Ovarian cyst
For patient information, click here
| Ovarian cyst | |
| ICD-10 | N83.2 |
|---|---|
| ICD-9 | 620.0-620.2 |
| DiseasesDB | 9433 |
| MedlinePlus | 001504 |
|
WikiDoc Resources for Ovarian cyst |
|
Articles |
|---|
|
Most recent articles on Ovarian cyst Most cited articles on Ovarian cyst |
|
Media |
|
Powerpoint slides on Ovarian cyst |
|
Evidence Based Medicine |
|
Clinical Trials |
|
Ongoing Trials on Ovarian cyst at Clinical Trials.gov Clinical Trials on Ovarian cyst at Google
|
|
Guidelines / Policies / Govt |
|
US National Guidelines Clearinghouse on Ovarian cyst
|
|
Books |
|
News |
|
Commentary |
|
Definitions |
|
Patient Resources / Community |
|
Patient resources on Ovarian cyst Discussion groups on Ovarian cyst Patient Handouts on Ovarian cyst Directions to Hospitals Treating Ovarian cyst Risk calculators and risk factors for Ovarian cyst
|
|
Healthcare Provider Resources |
|
Causes & Risk Factors for Ovarian cyst |
|
Continuing Medical Education (CME) |
|
International |
|
|
|
Business |
|
Experimental / Informatics |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]
Overview
An ovarian cyst is any collection of fluid, surrounded by a very thin wall, within an ovary. Any ovarian follicle that is larger than about two centimeters is termed an ovarian cyst. An ovarian cyst can be as small as a pea, or as large as a grapefruit.
Most ovarian cysts are functional in nature, and harmless (benign).[2] In the US ovarian cysts are found in nearly all premenopausal women, and in up to 14.8% of postmenopausal women. The incidence of ovarian carcinoma is approximately 15 cases per 100,000 women per year.[3]
Ovarian cysts affect women of all ages. They occur most often, however, during a woman's childbearing years.
Some ovarian cysts cause problems, such as bleeding and pain. Surgery may be required to remove those cysts.
Types
Functional cysts
Some, called functional cysts, or simple cysts, are part of the normal process of menstruation. They have nothing to do with disease, and can be treated.
Graafian follicle cyst
One type of simple cyst, which is the most common type of ovarian cyst, is the graafian follicle cyst, follicular cyst, or dentigerous cyst. This type can form when ovulation doesn't occur, and a follicle doesn't rupture or release its egg but instead grows until it becomes a cyst, or when a mature follicle involutes (collapses on itself). It usually forms during ovulation, and can grow to about 2.3 inches in diameter. It is thin-walled, lined by one or more layers of granulosa cell, and filled with clear fluid. Its rupture can create sharp, severe pain on the side of the ovary on which the cyst appears. This sharp pain (sometimes called mittelschmerz) occurs in the middle of the menstrual cycle, during ovulation. About a fourth of women with this type of cyst experience pain. Usually, these cysts produce no symptoms and disappear by themselves within a few months. Ultrasound is the primary tool used to document the follicular cyst. A pelvic exam will also aid in the diagnosis if the cyst is large enough to be seen. A doctor monitors these to make sure they disappear, and looks at treatment options if they do not.[4][5][6][7][8][9][10]
Corpus luteum cyst
Another is a corpus luteum cyst (which may rupture about the time of menstruation, and take up to three months to disappear entirely). This type of functional cyst occurs after an egg has been released from a follicle. The follicle then becomes a new, temporarily little secretory gland that is known as a corpus luteum. The ruptured follicle begins producing large quantities of estrogen and progesterone in preparation for conception. If a pregnancy doesn't occur, the corpus luteum usually breaks down and disappears. It may, however, fill with fluid or blood, causing the corpus luteum to expand into a cyst, and stay on the ovary. Usually, this cyst is on only one side, and does not produce any symptoms.[11][12][13] It can however grow to almost 4 inches in diameter and has the potential to bleed into itself or twist the ovary, causing pelvic or abdominal pain. If it fills with blood, the cyst may rupture, causing internal bleeding and sudden, sharp pain. The fertility drug clomiphene citrate (Clomid, Serophene), used to induce ovulation, increases the risk of a corpus luteum cyst developing after ovulation. These cysts don't prevent or threaten a resulting pregnancy.[14][15] Women on birth control pills usually do not form these cysts; in fact, preventing these cysts is one way the pill works.[16]
Hemorrhagic cyst
A third type of functional cyst, which is common, is a Hemorrhagic cyst, which is also called a blood cyst, hematocele, and hematocyst.[17] It occurs when a very small blood vessel in the wall of the cyst breaks, and the blood enters the cyst. Abdominal pain on one side of the body, often the right side, may be present. The bleeding may occur quickly, and rapidly stretch the covering of the ovary, causing pain. As the blood collects within the ovary, clots form which can be seen on a sonogram.[18] Occasionally hemorrhagic cysts can rupture, with blood entering the abdominal cavity. No blood is seen out of the vagina. If a cyst ruptures, it is usually very painful. Hemorrhagic cysts that rupture are less common. Most hemorrhagic cysts are self-limiting; some need surgical intervention. Even if a hemorrhagic cyst ruptures, in many cases it resolves without surgery. Patients who don't require surgery will experience pain for 4 - 10 days after, and may require several days rest. Studies have found that women on tetracycline antibiotics recover 25% earlier than the majority of patients, a surprising correlation found in 2004. Sometimes surgery is necessary,[19][20] such as a laparoscopy ("belly-button surgery" that uses small tools inserted through one or more tiny slits in the abdomen).[21]
Dermoid cyst
A dermoid cyst, also called a dermoid or mature cystic teratoma, is an abnormal relatively rare cyst that usually affects women during their childbearing years (15-40; the average age is 30), is usually benign, and can range in size from half an inch to 17 inches in diameter. It is similar to those present on skin tissue, and can contain fat and occasionally hair, bone, nails, teeth, eyes, cartilage, and thyroid tissue. Up to 10-15% of women with them have them in both ovaries. It develops from a totipotential germ cell (a primary oocyte) that is retained within the ovary. A CT scan and MRI can show the presence of fat and dense calcifications. Though it often does not cause any symptoms, it can on the other hand become inflamed, and can also twist around (a condition known as ovarian torsion), causing severe abdominal pain and imperiling its blood supply, which is an emergency and calls for urgent surgery. These cysts can generally be removed easily, which is usually the treatment of choice, with either conventional surgery (laparotomy; open surgery) or laparoscopy. Removal does not generally affect fertility. The larger it is, the greater the risk of rupture with spillage of the contents, which can create problems with adhesions and pain. Although the large majority (about 98%) are benign, the remaining fraction (about 2%) becomes cancerous (malignant) -- those are usually in women over 40. [22][23][24][25]
Endometrioid cyst
An endometrioma, endometrioid cyst, endometrial cyst, or chocolate cyst is caused by endometriosis, and formed when a tiny patch of endometrial tissue (the mucous membrane that makes up the inner layer of the uterine wall) bleeds, sloughs off, becomes transplanted, and grows and enlarges inside the ovaries. As the blood builds up over months and years, it turns brown. When it ruptures, the material spills over into the pelvis and onto the surface of the uterus, bladder, bowel, and the corresponding spaces between. Treatment for endometriosis can be medical or surgical. Nonsteroidal anti-inflammatory drugs (NSAIDs) are frequently used first in patients with pelvic pain, particularly if the diagnosis of endometriosis has not been definitively established. The goal of directed medical treatment is to achieve an anovulatory state. Typically, this is achieved initially using hormonal contraception. This can also be accomplished with progestational agents (i.e., medroxyprogesterone), danazol, gestrinone, or gonadotropin-releasing hormone agonists (GnRH), as well as other less well-known agents. These agents are generally used if oral contraceptives and NSAIDs are ineffective. GnRH can be combined with estrogen and progestogen (add-back therapy) without loss of efficacy but with fewer hypoestrogenic symptoms. Laparoscopic surgical approaches include ablation of implants, lysis of adhesions, removal of endometriomas, uterosacral nerve ablation, and presacral neurectomy. They frequently require surgical removal. Conservative surgery can be performed to preserve fertility in young patients. Laparoscopic surgery provides pain relief and improved fertility over diagnostic laparoscopy without surgery. Definitive surgery is a hysterectomy and bilateral oophorectomy. [26][27][28][29][30]
Pathological cysts
Other cysts are pathological, such as those found in polycystic ovary syndrome, or those associated with tumors.
A polycystic-appearing ovary is diagnosed based on its enlarged size — usually twice normal —with small cysts present around the outside of the ovary. It can be found in "normal" women, and in women with endocrine disorders. An ultrasound is used to view the ovary in diagnosing the condition. Polycystic-appearing ovary is different from the polycystic ovarian syndrome, which includes other symptoms in addition to the presence of ovarian cysts, and involves metabolic and cardiovascular risks linked to insulin resistance. These risks include increased glucose tolerance, type 2 diabetes, and high blood pressure. Polycystic ovarian syndrome is associated with infertility, abnormal bleeding, increased incidences of pregnancy loss, and pregnancy-related complications. Polycystic ovarian syndrome is extremely common, is thought to occur in 4-7% of women of reproductive age, and is associated with an increased risk for endometrial cancer. More tests than an ultrasound alone are required to diagnose polycystic ovarian syndrome.
Ovarian cyst differential diagnosis
| Disease | Findings |
|---|---|
| Ectopic pregnancy | History of missed menses, positive pregnancy test, ultrasound reveals an empty uterus and may show a mass in the fallopian tubes.[1] |
| Appendicitis | Pain localized to the right iliac fossa, vomiting, abdominal ultrasound sensitivity for diagnosis of acute appendicitis is 75% to 90%.[2] |
| Rupturedovarian cyst | Usually spontaneous, can follow history of trauma, mild chronic lower abdominal discomfort may suddenly intensify, ultrasound is diagnostic.[3] |
| Ovarian cyst torsion | Presents with acute severe unilateral lower quadrant abdominal pain, nausea and vomiting, tender adnexal mass palpated in 90%, ultrasound is diagnostic.[4] |
| Hemorrhagic ovarian cyst | Presents with localized abdominal pain, nausea and vomiting. Hypovolemic shock may be present, abdominal tenderness and guarding are physical exam findings, ultrasound is diagnostic.[4] |
| Endometriosis | Presents with cyclic pain that is exacerbated by onset of menses, dyspareunia. laparoscopic exploration is diagnostic.[4] |
| Acute cystitis | Presents with features of increased urinary frequency, urgency, dysuria, and suprapubic pain.[5][6] |
Symptoms
Some or all of the following symptoms may be present, though it is possible not to experience any symptoms:
- Dull aching, or severe, sudden, and sharp pain or discomfort in the lower abdomen (one or both sides), pelvis, vagina, lower back, or thighs; pain may be constant or intermittent -- this is the most common symptom
- Fullness, heaviness, pressure, swelling, or bloating in the abdomen
- Breast tenderness
- Pain during or shortly after beginning or end of menstrual period
- Irregular periods, or abnormal uterine bleeding or spotting
- Change in frequency or ease of urination (such as inability to fully empty the bladder), or difficulty with bowel movements due to pressure on adjacent pelvic anatomy
- Weight gain
- Nausea or vomiting
- Fatigue
- Infertility
- Increased level of hair growth
- Increased facial hair or body hair
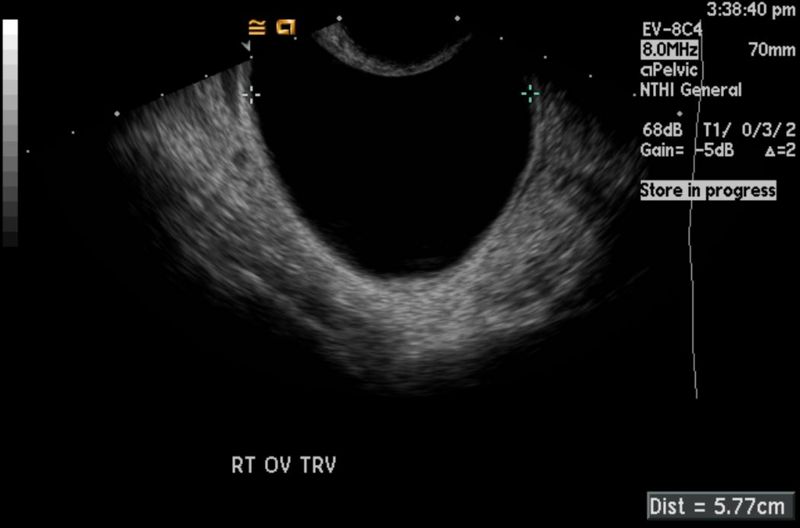
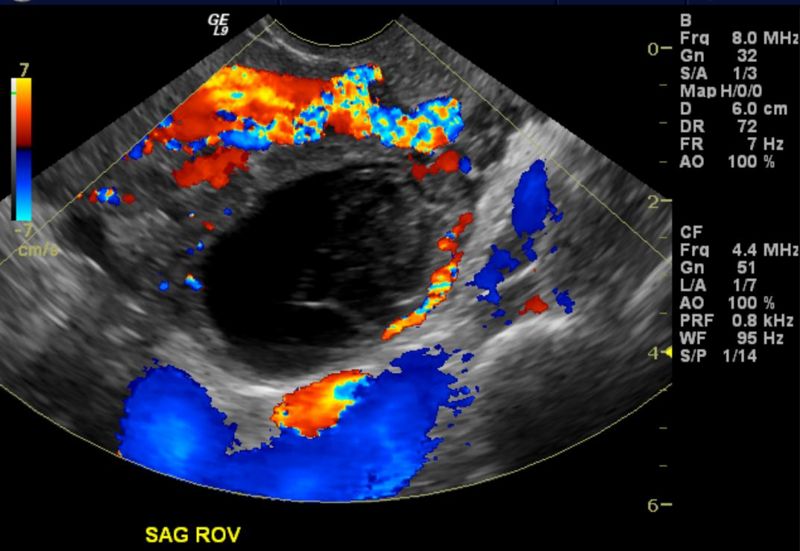
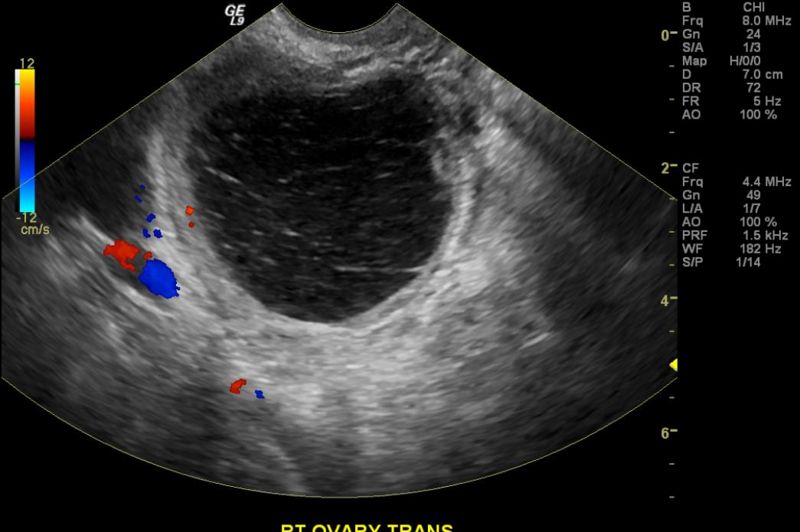
Imaging studies
CT and US images demonstrate a right ovarian cyst
Imaging Findings for Hemorrhagic ovarian cyst
- Hemorrhagic cysts have a variety of appearances depending on the stage of evolution of the clot.
- Most typically appearance: lacelike reticular echoes or an intracystic solid clot are most typical.
- Complex cysts with such appearances should lead to follow-up US or further assessment with MR imaging.
- The most helpful feature in distinguishing hemorrhagic cysts from ovarian neoplasms is the presence of papillary projections and nodular septa in the latter.
Patient #1
Patient #2: Lacelike internal echos are noted in this hemorrhage ovarian cyst
Treatment
About 95% of ovarian cysts are benign, meaning they are not cancerous.
Treatment for cysts depends on the size of the cyst and symptoms. For small, asymptomatic cysts, the wait and see approach with regular check-ups will most likely be recommended.
Pain caused by ovarian cysts may be treated with:
- pain relievers, including nonsteroidal anti-inflammatory drugs such as ibuprofen (Motrin, Advil), acetaminophen (Tylenol), or narcotic pain medicine (by prescription) may help reduce pelvic pain.[31] NSAIDs usually work best when taken at the first signs of the pain.
- a warm bath, or heating pad, or hot water bottle applied to the lower abdomen near the ovaries can relax tense muscles and relieve cramping, lessen discomfort, and stimulate circulation and healing in the ovaries.[32] Bags of ice covered with towels can be used alternately as cold treatments to increase local circulation.[33]
- chamomile herbal tea (Matricaria recutita) can reduce ovarian cyst pain and soothe tense muscles.[34][35]
- urinating as soon as the urge presents itself.[36]
- avoiding constipation, which does not cause ovarian cysts but may further increase pelvic discomfort.[37]
- in diet, eliminating caffeine and alcohol, reducing sugars, increasing foods rich in vitamin A and carotenoids (e.g., carrots, tomatoes, and salad greens) and B vitamins (e.g., whole grains).[38]
- combined methods of hormonal contraception such as the combined oral contraceptive pill -- the hormones in the pills may regulate the menstrual cycle, prevent the formation of follicles that can turn into cysts, and possibly shrink an existing cyst. (American College of Obstetricians and Gynecologists, 1999c; Mayo Clinic, 2002e)[39]
Also, limiting strenuous activity may reduce the risk of cyst rupture or torsion.
Cysts that persist beyond two or three menstrual cycles, or occur in post-menopausal women, may indicate more serious disease and should be investigated through ultrasonography and laparoscopy, especially in cases where family members have had ovarian cancer. Such cysts may require surgical biopsy. Additionally, a blood test may be taken before surgery to check for elevated CA-125, a tumor marker, which is often found in increased levels in ovarian cancer, although it can also be elevated by other conditions resulting in a large number of false positives.
For more serious cases where cysts are large and persisting, doctors may suggest surgery. Some surgeries can be performed to successfully remove the cyst(s) without hurting the ovaries, while others may require removal of one or both ovaries.[40]
Contraindicated medications
Ovarian cyst is considered an absolute contraindication to the use of the following medications:
Template:Diseases of the pelvis, genitals and breasts it:Cisti ovarica
- ↑ Morin L, Cargill YM, Glanc P (2016). "Ultrasound Evaluation of First Trimester Complications of Pregnancy". J Obstet Gynaecol Can. 38 (10): 982–988. doi:10.1016/j.jogc.2016.06.001. PMID 27720100.
- ↑ Balthazar EJ, Birnbaum BA, Yee J, Megibow AJ, Roshkow J, Gray C (1994). "Acute appendicitis: CT and US correlation in 100 patients". Radiology. 190 (1): 31–5. doi:10.1148/radiology.190.1.8259423. PMID 8259423.
- ↑ Bottomley C, Bourne T (2009). "Diagnosis and management of ovarian cyst accidents". Best Pract Res Clin Obstet Gynaecol. 23 (5): 711–24. doi:10.1016/j.bpobgyn.2009.02.001. PMID 19299205.
- ↑ 4.0 4.1 4.2 Bhavsar AK, Gelner EJ, Shorma T (2016). "Common Questions About the Evaluation of Acute Pelvic Pain". Am Fam Physician. 93 (1): 41–8. PMID 26760839.
- ↑ {{Cite journal | author = W. E. Stamm | title = Etiology and management of the acute urethral syndrome | journal = Sexually transmitted diseases | volume = 8 | issue = 3 | pages = 235–238 | year = 1981 | month = July-September | pmid = 7292216
- ↑ {{Cite journal | author = W. E. Stamm, K. F. Wagner, R. Amsel, E. R. Alexander, M. Turck, G. W. Counts & K. K. Holmes | title = Causes of the acute urethral syndrome in women | journal = The New England journal of medicine | volume = 303 | issue = 8 | pages = 409–415 | year = 1980 | month = August | doi = 10.1056/NEJM198008213030801 | pmid = 6993946