the system. | |||
*Should not be inserted until involution of the uterus is complete following abortion or child birth. | |||
====Abnormal uterine bleeding unrelated to menstrual cycle==== | |||
*Dosing Information: | |||
:*Progesterone 5 to 10 mg is injected IM daily for 6 doses. The [[bleeding]] should be expected to stop within 6 days. If the menstrual flow begins during the course of progesterone injections, therapy should be stopped. If estrogen therapy is to be used, progesterone should be initiated after 2 weeks of estrogen therapy. | |||
====Assisted reproductive technology; Adjunct - Female infertility==== | |||
*Dosing Information: | |||
:*Vaginal Gel: | |||
:*Progesterone gel (Crinone(R) 8%) 90 mg once daily is administered vaginally in women who require progesterone supplementation. In women with partial or complete ovarian failure who require progesterone replacement, a dose of 90 mg twice daily is administered. | |||
:*A desired dosage increase from the 4% gel can only be achieved by using the 8% gel rather than increasing the volume of the 4% gel. | |||
:*Vaginal Insert: | |||
:*Administer 100 mg vaginal insert vaginally 2 to 3 times a day starting the day after oocyte retrieval and continuing for up to 10 weeks total duration for women undergoing Assisted Reproductive Technology treatment for [[infertility]]. | |||
====Contraception==== | |||
====Endometrial hyperplasia; Prophylaxis==== | |||
*Dosing Information: | |||
:*Oral micronized progesterone should be given as a single daily dose in the evening, 200 mg for 12 days sequentially per 28-day cycle, to postmenopausal women with a uterus who are receiving daily conjugated estrogen tablets. | |||
==== | ====Secondary physiologic amenorrhea==== | ||
* Dosing Information | *Dosing Information: | ||
:* | :*In the treatment of [[amenorrhea]], progesterone 5 to 10 mg in oil should be administered IM daily for 6 to 8 days (Prod Info Progesterone USP, 2000). If a proliferative endometrium is produced, withdrawal [[bleeding]] should occur within 48 to 72 hours after discontinuing the progesterone. This may be followed by spontaneous normal cycles. | ||
:*Oral progesterone may be given as a single daily dose of 400 mg in the evening for 10 days. | |||
:*For [[secondary amenorrhea]], vaginal progesterone gel 4% is administered every other day up to a total of 6 doses. For those who fail to respond, a trial of 8% (90 mg) every other day up to a total of 6 doses may be used (Prod Info Crinone(R), 2000). | |||
:* | |||
<!--Off-Label Use and Dosage (Adult)--> | <!--Off-Label Use and Dosage (Adult)--> | ||
<!--Guideline-Supported Use (Adult)--> | <!--Guideline-Supported Use (Adult)--> | ||
|offLabelAdultGuideSupport= | |offLabelAdultGuideSupport=* There is limited information regarding <i>Off-Label Guideline-Supported Use</i> of {{PAGENAME}} in adult patients. | ||
* | |||
There is limited information regarding <i>Off-Label Guideline-Supported Use</i> of {{PAGENAME}} in adult patients. | |||
<!--Non–Guideline-Supported Use (Adult)--> | <!--Non–Guideline-Supported Use (Adult)--> | ||
|offLabelAdultNoGuideSupport======Premature birth of newborn, Short cervix; Prophylaxis===== | |offLabelAdultNoGuideSupport======Premature birth of newborn, Short cervix; Prophylaxis===== | ||
<!--Pediatric Indications and Dosage--> | <!--Pediatric Indications and Dosage--> | ||
<!--FDA-Labeled Indications and Dosage (Pediatric)--> | <!--FDA-Labeled Indications and Dosage (Pediatric)--> | ||
|fdaLIADPed= | |fdaLIADPed=* There is limited information regarding <i>FDA-Labeled Use</i> of {{PAGENAME}} in pediatric patients. | ||
* | |||
There is limited information regarding <i>FDA-Labeled Use</i> of {{PAGENAME}} in pediatric patients. | |||
<!--Off-Label Use and Dosage (Pediatric)--> | <!--Off-Label Use and Dosage (Pediatric)--> | ||
<!--Guideline-Supported Use (Pediatric)--> | <!--Guideline-Supported Use (Pediatric)--> | ||
|offLabelPedGuideSupport= | |offLabelPedGuideSupport=* There is limited information regarding <i>Off-Label Guideline-Supported Use</i> of {{PAGENAME}} in pediatric patients. | ||
* | |||
There is limited information regarding <i>Off-Label Guideline-Supported Use</i> of {{PAGENAME}} in pediatric patients. | |||
<!--Non–Guideline-Supported Use (Pediatric)--> | <!--Non–Guideline-Supported Use (Pediatric)--> | ||
|offLabelPedNoGuideSupport= | |offLabelPedNoGuideSupport=* There is limited information regarding <i>Off-Label Non–Guideline-Supported Use</i> of {{PAGENAME}} in pediatric patients. | ||
* | |||
There is limited information regarding <i>Off-Label Non–Guideline-Supported Use</i> of {{PAGENAME}} in pediatric patients. | |||
<!--Contraindications--> | <!--Contraindications--> | ||
|contraindications=PROMETRIUM Capsules should not be used in women with any of the following conditions: | |contraindications=*PROMETRIUM Capsules should not be used in women with any of the following conditions: | ||
:*PROMETRIUM Capsules should not be used in patients with known hypersensitivity to its ingredients. PROMETRIUM Capsules contain peanut oil and should never be used by patients allergic to peanuts. | |||
:*Undiagnosed abnormal genital [[bleeding]]. | |||
:*Known, suspected, or history of [[breast cancer]]. | |||
:*Active [[deep vein thrombosis]], [[pulmonary embolism]] or history of these conditions. | |||
:*Active [[arterial thromboembolic disease]] (for example, [[stroke]] and [[myocardial infarction]]), or a history of these conditions. | |||
:*Known liver dysfunction or disease. | |||
:*Known or suspected pregnancy. | |||
|warnings=* See BOXED WARNING. | |||
'''Cardiovascular disorders''' | |||
*An increased risk of pulmonary embolism, [[deep vein thrombosis]] (DVT), [[stroke]], and [[myocardial infarction]] has been reported with [[estrogen]] plus [[progestin]] therapy. Should any of these occur or be suspected, estrogen with progestin therapy should be discontinued immediately. | |||
*Risk factors for arterial vascular disease (for example, [[hypertension]], [[diabetes mellitus]], tobacco use, [[hypercholesterolemia]], and [[obesity]]) and/or [[venous thromboembolism]] (for example, personal history or family history of [[venous thromboembolism]] [VTE], [[obesity]], and [[systemic lupus erythematosus]]) should be managed appropriately. | |||
'''Stroke''' | |||
a. | *In the Women's Health Initiative (WHI) [[estrogen]] plus [[progestin]] substudy, a statistically significant increased risk of stroke was reported in women 50 to 79 years of age receiving daily CE (0.625 mg) plus MPA (2.5 mg) compared to women in the same age group receiving placebo (33 versus 25 per 10,000 women-years). The increase in risk was demonstrated after the first year and persisted. Should a stroke occur or be suspected, [[estrogen]] plus [[progestin]] therapy should be discontinued immediately. | ||
'''Coronary Heart Disease''' | |||
*In the WHI [[estrogen]] plus [[progestin]] substudy, there was a statistically non-significant increased risk of [[coronary heart disease]] (CHD) events (defined as nonfatal [[myocardial infarction]] [MI], [[silent MI]], or CHD death) reported in women receiving daily CE (0.625 mg) plus MPA (2.5 mg) compared to women receiving placebo (41 versus 34 per 10,000 women-years). An increase in relative risk was demonstrated in year 1 and a trend toward decreasing relative risk was reported in years 2 through 5. | |||
In | *In postmenopausal women with documented heart disease (n = 2,763, average age 66.7 years), in a controlled clinical trial of secondary prevention of cardiovascular disease (Heart and Estrogen/Progestin Replacement Study [HERS]), treatment with daily CE (0.625 mg) plus MPA (2.5 mg) demonstrated no cardiovascular benefit. During an average follow-up of 4.1 years, treatment with CE plus MPA did not reduce the overall rate of CHD events in postmenopausal women with established coronary heart disease. There were more CHD events in the CE plus MPA-treated group than in the placebo group in year 1, but not during the subsequent years. Two thousand, three hundred and twenty-one (2,321) women from the original HERS trial agreed to participate in an open-label extension of HERS, HERS II. Average follow-up in HERS II was an additional 2.7 years, for a total of 6.8 years overall. Rates of CHD events were comparable among women in the CE plus MPA group and the placebo group in HERS, HERS II, and overall. | ||
'''Venous Thromboembolism''' | |||
*In the WHI [[estrogen]] plus [[progestin]] substudy, a statistically significant 2-fold greater rate of [[VTE]] ([[DVT]] and [[pulmonary embolism]] [PE]) was reported in women receiving daily CE (0.625 mg) plus MPA (2.5 mg) compared to women receiving placebo (35 versus 17 per 10,000 women-years). Statistically significant increases in risk for both DVT (26 versus 13 per 10,000 women-years) and PE (18 versus 8 per 10,000 women-years) were also demonstrated. The increase in [[VTE]] risk was demonstrated during the first year and persisted. Should a [[VTE]] occur or be suspected, [[estrogen]] plus [[progestin]] therapy should be discontinued immediately. | |||
*If feasible, estrogens with progestins should be discontinued at least 4 to 6 weeks before surgery of the type associated with an increased risk of thromboembolism, or during periods of prolonged immobilization. | |||
'''Malignant neoplasms''' | |||
'''Breast Cancer''' | |||
a. | *The most important randomized clinical trial providing information about breast cancer in [[estrogen]] plus [[progestin]] users is the Women's Health Initiative (WHI) substudy of daily CE (0.625 mg) plus MPA (2.5 mg). After a mean follow-up of 5.6 years, the [[estrogen]] plus [[progestin]] substudy reported an increased risk of invasive breast cancer in women who took daily CE plus MPA. In this substudy, prior use of estrogen-alone or [[estrogen]] plus [[progestin]] therapy was reported by 26 percent of the women. The relative risk of invasive breast cancer was 1.24 (95 percent nCI, 1.01-1.54), and the absolute risk was 41 versus 33 cases per 10,000 women-years, for CE plus MPA compared with placebo. | ||
*Among women who reported prior use of hormone therapy, the relative risk of invasive breast cancer was 1.86, and the absolute risk was 46 versus 25 cases per 10,000 women-years, for [[estrogen]] plus [[progestin]] compared with placebo. Among women who reported no prior use of hormone therapy, the relative risk of invasive breast cancer was 1.09, and the absolute risk was 40 versus 36 cases per 10,000 women-years for CE plus MPA compared with placebo. In the same substudy, invasive breast cancers were larger, were more likely to be node positive, and were diagnosed at a more advanced stage in the CE (0.625 mg) plus MPA (2.5 mg) group compared with the placebo group. Metastatic disease was rare, with no apparent difference between the two groups. Other prognostic factors such as histologic subtype, grade and hormone receptor status did not differ between the groups. | |||
*Consistent with the WHI clinical trials, observational studies have also reported an increased risk of breast cancer for [[estrogen]] plus [[progestin]] therapy, and a smaller increased risk for estrogen-alone therapy, after several years of use. The risk increased with duration of use, and appeared to return to baseline over about 5 years after stopping treatment (only the observational studies have substantial data on risk after stopping). Observational studies also suggest that the risk of breast cancer was greater, and became apparent earlier, with [[estrogen]] plus [[progestin]] therapy as compared to estrogen-alone therapy. However, these studies have not generally found significant variation in the risk of breast cancer among different [[estrogen]] plus [[progestin]] combinations, doses, or routes of administration. | |||
*The use of [[estrogen]] plus [[progestin]] has been reported to result in an increase in abnormal mammograms requiring further evaluation. All women should receive yearly breast examinations by a healthcare provider and perform monthly breast self-examinations. In addition, mammography examinations should be scheduled based on patient age, risk factors, and prior mammogram results. | |||
'''Endometrial Cancer''' | |||
*An increased risk of [[endometrial cancer]] has been reported with the use of unopposed estrogen therapy in a woman with a uterus. The reported endometrial cancer risk among unopposed estrogen users is about 2 to 12 times greater than in non-users, and appears dependent on duration of treatment and on estrogen dose. Most studies show no significant increased risk associated with the use of estrogens for less than 1 year. The greatest risk appears associated with prolonged use, with increased risks of 15- to 24-fold for 5 to 10 years or more and this risk has been shown to persist for at least 8 to 15 years after estrogen therapy is discontinued. | |||
*Clinical surveillance of all women using [[estrogen]] plus [[progestin]] therapy is important. Adequate diagnostic measures, including directed or random endometrial sampling when indicated, should be undertaken to rule out malignancy in all cases of undiagnosed persistent or recurring abnormal genital [[bleeding]]. There is no evidence that the use of natural estrogens results in a different endometrial risk profile than synthetic estrogens of equivalent estrogen dose. Adding a progestin to estrogen therapy in postmenopausal women has been shown to reduce the risk of [[endometrial hyperplasia]], which may be a precursor to [[endometrial cancer]]. | |||
'''Ovarian Cancer''' | |||
*The WHI [[estrogen]] plus [[progestin]] substudy reported a statistically non-significant increased risk of [[ovarian cancer]]. After an average follow-up of 5.6 years, the relative risk for ovarian cancer for CE plus MPA versus placebo was 1.58 (95 percent nCI, 0.77 – 3.24). The absolute risk for CE plus MPA versus placebo was 4 versus 3 cases per 10,000 women-years. In some epidemiologic studies, the use of [[estrogen]] plus [[progestin]] and estrogen-only products, in particular for 5 or more years, has been associated with an increased risk of ovarian cancer. However, the duration of exposure associated with increased risk is not consistent across all epidemiologic studies and some report no association. | |||
'''Probable dementia''' | |||
*In the [[estrogen]] plus [[progestin]] Women's Health Initiative Memory Study (WHIMS), an ancillary study of WHI, a population of 4,532 postmenopausal women 65 to 79 years of age was randomized to daily CE (0.625 mg) plus MPA (2.5 mg) or placebo. | |||
In the estrogen plus progestin | *In the WHIMS [[estrogen]] plus [[progestin]] ancillary study, after an average follow-up of 4 years, 40 women in the CE plus MPA group and 21 women in the placebo group were diagnosed with probable dementia. The relative risk of probable dementia for [[estrogen]] plus [[progestin]] versus placebo was 2.05 (95 percent CI, 1.21-3.48). The absolute risk of probable dementia for CE plus MPA versus placebo was 45 versus 22 cases per 10,000 women-years. It is unknown whether these findings apply to younger postmenopausal women. | ||
'''Vision abnormalities''' | |||
*Retinal vascular thrombosis has been reported in patients receiving estrogen. Discontinue [[estrogen]] plus [[progestin]] therapy pending examination if there is sudden partial or complete loss of vision, or if there is a sudden onset of [[proptosis]], [[diplopia]] or [[migraine]]. If examination reveals [[papilledema]] or [[retinal vascular lesions]], [[estrogen]] plus [[progestin]] therapy should be permanently discontinued. | |||
Retinal vascular thrombosis has been reported in patients receiving estrogen. Discontinue estrogen plus progestin therapy pending examination if there is sudden partial or complete loss of vision, or if there is a sudden onset of proptosis, diplopia or migraine. If examination reveals papilledema or retinal vascular lesions, estrogen plus progestin therapy should be permanently discontinued. | |||
====Precautions==== | ====Precautions==== | ||
'''General''' | |||
'''Addition of a progestin when a woman has not had a hysterectomy''' | |||
Studies of the addition of a progestin for 10 or more days of a cycle of estrogen administration, or daily with estrogen in a continuous regimen, have reported a lowered incidence of endometrial hyperplasia than would be induced by estrogen treatment alone. Endometrial hyperplasia may be a precursor to endometrial cancer. | *Studies of the addition of a progestin for 10 or more days of a cycle of estrogen administration, or daily with estrogen in a continuous regimen, have reported a lowered incidence of [[endometrial hyperplasia]] than would be induced by estrogen treatment alone. [[Endometrial hyperplasia]] may be a precursor to [[endometrial cancer]]. | ||
There are, however, possible risks that may be associated with the use of progestins with estrogens compared with estrogen-alone regimens. These include an increased risk of breast cancer. | *There are, however, possible risks that may be associated with the use of progestins with estrogens compared with estrogen-alone regimens. These include an increased risk of breast cancer. | ||
'''Fluid Retention''' | |||
Progesterone may cause some degree of fluid retention. Women with conditions that might be influenced by this factor, such as cardiac or renal dysfunction, warrant careful observation. | *Progesterone may cause some degree of fluid retention. Women with conditions that might be influenced by this factor, such as cardiac or [[renal dysfunction]], warrant careful observation. | ||
'''Dizziness and Drowsiness''' | |||
PROMETRIUM Capsules may cause transient dizziness and drowsiness and should be used with caution when driving a motor vehicle or operating machinery. PROMETRIUM Capsules should be taken as a single daily dose at bedtime. | *PROMETRIUM Capsules may cause transient [[dizziness]] and [[drowsiness]] and should be used with caution when driving a motor vehicle or operating machinery. PROMETRIUM Capsules should be taken as a single daily dose at bedtime. | ||
'''Patient Information''' | |||
General: This product contains peanut oil and should not be used if you are allergic to peanuts. | *General: This product contains peanut oil and should not be used if you are allergic to peanuts. | ||
Physicians are advised to discuss the contents of the Patient Information leaflet with patients for whom they prescribe PROMETRIUM Capsules. | *Physicians are advised to discuss the contents of the Patient Information leaflet with patients for whom they prescribe PROMETRIUM Capsules. | ||
'''Drug-Laboratory Test Interactions''' | |||
The following laboratory results may be altered by the use of estrogen plus progestin therapy: | *The following laboratory results may be altered by the use of [[estrogen]] plus [[progestin]] therapy: | ||
:*Increased sulfobromophthalein retention and other hepatic function tests. | |||
:*Coagulation tests: increase in prothrombin factors VII, VIII, IX and X. | |||
:*Pregnanediol determination. | |||
:*Thyroid function: increase in PBI, and butanol extractable protein bound iodine and decrease in T3 uptake values. | |||
The Women's Health Initiative Study | '''The Women's Health Initiative Study''' | ||
In the Women's Health Initiative (WHI) estrogen plus progestin substudy (daily CE [0.625 mg] plus MPA [2.5 mg] versus placebo), there was a higher relative risk of nonfatal stroke and invasive breast cancer in women greater than 65 years of age. | *In the Women's Health Initiative (WHI) [[estrogen]] plus [[progestin]] substudy (daily CE [0.625 mg] plus MPA [2.5 mg] versus placebo), there was a higher relative risk of nonfatal stroke and invasive breast cancer in women greater than 65 years of age. | ||
The Women's Health Initiative Memory Study | '''The Women's Health Initiative Memory Study''' | ||
In the Women's Health Initiative Memory Study (WHIMS) of postmenopausal women 65 to 79 years of age, there was an increased risk of developing probable dementia in the estrogen plus progestin ancillary study when compared to placebo. | *In the Women's Health Initiative Memory Study (WHIMS) of postmenopausal women 65 to 79 years of age, there was an increased risk of developing probable dementia in the [[estrogen]] plus [[progestin]] ancillary study when compared to placebo. | ||
<!--Adverse Reactions--> | <!--Adverse Reactions--> | ||
<!--Clinical Trials Experience--> | <!--Clinical Trials Experience--> | ||
|clinicalTrials= | |clinicalTrials=*See BOXED WARNING, WARNINGS and PRECAUTIONS. | ||
*Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice. | |||
*In a multicenter, randomized, double-blind, placebo-controlled clinical trial, the effects of PROMETRIUM Capsules on the endometrium was studied in a total of 875 postmenopausal women. Table 6 lists adverse reactions greater than or equal to 2 percent of women who received cyclic PROMETRIUM Capsules 200 mg daily (12 days per calendar month cycle) with 0.625 mg conjugated estrogens or placebo. | |||
[[File:Progesterone table 6.png|600px|thumbnail|left]] | |||
{{clear}} | |||
'''Effects on Secondary Amenorrhea''' | |||
*In a multicenter, randomized, double-blind, placebo-controlled clinical trial, the effects of PROMETRIUM Capsules on secondary amenorrhea was studied in 49 estrogen-primed postmenopausal women. Table 7 lists adverse reactions greater than or equal to 5 percent of women who received PROMETRIUM Capsules or placebo. | |||
[[File:Progesterone table 7.png|600px|thumbnail|left]] | |||
{{clear}} | |||
*In a multicenter, parallel-group, open label postmarketing dosing study consisting of three consecutive 28-day treatment cycles, 220 premenopausal women with secondary amenorrhea were randomized to receive daily conjugated estrogens therapy (0.625 mg conjugated estrogens) and PROMETRIUM Capsules, 300 mg per day (n=113) or PROMETRIUM Capsules, 400 mg per /day (n=107) for 10 days of each treatment cycle. Overall, the most frequently reported treatment-emergent adverse reactions, reported in greater than or equal to 5 percent of subjects, were [[nausea]], [[fatigue]], [[vaginal mycosis]], [[nasopharyngitis]], [[upper respiratory tract infection]], [[headache]], [[dizziness]], [[breast tenderness]], [[abdominal distension]], [[acne]], [[dysmenorrhea]], mood swing, and [[urinary tract infection]]. | |||
|postmarketing=*The following additional adverse reactions have been reported with PROMETRIUM Capsules. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate the frequency or establish a causal relationship to drug exposure. | |||
*Genitourinary System: [[endometrial carcinoma]], [[hypospadia]], intra-uterine death, [[menorrhagia]], menstrual disorder, [[metrorrhagia]], [[ovarian cyst]], spontaneous abortion. | |||
*Cardiovascular: circulatory collapse, [[congenital heart disease]] (including [[ventricular septal defect]] and [[patent ductus arteriosus]]), [[hypertension]], [[hypotension]], [[tachycardia]]. | |||
*Gastrointestinal: [[acute pancreatitis]], [[cholestasis]], [[cholestatic hepatitis]], [[dysphagia]], [[hepatic failure]], [[hepatic necrosis]], [[hepatitis]], increased liver function tests (including alanine aminotransferase increased, aspartate aminotransferase increased, [[gamma-glutamyl transferase]] increased), [[jaundice]], swollen tongue. | |||
*Skin: [[alopecia]], [[pruritus]], [[urticaria]]. | |||
*Eyes: [[blurred vision]], [[diplopia]], [[visual disturbance]]. | |||
*Central Nervous System: [[aggression]], [[convulsion]], [[depersonalization]], depressed consciousness, [[disorientation]], [[dysarthria]], loss of consciousness, [[paresthesia]], [[sedation]], [[stupor]], [[syncope]] (with and without hypotension), [[transient ischemic attack]], suicidal ideation. | |||
*During initial therapy, a few women have experienced a constellation of many or all of the following symptoms: extreme [[dizziness]] and/or [[drowsiness]], [[blurred vision]], [[slurred speech]], difficulty walking, [[loss of consciousness]], [[vertigo]], [[confusion]], [[disorientation]], feeling drunk, and [[shortness of breath]]. | |||
*Miscellaneous: abnormal gait, [[anaphylactic]] reaction, [[arthralgia]], blood glucose increased, choking, [[cleft lip]], [[cleft palate]], difficulty walking, [[dyspnea]], face [[edema]] feeling abnormal, feeling drunk, [[hypersensitivity]], [[asthma]], [[muscle cramp]], throat tightness, [[tinnitus]], [[vertigo]], weight decreased, weight increased. | |||
|drugInteractions=<!--Use in Specific Populations--> | |||
|FDAPregCat=B | |||
|useInPregnancyFDA=*PROMETRIUM Capsules should not be used during pregnancy. | |||
Pregnancy Category B: Reproductive studies have been performed in mice at doses up to 9 times the human oral dose, in rats at doses up to 44 times the human oral dose, in rabbits at a dose of 10 mcg/day delivered locally within the uterus by an implanted device, in guinea pigs at doses of approximately one-half the human oral dose and in rhesus monkeys at doses approximately the human dose, all based on body surface area, and have revealed little or no evidence of impaired fertility or harm to the fetus due to progesterone. | |||
|useInPregnancyAUS=* '''Australian Drug Evaluation Committee (ADEC) Pregnancy Category''' | |||
*There is no Australian Drug Evaluation Committee (ADEC) guidance on usage of {{PAGENAME}} in women who are pregnant. | |||
|useInLaborDelivery=* There is no FDA guidance on use of {{PAGENAME}} during labor and delivery. | |||
|useInNursing=* Detectable amounts of progestin have been identified in the milk of nursing women receiving progestins. Caution should be exercised when PROMETRIUM Capsules are administered to a nursing woman. | |||
|useInPed=* PROMETRIUM Capsules are not indicated in children. Clinical studies have not been conducted in the pediatric population. | |||
|useInGeri=* There have not been sufficient numbers of geriatric women involved in clinical studies utilizing PROMETRIUM Capsules to determine whether those over 65 years of age differ from younger subjects in their response to PROMETRIUM Capsules. | |||
|useInGender=* There is no FDA guidance on the use of {{PAGENAME}} with respect to specific gender populations. | |||
|useInRace=* There is no FDA guidance on the use of {{PAGENAME}} with respect to specific racial populations. | |||
|useInRenalImpair=* There is no FDA guidance on the use of {{PAGENAME}} in patients with renal impairment. | |||
|useInHepaticImpair=* There is no FDA guidance on the use of {{PAGENAME}} in patients with hepatic impairment. | |||
|useInReproPotential=* There is no FDA guidance on the use of {{PAGENAME}} in women of reproductive potentials and males. | |||
|useInImmunocomp=* There is no FDA guidance one the use of {{PAGENAME}} in patients who are immunocompromised. | |||
<!--Administration and Monitoring--> | |||
|administration='''Prevention of Endometrial Hyperplasia''' | |||
*PROMETRIUM Capsules should be given as a single daily dose at bedtime, 200 mg orally for 12 days sequentially per 28-day cycle, to a postmenopausal woman with a uterus who is receiving daily conjugated estrogens tablets. | |||
'''Treatment of Secondary Amenorrhea''' | |||
*PROMETRIUM Capsules may be given as a single daily dose of 400 mg at bedtime for 10 days. | |||
*Some women may experience difficulty swallowing PROMETRIUM Capsules. For these women, PROMETRIUM Capsules should be taken with a glass of water while in the standing position. | |||
|monitoring=* There is limited information regarding <i>Monitoring</i> of {{PAGENAME}} in the drug label. | |||
| | |||
* Description | * Description | ||
<!--IV Compatibility--> | <!--IV Compatibility--> | ||
|IVCompat=There is limited information regarding <i>IV Compatibility</i> of {{PAGENAME}} in the drug label. | |IVCompat=* There is limited information regarding <i>IV Compatibility</i> of {{PAGENAME}} in the drug label. | ||
<!--Overdosage--> | <!--Overdosage--> | ||
|overdose=* No studies on overdosage have been conducted in humans. In the case of overdosage, PROMETRIUM Capsules should be discontinued and the patient should be treated symptomatically. | |||
|drugBox=[[File:Progesterone image.png|600px|thumbnail|left]] | |drugBox=[[File:Progesterone image.png|600px|thumbnail|left]] | ||
{{clear}} | {{clear}} | ||
|mechAction=* | |mechAction=* | ||
|structure=PROMETRIUM (progesterone, USP) Capsules contain micronized progesterone for oral administration. Progesterone has a molecular weight of 314.47 and a molecular formula of C21H30O2. Progesterone (pregn-4-ene-3, 20-dione) is a white or creamy white, odorless, crystalline powder practically insoluble in water, soluble in alcohol, acetone and dioxane and sparingly soluble in vegetable oils, stable in air, melting between 126° and 131°C. The structural formula is: | |structure=* PROMETRIUM (progesterone, USP) Capsules contain micronized progesterone for oral administration. Progesterone has a molecular weight of 314.47 and a molecular formula of C21H30O2. Progesterone (pregn-4-ene-3, 20-dione) is a white or creamy white, odorless, crystalline powder practically insoluble in water, soluble in alcohol, acetone and dioxane and sparingly soluble in vegetable oils, stable in air, melting between 126° and 131°C. The structural formula is: | ||
[[File:Progesterone structure.jpg|600px|thumbnail|left]] | [[File:Progesterone structure.jpg|600px|thumbnail|left]] | ||
{{clear}} | {{clear}} | ||
Progesterone is synthesized from a starting material from a plant source and is chemically identical to progesterone of human ovarian origin. PROMETRIUM Capsules are available in multiple strengths to afford dosage flexibility for optimum management. PROMETRIUM Capsules contain 100 mg or 200 mg micronized progesterone. | * Progesterone is synthesized from a starting material from a plant source and is chemically identical to progesterone of human ovarian origin. PROMETRIUM Capsules are available in multiple strengths to afford dosage flexibility for optimum management. PROMETRIUM Capsules contain 100 mg or 200 mg micronized progesterone. | ||
The inactive ingredients for PROMETRIUM Capsules 100 mg include: peanut oil NF, gelatin NF, glycerin USP, lecithin NF, titanium dioxide USP, FD&C Red No. 40, and D&C Yellow No. 10. | * The inactive ingredients for PROMETRIUM Capsules 100 mg include: peanut oil NF, gelatin NF, glycerin USP, lecithin NF, titanium dioxide USP, FD&C Red No. 40, and D&C Yellow No. 10. | ||
The inactive ingredients for PROMETRIUM Capsules 200 mg include: peanut oil NF, gelatin NF, glycerin USP, lecithin NF, titanium dioxide USP, D&C Yellow No. 10, and FD&C Yellow No. 6. | * The inactive ingredients for PROMETRIUM Capsules 200 mg include: peanut oil NF, gelatin NF, glycerin USP, lecithin NF, titanium dioxide USP, D&C Yellow No. 10, and FD&C Yellow No. 6. | ||
|PD=There is limited information regarding <i>Pharmacodynamics</i> of {{PAGENAME}} in the drug label. | |PD=* There is limited information regarding <i>Pharmacodynamics</i> of {{PAGENAME}} in the drug label. | ||
<!--Pharmacokinetics--> | <!--Pharmacokinetics--> | ||
|PK=PROMETRIUM Capsules are an oral dosage form of micronized progesterone which is chemically identical to progesterone of ovarian origin. The oral bioavailability of progesterone is increased through micronization. | |PK=* PROMETRIUM Capsules are an oral dosage form of micronized progesterone which is chemically identical to progesterone of ovarian origin. The oral bioavailability of progesterone is increased through micronization. | ||
Pharmacokinetics | '''Pharmacokinetics''' | ||
'''Absorption''' | |||
After oral administration of progesterone as a micronized soft-gelatin capsule formulation, maximum serum concentrations were attained within 3 hours. The absolute bioavailability of micronized progesterone is not known. Table 1 summarizes the mean pharmacokinetic parameters in postmenopausal women after five oral daily doses of PROMETRIUM Capsules 100 mg as a micronized soft-gelatin capsule formulation. | *After oral administration of progesterone as a micronized soft-gelatin capsule formulation, maximum serum concentrations were attained within 3 hours. The absolute bioavailability of micronized progesterone is not known. Table 1 summarizes the mean pharmacokinetic parameters in postmenopausal women after five oral daily doses of PROMETRIUM Capsules 100 mg as a micronized soft-gelatin capsule formulation. | ||
[[File:Progesterone table 1.png|600px|thumbnail|left]] | [[File:Progesterone table 1.png|600px|thumbnail|left]] | ||
{{clear}} | {{clear}} | ||
Serum progesterone concentrations appeared linear and dose proportional following multiple dose administration of PROMETRIUM Capsules 100 mg over the dose range 100 mg per day to 300 mg per day in postmenopausal women. Although doses greater than 300 mg per day were not studied in females, serum concentrations from a study in male volunteers appeared linear and dose proportional between 100 mg per day and 400 mg per day. The pharmacokinetic parameters in male volunteers were generally consistent with those seen in postmenopausal women. | *Serum progesterone concentrations appeared linear and dose proportional following multiple dose administration of PROMETRIUM Capsules 100 mg over the dose range 100 mg per day to 300 mg per day in postmenopausal women. Although doses greater than 300 mg per day were not studied in females, serum concentrations from a study in male volunteers appeared linear and dose proportional between 100 mg per day and 400 mg per day. The pharmacokinetic parameters in male volunteers were generally consistent with those seen in postmenopausal women. | ||
'''Distribution''' | |||
Progesterone is approximately 96 percent to 99 percent bound to serum proteins, primarily to serum albumin (50 to 54 percent) and transcortin (43 to 48 percent). | *Progesterone is approximately 96 percent to 99 percent bound to serum proteins, primarily to serum albumin (50 to 54 percent) and transcortin (43 to 48 percent). | ||
'''Metabolism''' | |||
Progesterone is metabolized primarily by the liver largely to pregnanediols and pregnanolones. Pregnanediols and pregnanolones are conjugated in the liver to glucuronide and sulfate metabolites. Progesterone metabolites which are excreted in the bile may be deconjugated and may be further metabolized in the intestine via reduction, dehydroxylation, and epimerization. | *Progesterone is metabolized primarily by the liver largely to pregnanediols and pregnanolones. Pregnanediols and pregnanolones are conjugated in the liver to glucuronide and sulfate metabolites. Progesterone metabolites which are excreted in the bile may be deconjugated and may be further metabolized in the intestine via reduction, dehydroxylation, and epimerization. | ||
'''Excretion''' | |||
The glucuronide and sulfate conjugates of pregnanediol and pregnanolone are excreted in the bile and urine. Progesterone metabolites are eliminated mainly by the kidneys. Progesterone metabolites which are excreted in the bile may undergo enterohepatic recycling or may be excreted in the feces. | *The glucuronide and sulfate conjugates of pregnanediol and pregnanolone are excreted in the bile and urine. Progesterone metabolites are eliminated mainly by the kidneys. Progesterone metabolites which are excreted in the bile may undergo enterohepatic recycling or may be excreted in the feces. | ||
'''Special Populations''' | |||
The pharmacokinetics of PROMETRIUM Capsules have not been assessed in low body weight or obese patients. | *The pharmacokinetics of PROMETRIUM Capsules have not been assessed in low body weight or obese patients. | ||
Hepatic Insufficiency: The effect of hepatic impairment on the pharmacokinetics of PROMETRIUM Capsules has not been studied. | *Hepatic Insufficiency: The effect of hepatic impairment on the pharmacokinetics of PROMETRIUM Capsules has not been studied. | ||
Renal Insufficiency: The effect of renal impairment on the pharmacokinetics of PROMETRIUM Capsules has not been studied. | *Renal Insufficiency: The effect of renal impairment on the pharmacokinetics of PROMETRIUM Capsules has not been studied. | ||
'''Food–Drug Interaction''' | |||
Concomitant food ingestion increased the bioavailability of PROMETRIUM Capsules relative to a fasting state when administered to postmenopausal women at a dose of 200 mg. | *Concomitant food ingestion increased the bioavailability of PROMETRIUM Capsules relative to a fasting state when administered to postmenopausal women at a dose of 200 mg. | ||
'''Drug Interactions''' | |||
The metabolism of progesterone by human liver microsomes was inhibited by ketoconazole (IC50 < 0.1 μM). Ketoconazole is a known inhibitor of cytochrome P450 3A4, hence these data suggest that ketoconazole or other known inhibitors of this enzyme may increase the bioavailability of progesterone. The clinical relevance of the in vitro findings is unknown. | *The metabolism of progesterone by human liver microsomes was inhibited by ketoconazole (IC50 < 0.1 μM). Ketoconazole is a known inhibitor of cytochrome P450 3A4, hence these data suggest that ketoconazole or other known inhibitors of this enzyme may increase the bioavailability of progesterone. The clinical relevance of the in vitro findings is unknown. | ||
Coadministration of conjugated estrogens and PROMETRIUM Capsules to 29 postmenopausal women over a 12-day period resulted in an increase in total estrone concentrations (Cmax 3.68 ng/mL to 4.93 ng/mL) and total equilin concentrations (Cmax 2.27 ng/mL to 3.22 ng/mL) and a decrease in circulating 17β estradiol concentrations (Cmax 0.037 ng/mL to 0.030 ng/mL). The half-life of the conjugated estrogens was similar with coadministration of PROMETRIUM Capsules. Table 2 summarizes the pharmacokinetic parameters. | *Coadministration of conjugated estrogens and PROMETRIUM Capsules to 29 postmenopausal women over a 12-day period resulted in an increase in total estrone concentrations (Cmax 3.68 ng/mL to 4.93 ng/mL) and total equilin concentrations (Cmax 2.27 ng/mL to 3.22 ng/mL) and a decrease in circulating 17β estradiol concentrations (Cmax 0.037 ng/mL to 0.030 ng/mL). The half-life of the conjugated estrogens was similar with coadministration of PROMETRIUM Capsules. Table 2 summarizes the pharmacokinetic parameters. | ||
[[File:Progesterone table 2.png|600px|thumbnail|left]] | [[File:Progesterone table 2.png|600px|thumbnail|left]] | ||
{{clear}} | {{clear}} | ||
|nonClinToxic='''Carcinogenesis, Mutagenesis, Impairment of Fertility''' | |||
*Progesterone has not been tested for carcinogenicity in animals by the oral route of administration. When implanted into female mice, progesterone produced mammary carcinomas, ovarian granulosa cell tumors and endometrial stromal sarcomas. In dogs, long-term intramuscular injections produced nodular hyperplasia and benign and malignant mammary tumors. Subcutaneous or intramuscular injections of progesterone decreased the latency period and increased the incidence of mammary tumors in rats previously treated with a chemical carcinogen. | |||
*Progesterone did not show evidence of genotoxicity in in vitro studies for point mutations or for chromosomal damage. In vivo studies for chromosome damage have yielded positive results in mice at oral doses of 1000 mg/kg and 2000 mg/kg. Exogenously administered progesterone has been shown to inhibit ovulation in a number of species and it is expected that high doses given for an extended duration would impair fertility until the cessation of treatment. | |||
|clinicalStudies='''Effects on the endometrium''' | |||
Progesterone | |||
*In a randomized, double-blind clinical trial, 358 postmenopausal women, each with an intact uterus, received treatment for up to 36 months. The treatment groups were: PROMETRIUM Capsules at the dose of 200 mg per day for 12 days per 28-day cycle in combination with conjugated estrogens 0.625 mg per day (n=120); conjugated estrogens 0.625 mg per day only (n=119); or placebo (n=119). The subjects in all three treatment groups were primarily Caucasian women (87 percent or more of each group). The results for the incidence of endometrial hyperplasia in women receiving up to 3 years of treatment are shown in Table 3. A comparison of the PROMETRIUM Capsules plus conjugated estrogens treatment group to the conjugated estrogens only group showed a significantly lower rate of hyperplasia (6 percent combination product versus 64 percent estrogen alone) in the PROMETRIUM Capsules plus conjugated estrogens treatment group throughout 36 months of treatment. | |||
In a randomized, double-blind clinical trial, 358 postmenopausal women, each with an intact uterus, received treatment for up to 36 months. The treatment groups were: PROMETRIUM Capsules at the dose of 200 mg per day for 12 days per 28-day cycle in combination with conjugated estrogens 0.625 mg per day (n=120); conjugated estrogens 0.625 mg per day only (n=119); or placebo (n=119). The subjects in all three treatment groups were primarily Caucasian women (87 percent or more of each group). The results for the incidence of endometrial hyperplasia in women receiving up to 3 years of treatment are shown in Table 3. A comparison of the PROMETRIUM Capsules plus conjugated estrogens treatment group to the conjugated estrogens only group showed a significantly lower rate of hyperplasia (6 percent combination product versus 64 percent estrogen alone) in the PROMETRIUM Capsules plus conjugated estrogens treatment group throughout 36 months of treatment. | |||
[[File:Progesterone table 3.png|600px|thumbnail|left]] | [[File:Progesterone table 3.png|600px|thumbnail|left]] | ||
{{clear}} | {{clear}} | ||
The times to diagnosis of endometrial hyperplasia over 36 months of treatment are shown in Figure 1. This figure illustrates graphically that the proportion of patients with hyperplasia was significantly greater for the conjugated estrogens group (64 percent) compared to the conjugated estrogens plus PROMETRIUM Capsules group (6 percent). | *The times to diagnosis of endometrial hyperplasia over 36 months of treatment are shown in Figure 1. This figure illustrates graphically that the proportion of patients with hyperplasia was significantly greater for the conjugated estrogens group (64 percent) compared to the conjugated estrogens plus PROMETRIUM Capsules group (6 percent). | ||
[[File:Progesterone fig 1.png|600px|thumbnail|left]] | [[File:Progesterone fig 1.png|600px|thumbnail|left]] | ||
{{clear}} | {{clear}} | ||
The discontinuation rates due to hyperplasia over the 36 months of treatment are as shown in Table 4. For any degree of hyperplasia, the discontinuation rate for patients who received conjugated estrogens plus PROMETRIUM Capsules was similar to that of the placebo only group, while the discontinuation rate for patients who received conjugated estrogens alone was significantly higher. Women who permanently discontinued treatment due to hyperplasia were similar in demographics to the overall study population. | *The discontinuation rates due to hyperplasia over the 36 months of treatment are as shown in Table 4. For any degree of hyperplasia, the discontinuation rate for patients who received conjugated estrogens plus PROMETRIUM Capsules was similar to that of the placebo only group, while the discontinuation rate for patients who received conjugated estrogens alone was significantly higher. Women who permanently discontinued treatment due to hyperplasia were similar in demographics to the overall study population. | ||
[[File:Progesterone table 4.png|600px|thumbnail|left]] | [[File:Progesterone table 4.png|600px|thumbnail|left]] | ||
{{clear}} | {{clear}} | ||
Effects on secondary amenorrhea | '''Effects on secondary amenorrhea''' | ||
In a single-center, randomized, double-blind clinical study that included premenopausal women with secondary amenorrhea for at least 90 days, administration of 10 days of PROMETRIUM Capsules therapy resulted in 80 percent of women experiencing withdrawal bleeding within 7 days of the last dose of PROMETRIUM Capsules, 300 mg per day (n=20), compared to 10 percent of women experiencing withdrawal bleeding in the placebo group (n=21). | *In a single-center, randomized, double-blind clinical study that included premenopausal women with [[secondary amenorrhea]] for at least 90 days, administration of 10 days of PROMETRIUM Capsules therapy resulted in 80 percent of women experiencing withdrawal [[bleeding]] within 7 days of the last dose of PROMETRIUM Capsules, 300 mg per day (n=20), compared to 10 percent of women experiencing withdrawal [[bleeding]] in the placebo group (n=21). | ||
In a multicenter, parallel-group, open label, postmarketing dosing study that included premenopausal women with secondary amenorrhea for at least 90 days, administration of 10 days of PROMETRIUM Capsules during two 28-day treatment cycles, 300 mg per day (n=107) or 400 mg per day (n=99), resulted in 73.8 percent and 76.8 percent of women, respectively, experiencing withdrawal bleeding. | *In a multicenter, parallel-group, open label, postmarketing dosing study that included premenopausal women with secondary amenorrhea for at least 90 days, administration of 10 days of PROMETRIUM Capsules during two 28-day treatment cycles, 300 mg per day (n=107) or 400 mg per day (n=99), resulted in 73.8 percent and 76.8 percent of women, respectively, experiencing withdrawal [[bleeding]]. | ||
The rate of secretory transformation was evaluated in a multicenter, randomized, double-blind clinical study in estrogen-primed postmenopausal women. PROMETRIUM Capsules administered orally for 10 days at 400 mg per day (n=22) induced complete secretory changes in the endometrium in 45 percent of women compared to 0 percent in the placebo group (n=23). | *The rate of secretory transformation was evaluated in a multicenter, randomized, double-blind clinical study in estrogen-primed postmenopausal women. PROMETRIUM Capsules administered orally for 10 days at 400 mg per day (n=22) induced complete secretory changes in the endometrium in 45 percent of women compared to 0 percent in the placebo group (n=23). | ||
A second multicenter, parallel-group, open label postmarketing dosing study in premenopausal women with secondary amenorrhea for at least 90 days also evaluated the rate of secretory transformation. All subjects received daily oral conjugated estrogens over 3 consecutive 28-day treatment cycles and PROMETRIUM Capsules, 300 mg per day (n=107) or 400 mg per day (n=99) for 10 days of each treatment cycle. The rate of complete secretory transformation was 21.5 percent and 28.3 percent, respectively. | *A second multicenter, parallel-group, open label postmarketing dosing study in premenopausal women with secondary amenorrhea for at least 90 days also evaluated the rate of secretory transformation. All subjects received daily oral conjugated estrogens over 3 consecutive 28-day treatment cycles and PROMETRIUM Capsules, 300 mg per day (n=107) or 400 mg per day (n=99) for 10 days of each treatment cycle. The rate of complete secretory transformation was 21.5 percent and 28.3 percent, respectively. | ||
Women's Health Initiative Studies | '''Women's Health Initiative Studies''' | ||
The Women's Health Initiative (WHI) enrolled approximately 27,000 predominantly healthy postmenopausal women in two substudies to assess the risks and benefits of daily oral conjugated estrogens (CE) [0.625 mg]-alone or in combination with medroxyprogesterone acetate (MPA) [2.5 mg] compared to placebo in the prevention of certain chronic diseases. The primary endpoint was the incidence of coronary heart disease [(CHD) defined as nonfatal myocardial infarction (MI), silent MI and CHD death], with invasive breast cancer as the primary adverse outcome. A “global index” included the earliest occurrence of CHD, invasive breast cancer, stroke, pulmonary embolism (PE), endometrial cancer (only in the CE plus MPA substudy), colorectal cancer, hip fracture, or death due to other cause. These sub studies did not evaluate the effects of CE–alone or CE plus MPA on menopausal symptoms. | *The Women's Health Initiative (WHI) enrolled approximately 27,000 predominantly healthy postmenopausal women in two substudies to assess the risks and benefits of daily oral conjugated estrogens (CE) [0.625 mg]-alone or in combination with [[medroxyprogesterone acetate]] (MPA) [2.5 mg] compared to placebo in the prevention of certain chronic diseases. The primary endpoint was the incidence of coronary heart disease [(CHD) defined as nonfatal [[myocardial infarction]] (MI), silent MI and CHD death], with invasive breast cancer as the primary adverse outcome. A “global index” included the earliest occurrence of CHD, invasive [[breast cancer]], [[stroke]], [[pulmonary embolism]] (PE), [[endometrial cancer]] (only in the CE plus MPA substudy), [[colorectal cancer]], hip fracture, or death due to other cause. These sub studies did not evaluate the effects of CE–alone or CE plus MPA on menopausal symptoms. | ||
WHI | '''WHI [[estrogen]] plus [[progestin]] Substudy''' | ||
The WHI estrogen plus progestin substudy was stopped early. According to the predefined stopping rule, after an average follow-up of 5.6 years of treatment, the increased risk of breast cancer and cardiovascular events exceeded the specified benefits included in the “global index.” The absolute excess risk of events in the “global index” was 19 per 10,000 women-years. | *The WHI [[estrogen]] plus [[progestin]] substudy was stopped early. According to the predefined stopping rule, after an average follow-up of 5.6 years of treatment, the increased risk of breast cancer and cardiovascular events exceeded the specified benefits included in the “global index.” The absolute excess risk of events in the “global index” was 19 per 10,000 women-years. | ||
For those outcomes included in the WHI “global index” that reached statistical significance after 5.6 years of follow-up, the absolute excess risks per 10,000 women-years in the group treated with CE plus MPA were 7 more CHD events, 8 more strokes, 10 more PEs, and 8 more invasive breast cancers, while the absolute risk reductions per 10,000 women-years were 6 fewer colorectal cancers and 5 fewer hip fractures. | *For those outcomes included in the WHI “global index” that reached statistical significance after 5.6 years of follow-up, the absolute excess risks per 10,000 women-years in the group treated with CE plus MPA were 7 more CHD events, 8 more strokes, 10 more PEs, and 8 more invasive breast cancers, while the absolute risk reductions per 10,000 women-years were 6 fewer colorectal cancers and 5 fewer hip fractures. | ||
Results of the estrogen plus progestin substudy, which included 16,608 women (average 63 years of age, range 50 to 79; 83.9 percent White, 6.8 percent Black, 5.4 percent Hispanic, 3.9 percent Other) are presented in Table 5. These results reflect centrally adjudicated data after an average follow-up of 5.6 years. | *Results of the [[estrogen]] plus [[progestin]] substudy, which included 16,608 women (average 63 years of age, range 50 to 79; 83.9 percent White, 6.8 percent Black, 5.4 percent Hispanic, 3.9 percent Other) are presented in Table 5. These results reflect centrally adjudicated data after an average follow-up of 5.6 years. | ||
[[File:Progesterone table 5.png|600px|thumbnail|left]] | [[File:Progesterone table 5.png|600px|thumbnail|left]] | ||
{{clear}} | {{clear}} | ||
Timing of the initiation of estrogen plus progestin therapy relative to the start of menopause may affect the overall risk benefit profile. The WHI estrogen plus progestin substudy stratified for age showed in women 50 to 59 years of age a non-significant trend toward reducing risk of overall mortality [hazard ratio (HR) 0.69 (95 percent CI, 0.44-1.07)]. | *Timing of the initiation of [[estrogen]] plus [[progestin]] therapy relative to the start of menopause may affect the overall risk benefit profile. The WHI [[estrogen]] plus [[progestin]] substudy stratified for age showed in women 50 to 59 years of age a non-significant trend toward reducing risk of overall mortality [hazard ratio (HR) 0.69 (95 percent CI, 0.44-1.07)]. | ||
Women's Health Initiative Memory Study | '''Women's Health Initiative Memory Study''' | ||
The estrogen plus progestin Women's Health Initiative Memory Study (WHIMS), an ancillary study of WHI, enrolled 4,532 predominantly healthy postmenopausal women 65 years of age and older (47 percent were 65 to 69 years of age; 35 percent were 70 to 74 years of age; and 18 percent were 75 years of age and older) to evaluate the effects of daily CE (0.625 mg) plus MPA (2.5 mg) on the incidence of probable dementia (primary outcome) compared to placebo. | *The [[estrogen]] plus [[progestin]] Women's Health Initiative Memory Study (WHIMS), an ancillary study of WHI, enrolled 4,532 predominantly healthy postmenopausal women 65 years of age and older (47 percent were 65 to 69 years of age; 35 percent were 70 to 74 years of age; and 18 percent were 75 years of age and older) to evaluate the effects of daily CE (0.625 mg) plus MPA (2.5 mg) on the incidence of probable dementia (primary outcome) compared to placebo. | ||
After an average follow-up of 4 years, the relative risk of probable dementia for CE plus MPA versus placebo was 2.05 (95 percent CI, 1.21 – 3.48). The absolute risk of probable dementia for CE plus MPA versus placebo was 45 versus 22 per 10,000 women-years. Probable dementia as defined in this study included Alzheimer's disease (AD), vascular dementia (VaD) and mixed type (having features of both AD and VaD). The most common classification of probable dementia in the treatment group and the placebo group was AD. Since the ancillary study was conducted in women 65 to 79 years of age, it is unknown whether these findings apply to younger postmenopausal women. ( | *After an average follow-up of 4 years, the relative risk of probable dementia for CE plus MPA versus placebo was 2.05 (95 percent CI, 1.21 – 3.48). The absolute risk of probable dementia for CE plus MPA versus placebo was 45 versus 22 per 10,000 women-years. Probable dementia as defined in this study included [[Alzheimer's disease]] (AD), [[vascular dementia]] (VaD) and mixed type (having features of both AD and VaD). The most common classification of probable dementia in the treatment group and the placebo group was AD. Since the ancillary study was conducted in women 65 to 79 years of age, it is unknown whether these findings apply to younger postmenopausal women. | ||
|howSupplied=*PROMETRIUM (progesterone, USP) Capsules 100 mg are round, peach-colored capsules branded with black imprint “SV.” | |||
*NDC 0032-1708-01 (Bottle of 100) | |||
*PROMETRIUM (progesterone, USP) Capsules 200 mg are oval, pale yellow-colored capsules branded with black imprint “SV2.” | |||
*NDC 0032-1711-01 (Bottle of 100) | |||
|storage=* Store at 25°C (77°F); excursions permitted to 15° to 30°C (59° to 86°F) [See USP Controlled Room Temperature]. | |||
*Protect from excessive moisture. | |||
*Dispense in tight, light-resistant container as defined in USP/NF, accompanied by a Patient Insert. | |||
*Keep out of reach of children. | |||
|packLabel=[[File:Progesterone pdp.jpg|600px|thumbnail|left]] | |packLabel=[[File:Progesterone pdp.jpg|600px|thumbnail|left]] | ||
{{clear}} | |||
[[File:Progesterone pdp2.jpg|600px|thumbnail|left]] | |||
{{clear}} | {{clear}} | ||
[[File:Progesterone label.png|600px|thumbnail|left]] | [[File:Progesterone label.png|600px|thumbnail|left]] | ||
{{clear}} | {{clear}} | ||
|fdaPatientInfo=General: This product contains peanut oil and should not be used if you are allergic to peanuts. | |fdaPatientInfo=*General: This product contains peanut oil and should not be used if you are allergic to peanuts. | ||
Physicians are advised to discuss the contents of the Patient Information leaflet with patients for whom they prescribe PROMETRIUM Capsules. | *Physicians are advised to discuss the contents of the Patient Information leaflet with patients for whom they prescribe PROMETRIUM Capsules. | ||
[[File:Progesterone medication guide.png|600px|thumbnail|left]] | [[File:Progesterone medication guide.png|600px|thumbnail|left]] | ||
| Line 555: | Line 416: | ||
<!--Brand Names--> | <!--Brand Names--> | ||
|brandNames= | |brandNames=Crinone, | ||
Prochieve, | |||
Prometrium, | |||
|lookAlike= | Endometrin. | ||
|lookAlike= | |||
<!--Drug Shortage Status--> | <!--Drug Shortage Status--> | ||
| Line 566: | Line 428: | ||
|fileName=No image.jpg | |fileName=No image.jpg | ||
}} | }} | ||
[[Category:Drug]] | [[Category:Drug]] | ||
Latest revision as of 11:12, 25 May 2015
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Deepika Beereddy, MBBS [2]
Disclaimer
WikiDoc MAKES NO GUARANTEE OF VALIDITY. WikiDoc is not a professional health care provider, nor is it a suitable replacement for a licensed healthcare provider. WikiDoc is intended to be an educational tool, not a tool for any form of healthcare delivery. The educational content on WikiDoc drug pages is based upon the FDA package insert, National Library of Medicine content and practice guidelines / consensus statements. WikiDoc does not promote the administration of any medication or device that is not consistent with its labeling. Please read our full disclaimer here.
Black Box Warning
|
WARNING: CARDIOVASCULAR DISORDERS, BREAST CANCER and PROBABLE DEMENTIA FOR ESTROGEN PLUS PROGESTIN THERAPY
See full prescribing information for complete Boxed Warning.
Cardiovascular Disorders and Probable Dementia:
Breast Cancer:
|
Overview
Progesterone (oral) is a hormone that is FDA approved for the treatment of secondary amenorrhea, and the prevention of endometrial hyperplasia in nonhysterectomized postmenopausal women who are receiving conjugated estrogens tablets. There is a Black Box Warning for this drug as shown here. Common adverse reactions include abdominal pain, constipation, nausea, swollen abdomen,viral disease, cramp, musculoskeletal pain, dizziness, headache, sleep disorder, somnolence, depression, mood swings, nocturia, breast tenderness, large breast, pain, post-oocyte retrieval , pain of breast, perineal pain, vaginal discharge, and fatigue.
Adult Indications and Dosage
FDA-Labeled Indications and Dosage (Adult)
Progesterone intrauterine insert (Progestasert(R)) was discontinued on 06/01/2001)
- Important Notes:
- Before insertion of the intrauterine device containing progesterone, the patient must read and initial each section of the Patient Information Leaflet supplied with the system. The intrauterine system should be inserted only by physicians familiar with the instructions. Prior to insertion, a cervical Pap smear, tests for Neisseria gonorrhoeae and Chlamydia, and a pelvic exam should be conducted.
- One system containing 38 mg of progesterone should be inserted into the uterus using the inserter provided. The system should be removed and replaced every 12 months for continued effectiveness.
- Patients should be advised that this product will not protect them from HIV infection or other sexually transmitted diseases.
- The patient should return for a check up 3 months after insertion and at 12 months for removal and replacement of the system.
- Should not be inserted until involution of the uterus is complete following abortion or child birth.
- Dosing Information:
- Progesterone 5 to 10 mg is injected IM daily for 6 doses. The bleeding should be expected to stop within 6 days. If the menstrual flow begins during the course of progesterone injections, therapy should be stopped. If estrogen therapy is to be used, progesterone should be initiated after 2 weeks of estrogen therapy.
Assisted reproductive technology; Adjunct - Female infertility
- Dosing Information:
- Vaginal Gel:
- Progesterone gel (Crinone(R) 8%) 90 mg once daily is administered vaginally in women who require progesterone supplementation. In women with partial or complete ovarian failure who require progesterone replacement, a dose of 90 mg twice daily is administered.
- A desired dosage increase from the 4% gel can only be achieved by using the 8% gel rather than increasing the volume of the 4% gel.
- Vaginal Insert:
- Administer 100 mg vaginal insert vaginally 2 to 3 times a day starting the day after oocyte retrieval and continuing for up to 10 weeks total duration for women undergoing Assisted Reproductive Technology treatment for infertility.
Contraception
Endometrial hyperplasia; Prophylaxis
- Dosing Information:
- Oral micronized progesterone should be given as a single daily dose in the evening, 200 mg for 12 days sequentially per 28-day cycle, to postmenopausal women with a uterus who are receiving daily conjugated estrogen tablets.
Secondary physiologic amenorrhea
- Dosing Information:
- In the treatment of amenorrhea, progesterone 5 to 10 mg in oil should be administered IM daily for 6 to 8 days (Prod Info Progesterone USP, 2000). If a proliferative endometrium is produced, withdrawal bleeding should occur within 48 to 72 hours after discontinuing the progesterone. This may be followed by spontaneous normal cycles.
- Oral progesterone may be given as a single daily dose of 400 mg in the evening for 10 days.
- For secondary amenorrhea, vaginal progesterone gel 4% is administered every other day up to a total of 6 doses. For those who fail to respond, a trial of 8% (90 mg) every other day up to a total of 6 doses may be used (Prod Info Crinone(R), 2000).
Off-Label Use and Dosage (Adult)
Guideline-Supported Use
- There is limited information regarding Off-Label Guideline-Supported Use of Progesterone (oral) in adult patients.
Non–Guideline-Supported Use
Premature birth of newborn, Short cervix; Prophylaxis
Pediatric Indications and Dosage
FDA-Labeled Indications and Dosage (Pediatric)
- There is limited information regarding FDA-Labeled Use of Progesterone (oral) in pediatric patients.
Off-Label Use and Dosage (Pediatric)
Guideline-Supported Use
- There is limited information regarding Off-Label Guideline-Supported Use of Progesterone (oral) in pediatric patients.
Non–Guideline-Supported Use
- There is limited information regarding Off-Label Non–Guideline-Supported Use of Progesterone (oral) in pediatric patients.
Contraindications
- PROMETRIUM Capsules should not be used in women with any of the following conditions:
- PROMETRIUM Capsules should not be used in patients with known hypersensitivity to its ingredients. PROMETRIUM Capsules contain peanut oil and should never be used by patients allergic to peanuts.
- Undiagnosed abnormal genital bleeding.
- Known, suspected, or history of breast cancer.
- Active deep vein thrombosis, pulmonary embolism or history of these conditions.
- Active arterial thromboembolic disease (for example, stroke and myocardial infarction), or a history of these conditions.
- Known liver dysfunction or disease.
- Known or suspected pregnancy.
Warnings
|
WARNING: CARDIOVASCULAR DISORDERS, BREAST CANCER and PROBABLE DEMENTIA FOR ESTROGEN PLUS PROGESTIN THERAPY
See full prescribing information for complete Boxed Warning.
Cardiovascular Disorders and Probable Dementia:
Breast Cancer:
|
- See BOXED WARNING.
Cardiovascular disorders
- An increased risk of pulmonary embolism, deep vein thrombosis (DVT), stroke, and myocardial infarction has been reported with estrogen plus progestin therapy. Should any of these occur or be suspected, estrogen with progestin therapy should be discontinued immediately.
- Risk factors for arterial vascular disease (for example, hypertension, diabetes mellitus, tobacco use, hypercholesterolemia, and obesity) and/or venous thromboembolism (for example, personal history or family history of venous thromboembolism [VTE], obesity, and systemic lupus erythematosus) should be managed appropriately.
Stroke
- In the Women's Health Initiative (WHI) estrogen plus progestin substudy, a statistically significant increased risk of stroke was reported in women 50 to 79 years of age receiving daily CE (0.625 mg) plus MPA (2.5 mg) compared to women in the same age group receiving placebo (33 versus 25 per 10,000 women-years). The increase in risk was demonstrated after the first year and persisted. Should a stroke occur or be suspected, estrogen plus progestin therapy should be discontinued immediately.
Coronary Heart Disease
- In the WHI estrogen plus progestin substudy, there was a statistically non-significant increased risk of coronary heart disease (CHD) events (defined as nonfatal myocardial infarction [MI], silent MI, or CHD death) reported in women receiving daily CE (0.625 mg) plus MPA (2.5 mg) compared to women receiving placebo (41 versus 34 per 10,000 women-years). An increase in relative risk was demonstrated in year 1 and a trend toward decreasing relative risk was reported in years 2 through 5.
- In postmenopausal women with documented heart disease (n = 2,763, average age 66.7 years), in a controlled clinical trial of secondary prevention of cardiovascular disease (Heart and Estrogen/Progestin Replacement Study [HERS]), treatment with daily CE (0.625 mg) plus MPA (2.5 mg) demonstrated no cardiovascular benefit. During an average follow-up of 4.1 years, treatment with CE plus MPA did not reduce the overall rate of CHD events in postmenopausal women with established coronary heart disease. There were more CHD events in the CE plus MPA-treated group than in the placebo group in year 1, but not during the subsequent years. Two thousand, three hundred and twenty-one (2,321) women from the original HERS trial agreed to participate in an open-label extension of HERS, HERS II. Average follow-up in HERS II was an additional 2.7 years, for a total of 6.8 years overall. Rates of CHD events were comparable among women in the CE plus MPA group and the placebo group in HERS, HERS II, and overall.
Venous Thromboembolism
- In the WHI estrogen plus progestin substudy, a statistically significant 2-fold greater rate of VTE (DVT and pulmonary embolism [PE]) was reported in women receiving daily CE (0.625 mg) plus MPA (2.5 mg) compared to women receiving placebo (35 versus 17 per 10,000 women-years). Statistically significant increases in risk for both DVT (26 versus 13 per 10,000 women-years) and PE (18 versus 8 per 10,000 women-years) were also demonstrated. The increase in VTE risk was demonstrated during the first year and persisted. Should a VTE occur or be suspected, estrogen plus progestin therapy should be discontinued immediately.
- If feasible, estrogens with progestins should be discontinued at least 4 to 6 weeks before surgery of the type associated with an increased risk of thromboembolism, or during periods of prolonged immobilization.
Malignant neoplasms
Breast Cancer
- The most important randomized clinical trial providing information about breast cancer in estrogen plus progestin users is the Women's Health Initiative (WHI) substudy of daily CE (0.625 mg) plus MPA (2.5 mg). After a mean follow-up of 5.6 years, the estrogen plus progestin substudy reported an increased risk of invasive breast cancer in women who took daily CE plus MPA. In this substudy, prior use of estrogen-alone or estrogen plus progestin therapy was reported by 26 percent of the women. The relative risk of invasive breast cancer was 1.24 (95 percent nCI, 1.01-1.54), and the absolute risk was 41 versus 33 cases per 10,000 women-years, for CE plus MPA compared with placebo.
- Among women who reported prior use of hormone therapy, the relative risk of invasive breast cancer was 1.86, and the absolute risk was 46 versus 25 cases per 10,000 women-years, for estrogen plus progestin compared with placebo. Among women who reported no prior use of hormone therapy, the relative risk of invasive breast cancer was 1.09, and the absolute risk was 40 versus 36 cases per 10,000 women-years for CE plus MPA compared with placebo. In the same substudy, invasive breast cancers were larger, were more likely to be node positive, and were diagnosed at a more advanced stage in the CE (0.625 mg) plus MPA (2.5 mg) group compared with the placebo group. Metastatic disease was rare, with no apparent difference between the two groups. Other prognostic factors such as histologic subtype, grade and hormone receptor status did not differ between the groups.
- Consistent with the WHI clinical trials, observational studies have also reported an increased risk of breast cancer for estrogen plus progestin therapy, and a smaller increased risk for estrogen-alone therapy, after several years of use. The risk increased with duration of use, and appeared to return to baseline over about 5 years after stopping treatment (only the observational studies have substantial data on risk after stopping). Observational studies also suggest that the risk of breast cancer was greater, and became apparent earlier, with estrogen plus progestin therapy as compared to estrogen-alone therapy. However, these studies have not generally found significant variation in the risk of breast cancer among different estrogen plus progestin combinations, doses, or routes of administration.
- The use of estrogen plus progestin has been reported to result in an increase in abnormal mammograms requiring further evaluation. All women should receive yearly breast examinations by a healthcare provider and perform monthly breast self-examinations. In addition, mammography examinations should be scheduled based on patient age, risk factors, and prior mammogram results.
Endometrial Cancer
- An increased risk of endometrial cancer has been reported with the use of unopposed estrogen therapy in a woman with a uterus. The reported endometrial cancer risk among unopposed estrogen users is about 2 to 12 times greater than in non-users, and appears dependent on duration of treatment and on estrogen dose. Most studies show no significant increased risk associated with the use of estrogens for less than 1 year. The greatest risk appears associated with prolonged use, with increased risks of 15- to 24-fold for 5 to 10 years or more and this risk has been shown to persist for at least 8 to 15 years after estrogen therapy is discontinued.
- Clinical surveillance of all women using estrogen plus progestin therapy is important. Adequate diagnostic measures, including directed or random endometrial sampling when indicated, should be undertaken to rule out malignancy in all cases of undiagnosed persistent or recurring abnormal genital bleeding. There is no evidence that the use of natural estrogens results in a different endometrial risk profile than synthetic estrogens of equivalent estrogen dose. Adding a progestin to estrogen therapy in postmenopausal women has been shown to reduce the risk of endometrial hyperplasia, which may be a precursor to endometrial cancer.
Ovarian Cancer
- The WHI estrogen plus progestin substudy reported a statistically non-significant increased risk of ovarian cancer. After an average follow-up of 5.6 years, the relative risk for ovarian cancer for CE plus MPA versus placebo was 1.58 (95 percent nCI, 0.77 – 3.24). The absolute risk for CE plus MPA versus placebo was 4 versus 3 cases per 10,000 women-years. In some epidemiologic studies, the use of estrogen plus progestin and estrogen-only products, in particular for 5 or more years, has been associated with an increased risk of ovarian cancer. However, the duration of exposure associated with increased risk is not consistent across all epidemiologic studies and some report no association.
Probable dementia
- In the estrogen plus progestin Women's Health Initiative Memory Study (WHIMS), an ancillary study of WHI, a population of 4,532 postmenopausal women 65 to 79 years of age was randomized to daily CE (0.625 mg) plus MPA (2.5 mg) or placebo.
- In the WHIMS estrogen plus progestin ancillary study, after an average follow-up of 4 years, 40 women in the CE plus MPA group and 21 women in the placebo group were diagnosed with probable dementia. The relative risk of probable dementia for estrogen plus progestin versus placebo was 2.05 (95 percent CI, 1.21-3.48). The absolute risk of probable dementia for CE plus MPA versus placebo was 45 versus 22 cases per 10,000 women-years. It is unknown whether these findings apply to younger postmenopausal women.
Vision abnormalities
- Retinal vascular thrombosis has been reported in patients receiving estrogen. Discontinue estrogen plus progestin therapy pending examination if there is sudden partial or complete loss of vision, or if there is a sudden onset of proptosis, diplopia or migraine. If examination reveals papilledema or retinal vascular lesions, estrogen plus progestin therapy should be permanently discontinued.
Precautions
General
Addition of a progestin when a woman has not had a hysterectomy
- Studies of the addition of a progestin for 10 or more days of a cycle of estrogen administration, or daily with estrogen in a continuous regimen, have reported a lowered incidence of endometrial hyperplasia than would be induced by estrogen treatment alone. Endometrial hyperplasia may be a precursor to endometrial cancer.
- There are, however, possible risks that may be associated with the use of progestins with estrogens compared with estrogen-alone regimens. These include an increased risk of breast cancer.
Fluid Retention
- Progesterone may cause some degree of fluid retention. Women with conditions that might be influenced by this factor, such as cardiac or renal dysfunction, warrant careful observation.
Dizziness and Drowsiness
- PROMETRIUM Capsules may cause transient dizziness and drowsiness and should be used with caution when driving a motor vehicle or operating machinery. PROMETRIUM Capsules should be taken as a single daily dose at bedtime.
Patient Information
- General: This product contains peanut oil and should not be used if you are allergic to peanuts.
- Physicians are advised to discuss the contents of the Patient Information leaflet with patients for whom they prescribe PROMETRIUM Capsules.
Drug-Laboratory Test Interactions
- Increased sulfobromophthalein retention and other hepatic function tests.
- Coagulation tests: increase in prothrombin factors VII, VIII, IX and X.
- Pregnanediol determination.
- Thyroid function: increase in PBI, and butanol extractable protein bound iodine and decrease in T3 uptake values.
The Women's Health Initiative Study
- In the Women's Health Initiative (WHI) estrogen plus progestin substudy (daily CE [0.625 mg] plus MPA [2.5 mg] versus placebo), there was a higher relative risk of nonfatal stroke and invasive breast cancer in women greater than 65 years of age.
The Women's Health Initiative Memory Study
- In the Women's Health Initiative Memory Study (WHIMS) of postmenopausal women 65 to 79 years of age, there was an increased risk of developing probable dementia in the estrogen plus progestin ancillary study when compared to placebo.
Adverse Reactions
Clinical Trials Experience
- See BOXED WARNING, WARNINGS and PRECAUTIONS.
- Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
- In a multicenter, randomized, double-blind, placebo-controlled clinical trial, the effects of PROMETRIUM Capsules on the endometrium was studied in a total of 875 postmenopausal women. Table 6 lists adverse reactions greater than or equal to 2 percent of women who received cyclic PROMETRIUM Capsules 200 mg daily (12 days per calendar month cycle) with 0.625 mg conjugated estrogens or placebo.
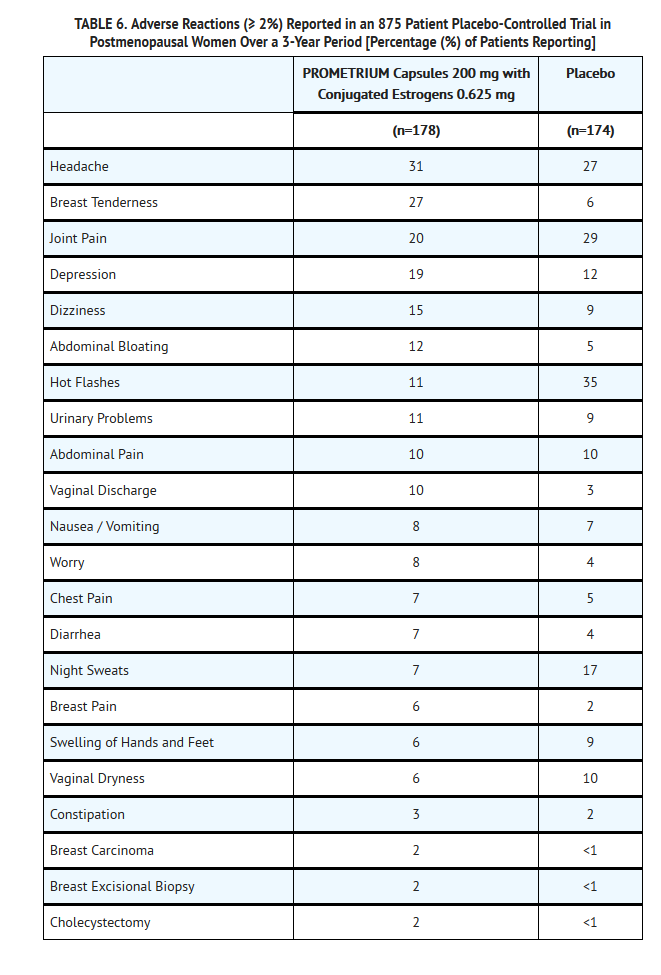
Effects on Secondary Amenorrhea
- In a multicenter, randomized, double-blind, placebo-controlled clinical trial, the effects of PROMETRIUM Capsules on secondary amenorrhea was studied in 49 estrogen-primed postmenopausal women. Table 7 lists adverse reactions greater than or equal to 5 percent of women who received PROMETRIUM Capsules or placebo.
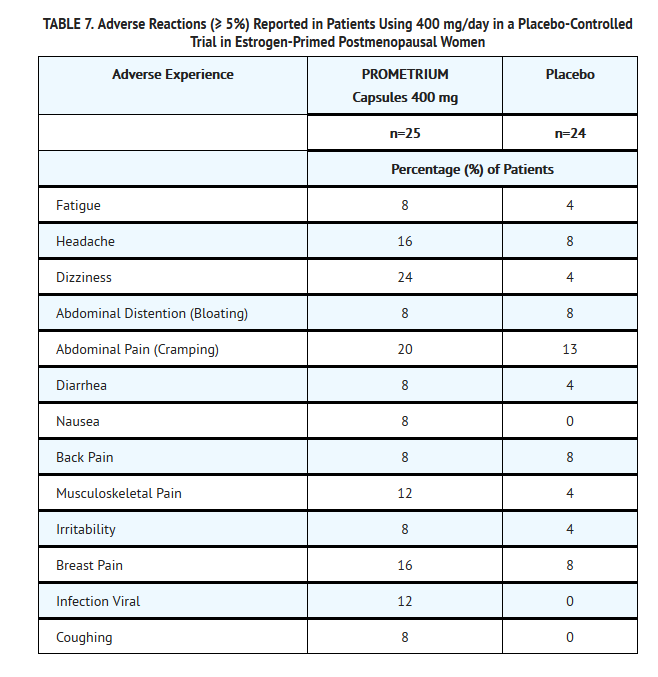
- In a multicenter, parallel-group, open label postmarketing dosing study consisting of three consecutive 28-day treatment cycles, 220 premenopausal women with secondary amenorrhea were randomized to receive daily conjugated estrogens therapy (0.625 mg conjugated estrogens) and PROMETRIUM Capsules, 300 mg per day (n=113) or PROMETRIUM Capsules, 400 mg per /day (n=107) for 10 days of each treatment cycle. Overall, the most frequently reported treatment-emergent adverse reactions, reported in greater than or equal to 5 percent of subjects, were nausea, fatigue, vaginal mycosis, nasopharyngitis, upper respiratory tract infection, headache, dizziness, breast tenderness, abdominal distension, acne, dysmenorrhea, mood swing, and urinary tract infection.
Postmarketing Experience
- The following additional adverse reactions have been reported with PROMETRIUM Capsules. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate the frequency or establish a causal relationship to drug exposure.
- Genitourinary System: endometrial carcinoma, hypospadia, intra-uterine death, menorrhagia, menstrual disorder, metrorrhagia, ovarian cyst, spontaneous abortion.
- Cardiovascular: circulatory collapse, congenital heart disease (including ventricular septal defect and patent ductus arteriosus), hypertension, hypotension, tachycardia.
- Gastrointestinal: acute pancreatitis, cholestasis, cholestatic hepatitis, dysphagia, hepatic failure, hepatic necrosis, hepatitis, increased liver function tests (including alanine aminotransferase increased, aspartate aminotransferase increased, gamma-glutamyl transferase increased), jaundice, swollen tongue.
- Eyes: blurred vision, diplopia, visual disturbance.
- Central Nervous System: aggression, convulsion, depersonalization, depressed consciousness, disorientation, dysarthria, loss of consciousness, paresthesia, sedation, stupor, syncope (with and without hypotension), transient ischemic attack, suicidal ideation.
- During initial therapy, a few women have experienced a constellation of many or all of the following symptoms: extreme dizziness and/or drowsiness, blurred vision, slurred speech, difficulty walking, loss of consciousness, vertigo, confusion, disorientation, feeling drunk, and shortness of breath.
- Miscellaneous: abnormal gait, anaphylactic reaction, arthralgia, blood glucose increased, choking, cleft lip, cleft palate, difficulty walking, dyspnea, face edema feeling abnormal, feeling drunk, hypersensitivity, asthma, muscle cramp, throat tightness, tinnitus, vertigo, weight decreased, weight increased.
Drug Interactions
There is limited information regarding Progesterone (oral) Drug Interactions in the drug label.
Use in Specific Populations
Pregnancy
- PROMETRIUM Capsules should not be used during pregnancy.
Pregnancy Category B: Reproductive studies have been performed in mice at doses up to 9 times the human oral dose, in rats at doses up to 44 times the human oral dose, in rabbits at a dose of 10 mcg/day delivered locally within the uterus by an implanted device, in guinea pigs at doses of approximately one-half the human oral dose and in rhesus monkeys at doses approximately the human dose, all based on body surface area, and have revealed little or no evidence of impaired fertility or harm to the fetus due to progesterone.
Pregnancy Category (AUS):
- Australian Drug Evaluation Committee (ADEC) Pregnancy Category
- There is no Australian Drug Evaluation Committee (ADEC) guidance on usage of Progesterone (oral) in women who are pregnant.
Labor and Delivery
- There is no FDA guidance on use of Progesterone (oral) during labor and delivery.
Nursing Mothers
- Detectable amounts of progestin have been identified in the milk of nursing women receiving progestins. Caution should be exercised when PROMETRIUM Capsules are administered to a nursing woman.
Pediatric Use
- PROMETRIUM Capsules are not indicated in children. Clinical studies have not been conducted in the pediatric population.
Geriatic Use
- There have not been sufficient numbers of geriatric women involved in clinical studies utilizing PROMETRIUM Capsules to determine whether those over 65 years of age differ from younger subjects in their response to PROMETRIUM Capsules.
Gender
- There is no FDA guidance on the use of Progesterone (oral) with respect to specific gender populations.
Race
- There is no FDA guidance on the use of Progesterone (oral) with respect to specific racial populations.
Renal Impairment
- There is no FDA guidance on the use of Progesterone (oral) in patients with renal impairment.
Hepatic Impairment
- There is no FDA guidance on the use of Progesterone (oral) in patients with hepatic impairment.
Females of Reproductive Potential and Males
- There is no FDA guidance on the use of Progesterone (oral) in women of reproductive potentials and males.
Immunocompromised Patients
- There is no FDA guidance one the use of Progesterone (oral) in patients who are immunocompromised.
Administration and Monitoring
Administration
Prevention of Endometrial Hyperplasia
- PROMETRIUM Capsules should be given as a single daily dose at bedtime, 200 mg orally for 12 days sequentially per 28-day cycle, to a postmenopausal woman with a uterus who is receiving daily conjugated estrogens tablets.
Treatment of Secondary Amenorrhea
- PROMETRIUM Capsules may be given as a single daily dose of 400 mg at bedtime for 10 days.
- Some women may experience difficulty swallowing PROMETRIUM Capsules. For these women, PROMETRIUM Capsules should be taken with a glass of water while in the standing position.
Monitoring
- There is limited information regarding Monitoring of Progesterone (oral) in the drug label.
- Description
IV Compatibility
- There is limited information regarding IV Compatibility of Progesterone (oral) in the drug label.
Overdosage
- No studies on overdosage have been conducted in humans. In the case of overdosage, PROMETRIUM Capsules should be discontinued and the patient should be treated symptomatically.
Pharmacology

Mechanism of Action
Structure
- PROMETRIUM (progesterone, USP) Capsules contain micronized progesterone for oral administration. Progesterone has a molecular weight of 314.47 and a molecular formula of C21H30O2. Progesterone (pregn-4-ene-3, 20-dione) is a white or creamy white, odorless, crystalline powder practically insoluble in water, soluble in alcohol, acetone and dioxane and sparingly soluble in vegetable oils, stable in air, melting between 126° and 131°C. The structural formula is:
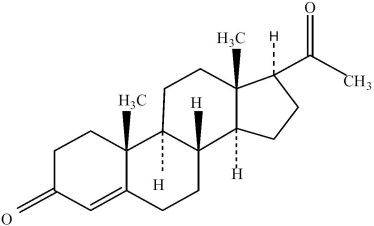
- Progesterone is synthesized from a starting material from a plant source and is chemically identical to progesterone of human ovarian origin. PROMETRIUM Capsules are available in multiple strengths to afford dosage flexibility for optimum management. PROMETRIUM Capsules contain 100 mg or 200 mg micronized progesterone.
- The inactive ingredients for PROMETRIUM Capsules 100 mg include: peanut oil NF, gelatin NF, glycerin USP, lecithin NF, titanium dioxide USP, FD&C Red No. 40, and D&C Yellow No. 10.
- The inactive ingredients for PROMETRIUM Capsules 200 mg include: peanut oil NF, gelatin NF, glycerin USP, lecithin NF, titanium dioxide USP, D&C Yellow No. 10, and FD&C Yellow No. 6.
Pharmacodynamics
- There is limited information regarding Pharmacodynamics of Progesterone (oral) in the drug label.
Pharmacokinetics
- PROMETRIUM Capsules are an oral dosage form of micronized progesterone which is chemically identical to progesterone of ovarian origin. The oral bioavailability of progesterone is increased through micronization.
Pharmacokinetics
Absorption
- After oral administration of progesterone as a micronized soft-gelatin capsule formulation, maximum serum concentrations were attained within 3 hours. The absolute bioavailability of micronized progesterone is not known. Table 1 summarizes the mean pharmacokinetic parameters in postmenopausal women after five oral daily doses of PROMETRIUM Capsules 100 mg as a micronized soft-gelatin capsule formulation.
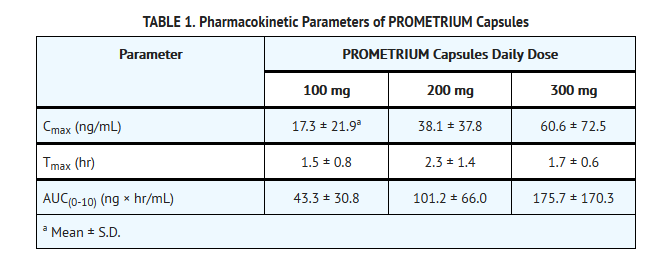
- Serum progesterone concentrations appeared linear and dose proportional following multiple dose administration of PROMETRIUM Capsules 100 mg over the dose range 100 mg per day to 300 mg per day in postmenopausal women. Although doses greater than 300 mg per day were not studied in females, serum concentrations from a study in male volunteers appeared linear and dose proportional between 100 mg per day and 400 mg per day. The pharmacokinetic parameters in male volunteers were generally consistent with those seen in postmenopausal women.
Distribution
- Progesterone is approximately 96 percent to 99 percent bound to serum proteins, primarily to serum albumin (50 to 54 percent) and transcortin (43 to 48 percent).
Metabolism
- Progesterone is metabolized primarily by the liver largely to pregnanediols and pregnanolones. Pregnanediols and pregnanolones are conjugated in the liver to glucuronide and sulfate metabolites. Progesterone metabolites which are excreted in the bile may be deconjugated and may be further metabolized in the intestine via reduction, dehydroxylation, and epimerization.
Excretion
- The glucuronide and sulfate conjugates of pregnanediol and pregnanolone are excreted in the bile and urine. Progesterone metabolites are eliminated mainly by the kidneys. Progesterone metabolites which are excreted in the bile may undergo enterohepatic recycling or may be excreted in the feces.
Special Populations
- The pharmacokinetics of PROMETRIUM Capsules have not been assessed in low body weight or obese patients.
- Hepatic Insufficiency: The effect of hepatic impairment on the pharmacokinetics of PROMETRIUM Capsules has not been studied.
- Renal Insufficiency: The effect of renal impairment on the pharmacokinetics of PROMETRIUM Capsules has not been studied.
Food–Drug Interaction
- Concomitant food ingestion increased the bioavailability of PROMETRIUM Capsules relative to a fasting state when administered to postmenopausal women at a dose of 200 mg.
Drug Interactions
- The metabolism of progesterone by human liver microsomes was inhibited by ketoconazole (IC50 < 0.1 μM). Ketoconazole is a known inhibitor of cytochrome P450 3A4, hence these data suggest that ketoconazole or other known inhibitors of this enzyme may increase the bioavailability of progesterone. The clinical relevance of the in vitro findings is unknown.
- Coadministration of conjugated estrogens and PROMETRIUM Capsules to 29 postmenopausal women over a 12-day period resulted in an increase in total estrone concentrations (Cmax 3.68 ng/mL to 4.93 ng/mL) and total equilin concentrations (Cmax 2.27 ng/mL to 3.22 ng/mL) and a decrease in circulating 17β estradiol concentrations (Cmax 0.037 ng/mL to 0.030 ng/mL). The half-life of the conjugated estrogens was similar with coadministration of PROMETRIUM Capsules. Table 2 summarizes the pharmacokinetic parameters.

Nonclinical Toxicology
Carcinogenesis, Mutagenesis, Impairment of Fertility
- Progesterone has not been tested for carcinogenicity in animals by the oral route of administration. When implanted into female mice, progesterone produced mammary carcinomas, ovarian granulosa cell tumors and endometrial stromal sarcomas. In dogs, long-term intramuscular injections produced nodular hyperplasia and benign and malignant mammary tumors. Subcutaneous or intramuscular injections of progesterone decreased the latency period and increased the incidence of mammary tumors in rats previously treated with a chemical carcinogen.
- Progesterone did not show evidence of genotoxicity in in vitro studies for point mutations or for chromosomal damage. In vivo studies for chromosome damage have yielded positive results in mice at oral doses of 1000 mg/kg and 2000 mg/kg. Exogenously administered progesterone has been shown to inhibit ovulation in a number of species and it is expected that high doses given for an extended duration would impair fertility until the cessation of treatment.
Clinical Studies
Effects on the endometrium
- In a randomized, double-blind clinical trial, 358 postmenopausal women, each with an intact uterus, received treatment for up to 36 months. The treatment groups were: PROMETRIUM Capsules at the dose of 200 mg per day for 12 days per 28-day cycle in combination with conjugated estrogens 0.625 mg per day (n=120); conjugated estrogens 0.625 mg per day only (n=119); or placebo (n=119). The subjects in all three treatment groups were primarily Caucasian women (87 percent or more of each group). The results for the incidence of endometrial hyperplasia in women receiving up to 3 years of treatment are shown in Table 3. A comparison of the PROMETRIUM Capsules plus conjugated estrogens treatment group to the conjugated estrogens only group showed a significantly lower rate of hyperplasia (6 percent combination product versus 64 percent estrogen alone) in the PROMETRIUM Capsules plus conjugated estrogens treatment group throughout 36 months of treatment.

- The times to diagnosis of endometrial hyperplasia over 36 months of treatment are shown in Figure 1. This figure illustrates graphically that the proportion of patients with hyperplasia was significantly greater for the conjugated estrogens group (64 percent) compared to the conjugated estrogens plus PROMETRIUM Capsules group (6 percent).
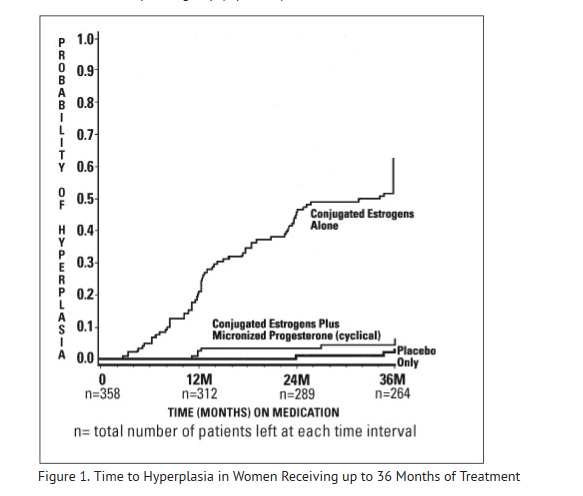
- The discontinuation rates due to hyperplasia over the 36 months of treatment are as shown in Table 4. For any degree of hyperplasia, the discontinuation rate for patients who received conjugated estrogens plus PROMETRIUM Capsules was similar to that of the placebo only group, while the discontinuation rate for patients who received conjugated estrogens alone was significantly higher. Women who permanently discontinued treatment due to hyperplasia were similar in demographics to the overall study population.
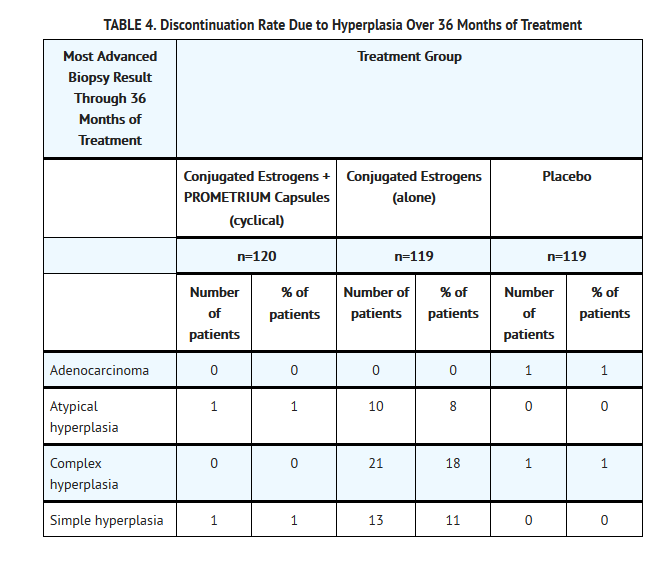
Effects on secondary amenorrhea
- In a single-center, randomized, double-blind clinical study that included premenopausal women with secondary amenorrhea for at least 90 days, administration of 10 days of PROMETRIUM Capsules therapy resulted in 80 percent of women experiencing withdrawal bleeding within 7 days of the last dose of PROMETRIUM Capsules, 300 mg per day (n=20), compared to 10 percent of women experiencing withdrawal bleeding in the placebo group (n=21).
- In a multicenter, parallel-group, open label, postmarketing dosing study that included premenopausal women with secondary amenorrhea for at least 90 days, administration of 10 days of PROMETRIUM Capsules during two 28-day treatment cycles, 300 mg per day (n=107) or 400 mg per day (n=99), resulted in 73.8 percent and 76.8 percent of women, respectively, experiencing withdrawal bleeding.
- The rate of secretory transformation was evaluated in a multicenter, randomized, double-blind clinical study in estrogen-primed postmenopausal women. PROMETRIUM Capsules administered orally for 10 days at 400 mg per day (n=22) induced complete secretory changes in the endometrium in 45 percent of women compared to 0 percent in the placebo group (n=23).
- A second multicenter, parallel-group, open label postmarketing dosing study in premenopausal women with secondary amenorrhea for at least 90 days also evaluated the rate of secretory transformation. All subjects received daily oral conjugated estrogens over 3 consecutive 28-day treatment cycles and PROMETRIUM Capsules, 300 mg per day (n=107) or 400 mg per day (n=99) for 10 days of each treatment cycle. The rate of complete secretory transformation was 21.5 percent and 28.3 percent, respectively.
Women's Health Initiative Studies
- The Women's Health Initiative (WHI) enrolled approximately 27,000 predominantly healthy postmenopausal women in two substudies to assess the risks and benefits of daily oral conjugated estrogens (CE) [0.625 mg]-alone or in combination with medroxyprogesterone acetate (MPA) [2.5 mg] compared to placebo in the prevention of certain chronic diseases. The primary endpoint was the incidence of coronary heart disease [(CHD) defined as nonfatal myocardial infarction (MI), silent MI and CHD death], with invasive breast cancer as the primary adverse outcome. A “global index” included the earliest occurrence of CHD, invasive breast cancer, stroke, pulmonary embolism (PE), endometrial cancer (only in the CE plus MPA substudy), colorectal cancer, hip fracture, or death due to other cause. These sub studies did not evaluate the effects of CE–alone or CE plus MPA on menopausal symptoms.
WHI estrogen plus progestin Substudy
- The WHI estrogen plus progestin substudy was stopped early. According to the predefined stopping rule, after an average follow-up of 5.6 years of treatment, the increased risk of breast cancer and cardiovascular events exceeded the specified benefits included in the “global index.” The absolute excess risk of events in the “global index” was 19 per 10,000 women-years.
- For those outcomes included in the WHI “global index” that reached statistical significance after 5.6 years of follow-up, the absolute excess risks per 10,000 women-years in the group treated with CE plus MPA were 7 more CHD events, 8 more strokes, 10 more PEs, and 8 more invasive breast cancers, while the absolute risk reductions per 10,000 women-years were 6 fewer colorectal cancers and 5 fewer hip fractures.
- Results of the estrogen plus progestin substudy, which included 16,608 women (average 63 years of age, range 50 to 79; 83.9 percent White, 6.8 percent Black, 5.4 percent Hispanic, 3.9 percent Other) are presented in Table 5. These results reflect centrally adjudicated data after an average follow-up of 5.6 years.

- Timing of the initiation of estrogen plus progestin therapy relative to the start of menopause may affect the overall risk benefit profile. The WHI estrogen plus progestin substudy stratified for age showed in women 50 to 59 years of age a non-significant trend toward reducing risk of overall mortality [hazard ratio (HR) 0.69 (95 percent CI, 0.44-1.07)].
Women's Health Initiative Memory Study
- The estrogen plus progestin Women's Health Initiative Memory Study (WHIMS), an ancillary study of WHI, enrolled 4,532 predominantly healthy postmenopausal women 65 years of age and older (47 percent were 65 to 69 years of age; 35 percent were 70 to 74 years of age; and 18 percent were 75 years of age and older) to evaluate the effects of daily CE (0.625 mg) plus MPA (2.5 mg) on the incidence of probable dementia (primary outcome) compared to placebo.
- After an average follow-up of 4 years, the relative risk of probable dementia for CE plus MPA versus placebo was 2.05 (95 percent CI, 1.21 – 3.48). The absolute risk of probable dementia for CE plus MPA versus placebo was 45 versus 22 per 10,000 women-years. Probable dementia as defined in this study included Alzheimer's disease (AD), vascular dementia (VaD) and mixed type (having features of both AD and VaD). The most common classification of probable dementia in the treatment group and the placebo group was AD. Since the ancillary study was conducted in women 65 to 79 years of age, it is unknown whether these findings apply to younger postmenopausal women.
How Supplied
- PROMETRIUM (progesterone, USP) Capsules 100 mg are round, peach-colored capsules branded with black imprint “SV.”
- NDC 0032-1708-01 (Bottle of 100)
- PROMETRIUM (progesterone, USP) Capsules 200 mg are oval, pale yellow-colored capsules branded with black imprint “SV2.”
- NDC 0032-1711-01 (Bottle of 100)
Storage
- Store at 25°C (77°F); excursions permitted to 15° to 30°C (59° to 86°F) [See USP Controlled Room Temperature].
- Protect from excessive moisture.
- Dispense in tight, light-resistant container as defined in USP/NF, accompanied by a Patient Insert.
- Keep out of reach of children.
Images
Drug Images
{{#ask: Page Name::Progesterone (oral) |?Pill Name |?Drug Name |?Pill Ingred |?Pill Imprint |?Pill Dosage |?Pill Color |?Pill Shape |?Pill Size (mm) |?Pill Scoring |?NDC |?Drug Author |format=template |template=DrugPageImages |mainlabel=- |sort=Pill Name }}
Package and Label Display Panel


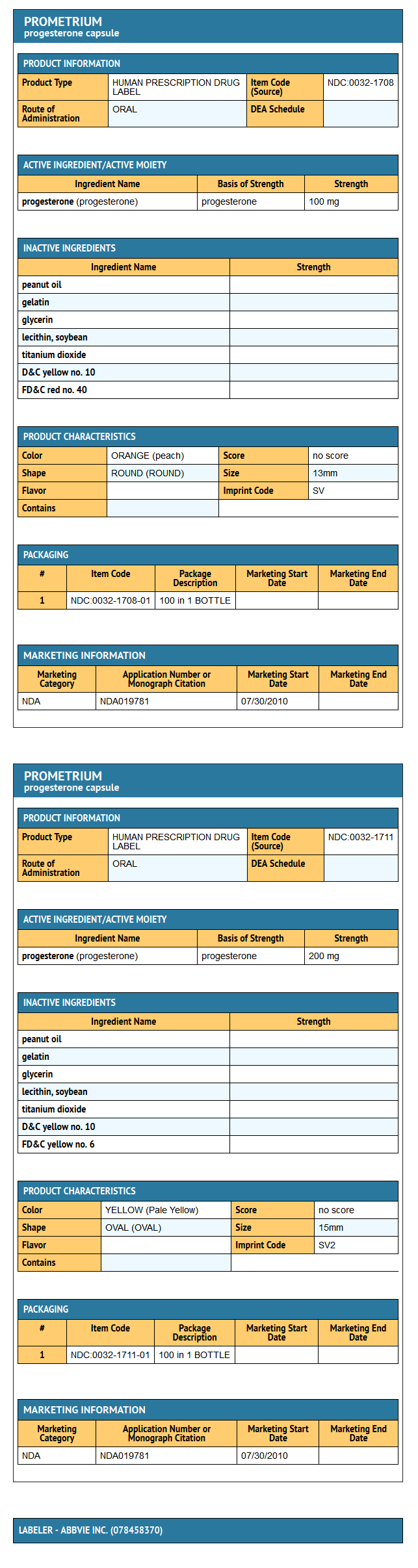
{{#ask: Label Page::Progesterone (oral) |?Label Name |format=template |template=DrugLabelImages |mainlabel=- |sort=Label Page }}
Patient Counseling Information
- General: This product contains peanut oil and should not be used if you are allergic to peanuts.
- Physicians are advised to discuss the contents of the Patient Information leaflet with patients for whom they prescribe PROMETRIUM Capsules.

Precautions with Alcohol
- Alcohol-Progesterone (oral) interaction has not been established. Talk to your doctor about the effects of taking alcohol with this medication.
Brand Names
Crinone, Prochieve, Prometrium, Endometrin.
Look-Alike Drug Names
There is limited information regarding Progesterone (oral) Look-Alike Drug Names in the drug label.
Drug Shortage Status
Price
References
The contents of this FDA label are provided by the National Library of Medicine.
{{#subobject:
|Page Name=Progesterone (oral)
|Pill Name=No image.jpg
|Drug Name=
|Pill Ingred=|+sep=;
|Pill Imprint=
|Pill Dosage={{{dosageValue}}} {{{dosageUnit}}}
|Pill Color=|+sep=;
|Pill Shape=
|Pill Size (mm)=
|Pill Scoring=
|Pill Image=
|Drug Author=
|NDC=
}}